Abstract
Patients with glycogen storage disease (GSD) are either orally fed (ORF) or gastronomy-tube fed (GTF) with cornstarch to maintain normal glucose levels. It is not known whether the use of cornstarch affects the microbiological oral profile of patients with GSD. Thus, the purpose of this study was to compare supragingival and subgingival plaque samples collected from 53 participants with GSD (2-56 years)—29 ORF and 24 GTF. The 16S sequence bacterial profiles of plaque DNA were obtained and a total of 768 probes were detected across the plaque groups. Orally fed patients showed higher means of cariogenic species and periodontal health-associated species, whereas GTF patients showed higher means of periopathogenic species (P < .05). Orally fed patients exhibited high levels of caries pathogens and lower levels of periodontal pathogens possibly due to the acidic environment created by their cornstarch diet, when compared to GTF patients.
Keywords
Introduction
Glycogen storage disease (GSD), also known as glycogenosis, is a group of rare conditions that affect glycogen metabolism. 1 Since the brain has minimal energy reserves and depends mostly on glucose delivery from the blood stream, maintenance of normoglycemia is critical. 2 Following a meal, glucose is stored as glycogen in the liver and muscle, acting as an important energy reserve for the body. Glycogenolysis in the liver and kidney occurs during periods of fasting to maintain normoglycemia.
The etiology of GSD is based on abnormalities of enzymes that regulate the synthesis and degradation of glycogen. Glycogen storage disease mainly affects the liver and muscles, and is categorized by which enzyme is affected. Glycogen storage disease 0, I, III, IV, VI, and IX affect the liver and cause hepatomegaly and hypoglycemia. Glycogen storage disease II, III, V, and VII affect the muscle and present as muscle pain, exercise intolerance, and progressive weakness. 1 Glycogen storage disease type XI, or also known as “Fanconi–Bickel syndrome,” affects GLUT2, a glucose transport protein, resulting in hepatomegaly, glucose and galactose intolerance, fasting hypoglycemia, proximal tubular nephropathy, and severe short stature. 3
The main goal of treatment for the hepatic forms of GSD is to maintain normal glucose levels despite deficiencies in metabolism. In infancy and early childhood, this is achieved by frequent intake of glucose and overnight nasogastric feeding. In children older than 6 to 12 months, the glucose is replaced with cornstarch mixed with water or formula. Children receive their cornstarch feeding either by mouth or through a gastrostomy tube (G-tube) that is directly inserted into their stomach. 1 All patients with the hepatic forms of GSD are also treated with a diet restricting intake of sugars and carbohydrates.
Considering the impact of diet on oral health, we hypothesized that these unique diets of with GSD might play a significant role in their oral health status. A previous study from our research group examined the oral health status of patients with GSD and revealed that patients with GSD who received cornstarch orally showed greater levels of dental caries activity as compared to the GTF group. 4 It is hypothesized that cornstarch acts as a slow release of glucose, which aids in the formation of biofilms over tooth surfaces. The frequent oral ingestion of glucose and subsequent glucose metabolism by oral biofilms result in acid production, which leads to demineralization of enamel and development of dental caries.
Previous research delineates that bacteria found in plaque biofilms are responsible for the etiology of the 2 major oral diseases that can ultimately lead to tooth loss—caries and periodontitis. 5 For instance, the initiation of dental caries has been associated with Streptococcus mutans, Streptococcus sobrinus, and Lactobacillus acidophilus, whereas Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis, Tannerela forsythia, and Trepenoma denticola are some of the suspected periodontal pathogens. 5 The evidence for the oral health status of patients with GSD is scarce. It has been reported that patients with type Ib can develop periodontitis likely due to the usual diagnosis of neutropenia. 6 Our preliminary findings demonstrated higher rates of caries development on orally fed (ORF) GSD as compared to G-tube fed (GTF) patients as mentioned above. However, no study to date has compared the oral microbial profile of patients with GSD who are ORF with those who are GTF with cornstarch.
Aim
The main purpose of this study was to compare the microbiological profile of supragingival and subgingival plaque samples of patients with GSD who are either ORF with cornstarch with those GTF. Our main hypothesis is that the microbial profiles of plaque samples from ORF patients are different from those who are GTF. An understanding of the impact of treatment of the flora will allow improved prevention and treatment of oral pathology.
Methods
This study was approved by the institutional review board of the University of Florida (protocol #714-2010). Study participants were recruited from the Glycogen Storage Disease Program of the University of Florida, from June 2011 to March 2013. A total of 53 patients with a confirmed diagnosis of GSD who were receiving cornstarch either orally (ORF) or via a G-tube (GTF) were included in the study. All participants were receiving Regular Argo cornstarch. Patients with GSD excluded from the study were those who declined participation and females who were confirmed to be pregnant.
A questionnaire was developed to record patients’ demographic information, historical information, modality of cornstarch feeding (ie, ORF or GTF), basic oral hygiene habits, age at first dental visit, and frequency of prophylactic dental care. Once inclusion criteria were assessed and informed consent was obtained, participants received a full mouth hard tissue and soft tissue clinical examination. Dental plaque samples were then collected as described below and a dental prophylaxis was performed followed by topical fluoride application.
Hard Tissue Examination
Using a mouth mirror and explorer, dental charting was performed to record the number of decay, missing (due to caries), and filled teeth. Bitewings and occlusal radiographs were taken to confirm diagnosis whenever possible.
Soft Tissue Examination
The following periodontal clinical parameters were taken at the initial visit for all patients by 1 calibrated examiner. All standard periodontal measurements were performed using a UNC-15 periodontal probe at 6 sites per tooth and recorded using a computer software (Florida probe, version 9.12.41, Gainesville, FL) to achieve periodontal diagnosis, as described previously. 7 Periapical and bite-wing X-rays were examined to assess bone loss and confirm diagnosis.
Collection of Supragingival Plaque
Supragingival dental plaque was collected from 1 carious active site (when present) and 1 noncarious tooth site (caries-free) from all participants. The area of collection was isolated with cotton rolls and plaque was carefully removed with sterile curettes and placed on Eppendorf tubes containing sterile 10 mM sodium phosphate buffer (pH 7.0). Collected samples were snap frozen and stored at −80°C until analyzed. Only plaque samples from noncarious sites were evaluated in this study in order to determine whether the composition of the bacterial flora is influenced by the mode of feeding rather than by preexisting oral conditions.
Collection of Subgingival Plaque
Bacterial subgingival biofilm was collected from 1 diseased site (when present) with probing depth (PD) ≥5 mm with bleeding on probing (BoP) and 1 nondiseased (healthy) site (PD ≤ 3 mm with no BoP) from all participants. The area of collection was isolated with cotton rolls and supragingival plaque was carefully removed with curettes. Collection was done with a sterile endodontic paper point by inserting the point to the depth of the sulcus and moving it laterally along the axis of the tooth. Immediately following sampling, the paper point was placed in an Eppendorf tube and stored at −70°C until processed. Only healthy sites were evaluated in this study in order to determine whether the composition of the bacterial flora is influenced by the mode of feeding rather than by preexisting oral conditions.
DNA Extraction and Purification
DNA was isolated from all plaque samples using a DNA Purification Kit and the protocol recommended by the manufacturer (Masterpure, Epicentre Biotechnologies, Madison, Wisconsin). Briefly, samples were lysed in PBS, sonicated, and T and C lyses solution with protease K were added. They were then incubated at 65°C water bath for 15 minutes with vortexing every 5 minutes. RNaseA (5μg/μL) was added, and samples were incubated at 37°C for an additional 30 minutes. Following the addition of 175μL of MPC protein precipitation reagent, samples were centrifuged at 4°C. Isopropanol was added and the DNA cleaned with 70% ethanol. TE buffer (25μL) was added to resuspend the DNA, and its concentration was tested using the Nanodrop ND-1000 spectrophotometer (Nanodrop Technologies, Inc, Wilmington, Delaware).
Human Oral Microbe Identification Using Next-Generation Sequencing
Purified plaque DNA at a minimum concentration of 20 ng/μL was analyzed by human oral microbe identification using next-generation sequencing (HOMINGS) at the Forsyth Institute as previously described. 8 Briefly, DNA was polymerase chain reaction (PCR)-amplified using V3-V4 primers (forward primer: CCTACGGGAGGCAGCAG and reverse primer: GGACTACHVGGGTWTCTAAT) and a 5 Prime Hot Master Mix. Polymerase chain reaction samples were purified using AMPure beads. One hundred nanograms of each library was pooled, gel-purified, and quantified using a bioanalyser and subsequently with quantitative PCR. The library mixture (12 pM), spiked with 20% Phix, was run on the MiSeq at Forsyth institute. An average of >50 000 sequences of about 441 bp per sequence were typically obtained in a MiSeq run of about 90 samples. Five hundred ninety-eight species-specific, 16S rRNA-based oligonucleotide “probes” were used in a BLAST program (called ProbeSeq for HOMINGS) to identify the frequency of oral bacterial targets. In order to get nearly complete coverage, an additional panel of 94 genus-specific probes is used. ProbeSeq outputs are expressed as percentage frequencies of target taxa.
Statistical Analysis
Percentage frequencies of each targeted species in healthy sites (nonperiodontally diseased and caries-free) were analyzed and compared between GTF and OTF patients using an unpaired t test. Probes with P < .05 were considered nominally significant. Those with false discovery rate <0.1 were considered statistically significant. All statistical analyses were performed using SAS 9.4 (Cary, North Carolina).
Results
Of the 53 participants, 30 were males and 23 females. Participants ranged from 2 to 56 years of age (mean age: 17.28 ± 14.5 years), and the breakdown of GSD types was 26 GSD Ia, 8 GSD Ib, 5 GSD III, and 14 GSD IX. A total of 29 participants were ORF and 24 participants were GTF. Among the 24 GTF patients, 1 had active carious lesions and 5 had periodontitis. In contrast, among the 29 ORF patients, 5 had active caries and 2 had periodontitis (P = .20 and .22, respectively). Among caries-active patients, 4 were type IX, 1 was type III, and 1 was type Ia. Among the periodontitis patients, 5 were type Ib, 1 was type IX, and 1 was type III. The distributions of different GSD types among the GTF and ORF groups and their corresponding caries and periodontal status are summarized in Table 1.
Distribution of Participating Individuals by GSD Type, Mode of Feeding, and the Presence of Active Caries and Periodontitis.a,b
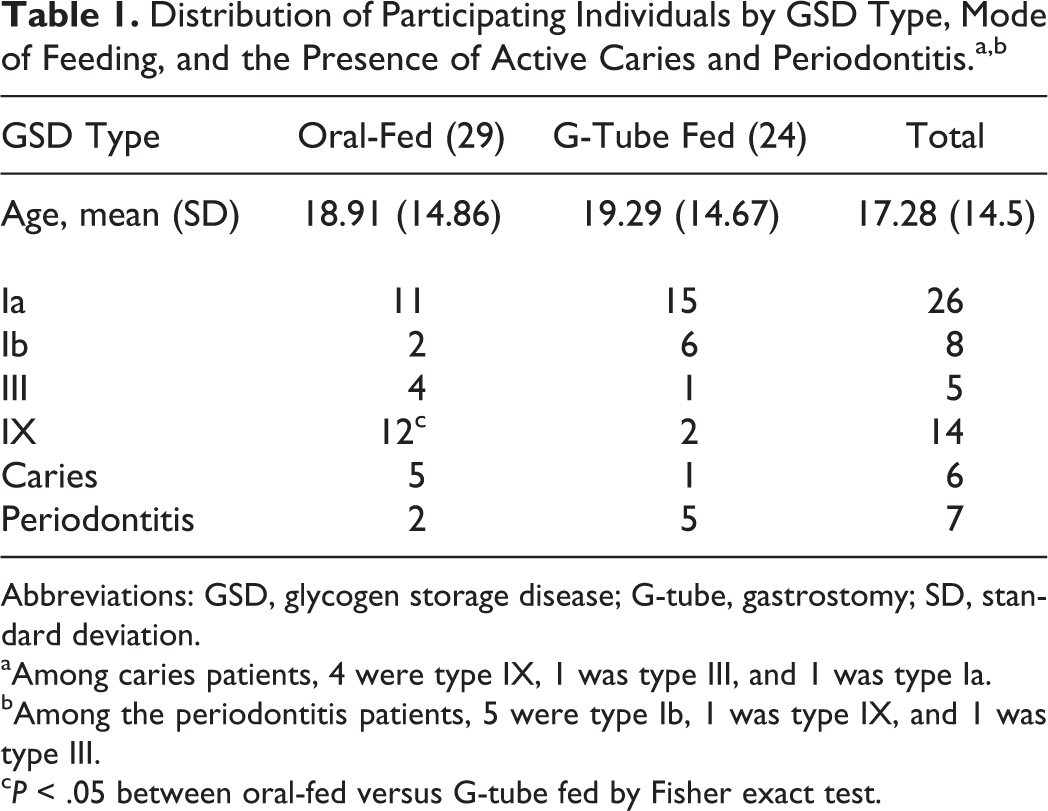
Abbreviations: GSD, glycogen storage disease; G-tube, gastrostomy; SD, standard deviation.
aAmong caries patients, 4 were type IX, 1 was type III, and 1 was type Ia.
bAmong the periodontitis patients, 5 were type Ib, 1 was type IX, and 1 was type III.
c P < .05 between oral-fed versus G-tube fed by Fisher exact test.
A total of 768 HOMINGS probes were assigned in both GSD groups. In the supragingival plaque, the frequency of 21 bacterial species were found to be significantly different (P < .05) between the ORF and GSD groups, including higher frequencies of Veillonella, Leptotrichia, and Actinomyces naeslundii species in ORF, whereas GTF patients showed higher frequencies of Fusobacterium, Aggregatibacter, and Cardiobacterium valvarum species (P < .05; Table 2). In the subgingival plaque, 24 species were found to be significantly different (P < .05) between the ORF and GTF groups, including higher frequencies of A naeslundii and Veillonella in ORF, whereas GTF had higher means of Fusobacterium, Capnocytophaga, Campylobacter, and Porphyromonas species (P < .05; Table 3).
Distribution of Significant Species in the Supragingival Plaque Between G-Tube Fed (GTF) and Orally Fed (ORF) Individuals With GSD.a,b
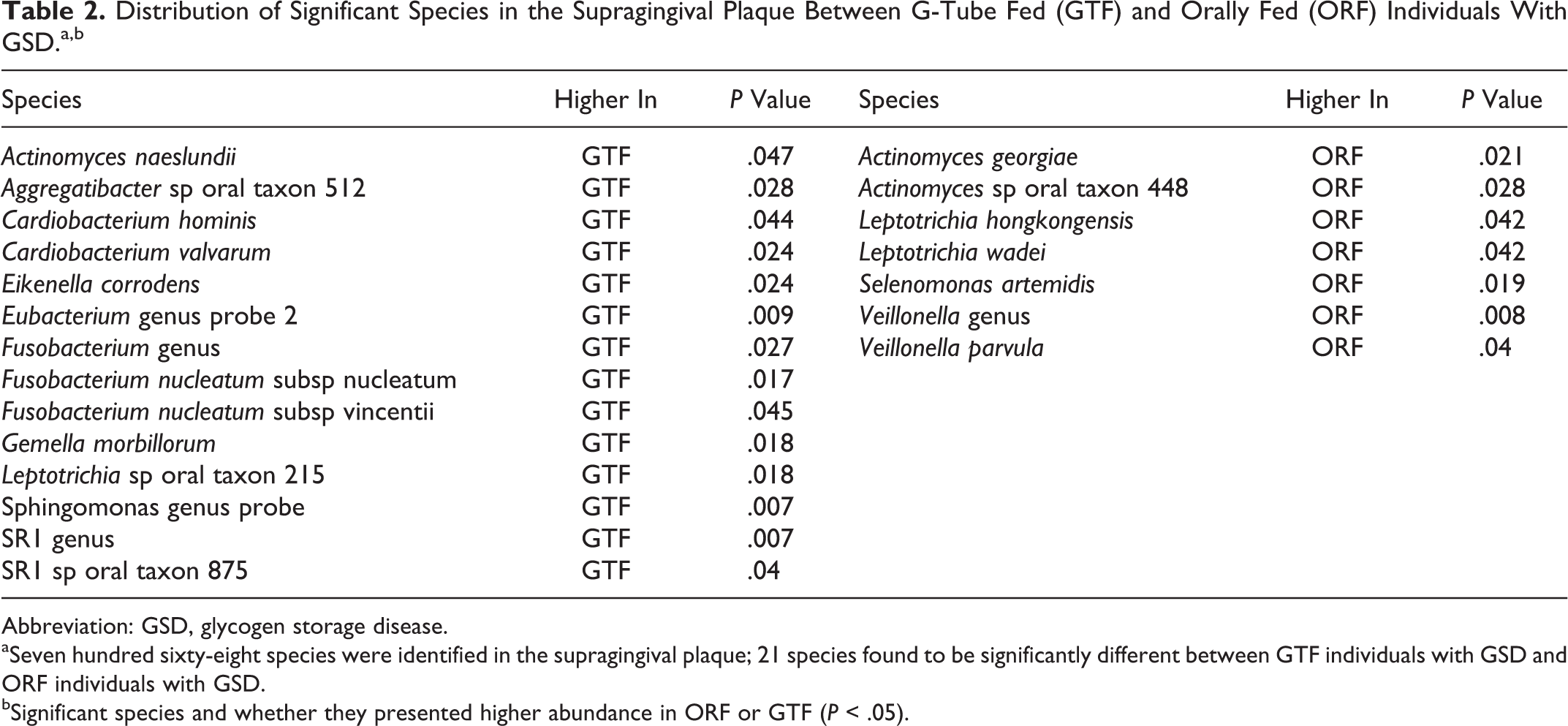
Abbreviation: GSD, glycogen storage disease.
aSeven hundred sixty-eight species were identified in the supragingival plaque; 21 species found to be significantly different between GTF individuals with GSD and ORF individuals with GSD.
bSignificant species and whether they presented higher abundance in ORF or GTF (P < .05).
Distribution of Significant Species in the Subgingival Plaque Between G-Tube Fed (GTF) and Orally Fed (ORF) Individuals With GSD.a,b
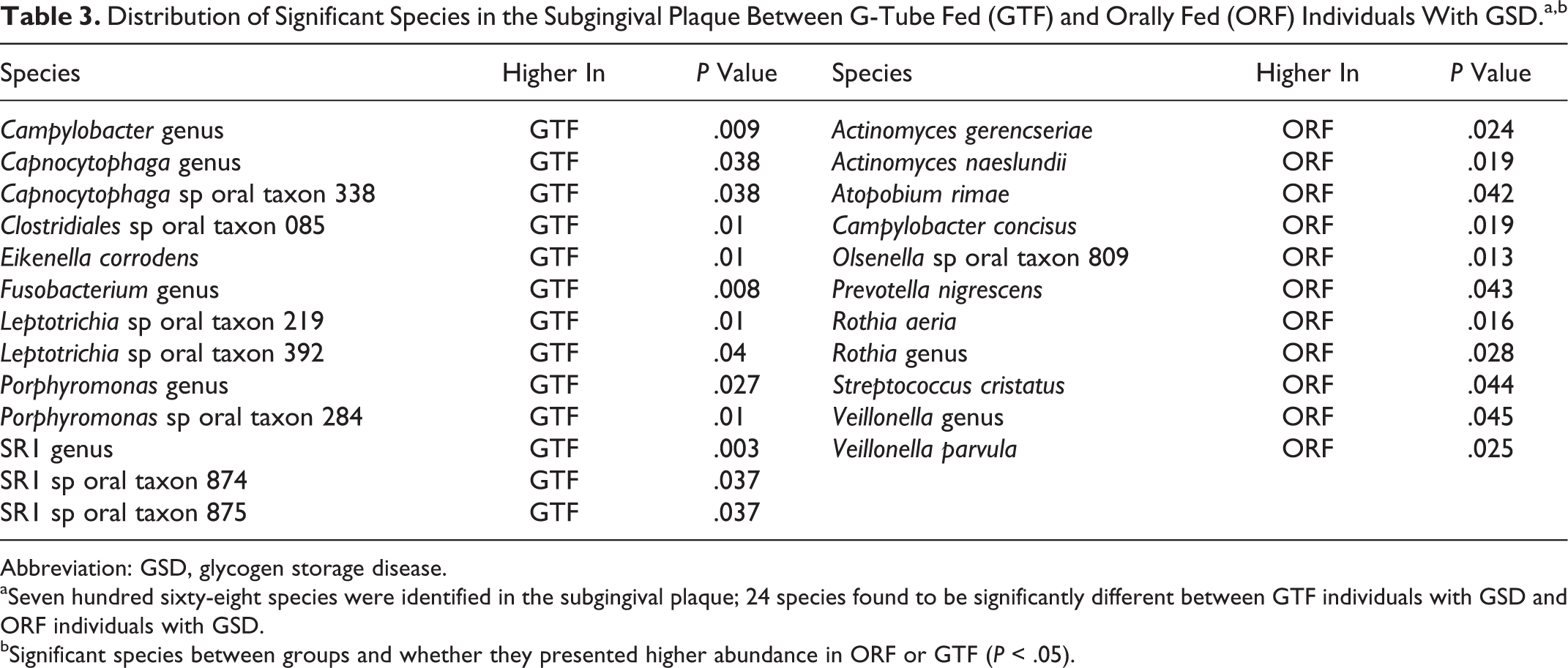
Abbreviation: GSD, glycogen storage disease.
aSeven hundred sixty-eight species were identified in the subgingival plaque; 24 species found to be significantly different between GTF individuals with GSD and ORF individuals with GSD.
bSignificant species between groups and whether they presented higher abundance in ORF or GTF (P < .05).
Discussion
Distinct bacterial communities were observed when comparing the bacterial profile of supragingival and subgingival dental plaque samples from ORF and GTF groups. In particular, ORF had higher mean frequency of Veillonella, Leptotrichia, A naeslundii species (P < .05) in the supragingival plaque, whereas GTF samples showed higher means of Fusobacterium, Aggregatibacter, and C valvarum species (P < .05). In the subgingival plaque, ORF samples showed higher means of A naeslundii and Veillonella species (P < .05), whereas the GTF had higher means of Fusobacterium, Capnocytophaga, Campylobacter, and Porphyromonas species (P < .05). The bacterial species detected have been previously associated with either dental caries or periodontal disease, as discussed below.
Interestingly, studies have shown an inverse relationship between caries and periodontal disease in terms of the clinical and bacteriological findings. 8 Previous research has demonstrated that pH is an important determinant of the microbial composition of plaque and that the production of organic acids from carbohydrate fermentation by lactic acid-producing bacteria and concomitant reduction in pH can interfere with the growth of surrounding microorganisms including periodontal pathogens. 9 In particular, the inability of P gingivalis, and other periodontal pathogens to grow at a pH below 6.5 makes its growth dependent on specific environmental conditions. Thus, the ecological determinants that reduce the proportion of lactic acid bacteria may favor the periodontal disease-inducing flora due to insufficient control mechanisms. 8
Microbial studies have shown that dental caries have a polymicrobial etiology of high complexity. 10 Although the composition of the bacterial consortia in oral biofilms varies among individuals and among carious sites of the same individuals, Veillonella, Leptotrichia, and Actinomyces naselundii species have been identified within carious lesions at different stages of disease progression. Therefore, these species have been identified as etiological agents of tooth decay. 11 In our study, these species were detected in higher proportions in the ORF group as compared to the GTF group.
In contrast to the flora associated with the caries process, periodontal disease sites tend to be dominated by gram-negative rods and motile forms including spirochetes. Fusobacterium nucleatum and Bacteroides species have been considered important colonizers in this disease. 11 In order to explain and identify species related to disease and health, species have been categorized into microbial complexes. 12 Evidence shows that species in the red and orange complexes are more prevalent and found in higher numbers in gingivitis and periodontitis. 12 Porphyromonas species for instance, are a part of the red complex, frequently associated with diseased sites, whereas F nucleatum is a part of the orange complex, considered an important “bridge” species between health and disease-associated species. Research has also demonstrated an increase in Campylobacter and Capnocytophaga species in patients with periodontal disease and in sites of inflammation. 12 Patients fed by G-tube were found to present higher proportions of Fusobacterium, Capnocytophaga, Campylobacter, and Porphyromonas species in their subgingival microbial environment.
Supragingival and subgingival plaque samples of GTF patients with GSD exhibited significantly higher levels of periodontal disease–associated species. The supragingival plaque samples of ORF patients had significantly more acidogenic as well as caries-associated species, whereas their subgingival samples showed significantly higher numbers of periodontally health-associated species, such as Veillonella and Actinomyces. 12 This microbial diversity can be explained by the fact that patients with GSD who are orally fed have an oral environment that is acidic and selective for cariogenic bacteria due to their constant intake of glucose. Thus, this environment and the selection for cariogenic bacteria might explain the increased caries risk as compared to the GTF patients observed previously. There were 5 caries-active patients among the OTF individuals compared to only 1 in the GTF group. Although this difference was not statistically different, possibly because of the overall low caries prevalence in this population, the higher number of caries-active individuals fed orally with corn starch does corroborate the microbial data found in the present investigation. On the other hand, the acidic environment created by this microbial community in these individuals, can also act to inhibit the growth of surrounding periodontal pathogens. 9 Therefore, caries and periodontal disease may demonstrate an inverse microbial relationship. 9 To corroborate this hypothesis, the subgingival environment of ORF patients do show higher abundance of A naeslundii and Veillonella species, which are known to be associated with periodontally healthy individuals. 12
Conversely, the oral environment of GTF patients might be more selective for periodontal pathogens than that of the ORF patients, which could increase their risk for periodontal disease. In this study, 8 patients presented with a diagnosis of GSD Type Ib, majority in the GTF group and with a periodontitis diagnosis. Glycogen storage disease type Ib is characterized by abnormal glucose homeostasis as well as neutropenia and neutrophil dysfunction. 13 Neutropenia is commonly associated with aggressive periodontal disease due to a breakdown in the body’s innate immune response and inability to fight infection. 6,13 Previous clinical data from this study found that a total of 7 patients presented with periodontal disease, 5 of these patients were GTF and only 2 were ORF. 4 Although not statistically different, these clinical data could support our microbial findings which suggest an increased risk for periodontal disease in GTF patients, presenting higher levels of Fusobacterium, Capnocytophaga, Campylobacter, and Porphyromonas species in their subgingival microbial environment versus those who are ORF. We cannot rule out, however, the influence of neutropenia on the development of periodontal disease in these patients as most periodontally diseased patients were type Ib. Although, we should point out here, that only healthy sites were used for the present evaluation, and even these healthy sites with “undisturbed plaque” could be more predisposed to periodontal disease breakdown due to their higher abundance of periodontally associated species. Additionally, only 5 patients presented a diagnosis of periodontal disease in the GTF group, and thus, the other periodontally healthy individuals could also be more predisposed to the disease due to a different oral microflora. However, the mere presence of periodontal disease in a higher number of individuals in the GTF group could have skewed the microbial environment of these individuals’ healthy sites and help explain the higher abundance of periodontal pathogens in this group.
Noteworthily, previous preliminary data from this study have shown that GTF individuals have not shown a different inflammatory response to bacterial stimuli when compared to ORF individuals. 14 Since the underlying and complex interaction of bacterial flora with host response is essential for the development of inflammation and periodontal disease, 15 the mechanisms for this microbial change toward a more periodontal pathogenic flora in the GTF group need to be further investigated, as well as their future susceptibility for periodontal breakdown.
The findings of our study should encourage health professionals to inform patients with GSD regarding their risks in developing potential oral diseases, depending on their type and mode of corn starch feeding, since a distinct oral bacterial profile can be found in these 2 groups, which may predispose these individuals to different oral diseases. Health professionals can also provide guidance on how to prevent and control oral diseases including dietary assessment and counseling, oral hygiene instructions, and appropriate referral to dental care.
Conclusions
Patients with GSD may present a distinctive microbial profile depending on their dietary restrictions.
Patients with GSD who are ORF with high glucose-containing diet have a dental plaque bacterial profile which indicates an increased risk for caries.
Patients with GSD who are GTF present a dental plaque bacterial profile which indicates an increased risk for periodontal disease.
Our findings support that patients with GSD should be encouraged to seek a dental home, and dental professionals should provide anticipatory guidance to patients/parents regarding their increased risks for developing caries and/or periodontal disease.
Footnotes
Acknowledgments
The authors would like to thank the financial support declared below and the assistance of all doctors and staff from the Clinical Research Center at the University of Florida.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Jonah Pournazarian Type Ib GSD Research Fund (F014421) and GSD Dream Fund (F018393), managed by the University of Florida Foundation.
