Abstract
Safe medication administration is a critical responsibility of registered nurses and is an essential skill developed during nursing education. Student confidence and preparation regarding medication administration are essential aspects of professional skill building. The Confidence and Preparation Survey (CPS) was used previously among homogeneous nursing student samples. The existing dominant discourse, shaped by ideologies and systems, can unfortunately lead to limited perspectives; therefore, the purpose of this study was to evaluate and refine the CPS for feasibility, clarity, and validity among nursing students primarily from groups that have been historically marginalized. A secondary purpose considered the conditions that affect perceived confidence and preparedness. Cognitive interviews were undertaken with baccalaureate nursing students (n = 11) attending an urban college of nursing in the Northeastern region of the United States. Data were analyzed using rapid qualitative techniques and the framework matrix method. The CPS was readily understood and interpreted by this sample. Student perspectives of conditions that influence their understanding and interpretation of the CPS are described under three themes: (1) prior outside of school healthcare experiences influence understanding, (2) school experiences support survey comprehension, and (3) concerns over insufficient training within school. Findings also include a revised CPS instrument ready for further testing.
Introduction and Background
Quality and safety are essential domains of professional nursing practice (American Association of Colleges of Nursing, 2021). Within healthcare, medical errors remain a significant problem (Bates et al., 2023; Makary & Daniel, 2016). Medication errors are among the most common medical errors (Institute of Medicine, 2007; Schroers, 2018) and frequently involve issues in medication administration (Bates et al., 1995; Suclupe et al., 2020). Medication administration is a critical responsibility of registered nurses and remains an essential skill developed during professional nursing education. Documenting medication administration involves a written medication administration record (MAR) or an electronic version, although use and purpose may depend on setting and country of use (Karnehed et al., 2024). Nursing students are taught the rights of medication administration, including the traditional and globally accepted five rights of right patient, medication, time, dose, and route; other “rights” have been suggested, highlighting educational challenges with the rights framework (Hanson & Haddad, 2023). A medication error occurs when there is a failure regarding one of the rights (MacDowell et al., 2021). Confidence and preparation are essential aspects of nursing and professional skill building (Guerrero et al., 2022; Porter et al., 2013) within the nursing workforce. Confidence is defined as an individual’s belief in their ability to complete a task (Allobaney et al., 2022) and prepared nurses are able to improve outcomes for patients, organizations, and their profession (Chicca & Shellenbarger, 2024).
Over the past several decades, the nursing workforce in the United States has become increasingly diverse (Phillips & Malone, 2014; US Census Bureau, 2021). Latest statistics show that nursing students now come from an increasing diversity of ethnic and cultural backgrounds, including Black or African American, Hispanic or Latino, Asian, Native Hawaiian or Pacific Islander, and American Indian or Alaskan Native (American Association of Colleges of Nursing, 2022, 2023). The increasing diversity of nursing students has also become an important area of nursing research. Diverse nursing students, known for the purposes of this manuscript as, and intentionally using equity-focused alternative language, “groups that have been historically marginalized” (American Medical Association & Association of American Medical Colleges, 2021, p. 8; hereinafter, “GHM”) and further defined here as groups associated with loss of power, as at “stake is the connection of status to power differentials” (American Medical Association & Association of American Medical Colleges, 2021, p. 13). Nursing students from GHM are an important cohort of the nursing student population that have been historically marginalized and have experienced racism and discrimination.
The Future of Nursing 2020 to 2030 reported that workforce development is one key area for strengthening the nursing profession. One desired outcome is to have nurses reflect the populations and communities they serve (National Academies of Sciences, Engineering, and Medicine, 2021), requiring the advancement of nurses from GHM in all areas of the profession. However, racism and discrimination are pervasive in nursing (Cooper Brathwaite et al., 2022; Wheeler et al., 2014), both in the workplace and within nursing education (K. Iheduru-Anderson et al., 2021). In addition, literature notes the challenges and disadvantages to under-represented minority groups from standardized, or high stakes testing, particularly for nursing licensure (Muirhead et al., 2022). Accordingly, nurse educators need to assess skills among their students with special attention to students from GHM.
Within healthcare, nursing students from GHM arrive to both schools of nursing and healthcare institutions with the weight and impact of structural racism and unique life experiences. Prior research suggests that in a sample of senior-year, baccalaureate nursing students (n = 60), confidence in medication administration is high, despite an appreciation for future risks of errors (Roman Jones et al., 2022a, 2022b). Importantly, there is evidence that the development of confidence among students from GHM is influenced by structural racism, including discrimination and micro-aggressions: discrimination can affect students’ physical health and mental well-being (Lei et al., 2021) and microaggressions negatively affect academic self-confidence (Acevedo-Gil, 2022; Nadal et al., 2014). Nursing students from a minority group have significantly higher perceived stress than the nursing students from the dominant group (Ahmad & Mushtaq, 2014). Furthermore, marginalized nursing students’ help-seeking may be impacted by implicit bias and microaggressions (Attis-Josias, 2023). Confidence is critical for medication administration, as confidence is directly related to performance (Westman et al., 2024), and it is crucial to understand how confidence in medication administration develops among all nursing students, not solely the dominant group. An essential first step is a vetted measure of confidence and preparation in medication administration that is valid across varied populations.
The Confidence and Preparation Survey (CPS; Booth et al., 2018; Sung et al., 2008) is one such vetted measure, that had satisfactory internal consistency in the original study (Cronbach’s alpha of .929; Sung et al., 2008) and was also used to evaluate medication error differences among nursing students in clinical simulations in relation to nursing students’ perceived levels of confidence (Chan et al., 2019). The CPS was successfully used in prior research by the primary investigator investigating confidence and preparation among undergraduate students in a homogenous sample (Roman Jones et al., 2022a, 2022b). Originally, the CPS included six questions on confidence with a seven-point Likert scale from 1 (Not Confident at All) to 7 (Absolutely Confident) and eight questions on preparation with a seven-point Likert scale from 1 (Not Prepared at All) to 7 (Absolutely Prepared; Table 1).
Confidence and Preparation Survey [Original].

Validity in this study follows Streiner and Kottner’s (2014) instruction that all validity testing is assessing construct validity, as opposed to delineating particular validity types (Streiner & Kottner, 2014). Construct validity considers whether the tool indeed measures what it means to measure. Prior to wider testing, cognitive interviews are a well-studied method and process to support this validity assessment (Hill et al., 2022). The purpose of this work was to evaluate and refine the CPS for feasibility, clarity, and validity among nursing students primarily from GHM. Enhancing the effectiveness of education methods requires the wholistic examination of medication administration skills prior to licensure. This, in turn, further requires ensuring the rigor of an existing approach to confidence and preparation measurement. The current sample is purposefully different from prior samples. The methods used to generate instruments can include bias (Stantcheva, 2023). Obtaining a diverse sample to interview as an approach can help to address this type of bias that commonly gets infused into instrument development, especially when the topic being examined has historical involvement with established, hegemonic structures. Refining instruments is a strategy to enhance accuracy (Hulley et al., 2013). In sum, the existing dominant discourse, shaped by ideologies and systems, can unfortunately lead to limited perspectives in nursing education (Lapum et al., 2022). Therefore, the aims for this project were (1) to examine the CPS’ applicability to baccalaureate nursing students primarily from GHM and to propose and present revisions based on participants’ responses; and (2) to further consider the conditions that may affect perceived confidence and preparedness as described through the perspectives of the participants.
Positionality
The research team (JRJ, JM, AAL, RC, RB, LB, PKG) represents varied professional (nursing, public health, administrative), clinical (critical care, public health, gerontology, informatics), academic work setting (private, public), and personal (country of origin, locality, education) experiences. In sum, our approach was informed by the team’s shared educational, clinical, and research experiences.
Methods
Study Design
Cognitive interviews are a qualitative technique used to examine and improve survey questions in an iterative process, informing survey item revisions and providing evidence of survey validity (Beatty & Willis, 2007; Peterson et al., 2017; Willis et al., 2011). The CPS required testing among a population including GHM prior to further use and study among a larger sample, to minimize future non-response or response error (Drennan, 2003).
During a participant’s cognitive interview, after each survey question is read, the participants are asked to share their interpretation of the survey question and are further asked to share what information they used to answer that question. The four cognitive operations of (1) comprehension, (2) retrieval, (3) judgment, and (4) response/reaction were specifically targeted to appraise each survey item (Drennan, 2003; Willis & Artino, 2013). After each specific survey item was assessed, the constructs (confidence, preparation) as a whole were queried to provide a wider view assessment of each survey section and then, the survey as a whole was considered (Peterson et al., 2017). After the first testing round, the survey questions were revised prior to the second round of testing, where the entire process was repeated. Additional analysis was conducted using data from both cognitive interview rounds to explore participants’ understanding and interpretation of survey questions, and their perspectives on conditions that may affect perceived confidence and preparedness. Figure 1 below depicts the methods process used by the study team.
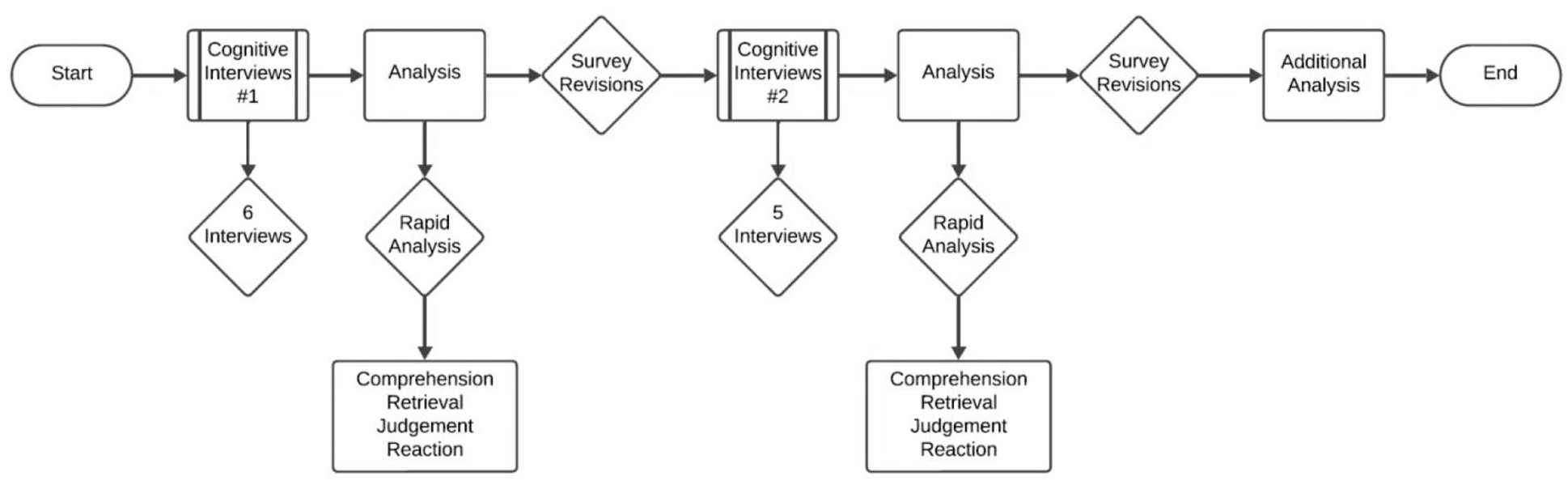
Study methodology.
Setting and Sample
We used a purposive sampling technique to recruit participants meeting pre-determined criteria at an urban nursing school in the Northeastern region of the United States. Inclusion criteria included individuals over 18 years of age, current nursing students at the study site, and specifically seeking students from GHM. All participants who expressed an interest were included in the sample, including one white, female participant, in order to allow for all possible viewpoints of students from GHM. There were no ESL considerations as this nursing program required an English-language proficiency for admission. We posted recruitment information on printed flyers in the undergraduate nursing student simulation lab, where all students frequently attend, and sent emails after the completion of the semester to undergraduate nursing students inviting them to participate in one interview that would last between 45 and 60 min. All interested participants received study information and a copy of the informed consent prior to participating in a scheduled internet-based (Zoom) interview.
At the study location, by graduation, students complete approximately 600 clinical hours, 123 credits (in the United States, credits are a unit of measurement indicating course hours required by the program), and five clinical semesters. For this study, all eleven participants were rising seniors, meaning they had completed three clinical semesters (in settings including long-term care, adult health, maternity and women’s health, and mental health) and three semesters of nursing coursework (including 40 credits hours of Nursing Core coursework), including clinical and simulation lab hours each semester. Each student had the opportunity to practice on MARs in their lab before entering the clinical setting. Sample sizes were consistent with cognitive interview literature (n = 5–15; Peterson et al., 2017).
Ethical Considerations
All activities were approved by the University of Massachusetts Institutional Review Board (#3420). Each participant reviewed the informed consent including study details prior to participation in the study. Verbal consents were obtained prior to each interview and audio-recorded. Participant responses were recorded and transcribed with a transcription service and all files were de-identified and secured.
Data Collection
The first round of interviews (round 1) began on May 30, 2023, and concluded June 5, 2023. The second round of interviews (round 2) began on November 17, 2023, and concluded December 7, 2023. The primary investigator obtained participant consent and collected demographic data (e.g., gender, race, age). All interviews were conducted via Zoom by an experienced interviewer (JRJ) and one note taker (JM), and ranged from 22 to 57 min. All interviews were conducted with no video component (recording audio only) and followed an interview guide. Interview recordings were de-identified, transcribed by a professional transcription service, and then checked for accuracy. Participants received a gift card for an online marketplace as a token of thanks for their participation after completing their interview.
Prior to each cognitive interview, the primary investigator read instructions for the CPS and then administered the CPS. Interview questions targeted the student’s (1) comprehension, (2) retrieval, (3) judgment, and (4) reaction to information (Lewinski et al., 2021) to uncover opinions and views on the CPS. Comprehension focused on the student’s interpretation of the survey question; retrieval focused on the student’s response to the survey question; judgment focused on the ease of the survey question; and reaction focused on any emotional reaction in response to the survey question. The team reviewed the participants’ self-identified race and ethnicity characteristics, gender, and age at the close of the first round of interviews, in order to consider the diversity of participants and their thoughts on the CPS. In addition, as several participants in the first round independently brought up work experiences (i.e., nursing experiences other than school and clinical), the team decided to ask round 2 participants directly about potentially influential work experiences. Audio files, responses, and interview notes were saved in a secure database.
Data Analysis
Data were analyzed using rapid qualitative analysis techniques (Beck et al., 2018; Hamilton & Finley, 2019; Vindrola-Padros & Johnson, 2020) and the framework matrix method (Abraham et al., 2021; Averill, 2002) to uncover both similar and contrasting participant depictions. Rapid analysis is a team-based approach to analysis that can improve efficiency and accuracy. After each interview round, the data were entered into Microsoft Excel to facilitate analysis by each survey item. The participant responses were captured and subsequently serially summarized in a structured framework matrix based on the interview guide and categorized by survey question and participant. Two authors (JRJ, JM) read each entry and wrote summaries for each item and then compared results. The remaining authors reviewed the analysis and framework matrix for each round; any analysis discrepancies were resolved through discussion and team consensus. Each summary included four distinct aspects underlying the structure of the interviews: comprehension, retrieval, judgment, and reaction. The final framework matrix highlighted the participants’ survey insights and captured the researchers’ interpretation of the participants’ responses to the survey questions. The analysis was iterative (Fereday & Muir-Cochrane, 2006; Harper & Thompson, 2011) and included research team members during multiple occasions, which contributed to study dependability (Thomas & Magilvy, 2011). Analyst triangulation combined multiple perspectives to further strengthen credibility (Barusch et al., 2011) and encouraged team reflexivity (Rankl et al., 2021; Twist et al., 2024) during analysis.
Following the data analysis after each round of interviews, the team created a revised CPS, having planned a priori for revisions pursuant to participant responses, and edited as agreed upon by the team. A final revised CPS was created by the team after the conclusion of round 2 and incorporating both rounds of analysis and edits to the CPS. To promote reliability and validity, all independently created summaries, resulting findings, and revised CPS drafts were shared and discussed to consensus with the larger research team. Additional thematic analysis detailed evidence of participant understanding and interpretation and followed the same techniques. The qualitative aspects of the cognitive interviews were specifically used to generate new knowledge about nursing students’ perspectives and experiences, along with tool refinement.
Results
A total of 11 students participated in the interviews, the majority were female (n = 9, 82%) and non-white (n = 10, 91%). The sample ranged in age from 20 to 32, with a mean age of 23.09 years. All participants were about to enter their final year in the baccalaureate nursing program. Four (36%) students were first generation American, two (18%) students were first in their family to attend college, and five (45%) students were born outside of the United States. In the following sections, we present findings from the cognitive interviews, revisions to the CPS based on these findings, and themes that reflect student perspectives of conditions that influence their understanding and interpretation of the CPS.
Cognitive Interview Findings
Student nurse participants shared that the CPS concepts addressed relevant and meaningful issues related to their personal experiences with confidence and preparation associated with medication administration and experiences with the MAR while in their baccalaureate nursing program. Participants detailed how medication administration and aspects of nursing care related to the MAR were closely connected with nursing school activities, outside work experiences, and clinical challenges. The findings below describe participant responses from both rounds of the cognitive interviews specifically regarding comprehension, retrieval, judgment, and reaction.
Comprehension
Participants indicated that most CPS items were clear and “very straightforward” (C1, P4) and captured their experiences with medication administration and using the MAR while in their baccalaureate program. Items that were not clear to the participants were discussed by the study team and edited within the CPS versions. Overall, the participants understood and interpreted the content discussed in each CPS item as intended. Specific participant recommendations for clarification did occur for multiple items, including requests to modify and clarify CPS prompts and item terms including “understand,” “time-efficient,” and “element.” Participants suggested that the team consider adding information about the rights of medication. For example, one student stated, “for even more clarification, you could probably add the rights of medication or in little parentheses ‘make sure you have all your rights’ or something like that” (C1, P3). Another suggested adding questions that focus on medication dosage calculation to the CPS: “Maybe like math situations. Like you might have to do dosage calculations and things like that. I think it’s important too, to question” (C1, P5).
Retrieval
Participants readily, and with significant detail, recalled information about medication administration and MAR use for each CPS item, based on personal, educational (including simulation), clinical, and/or work experiences. One student participant shared that she was able to answer the questions “mostly through review of my education from fundamentals up till nursing capstone right now” (C2, P2) and another student was able to retrieve information because she was “thinking about the times I’ve been in clinical and going through med orders with my nurse” (C2, P5). Differences in responses, and recommendations for clarification, occurred for multiple items, including, for example, student participants asking for clarification about particular or necessary steps required to follow a MAR, with one student commenting: “There’s an actual algorithm or step you have to follow when looking through the MAR, [but] we were never really taught that.” (C1, P5). Participants shared that depending on an individual student’s experiences both outside of nursing school (either in personal experiences, with family members and medication, or healthcare work experience) and within clinical placements, unique encounters may result in a difference in understanding and different responses to the survey questions. One student explained, “I think depending on what experiences we’ve had as individuals, I feel like that could skew the results” (C1, P4).
Judgment
Although a majority of the participants found that responding to the CPS items was easy, we noted difficulties with multiple items. Several participants wanted a reference to a particular software when asked to consider MARs. One student shared: “I wouldn’t quite say easy just because I would like to know what software they’re referring to” (C1, P3). Several participants asked for more specificity regarding assessments prior to medication administration (i.e., a physical assessment or asking for the rights of medication). Several participants found questions confusing when they had multiple question stems within one question, for example one student noted: “I feel like maybe break that up into a couple different ones” . . . It’s two parts, it’s identifying and documenting” (C1, P3). Confusion also surrounded whether they were supposed to think about their current experience as a student or forecast into the future. One student explained, “It’s a bit confusing because I’m still a nursing student but this is asking more like [the] future” (C1, P1).
Reaction
Participants willingly discussed medication administration and their experiences with MARs and reported no extreme negative reactions while completing the CPS. The term “correct steps” was jarring to one participant: “I think just defining what they mean by correct steps. So like, . . .are we talking about the patient specifically or the process on the computer or everything or what specific steps are they talking about?” (C1, P3). The terms “integrating,” “contraindications,” “element,”, and “efficient” created confusion and caused a reaction in some participants.
Application of Cognitive Interview Findings and a Revised CPS
Following the analysis from the cognitive interviews and both revisions of the CPS, the research team reviewed all CPS questions to address issues participants raised throughout both rounds of the cognitive interviews. After discussion, the research team reached consensus on the final revised CPS (Table 2). Although the team considered the impact of potential increased respondent burden, because of the original CPS brevity, additional CPS questions, along with revised questions, clarified and shortened Likert scale responses, and grammatical changes were made to the CPS in its final, revised form. Table 2 details the revised CPS, also included in full format in the Appendix. The answers are in a Likert scale of 1 to 5, of confidence (1. Not Confident at All; 2. Somewhat Unconfident; 3. Neither Unconfident nor Confident; 4. Somewhat Confident; 5. Confident) and of preparation (1. Not Prepared at All; 2. Somewhat Unprepared; 3. Neither Unprepared nor Prepared; 4. Somewhat Prepared; 5. Prepared). Wholly new survey items include Confidence questions 2 and 8, along with Preparation questions 2, 8, and 10. All other questions were edited to their revised versions below.
Revised Confidence and Preparation Survey.

Themes of Understanding and Interpretation
The findings from the additional analysis evidenced the participants’ clear understanding and interpretation of the final revised CPS, supporting the validity of the study’s tool refinement among this sample of nursing students and also addressing the secondary purpose of participant perspectives of conditions that may affect perceived confidence and preparedness. The three resulting themes from the data include: (1) prior outside of school healthcare experiences influence understanding, (2) school experiences support survey comprehension, and (3) concerns over insufficient training within school.
Prior Outside of School Healthcare Experiences Influence Understanding
Individual, outside healthcare experiences influenced the participants’ understanding and comprehension of the CPS, and also supported their answers to the survey questions. As one student stated: “as a home health aide, without being in the hospital, you get used to giving meds” (C2, P1). Participants shared that their outside work experiences informed their comprehension of the CPS questions and impacted their responses; “I would say my own personal, like outside of school, my work experience definitely helped me answer more of the confidence questions.” (C2, P3). Watching professional nurses at their workplace offered perspective on the responsibilities of nurses and their challenges and frustrations. Resources for drug information and identification were available at the participants’ workplaces, offering additional review opportunities, with a student explaining that: “the hospital that I work at has resources so we can look those up” (C2, P4). Multiple participants agreed that their experiences were represented in the CPS, because of their roles and job responsibilities as a personal care assistant, home health aide, or emergency medical technician, further noting that: “you get used to the work environment, and it’s not as hard as navigating if it’s your first time [in the healthcare setting].” (C2, P5). Even personal experiences with family members supported participants’ understanding of confidence and preparation, as one student shared: “I’m in charge of . . . setting up the medication boxes for my grandmother” (C2, P1).
School Experiences Support Survey Comprehension
Participant item comprehension and answers to the CPS were based on personal and individual school experiences, including coursework, lab experiences, and clinical assignment rotations. One student explained: “I have so many examples from med surg because I had a really good clinical instructor and we learned a lot” (C1, P4). Clinical instructors were instrumental, offering critiques on assessment and charting and offering critical instruction and guidance to students: “the instructor was with me one-on-one, step by step to help me administer the medication to my patient” (C1, P1). One particularly helpful strategy in clinical was to begin with one patient and then slowly receive more patient assignments, thereby improving in multitasking throughout the clinical experience. Other school experiences supportive to the participants included pharmacology class, simulation lab, and medication dosage calculation tests. Memorable clinical experiences (including working with the MAR/technology, patient experiences (including patients refusing medication), and preceptorships) helped students work through challenging lessons: “the more you have clinical experience or . . . hands-on knowledge about medication administration in comparison to just hearing it in class, it makes a big difference” (C2, P2). Some clinical sites offered resources to support the participants in their assignments, such as searching for medication interactions or confirming necessary patient assessments. Clinical assignments allowed for experiences with different types of medications and routes: “Because the school does a lot to give us experience in clinical to give medication. And the instructors are really thorough on making sure we know what we’re giving, we know how to give it, if so, it’s at the right time, right dose, so on and so forth. So we get a good amount of practice.” (C2, P1).
Concerns Over Insufficient Training Within School
Several participants shared their concerns that they received insufficient training, practice time, and hands-on experiences with medication administration within their school program. One student explained that “every time I’m on a clinical site, the instructor [is] always busy with 10 other students” (C1, P1). Others felt they did not learn about the MAR in school and were never taught any steps for how to advance through a MAR. Participants described a wish for more experiences with the MAR and with medication administration: “I did hear from some other people in my cohort that didn’t really give out meds too much. So I feel like I got practice but not enough.” (C1, P2). Participants wanted more support from, and time with, their instructors: “I wish that my clinical instructor would spend more time with me to see that I actually do the right step.” (C1, P1). Specific examples of clinical areas or experiences where participants identified lacking preparedness included being ready to assess for a drug reaction after medication administration, with one student sharing: “I’ve not really witnessed a drug reaction with a patient” (C2, P2). Another student shared insufficient experiences with blood transfusions and cardiac medications, noting: “I’m thinking about blood transfusions, when you give blood. I’m still learning about the different reactions or even side effects of heart medications, I’m still learning about that” (C2, P3). In response to these concerns, student participants suggested additional learning opportunities, such as students using the MAR on their own or being watched through a two-way mirror.
Discussion
The study focused on a close examination of confidence and preparation in administering medications within a nursing student population primarily from GHM. The purpose of this study was to evaluate and refine the CPS for feasibility, clarity, and validity among nursing students primarily from GHM. The revised CPS was presented and participant feedback indicates that this revised CPS can be used to assess medication administration confidence and preparation in a broad sample of nursing students.
Medication Administration Confidence and Preparation
Tool refinement for use with nursing students has multiple educational and clinical implications. The resulting revised CPS can contribute to future work regarding medication administration safety and workforce preparation. Evidence suggests that nursing students, including in international settings, require additional support in administering medications safely (Musharyanti et al., 2021). Confidence scales are available to measure levels of confidence in different populations, including to measure nursing student confidence in meeting challenges in practice (Walsh et al., 2021). However, to this team’s knowledge, the CPS was the best available confidence scale designed specifically to capture confidence and preparation regarding medication administration among nursing students and was, therefore, an appropriate target for tool refinement. Broader implications for nursing education include that with the revised CPS, educators can address issues of confidence and preparation during the nursing program, at different time points during the educational process, to work to improve these skills among nursing students, and to support safer medication administration. Specifically, the revised CPS could be used before and after planned simulation-based activities for nursing students, which have successfully been used to improve medication administration skills (Pol-Castañeda et al., 2022). The revised CPS could also be integrated into curriculum assessment practices, possibly also involving the concept of a growth mindset (Carter et al., 2025), to support the nursing students’ striving toward their own competency goals. Additional educational implications include the use of the revised CPS for nursing educators to reflect on available academic support (Iheduru-Anderson & Foley, 2022) and/or their own teaching in clinical settings, which could be combined with existing clinical site environment tools (Al-Daken et al., 2024; Zhang et al., 2022) to more fully appreciate the outcomes and needs of all parties. Effective feedback mechanisms can support both students and faculty during nursing clinicals and other areas of nursing education.
As noted in the Limitations section below, although sex (biological attributes) and gender (social and cultural constructs) were considered for tool refinement purposes, the implications of sex and gender as potential influences on participants’ confidence and preparedness in medication administration were not explicitly examined. Literature reports that sex-based physiological factors and gender-related socialization patterns may impact experiences with medication administration (Romem & Rozani, 2024). In addition, there are reported gender differences in risk assessment and risk behaviors (Dawson, 2023; Harris et al., 2006). As such, this area of study is vital to investigate in future work and scholars should consider these factors directly in data collection, analysis, and interpretation.
Nursing Student Experiences
Participant responses within the cognitive interviews highlight challenges experienced by nursing students during their formative medication administration education. For example, participants shared that during school clinical experiences, opportunities for medication administration skills practice could be limited for some, depending on faculty availability and clinical settings. Available literature reports similar results, in that practical experiences necessary for skill practice can be limited due to various reasons, including ratios of students to faculty and individual restrictions placed by healthcare facilities (Schneidereith, 2021), meaning nursing students do not have the opportunity to administer medications on most clinical days (Jarvill et al., 2022). And although participants appreciated the efforts of clinical sites, nursing instructors, and institutional pedagogic efforts, those students with outside work experiences reported deeper familiarity with medication administration compared to peers without this additional experience, consistent with recent similar literature (Roman Jones et al., 2022a, 2022b). A more targeted examination as to the potential benefits of working in healthcare during a student’s nursing education, and which students may be more likely to work and why, is a potential future research inquiry worthy of consideration.
Future Research Implications
Cognitive interviews conducted early in stages of research may address issues in survey question understanding, which can be resolved prior to more extensive testing (Peterson et al., 2017). The next steps are to have the revised CPS examined and tested for its psychometric properties, and further examined with a larger sample, including GHM. The revised CPS could also be adapted and validated for different populations, including international nursing students or non-traditional learners. And while the original CPS has been used successfully in Canada and the United States, the revised CPS could also be adapted and tested in international contexts to further establish validity (Hill et al., 2022). In addition, evaluating potential differences in nursing students in relation to cultural differences, including even exposure to nurses/nursing from family members’ experiences, could be further instructive to nursing educators. In the future, once psychometric properties are established, the revised CPS will be used for testing confidence and preparation among a larger sample of undergraduate nursing students in a national nursing education study.
Limitations and Strengths
This study has several limitations. First, the interview sample was composed of 11 baccalaureate nursing students from one undergraduate college of nursing, which may have limited the diversity of perspectives. The findings are likely context-specific to the institution’s educational environment and may not capture variations in different geographical, cultural, or linguistic contexts. Second, while the cognitive interview data has resulted in a revised CPS, the revised CPS must now be psychometrically tested. As such, the study’s finding serve as preliminary evidence for refining the CPS. Third, although consistent with the literature, the small sample size leaves open the possibility of bias. Fourth, while sex and gender were reviewed for tool refinement, the implications of sex and gender as potential influences on participants’ confidence and preparedness in medication administration were not explicitly examined. Despite these limitations, the study has several strengths. First, the research team identified key revisions to the CPS through two rigorous rounds of cognitive interviews. Second, the overall reaction from the student participants indicate that this CPS asks items that closely track their experiences and is understood and answered without difficulty. Third, the results of this work present a revised CPS for other investigators to consider and further improve.
Conclusions
Cognitive interviews were conducted to assess the CPS for feasibility, clarity, and validity, with a nursing student population primarily from GHM for potential use in a larger future study. These cognitive interview data confirmed the appropriateness and usability of the revised CPS to assess confidence and preparation in a broad sample of baccalaureate nursing students. This study resulted in vital information about the thought processes underlying CPS item understanding and participant responses, as well as the resulting validity of the survey interpretation, leading to a revised CPS ready for further use and testing.
Footnotes
Appendix
Ethical Considerations
The University of Massachusetts Boston Institution Review Board approved all activities in the described research (Protocol #3420).
Consent to Participate
Informed consent was obtained verbally before participation.
Authors’ Contributions
JRJ conceptualized the grant, obtained funding, conceptualized the analysis, and wrote the manuscript. JM, AAL, RC, RB, LB, and PKG assisted with the conceptualization, conduct, and interpretation of the analysis, manuscript drafting, and editing of the manuscript.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research reported in this publication was supported by the University of Massachusetts Boston Proposal Development Grant Program (to JRJ), the Durham Center of Innovation to Accelerate Discovery and Practice Transformation (#CIN 13-410) at the Durham VA Healthcare System, and VA HSR&D grants #18-234 (to AAL). The content is solely the responsibility of the authors and does not reflect the position or policy of the University of Massachusetts, Duke University, Western University, The Pennsylvania State University, the US Department of Veterans Affairs, or the US government.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Lewinski reports receiving funds from PhRMA and Otsuka. The remaining authors have no competing interests to declare.
Data Availability Statement
Please contact the corresponding author.
