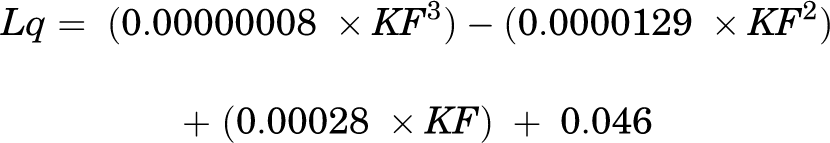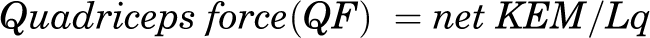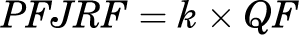Abstract
Background:
Patellofemoral joint complications have commonly been reported in long-term outcome studies for anterior cruciate ligament reconstruction (ACLR); however, the biomechanics in the early phases of rehabilitation that could be associated with the development of these abnormalities is unclear. Limb dominance may affect the biomechanics of the knee joint in patients after ACLR.
Purpose:
To compare knee joint loading between surgical and nonsurgical limbs at 12 weeks postoperatively in patients who underwent ACLR on either their dominant limb (ACL-D) or nondominant limb (ACL-ND).
Study Design:
Controlled laboratory study.
Methods:
Included were 54 patients (32 ACL-D and 22 ACL-ND). Peak and integrated patellofemoral joint stress (PFJS), peak patellofemoral joint reaction force (PFJRF), and peak knee extension moment (KEM) were assessed during the stance phase of gait while participants walked on a 10-m runway at a self-selected speed.
Results:
The surgical limb of the ACL-D group had significantly decreased peak PFJS (P < .001), integrated PFJS (P < .001), peak PFJRF (P < .001), and peak KEM (P < .001) compared to the nonsurgical limb. The surgical limb of the ACL-ND group demonstrated significantly increased peak PFJS (P = .001), integrated PFJS (P = .023), peak PFJRF (P < .001), and peak KEM (P = .001) compared to the nonsurgical limb. For the surgical limb, the ACL-ND group demonstrated significantly greater peak PFJS (P < .001), peak PFJRF (P < .001) , (PFJRF [P<.001]) and peak KEM (P < .001) than the ACL-D group. For the nonsurgical limb, the ACL-D group demonstrated greater peak PFJS (P < .001), integrated PFJS (P = .023), peak PFJRF (P = .003), and peak KEM (P < .001) than the ACL-ND group.
Conclusion:
Significantly larger knee joint loading on the surgical limb of the ACL-ND group and smaller knee joint loading on the surgical limb of the ACL-D group were observed compared to the contralateral nonsurgical limb, which suggests that limb dominance has a key role in loading at the knee joint during gait.
Clinical Relevance:
Altered knee joint loading during gait at 12 weeks after ACLR may lead to the development of patellofemoral joint abnormalities.
Keywords
Patellofemoral joint complications such as patellofemoral pain (PFP) and patellofemoral osteoarthritis (PFOA) are common after anterior cruciate ligament (ACL) reconstruction (ACLR). Complications begin to emerge shortly after the completion of rehabilitation. Approximately 6% to 26% of patients who have undergone ACLR develop either PFP or PFOA in the first 2 years after surgery. 7,25,34 Furthermore, up to 72% who have undergone ACLR develop PFOA and symptoms within 15 years after ACLR. 8,27,29 Despite the high prevalence of patellofemoral joint complications after ACLR, the underlying mechanism of these abnormalities has not fully been investigated.
PFP has been suggested as a potential precursor to the progression of PFOA. 9 These abnormalities are hypothesized to develop as a result of repetitive and increased loading at the patellofemoral joint over time. Although it is still unclear if PFP and PFOA share similar mechanisms of injury, patients with PFP and PFOA have been shown to have altered loading patterns at the knee joint, including increased and decreased patellofemoral joint stress (PFJS), patellofemoral joint contact force, 3,9,11,42 and internal knee extension moment (KEM) 22,42 during functional activities, suggesting that the change in biomechanics of the knee may be associated with an increased risk of the development of PFP and PFOA.
Investigations of patellofemoral joint loading after ACLR are limited, and the results are inconclusive. 15,17,41 Herrington et al 17 reported greater peak patellofemoral joint loading in the surgical limb during running. In contrast, Sritharan et al 41 and Hannon et al 16 reported lower peak PFJS in the nonsurgical limb during running and single-leg tasks. The inconsistencies between studies demonstrate a lack of definitive understanding of patellofemoral joint loading after ACLR.
The discrepancy in the aforementioned conclusions regarding patellofemoral joint loading after ACLR may be attributed to limb dominance, which these studies did not account for. There is growing evidence that asymmetric biomechanics is present between dominant and nondominant limbs of both healthy participants 12,40 and patients undergoing ACLR. 24 A recent study demonstrated that patients who underwent ACLR on their dominant limb had greater knee joint loading in their surgical limb during drop jump landing compared with those who underwent ACLR on their nondominant limb. 24 Additionally, knee joint loading of the surgical limb was greater in patients who underwent ACLR on their dominant limb but smaller in patients who underwent ACLR on their nondominant limb compared to the contralateral nonsurgical limb. The bilateral comparison method has been frequently used to show how much alteration occurs in the surgical limb relative to the contralateral nonsurgical limb; however, this method could possibly mask the true effect of limb dominance.
After ACLR, patients traditionally begin to increase the level of activities at or near the 12-week postoperative time point by performing more functional tasks, such as single-leg tasks and jogging, 44 which consequently increase loading at the knee joint. Because joint loading patterns appear to be established during the early stages of rehabilitation and persist across time, 38 it is important to address knee joint loading patterns that may be associated with the subsequent development of patellofemoral joint abnormalities in the same time frame. Considering the side of limb dominance after an injury and ACLR may provide greater insight into the complexity of biomechanical alterations after a surgical intervention, with the added benefit of designing rehabilitation programs individualized to the patient.
Therefore, the primary purpose of this study was to compare knee joint loading between the surgical and nonsurgical limbs in patients who had undergone ACLR in either their dominant limb (ACL-D group) or nondominant limb (ACL-ND group). The secondary purpose was to examine the differences in knee joint loading between the surgical limb of the 2 groups and also the nonsurgical limb of the 2 groups. We hypothesized that the ACL-D and ACL-ND groups would demonstrate significantly different side-to-side knee joint loading (within-group comparison). We also hypothesized that that there would be a difference in knee joint loading in the surgical and nonsurgical limbs of the ACL-D and ACL-ND groups (between-group comparison).
Methods
Participants
A total of 54 patients (32 men and 22 women) aged between 12 and 25 years were evaluated in this ongoing prospective study of clinical and biomechanical outcomes after ACLR at our laboratory. Participants were included in the study if they: (1) underwent unilateral ACLR; (2) had a bone–patellar tendon–bone autograft; (3) participated in high-risk sport activities that require jumping, landing, cutting, and pivoting at the time of injury; (4) had an intention to return to sport activities; and (5) participated in physical therapy for the purpose of returning to sport. Participants were excluded from the study if they had any of the following concomitant injuries: (1) full-thickness chondral defect of 1 cm2, (2) grade 2 or 3 medial collateral ligament or lateral collateral ligament sprain, (3) posterior cruciate ligament tear (grade 3), or (4) simultaneous fracture with an ACL tear. Participants were also excluded if they had a history of ACL injuries in the ipsilateral limb (graft tear) or contralateral limb (ACL tear). Before participation in the study, patients signed consent forms as approved by the Texas Health Resources Institutional Review Board; participants aged ≤17 years provided parental permission and child assent.
Procedures
A cross-sectional study design was used. This current study is part of a large ongoing outcome study for ACLR. The assessment for the current study was conducted once at the clinical biomechanics laboratory of Texas Health Sports Medicine at 12 weeks (±7 days) after surgery. Participants were recruited between February 2017 and August 2019. Before the biomechanical assessment, participants completed the International Knee Documentation Committee (IKDC) measure to assess subjective knee function. There were 8 3-dimensional cameras (Oqus 700; Qualisys) and 2 force plates (AMTI) that collected kinematic and ground-reaction force data during gait at a sampling frequency of 120 Hz and 1200 Hz, respectively. Isokinetic quadriceps strength was assessed at 60 deg/s using the Multi-Joint System (Biodex).
Gait Analysis
A total of 33 retroreflective markers were secured to the bilateral acromion process, posterior superior iliac spine, greater trochanter, medial and lateral femoral condyles, medial and lateral malleoli, base of the first and fifth metatarsals, calcaneus, midthigh, and midshank. Additionally, markers were placed at the 7th cervical vertebra, the 12th thoracic vertebra, between the 4th and 5th lumbar vertebrae, and the manubrium.
All participants walked on an approximately 10-m runway at a self-selected speed until striking the force plate with the foot of their testing limb. We chose a self-selected velocity because it allowed for the participants to walk at their comfortable gait speed with natural gait mechanics. Each participant’s self-selected gait speed was recorded with an electrical timing gate system (Dashr). Participants performed practice trials until they were comfortable with the testing procedure and were able to strike the force plate without altering their gait pattern and with a consistent speed. The average speed was calculated using the closest 3 speeds during the practice trials. During data collection, participants walked at a velocity within ±5% of the average walking speed recorded during their practice trials. Trials were repeated if the participants did not make natural foot contact on the force plate, the participant’s foot was not completely on the force plate during foot strike, or the walking velocity was 5% above or below their predetermined walking velocity. These procedures were repeated until 3 acceptable trials were collected from the nonsurgical limb, followed by the surgical limb.
Isokinetic Quadriceps Strength Test
Participants were seated on the Biodex system and secured with padded straps around the distal end of the shank, thigh, pelvis, and torso to minimize accessory and compensatory movements during testing. 10,20 The femoral condyle of the testing limb was aligned with the Biodex axis of rotation following the manufacturer’s instructions. After a familiarizing session consisting of up to 5 repetitions of submaximal knee extension/flexion, participants were instructed to extend and flex their knees as hard and as quickly as possible 5 consecutive times. The order of testing was the nonsurgical limb, followed by the surgical limb. Peak quadriceps strength values (N·m) were averaged across 5 trials, and the average was normalized to body mass (N·m/kg).
Data Processing and Reduction
All kinematic and force data were transported into Visual3D software (C-Motion) for data processing and reduction. Marker and ground-reaction force data were filtered using fourth-order Butterworth filters using a cutoff frequency of 12 Hz. KEM was calculated using the inverse dynamics approach, normalized to the participants’ body height × weight, and presented as internal moment, with negative values representing extension.
PFJS and patellofemoral joint reaction force (PFJRF) were estimated using a previously developed algorithm. 4,14 The algorithm consists of sagittal-plane biomechanics (knee flexion angle [KF] and KEM) as well as previously identified variables, including quadriceps lever arm length (Lq), 3,35,43 patellofemoral joint contact area, 2,32 and coefficient value (k), 3,39 as follows:
Peak PFJS, integrated PFJS with respect to the length of the stance phase, peak PFJRF, and peak KEM during the stance phase of gait were calculated and averaged across 3 trials. Integrated PFJS was calculated because it represents the amount of stress in relation to the patellofemoral joint contact area during the entire stance phase of gait. Because PFP and PFOA develop over time, reporting the overall amount of stress along with peak PFJS during the stance phase of gait might help to explain the potential risk of the development of PFOA. Stance phase was defined as the period from initial contact to toe-off when the vertical ground-reaction force exceeded 20 N and dropped below 20 N, respectively. PFJRF was normalized to body weight.
Statistical Analysis
Participants were divided into 2 groups: those who had undergone ACLR on their dominant limb (ACL-D) and those who had undergone ACLR on their nondominant limb (ACL-ND). The dominant limb was defined as the limb used to kick a ball for a maximal distance. 24,26 Independent t tests were performed to examine differences in height, weight, age, and isokinetic quadriceps strength between the groups. Separate 2 (surgical vs nonsurgical) by 2 (ACL-D vs ACL-ND) repeated-measures analysis of variance was performed to examine if leg dominance influenced surgical status for dependent variables. When a significant interaction was observed, post hoc Bonferroni tests were performed to examine the differences in each dependent variable between the surgical and nonsurgical limbs of each group (ACL-D and ACL-ND), the surgical limbs between the groups, and the nonsurgical limbs between the groups. SPSS Statistics Version 25 (IBM) was used for all statistical analyses, with the alpha level set a priori at 0.05.
Results
Overall, 22 participants were assigned to the ACL-D group (11 men and 11 women; mean age, 16.00 ± 1.35 years), and 32 participants were assigned to the ACL-ND group (21 men and 11 women; mean age, 16.24 ± 1.70 years) (Table 1). There were no statistically significant differences observed for height, weight, or age between the groups. Shapiro-Wilk tests revealed that data were normally distributed for each dependent variable in each group (P > .05). There were main effects for limb in peak PFJS (nonsurgical > surgical; P = .017) and peak PFJRF (nonsurgical > surgical; P = .017). No other main effects for limb or group were observed in any of the variables. There were significant limb-by-group interactions observed for peak PFJS (F 1,52 = 43.83; P < .001) (Figure 1A), integrated PFJS (F 1,52 = 22.66; P < .001) (Figure 1B), peak PFJRF (F 1,52 = 41.46; P < .001) (Figure 1C), and peak KEM (F 1,52 = 38.16; P < .001) (Figure 1D).
Participant Demographics a

a Data are reported as mean ± SD unless otherwise specified. ACL-D, anterior cruciate ligament reconstruction on dominant limb; ACL-ND, anterior cruciate ligament reconstruction on nondominant limb; IKDC, International Knee Documentation Committee; NA, not applicable.

(A) Peak patellofemoral joint stress (PFJS), (B) integrated PFJS, (C) peak patellofemoral joint reaction force (PFJRF), and (D) peak knee extension moment (KEM) between the surgical and nonsurgical limbs of the ACL-D and ACL-ND groups. ACL-D, anterior cruciate ligament reconstruction on dominant limb; ACL-ND, anterior cruciate ligament reconstruction on nondominant limb; BW, body weight. Error bars represent SDs. *Significant difference between the surgical and nonsurgical limbs. #Significant difference in the surgical limbs between groups. §Significant difference in the nonsurgical limbs between groups.
Within-Group Differences
Figure 1 and Table 2 show the results of the knee joint loading trials for the study groups. Post hoc tests demonstrated that the surgical limb of the ACL-D group had significantly decreased peak PFJS (P < .001), integrated PFJS (P < .001), peak PFJRF (P < .001), and peak KEM (P < .001) compared to the nonsurgical limb. Unlike the ACL-D group, the surgical limb of the ACL-ND group demonstrated significantly increased peak PFJS (P = .001), integrated PFJS (P = .023), peak PFJRF (P < .001), and peak KEM (P = .001) compared to the nonsurgical limb. When limited to the surgical limb, the ACL-ND group demonstrated significantly greater peak PFJS (P < .001) and peak KEM (P < .001) than the ACL-D group. For the nonsurgical limb, the ACL-D group demonstrated greater peak PFJS (P < .001), integrated PFJS (P = .029), peak PFJRF (P = .003), and peak KEM (P < .001) than the ACL-ND group.
Knee Joint Loading Results a

a Data are reported as mean ± SD (95% CI). ACL-D, anterior cruciate ligament reconstruction on dominant limb; ACL-ND, anterior cruciate ligament reconstruction on nondominant limb; BW, body weight; ht, height; KEM, knee extension moment; PFJRF, patellofemoral joint reaction force; PFJS, patellofemoral joint stress.
Between-Group Differences
Post hoc tests demonstrated that the surgical limb of the ACL-ND group had significantly greater peak PFJS (P < .001), peak PFJRF (P < .001), and peak KEM (P < .001) than the surgical limb of the ACL-D group, while there was no significant difference observed in integrated PFJS (P = .205). For the nonsurgical limb, the ACL-D group had significantly greater peak PFJS (P < .001), integrated PFJS (P = .023), peak PFJRF (P = .003), and peak KEM (P < .001) than the ACL-ND group.
Discussion
The purpose of the current study was to examine the knee joint mechanical loading differences in those who underwent ACLR on their dominant versus nondominant limb. The results of our study support our hypotheses and clearly indicate that the side of limb dominance after ACLR played a role in knee joint mechanical loading during gait at 12 weeks postoperatively. These findings may be associated with the future development of patellofemoral joint abnormalities. Significant differences were observed in both groups; however, the patterns were different. The ACL-D group demonstrated less knee joint loading in the surgical limb compared to the nonsurgical limb, while the ACL-ND group demonstrated greater knee joint loading in the surgical limb compared to the nonsurgical limb. Furthermore, knee joint loading of the surgical limb in the ACL-ND group was greater than that of the surgical limb in the ACL-D group, while knee joint loading of the nonsurgical limb in the ACL-D group was greater than that of the nonsurgical limb in the ACL-ND group.
Patellofemoral Joint Loading
Side-to-side differences in patellofemoral joint loading after ACLR have been observed in a limited number of studies and suggested as a possible factor for the development of PFP and PFOA. 16,18,41 The results of the present study both support and contradict previous findings. 16,17,41 The findings of greater peak PFJS, integrated PFJS, and peak PFJRF of the surgical limb in the ACL-ND group relative to the contralateral nonsurgical limb support the earlier results of Herrington et al, 17 who demonstrated greater patellofemoral joint contact pressure and force in the surgical limb compared to the contralateral nonsurgical limb and healthy participants during running at the time of return to sport. On the other hand, the results of our ACL-D group support the findings of Sritharan et al 41 and Hannon et al, 16 who demonstrated decreased patellofemoral joint loading, including peak patellofemoral joint contact force and impulse 41 and integrated PFJS 16 during running 41 and single-leg squats 16 at various time points ranging from 12 weeks to approximately 18 months after ACLR. The discrepancies of these studies should be interpreted with caution, as limb dominance was not accounted for, which can be a confounding variable.
Knee Extension Moment
Greater peak KEM was observed in the surgical limb of the ACL-ND group, while the surgical limb of the ACL-D group demonstrated decreased peak KEM. The result of the ACL-ND group is unexpected, while the result of the ACL-D group supports the common understanding of knee joint loading after ACLR that surgical limbs have decreased KEM compared to nonsurgical limbs at a variety of time points during various tasks. 13,17,21,28,38,41 Decreased KEM has been suggested as a compensatory mechanism for decreased quadriceps strength, 23 as a smaller KEM does not require as much force generation from the quadriceps muscle group to counteract the external knee flexion moment. When a subanalysis on quadriceps strength in the current study was conducted between groups for surgical and nonsurgical limbs, no statistically significant differences were observed (surgical: P = .433; nonsurgical: P = .271). Therefore, the aforementioned hypothesis of decreased quadriceps strength in those patients with a smaller KEM may not be the case for the ACL-ND group in the current study. Previous studies have identified that center of pressure (COP) location is associated with the magnitude of the KEM. 5 In one study examining patients after ACLR during double-leg squats, Chan and Sigward 5 demonstrated that a more anteriorly located COP is associated with a smaller KEM, as an anteriorly located COP decreases the moment arm for the knee, consequently decreasing the KEM. We did not examine COP location in the current study; however, there may be a possibility that the location of the COP was shifted more anteriorly for the dominant limb (surgical limb of the ACL-D group and nonsurgical limb of the ACL-ND group) compared to the contralateral nondominant limb. This loading pattern could suggest that the neuromuscular system in these patients tends to “prefer” to use a more protective pattern in the dominant limb compared to those in the ACL-ND group and that loading patterns observed in the current study may not rely solely on quadriceps strength or the injury but that limb dominance and some aspects of neuromuscular control may be key factors. However, this is purely speculation and will require further investigations to validate these thoughts. At this time, there is too little research available to speculate or draw conclusions on what leads to this loading pattern based on limb dominance.
Overloading Versus Underloading
Altered patellofemoral joint loading and KEM have been observed in patients with PFP and PFOA and have been suggested as factors for the development of these abnormalities. Several research studies have demonstrated increased PFJS in patients with PFP compared to those without PFP during stair-stepping and walking tasks. 3,9 Furthermore, increased peak KEM and impulse have been observed in patients who progressively developed PFOA over 1 year confirmed by magnetic resonance imaging 42 and self-rated functional scores 22 during gait compared to those who did not. Finally, finite element models have demonstrated increased pressure and shear stress within the patellofemoral joint in female patients with PFP. 9 Cause-and-effect relationships cannot be drawn from these studies; however, these findings could suggest that increased knee joint loading may lead to the development of patellofemoral joint abnormalities. On the other hand, decreased patellofemoral joint loading has been observed in patients with PFP and PFOA during gait 30 and stair-stepping tasks. 4,11 A decreased KEM was also observed in patients with PFP and PFOA during gait and stair-stepping tasks. 11,30,36 These underloading strategies have been believed to serve as a compensatory strategy for weak quadriceps strength and to minimize pain. It is also believed to be linked to the development of osteoarthritis. 1 Furthermore, the association between underloading and morphological changes, including reduced metabolism 31 and thinner cartilage, 37 is well described, which is suggested to lead to the development of osteoarthritis.
The aforementioned evidence suggests that both overloading and underloading could lead to the development of PFP and PFOA; therefore, both the surgical and nonsurgical limbs of each group may have the potential to develop these abnormalities. To support this notion of PFOA, the occurrence is not limited to the surgical limb. A recently published systematic review 6 reported that PFOA occurs in both surgical and nonsurgical limbs. Between 10 and 23 years after ACLR, 28% to 80% of patients developed PFOA in the surgical limb. 6 Although a statistical analysis was not performed, the percentage of those who developed PFOA in the nonsurgical limb was not as high (9%-56%) as that for the surgical limb. 6 The results of the current study may help to explain why PFOA has previously been reported in both the surgical and nonsurgical limbs after ACLR. 6 Although this systematic review did not report the side of dominance, we could speculate that there may be a risk of the development of PFOA in both the surgical and nonsurgical limbs depending on which limb underwent surgery.
Impact of Limb Dominance
Previous studies have shown biomechanical differences between dominant and nondominant limbs during landing in healthy participants as well as patients who have undergone ACLR. 12,24,26,40 Specific to peak KEM, a greater KEM was previously observed in the nondominant limb of collegiate athletes during the first 40 milliseconds of a drop vertical jump task, 26 while a smaller KEM was observed in the dominant limb of volleyball athletes during single-leg landing. 40 In a recent investigation on patients who had undergone ACLR, Malafronte et al 24 demonstrated that, at the time of return to sport, athletes who underwent ACLR on the dominant limb had greater knee joint energy absorption in the surgical limb during the loading phase of a jump landing task compared to the contralateral nonsurgical limb and the surgical limb of patients who underwent ACLR on their nondominant limb. Although these results are inconsistent as to which limb had greater joint loading, these studies consistently demonstrated limb asymmetry in healthy participants and patients who underwent ACLR. 24
In the current study, when limiting to the surgical limb, the ACL-ND group had significantly greater peak PFJS (P < .001), peak PFJRF (P < .001), and peak KEXTmm (P < .001) than the surgical limb of the ACL-D group. For the nonsurgical limb, peak PFJS, integrated PFJS, peak PFJRF, and peak KEM were significantly greater in the ACL-D group compared to the ACL-ND group. This suggests that ACLR may not necessarily be the only factor that contributes to altered knee joint loading patterns observed in the current study during the stance phase of gait at 12 weeks after ACLR. Furthermore, the side of limb dominance may play a key role in the knee joint loading pattern during functional tasks. Perhaps the altered loading pattern observed in the current study is innate and was not solely affected by ACLR. Previous investigations on healthy participants have demonstrated differences in motor learning patterns, 19 brain activities, 19 and movement strategies 33 between dominant and nondominant limbs, which could support the loading pattern difference observed in the current study may have already existed before the injury. This is one of the first studies examining side-to-side differences based on limb dominance in patients who underwent surgery. More investigations should be conducted for better understanding of the impact of limb dominance after ACLR.
There are no specific rehabilitation protocols for patients who have undergone ACLR on the dominant and nondominant limbs. Given the findings of the current study that there may be a possibility of the development of patellofemoral joint abnormalities for both surgical and nonsurgical limbs, there may be a benefit in treating the nonsurgical limb as much as the surgical limb is treated after ACLR.
Limitations
None of the participants included in the current study had self-reported pain associated with PFP or PFOA or were diagnosed with PFP or PFOA at 12 weeks after ACLR. The altered joint loading patterns observed in the current study may have been affected by pain at the graft site, residual swelling, and range of motion deficits in the knee joint, which we would expect to improve over time. Therefore, we do not know how the observed biomechanical differences would lead to the development of patellofemoral joint abnormalities or diminish over time. Prospective research studies should be conducted to better understand the influence of the side of dominance on changes in the knee loading pattern across time and patellofemoral joint abnormalities. The results of the current study were derived from a mixed-sex cohort, and the proportions of male and female patients in each group were different. Knee biomechanics is affected by sex 12 ; therefore, our results may be different if stratified by patient sex. We reported on biomechanics in patients with bone–patellar tendon–bone grafts, which may be different from patients with other graft types, such as hamstring and quadriceps tendon autografts. Finally, we did not include healthy participants in the current study. As the ultimate goal of rehabilitation is to restore function and biomechanics as close to those of healthy people, further studies including healthy participants are needed for more in-depth understanding of the effect of limb dominance.
Conclusion
The results of our study provide evidence that the side of dominance that underwent ACLR had an impact on asymmetric biomechanical patterns, including peak PFJS, integrated PFJS, peak PFJRF, and peak KEM during gait at 12 weeks after ACLR. The ACL-D group had decreased knee joint loading in the surgical limb, while the ACL-ND group had increased knee joint loading in the surgical limb. Because mechanisms of developing patellofemoral joint abnormalities such as PFP and PFOA are not well understood, further work on the long-term effects of these altered biomechanics is needed to better understand the impact of the findings.
Footnotes
Final revision submitted January 4, 2022; accepted January 21, 2022.
One or more of the authors has declared the following potential conflict of interest or source of funding: S.B.S. has received education payments from Arthrex. L.N.D. has received education payments from Pylant Medical. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from the University of Texas Southwestern Medical Center (protocol No. STU-2019-1184).