Abstract
Background:
Acetabular labral tear morphology or orientation may influence hip stability.
Hypothesis:
A radial tear of the acetabular labrum would result in greater rotational and translational motion compared with a chondrolabral separation.
Study Design:
Controlled laboratory study.
Methods:
Included were 12 unpaired nonarthritic hip specimens, none of which had capsular laxity (8 male; mean age, 34.5 years). The specimens were stripped of all soft tissue except the hip capsule and labrum and, then potted using a custom jig. In 6 specimens, a 1-cm anterosuperior separation of the labrum from the acetabular rim (chondrolabral junction tear; CLJT) was created. In the other 6 specimens, a radial tear was created at the anterosuperior acetabulum. Subsequently, a complex labral tear was created in all specimens by adding a radial tear to the CLJT specimens and vice versa. The specimens were mounted on a load frame, and the femoral head displacement in the neutral and hyperextended positions was recorded at 5 N·m of internal/external rotation (IR/ER) torque and at 50 N of superior-inferior (S-I), anterior-posterior (A-P), and medial-lateral (M-L) force. Testing occurred at 0° extension and at maximal extension both before and after initial labral tear creation and again after creation of the complex labral tear. Before testing (intact state), the joint was vented to remove the effect of intra-articular pressure difference between the intact capsule and after capsulotomy for labral tear creation. The t test was used to calculate group differences by each range of motion measure (IR/ER and S-I, A-P, and M-L translations) for neutral and hyperextension.
Results:
Neither the radial labral injury nor the CLJT produced differences from the vented state in any combination of hip position or plane of motion. The complex labral tear showed increased IR/ER rotation at maximal hip extension. There was no difference between CLJT and radial labral tear in any combination of hip position or plane of motion.
Conclusion:
A simple labral tear did not affect hip joint stability when the capsule was intact, and no capsular laxity was present. A complex labral tear caused increased rotational laxity at maximal extension. Capsular laxity or a complex labral tear may be a prerequisite for labral injury to cause increased hip joint motion and/or translation.
Clinical Relevance:
Study findings suggest that labral tears in the absence of capsular laxity may not play a role in producing microinstability by increasing motion or translation.
Nonarthritic atraumatic hip pain is prevalent and frequently leads patients to seek musculoskeletal care. The differential diagnosis for hip pain is broad and includes labral tears among other diagnoses, both intra- and extra-articular. Hip labral pathology is prevalent among patients with and without hip pain and is a frequent source of referral to orthopaedic clinics. 3 Patients with labral tears of uncertain significance frequently undergo comprehensive workup with multiple physician visits, advanced imaging, and referrals for physical therapy as well as consideration for intra-articular injections or surgical treatment, generating a significant expense to the patient and the health care system.
Consensus about the evaluation and management of labral tears continues to be refined. The surgical treatment of hip pathology, in general, and labral tears, more specifically, has advanced significantly over the past 2 decades as new techniques, equipment, and implants have been introduced. However, the indications for these techniques continue to evolve and remain controversial as there is disagreement about the relative roles and contributions of the many soft tissue structures about the hip.
Recent recognition of hip microinstability—pathologic femoral head motion without dislocation—as a source of symptomatic hip pain in patients with otherwise normal anatomy has prompted biomechanical and clinical studies examining the role of the hip joint capsule, labrum, ligamentum teres, and hip musculature.1,4,17 Despite this significant research interest in hip microinstability, there is a lack of knowledge regarding the role of labral hip tears in pathologic motion.
The acetabular labrum is a fibrocartilaginous structure at the rim of the acetabulum with several purported roles in hip function, including suction seal and fluid mechanics, deepening the hip socket, and supporting load from joint reactive forces. 18 Histological studies demonstrate that the labrum derives its structural properties from bundles of collagen fibers arranged in radial and longitudinal orientations. The relative contributions of the fibers in each orientation have not been studied.
This study was designed to evaluate the contribution of the hip labrum radial and longitudinal fibers to hip joint motion in a cadaveric model. We evaluated different labral hip tear patterns by dividing the radial fibers (chondrolabral junction tear; CLJT) and longitudinal fibers (radial tear) and testing their effects on hip motion. We hypothesized that radial tears would lead to more motion than CLJTs.
Methods
A total of 13 unpaired nonarthritic hip specimens were studied. Specimens were isolated from 13 fresh-frozen cadaveric pelvi with full femurs (8 male, 5 female; mean age, 34.5 years [range, 18-50 years]). An age cutoff of <50 years at the time of death was used to best represent the standard clinical hip arthroscopy population. 13 Specimens were obtained from commercial, licensed, third-party organizations. Only donors without a history of hip surgery or arthritis were included in the study.
Specimen screening, preparation, alignment, and potting were performed using a previously published protocol that included screening radiographs to rule out arthritis and femoroacetabular impingement. 5 Anteroposterior pelvic radiographs were evaluated to screen hips with dysplasia or borderline dysplasia (lateral center-edge angle <25°) to exclude specimens with capsular laxity. Specimens consisting of the pelvis and bilateral femurs were stripped of all soft tissue except the hip capsule and labrum, aligned using a custom jig and potted in cement for mounting on the testing apparatus (Figure 1). 6 We used a previously described protocol to align the mechanical axis of the femur at 0° of hip extension and to determine the maximal hip extension for each specimen. 5 A materials testing system (Instron) and motion tracking system (3D Creator; Boulder Innovation Group) were used for data collection, with an estimated margin of error of 0.1 mm and 0.1°, respectively (root mean square error).
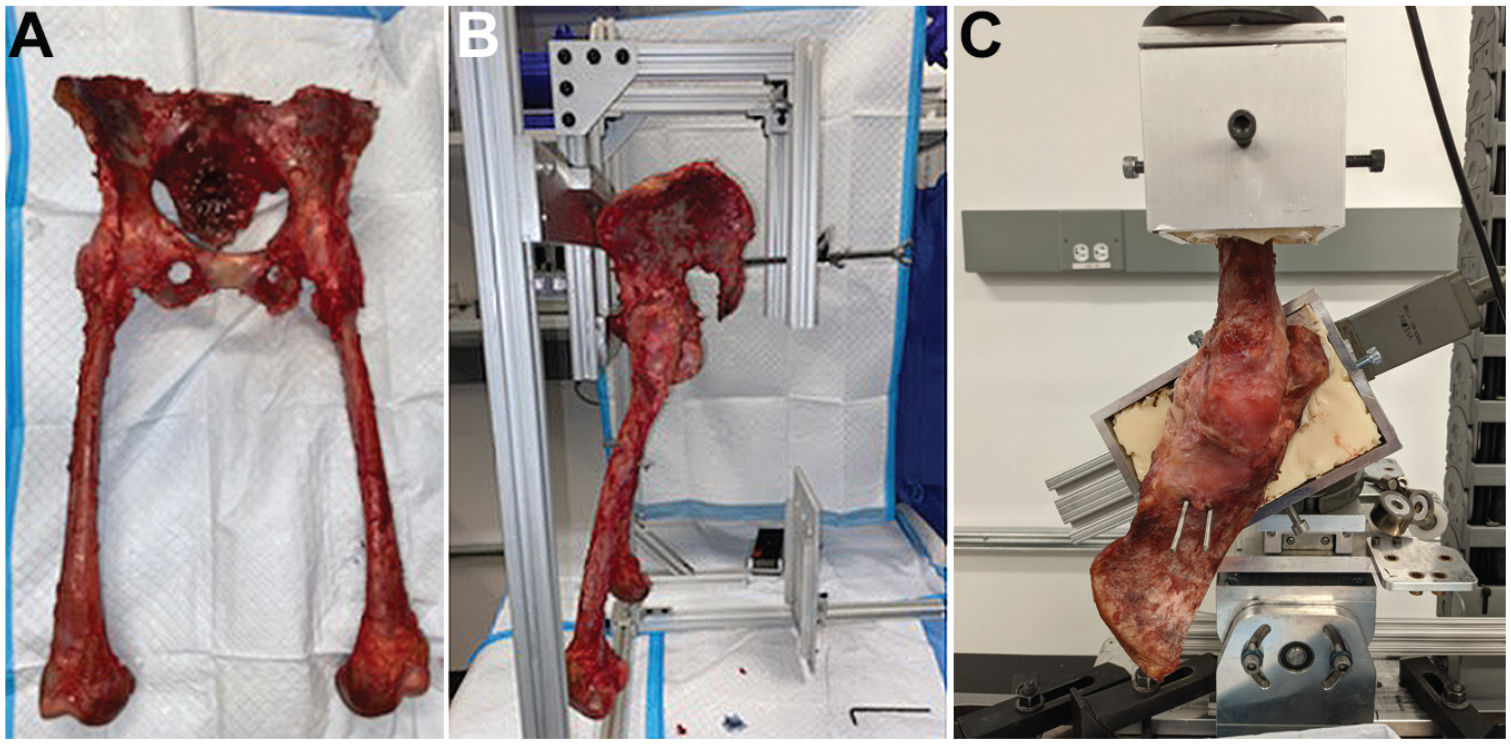
Specimen preparation, alignment, potting, and testing. (A) Pelvis and bilateral femurs were stripped of soft tissue, except the bilateral hip capsule. (B) Specimen aligned in the coronal plane on the mounting jig using the bilateral anterior superior iliac spine and pubic symphysis as reference points. (C) After alignment, the specimen was potted in cement and mounted onto the materials testing system.
Specimens were mounted onto the materials testing system, and the capsule was vented with an 18-gauge spinal needle to remove the effect of negative intra-articular pressure on joint motion. This was necessary to compare the specimens before and after creation of the labral tear states that required the creation and repair of a small capsulotomy to access the labrum. The spinal needle was introduced while a 100-N distracting and 50-N lateralizing force was applied to the femur. Venting was confirmed by noting a release in the amount distractive force displayed on the materials testing system.
After venting, baseline hip internal-external rotation (IR/ER) range of motion and femoral head translation in the superior-inferior (S-I), anterior-posterior (A-P), and medial-lateral (M-L) planes were recorded with the hip at 0° of extension as well as with the hip at maximal extension. IR/ER and femoral head motion were recorded in the anatomic neutral rotational plan of the acetabulum with the femur at 0° of extension as well as maximal extension. Specimens were randomized to undergo a radial labral tear or a CLJT.
The labral injury states were created at the most superior-lateral portion of the acetabulum between the 1-o’clock and 12-o’clock positions on the acetabulum. This position was chosen to most closely mimic the position of common labral pathology treated with hip arthroscopy.7,8,20 A 1- to 2-cm longitudinal capsular incision was made at the chondrolabral junction just lateral to the iliofemoral ligament to expose the labrum. Specimens randomized to simulate a radial labral tear received a complete radial incision of the longitudinal fibers of the labrum at the superior-lateral position between 1- and 12-o’clock. Specimens randomized to CLJT received a 1-cm chondrolabral separation between 1- and 12-o’clock. After initial testing, the complex labral tear state was created by making a radial tear centered in the chondrolabral separation or making a chondrolabral separation centered on the radial tear of respective specimens. The capsule was closed without imbrication with interrupted No. 3-0 Nylon suture for testing.
Data were collected for each hip specimen after venting, after creation of a radial tear or a chondrolabral separation depending on the arm of the study, and after creation of a complex labral tear. For each injury state, we recorded IR/ER and femoral head translations in the S-I, A-P, and M-L planes with the hip at 0° of extension and maximal extension. 5
For mechanical testing, a constant axial force of 10 N was applied to seat and center the femoral head in the acetabulum. Rotation was tested with a rotational torque of 5 N·m, and translation loads were applied with loads of 50 N in each plane using pulleys. 5 The McKibbin index 11 was calculated for each specimen by combining the femoral and acetabular versions. Both the femoral and acetabular versions were calculated using the motion capture data and geometric modeling. 5
As this was an exploratory study, a power analysis was not completed, and sample sizes were determined based on previous cadaveric studies.2,5 Means with standard deviations were calculated for each group, and t tests were used to examine the differences between groups by each range of motion measure (IR/ER and S-I, A-P, and M-L translations), separately for neutral and hyperextension. Four sets of tests were conducted: (1) CLJT versus vented controls; (2) radial tear versus vented controls; (3) CLJT versus radial tear; and (4) combined tear versus vented controls. Significance was set at P < .05. All analyses were conducted using R (Version 4.1.3), 14 RStudio (Version 2022.02.0), 16 and the psych package (Version 2.2.3). 15
Results
By convention, motion and rotation were reported as net motion along the axis of loading with respect to the pelvis.
Intact Labrum State Versus Vented Intact Labrum State
There were no differences between vented and nonvented groups regarding rotation or translation in either the neutral or the maximal extension hip positions.
Radial Tear Versus Vented Intact Labrum State
With the hip in neutral position, the radial tear state showed a mean increase in IR/ER of 3.75°± 4.97° compared to the vented intact labrum state (P = .533) (Table 1). Radial tear resulted in a mean increase in femoral head motion of 0.77 ± 1.09 mm in the S-I plane (P = .260), 0.54 ± 1.28 mm in the A-P plane (P = .447), and 0.91 ± 0.86 mm in the M-L plane (P = .138) (Table 1).
Vented State vs Radial Tear a

Values are expressed as mean ± SD unless otherwise indicated.
95% CI for the difference between the capsule vented state and radial tear.
With the hip at maximal extension, the radial tear state showed a mean increase in IR/ER of 2.66°± 2.81° (P = .249), a mean increase in distraction of 0.09 ± 0.21 mm in the S-I plane (P = .742), a mean decrease in femoral head motion of 0.02 ± 0.36 mm in the A-P plane (P = .456), and a mean increase in femoral head motion of 0.08 ± 0.62 mm in the M-L plane (P = .359) relative to the vented intact state (Table 1).
CLJT Versus Vented Intact Labrum State
In the neutral hip position, the chondrolabral separation state showed a mean increase in IR/ER of 2.26°± 1.92° compared to the vented intact labrum state (P = .938) (Table 2). CLJT resulted in a mean increase in femoral head motion of 0.35 ± 0.47 mm in the S-I plane (P = .243), 0.13 ± 0.21 mm in the A-P plane (P = .796), and 1.53 ± 1.53 mm in the M-L plane (P = .140) (Table 2).
Vented State vs CLJT a

Values are expressed as mean ± SD unless otherwise indicated. CLJT, chondrolabral junction tear.
95% CI for the difference between the capsule vented state and CLJT.
With the hip at maximal extension, the chondrolabral separation state showed a mean increase in IR/ER of 3.32°± 2.54° relative to the vented intact labrum state (P = .075) (Table 2). CLJT resulted in a mean increase in femoral head motion of 0.08 ± 0.49 mm in the S-I plane (P = .770), 0.02 ± 0.15 mm in the A-P plane (P = .915), and 0.11 ± 0.64 mm in the M-L plane (p = 0.793) (Table 2).
Complex Labral Tear Versus Vented Intact Labrum State
In the neutral position, the complex labral tear state showed a mean increase in IR/ER of 3.85°± 3.86° compared to the vented intact labrum state (P = .111) (Table 3). A complex labral tear resulted in a mean increase in femoral head motion of 0.56 ± 0.59 mm in the S-I plane (P = .258), 0.43 ± 0.79 mm in the A-P plane (P = .214), and 1.13 ± 1.39 mm in the M-L plane (P = .065) (Table 3).
Vented State vs Complex Degenerative Labral Tear a

Values are expressed as mean ± SD unless otherwise indicated. Boldface P value indicates a statistically significant difference between groups (P < .05).
95% CI for the difference between the capsule vented state and complex labral tear.
With the hip at maximal extension, the complex labral tear state showed a mean increase in IR/ER of 3.17°± 2.66° relative to the vented intact labrum state (P = .015) (Table 3). A complex labral tear resulted in a mean decrease in femoral head motion of 0.23 ± 1.15 mm in the S-I plane (P = .388), a mean increase in motion of 0.08 ± 0.34 mm in the A-P plane (P = .084), and a mean increase in motion of 0.18 ± 0.64 mm in the M-L plane (P = .369) (Table 3).
Radial Tear Versus Chondrolabral Separation
In the neutral position relative to CLJT, a radial labral tear resulted in a mean increase in IR/ER of 1.49° (P = .517) (Table 4). Radial labral tear resulted in increased femoral head motion of 0.20 mm in the S-I plane (P = .717), increased motion of 0.31 mm in the A-P plane (P = .593), and decreased motion of 0.45 mm in the M-L plane (P = .529) compared to the chondrolabral separation (Table 4).
CLJT vs Radial Tear a

Values are expressed as mean ± SD unless otherwise indicated. CLJT, chondrolabral junction tear.
95% CI for the difference between CLJT and radial tear.
At maximal hip extension, relative to chondrolabral separation, the radial labral tear state resulted in decreased IR/ER by 0.66° (P = .678) (Table 4). Radial labral tear resulted in increased femoral head motion of 0.05 mm in the S-I plane (P = .795), decreased motion of 0.08 mm in the A-P plane (P = .652), and decreased motion of 0.03 mm in the M-L plane (P = .937) compared to the chondrolabral separation (Table 4).
Discussion
Our study was designed to test if the individual radial or longitudinal components of the combined tear showed different patterns of increased femoral head motion. Based on our results, it appears in the absence of other pathology, that simple labral tear patterns do not lead to a clear pattern of increased hip motion. In fact, only the combined labral tear pattern showed statistically increased motion over controls and only in IR/ER.
To the best of our knowledge, this is one of few studies to differentiate and compare labral tear morphology as it relates to hip motion. The proposed biomechanical functions of the labrum, including increasing joint surface contact area and the suction seal effect, would be expected to rely differentially on the longitudinal or radial fibers as well as the height of the labrum and so different tear patterns may lead to different patterns of increased hip motion.9,10,12,21,22 Lertwanich et al 9 established that a 1-cm resection at the anterosuperios labrum leads to increased hip joint motion. Storaci et al 22 showed a correlation between labral height and the stabilizing effect of the hip labral suction seal. Nepple et al 12 showed that labral repair or reconstruction improves stability of the hip joint. Smith et al 21 used a cadaveric model to show that labral tears did not increase labral strain; however, a joint compression model may emphasize the contributions of bony constraints over soft tissue stabilizers. Previous work by Johannsen et al 6 has shown that degenerative labral tears significantly increase femoral head motion compared to hips with an intact labrum. In that experiment, the degenerative labral tear model was created with a combined radial tear and a CLJT at the anterosuperior position. Our study directly compared radial tears, CLJTs, and combined tears and their effects on hip motion. However, the fact that the radial tear did not increase femoral head motion more than the CLJT, despite interrupting the radial fibers, may be due to the circumferential attachment of the labrum to the acetabular rim. Based on our data, an isolated hip labral tear in the absence of other pathology would not be expected to affect hip joint instability. However, it remains possible that simple tear patterns in combination with associated pathology, such as capsular laxity, adult hip dysplasia, or femoroacetabular impingement, could lead to increased hip motion. Further studies are needed to determine the level of femoral head translation that is clinically relevant in patients with symptomatic hip microinstability.
Limitations
There are important limitations to this study to consider. The effect of venting the hip capsule was not expressly studied in this study despite it influencing hip constraint. 5 However, we felt that it was necessary to use the vented capsule state to compare it to subsequent labral deficient states. To create the labral tear states, it was necessary to create a small (1-2 cm) capsulotomy. Care was taken to make the capsulotomy small and avoid transection of the iliofemoral ligament, but this remains a potential confounding variable. Our model examined a relatively small (1 cm) CLJT, and it is possible that larger tears would cause greater instability. No cases of capsulotomy repair failure were seen. Testing was performed with the hip in 0° of extension and in maximal hip extension, as in previous studies.5,6 However, it is possible that different results would be obtained with additional testing in midextension or possibly flexion. However, flexion of the hip tends to load the posterior labrum more and the anterior labrum less. 19
Another limitation is that the study was conducted in cadavers. The contributions of the hip labrum and the effects of the bony geometry, capsular ligaments, ligamentum teres, tendons, and muscles have yet to be characterized. Further, it is unknown what relative or absolute thresholds of femoral head motion constitute pathologic motion and symptomatic hip microinstability, and it is possible that statistically significant changes shown in cadaveric models would not be clinically significant in vivo. However, given the lack of reliable in vivo data on the topic, well-designed cadaveric studies and models are needed to test and validate biomechanical theories.
Conclusion
In this study, we found no evidence that simple labral tears, either radial (and thus disrupting the circumferential fibers) or chondrolabral junction separations of 1 cm, affect hip joint stability when the capsule is intact and no capsular laxity is present. Complex labral tear did cause increased rotational laxity at maximal extension. Capsular laxity or a complex labral tear may be prerequisite for labral injury to cause increased hip joint motion and/or translation.
Footnotes
Final revision submitted January 30, 2024; accepted February 13, 2024.
One or more of the authors has declared the following potential conflict of interest or source of funding: M.R.S. has received grant/research support from Smith & Nephew; consulting fees from Medacta, Anika Therapeutics, and Smith & Nephew; nonconsulting fees from Smith & Nephew; honoraria from Medacta and Smith & Nephew; and royalties from DJO, Stryker, Smith & Nephew, Top Shelf, Vive, Subchondral Solutions, Marrow Access Technologies, Elsevier, and Lippincott. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval was not sought for the present study.
