Abstract
Isolated angiokeratomas (AKs) are common cutaneous lesions, generally deemed unworthy of further investigation. In contrast, diffuse AKs should alert the physician to a possible diagnosis of Fabry disease (FD). Angiokeratomas often do not appear until adolescence or young adulthood. The number of lesions and the extension over the body increase progressively with time, so that generalization and mucosal involvement are frequent. Although rare, FD remains an important diagnosis to consider in patients with AKs, with or without familial history. Dermatologists must have a high index of suspicion, especially when skin features are associated with other earlier symptoms such as acroparesthesia, hypohidrosis, or heat intolerance. Once the diagnosis is established, prompt screening of family members should be performed. In all cases, a multidisciplinary team is necessary for the long-term follow-up and treatment.
Introduction
Fabry disease (FD, also known as Anderson-Fabry disease or angiokeratoma corporis diffusum [ACD]) is a rare X-linked disease caused by the partial or complete deficiency of a lysosomal enzyme, α-galactosidase A (α-Gal A), responsible for the catabolism of neutral sphingolipids. 1 These nonmetabolized substrates accumulate in the lysosomes of different cells (predominantly in the endothelial cells) along the whole organism. It is a multisystemic and progressive disease with a great clinical heterogenicity, with classical and mild late-onset phenotypes. 2 It is highly penetrant in males, with a variable expressivity in females. It is a rare disease with calculated incidence of 1:40.000 for the classical variant. The skin harbors 1 cardinal symptom: angiokeratomas (AKs).
Dermatologic Manifestation
Angiokeratoma Corporis Diffusum
The term AKs describes a heterogenous group of lesions characterized by the presence of vascular hyperkeratotic papules. They are mainly divided into 2 groups: localized and generalized. 1
Localized AK includes AKs of Fordyce, AKs of Mibelli, solitary AK, naeviforme AK, 3 -5 and AK of the tongue. 6 These lesions show a distinct clinical appearance while sharing histopathologic findings described in Table 1.
Different Types of Angiokeratomas.
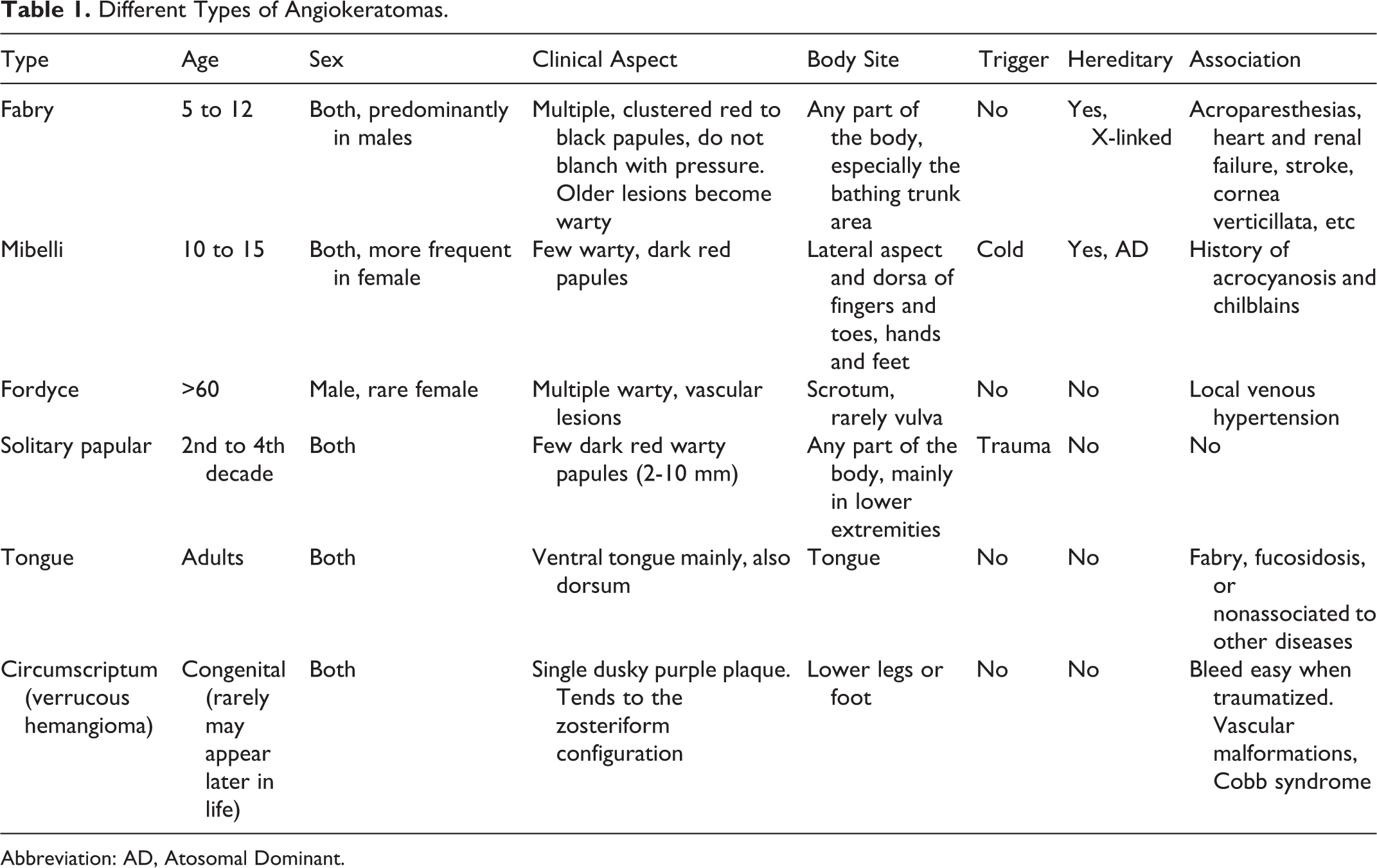
Abbreviation: AD, Atosomal Dominant.
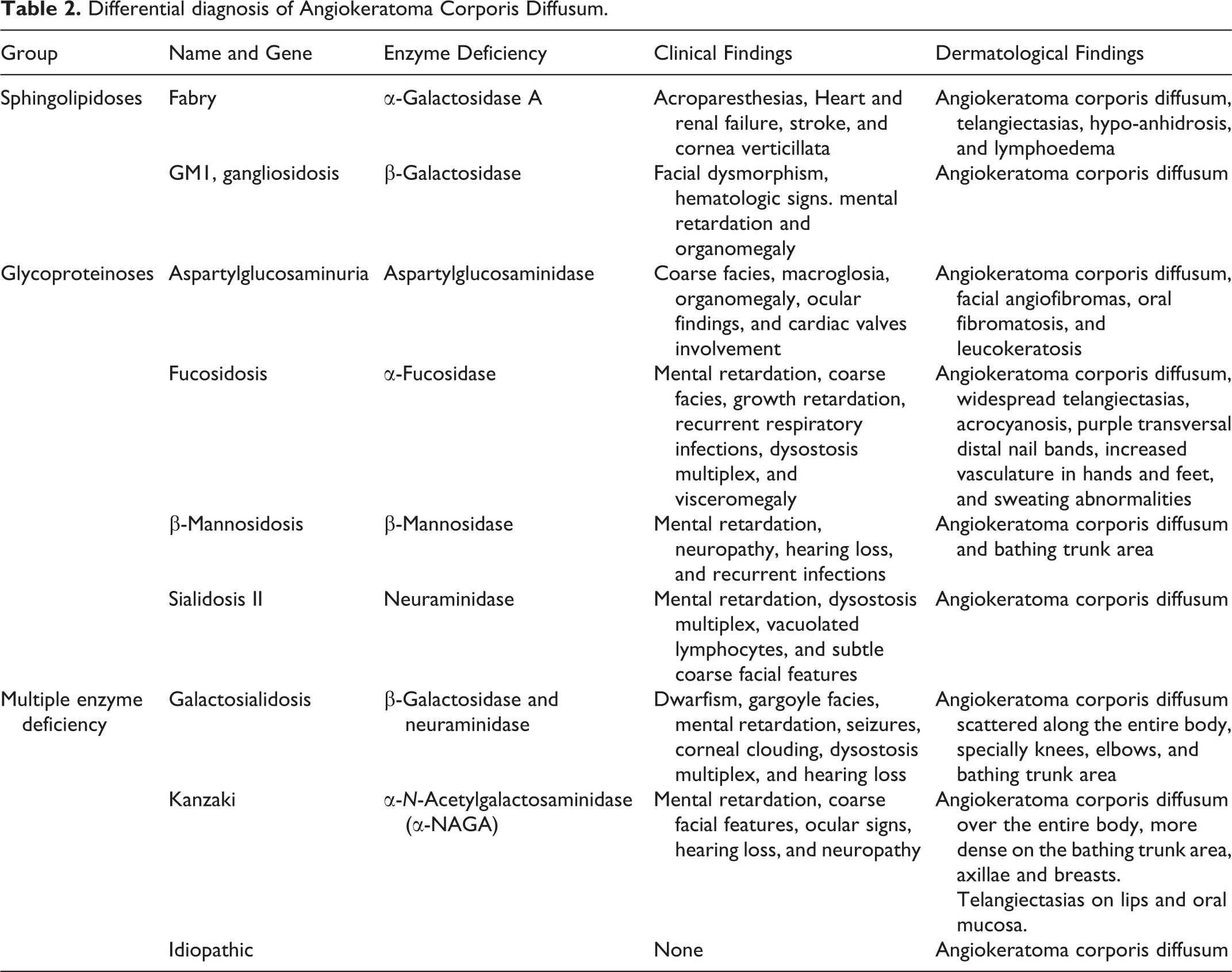
Diffuse AKs are characterized by the presence of multiple lesions that affect more than 1 area of the skin. Although any region of the skin can be affected, lesions usually localize to the bathing suit area (from the umbilicus to the upper thighs); this phenotype is known as ACD. This type of AKs, previously considered a synonym of FD, has also been described in several other lysosomal storage diseases 7 -11 (Table 2) and exceptionally in other systemic conditions. 12 -15 The rare occurrence of the ACD phenotype with no underlying diseases or metabolic alterations has also been described. This type is known as idiopathic ACD or “ACD with no known underlying enzyme alteration.” The occurrence of cases of idiopathic ACD with a familiar trait raises the issue that there might be an unknown underlying genetic disease. 16 -19
Differential diagnosis of Angiokeratoma Corporis Diffusum.
Angiokeratomas in FD are found in a high percentage of patients: 90% of males and 75% of females. 20 In hemizygous patients, lesions began to appear around the age of 5 to 8 years, although at that age, they usually go unnoticed or misdiagnosed, mostly when they are isolated (Figure 1). 21,22 Lesions usually appear as minute, isolated red to black papules that do not blanch with pressure. As disease progresses, they tend to group and turn more verrucous. The most characteristic localization is the bathing trunk area (gluteal, genital and periumbilical areas, lower abdomen, and upper part of the thighs; Figures 2 -4). 23 -25 Isolated lesions might also be found over the chest, hands and feet, axillae, extensor surface of the arms, elbows (Figure 5), and along the spine (suggesting trauma might act as a trigger in some areas, the Köebner phenomenon). 1 There seems not to be a correlation between the severity of the disease and the extension of the AKs, the mutation, or the amount of residual enzyme. 26
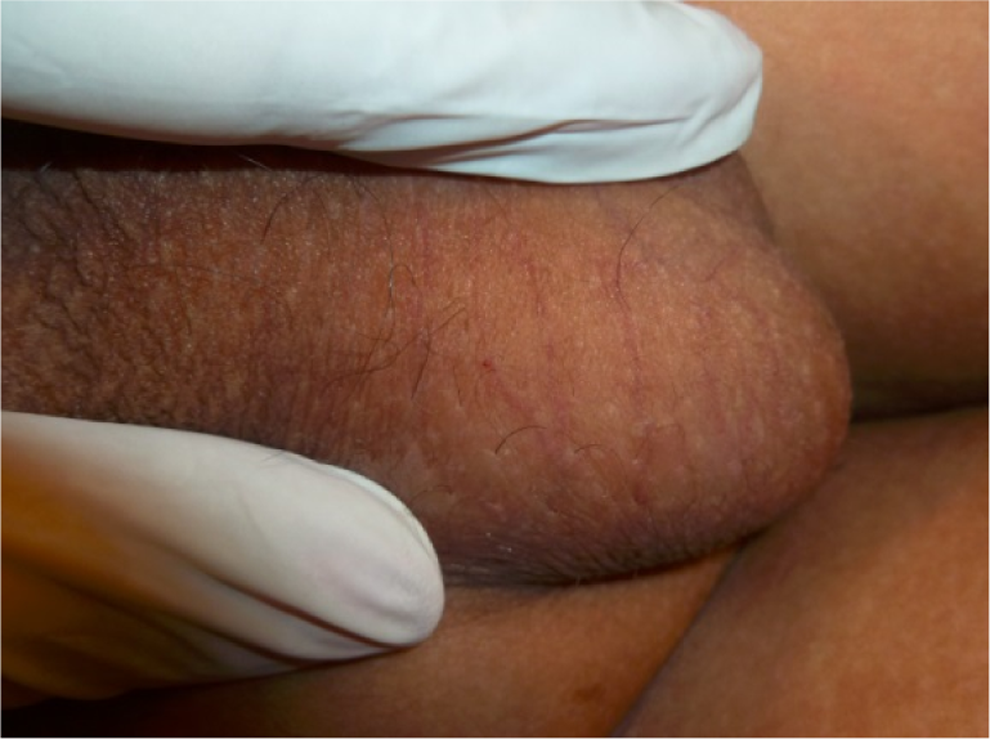
Few lesions over the scrotum of a young kid.
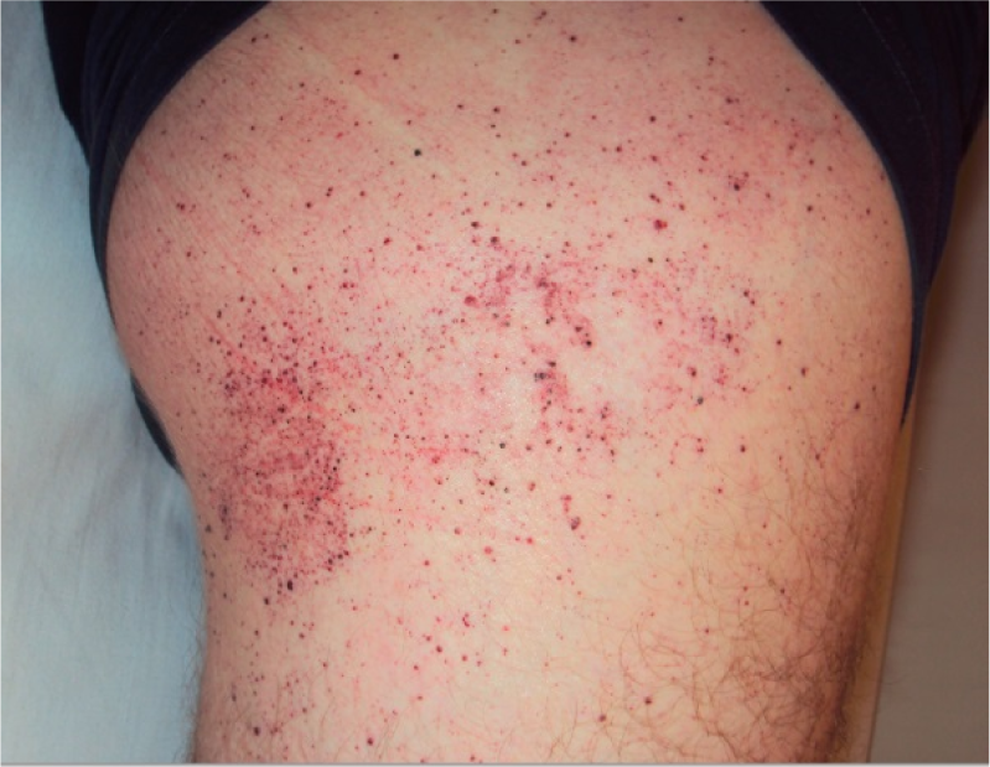
Lateral aspect of the thigh.
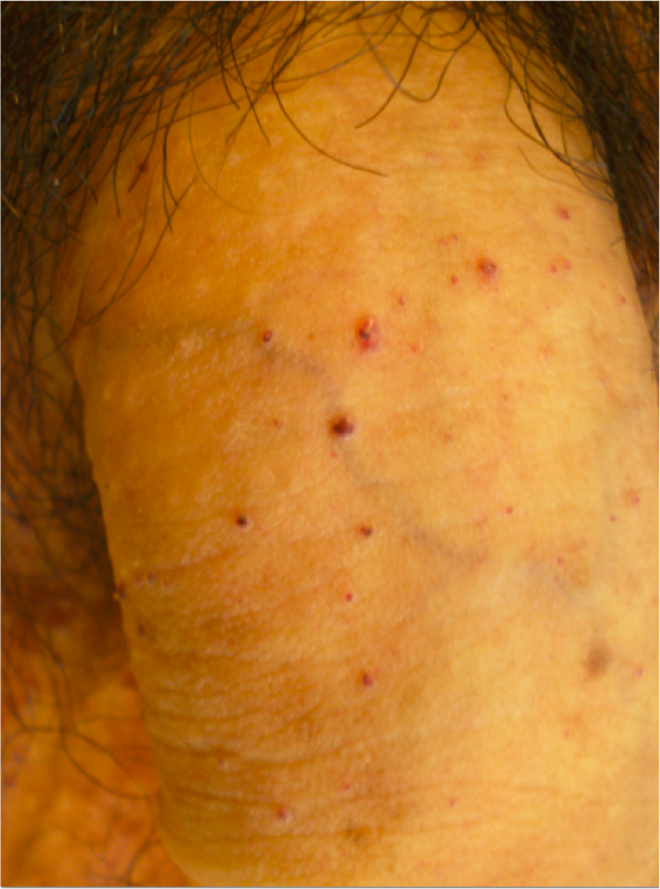
Few lesions over the penis of a severely affected patient.
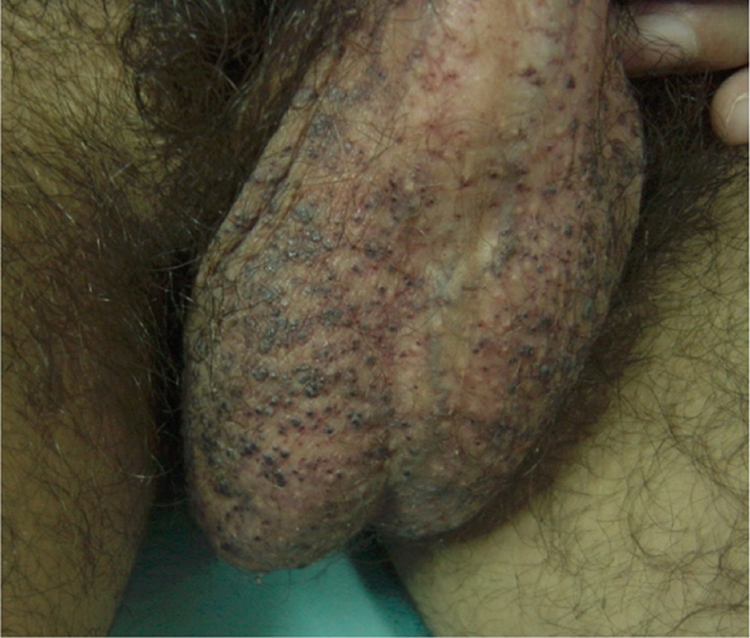
Widespread keratotic lesions over the scrotum.
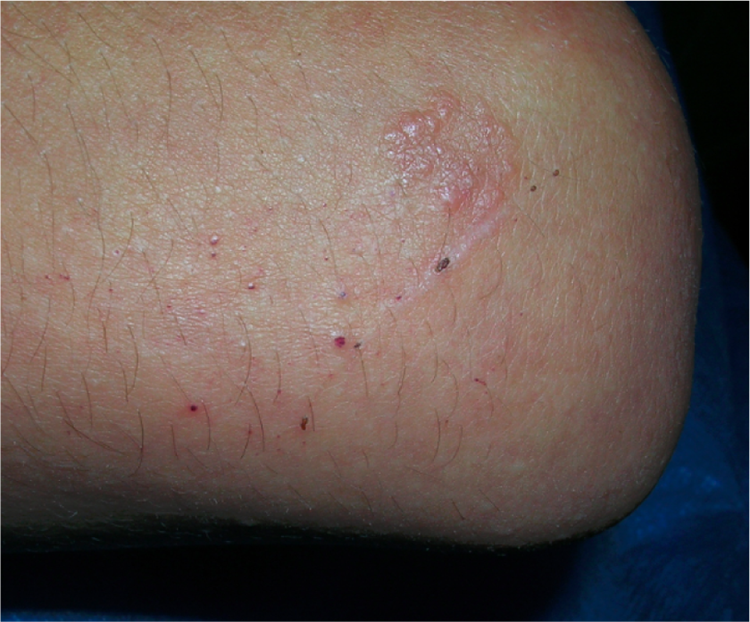
Lesions over the elbow (Köebner phenomenon).
Female patients show a great clinical heterogeneity; some may show a full-blown disease and AKs mainly in the bathing trunk area, such as male patients, whereas others show few scattered telangiectatic lesions. 27 Although the literature reports a low frequency of vulvar lesions, in our experience, they are not so infrequent but they might usually be subtle and easily missed (Figures 6 and 7). There are several differential diagnosis of AKs. 28 -30 When lesions are few with a highly verrucous component, they can be misinterpreted as viral warts. Their vascular origin of these lesions may be confused with petechiae, cherry angiomas, capillary aneurisms, pyogenic granulomas, eruptive angiomas, 31 or even Schonlein-Henoch purpura. 32 Dermoscopy might be useful to recognize AKs, showing a well-limited red to black lesion with grouped vascular lacunae and some hyperkeratosis. 33 From a practical point of view when assessing patients with multiple AKs, the umbilicus should always be evaluated for lesions inside the navel, given their presence is highly evocative of FD (Figure 8). On the other hand, genitals should be completely evaluated both in males and females. Lesions over the dorsum of the penis (not only over the scrotum) might be a sign that help differentiate from the most common and benign Fordyce AK. In females, vulvar AKs might be easily unnoticed, as they are usually asymptomatic and most patient’s lesions are quite subtle. Rare reports of male adults with few lesions, but with suggestive personal or family history, have been previously published, 34 raising the need to rule out FD even in patients with scattered cutaneous lesions in the correct clinical context. Under the light microscope, histopathologic findings are similar in all AKs, showing numerous dilated and congestive capillaries with thin walls in the papillary dermis underlying an epidermis that shows different degrees of acanthosis and orthokeratosis. 35 Due to technical issues, the recognition of the lysosomal deposits in these types of biopsies is very difficult. It is worth mentioning that not all the lesions show hyperkeratosis, with some biopsies only revealing vascular dilation, more similar to cherry angiomas or telangiectasias. 36 For these reasons, further evaluation should be performed when other clinically significant signs are present. Characteristic electron-dense concentric or lamellar (zebra-like) inclusion bodies (with alternating light- and dark-staining bands) are evident under the electron microscope. These inclusion bodies can also be recognized in clinically normal skin. 37,28 They are especially evident in the eccrine sweat glands.
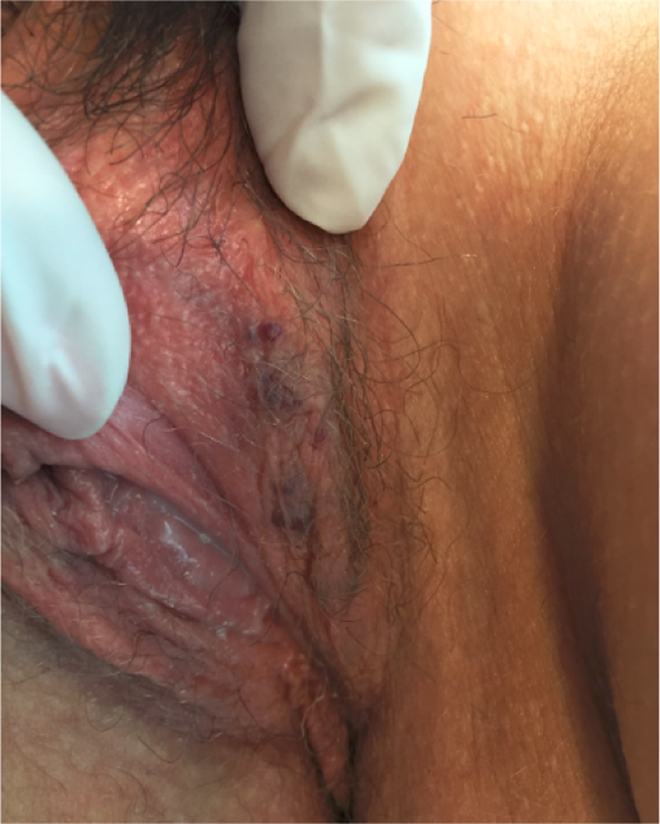
Multiple vulvar lesions.
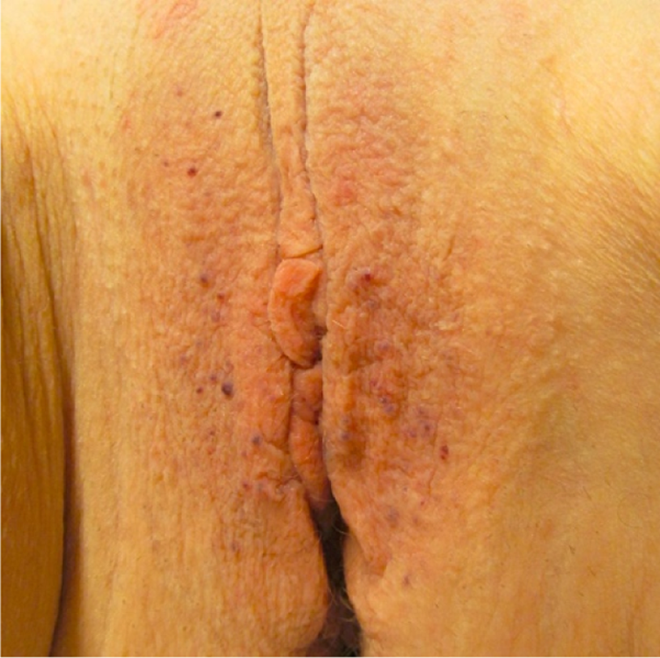
Few vulvar lesions.
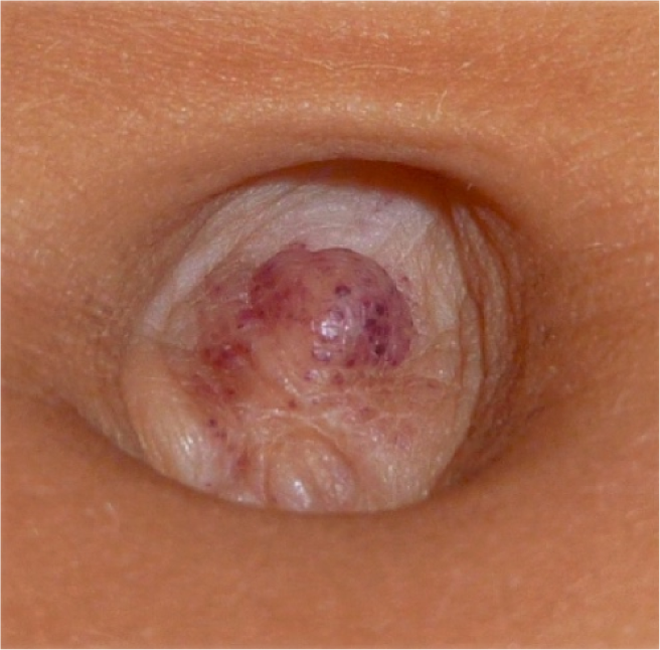
Umbilical papules.
Other Cutaneous Findings
Oral Manifestations
More than one-third of patients develop oral lesions. Angiokeratomas and telangiectasias can be found in the lips and intraorally, 38 specially in the anterior buccal mucosa. The tongue might also develop glossitis, fissures, and erythematous papillae. Xerostomia is a usual complain.
Raynaud Phenomenon
The presence of episodical color changes (pallor and cyanosis) on the acral extremities, mainly secondary to the exposure to cold and in the absence of lupus and scleroderma or antinuclear antibodies, has been recently described in up to 13% of patients with FD. Germain et al evaluated the presence of this symptom in 207 patients with FD reporting this phenomenon in 28 cases. This finding was noticed both in female and male patients and was independent of the mutation and the presence and amount of AKs, expanding the phenotype of vasculopathy observed in patients with FD. 39
Hypohidrosis or Anhidrosis
Hypohidrosis or anhidrosis is a frequent manifestation in hemizygous adults with FD (53%-93% of patients) and not so frequent in female patients (17%-28%). 40 -42 It usually starts early, during childhood or adolescence, 43 and leads to dry skin, heat intolerance, or fever of unknown origin, (due to the inability to sweat and eliminate heat transepidermically). The pathophysiology is thought to be due to the accumulation of nondegraded substances in the peripheric nerves and the endothelial deposits of the vessels surrounding the eccrine glands and the eccrine cells, as well as an abnormal autonomic nerve response.
Lymphedema
Lymphedema of the lower legs is another cutaneous finding in some patients with FD. It is thought to be due to the direct deposit of sphingolipids in lymphatic vessels with a fragmentation of the microlymphatic net (as demonstrated by Amann-Vesti et al by fluorescence microlymphography). 44
Hair Alterations
Hypotrichosis and sparse, fine facial hair have been typically described in patients with FD. It seems to be more accentuated in the lower legs. One report of “hard and thick scalp hair” failed to demonstrate the deposit of sphingolipids in the hair bulb, but suggested that the hair alterations could be due to the indirect effect of the microvessel disturbances and a secondary micronutrient deficiency. 45
Facial Features
Although facial dysmorphism is usually important in most lysosomal storage disorders, facial features in patients with FD have been historically considered unrevealing. 46 More recent evaluation of patients has allowed the recognition of certain minor facial abnormalities such as periorbital fullness, prominent lobules of the ears, bushy eyebrows, recessed forehead, pronounced nasal angle, generous nose/bulbous nasal tip, full lips, coarse features, and prognathism, among others, 47 in both male and female patients with FD.
Other Skin Findings in Histopathology
The skin is a very accessible organ where to perform a biopsy if we compare it with other sites such as the kidney or heart. Repeated skin biopsies performed in patients in 1 trial performed by Thurberg et al 48 allowed the assessment of enzyme replacement therapy (ERT) effects (agalsidase-β 1 mg/kg every 2 weeks) in the substrate clearance of the superficial capillary endothelium, showing an excellent response.
Diagnosis
A thorough discussion of the diagnostic methods of FD is beyond the scope of this article, but some points are worth mentioning. Definite diagnosis requires the demonstration of low α-Gal A activity in plasma, serum or leukocytes, and in dried blood spots on the filter paper. 27,49,50 As female patients have variable enzymatic activities, with a great amount of patients showing normal activity, the diagnosis should be confirmed with the detection of the pathogenic mutation. 51
Treatment
The many different debilitating symptoms of FD demand a multidisciplinary evaluation that involves the primary caregiver, as well as experienced nephrologists, cardiologists, dermatologists, and neurologists. 1,52 -54
A specific treatment (ERT) is available for eligible patients and has shown to be safe and effective. 55,56 It will be discussed in-depth elsewhere in this supplement.
The nonspecific treatment of cutaneous lesions includes different types of destructive measures such as cryotherapy, electrocoagulation, or excisional surgery. However, the treatment of choice is laser therapy (neodymium YAG, pulsed dye, KTP 532 nm, copper, argon, candela V, or beam laser). 1,57,58 It should be taken into account that lesions may continue appearing even under specific treatment in some patients, so a palliative measure should be offered when cutaneous manifestations show an impact in the quality of life.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
