Abstract
Introduction:
Real-time frozen section analysis of cancer margins is considered the gold standard in head and neck oncologic surgery to ensure clear margins and improve patient outcomes. 1 However, its role in thyroid cancer remains controversial, particularly in determining the need for lobectomy versus total thyroidectomy.2,3 In contrast, grossly invasive thyroid cancer involving adjacent structures often warrants intraoperative margin assessment to determine the extent of resection. 4 Here, we present the first use of a novel intraoperative workflow and pathology reporting platform, MarginView3D, in the surgical management of invasive thyroid cancer. This workflow integrates three-dimensional (3D) scans of the surgical specimen and defect to enhance communication between physicians in the operating room and the pathology lab.
Materials and Methods:
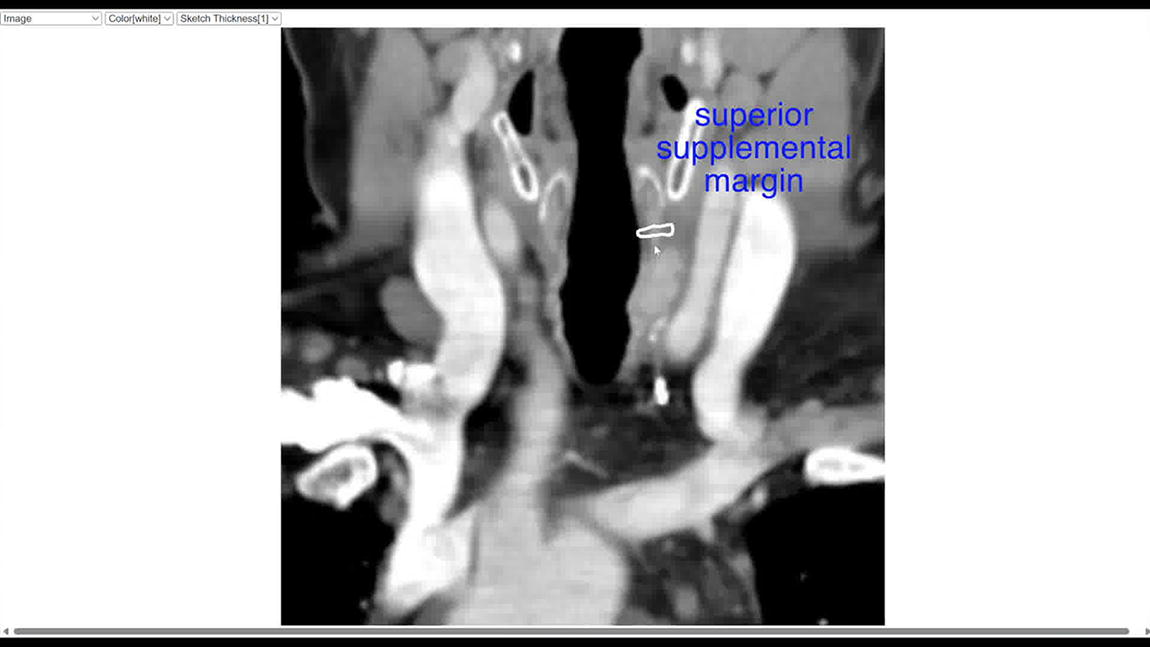
A 69-year-old female with recurrent Hurthle cell carcinoma presented with a hypermetabolic lesion in the thyroid bed extending into the tracheal wall. Intraoperative frozen section confirmed carcinoma in the left paratracheal lesion, prompting a window resection involving the inferior border of the cricoid and three hemi-tracheal rings. Given the need for real-time pathological assessment to determine the extent of resection, we initiated a novel surgical workflow incorporating 3D scanning and MarginView3D, an internally developed software for visual and interactive pathological documentation. The 3D scans of the specimen and ablative defect were created using third-party scanning software (EXScan Pro Version 3.7.4.0. and EXScan S Version 3.1.4.3.) and hardware (Einscan Pro HD, Shining 3D, Hangzhou, China and Einscan-SP, Shining 3D, Hangzhou, China).5,6 The 3D scans were imported into MarginView3D, and a series of video conferences facilitated information exchange between the surgery and pathology teams. 7 Supplemental margins confirmed tumor clearance, and reconstruction was achieved using a stair-step sliding tracheal advancement and sternocleidomastoid muscle flap.8,9 Immediately post-operation, the surgeon imported annotated radiographs and recorded a narrative summary, demonstrating the extent of surgery and area of clinical interest. The pathologist recorded an audiovisual narrative summary after the completion of permanent section analysis, providing a statement of the final oncologic status a few days after surgery.
Results:
Despite introducing new tools, the workflow was integrated without significant disruption to standard surgical or pathological procedures. MarginView3D optimized intraoperative communication between the surgery and pathology teams, facilitating critical decisions by reducing the ambiguity often associated with anatomically challenging resections. The novel workflow and software were particularly valuable for this case of thyroid cancer, where spatial understanding of tumor invasion into the trachea was critical to surgical decision-making and treatment planning. Ultimately, oncologic clearance was achieved on both intraoperative frozen section and postoperative permanent section analysis. In addition, a dynamic, 3D surgical pathology report was created in MarginView3D, bringing together 3D scans, annotated radiographs, and narrative summaries to create a dynamic, visual, and comprehensive pathology document for downstream providers involved in the patient’s cancer care.
Conclusions:
We demonstrate a novel approach to oncologic resections in invasive thyroid cancer. The use of 3D scanning and MarginView3D help to codify elements of a new workflow designed to improve oncologic clearance and understanding by all members of the patient’s care team.
The authors have no competing financial interests to be disclosed. Informed consent was obtained for publication of the video.
Runtime of video: 9 mins 26 secs.

Get full access to this article
View all access options for this article.
