Abstract
This study investigated the behavioral intention of Filipino older adults toward using telemedicine and the pivotal role of initial trust in influencing this intention. A cross-sectional method was employed, involving a questionnaire administered to 180 participants using convenience sampling. The structural model test results indicate that subjective norm, attitude, and notably, initial trust positively impact the behavioral intention to use telemedicine, whereas perceived behavioral control does not significantly affect intention. This underscores the significance of subjective norm and attitude in shaping behavioral intention, consistent with the Theory of Planned Behavior (TPB), while the extended construct of initial trust played a crucial role in influencing the attitude and intention of older adults, highlighting its importance in technology adoption. The study aligns with the trend of increased telemedicine adoption during the COVID-19 pandemic, emphasizing the need for trust in sensitive healthcare contexts. Establishing initial trust is vital for successful telemedicine implementation among Filipino older adults, enhancing healthcare accessibility and well-being.
Introduction
Aging is a stage where happiness and productivity can be experienced, and where legacy-building can be achieved. These goals are largely affected by several socioeconomic factors (Mhaske, 2017). The World Health Organization (WHO) supports the United Nations Decade of Healthy Ageing (2021–2030) by working on supportive factors such as an age-friendly environment, integrated and long-term care, and combating ageism (World Health Organization [WHO], 2023). Studies show that healthy aging is feasible given that an appropriate environment and opportunities are provided for older adults to live a functional life. To support this functional ability, factors such as meeting basic needs, learning and making decisions, being mobile, building and maintaining relationships, and contributing to society play vital roles (WHO, 2020). Underpinning this functional state is one’s immune resilience which allows the body to prevent diseases, and if sick, can recover and adjust quickly (Ahuja et al., 2023). To boost one’s immune resilience, several actions are highly influential such as regular exercise, making healthy food choices, getting enough sleep, and effective overall health management (National Institute on Aging, 2022).
Complementing health management are technological enablers such as telemedicine. Telemedicine, a component of telehealth or virtual health, refers to the delivery of healthcare services at a distance using technology (Watson, 2020). It encompasses a range of services from conducting medical visits over the computer or mobile devices to promoting patient monitoring. However, studies indicate that a significant number of older adults feel unprepared or hesitant to adopt telemedicine as a mode of health delivery, such as the study by Lam et al. (2020) where an estimated 38% of older adults surveyed are ill-prepared for video appointments. Factors contributing to this telemedicine unreadiness include challenges with technology, physical limitations, and economic circumstances (Kuang et al., 2022; Lam et al., 2020). The same is observed in the Philippine setting where the adoption of telemedicine in general is challenged by concerns about higher perceived costs, diagnostic limitations, and technical issues (Noceda et al., 2023). Moreover, concerns about privacy and mistrust of technology further contribute to the hesitancy in adopting telemedicine (Lam et al., 2020).
The need for trust to be established first before using various technologies was studied, and trust was found to be highly influential and a crucial element for older adults (Braun, 2013; Coughlin et al., 2007; Stuck & Rogers, 2018). In a prior study by Czaja and Sharit (2009), trust is a crucial factor that should be considered by designers of technology-enabled applications for older adults. To overcome the challenges faced by older adults in adopting telemedicine, innovative strategies have been implemented such as proactively engaging older adults via telehealth assessing their technological capabilities and preferences, involvement of caregivers in supporting and guiding older adults through technology, and providing telemedicine literacy through technological support, practice visits, and coaching (Lam et al., 2020). Aside from strategies that involve engagement, caregiver support, technological capability assessment and development, providing high-tech and reliable telemedicine services can also provide a positive experience and increase trust such as the experience on the introduction of RxBox telemedicine device in the country (Marcelo et al., 2021).
Despite all the challenges, the potential benefits of telemedicine for older adults are undeniable. It can enhance healthcare experiences by connecting older adults with doctors who can diagnose and treat various medical conditions without requiring physical presence (Watson, 2020). Moreover, telemedicine offers convenience, timeliness of medical intervention, cost savings, and the ability to provide care to individuals with mobility limitations or those residing in rural areas with limited access to healthcare facilities (Doraiswamy et al., 2021; Goldberg et al., 2022; Haimi & Gesser-Edelsburg, 2022; Watson, 2020).
This study contributes to the gerontology literature in two areas that necessitate scholarly investigation. First, studies on the use of telemedicine gained significant attention in recent years due to its potential to improve access to healthcare and enhance health outcomes for older adults. Most of these studies are concentrated on high-income countries because of their advanced adoption of the technology while studies conducted in low- to middle-income countries remain a gap (Doraiswamy et al., 2021). Second, trust in general is among the least explored factors in literature despite its considerable significance (Tsertsidis et al., 2019). In assessing the receptiveness of older adults to technology, it is important to cover different dimensions of trust including initial trust which is important in technology adoption literature. Thus, this study aims to address these gaps by investigating the behavioral intention of older adults to use telemedicine in a developing country like the Philippines considering that initial trust is critical to telemedicine adoption which is not yet widely practiced in the country (Macariola et al., 2021; Ong et al., 2022).
Theoretical Foundations
The theory of planned behavior (TPB) is commonly used in studying behavioral intention in the field of health information technology (J. Chen et al., 2023; Kim et al., 2022; Li et al., 2020; Zhang et al., 2019). It is also applied in studies specifically on telemedicine (Chau & Hu, 2002; Glock et al., 2021; Ly et al., 2019). Compared with the Technology Acceptance Model (TAM), which is widely used in investigating the acceptance of telemedicine (Garavand et al., 2022) focusing on the technology’s usefulness and ease of use, TPB considers broader social influences and perceived control which is more appropriate for analyzing the behavioral intentions of older adults. In studying telemedicine adoption, TPB provides significant explanatory power than TAM (Ramirez-Correa et al., 2020). Another model that is relevant to the technology acceptance of older adults is the Senior Technology Acceptance Model (STAM) by K. Chen and Chan (2014). However, STAM assesses the acceptance of technology based on actual usage (K. Chen & Chan, 2014; K. Chen & Lou, 2020). Given that initial trust is critical to the behavioral intention of technology adoption, STAM may not be appropriate as trust and not initial trust may have been established due to the actual usage of the technology. Thus, this study adopted the TPB as the theoretical model which is consistent with the study’s objective.
The fundamental constructs of TPB are attitude, subjective norm, perceived behavioral control, intention, and behavior (Ajzen, 1991). Recent studies referred to the intention construct as behavioral intention and behavior as actual behavior (Chau & Hu, 2002; Li et al., 2020;). Studies that intend to investigate behavioral intention no longer include the actual behavior construct. In TPB, behavioral intention is determined by subjective norms, perceived behavioral control, and attitude (Li et al., 2020; Zhang et al., 2019).
Subjective norm is the influence to behavioral intention from the external environment (Zhang et al., 2019). This is the way individuals perceive the beliefs of other people around them regarding their behavior (Ramírez-Correa et al., 2020). If the people surrounding the individual see the behavior as beneficial, the individual is more likely to perform the behavior. Studies on the behavioral intention of using telemedicine have mixed results. For example, the study of Ramírez-Correa et al. (2020) showed that subjective norm is a significant predictor of behavioral intention of using telemedicine while the study of Hsieh et al. (2022) showed that subjective norm does not influence the continuance intention in using telehealth systems. Given the contrasting results in similar studies, the subjective norm is investigated in this study.
Perceived behavioral control is the perception of the individual on the factors that promote or prevent the execution of behavior (Zhang et al., 2019). This includes the perceived ability of the individual to perform the behavior based on their capabilities (Ramírez-Correa et al., 2020). If the individual believes that they can do it, there is a higher likelihood for that individual to perform the behavior. Thus, perceived behavioral control is included in the investigation of this study.
Attitude represents how a person evaluates a behavior by weighing its potential cost and benefits (Ajzen, 1991). In technology adoption such as telemedicine, if the individual sees the benefits of doing the behavior, there is a higher likelihood for that individual to use a specific technology artifact (Ramírez-Correa et al., 2020).
Although several studies have used the TPB as it is (Glock et al., 2021; Kim et al., 2022; Ly et al., 2019), there were studies that have extended TPB to include other models or constructs (Chau & Hu, 2002; J. Chen et al., 2023; Li et al., 2020; Ramírez-Correa et al., 2020; Zhang et al., 2019). This study extends TPB to include Initial Trust as an additional construct.
Recent literature shows that trust is an important factor in the behavioral intention of older adults in technology acceptance (Harris & Rogers, 2023; Liu et al., 2023). Older adults trust technology because of their personal experience, once they know that issues would not arise, or they trust the person who told them to use the technology (Harris & Rogers, 2023). In assessing the behavioral intention, since much of the technology is unknown, initial trust plays an important role (Octavius & Antonio, 2021). Initial trust refers to trust in unfamiliar technology products and related services (Weck & Afanassieva, 2023). The study conducted by Octavius and Antonio (2021) showed that initial trust in technology explains the intention to adopt.
As we delve deeper into the behavioral intention to use telemedicine among Filipino older adults, the integration of trust-related constructs becomes crucial. Extending the theoretical framework can provide a more comprehensive understanding of the antecedents that influence the initial adoption of telemedicine (I.-L. Wu & Chen, 2005). The intricate interplay between initial trust, subjective norm, perceived behavioral control, and attitude, rooted within the context of healthcare, becomes particularly pertinent for older adults as they navigate the adoption of new technology (Dhagarra et al., 2020). Thus, this study posits this hypothesis:
Moreover, studies that investigated the impact of trust on technology acceptance showed a strong relationship between trust and attitude (Shrestha et al., 2021; Uche et al., 2021; K. Wu et al., 2011). In this study, whether the initial trust would also impact attitude is investigated.
Given those theoretical foundations, the theoretical model of the study for the five hypotheses is presented in Figure 1.
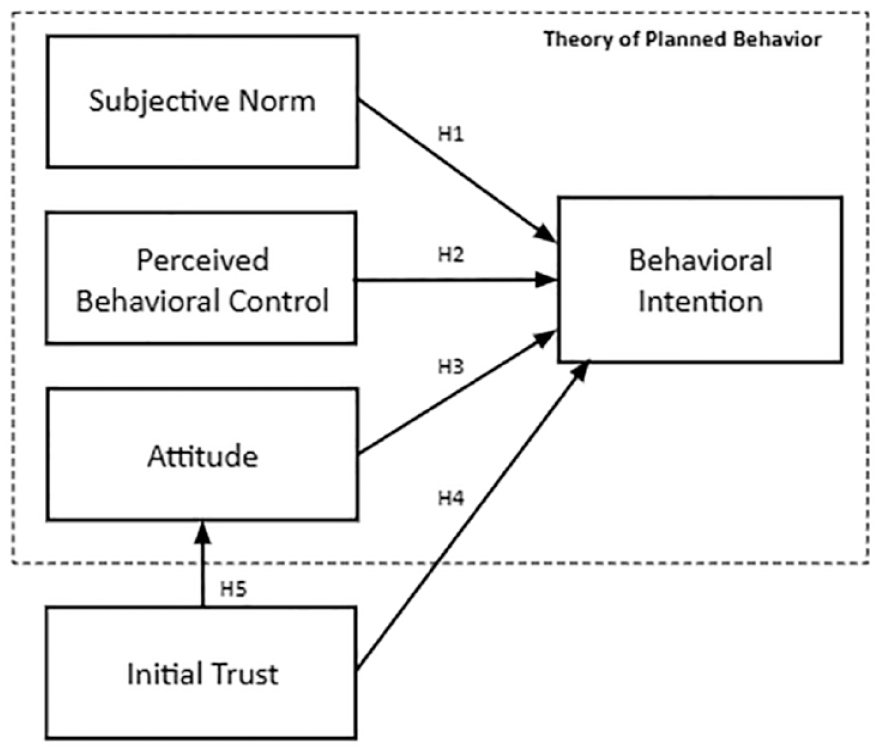
Theoretical model of the study.
Methods
A cross-sectional method was conducted using a questionnaire to investigate the behavioral intention of older adults residing in Quezon City in the Philippines. This specific locale was identified as it was a pioneer of telemedicine during the COVID-19 pandemic (Hallare, 2020). Before the administration of the questionnaire to the participants, an instrument validation was performed on 35 older adult respondents referred by the Office of Senior Citizen’s Affairs or OSCA. The succeeding subsections discuss the questionnaire and the result of instrument validation.
The Questionnaire
The questionnaire was written in the English language and includes these four sections: the introduction, to state the overview and objective of the study; the data privacy statement and consent, to explain how the study ensures data privacy and gets the informed consent of the participants; the general questions, to provide the demographics and the telemedicine usage of the participants; and the items pertaining to the constructs of the theoretical model of the study, to measure factors influencing the behavioral intention of the participants in using telemedicine. Although the primary language spoken by the older adults is Tagalog, the questionnaire was administered in the English language considering that Filipinos are generally proficient in reading and understanding the English language, as it is being taught as early as in primary school.
The general questions include personal data of the participants: name, location, sex, educational level, age, employment status, and marital status. As for the telemedicine usage of the participants, questions on the number of times they used telemedicine and the specific applications that they used were asked.
There were 16 items for measuring the behavioral intention of the participants based on the constructs of the theoretical model used in this study. The items for each of the TPB constructs were adopted from the study of Ramírez-Correa et al. (2020) which investigated telemedicine acceptance during the pandemic. For the Initial Trust construct, the items used by Octavius and Antonio (2021) were adopted. All the items (see Table 1) are on a 5-point Likert scale where 1 is the lowest and 5 is the highest value which represents the agreement of the participants to what is stated in each item.
Theoretical Model Constructs’ Items.

Questionnaire Validation
To ensure reliable analysis and interpretations of the relationships between the constructs in the theoretical model of the study, the outer loadings of the items and the internal reliability and validity of the constructs were assessed using the PLS-SEM algorithm (J. F. Hair et al., 2019) based on the responses of 35 participants.
By computing the outer loadings, the strength of how well the variables capture the constructs in the model is determined. The lowest outer loading is 0.778 on SN2 and the highest outer loading is 0.983 on PCB2. This shows that all the items in the model are good indicators of the constructs based on the ideal value of at least 0.708 (J. F. Hair et al., 2019; Risher et al., 2018).
To evaluate the reliability and validity of the constructs, Cronbach’s alpha, composite reliability (CR), and average variance extracted (AVE) were determined and checked against the acceptable values of greater than .70 for both the Cronbach’s alpha and CR and greater than .50 for AVE (Al-Emran et al., 2019; Bayaga & Kyobe, 2021; J. F. Hair et al., 2019; Risher et al., 2018; Sarstedt et al., 2021). The results of the test (see Table 2) showed that the Cronbach’s alpha and CR of the constructs are acceptable with the minimum value of .807 and .859 respectively, indicating that the items are measuring the same construct consistently (Al-Emran et al., 2019; Bayaga & Kyobe, 2021). As for the AVE values, it was also within the acceptable range with the minimum value of 0.713 establishing the convergent validity (Bayaga & Kyobe, 2021). From these results, the questionnaire was validated and administered to accept more responses.
Construct Reliability and Validity Test Results.

The validated questionnaire was then distributed in person using convenience sampling to collect responses that were used to investigate the intention to use telemedicine of older adults in the area of study from May to June of 2023. During the data collection phase, respondents who have used telemedicine at least once, at least 60 years old, and a resident of Quezon City were selected and requested to participate in the conduct of the study. The questionnaire was administered by a surveyor and supervised by one of the authors, JDT, who has extensive experience in quantitative investigations. JDT was present throughout the survey duration to clarify any questions when the participant needed assistance in the interpretation of the questions.
A total of 180 responses were collected and analyzed using PLS-SEM. The analysis included checking the discriminant validity of the model using the Fornell-Larcker Criterion and structural model testing using the bootstrapping procedure. The results of these analyses are presented in the next section.
Results
Participant Demographics
The participants’ demographic profiles revealed that the majority are female (69%) followed by male (29%), and the rest preferred not to say (2%). In terms of age, most of the participants are between 60 and 65 years old (44%), followed by 71% to 75 (22%), 66% to 70% (18%), and 76 and above (16%) age groups. To describe further the demographics of the respondents in terms of age, the mean and standard deviation were calculated. The mean age of the respondents is 68 years old and the standard deviation is 6 years which implies that 68% of the respondents are between 62 and 74 years old.
Moreover, more than half of the participants are married (57%), followed by widowed (34%), single (6%), and separated/divorced (3%). The educational level profile shows that most are in high school or below (45%), followed by college (36%), post-graduate (12%), and vocational (7%) levels. In terms of employment status, the majority are retired (39%), followed by housewife/househusband (33%), self-employed (15%), full-time employee (7%), and part-time employee (6%). The majority of the respondents (87%) have used telemedicine applications (e.g., Telekonsulta, Health Now PH, and Doctors Anywhere) only one or two times.
Discriminant Validity
The discriminant validity measures the distinctiveness of the constructs in the model (J. F. Hair et al., 2019). By extracting the Fornell-Larcker Criterion test scores, the result is presented in Table 3. The diagonal values in bold format are the square root of the AVEs and the other values are the correlations with the constructs. When the diagonal values are the highest value in their respective column, it means that the construct has good discriminant validity. As shown in Table 3, the diagonal values are the highest in all the constructs of the model indicating discriminant validity.
Fornell-Larcker Discriminant Validity Test.

Structural Model Testing
To describe how the respondents answered the questionnaire, on a Likert scale of 1 to 5, answers 1 to 2 represent disagreement, 3 stand on being neutral, and 4 to 5 represent agreement. From the 180 responses, Table 4 shows the percentages of disagreement, neutrality, and agreement for each of the constructs.
Agreement and Disagreement of the Respondents for Each Construct.

Among the five constructs, most of the participants have a positive attitude, behavioral intention, and initial trust toward telemedicine. On the other hand, in the perceived behavioral control, most of the respondents disagree which means that on their own, older adults don’t think they have the knowledge and ability to use telemedicine. As for the subjective norm, it is noteworthy that the disparity between agreement and disagreement is not significant indicating a polarity of the inclination and non-inclination in adopting telemedicine based on how the environment supports the use of telemedicine.
To test the structural model, a bootstrapping procedure was conducted using PLS-SEM. As presented in Table 5, the coefficient values for H1, H2, H3, H4, and H5 are all positive values indicating the positive relationship between the constructs. However, looking at the t-statistics values where H2 (0.907) does not have a value above 1.96 indicates that the relationship between PBC and BI is not significant as compared to H1 (2.596), H3 (7.229), H4 (4.498), and H5 (32.262) which shows that the relationship between the constructs is significant. Moreover, the p-values of H1 (0.009), H3 (0.000), H4 (0.000), and H5 (0.000) which are less than .05 indicate that the path coefficient is statistically significant at a 95% level confidence level. On the other hand, the p-value of H2 (3.64) indicates that there is not enough evidence to conclude that there is a causal relationship between PBC and BI.
Hypothesis Testing Results. .

The result of the structural model test reveals that subjective norm (H1), attitude (H3), and initial trust (H4) positively affect the behavioral intention of older adults in using telemedicine. Perceived behavioral control (H2) on the other hand does not significantly affect the behavioral intention. Moreover, initial trust positively affects the attitude of older adults toward the use of telemedicine (H5).
Discussion
In a sample of 180 Filipino older adults, subjective norm, attitude, and initial trust influenced the behavioral intention of using telemedicine, while perceived behavioral control did not. Literature has mixed results in terms of how subjective norm and perceived behavioral control influence the usage of telemedicine. Consistent with the result of this study, Ramírez-Correa et al. (2020) and Hsieh et al. (2022) found that subjective norm is a predictor of behavioral intention while in the study of Cobelli et al. (2021), it is not. Even though older Filipino adults have a strong sense of independence in making decisions (Ramos & Mahmoud, 2020), this study shows that the opinion of others about the use of telemedicine influences their behavioral intention. This result may also be affected by the educational level of the participants of the study where 45% are at most high school level which would prompt them to consider the opinion of others. In terms of the perceived ability of older adults to use telemedicine, it does not significantly affect their intention to use the technology. This can be attributed to the fact that Filipino older adults traditionally rely on the support provided by their immediate family members (Badana & Andel, 2018; Montayre et al., 2017; Ramos & Mahmoud, 2020).
Consistent with other studies that investigated the behavioral intention of using telemedicine (Cobelli et al., 2021; Ramírez-Correa et al., 2020; Zhang et al., 2019), attitude positively influences the behavioral intention of older adults. Despite being not familiar with the technology and the limited experience in the use of telemedicine, the attitude of older adults toward it may be affected by the recent pandemic where they have seen the relevance and importance of telemedicine. The COVID-19 pandemic increased the awareness of the value of telemedicine for both consumers and healthcare providers (Leochico et al., 2022). Based on the study of Cruz-Lim et al. (2021), from 59% usage of telemedicine before the pandemic, it has increased to 96% of physicians mostly for follow-up virtual consultations.
From the examination of attitude, which encompass a person’s favorable or unfavorable evaluation of behavior, we shift our focus to the construct of initial trust, which delves deeper into the interpersonal dynamics that underlie the decision-making process within this demographic (Ajzen, 1991; Glock et al., 2021). The results of this study shed light on the pivotal role of initial trust in influencing the behavioral intention of Filipino older adults to utilize telemedicine services. This finding aligns with prior research in the field of eHealth, which has highlighted the significance of trust as a central factor in technology adoption, particularly in sensitive healthcare contexts (Zanaboni & Wootton, 2012). The initial trust established between users and the telemedicine platform is a crucial precursor to fostering positive attitudes and intentions toward its use. This phenomenon is underscored by the fact that healthcare services, especially those facilitated remotely, necessitate a strong foundation of trust due to the sensitive nature of medical information and care delivery (Zanaboni & Wootton, 2012).
The interplay between initial trust and behavioral intention among Filipino older adults holds strategic implications for the successful implementation of telemedicine initiatives. Establishing a sense of security, reliability, and confidentiality at the outset of engagement is pivotal in promoting continued utilization and enhancing the older adults’ experience with the use of telemedicine. Our findings not only contribute to the extant literature on technology acceptance within the healthcare domain but also provide valuable insights for healthcare providers, policymakers, and stakeholders seeking to promote telemedicine adoption among this demographic group.
As the digital transformation of healthcare continues to evolve, recognizing and addressing the nuanced role of initial trust becomes paramount. By nurturing an environment of trust and addressing potential concerns, healthcare systems can pave the way for more widespread and meaningful integration of telemedicine services, ultimately improving access to quality healthcare for Filipino older adults.
Conclusion
This study underscores the significance of subjective norm, attitude, and initial trust as influential factors in shaping the behavioral intention of older adults to adopt telemedicine services among the Filipino population. The positive influences of subjective norm and attitude align with the original study of the Theory of Planned Behavior (TPB), highlighting the role of social influence and personal evaluations in driving behavioral intentions (Ajzen, 1991). More importantly, this study has emphasized that initial trust is an important factor in the positive attitude of older adults toward using telemedicine and behavioral intention. When there is a lack of trust in technology, older adults see telemedicine to have limited benefits (Karlin & Weil, 2022), thus, the importance of building initial trust among older adults to promote the usage of the technology. Furthermore, the presence of initial trust as a positive influencer emphasizes the importance of interpersonal perceptions, especially in establishing a foundation of confidence, reliability, and confidentiality in the context of telemedicine adoption.
However, the non-significant impact of perceived behavioral control points to the nuanced nature of perceived ease or difficulty in utilizing telemedicine services among older adults. This outcome suggests that the older adults’ perceived control does not strongly contribute to their behavioral intentions in this context. This insight correlates with the Filipino culture of the presence of help and assistance among family members, especially in the older adults’ regular tasks of attending to their health-related activities.
As telemedicine continues to gain prominence and acceptance as a viable healthcare alternative, it is imperative to recognize the multifaceted nature of factors influencing adoption (Gregory et al., 2023). To facilitate broader acceptance and utilization, future interventions and initiatives should not only focus on addressing barriers but also emphasize the cultivation of initial trust, positive attitudes, and supportive social norms. By addressing these factors comprehensively, implementers can pave the way for the successful integration of telemedicine services among Filipino older adults, contributing to enhanced healthcare accessibility and overall well-being within this demographic.
While this study provides significant insights into the behavioral intention of older adults in using telemedicine, this study is not without limitations. First, this study relied on self-reported data from participants which may be a limitation. Second, this study applied the convenience sampling method to a relatively small sample size. Therefore, the authors recommend a replication of the study on a larger sample size that considers the impact of technological support in the homes of older adults and their Information and Communication Technology (ICT) literacy in different age groups to explain further the perceived behavioral control factor in the usage of telemedicine. The 68% of the respondents (ages between 62 and 74) are considered baby boomers who were already exposed to advancements in technology when they were in working age. This group has a somewhat higher level of propensity to adapt to technologies like telemedicine compared to their older counterparts. However, it was not determined in this study whether this factor affected the perceived behavioral control which could be an opportunity for future research. Moreover, a subset within the study cohort comprising older adults aged 76 years and older potentially stands as the segment that could derive the greatest advantages from the adoption of telemedicine due to challenges regarding transportation and mobility. However, accounting for only 16% of the respondents, there is still a research opportunity to delve deeper into this specific generation. Third, we did not account for the effect of control variables such as age and frequency used to initial trust. These sociodemographic characteristics may provide interesting insights as to how initial trust influences perceptions of older adults to telemedicine use (Ajzen, 2020). Lastly, based on how the respondents answered the questionnaire, the respondents have a positive inclination toward most of the constructs of the study which may also reflect their perceptions of the healthcare system. Thus, further analysis of the relationship between the amount of trust in the healthcare system and the formation of initial trust would provide more insights that will guide the implementation of telemedicine in consideration of the context and capacity of older adults.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
