Abstract
Background:
The Latarjet procedure may be performed arthroscopically or via an open approach, utilizing screws or suture buttons for graft fixation. There has been recent interest in suture button techniques in arthroscopic surgery, and proponents assert that these techniques may lead to fewer hardware-related complications while allowing for easier graft positioning.
Hypothesis/Purpose:
This study aimed to compare the complication and return to sports (RTS) rates between screw fixation (SF) and suture button fixation (SB) for patients undergoing the arthroscopic Latarjet procedure. It was hypothesized that each group would have similar outcomes.
Study Design:
Cohort study; Level of evidence, 3.
Methods:
A total of 112 patients underwent arthroscopic Latarjet procedures at a single center between January 2012 and December 2019. All patients had >20% glenoid bone loss, and 11.6% (n = 13) had previous arthroscopic Bankart repair. SF was utilized in 65 (58%) cases, and SB in 47 (42%) cases. Complications, reoperations, and RTS rates were analyzed. Patients were included for analysis if they had a 2-year follow-up and did not require conversion to open surgery.
Results:
Total complications were similar between SF and SB and occurred in 15.4% (n = 10) and 14.9% (n = 7) of cases, respectively (P = .943). Recurrent dislocation was noted in 3.1% (n = 2) of SF cases and 4.3% (n = 2) of SB cases (P = .740). Reoperations were required in 4.6% (n = 3) of the SF group and 4.3% (n = 2) of the SB group (P = .927). There were no hardware complications in the SB group compared with 1 hardware complication in the SF group. RTS was also similar between groups, with 92.3% and 93.6% returning to sports and 75.4% and 80.9% returning to the same level of sports in the SF and SB groups, respectively.
Conclusion:
Graft fixation using SF or SB yielded similar results for arthroscopic Latarjet procedures with respect to complications and RTS. The fixation method may be dictated by surgeon preference without an increased risk of complications.
Keywords
Shoulder instability is a common condition in young athletic populations, especially in patients who participate in contact sports.22,23 An osseous Bankart lesion—commonly observed in patients with anterior shoulder dislocation—is characterized by the detachment of the anteroinferior labrum along with a fracture of the glenoid rim. The glenoid defect may result from a bone fracture due to a primary injury or from bone erosion caused by repeated episodes of subluxations and dislocations.8,15 The literature has demonstrated that isolated soft tissue Bankart repairs have increased rates of failure when bony defects reach a certain threshold, although the exact level at which a bony procedure is indicated continues to be debated.16,24 The Latarjet procedure has yielded good results in populations with recurrent shoulder instability or in patients at high risk for recurrence.12,14 In addition to cases with substantial bone loss in either a primary or revision setting, the Latarjet procedure has also been used for primary stabilization for patients participating in contact sports, such as hockey or wrestling.10,13
The Latarjet procedure is performed via an osteotomy of the coracoid and fixation to the anterior glenoid rim. 19 This may be accomplished either arthroscopically or via an open approach. Arthroscopic surgery is technically complex, with a reported learning curve of between 30 and 50 cases with respect to bone bock positioning, surgical time, and complications.1,29 However, arthroscopic procedures provide possible benefits—including minimal invasiveness, less postoperative stiffness, early rehabilitation, and improved visualization—while allowing for concomitant treatment of pathologies if necessary. Traditionally, graft fixation has been achieved using screws directed from anterior to posterior through the graft and the glenoid, which has demonstrated good clinical outcomes. Screw-related complications, however, have been identified as a leading cause for revisions with this technique. 20 Recently, there has been increased interest in alternative methods of coracoid graft fixation, such as suture button devices. 5 Reported benefits of cortical fixation using suture buttons include improved bone block position and fewer hardware-related complications. 2 Biomechanical investigation, however, has suggested that suture buttons may not resist loads as effectively compared with screws for the Latarjet procedure, 32 but additional studies have found effective graft fixation with minimal migration and good osseous healing.25,31
Previous clinical studies have investigated the Latarjet procedure using a suture button fixation (SB) device and have found similar results to fixation with screws in terms of patient-reported outcomes, range of motion, graft incorporation, and complications.9,28 However, most of the current literature consists of retrospective case series of relatively small sample sizes. Few studies have directly compared fixation methods within an entirely arthroscopic cohort. This study aimed to compare complication rates and return to sports (RTS) between the arthroscopic Latarjet procedure with screw fixation (SF) and the arthroscopic Latarjet procedure with SB. We hypothesized that there would be similar complications and RTS rates between groups.
Methods
Study Design and Setting
This was a retrospective study of patients undergoing the arthroscopic Latarjet procedure. Approval was obtained from the Carthage Area Hospital Institutional Review Board. All patients undergoing an arthroscopic Latarjet procedure at a single center between January 2012 and December 2019 via an SB or the cortical suspension device technique (Endobutton; Smith & Nephew) were identified for possible inclusion. Arthroscopic SB was performed using the method initially described by Lafosse et al. 18 This procedure begins with an anterior capsulectomy and opening of the rotator interval. The anterior labrum and the middle glenohumeral ligament are resected. The lateral border of the conjoined is debrided to visualize the coracoid. While taking care to visualize and protect the musculocutaneous nerve, the inferior coracoid is debrided and prepared with a bur. Two drill holes are then made in the coracoid, and an osteotomy is performed 2 to 2.5 cm above the tip. The graft is passed through a split in the subscapularis tendon and positioned on the anterior rim of the glenoid, oriented with the conjoined tendon directed in an inferior trajectory. A guidewire is drilled anterior to posterior through the graft, and a 3.5-mm cannulated drill is used to place a 5-mm screw. A second 5-mm screw is placed using the same technique resulting in 1 superior screw and 1 inferior screw.
The arthroscopic Latarjet procedure with double SB was performed after the guided technique described by Boileau et al. 2 This procedure is performed similarly to the above description with respect to glenoid preparation, coracoid preparation, and coracoid osteotomy. Graft fixation is accomplished by passing 2 suture button devices from posterior to anterior to capture the graft. There is 1 superior suture button and 1 inferior, similar to screw orientation. Graft orientation is the same, and tensioning is done from the posterior aspect of the shoulder.
The procedures were performed using a trans-subscapularis split approach (Figure 1).

Trans-subscapularis split approach.
The 2 screws in the SF group were placed parallel to the glenoid surface (Figures 2 and 3). Two tight ropes transglenoid were used in the SB group (Figures 4 and 5).
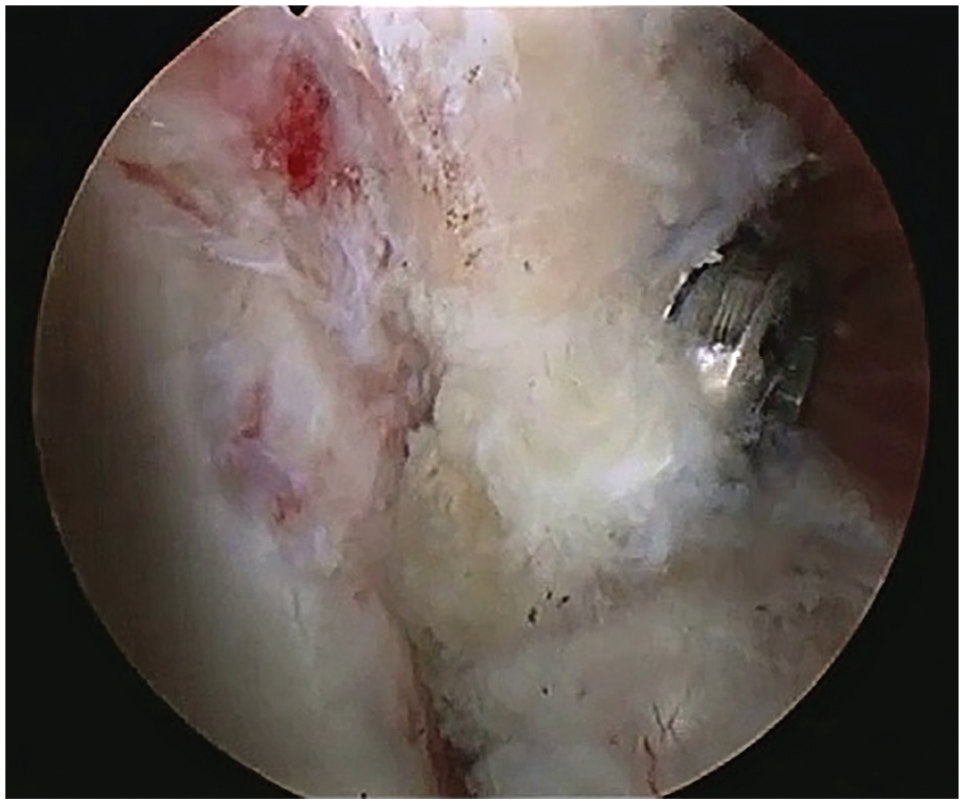
Screw fixation.

Postoperative computed tomography of screw fixation.

Suture fixation.

Postoperative computed tomography of suture button fixation.
All patients had an anterior glenoid bone loss of >20% based on a perfect circle measurement. 27 Intraoperatively, the amount of the bone block was verified to ensure it exceeded the size of the missing bone. The first 30 cases performed via each technique were excluded to account for a learning curve. Patients were included for analysis if they had a minimum 2-year follow-up. Procedures that were converted to open surgical techniques intraoperatively were excluded. Patient characteristics were recorded, as well as arthroscopic fixation type, complications, revisions, and information regarding return to athletic activity. Patients were grouped according to the fixation method as either the SF group or the SB group. SF was used at the beginning of the series before the primary surgeon switched to SB as the preferred method, but the technique was ultimately determined by surgeon preference. The switch was done due to concerns about implant prominence resulting in possible pain caused by screws and the preference for a lower profile implant. There were some theoretical concerns that screw irritation could lead to eventual arthritis. The suture button technique was seen as an alternative to potentially avoid this long-term complication.
Outcomes
The primary outcome was a comparison of complication rates between the SF and SB groups—including hardware failure, graft nonunion, recurrent instability, stiffness, infection, nerve injury, and the need for revision surgery. Secondary outcomes included a comparison of RTS rates, along with the level at which RTS occurred after surgery. All analyzed data were from the 2-year follow-up timepoint to avoid skewing the follow-up length between groups.
Statistical Analysis
All statistical analyses were performed using RStudio 2023 (Posit Software, PBC). Continuous variables were analyzed with Student t tests, while categorical variables were analyzed with the chi-square test or the Fisher exact test. Continuous data were reported as the mean and standard deviation. Categorical data were reported as n (%). Statistical significance was set at P < .05.
Results
Patient Population
During the study period, 185 patients underwent the arthroscopic Latarjet procedure by a single surgeon (G.M.). The first 30 patients in each group were considered to be the learning curve of each technique and thus excluded. Eleven cases were converted to open procedures and thus excluded. Two patients were lost to follow-up before the 2-year postoperative follow-up. Overall, 112 patients met the eligibility criteria for analysis (Figure 6). There were 65 (58%) in the SF group and 47 (42%) in the SB group. Age was similar between groups, with a mean of 32.4 ± 8.6 years for the SF group and 31.7 ± 11 years for the SB group (P = .713) (Table 1). Seven patients in the SF group and 6 in the SB group had undergone previous arthroscopic Bankart repair. Most cases were performed on the dominant shoulder in both groups. The mean bone loss was 23.4% in the SF group and 23.6% in the SB group.

Flowchart of patient inclusion.
Patient Characteristics a

Data are presented as means ± SD or n (%). SB, suture button fixation; SF, screw fixation.
Complications
Overall complication rates were similar between groups, with 15.4% of the SF and 14.9% of the SB groups experiencing a postoperative complication (P = .943). Individual complications also occurred at similar rates between groups (Table 2). Two patients in each group experienced a dislocation after surgery—a total of 4 patients with dislocation. Two dislocations occurred during sports, and 2 occurred as a result of falls. Of those with recurrent dislocation, both patients in the SB and 1 in the SF groups underwent additional surgical stabilization procedures due to recurrent instability. One patient in the SF and 2 patients in the SB group experienced transient musculocutaneous nerve injury, with all patients recovering fully without reoperation. Each of the following occurred once in the SF group: postoperative hematoma, deep infection, hardware complication, and graft fracture. The hardware complication was pain attributed to the screwhead position causing impingement with the humeral head due to the angle of screw insertion. Two patients in the SF group reported stiffness compared with 1 in the SB group. Two nonunion incidents occurred in the SB group and 1 in the SF group. Nonunion was defined as failure of graft union after 6 months. Two additional patients in the SF group underwent reoperations for deep infection and graft fracture.
Complications a

Data are presented as n (%). SB, suture button fixation; SF, screw fixation.
Return to Sports
Overall, 92.9% of patients were able to return to athletic activity after surgical stabilization. All sports were played at a recreational level, with the majority (two-thirds) being overhead sports and the rest (one-third) being collision sports. RTS rates were similar between groups, with 92.3% (60/65) and 93.6% (44/47) returning to sports in the SF and SB groups, respectively (P = .791). Of those patients treated with SF, 75.4% (49/65) reported that they returned to their preoperative level of activity compared with 80.9% (38/47) treated with SB (P = .493).
Discussion
Overall, the results of this study support our hypothesis. At a 2-year follow-up, complication and RTS rates were similar between the 2 fixation strategies, with no single technique demonstrating superiority. These findings suggest that surgeons may perform fixation via their preferred method without concern for increased complications.
While the original Latarjet procedure was first described in 1954, the arthroscopic Latarjet procedure was described by Lafosse et al 18 in 2007. In their preliminary report of 44 cases, the authors reported no complications related to neurovascular injury or infection. The authors did note, however, a profound learning curve but highlighted that once surgical comfort was achieved, surgical time reliably decreased and technical proficiency increased, allowing for reliable graft placement through a reproducible technique. In 2010, the same authors reported outcomes of 180 patients, noting high rates of patient satisfaction and RTS. 17 In their study, coracoid fixation was obtained using one or two 3.5-mm cannulated screws. Excellent satisfaction was reported by 80% of patients, with return to work occurring at a mean of 2 months and RTS at a mean of 10 weeks. With SF in this technique, a flush graft position was confirmed in 80% of patients. They reported early perioperative complications in 4 patients—including 2 hematomas, 1 transient musculocutaneous nerve palsy (recovered fully), and 1 intraoperative graft fracture. Late complications consisted of 4 graft nonunions and 3 cases of screw prominence. Of the nonunions, 2 occurred in patients who had a fixation with only 1 screw.
Boileau et al 3 initially described SB for the arthroscopic Latarjet procedure as an alternative to SF to reduce symptomatic hardware. They noted that a substantial proportion of Latarjet complications are due to SF and graft malpositioning. SB was developed to allow for a lower profile implant and optimization of graft positioning. Recent data have shown low rates of recurrence, a high rate of RTS, and little evidence of osteoarthritis at a 10-year follow-up after SB for the arthroscopic Latarjet procedure. 6 From the experience of the authors of the present study, the primary benefit of SB is the increased forgiveness with graft positioning and the lower profile implant, reducing the likelihood of symptomatic screw head position.
A recent systematic review by Hali et al 9 evaluated the current literature regarding screw versus SB for the Latarjet procedure. They identified 7 clinical studies that directly compared SB versus SF in a total of 1124 patients (SB, 279; SF, 845). Six of the studies reported complications, which occurred at a combined rate of 5.4% after SB and 10.2% after SF. The most common overall complication type was hardware-related, which occurred in 3.3% of SF cases but was not reported in any SB cases, similar to our study. In addition, a higher combined reoperation rate was observed in the SF group compared with the SB (5.1% vs 0.3%). This was primarily driven by the removal of hardware (17 out of 34 reoperations, 50%) and irrigation and debridement procedures for infection/hematoma (10 out of 34, 29.4%) in the SF group.
The current literature comparing SF to SB is limited by both a small overall sample size and heterogeneity. Of the publications included in the systematic review by Hali et al, 9 all studies utilized an arthroscopic approach for a subset of cases using SB. However, there is variability within the comparison groups of other studies, with only 2 studies directly comparing arthroscopic SF with arthroscopic SB and only a single study utilizing the Latarjet technique. Wang et al 30 compared 6 patients undergoing the arthroscopic Latarjet procedure with SF with 6 patients undergoing the arthroscopic Latarjet procedure with SB. At a mean 24.9-month follow-up (range, 13-55 months), they found comparable American Shoulder and Elbow Surgeons and Rowe scores along with a similar range of motion and union rates in both groups. They noted no severe complications in either group. Song et al 26 reported similar results on a group of 117 patients, comparing SF and SB for a modified inlay Bristow technique. They looked at 63 patients with SF and 54 with SB at a mean follow-up of 3.3 ± 0.7 years and found similar improvements in clinical outcome scores, RTS rates, range of motion, graft position, and reoperation rates. They found complication rates of 9.5% in the SF and 9.3% in the SB groups. Most complications (5 out of 6) in the SF group were directly related to hardware—including 2 intraoperative graft fractures, 2 breakages, and 1 case of screw pullout. There were no hardware complications in the SB group, and complications consisted of recurrent instability, postoperative hematoma, temporary hematoma, and 2 instances of transient musculocutaneous nerve palsy.
The largest study to date reporting on SF versus SB for coracoid fixation was published by Metais et al 21 in 2016 to primarily compare open versus arthroscopic Latarjet procedures. 21 They looked at 390 patients treated with a combination of open SF (n = 104), arthroscopic SF (n = 222), and arthroscopic SB (n = 64). Overall, they found similar results with respect to clinical outcomes, range of motion, and complication rates among the 3 groups. Recurrent instability was experienced by 1.9%, 0.9%, and 6.3% of patients in the open screw, arthroscopic screw, and arthroscopic SB groups, respectively—these rates are comparable with those of our study (SF, 3.1%; SB, 4.3%). Hardy et al 11 published the next largest series to date of patients comparing SF to SB for the Latarjet procedure—including comparisons of mini-open SF, arthroscopic SF, and arthroscopic SB. They looked at 236 patients with SF (52 mini-open, 184 arthroscopic) and 72 with SB at 3.4 ± 0.8 years. Clinical outcome scores were similar between groups, but there was a significantly higher instability recurrence rate in the SB group (8.3% vs 2.5%; P = .02), and there was no difference in rates between arthroscopic and mini-open SF. Interestingly, no patients in the SB group required reoperation despite the higher rate of recurrence. All reoperations occurred in the SF groups, with 14 patients (5.9%) requiring additional surgeries for hardware removal (n = 8), arthrolysis (n = 3), recurrent instability (n = 2), and hematoma irrigation (n = 1). As discussed above, the results of our study showed similar rates of recurrent instability between groups, and there were similar rates of reoperation between the SF and SB groups (4.6% vs 4.3%; P = .927).
Additional studies comparing SF with SB have compared the open Latarjet procedure with SF with arthroscopic SB. In a study of 39 patients, Bonnevialle et al 4 found similar short-term patient-reported outcome scores and no difference in graft position but found that SB had a smaller bone contact area and required a longer duration to achieve bone block fusion compared with SF. Their findings further indicate a learning curve for graft positioning in the arthroscopic Latarjet procedure, although they did not specifically identify any complications. Girard et al 7 looked at 50 patients, reporting a 27% complication rate with SF compared with 12.5% with SB, although this was not statistically significant. They experienced 4 cases of transient axillary nerve palsy in the SF group, with no nerve injuries in the SB group.
Overall, our study found similar rates of overall complications, at 15.4% and 14.9% for the SF and SB groups, respectively. Interestingly, there were fewer hardware complications within the present study cohort compared with previously published rates. In our study, only 1 hardware complication was identified (likely due to suboptimal screw position), which occurred in the SF group, although there were 3 overall instances of nonunion (1 in the SF group and 2 in the SB group). As in previous reports, we found a similarly low reoperation rate in between groups (SF, 3 of 65; SB, 2 of 47). Both reoperations in the SB group occurred due to recurrent dislocation, while the SF group had 1 reoperation each for recurrent dislocation, deep infection, and graft fracture.
As many patients with instability are athletes, particularly those with significant bone loss, RTS is a major consideration after stabilization procedures. Our study found that >90% of patients in both groups were able to RTS. Also, 75.4% of the SF group and 80.9% of the SB group were able to return to the preinjury level of sports, which was not statistically different. Girard et al 7 also found similar RTS rates at 1 year between SF and SB, at 87% and 86%, respectively. They found a lower return to the same level (61% and 50%), although these were not significantly different between groups. Boileau et al 3 reported RTS rates on 121 patients who underwent the arthroscopic Latarjet procedure with SB at a minimum 2-year follow-up, finding that 93% returned to sports and only 3% experienced recurrence. These rates are comparable with both the SF and SB groups from our study.
Limitations
Limitations of our study include the retrospective design and relatively small overall sample size, with a post-hoc power calculation of 3%. The single surgeon design may reduce generalizability. Furthermore, additional demographic information was not collected—including smoking status, recurrent vs primary instability, and the number of dislocations sustained. Postoperative computed tomography scans or magnetic resonance imaging were not routinely obtained to assess implant position and graft healing. Scores—including the Tegner Activity Scale, Rowe Score, Constant-Murley Shoulder Outcome Score, and Western Ontario Shoulder Instability Index—were not calculated because the primary purpose was to assess complications. Future studies should aim to incorporate and assess these parameters and should also analyze potential subscapularis insufficiencies after a trans-subscapularis split approach. Strengths include the high follow-up rate at 2 years (112 of 114 [98.2%]) and the direct comparison of SF and SB within a series of patients treated entirely arthroscopically. To our knowledge, this is the largest cohort to date reporting on complications and RTS while directly comparing SF with SB for the arthroscopic Latarjet procedure.
Conclusion
The findings of this study showed that the arthroscopic Latarjet procedure using SB resulted in similar complications and RTS rates compared with arthroscopic SF. RTS was achieved by >90% of patients in each group, while recurrence and the need for reoperation occurred in <5% for both groups. These findings demonstrate that both SF and SB are acceptable methods for the arthroscopic Latarjet procedure graft fixation.
Footnotes
Final revision submitted September 9, 2024; accepted October 9, 2024.
One or more of the authors has declared the following potential conflict of interest or source of funding: N.P. has received consulting fees from DePuy Synthes Products and Medical Device Business Services; J.P.S. has received hospitality payments from Stryker and Encore Medical. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Carthage Institutional Review Board (2023-7).
