Abstract
Background:
Recent studies have shown that legislation regulating opioid prescriptions in the United States has been successful in reducing the morphine milligram equivalent (MME) prescribed after certain orthopaedic procedures.
Purpose:
To (1) determine the effect of Ohio’s legislation limiting opioid prescriptions after shoulder arthroscopy and (2) identify risk factors associated with prolonged opioid use and increased postoperative opioid dosing.
Study Design:
Cohort study; Level of evidence, 3.
Methods:
We reviewed the data of patients who underwent shoulder arthroscopy between January 1, 2016, and March 31, 2020. Patients were classified according to the date of legislation passage (August 31, 2017) as before legislation (PRE) or on/after legislation (POST). Patients were also classified based on the number of opioid prescriptions filled within 30 days of surgery as opioid-tolerant (at least 1 prescription) or opioid-naïve (zero prescriptions). We recorded patient characteristics, medical comorbidities, and surgical details, as well as the number of opioid prescriptions, MME per prescription from 30 days preoperatively to 90 days postoperatively, and the number of gamma-aminobutyric acid (GABA) analogues and benzodiazepine prescriptions from 30 days preoperatively to the date of surgery. Differences between cohorts were compared with the Fisher exact test and Wilcoxon test. A covariate-adjusted regression analysis was used to evaluate risk factors associated with increased postoperative opioid dosing.
Results:
Overall, 279 patients (n = 97 PRE; n = 182 POST; n = 42 opioid-tolerant; n = 237 opioid-naïve) were included in the final analysis. There was a significant reduction in the cumulative MME prescribed in the immediate (0-7 days) postoperative period (PRE, 450 MME vs POST, 315 MME), the first 30 postoperative days (PRE, 590 MME vs POST, 375 MME), and the first 90 postoperative days (PRE, 600 MME vs POST, 420 MME) (
Conclusion:
Opioid prescription–limiting legislation in Ohio significantly reduced the cumulative MME prescribed in the first 30 days postoperatively for both opioid-naïve and opioid-tolerant patients after shoulder arthroscopy. Consumption of opioids, benzodiazepines, and GABA analogues preoperatively was associated with increased postoperative opioid dosage.
The use of opioids for nonmedical and recreational purposes has fueled a public health emergency in the United States over the past few decades. Between 2002 and 2011, approximately 25 million people throughout the country used opioid pain medications for nonmedical use. 7 In 2016 alone, 11 million people in the United States misused opioids. 4 This upward trend in consumption has led to a predictable increase in the mortality rate attributed to prescription opioid medications, which quadrupled 6 between 2000 and 2014. Although many overdose cases are due to the consumption of illicit substances, including fentanyl and heroin, the prevalence of prescription opioid medications has also contributed to this issue. 6
Policymakers in the United States have instituted reasonable prescriber practice changes in many states to reduce the prevalence of circulating opioids. Many states have installed prescription drug monitoring programs, 13 while state-level legislation has been passed that regulates how opioids can be prescribed postoperatively. Ohio passed such legislation 12 on August 31, 2017. In Ohio, this legislation states that opioid prescriptions for acute pain, such as acute postoperative pain, cannot exceed a maximum dose per day of 30 morphine milligram equivalents (MMEs) and that they cannot be prescribed for more than 7 days for adults. Previous studies from various states have demonstrated that opioid prescription–limiting legislation is associated with significant reductions in the number and cumulative dosage of opioids prescribed after numerous orthopaedic procedures.3,13-17
Although the success of opioid prescription–limiting legislation has been exhibited in the context of numerous orthopaedic procedures, few studies have evaluated the effect of such legislation in the context of shoulder arthroscopy. It is important to ascertain this effect for numerous reasons. Perioperative and postoperative opioid consumption have been associated with relatively poor functional outcomes after shoulder arthroscopy. In a retrospective review of 1242 patients who underwent shoulder arthroscopy, Lu et al 9 identified preoperative opioid use as a significant predictor of reduced achievement of the Patient Acceptable Symptom State and increased likelihood of endorsing persistent pain. They also demonstrated that the risk of revision surgery increased with the consumption of high-dose opioids during the perioperative period. Likewise, Farley et al 8 revealed that any patient using ≥1 oral morphine equivalent per day had increased rates of 3-year revision surgery, reoperations, hospital readmission, emergency department encounters, and infections after arthroscopic rotator cuff repair. In addition, in contrast to many arthroscopic procedures, arthroscopic shoulder surgery is associated with considerable postoperative pain.1,11,19
The purpose of the present study was twofold. The first purpose was to determine the effect of Ohio’s opioid prescription–limiting legislation on opioid prescribing practices after shoulder arthroscopy. The second purpose was to identify patient factors that are associated with long-term (ie, after 30 days postoperatively) opioid use and increased opioid dosing postoperatively. We hypothesized that there would be a decrease in the number of postoperative opioid prescriptions filled, a decrease in the MME prescribed in the immediate postoperative period (ie, prescriptions filled within 7 days postoperatively) and in the first 30 postoperative days but no significant difference in the MME prescribed in the first 90 postoperative days.
Methods
Study Design and Data Collection
Approval for the study protocol was obtained from our institutional review board and the State of Ohio Board of Pharmacy. This retrospective cohort study included patients who underwent arthroscopic shoulder surgery between January 1, 2016, and March 31, 2020, by a single surgeon (R.J.G.) at an academic tertiary referral center. The Current Procedural Terminology codes 29805, 29806, 29807, 29822, 29823, 29825, 29826, and 23430 were used to identify potentially eligible participants. Patients who underwent arthroscopic rotator cuff repair were excluded because the procedure is associated with considerable postoperative pain when compared with other arthroscopic shoulder procedures.1,19 Likewise, we excluded arthroscopic distal clavicle excision from our cohort of patients because it is routinely performed as an open procedure at our institution. In addition, patients were excluded from the study if their information in the electronic medical record or the Ohio Automated Rx Reporting System (OARRS), the State of Ohio’s Board of Pharmacy prescription drug monitoring program, was absent or incomplete.
Patients were categorized into 1 of the 2 cohorts based on their date of surgery. Those patients who underwent shoulder arthroscopy before August 31, 2017, (the date the opioid prescription–limiting legislation was passed) were placed into the prelegislation (PRE) cohort, while patients who underwent surgery on or after August 31, 2017, were placed into the postlegislation (POST) cohort. In addition, patients were classified as opioid-naïve if they did not have an opioid prescription prescribed within 30 days before surgery and as opioid-tolerant if they had at least 1 opioid prescription prescribed within the 30 days before surgery. This is in accordance with previously published studies14-17 that used the 30-day cutoff as per the regulations of the Department of Health in the State of Rhode Island.
The patients’ electronic medical records were reviewed, and information on age, sex, body mass index (BMI), laterality of the procedure, medical comorbidities, and preoperative medication/substance use were extracted (ie, tobacco, alcohol). In addition, a query was performed on the OARRS database, which is a 5-year rolling database; thus, data before the 5-year period were automatically expunged daily from the system. Data regarding controlled substance prescriptions were obtained for all patients from 30 days preoperatively to 90 days postoperatively. Information was obtained regarding the type and dose of oral opioids, the number of prescriptions, and the number of pills per prescription. To account for the relative potency of each opioid, the dosage was converted into MME using the following multipliers
10
: oxycodone,
Statistical Analysis
The patients’ sociodemographic variables were stratified by time with respect to the passage of legislation (PRE vs POST) using frequency and percentage for categorical variables and medians and interquartile ranges (IQRs) for continuous variables. Differences between PRE and POST data were compared using the Fisher exact test for categorical variables and Wilcoxon test for continuous variables. The Wilcoxon test was also used to distinguish intracohort measures for the opioid-tolerant versus opioid-naïve groups. The Kruskal-Wallis equality of populations rank test was applied to assess the interaction between both opioid use and legislation.
An average treatment effect (ATE) regression model was used to determine the effect of the opioid prescription–limiting legislation on the cumulative MME prescribed postoperatively, with inverse-probability weighting to correct the imbalance in the distributions of the patient characteristics and surgical procedures on the potential outcomes before and after the enactment of the legislation. We performed a covariate-adjusted regression analysis to evaluate risk factors associated with increased postoperative opioid dosing. In all regression models, the variables of interest were adjusted or controlled for age, sex, BMI, and date of legislation passage (August 31, 2017). Finally, a post hoc power analysis was conducted, which was powered to the cumulative MME in the first 30 days based on our ATE analysis.
All statistical tests were 2-sided, and statistical significance was defined as
Results
Overall, 279 patients were selected for this study, with 97 and 182 patients placed into the PRE and POST cohorts, respectively (Table 1). The percentage of patients who reported that they consumed any amount of alcohol was the only significant difference between the 2 cohorts (PRE, 18.6% vs POST, 37.4%;
Patient Characteristics According to Pre- and Postlegislation Cohorts (N = 279) a
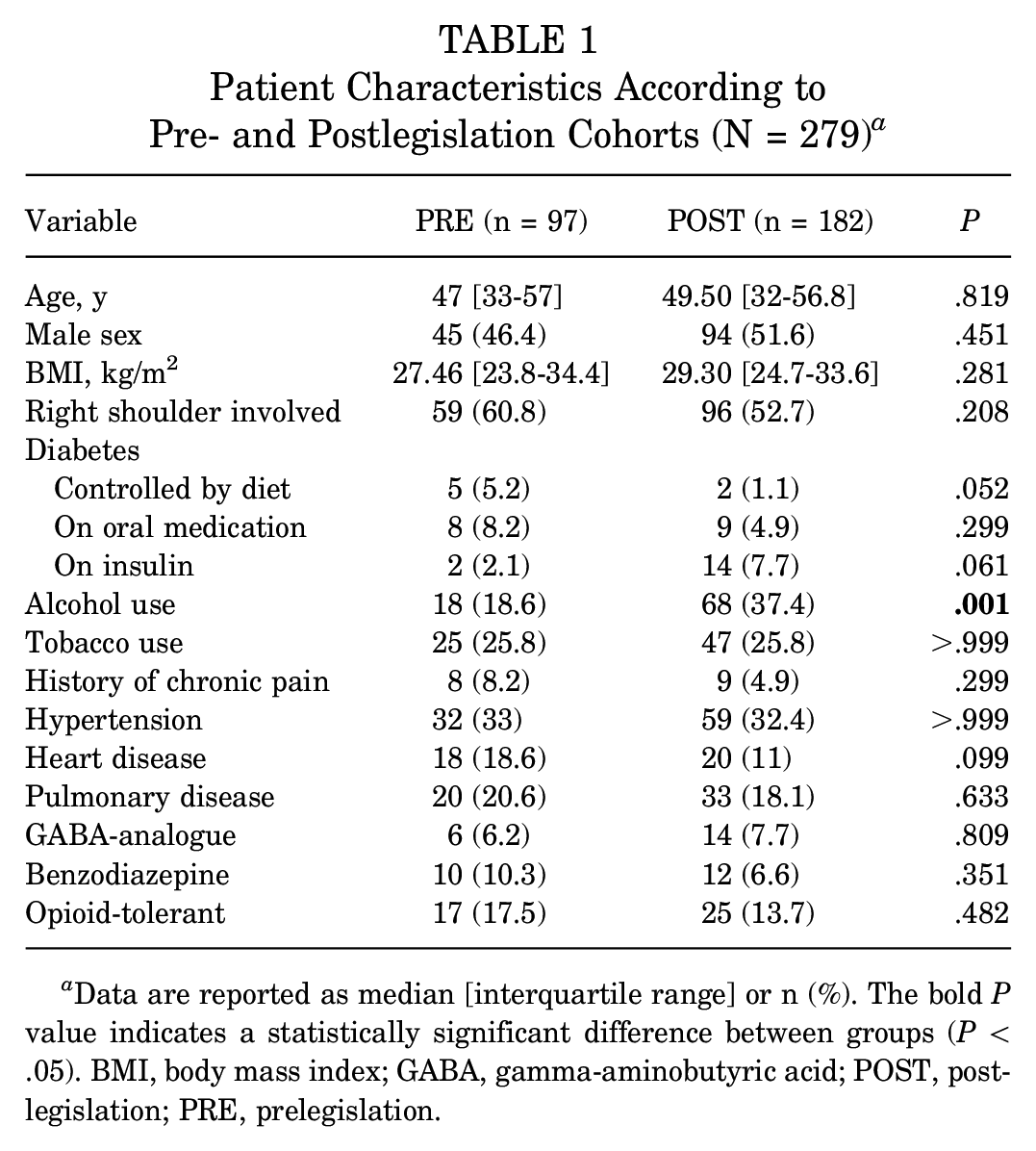
Data are reported as median [interquartile range] or n (%). The bold
Effect of Legislation on Postoperative Opioid Prescription
There was a significant reduction in the median [IQR] cumulative MME prescribed in the immediate postoperative period (PRE, 450 [450-600] MME vs POST, 315 [210-450] MME;
Cumulative Opioid Prescriptions According to Pre- and Postlegislation Cohorts a

Data are reported as median [interquartile range]. Bold
The ATEs of the opioid prescription–limiting legislation on cumulative postoperative MMEs are shown in Table 3. The legislation was associated with a significant reduction in the cumulative MME prescribed in the immediate postoperative period (ATE, −149.34 MME;
Average Treatment Effects of the Opioid Prescription–Limiting Legislation on MME and Prescriptions a
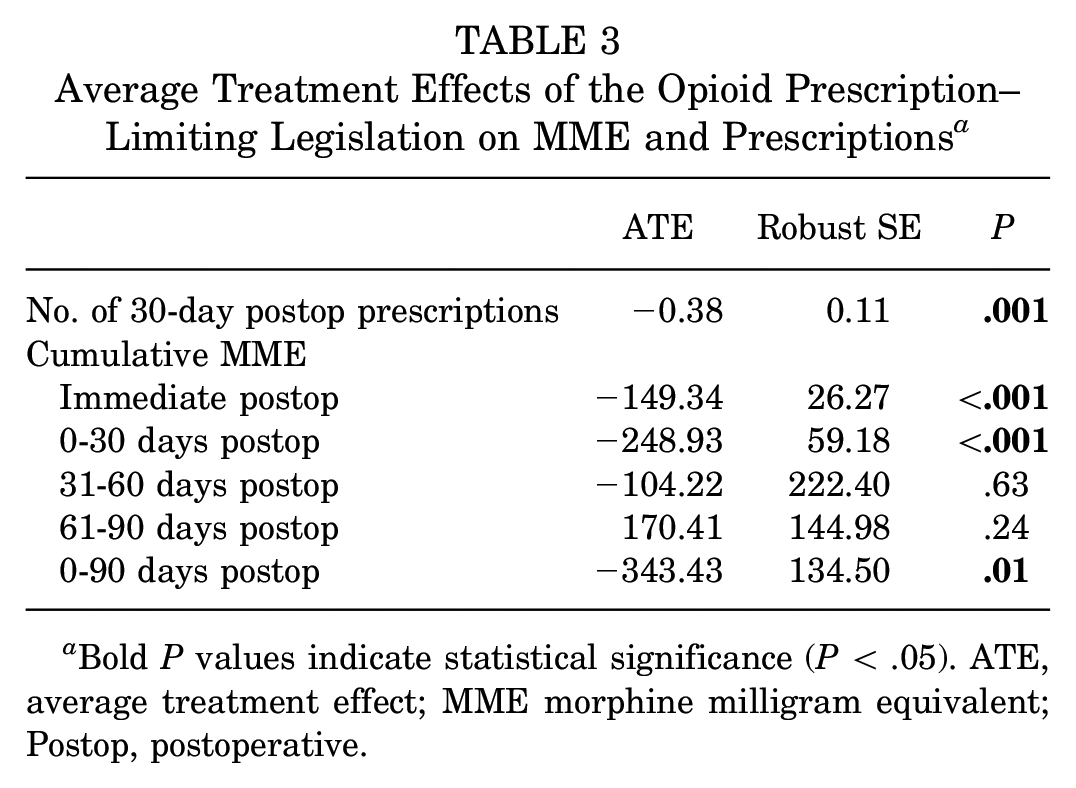
Bold
Effect of Preoperative Opioid Tolerance Status on Postoperative Opioid Prescriptions
Table 4 illustrates the effects of the preoperative opioid use status (ie, opioid-naïve vs opioid-tolerant) on postoperative opioid prescriptions. The median [IQR] cumulative MME was significantly less in the opioid-naïve cohort compared with the opioid-tolerant cohort in the immediate postoperative period (tolerant, 450 [375-600] MME vs naïve, 337.5 [210-450] MME;
Opioid Prescription Data According to Opioid Tolerance a
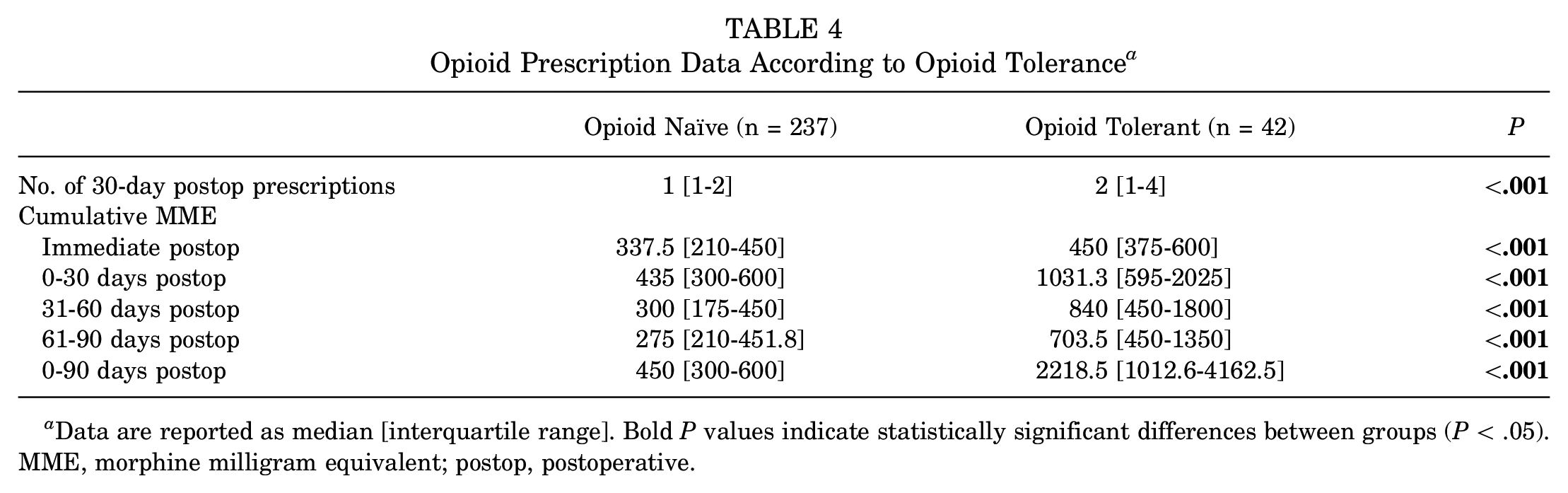
Data are reported as median [interquartile range]. Bold
Combined Effect of Legislation and Preoperative Opioid Status on Postoperative Opioid Prescriptions
Opioid prescription patterns stratified by the legislation period and preoperative opioid tolerance status are shown in Table 5. Within the opioid-naïve cohort, 80 patients were placed into the PRE subcohort, and 157 patients were placed into the POST subcohort. In the opioid-tolerant cohort, 17 patients were placed into the PRE subcohort, and 25 patients were placed into the POST subcohort. There was a significant reduction in the median [IQR] cumulative MME prescribed in the immediate postoperative period (PRE, 450 [450-600] MME vs POST, 315 [210-420] MME;
Opioid Prescription Data According to Both Opioid Tolerance and Legislation a

Data are reported as median [interquartile range]. Bold
Risk Factors for Increased Postoperative Opioid Use
The risk factors for increased postoperative opioid dosing are shown in Table 6. Preoperative opioid tolerance was an independent risk factor for increased cumulative MME at 0-30 postoperative days (β = 705.33;
Results of Covariate-adjusted Regression Analysis Evaluating Independent Risk Factors for Postoperative Opioid Prescribing a

Bold
Coefficients from quantile regression analysis for the outcome of interest: MME intake up to first 30 days; MME intake 0 to 90 days.
OR from logistic regression analysis of prolonged opioid use (yes or no) in the 31- to 90-day postoperative period. In all regression models, the variables of interest were adjusted or controlled for age, sex, body mass index, and date of legislation passage.
Results of Post Hoc Power Analysis
Based on our ATE analysis, the difference in the cumulative MME in the first 30 days is 248.93 ± 59.18. Using this MME value, an alpha of .05, and a 2-sided 2-sample equal variance
Discussion
The major findings of our study demonstrate that there were significant reductions in the cumulative MME prescribed in the immediate (PRE, 450 MME; POST, 315 MME), first 30-day (PRE, 590 MME; POST, 375 MME), and first 90-day (PRE, 600 MME; POST, 420 MME) postoperative periods after shoulder arthroscopy between the prelegislation and postlegislation cohorts, respectively (
Our results are congruent with previously published studies that examined the effect of similar legislation on opioid-prescribing practices after shoulder surgery.14,18 In a retrospective review of 446 patients who underwent arthroscopic rotator cuff repair in Rhode Island, Shah et al 18 highlighted a significant reduction in the number of opioid prescriptions filled within the first 30 days postoperatively and the cumulative MME prescribed in the first postoperative prescription as well as the first 30 days postoperatively between their PRE and POST cohorts. Similarly, in an analysis of 334 patients who underwent shoulder arthroplasty in Ohio, Raji et al 14 demonstrated significant reductions in the cumulative MME prescribed in the 0-7 days and 0-30 days postoperative periods when comparing their PRE and POST cohorts.
We could not demonstrate a significant decrease in the cumulative MME prescribed in the 31-60 days or 61-90 days postoperative periods. These results are comparable to previously published studies. Reid et al were able to show significant decreases in the cumulative MME prescribed during the first 30 days after lumbar spine surgery 15 and total joint arthroplasty 17 but not within 30 to 90 days after these procedures in Rhode Island. Together, these findings suggest the laws in Ohio and Rhode Island are not likely to decrease chronic opioid use. However, these laws still provide a larger societal benefit by reducing the number of circulating opioids and thus potentially decreasing the risk of opioid diversion, a practice in which legal prescription drugs are distributed illegally for use not intended by the prescriber.
Reducing the prevalence and accessibility to opioid medications after orthopaedic surgery is critical in the effort to curtail the opioid epidemic in the United States as well as to improve patient outcomes postoperatively. Increased opioid consumption after hip arthroscopy for femoroacetabular impingement syndrome is associated with significantly worse Harris Hip scores and visual analog satisfaction and pain scores.2,20 With respect to shoulder arthroscopy, preoperative opioid use is a significant predictor of worse outcomes postoperatively, 9 while the consumption of ≥1 oral morphine equivalent was associated with increased rates of revision surgery, reoperations, hospital readmission, emergency department encounters, and infection. 8 Future studies are warranted to examine the impact of opioid prescription–limiting legislation on clinical outcomes, including reoperations, hospital readmissions, and emergency department utilization.
Limitations
The outcomes of this study must be interpreted within its limitations. First, although the post hoc power analysis demonstrated that our study was adequately powered with our given sample sizes, we acknowledge that our patient population was relatively small. We attribute this to an inherent flaw of the OARRS database. Although the OARRS database tracks the prescription of all scheduled medications within Ohio, the database can be incomplete and/or inaccurate. Second, the results of this study ostensibly reflect the experience of a single surgeon at a single, academic, tertiary referral center. Third, the OARRS database tracks written and filled opioid prescriptions, but it does not track opioid consumption. It is reasonable to conclude that patients consumed less opioids than what was originally prescribed and either disposed of or diverted any unused medication. However, a recent survey of patients receiving opioids for pain management reported that only 33% of patients disposed of their unused opioid medication. 5 Therefore, we believe that filled opioid prescriptions serve as a valid metric for opioid consumption. Fourth, the OARRS database does not track inpatient opioid prescription or consumption patterns. Although many, if not all, patients within this cohort underwent surgery on an outpatient basis, they still received opioids intraoperatively and during their brief stay in the postanesthesia care unit.
Conclusion
Opioid prescription–limiting legislation in Ohio significantly reduced the cumulative MME prescribed in the first 30 days postoperatively for both opioid-naïve and opioid-tolerant patients after shoulder arthroscopy. Consumption of opioids, benzodiazepines, and GABA analogues preoperatively was associated with a larger cumulative MME prescribed postoperatively. The results of this study demonstrate that such legislation in Ohio is associated with a significant reduction in the amount of MME prescribed after shoulder arthroscopy.
Footnotes
Final revision submitted April 22, 2023; accepted May 19, 2023.
One or more of the authors has declared the following potential conflict of interest or source of funding: Y.R. has received education payments from Rock Medical Orthopedics. N.N.T. has received education payments from Evolution Surgical and Smith & Nephew. J.G.C. has received education payments from Evolution Surgical, Rock Medical Orthopedics, and Smith & Nephew. J.E.V. has received consulting fees from DePuy Synthes and nonconsulting fees from Arthrex. R.J.G. has received education payments from Rock Medical Orthopedics; consulting fees from Encore Medical and Stryker; and royalties from Shoulder Innovations. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Case Western Reserve University, Cleveland, Ohio, USA (No. STUDY20200623).
