Abstract
Background
It is difficult to reach migrant or refugee agricultural workers about pesticide exposure prevention. Here, we describe a community health worker (CHW)-led pesticide exposure prevention workshop and the impact of this program among migrant and refugee workers in Washington state.
Methods
A focus group of migrants and refugees participated in the development of a CHW-led Spanish language pesticide exposure prevention mobile phone app and workshop. Pre- and post-workshop surveys assessed pesticide training, knowledge, and characteristics.
Results
Community health workers facilitated 28 workshops attended by 263 participants from 49 agricultural communities. Approximately 79% of participants reported no prior pesticide training. Significant improvements were observed in the proportion familiar with illnesses associated with pesticides, knowledge about pesticide definition, ability to correctly identify the content of pesticide labels, and the correct method to wash fruits and vegetables.
Conclusions
Community health workers are effective in addressing the gaps in pesticide safety education and awareness among migrant and refugee communities. Further work is needed to assess how to better integrate a mobile phone app into this training and subsequent use of the knowledge.
Agricultural workers face both acute and chronic health risks from pesticide exposure, including skin irritation, respiratory issues, and even some cancers. 1 They are particularly vulnerable to pesticide exposure due to insufficient knowledge and training on how to protect themselves.2–4 Not only are they exposed to chemicals in the fields and surrounding areas during work hours but they may also inadvertently carry these substances home on their skin and clothing.4,5 This poses a risk of secondary exposure to their families..
Washington State ranks second only to California in the production of fruits, tree nuts, and vegetables. 6 Pesticide application rates for these crops are 4.5 times the national average, posing significant health risks to farmworkers. 7 The Washington State Department of Health's Pesticide Illness Surveillance and Prevention Program investigated 251 events affecting 275 individuals in 2022. 8 Nearly 70% of these events met the Centers for Disease Control and Prevention and National Institute for Occupational Safety and Health criteria for acute pesticide exposure illnesses. In addition, underreporting of potential acute pesticide-related illnesses remains a significant issue. 3 Many affected individuals do not seek medical attention due to a lack of awareness, fear of job loss, or risk of deportation.
While numerous resources on pesticide exposure are available from state and federal agencies, many of these are only available in English. Although professionals often conduct training sessions such as agricultural extension agents, it is difficult to reach agricultural workers within migrant or refugee communities. 3 Rarely is this information disseminated by individuals working in the agricultural sector.
Community Health Workers (CHWs), also known as “Promotores” within the Hispanic community, can be effective in disseminating health information to underserved communities through linguistically appropriate and culturally sensitive methods.9,10 The Community Health Worker Coalition for Migrants and Refugees (CHWCMR), a nonprofit in Washington State, has experience with a community-informed approach to train CHWs who then facilitate educational workshops as trusted members of their local community. Examples include programs that address influenza vaccination, diabetes, and oral health.11–13
Community Health Worker Coalition for Migrants and Refugees identified a need to offer pesticide training in Washington state that is both culturally and linguistically appropriate, aimed at enhancing Hispanic agricultural workers’ understanding of pesticide safety while considering their language and literacy. 4 Although CHWs have been utilized in many states to disseminate information about mitigating the harms from pesticide exposure, there are few if any evaluations of the impact of those programs within Hispanic migrant and refugee agricultural workers. Here, we describe the structure and components of the pesticide exposure prevention program, evaluation outcomes from the workshops conducted by CHWs, lessons learned, and future steps.
Methods
Participants and Setting
Community health workers who were members of CHWCMR were recruited from agricultural communities in mostly rural areas across the state for the program. Washington state counties represented by these CHWs included Skagit, Thurston, Pierce, Yakima, Benton, Franklin, and Whatcom. Community health workers worked in pairs to recruit local community members to participate in the workshops. The goal for each workshop was to have 10 to 25 participants.
Program Development and Implementation
The project commenced with the creation of the “Pestisol” mobile phone app (developed in Spanish for CHWCM). The app provides the user with access to a series of short videos about pesticide exposure prevention in Spanish developed by the University of California Davis in collaboration with the University of Oregon with support from the United States Department of Agriculture. An interactive series of questions allows the user to assess their knowledge and review materials to refresh their knowledge. A focus group of 47 community members, primarily migrants and refugees, informed the development of the phone app and then tested the pesticide exposure prevention measures guided by the app. A training curriculum for 2-h pesticide workshops was subsequently developed by incorporating feedback from the focus group. An outline of the 2-h workshop and topics covered can be found in Table 1.
Workshop Content.
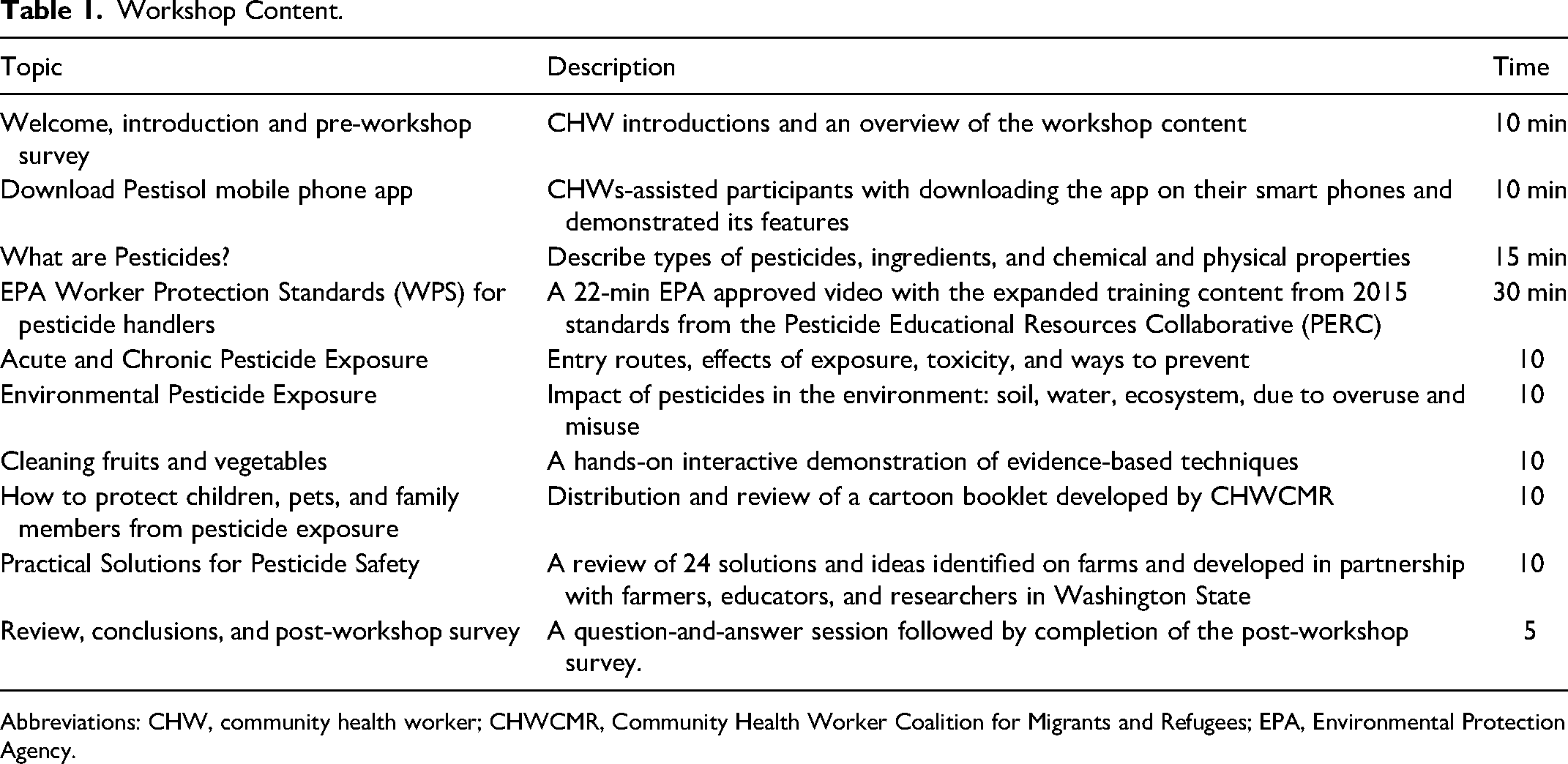
Abbreviations: CHW, community health worker; CHWCMR, Community Health Worker Coalition for Migrants and Refugees; EPA, Environmental Protection Agency.
The training approach taken by CHWs involved first building trust and forging personal connections with agricultural workers within their local community and then recruiting them to participate in the 2-h interactive workshop either at a local community center or agricultural worker housing sites. The workshop curriculum used real-world examples to highlight the critical nature of pesticide safety and was tailored to align with cultural beliefs, practices, and values. During these workshops, participants downloaded the Pestisol phone app. After each workshop, CHWs conducted home visits to the residences of agricultural workers and collaborated with local community leaders to discuss pesticide safety.
Data Collection and Analysis
This is an observational pre-post intervention study. A survey was administered by the CHWs to all workshop participants before and after the educational program to evaluate the workshop. The survey asked about their characteristics, prior pesticide training experience, their knowledge about pesticides and associated health risks, and how to reduce the risk of pesticide exposure (see Appendix). The change in the proportion of the correct response to individual questions on the survey from pre-workshop to post-workshop was assessed using a χ2 test.
This program was supported by funding from the Washington Department of Ecology's Public Participation Grant program in 2019. The overall evaluation design and methods were reviewed and determined to meet Category 1 exempt criteria by the Kaiser Permanente Washington Health Research Institute's Institutional Review Board.
Results
From 2019 to 2023, 48 migrant CHWs facilitated pesticide workshops. Collaborating in pairs, they held 28 sessions attended by 263 participants from 49 agricultural communities across Washington state. All attendees successfully downloaded the “Pestisol” phone app and shared it with an additional 10 migrants each, totaling 2950 downloads. While the first workshops in 2019 were in-person, subsequent sessions shifted online due to the COVID-19 pandemic. Community health workers trained between 10 and 25 migrants per workshop. Participant characteristics are displayed in Table 2. All participants in the workshops returned both pre- and post-workshop surveys.
Characteristics of Workshop Participants.

Prior to the workshop, 79% reported that they had no prior training in preventing pesticide exposure. Two-thirds of participants (66%) reported they had worked with pesticides for more than 3 years. Among those with 5 or more years of experience working with pesticides, only 30% of participants had received pesticide-specific training (see Figure 1).

Years worked with pesticides and prior training.
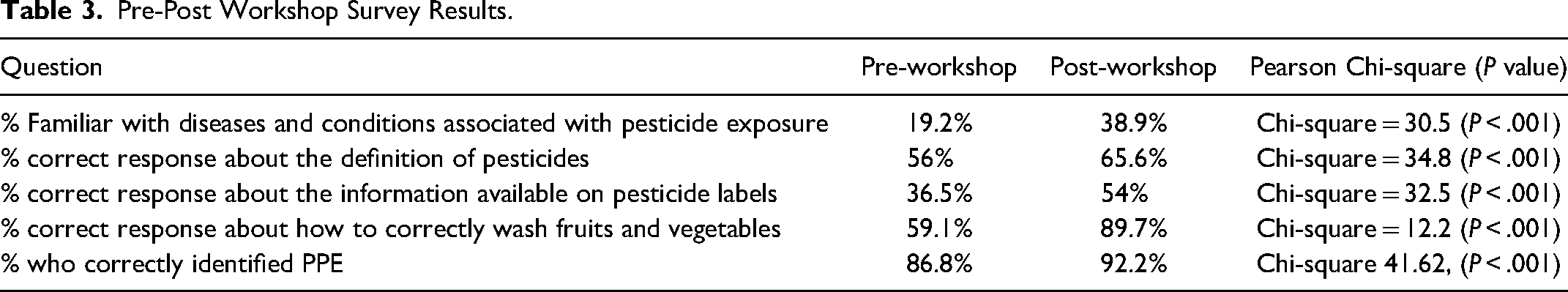
The proportion with correct responses to individual questions within each group on the pre- and post-workshop surveys is found in Table 3. These improvements were statistically significant across all questions: the proportion who were familiar with illnesses associate with pesticide exposure (from 19.2% to 38.9%), knowledge about the definition of pesticides (from 56% to 65.6%), ability to correctly identify the content of labels on pesticides (from 36.5% to 54%), and identification of the correct method to wash fruits and vegetables (from 59% to 90%).
Pre-Post Workshop Survey Results.
Discussion
Community Health Workers were successful in engaging with and training members of their local community about pesticides. Remarkably, 79% of all workshop participants reported no prior training regarding pesticide exposure, and even among those who had worked with pesticides for 5 years or more, only 70% reported any prior training. The agricultural workforce is increasingly diverse, comprising many immigrant workers with limited English proficiency and educational backgrounds. 3 These factors make safety and health training a challenge.
Although a significant improvement, only 54% were able to correctly identify the content of pesticide labels after completing the workshop. In the context of pesticide regulation, the Environmental Protection Agency mandates that pesticides come with detailed labels. Adhering to the guidelines on these labels can minimize exposure risks. 14 Equally concerning is that only 38.9% were familiar with illnesses associated with pesticide exposure after the workshop, although a significant improvement from the 19.2% before the workshop. This may delay seeking appropriate health care and thus contribute to underreporting of pesticide-associated illnesses.
Limitations of the results from this evaluation include the potential for desirability bias in the responses provided on the surveys, especially the post-workshop survey as participants may want to provide the response that the CHW wanted to see. Although a higher percentage of workshop participants were female than in the agricultural worker population, most of these were spouses of farmworkers. Otherwise, participants have characteristics like agricultural workers in other states. No data are available to evaluate the subsequent usefulness of the Pestisol app to workshop participants, although to date 2950 individuals have downloaded the app, far more than the number of workshop participants. Finally, we were unable to perform a long-term impact evaluation. Understanding the sustained effects of the intervention beyond the immediate post-workshop period is crucial for practical implications and future research.
Conclusions
Community health workers offered a unique approach to address gaps in pesticide safety education and awareness among migrant and refugee communities in Washington State. As a trusted member of their community, they were able to successfully recruit and engage with workshop participants and improve their pesticide safety knowledge. Although CHW-led workshops can be a successful approach for pesticide exposure prevention, further evaluation of how to integrate workshops more successfully with a mobile phone app and subsequent use of the knowledge by participants is needed.
Footnotes
Acknowledgments
The authors would like to recognize our CHWCMR champions and members of our community who participate in our Pesticide workshops statewide and the Department of Ecology State of Washington.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by a series of contracts from the Washington State Department of Ecology to the Community Health Worker Coalition for Migrants and Refugees: Contract #SWMPPG-1921-CHWCMR-00043, #SWMPPG-2021-CHWCMR-00026 and #SWMPPG-2023-CHWCMR-00016.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
