Abstract
Background:
Human factors play an important role in health-care outcomes of heart failure (HF) patients. A systematic review and meta-analysis of clinical trial studies on HF hospitalization may yield positive proofs of the beneficial effect of specific care management strategies.
Purpose:
To investigate how the 8 guiding principles of choice, rest, environment, activity, trust, interpersonal relationships, outlook, and nutrition reduce HF readmissions.
Basic Procedures:
Appropriate keywords were identified related to the (1) independent variable of hospitalization and treatment, (2) the moderating variable of care management principles, (3) the dependent variable of readmission, and (4) the disease of HF to conduct searches in 9 databases. Databases searched included CINAHL, Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, ERIC, MEDLINE, PubMed, PsycInfo, Science Direct, and Web of Science. Only prospective studies associated with HF hospitalization and readmissions, published in English, Chinese, Spanish, and German journals between January 1, 1990, and August 31, 2015, were included in the systematic review. In the meta-analysis, data were collected from studies that measured HF readmission for individual patients.
Main Findings:
The results indicate that an intervention involving any human factor principles may nearly double an individual’s probability of not being readmitted. Participants in interventions that incorporated single or combined principles were 1.4 to 6.8 times less likely to be readmitted.
Principal Conclusions:
Interventions with human factor principles reduce readmissions among HF patients. Overall, this review may help reconfigure the design, implementation, and evaluation of clinical practice for reducing HF readmissions in the future.
Keywords
Introduction
Heart failure (HF) is a chronic and progressive condition in which the heart muscle is unable to pump enough blood to meet the body’s need for blood and oxygen. 1 Placement into class I, II, III, or IV of the New York Heart Association functional classification depends on the severity of patient symptoms and physical activity limitations. 1 Heart failure is a leading cause of hospitalization and health-care costs in the United States. Nearly 5.1 million Americans have been diagnosed with HF, and approximately half die within 5 years of diagnosis. 2,3 The total costs of HF to the nation, in terms of direct medical costs and lost productivity, are estimated to be US$32 billion annually. 2,3 Congestive HF is the most common reason for readmission among Medicare fee-for-service patients, 4 and up to 25% of HF patients are readmitted within 30 days. 5 An analysis of Medicare claims data from 2007 to 2009 showed that 35% of readmissions within 30 days were for HF. 5 Section 3025 of the Affordable Care Act amended the Social Security Act to establish the Hospital Readmissions Reduction Program, which requires the Centers for Medicare and Medicaid Services to decrease reimbursements to hospitals with excessive risk-standardized readmissions. 6 This program encourages hospitals to develop interventions to reduce the readmission rates for HF patients. Increasingly, care management practices incorporate human factors that can influence the relationship between therapeutic interventions and patient outcomes. These interventions commonly involve human factors, including components such as education and assessment, rest and relaxation, exercise, interpersonal relationships, outlook, and dietary recommendations.
Research Questions
In a search for the causal mechanisms for enhancing patient care outcomes, this investigation explored how scientific literature has documented the moderating influence of varying care management principles involving human factors on hospital outcomes of HF patients. A systematic review of intervention strategies was conducted, and a broad range of intervention types aimed at reducing HF readmissions was included. The selected intervention components include education and assessment, rest and relaxation, exercise, interpersonal relationships, outlook, and dietary recommendations. The systematic review and meta-analysis aimed to answer the following research questions: Is there evidence that particular intervention components may modify the care management effects on HF readmission? Does a single intervention component work more effectively than a combination of intervention components in care management for HF patients? How can the knowledge gained from the systematic review and meta-analysis be applied in population health management for HF?
Material and Methods
Data Sources and Searches
Appropriate keywords were identified related to (1) the independent variable of hospitalization and treatment, (2) the moderating variable of intervention components, (3) the dependent variable of readmission, and (4) HF. Combinations with 1 keyword from each of the 4 categories (see Table 1) were used to conduct searches in 9 databases: CINAHL, Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, ERIC, MEDLINE, PubMed, PsycInfo, ScienceDirect, and Web of Science. Although systematic reviews were not included in the meta-analysis, the Cochrane Database of Systematic Reviews was searched in case any similar studies existed.
List of Keywords for Database Searches.

Study Selection, Data Extraction, and Quality Assessment
Table 2 shows the inclusion and exclusion criteria in regard to population, interventions, outcomes, timing of outcomes, time period, settings, publication language, design, and publication format. Only studies associated with HF hospitalization and readmissions, published in English, Chinese, French, German, Italian, Portuguese, and Spanish between January 1, 1990, and August 31, 2015, were compiled. Retrospective studies were excluded. Studies that evaluated interventions focused on only pharmaceuticals, surgical procedures, technology, or other therapeutic strategies and that did not incorporate any of the selected human factors were excluded. Each selected study was reviewed by a team of 5 graduate students with training in rating the quality. The detailed characteristics of cited studies are listed in Appendix A.
Inclusion and Exclusion Criteria for Studies of Intervention Patients Hospitalized for HF.

Data Synthesis and Analysis
Studies that focused on HF and other chronic illnesses and reported the number of readmissions for only HF patients were included if they met the inclusion criteria. All studies that reported the number of persons readmitted in each group were included in the meta-analysis. Although a study that only reported the total number of readmissions per group was included in the systematic review, it was not included in the meta-analysis. Additionally, studies in the systematic review could not be included in the meta-analysis if they evaluated multiple intervention groups and a control group rather than only 1 intervention group and 1 control group, or if the study reported numbers for only composite outcomes, such as readmission and death.
In the Comprehensive Meta-Analysis (Version 2) software, 7 a mixed-effects model was used to synthesize effect sizes from independent studies, which were also categorized into subgroups based on the moderator variable of intervention components. A random-effects model was used to combine studies within each subgroup, and a fixed-effect model was used to combine subgroups and yield the overall effect. The study-to-study variance was not assumed to be the same for all subgroups. This is the method used by Review Manager (RevMan). 7 The odds ratio represented the odds of successfully avoiding HF readmissions, given exposure to an intervention involving 1 or more intervention components. A funnel plot of log odds ratio was created to test for publication bias.
Results of Systematic Review
A flow diagram of the systematic review of literature is shown in Figure 1. The characteristics of the 113 included studies are shown in Appendix A. The interventions were grouped by components. Limited biases were introduced since only studies with proven quality were included. The empirical evidence provided by the systematic review is summarized in this section.

Flowchart of the systematic review of literature.
Education and Assessment
Eleven studies incorporated education and assessment.
8
–18
In 9 of these studies, readmissions were significantly lowered. These interventions included: Patient education during hospitalization and postdischarge telemonitoring for reinforcement of education and assessment of patients
13
or postdischarge home visits and monthly calls for reinforcement, assessment, and medication compliance
8
Phone calls after discharge for patient education, assessment of symptoms and compliance, and review of medication adherence
14
Postdischarge patient education at outpatient clinics and assessment of symptoms and compliance during clinic visits
12
or during follow-up calls every 2 to 4 weeks
16
Postdischarge assessments of medication adherence, symptoms/health, and compliance through a single home visit 1 week after discharge,
18
through daily telemonitoring and outpatient clinic visits every 1 to 2 weeks,
11
and through a daily telemonitoring system.
9
Exercise
Four studies incorporated exercise. 19 –22 In all 4 studies, readmissions were significantly lowered. These interventions included:
Interpersonal Relationships
Two studies incorporated interpersonal relationships. 23,24 In these studies, readmissions were not significantly lowered.
Outlook
Two studies incorporated outlook. 25,26 In these studies, readmissions were not significantly lowered.
Dietary Recommendations
Three studies incorporated dietary recommendations.
27
–29
In 2 of these studies, readmissions were significantly lowered. These interventions included: A comparison of 2 groups, one with a low-sodium diet and the other with a medium-sodium diet. Both groups had 1000 mL/d fluid restriction and a high diuretic dose. The group with the medium-sodium diet showed a significant reduction in readmissions
28
Eight different combinations of levels of fluid intake restriction, sodium intake, and diuretic dosages. A normal sodium diet with high diuretic doses and fluid intake restriction was most effective in reducing readmissions.
29
Education and Assessment Combined With Exercise
Two studies incorporated these 2 components.
30,31
In 1 of these studies, readmissions were significantly lowered. This intervention included: Patient education during hospitalization and postdischarge assessment of symptoms and compliance with emphasis on activity and treatment through Internet-based monitoring 3 times per week.
30
Education and Assessment Combined With Interpersonal Relationships
Four studies incorporated these 2 components.
32
–35
In 2 of these studies, readmissions were significantly lowered. These interventions included: Postdischarge education and counseling for patients and families to influence medication adherence through clinic visits and phone calls focused on incorporating significant others and building positive medication-taking behaviors.
35
Education and Assessment Combined With Outlook
One study incorporated these 2 components. 36 In this study, readmissions were not significantly lowered.
Education and Assessment Combined With Dietary Recommendations
Thirty studies incorporated these 2 components.
37
–65
In 16 of these studies, readmissions were significantly lowered. These interventions included: Patient education during hospitalization and weekly or biweekly phone calls postdischarge to reinforce education and assess symptoms, compliance,
62,63
and medication adherence
45,58
Diet and self-care education during hospitalization and reinforcement of education and assessment of symptoms and compliance after discharge through weekly calls for 2 weeks,
42
weekly calls for 12 weeks and 2 clinic visits,
53
or calls and clinic visits tailored to individual patient needs
55
Diet, disease, and drug therapy education at discharge and after discharge on monthly phone calls, clinic assessments, and using a pill counter
43
Postdischarge phone calls weekly or biweekly for patient education
39,40
Telemonitoring to assess diet, weight, symptoms,
57
and medication adherence, along with home visits
38
Patient education about symptoms and diet at discharge and after discharge over the phone, monthly home visits, and a daily diary for assessment of symptoms and compliance
52
Postdischarge patient education on HF and diet at outpatient clinics, assessment of symptoms and compliance during clinic visits, and monitoring diet and/or medication adherence on calls
47,64
or through the use of a diary and printed guide.
50
Rest and Relaxation Combined With Outlook
One study incorporated these 2 components.
66
In this study, readmissions were significantly lowered. This intervention included: Relaxation therapy consisting of relaxation training and music therapy for 1 hour daily and basic psychological care lasting 4 weeks.
66
Exercise Combined With Outlook
One study incorporated these 2 components. 67 In this study, readmissions were not significantly lowered.
Education and Assessment Combined With Exercise and Interpersonal Relationships
One study incorporated these 3 components.
68
In this study, readmissions were significantly lowered. This intervention included: A cardiac rehabilitation program for 12 weeks with individualized exercise plans and group-based educational session for patients and families.
68
Education and Assessment Combined With Exercise and Dietary Recommendations
Twenty-two studies incorporated these 3 components.
69
–90
In 12 of these studies, readmissions were significantly lowered. These interventions included: Comprehensive patient education during hospitalization and a follow-up call 1 to 2 weeks after discharge
76
and at 90 days for high-risk patients
72
Patient education during hospitalization and postdischarge assessment of symptoms and compliance with emphasis on diet, activity, and treatment through biweekly phone calls
74
Comprehensive patient education during hospitalization and postdischarge reinforcement and assessment of symptoms and compliance emphasizing diet, activity, and treatment through home visits at least once weekly for 6 weeks
70
Postdischarge clinic visits and phone calls at 6-month intervals to provide patient education and assess symptoms and compliance
86
Patient education postdischarge during 2 to 5 clinic visits and assessment of symptoms, compliance, and medication use through follow-up phone calls
77
or through the use of a diary and/or pill counter,
73
as well as motivational interviewing,
81
or during monthly home visits with follow-up phone calls every 10 to 15 days
89
One home visit during the first 2 weeks after discharge to provide patient education on self-management, diet, and physical activity and assess medication adherence and/or symptoms
69
and follow-up phone calls at 3 and 6 months for assessment
85
Education on self-care management, diet, and exercise delivered by a multidisciplinary team weekly for 6 weeks with a 1-hour exercise component.
78
Education and Assessment Combined With Interpersonal Relationships and Dietary Recommendations
Six studies incorporated these 3 components.
91
–96
In 4 of these studies, readmissions were significantly lowered. These interventions included: Postdischarge education on diet and sodium restriction for patients and caregivers through weekly outpatient clinic visits
92
or coaching phone calls
96
Education on HF, diet, and drug therapy for patients and caregivers at discharge and postdischarge on monthly phone calls, clinic assessments, and medication checklist
94
Development of care plan and patient and caregiver education by a multidisciplinary team during hospitalization and weekly home visits to reinforce education and assess symptoms and compliance for 9 weeks postdischarge.
95
Education and Assessment Combined With Outlook and Dietary Recommendations
Two studies incorporated these 3 components. 97,98 In these studies, readmissions were not significantly lowered.
Education and Assessment Combined With Rest and Relaxation, Exercise, and Dietary Recommendations
One study incorporated the 4 components.
99
In this study, readmissions were significantly lowered. This intervention included: Pharmaceutical care, education about self-care, drugs, and medication, and 1 month of self-monitoring diary cards to record medication use, physical activity, diet, and symptoms.
99
Education and Assessment Combined With Exercise, Interpersonal Relationships, and Dietary Recommendations
Eight studies incorporated these 4 components.
100
–107
In 6 of these studies, readmissions were significantly lowered. These interventions included: Educational programs in clinics for patients and families
102,103
Predischarge education on self-monitoring, diet, exercise, and medication and interview of patients and caregivers by nurse and postdischarge outpatient clinic visits every 3 months to review performance and introduce strategies to improve treatment adherence and response
100
Comprehensive patient education with families/caregivers during hospitalization and postdischarge reinforcement and assessment of symptoms and compliance emphasizing diet, activity, and treatment through clinic visits every 3 months
106
or clinic visits and phone calls every 2 to 8 weeks
101
Home visit once during the first month after discharge for education on self-management, diet, physical activity, and vaccinations for the patient and caregiver, and pill organizers provided for medication adherence.
104
Education and Assessment Combined With Exercise, Outlook, and Dietary Recommendations
Three studies incorporated these 4 components.
108
–110
In 1 of these studies, readmissions were significantly lowered. This intervention included: A multidisciplinary disease management program to provide in-person education to patients when enrolled in the intervention and through follow-up, which included outpatient clinic visits and monthly telephone calls and then visits every few months beginning at 6 months if patients had stabilized.
110
Education and Assessment Combined With Exercise, Interpersonal Relationships, Outlook, and Dietary Recommendations
Nine studies incorporated these 5 components.
111
–119
In 2 of these studies, readmissions were significantly lowered. These interventions included: A telehealth system that combined self-monitoring and motivational support tools in addition to a comprehensive, multidisciplinary HF care program
112
Patient education about HF, medication, diet, and activity during hospitalization, at discharge, or after discharge during home visits and phone calls, which also included assessment of diet, weight, and medication checklist
117
Education and Assessment Combined With Rest and Relaxation, Exercise, Interpersonal Relationships, Outlook, and Dietary Recommendations
One study incorporated these 6 components. 120 In this study, readmissions were not significantly lowered.
Results of Meta-Analysis
A meta-analysis allowed for the combination of data from 67 studies to determine the impact of single or combined intervention components aiming to reduce HF readmissions. Studies included in the systematic review could not be included in the meta-analysis if only the total number of readmissions per group was reported, if multiple intervention groups were assessed, or if only composite outcomes were reported. Figure 2 shows the forest plot of the effect sizes and confidence intervals for each study in the fixed-effect and random-effects models. In the mixed-effects model, the overall odds of being readmitted were 1.79 times lower among participants of interventions that involved any of these intervention components. The funnel plot of log odds ratio was symmetrical, which indicates that publication bias was unlikely. 121

Forest plot of odds ratios for heart failure (HF) readmission in included studies.
Discussion and Conclusions
This analysis yields robust results that are based on a systematic review and meta-analysis of published studies that evaluate interventions involving particular components aimed at reducing HF readmissions. Intervention strategies incorporating certain human factors or combinations of such factors have the potential to enhance therapeutic outcomes for HF patients following hospitalization. The implications of the key findings are as follows: The independent and combined effects of education and assessment are the most beneficial strategies to yield a positive benefit to avoid or reduce readmissions of HF patients. A care management or disease management team could consider a person-centered approach to enhance individual choice or self-efficacy for the patients. Exercise combined with education and assessment or rest and relaxation shows greater benefits than exercise alone. A clinical team could examine how activities were prescribed, implemented, and evaluated. Lack of adherence to or uncertainty about prescribed activities for the therapeutic outcomes may have prevented activities from demonstrating their beneficial effects on readmissions. Nutrition combined with other intervention components reveals a clear positive effect. Dietary interventions should be combined with other strategies in order to maximize their benefit in the reduction of risk for HF readmissions. Interventions with the aforementioned components increase the likelihood of not being readmitted to the hospital for HF. The meta-analysis results indicate that an intervention involving 1 or more of these components doubles an individual’s probability of not being readmitted.
This study is not without limitations. Potential limitations include the risk of bias at the study level and the possibility of incomplete retrieval of studies that meet the criteria. Furthermore, consideration should be given to other human factors and information technology that may facilitate patient–provider communications and coordinated care for chronic conditions as effective care modalities are developed and implemented for HF care management. This study focused on therapeutic interventions that incorporated certain human factors; therefore, comparison of these interventions to those not incorporating human factors was beyond the scope of this analysis. Overall, this research may help reconfigure the design, implementation, and evaluation of clinical practice for reducing HF readmissions in the future.
Footnotes
Appendix A
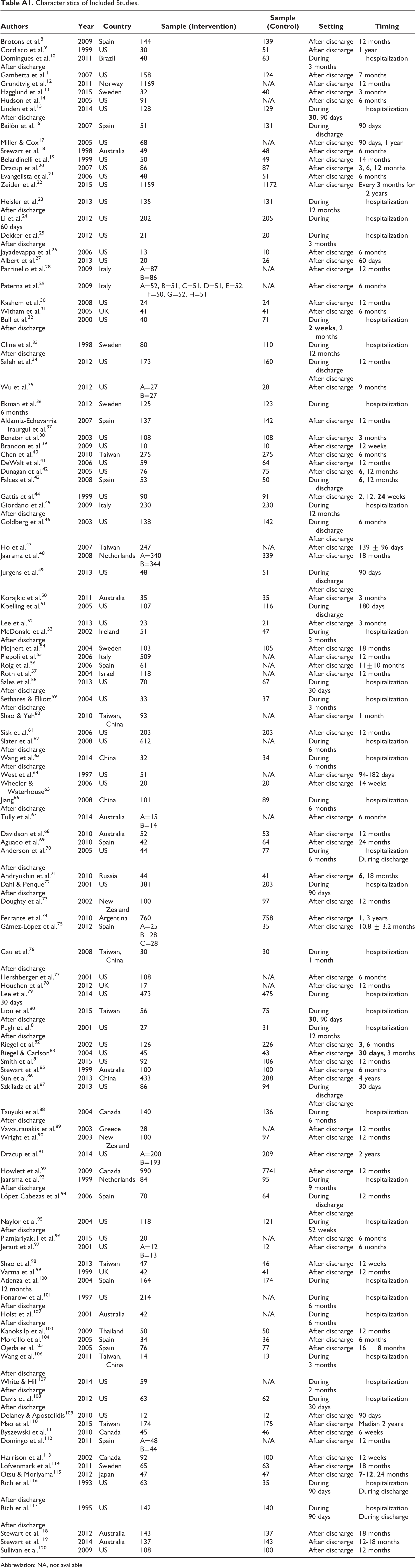
Characteristics of Included Studies.
|
|
|
|
|
|
|
|
|---|---|---|---|---|---|---|
| Brotons et al. 8 | 2009 | Spain | 144 | 139 | After discharge | 12 months |
| Cordisco et al. 9 | 1999 | US | 30 | 51 | After discharge | 1 year |
| Domingues et al. 10 | 2011 | Brazil | 48 | 63 | During hospitalization | 3 months |
| After discharge | ||||||
| Gambetta et al. 11 | 2007 | US | 158 | 124 | After discharge | 7 months |
| Grundtvig et al. 12 | 2011 | Norway | 1169 | N/A | After discharge | 12 months |
| Hagglund et al. 13 | 2015 | Sweden | 32 | 40 | After discharge | 3 months |
| Hudson et al. 14 | 2005 | US | 91 | N/A | After discharge | 6 months |
| Linden et al. 15 | 2014 | US | 128 | 129 | During hospitalization |
|
| After discharge | ||||||
| Bailón et al. 16 | 2007 | Spain | 51 | 131 | During discharge | 90 days |
| Miller & Cox 17 | 2005 | US | 68 | N/A | After discharge | 90 days, 1 year |
| Stewart et al. 18 | 1998 | Australia | 49 | 48 | After discharge | 6 months |
| Belardinelli et al. 19 | 1999 | US | 50 | 49 | After discharge | 14 months |
| Dracup et al. 20 | 2007 | US | 86 | 87 | After discharge | 3, 6, |
| Evangelista et al. 21 | 2006 | US | 48 | 51 | After discharge | 6 months |
| Zeitler et al. 22 | 2015 | US | 1159 | 1172 | After discharge | Every 3 months for 2 years |
| Heisler et al. 23 | 2013 | US | 135 | 131 | During hospitalization | 12 months |
| After discharge | ||||||
| Li et al. 24 | 2012 | US | 202 | 205 | During hospitalization | 60 days |
| Dekker et al. 25 | 2012 | US | 21 | 20 | During hospitalization | 3 months |
| After discharge | ||||||
| Jayadevappa et al. 26 | 2006 | US | 13 | 10 | After discharge | 6 months |
| Albert et al. 27 | 2013 | US | 20 | 26 | After discharge | 60 days |
| Parrinello et al. 28 | 2009 | Italy | A=87 | N/A | After discharge | 12 months |
| B=86 | ||||||
| Paterna et al. 29 | 2009 | Italy | A=52, B=51, C=51, D=51, E=52, F=50, G=52, H=51 | N/A | After discharge | 6 months |
| Kashem et al. 30 | 2008 | US | 24 | 24 | After discharge | 12 months |
| Witham et al. 31 | 2005 | UK | 41 | 41 | After discharge | 6 months |
| Bull et al. 32 | 2000 | US | 40 | 71 | During hospitalization |
|
| After discharge | ||||||
| Cline et al. 33 | 1998 | Sweden | 80 | 110 | During hospitalization | 12 months |
| After discharge | ||||||
| Saleh et al. 34 | 2012 | US | 173 | 160 | During discharge | 12 months |
| After discharge | ||||||
| Wu et al. 35 | 2012 | US | A=27 | 28 | After discharge | 9 months |
| B=27 | ||||||
| Ekman et al. 36 | 2012 | Sweden | 125 | 123 | During hospitalization | 6 months |
| Aldamiz-Echevarria Iraúrgui et al. 37 | 2007 | Spain | 137 | 142 | After discharge | 12 months |
| Benatar et al. 38 | 2003 | US | 108 | 108 | After discharge | 3 months |
| Brandon et al. 39 | 2009 | US | 10 | 10 | After discharge | 12 weeks |
| Chen et al. 40 | 2010 | Taiwan | 275 | 275 | After discharge | 6 months |
| DeWalt et al. 41 | 2006 | US | 59 | 64 | After discharge | 12 months |
| Dunagan et al. 42 | 2005 | US | 76 | 75 | After discharge |
|
| Falces et al. 43 | 2008 | Spain | 53 | 50 | During discharge |
|
| Gattis et al. 44 | 1999 | US | 90 | 91 | After discharge | 2, 12, |
| Giordano et al. 45 | 2009 | Italy | 230 | 230 | During hospitalization | 12 months |
| After discharge | ||||||
| Goldberg et al. 46 | 2003 | US | 138 | 142 | During discharge | 6 months |
| After discharge | ||||||
| Ho et al. 47 | 2007 | Taiwan | 247 | N/A | After discharge | 139 ± 96 days |
| Jaarsma et al. 48 | 2008 | Netherlands | A=340 | 339 | After discharge | 18 months |
| B=344 | ||||||
| Jurgens et al. 49 | 2013 | US | 48 | 51 | During discharge | 90 days |
| After discharge | ||||||
| Korajkic et al. 50 | 2011 | Australia | 35 | 35 | After discharge | 3 months |
| Koelling et al. 51 | 2005 | US | 107 | 116 | During discharge | 180 days |
| Lee et al. 52 | 2013 | US | 23 | 21 | After discharge | 3 months |
| McDonald et al. 53 | 2002 | Ireland | 51 | 47 | During hospitalization | 3 months |
| After discharge | ||||||
| Mejhert et al. 54 | 2004 | Sweden | 103 | 105 | After discharge | 18 months |
| Piepoli et al. 55 | 2006 | Italy | 509 | N/A | After discharge | 12 months |
| Roig et al. 56 | 2006 | Spain | 61 | N/A | After discharge | 11±10 months |
| Roth et al. 57 | 2004 | Israel | 118 | N/A | After discharge | 12 months |
| Sales et al. 58 | 2013 | US | 70 | 67 | During hospitalization | 30 days |
| After discharge | ||||||
| Sethares & Elliott 59 | 2004 | US | 33 | 37 | During hospitalization | 3 months |
| After discharge | ||||||
| Shao & Yeh 60 | 2010 | Taiwan, China | 93 | N/A | After discharge | 1 month |
| Sisk et al. 61 | 2006 | US | 203 | 203 | After discharge | 12 months |
| Slater et al. 62 | 2008 | US | 612 | N/A | During hospitalization | 6 months |
| After discharge | ||||||
| Wang et al. 63 | 2014 | China | 32 | 34 | During hospitalization | 6 months |
| After discharge | ||||||
| West et al. 64 | 1997 | US | 51 | N/A | After discharge | 94-182 days |
| Wheeler & Waterhouse 65 | 2006 | US | 20 | 20 | After discharge | 14 weeks |
| Jiang 66 | 2008 | China | 101 | 89 | During hospitalization | 6 months |
| After discharge | ||||||
| Tully et al. 67 | 2014 | Australia | A=15 | N/A | After discharge | 6 months |
| B=14 | ||||||
| Davidson et al. 68 | 2010 | Australia | 52 | 53 | After discharge | 12 months |
| Aguado et al. 69 | 2010 | Spain | 42 | 64 | After discharge | 24 months |
| Anderson et al. 70 | 2005 | US | 44 | 77 | During hospitalization | 6 months |
| During discharge | ||||||
| After discharge | ||||||
| Andryukhin et al. 71 | 2010 | Russia | 44 | 41 | After discharge |
|
| Dahl & Penque 72 | 2001 | US | 381 | 203 | During hospitalization | 90 days |
| After discharge | ||||||
| Doughty et al. 73 | 2002 | New Zealand | 100 | 97 | After discharge | 12 months |
| Ferrante et al. 74 | 2010 | Argentina | 760 | 758 | After discharge |
|
| Gámez-López et al. 75 | 2012 | Spain | A=25 | 35 | After discharge | 10.8 ± 3.2 months |
| B=28 | ||||||
| C=28 | ||||||
| Gau et al. 76 | 2008 | Taiwan, China | 30 | 30 | During hospitalization | 1 month |
| After discharge | ||||||
| Hershberger et al. 77 | 2001 | US | 108 | N/A | After discharge | 6 months |
| Houchen et al. 78 | 2012 | UK | 17 | N/A | After discharge | 12 months |
| Lee et al. 79 | 2014 | US | 473 | 475 | During hospitalization | 30 days |
| Liou et al. 80 | 2015 | Taiwan | 56 | 75 | During hospitalization |
|
| After discharge | ||||||
| Pugh et al. 81 | 2001 | US | 27 | 31 | During hospitalization | 12 months |
| After discharge | ||||||
| Riegel et al. 82 | 2002 | US | 126 | 226 | After discharge |
|
| Riegel & Carlson 83 | 2004 | US | 45 | 43 | After discharge |
|
| Smith et al. 84 | 2015 | US | 92 | 106 | After discharge | 12 months |
| Stewart et al. 85 | 1999 | Australia | 100 | 100 | After discharge | 6 months |
| Sun et al. 86 | 2013 | China | 433 | 288 | After discharge | 4 years |
| Szkiladz et al. 87 | 2013 | US | 86 | 94 | During discharge | 30 days |
| After discharge | ||||||
| Tsuyuki et al. 88 | 2004 | Canada | 140 | 136 | During hospitalization | 6 months |
| After discharge | ||||||
| Vavouranakis et al. 89 | 2003 | Greece | 28 | N/A | After discharge | 12 months |
| Wright et al. 90 | 2003 | New Zealand | 100 | 97 | After discharge | 12 months |
| Dracup et al. 91 | 2014 | US | A=200 | 209 | After discharge | 2 years |
| B=193 | ||||||
| Howlett et al. 92 | 2009 | Canada | 990 | 7741 | After discharge | 12 months |
| Jaarsma et al. 93 | 1999 | Netherlands | 84 | 95 | During hospitalization | 9 months |
| After discharge | ||||||
| López Cabezas et al. 94 | 2006 | Spain | 70 | 64 | During discharge | 12 months |
| After discharge | ||||||
| Naylor et al. 95 | 2004 | US | 118 | 121 | During hospitalization | 52 weeks |
| After discharge | ||||||
| Piamjariyakul et al. 96 | 2015 | US | 20 | N/A | After discharge | 6 months |
| Jerant et al. 97 | 2001 | US | A=12 | 12 | After discharge | 6 months |
| B=13 | ||||||
| Shao et al. 98 | 2013 | Taiwan | 47 | 46 | After discharge | 12 weeks |
| Varma et al. 99 | 1999 | UK | 42 | 41 | After discharge | 12 months |
| Atienza et al. 100 | 2004 | Spain | 164 | 174 | During hospitalization | 12 months |
| Fonarow et al. 101 | 1997 | US | 214 | N/A | During hospitalization | 6 months |
| After discharge | ||||||
| Holst et al. 102 | 2001 | Australia | 42 | N/A | During hospitalization | 6 months |
| After discharge | ||||||
| Kanoksilp et al. 103 | 2009 | Thailand | 50 | 50 | After discharge | 12 months |
| Morcillo et al. 104 | 2005 | Spain | 34 | 36 | After discharge | 6 months |
| Ojeda et al. 105 | 2005 | Spain | 76 | 77 | After discharge | 16 ± 8 months |
| Wang et al. 106 | 2011 | Taiwan, China | 14 | 13 | During hospitalization | 3 months |
| After discharge | ||||||
| White & Hill 107 | 2014 | US | 59 | N/A | During hospitalization | 2 months |
| After discharge | ||||||
| Davis et al. 108 | 2012 | US | 63 | 62 | During hospitalization | 30 days |
| After discharge | ||||||
| Delaney & Apostolidis 109 | 2010 | US | 12 | 12 | After discharge | 90 days |
| Mao et al. 110 | 2015 | Taiwan | 174 | 175 | After discharge | Median 2 years |
| Byszewski et al. 111 | 2010 | Canada | 45 | 46 | After discharge | 6 weeks |
| Domingo et al. 112 | 2011 | Spain | A=48 | N/A | After discharge | 12 months |
| B=44 | ||||||
| Harrison et al. 113 | 2002 | Canada | 92 | 100 | After discharge | 12 weeks |
| Löfvenmark et al. 114 | 2011 | Sweden | 65 | 63 | After discharge | 18 months |
| Otsu & Moriyama 115 | 2012 | Japan | 47 | 47 | After discharge |
|
| Rich et al. 116 | 1993 | US | 63 | 35 | During hospitalization | 90 days |
| During discharge | ||||||
| After discharge | ||||||
| Rich et al. 117 | 1995 | US | 142 | 140 | During hospitalization | 90 days |
| During discharge | ||||||
| After discharge | ||||||
| Stewart et al. 118 | 2012 | Australia | 143 | 137 | After discharge | 18 months |
| Stewart et al. 119 | 2014 | Australia | 137 | 143 | After discharge | 12-18 months |
| Sullivan et al. 120 | 2009 | US | 108 | 100 | After discharge | 12 months |
Abbreviation: NA, not available.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
