Abstract
Background:
Reconstruction of the medial patellofemoral ligament (MPFL) with nonresorbable suture tape (FiberTape) could be an alternative to MPFL reconstruction (MPFLR) using an autologous tendon graft after a first-time patellar dislocation.
Purpose:
To investigate whether good clinical and radiological results are achievable with this technique.
Level of Evidence:
Case series; Level of evidence, 4.
Methods:
Between January 2017 and September 2020, a total of 30 patients with acute first-time patellar dislocation and a low anatomic risk factor constellation of patellar instability underwent MPFLR using nonresorbable suture tape combined with cartilage surgery if necessary. After a minimum 2-year follow-up, the Banff Patella Instability Instrument 2.0 (BPII 2.0)—a numerical analog scale (NAS, 0-10) for patellofemoral pain (PFP) (NAS pain) and subjective knee joint function (NAS function)—was used to assess patients’ reported quality of life after surgery in 20 patients (men/women: 14/6; age, 22.2 ± 6.1 years; 67% follow-up rate). Magnetic resonance imaging (MRI) scans of the surgically treated knee joint were conducted, and the Area Measurement And DEpth & Underlying Structures (AMADEUS) scores were evaluated pre- and postoperatively.
Results:
The BPII 2.0 score was 81 ± 12.5 (55.2-94.7) points postoperatively. The subjective rating of knee joint function (NAS function) was 8.5 ± 1.5 (4-10), and the PFP (NAS pain) was 1.5 ± 1.7 (0-5) postoperatively. MRI evaluations showed an increase in the AMADEUS score in all patients from 79 ± 24.3 points (40-100 points) preoperatively to 92.3 ± 9 points (75-100 points) postoperatively (P = .02).
Conclusion:
MPFLR with nonresorbable suture material can achieve satisfactory clinical and radiological outcomes after an acute first-time patellar dislocation.
Keywords
Nonoperative treatment of acute patellar first-time dislocation without osteochondral lesions was considered the method of choice for a long time. However, the observed risk of 60% to 70% of redislocation and unsatisfactory clinical-functional results have recently made this approach questionable.1,19,50,10,40,23 In addition, primary surgery might be indicated in the acute setting because of chondral or osteochondral flake fractures.13,38,15 Accordingly, an increasing trend toward surgical treatment of patellar first-time dislocation can be observed in the current literature. For surgical stabilization of the medial patellofemoral ligament (MPFL), which may be ruptured in up to >90% after the first-time patellar dislocation,30,31 MPFL reconstruction (MPFLR) using an autologous tendon graft (ie, quadriceps, gracilis, or semitendinosus tendons) is the current gold standard.25,33,51,27 Regarding tendon selection, no superiority of any of these grafts has been shown.27,41 However, harvesting these autologous tendon grafts can be technically challenging and may be associated with potential complaints.47,26,35,44 These disadvantages would not exist with the use of allografts, but the risk of disease transmission, lesser mechanical properties of the allograft, and higher costs are reported. 29 Therefore, MPFLR with a nonresorbable suture tape is becoming increasingly relevant in the available literature.52,53,28,32,22 Even though most of these publications are biomechanical evaluations or case series, 2 of them were able to show good clinical-functional results of MPFLR using nonresorbable suture tape after recurrent patellar instability.32,22
However, it remains unclear which clinical-functional and radiological results could be achieved after MPFLR using nonresorbable suture tape after an acute first-time patellar dislocation. The hypothesis was that MPFLR using nonabsorbable sutures would achieve good clinical-functional and radiologic outcomes.
Methods
This retrospective case series was approved by the local ethics committee (reference no. 2022-16567-andere Forschung erstvotierend). Since the implementation of MPFLR using nonresorbable suture tape (FiberTape [FT]; Arthrex) in our clinic between January 2017 and September 2020, a total of 30 patients who met the inclusion and exclusion criteria of this study underwent MPFLR, of whom 20 patients (67%; men/women: 14/6; age, 22.2 ± 6.1 years) completed the clinical and radiological follow-up examinations and were included in the study group.
The inclusion criteria were as follows: (1) acute first-time patellar dislocation with or without flake fracture; (2) no or 1 relevant pathoanatomic risk factor for patellar instability using the thresholds (see below lines 99-106) with Patellar Instability Severity (PIS) score 2 ≥3; and (3) at least a follow-up of 24 months.
The exclusion criteria were as follows: (1) age <14 years; (2) previous medial soft tissue-stabilizing and/or other bony procedures; (3) patellofemoral pain (PFP) without objective findings of lateral patellar instability; and (4) previous knee ligament surgical procedures.
The MPFLR technique using nonresorbable synthetic suture material (FT) was the same in all included patients (Figure 1). For this purpose, the FT was fixed at the patellar side implant-free through bony transpatellar tunnels and at the femoral side using suture anchors (BioComposite 4.75mm SwiveLock-anchor; Arthrex). The patient was placed in the supine position, with the operated leg fixed in the electric leg holder and a pneumatic tourniquet. A diagnostic arthroscopy using standardized anteromedial and anterolateral portals was performed on every patient. In cases of chondral or osteochondral traumatic flake fractures identified during diagnostic arthroscopy, which were considered suitable for refixation because of their size and quality, refixation was performed using nonresorbable headless compression screws (HCS) screws (Synthes). However, if the flake fracture could not be refixed because of its size and quality, stage-appropriate cartilage therapy was performed using debridement or microfracture.

Schematic illustration of the patella-side fixation of the FT without implants in the patella. After transpatellar drilling from the medial to lateral margin, the FT was passed through the patella, creating a triangular construct. FT, FiberTape; MPFL, medial patellofemoral ligament.
After a medial parapatellar skin incision at the medial patellar margin and blunt dissection through the subcutaneous tissue, the medial patellar margin was visualized. After parallel transpatellar drilling using two 2.0-mm K-wires from the medial to lateral margin on the proximal two-thirds of the patella at the midway of the patella, the FT was passed through the patella, creating a triangular construct, and passed to the femoral insertion between the second and third layers of the medial retinaculum to augment the injured MPFL as described by Milinkovic et al. 32 Then, after another skin incision and blunt dissection, the femoral tunnel was determined under a true-lateral fluoroscope according to Schöttle et al. 42 and created by overdrilling a K-wire placed at “Schöttle-Point” using a 4-mm cannulated drill. Finally, the FT was shuttled laterally through the femoral drill channel. After applying mild tension of approximately 2 N, the FT was temporarily fixed on the lateral side of the thigh using a clamp. Then, the isometricity of the FT was checked while the full range of motion and extension of the patella were checked for stability, allowing 2 quadrants of mediolateral translation. Finally, the FT was fixed with the suture anchor at approximately 60° of knee joint flexion after adequate tensioning with approximately 2 N, as previously described. 39
For all included patients, descriptive data were assessed using a clinical internal database. Preoperative magnetic resonance imaging (MRI) data and routine radiographs (standing long leg axis radiograph and lateral view radiograph of the knee joint [≤3 mm of overlap between the femoral condyles]) were evaluated in the context of this study. Torsion MRI scans were also evaluated if available. These are performed regularly with clinically important femoral or tibial torsional deformities. Radiological data were rated using predetermined thresholds and grading scales 51 : regarding the severity of trochlear dysplasia (absent, low grade [Dejour type A], or high grade [Dejour type B-D]), 11 only high-grade trochlea dysplasia was considered as a relevant risk factor; patellar height, with a Caton-Deschamps index of ≥1.3 was recorded as elevated 9 ; tibial tuberosity-trochlear groove distance, with ≥20 mm was considered elevated 2 ; tibial tuberosity-posterior cruciate ligament distance, with ≥24 mm was recorded as relevant 43 ; ≥4° valgus malalignment was considered elevated, 16 and >25° of antetorsion of the femur was considered elevated. 3 Furthermore, the cartilage status of the patellofemoral joint was assessed in the preoperative MRI scan (Figure 2) using the Area Measurement And DEpth & Underlying Structures (AMADEUS) score, 20 with the patellofemoral joint defined as previously published. 36 To assess patellar tracking in MRI scans, the patellar tilt (PT) according to Dejour et al, 12 the congruence angle (CA) according to Wolfe et al, 48 and the posterior patellar edge-trochlear groove ratio (PTR) according to Balcarek and Zimmermann 4 were evaluated.

(A) Typical constellation after acute patellar dislocation with knee joint effusion, contusion edema of the lateral femoral condyle, and a femoral rupture (arrow) of the MPFL is shown in the preoperative axial MRI image. (B) A sufficient restoration of the medial capsule and ligamentous structures in the area of the former MPFL rupture can be observed (arrow) 34 weeks after MPFLR with suture anchor fixation (circle). MPFL, medial patellofemoral ligament; MPFLR, medial patellofemoral ligament reconstruction; MRI, magnetic resonance imaging.
At least 24 months after MPFLR with FT, the patients included were reexamined for study reasons in an outpatient consultation in our clinic. As part of this evaluation, the validated Banff Patella Instability Instrument 2.0 (BPII 2.0) 5 was used to evaluate the patient-reported disease-specific quality of life for the current state. In addition, a numerical analog scale (NAS; 0-10 points) was used to evaluate the intensity of PFP (0 = no pain; 10 = most severe pain) and to evaluate subjective knee joint function (0 = severely restricted; 10 = normal function) for the current state. Moreover, MRI scans were performed for all patients with surgically treated knee joints (Figure 2). The image data obtained postoperatively were analyzed again regarding the pathoanatomic risk factors for patellar instability as described above. In addition, the AMADEUS score for the patellofemoral joint and the abovementioned parameters for the assessment of patella tracking were again determined in postoperative MRI scans in all patients. The evaluation of MRI scans was determined by mutual consensus of 2 investigators (1 senior resident, F.Z., and 1 consultant surgeon, S.Y.V.).
Statistical Analysis
Continuous data were assessed for normality with the Shapiro-Wilk test and graphically using histograms, quantile-quantile plots, and boxplots. They are presented as means and standard deviations (ranges). For a given normal distribution, the paired 2-tailed t test was used to assess the differences between the values. If the data were not normally distributed, the Wilcoxon signed ranks test was used. All analyses were performed using GraphPad Prism Version 9 (GraphPad Software). The significance level was set at P = .05. A post hoc power analysis was performed with G*Power Version 3.1.9.4.
Results
Patients’ characteristics and pathoanatomic risk factor profiles are presented in Table 1. A retropatellar flake fracture was observed and surgically treated in 10 patients (50%). The different procedures of cartilage surgery combined with MPFL-R are listed in Table 2.
Patients’ Characteristics, Pathoanatomic Risk Factor Profiles, and the Absolute and Relative Number of Flake Fractures a

Data are presented as mean ± SD or (range). Trochlear dysplasia was assessed according to the Dejour classification, and the patellar height was assessed according to the Caton-Deschamps Index. TT-PCL distance, tibial tuberosity-posterior cruciate ligament distance; TT-TG distance, tibial tuberosity-trochlear groove distance.
Overview of the Operative Procedures a
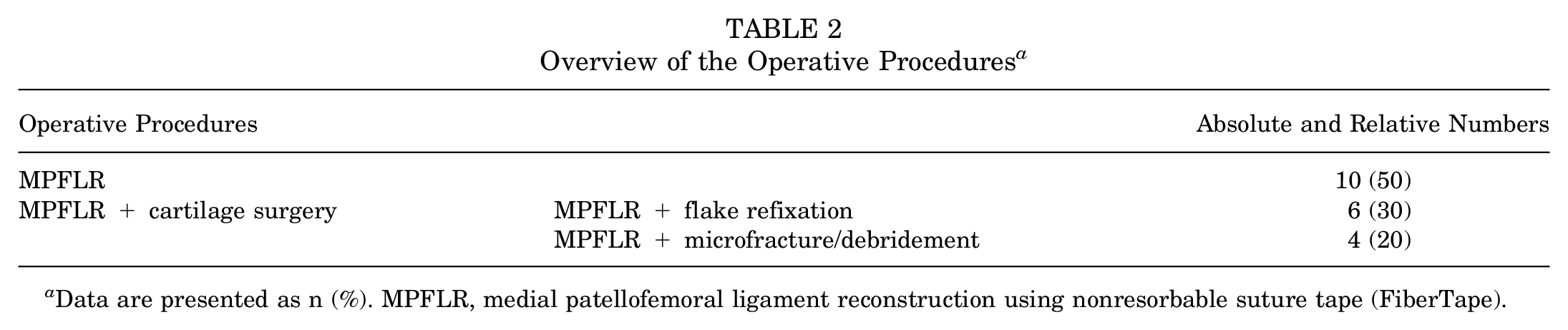
Data are presented as n (%). MPFLR, medial patellofemoral ligament reconstruction using nonresorbable suture tape (FiberTape).
Clinical and radiological evaluation was performed after a mean of 42.5 ± 14.6 months (range, 27-69 months)—the time from surgery to final follow-up. The BPII 2.0 score was 81 ± 12.5 points (range, 55.2-94.7 points) postoperatively. The subjective rating of knee joint function (NAS function) was 8.5 ± 1.5 points (range, 4-10 points), and that of PFP (NAS pain) was 1.5 ± 1.7 points (range, 0-5 points) postoperatively.
MRI evaluation (Figure 3) showed an increase in the AMADEUS score for the patellofemoral joint in the total cohort from 79 ± 24.3 points (40-100 points) preoperatively to 92.3 ± 9 points (75-100 points) postoperatively (P = .02). Moreover, in those patients who received MPFLR without cartilage surgery (n = 10 [50%]), the AMADEUS score decreased slightly without statistical significance from 99 ± 3.2 points (90-100 points) preoperatively to 95.5 ± 6 points (85-100 points) postoperatively (P = .102). In contrast, in those patients who received MPFLR concomitant cartilage surgery (n = 10 [50%]), the AMADEUS score increased significantly from 59 ± 18.5 points (40-100 points) preoperatively to 89 ± 10.5 points (75-100 points) postoperatively (P = .007). Moreover, from pre- to postoperative, patellar position improved, with a significant decrease in PT and CA from 18.4°± 4.7° and 31.2°± 20.3°, respectively, to 8.5°± 4.6° and 9.8°± 9.3°, respectively (P < .0001 and P < .001) and a significant increase in PTR from 0.84 ± 0.15 to 1 ± 0.1 (P < .0001). The patellar height—measured with the Caton-Deschamps index—showed no significant difference between before and after surgery (1.1 ± 0.1 to 1.0 ± 0.1) (P > .05) in all patients.

(A) The AMADEUS score in the total cohort before and after MPFLR (B-C) and in patients with and without cartilage surgery before and after MPFLR. (D) The congruence angle, (E) the posterior patellar edge-trochlear groove ratio (F) and the patellar tilt before and after MPFLR. *P < .05; **P < .01; ***P < .001; ****P < .0001. AMADEUS, Area Measurement And DEpth & Underlying Structures; MPFLR, medial patellofemoral ligament reconstruction.
At the final follow-up, no patellar redislocation occurred, and no patient reported patellar subluxations. Two patients (10%) had to undergo revision surgery. In both cases, the procedure involved hardware removal of HCS screws, which had previously been used for flake refixation in combination with arthroscopic arthrolysis. The reason for the removal of these HCS screws was that they overlapped the retropatellar cartilage surface. Arthrolysis was performed because of persistent knee joint flexion deficits. However, there was no clinical evidence of incompatibility, overtensioning, or foreign body reaction to the synthetic material used for MPFLR.
Discussion
The most important findings of this study on the outcome of MPFLR with FT after acute first-time patellar dislocation were that this treatment showed satisfactory functional outcomes of patients in terms of patient-reported outcome measures and patellar stability in two-thirds of patients who returned for the follow-up. Second, patellar tracking, which was evaluated in MRI scans using the PT, CA, and PTR, improved in all patients, and the patellofemoral cartilage status of patients with preoperatively intact cartilage conditions, which was measured using the AMADEUS score, was approximately the same at the follow-up. Consequently, the nonresorbable suture material used does not seem to have a negative influence on the cartilage status. Patients who received cartilage therapy because of a flake fracture showed significantly improved patellofemoral cartilage conditions measured using the AMADEUS score compared with their preoperative status. However, no significant difference was observed between the 2 subgroups.
The MPFL represents one of the decisive factors of patellofemoral joint stability, and its reconstruction (MFPLR) has become a cornerstone in the operative treatment of patients with recurrent patellar dislocation. 37 In recent years, because of the observed high risk of redislocation after nonoperative treatment,1,19,50,10,40,23 primary reconstruction of the torn MPFL has also been considered in patients with a high pathoanatomic risk factor constellation or with flake fractures after the first-time dislocation.14,18,49,25 In this study, MPFLR was performed in 50% of the patients due to flake fractures and in the other patients due to an increased risk of dislocation according to the PIS score. 2
Many different techniques with various autologous tendon grafts and a wide variety of fixation methods have been published to date and have shown favorable results.25,33,51,27 The influence on redislocation rates and clinical outcomes does not appear to differ depending on the type of graft fixation.41,27 Complaints associated with autologous tendon graft harvesting have been reported as potential complaints in studies reporting on the outcomes of autologous MPFLR techniques.44,35 However, donor-site morbidity has been reported as a possible complication in anterior cruciate ligament reconstruction using autologous tendons. These complaints include lesions to the saphenous nerve, donor-site tenderness, hematoma, extensor lag, and, in rare cases, muscle retraction and short-term loss of muscle function.7,24,45 Functional limitations of knee joint flexion within the first months after gracilis or semitendinosus tendon harvest have also been described in the current literature, even though these can be recovered by specific training. 8 Accordingly, MPFLR techniques using nonabsorbable sutures to avoid these risks of tendon harvesting could be interesting options. However, to our knowledge, only limited clinical and biomechanical data are available in the literature on MPFLR using FT. ‡
Two recent studies by Lee et al 22 and Milinkovic et al 32 have reported clinical outcomes for MPFLR using nonresorbable sutures.22,32 Lee et al compared the results after MPFLR using autologous tendon grafts with nonresorbable sutures at a 48-month follow-up. Regarding outcomes measured by the Kujala score, Bartlett score, Tegner Activity Rating Scale, Short Form 12 score, and Lysholm score, no significant difference was observed between the 2 groups. Accordingly, they concluded that MPFLR using FT is a safe and effective therapeutic alternative. 22
These results could be confirmed by Milinkovic et al. 32 They observed improvements in various patient-reported outcome measures after isolated MPFLR by FT in a mid-term follow-up. Furthermore, they found that MPFLR using nonresorbable suture tape in combination with bony correction procedures, such as deepening trochleoplasty and tibial tuberosity osteotomy, resulted in good clinical outcomes. 32
The results of our study also confirmed the achievement of satisfactory clinical-functional outcomes after isolated MPFLR in the presence of a mild anatomic risk factor constellation after acute first-time patellar dislocation in two-thirds of patients who returned for the follow-up.
In addition, to our knowledge, this study was the first to analyze MRI outcomes after MPFLR using nonresorbable suture material. The almost constant postoperative values of the AMADEUS score in those patients without preoperative flake fractures indicate that the higher stiffness of the FT compared with a tendon graft does not seem to have a negative influence on the cartilage status of the patellofemoral joint. Simultaneously, in patients with preoperative flake fractures, the patellofemoral cartilage conditions significantly improved as a result of the cartilage therapy performed. In addition, postoperative patellar tracking—assessed with the PT, CA, and posterior patellar PTR—was normalized in the follow-up MRI after MPFLR. The ability of MPFLR with a nonresorbable suture tape to normalize patellar maltracking in fresh-frozen human knee joint specimens in earlier degrees of knee joint flexion independent of the patella-side fixation technique has recently been demonstrated in a biomechanical study. 52
For daily clinical practice, it can be summarized that MPFLR with nonresorbable suture material could be a possible alternative to reconstruction with an autologous tendon graft after acute first-time patellar dislocation with satisfactory clinical and radiological outcomes. Based on the present data, a possible negative influence of the nonresorbable suture material used on the cartilage of the patellofemoral joint cannot be assumed.
Limitations
The results of this study must be interpreted in light of several limitations: (1) The overall number of included patients can be regarded as small, and the follow-up rate was relatively low at 67% (20 of 30 patients). Recurrent instability with just a couple of these patients who were lost to follow-up would change the conclusion of this study. (2) The limitations and potential bias characteristics of a retrospective study need to be considered. (3) Clinical-functional outcomes were assessed only with the BPII 2.0 and NAS, but these outcomes were not verified with clinical and/or functional testing. (4) The assessment of the cartilage status of the patellofemoral joint was performed with the AMADEUS score for better comparability of the values. Nevertheless, the limitations of the AMADEUS score must be considered limitations of the study. (5) The follow-up period was limited to a minimum 2-year postoperatively. This does not allow us to fully evaluate the long-term application potential, especially when considering that synthetic materials cannot be replaced by autologous tissue.
Conclusion
MPFLR with nonresorbable suture material can achieve satisfactory clinical and radiological outcomes after an acute first-time patellar dislocation.
Footnotes
Final revision submitted September 16, 2024; accepted October 7, 2024.
The authors have declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Landesaerztekammer Rheinland-Pfalz (reference No. 2022-16567-andere Forschung erstvotierend).
