Abstract
Background:
Considering the lengthy recovery and high recurrence risk after a hamstring injury, effective rehabilitation and accurate prognosis are fundamental to timely and safe return to play (RTP) for athletes.
Purpose:
To analyze methods of rehabilitation for acute proximal and muscular hamstring injuries and summarize prognostic factors associated with RTP.
Study Design:
Systematic review; Level of evidence, 4.
Methods:
In August 2020, MEDLINE, CINAHL, Cochrane Central Register of Controlled Trials, and SPORTDiscus were queried for studies examining management and factors affecting RTP after acute hamstring injury. Included were randomized controlled trials, cohort studies, case-control studies, and case series appraising treatment effects on RTP, reinjury rate, strength, flexibility, hamstrings-to-quadriceps ratio, or functional assessment, as well as studies associating clinical and magnetic resonance imaging factors with RTP. Risk of bias was assessed using the Cochrane Risk-of-Bias Tool for Randomized Trials or the Methodological Index for Non-Randomized Studies (MINORS).
Results:
Of 1289 identified articles, 75 were included. The comparative and noncomparative studies earned MINORS scores of 18.8 ± 1.3 and 11.4 ± 3.4, respectively, and 12 of the 17 randomized controlled trials exhibited low risk of bias. Collectively, studies of muscular injury included younger patients and a greater proportion of male athletes compared with studies of proximal injury. Surgery for proximal hamstring ruptures achieved superior outcomes to nonoperative treatment, whereas physiotherapy incorporating eccentric training, progressive agility, and trunk stabilization restored function and hastened RTP after muscular injuries. Platelet-rich plasma injection for muscular injury yielded inconsistent results. The following initial clinical findings were associated with delayed RTP: greater passive knee extension of the uninjured leg, greater knee extension peak torque angle, biceps femoris injury, greater pain at injury and initial examination, “popping” sound, bruising, and pain on resisted knee flexion. Imaging factors associated with delayed RTP included magnetic resonance imaging-positive injury, longer lesion relative to patient height, greater muscle/tendon involvement, complete central tendon or myotendinous junction rupture, and greater number of muscles injured.
Conclusion:
Surgery enabled earlier RTP and improved strength and flexibility for proximal hamstring injuries, while muscular injuries were effectively managed nonoperatively. Rehabilitation and athlete expectations may be managed by considering several suitable prognostic factors derived from initial clinical and imaging examination.
Hamstring injury is one of the most common injuries among athletes. 31 Athletes involved in activities requiring high-speed running 6,10 or stretching to extreme muscle lengths 7,8 are particularly subject to hamstring injury, which is classified according to location within the muscle complex, specific muscle(s) affected, severity, and chronicity. Because of the complex anatomic and biomechanical properties necessary to facilitate movement at both the hip and the knee, however, uniform assessment of hamstring injury epidemiology is challenging. 22 Determining whether the injury affects the proximal origin or muscle belly is an important first step to elucidating injury epidemiology, understanding clinical presentation, and identifying potential complications. Proximal hamstring injuries occur predominantly in middle-aged patients and are often more severe, 43 usually associated with prolonged convalescence and carrying greater risk for complications such as postoperative weakness and sciatic nerve injury. 13,81 Conversely, muscular injuries occur more commonly in younger male athletes with risk factors such as strength or flexibility deficits, and although initially milder than proximal injuries, there exists substantial risk for recurrent injury of greater severity. 32,67
Consideration of injury location is also important when determining clinical management. Although approach to rehabilitation is tailored according to injury location, severity, and patient goals of therapy, management generally includes physiotherapy ∥ with possible concomitant surgical intervention ¶ or injections of platelet-rich plasma (PRP). # Despite extensive research investigating methods of rehabilitation and advances in therapeutic techniques designed to return athletes to competition quickly while minimizing reinjury risk, 61,74 acute hamstring injury continues to account for significant absence from sports, and little consensus has been reached regarding optimal management strategies. Accurate prediction of time to return to play (RTP) is necessary to guide activity progression and manage patient expectations for recovery. Although clinicians often rely on clinical and structural factors gleaned from initial examination and magnetic resonance imaging (MRI) scans to inform their prognosis, whether these adequately correlate with recovery time remains a topic of debate.
The purpose of this study was to systematically review the literature concerning evidence-based management of acute proximal and muscular hamstring injuries in athletes and to report the baseline clinical and MRI factors associated with RTP.
Methods
Research Framework
The design and reporting of this systematic review are compliant with the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. 60
Eligibility Criteria
English-language articles examining management and factors affecting RTP after acute hamstring injury were considered for eligibility, and those meeting each of the following criteria were included: (1) the article employed a randomized controlled trial (RCT), cohort, case-control, or case series design; (2) patients had sustained acute proximal or muscular hamstring injury, defined as <6 weeks between injury and initial evaluation; (3) the authors investigated the effects of a well-described intervention on hamstring rehabilitation or associated baseline clinical or MRI assessment findings with RTP; and (4) outcome measures included time to RTP, reinjury rate, hamstring strength, hamstring range of motion (ROM), hamstrings-to-quadriceps (H:Q) ratio, or results of standardized functional assessment. Studies limited to only chronic tendinopathy or only recurrent hamstring injuries were excluded.
Information Sources and Search
Searches of MEDLINE (1966 to present), CINAHL (1981 to present), Cochrane Central Register of Controlled Trials (1996 to present), and SPORTDiscus (1949 to present) were conducted in August 2020. To identify articles pertinent to acute hamstring injury management and prognosis, a comprehensive search strategy was developed using applicable Medical Subject Headings terms and keywords (see Appendix Table A1). Subsequent manual inspection of included article reference lists ascertained any additional relevant articles not found via the computerized search.
Study Selection
Two reviewers (S.S.R. and M.P.K.)independently screened all articles on the basis of title and abstract using a specialized systematic review software (Covidence systematic review software; Veritas Health Innovation). Potentially eligible articles underwent full-text review prior to final determination of study inclusion. Any disagreements between reviewers were resolved via discussion.
Data Collection
Based on the Cochrane Handbook for Systematic Reviews of Interventions recommendations for data extraction, 28 a custom data extraction form was developed to collect information on study design; methods; population; intervention(s); and outcome measures, including time to RTP, reinjury rate, hamstring strength, hamstring ROM, H:Q ratio, and/or standardized functional assessment. All data were extracted by a single reviewer (S.S.R.) and verified by a second reviewer (M.P.K.).
Risk-of-Bias and Quality Assessment
A risk-of-bias assessment was performed for all included studies. RCTs were assessed using the Revised Cochrane Risk-of-Bias Tool for Randomized Trials, which appraises studies based on patient randomization, assignment to intervention, availability of outcome data, outcome measurement, and selection of reported results. 80 Overall risk of bias for each RCT was judged as “low,” “some concerns,” or “high.” Nonrandomized studies were assessed using the Methodological Index for Non-Randomized Studies (MINORS) tool. 79 The MINORS tool represents a 12-item assessment of methodological value, with 8 criteria indicated for noncomparative studies and an additional 4 criteria indicated for comparative studies. Each criterion was scored from 0 to 2, with higher overall scores indicating higher quality of evidence.
Statistical Analysis
Patient characteristics were quantified using descriptive statistics, calculated as weighted means and standard deviations across included studies. We used t tests to identify any differences in characteristics between patients with acute proximal and muscular hamstring injuries. A P value < .05 was used to determine statistical significance. Stata (Version 13.1; StataCorp) software was used for all statistical analyses.
Results
Study Selection
The database search retrieved 1704 articles, with an additional 22 identified via manual search as potentially relevant. After removing duplicates, 1289 articles were screened on the basis of title and abstract. A total of 126 articles were retained for full-text review, of which 51 were excluded for failure to satisfy the inclusion criteria, and 75 were included (Figure 1).
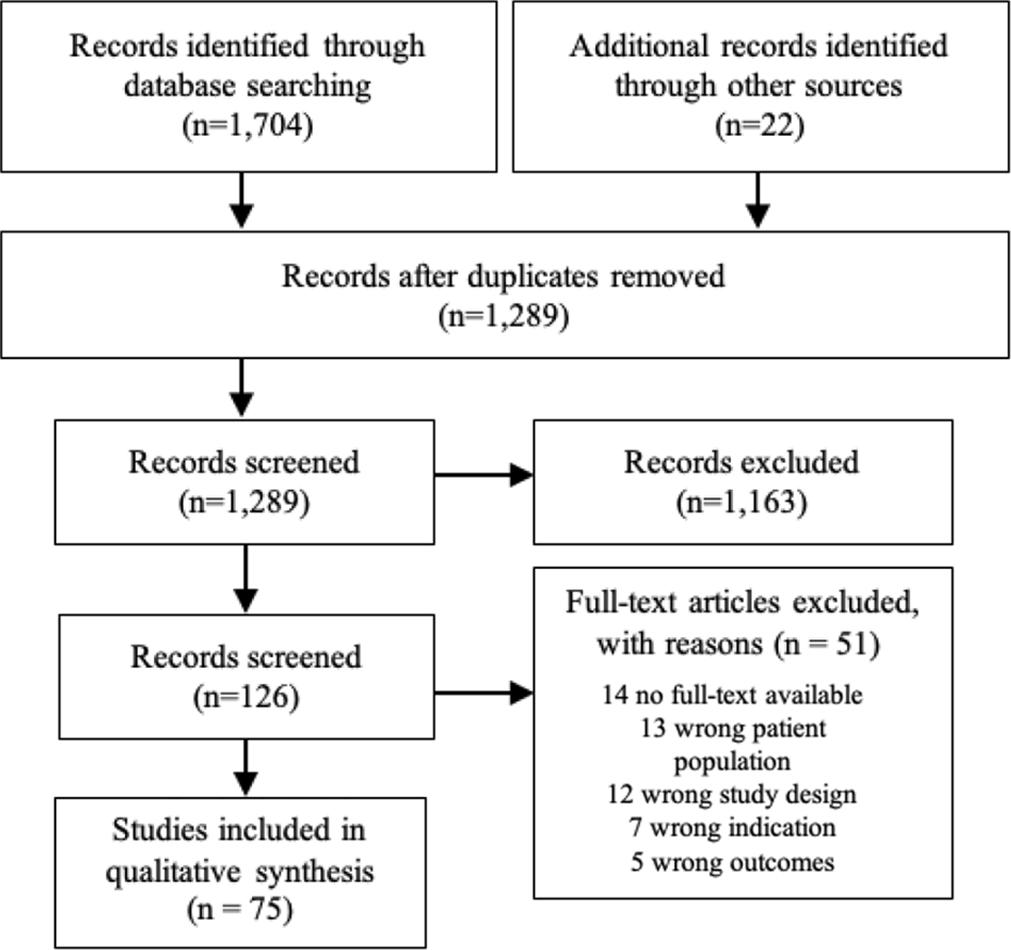
Study flowchart.
Study Characteristics
A total 45 of the included studies pertained to injury management,** 25 defined factors associated with RTP, †† and 5 integrated both. 1,9,10,45,76 Studies investigated 3 to 360 male and female athletes engaged in various sports of all competitive levels with a mean age of 14 to 58 years. Of the studies pertaining to injury management, 22 ‡‡ concerned injuries to the proximal origin, and 28 §§ were specific to muscular injuries. A variety of techniques and programs were assessed according to recovery time, reinjury risk, and degree of functional improvement, including surgical and nonsurgical treatment, ∥∥ PRP injection, ¶¶ and physiotherapeutic interventions. ## There was a lack of uniformity across studies regarding diagnostic methods, criteria for RTP, and assessment of outcomes. Prognostic studies determined whether baseline findings were correlated with time to RTP by conducting clinical and/or MRI assessment shortly after injury.
Of note, study samples were duplicated in a few articles. 5 –7,39,40,44,83,85 Specifically, injuries to the 18 sprinters and 15 dancers described in Askling et al 5 were also investigated separately in 2 other studies by the same authors. 6,7 Hamilton et al, 40 Jacobsen et al, 44 van der Made et al, 83 and Wangensteen et al 85 additionally shared considerable overlap in patient populations due to their use of pooled data from a prior RCT. 39
Risk-of-Bias Assessment
Seventeen RCTs were included, of which 12 were determined to present low risk of bias, a and 5 were judged to raise some concerns. 9,10,46,49,70 Nonrandomized studies comprised 11 comparative b and 47 noncomparative c designs with average scores of 18.8 ± 1.3 and 11.4 ± 3.4 on MINORS assessment, respectively.
Synthesis of Results
Patient Characteristics
Acute hamstring injuries were classified according to location within the muscle complex. Collectively, 775 patients with proximal hamstring injury and 1057 patients with muscular hamstring injury were assessed by the included studies. Studies investigating methods of proximal injury management generally included younger patients and a greater proportion of male patients compared with studies of proximal hamstring injury rehabilitation (Table 1).
Comparison of Patient Characteristics Between Studies of Proximal Versus Muscular Hamstring Injury a

a Bold values were statistically significantly different between groups (P < .05).
Management
Management of hamstring injury was also dependent upon localization to the proximal origin or muscle belly. Time to RTP and reinjury rate at final follow-up are listed according to intervention in Tables 2 to 4. Because of extensive variation in the methods of measuring and reporting hamstring strength, ROM, H:Q ratio, and functional assessment, individual study results for these outcomes are discussed in the text only and not presented in the tables.
Summary of Studies on Management of Acute Injuries to the Proximal Hamstring a

a Dashes indicate data not reported. H:Q, hamstrings-to-quadriceps ratio; IQR, interquartile range; MTJ, myotendinous junction; ROM, range of motion; RTP, return to play; X, outcome(s) reported.
b Reported as Methodological Index for Non-Randomized Studies score (maximum score).
Summary of Studies Managing Acute Muscular Hamstring Injury Using PRP or Autologous Conditioned Serum a

a Dashes indicate data not reported. BAMIC, British Athletics Muscle Injury Classification; IQR, interquartile range; PPP, platelet-poor plasma; PRP, platelet-rich plasma; ROM, range of motion; RTP, return to play; X, outcome(s) reported.
b Reported as Methodological Index for Non-Randomized Studies score (maximum score) for nonrandomized studies or Cochrane Risk-of-Bias Tool for Randomized Trials.
c Significant difference between interventions (P < .05).
Summary of Studies Managing Acute Injuries to Hamstring Muscle With Physiotherapy a
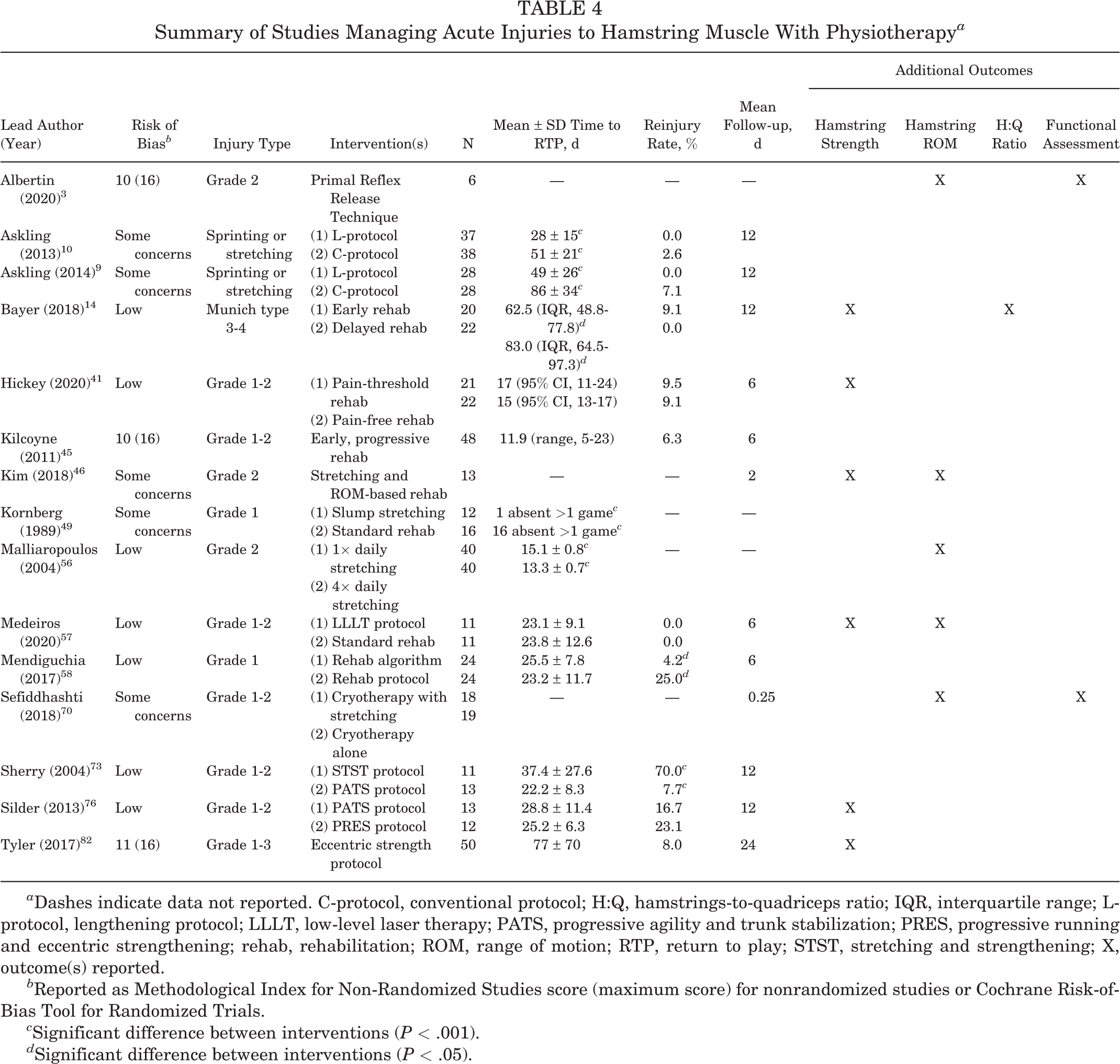
a Dashes indicate data not reported. C-protocol, conventional protocol; H:Q, hamstrings-to-quadriceps ratio; IQR, interquartile range; L-protocol, lengthening protocol; LLLT, low-level laser therapy; PATS, progressive agility and trunk stabilization; PRES, progressive running and eccentric strengthening; rehab, rehabilitation; ROM, range of motion; RTP, return to play; STST, stretching and strengthening; X, outcome(s) reported.
b Reported as Methodological Index for Non-Randomized Studies score (maximum score) for nonrandomized studies or Cochrane Risk-of-Bias Tool for Randomized Trials.
c Significant difference between interventions (P < .001).
d Significant difference between interventions (P < .05).
Proximal Injuries
To determine optimal treatment for acute proximal hamstring injuries, 22 studies investigated the efficacy of surgical and nonsurgical intervention ‡‡ (Table 2). When supplemented with postoperative rehabilitation, surgical repair for partial avulsion was associated with a high rate of RTP 13,51,87 and low levels of pain and functional limitation. 4,20,54,77 Piposar et al 62 found no differences in objective outcomes between operative and nonoperative management, although subjective results were superior after surgery. Satisfactory operative results were also observed in the context of complete avulsion, regardless of tendon retraction 19,48,52,81 or ischial tuberosity fracture. 17 Mean hamstring strength recovered to 78.0% to 94.6% within 12 months of surgery, and the rate of RTP surpassed 75%, 11,18,47,81 although up to 45% of patients reported decreased level of activity. 23,87 Two studies measuring hamstring ROM demonstrated >90% recovery within 12 months of surgical repair. 11,12 Functional outcomes did not differ by sex in any study except that by Chahal et al, 23 in which all 4 patients experiencing poor outcomes were female. Comparatively, nonoperative management of complete proximal avulsion resulted in noticeable strength deficits and lower functional scores. 42
Muscular Injuries
Management of acute muscular hamstring injury was the focus of 28 studies. Eleven studies evaluated the efficacy of autologous PRP d or autologous conditioned serum 88 injection using various injection volumes, locations, and frequencies (Table 3). Although 3 studies found patients receiving PRP achieved earlier RTP than controls by 10 to 15 days, 1,16,33 5 studies showed no such effect. 21,37,39,65,66 Despite finding no relationships between PRP injection and days or practices missed because of hamstring injury in National Football League athletes, Bradley et al 21 reported PRP injection to be associated with fewer games missed. Zanon et al 89 noted a decreased reinjury rate in patients receiving PRP in the short term; however, the long-term rate was not different from that of controls. None observed strength differences associated with PRP injection 1,39,66 except Gaballah et al, 33 who demonstrated a transient increase in strength 4 weeks after injection relative to controls that dissipated by week 8. Only Reurink et al 66 measured hamstring ROM and elucidated no effect of PRP injection on straight-leg raise or active knee extension ROM. None of the included studies concerning PRP or autologous conditioned serum injection reported the H:Q ratio or standardized functional assessment.
Physiotherapeutic programs for acute hamstring muscular injuries were assessed in 15 studies e (Table 4). Eccentric training enabled faster RTP for elite soccer 10 and track and field 9 athletes compared with conventional training regardless of whether the injury was of sprinting or stretching type. Reinjury rate did not differ between eccentric and conventional rehabilitation protocols. 9,10 However, athletes fully compliant with an eccentric training program experienced fewer reinjuries and reduced strength deficits compared with noncompliant patients. 82 Reinjury risk was further reduced via an individualized rehabilitation algorithm designed to address risk factors, although this approach resulted in possibly slower RTP. 58
Kim et al 46 found stretching and ROM exercises were effective in restoring passive ROM and reducing pain in athletes with grade 2 injury, but active ROM and strength were not improved. 46 Active ROM was increased by increasing the frequency of stretching from 1 to 4 daily sessions, however, as patients were quicker to normalize flexibility between injured and uninjured limbs and RTP. 56 Stretching after icing (“cryostretching”) yielded greater increases in active knee extension and lower extremity functional scale scores compared with icing alone. 70 A stretching and strengthening (STST) intervention was compared with progressive agility and trunk stabilization (PATS) by Sherry and Best, 73 who reported similar time to RTP between groups but a significantly greater reinjury rate in the 12 months after STST. Silder et al 76 compared a progressive running and eccentric strengthening program with PATS and found no benefit in RTP, reinjury risk, strength, or ROM. Notably, all 25 athletes in this study displayed residual injury markers on MRI scans at RTP, and half of those who experienced reinjury did so within 2 weeks.
Two studies demonstrated the benefit of early intervention. 45,14 After 24 hours of immobilization, a progressive rehabilitation program developed by Kilcoyne et al 45 returned patients with grade 1 to 2 injury to activity in an average of <2 weeks with a 6-month reinjury rate of 6.3%. Athletes who began physiotherapy 2 days after grade 3 to 4 injury achieved faster RTP than athletes beginning at 9 days, with no difference in reinjury rate within 1 year. 14 Peak hamstring strength was increased in the early group 13 weeks after injury, but this difference disappeared by 26 weeks. Both early and late groups exhibited decreased H:Q ratios compared with the uninjured leg. Hickey et al 41 determined that pain threshold—based rehabilitation failed to accelerate RTP or influence reinjury rate relative to pain-free therapy. However, isometric hamstring strength was 15% greater after 2 months of training in the pain-threshold group. The Primal Reflex Release Technique, a method of downregulating the autonomic nervous system to reset reflexes via reciprocal inhibition, was shown to significantly increase active and passive ROM as well as functional scores. 3 A neurologically based approach was also examined by Kornberg and Lew, 49 who reported that slump stretching resulted in fewer games missed after grade 2 injury in Australian Rules football players. Last, an RCT by Medeiros et al 57 investigating low-level laser therapy revealed no effect in any reported outcome measure.
Surgical intervention for muscular injury was examined in 2 studies. Lempainen et al 53 (MINORS score, 10/16) assessed outcomes of surgical repair for muscular injury with concomitant complete rupture of the central hamstring tendon, reporting RTP within 4 months and no reinjuries by 1 year for the 2 patients with nonrecurrent injury included in the study. In addition, Cooper and Conway 26 (MINORS score, 18/24) compared surgical and nonoperative treatments for complete distal semitendinosus rupture and found no difference in time to RTP. However, 42% of patients treated nonoperatively did not achieve acceptable results and required subsequent surgical intervention.
Prognostic Factors
Characteristics and findings of studies correlating baseline clinical and/or MRI findings with time to RTP are summarized in Tables 5 and 6.
Summary of Studies Assessing Prognostic Value of Baseline Assessment a
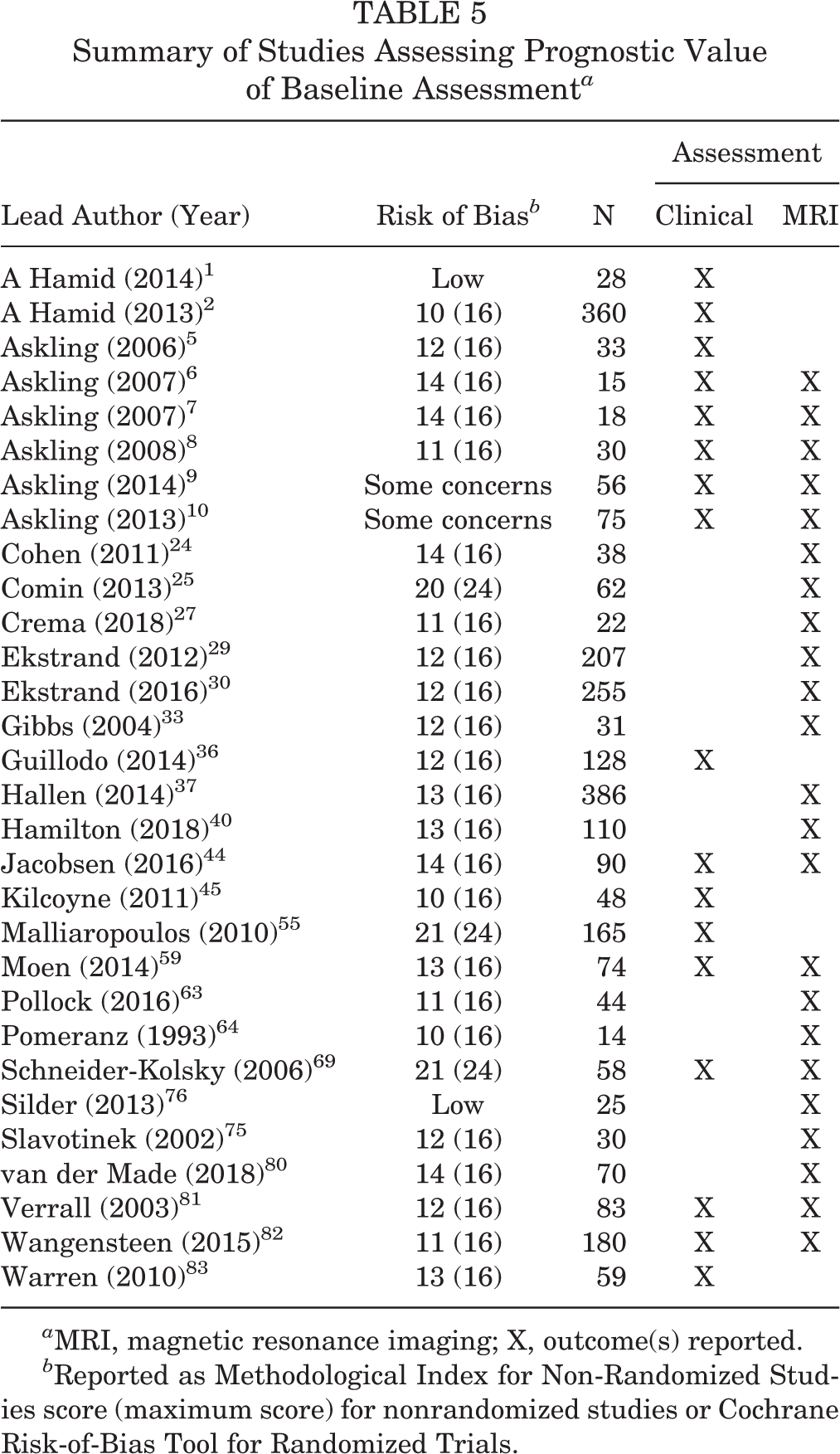
a MRI, magnetic resonance imaging; X, outcome(s) reported.
b Reported as Methodological Index for Non-Randomized Studies score (maximum score) for nonrandomized studies or Cochrane Risk-of-Bias Tool for Randomized Trials.
Baseline Assessment Findings and Prognostic Relationships With RTP Times a

a ACL, anterior cruciate ligament; BAMIC, British Athletics Muscle Injury Classification; CSA, cross-sectional area; MRI, magnetic resonance imaging; NSAID, nonsteroidal anti-inflammatory drug; PKE, passive knee extension; ROM, range of motion; RTP, return to play; SLR, straight-leg raise; VAS, visual analog scale.
Clinical Factors
Seventeen studies investigated relationships between clinical assessment findings and time to RTP f . Pain during outer-range strength testing, 44 greater midrange strength as a percentage of uninjured leg strength, 44 and shorter clinician-predicted recovery 69 were associated with accelerated RTP. In contrast, factors associated with delayed RTP included greater passive knee extension of the uninjured leg, 44 greater peak torque angle in knee extension, 44 injury to the biceps femoris, 69 greater maximum pain at injury, 44,85 worst visual analog scale (VAS) pain score >6, 36 higher VAS pain score at initial examination, 84 popping sound at injury, 36 bruising, 36 pain on resisted knee flexion, 85 and longer clinician- 69,84 and self-predicted time to RTP. 59 Several examined factors had contradictory results across studies. Two studies by Askling et al 5,10 noted stretching-type injuries took longer to recover than did sprinting-type ones, while others found injury mechanism to have no effect on recovery time. 2,44,59,85,86 There was no consensus regarding the effect on time to RTP for sex, 2,45 injury grade, 2,45,69 physiotherapy attendance, 1,2,44 hip ROM, 5,44,59,86 number of days to walk pain-free, 44,59,86 history of ipsilateral or contralateral lower limb injury, 1,2,44,45,59,85,86 craniocaudal length of pain, 1,6,7,44,59,85 need to cease activity within 5 minutes of injury, 44,85 level of play, 2,8,59 or active knee extension deficit. 1,36,55,59,86
MRI Factors
Twenty-three studies evaluated the role of MRI in predicting time to RTP. g Accelerated RTP was associated with MRI-negative injury, 9,10,34,38,64 lower percentage of muscle/tendon involvement, 24 and shorter radiologist-predicted recovery. 69 Conversely, the following were associated with prolonged recovery time: MRI-positive injury, 84 greater normalized length of lesion, 34 greater percentage of muscle/tendon involvement, 24 complete tendinous/myotendinous rupture, 63,64 complete central tendon disruption, 25,83 central tendon waviness, 83 greater number of muscles involved, 40 and longer radiologist-predicted recovery. 69 Studies reported conflicting results for injury grade, 24,29,30,38,59,63,85 length, h width, 6,7,30,44 depth, 6,7,30 cross-sectional area, 6,27,34,44,59,64,69,78 volume, 6,7,27,44,59,78 tendon involvement, 6,9,10,24,30,44 amount of tendon retraction, 24,83 site of injury within the muscle, 6,24,30,63,64,78 presence of extramuscular fluid, 59,64 distance from ischium, 6 –10,44,59,85 and the Cohen MRI score. 24,40 Of note, the Cohen MRI score refers to an assessment tool designed to evaluate hamstring injuries on the basis of patient age, muscles involved, injury location, extent of injury, and retraction. 24
Discussion
This review assessed management of acute proximal and muscular hamstring injuries by reviewing interventions and prognostic factors associated with RTP. According to the literature, patients undergoing surgical treatment for partial or complete proximal hamstring ruptures achieved consistently better outcomes compared with those managed nonoperatively. 11,12,15,19,68 For patients with acute muscular injuries, physiotherapy incorporating eccentric training 9,10,82 and PATS 73,76 attained favorable outcomes in time to RTP, reinjury rate, and restoration of strength. Stretching-based protocols increased ROM but failed to reduce reinjury risk or improve strength. 46,56,73 Supported by findings that rehabilitation with pain-threshold limits does not predispose to adverse effects, 41 early initiation of rehabilitation enabled faster RTP. 14,45 Slump stretching 49 and reflexive release techniques 3 also offered functional benefit by addressing neurological components of hamstring strain. Regarding the efficacy of PRP injection, results were inconclusive, confounded by a lack of standardization in PRP formulation and injection protocol. Similar inconsistencies have been reported in recent meta-analyses, 35,61,71,75 emphasizing the need to determine the optimal injection protocol for standard use in future research investigating the effect of PRP on time to RTP. Overall, although the quality of evidence of included studies varied, the diverse methods and predictive factors examined warrant consideration by clinicians seeking to optimize injury recovery.
Studies quantifying the prognostic value of baseline assessments have indicated that certain clinical and MRI findings are correlated with time to RTP. Clinical factors associated with accelerated RTP included lesser deficit in strength of the injured leg relative to the uninjured leg 44 and shorter physician-predicted recovery time, 69 whereas prolonged time to RTP was observed in patients with greater pain, 36,44,84,85 injury to the biceps femoris, 69 and longer physician- 69,84 and self-predicted 59 recovery times. It is possible that patients with greater strength and decreased pain in the injured leg at baseline may be able to begin physiotherapeutic activity and facilitate rehabilitation sooner after injury, resulting in earlier RTP. On MRI scans, findings indicating greater injury severity at initial presentation, such as greater lesion size, 24,34,84 tendinous/myotendinous rupture, 25,63,64,83 and greater number of muscles affected, 40 were correlated with prolonged RTP. Despite associations of initial examination and MRI findings with time to RTP, accurate prognostication of recovery time remains difficult. In a multivariate analysis of 180 patients, Wangensteen et al 85 determined that a single clinical examination at initial presentation accounted for 29% of variance in time to RTP, whereas supplementation with MRI findings explained only an additional 2.8%. Jacobsen et al 44 likewise reported that 59.0% and 8.6% of variance in RTP was accounted for by clinical and MRI examination, respectively, suggesting the added benefit of MRI findings in prognosticating RTP is less pronounced.
This study has several important limitations. First, the strength of any systematic review is dependent upon the quality of evidence of included studies. This review included 17 RCTs, of which 5 were determined as raising “some concerns” on risk-of-bias assessment. The remaining 58 studies consisted of cohort, case-control, and case series study designs included in an effort to be comprehensive in evaluating rehabilitative techniques. When critically appraised, comparative nonrandomized studies achieved a mean MINORS score of 18.8 ± 1.3, and noncomparative nonrandomized studies achieved a score of 11.4 ± 3.4. These scores indicate a reasonable risk of bias and are mainly attributable to a lack of prospective data collection, blinding, and/or prospective calculation of sample size. Differences in study design, patient population, and outcome measures limited direct comparisons between studies and precluded data pooling for meta-analyses, making it difficult to draw concrete conclusions in circumstances of conflicting results. This was particularly apparent when analyzing the efficacy of PRP injection for treatment of hamstring muscular injury, as studies varied in terms of volume, location, and number of injections. With regard to studies examining the prognostic value of clinical and MRI examination, the majority conducted only univariate analyses correlating baseline findings with RTP. Furthermore, criteria for RTP and methods of functional assessment were inconsistent, likely explaining some of the variance in time to RTP across studies. Future large-scale research using standardized RTP criteria and outcome measures are required to determine reliable associations between baseline findings and RTP prognosis via multivariate analysis.
Conclusion
Surgical intervention offers substantial benefits over nonoperative care for treatment of acute partial and complete proximal hamstring ruptures, while muscular injuries are effectively treated with physiotherapy encompassing eccentric training and PATS. The efficacy of PRP, however, remains controversial. Prognostication of RTP is of great importance, and the ability to accurately predict recovery time can be improved with a thorough clinical examination shortly after injury. Although the added benefit may be limited, structural factors observed on MRI scans can also inform RTP prognosis. Future high-quality research evaluating novel therapeutic protocols and prognostic determinants of RTP is needed to further enhance rehabilitation and better predict recovery timelines for athletes with acute hamstring injury.
Footnotes
Final revision submitted July 5, 2021; accepted August 10, 2021.
One or more of the authors has declared the following potential conflict of interest or source of funding: Funding was provided by the Conine Family Fund for Joint Preservation. S.D.M. has received education payments from Kairos Surgical and honoraria from Allergan. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Notes
APPENDIX
Search Strategy

| MEDLINE (Ovid) |
|
Exp Hamstring muscles/ ((hamstring* or (biceps adj2 femoris) or semimembranosus or semitendinosus or thigh or (posterior adj2 thigh)) not ACL not cruciate).tw, kw 1 or 2 Exp “Wounds and Injuries”/ Exp “Sprains and Strains”/ Exp Pain/ (injur* or (leg adj2 injur*) or (sports adj2 injur*) or (athletic adj2 injur*) or strain* or sprain* or tear* or ruptur* or trauma* or pain* or dysfunction*).tw, kw 4 or 5 or 6 or 7 Exp Therapeutics/ Exp Rehabilitation/ Exp Diagnostic Imaging/ (therap* or rehab* or manag* or interven* or imag*).tw, kw 9 or 10 or 11 or 12 or 13 Exp “Recovery of Function”/ Exp Sports Medicine/ (recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participation” or “return to training” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participation” or “return-to-training”).tw, kw (re-occur* or recur* or reoccur* or re-inj* or reinj*).tw, kw 14 or 15 or 16 or 17 3 and 8 and 13 and 18 Limit 19 to (English language and full text) Limit 20 to MEDLINE |
|
|
|
(MH “hamstring muscles” OR MH thigh OR TI ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh))) OR AB ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh)))) NOT TI ACL NOT TI cruciate MH (“Wounds and Injuries”) OR MH (“Sprains and Strains”) OR MH “Pain” or TI ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) OR AB ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) MH Therapeutics OR MH Rehabilitation OR MH “Diagnostic Imaging” OR TI ((therap* or rehab* or manag* or interven* or imag*)) OR AB ((therap* or rehab* or manag* or interven* or imag*)) MH “Recovery of Function” OR MH “Sports Medicine” OR TI ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) OR AB ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) S1 AND S2 AND S3 AND S4 Narrow by language – English Limiters – full text |
|
|
|
(MH “hamstring muscles” OR MH thigh OR TI ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh))) OR AB ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh)))) NOT TI ACL NOT TI cruciate MH (“Wounds and Injuries”) OR MH (“Sprains and Strains”) OR MH “Pain” or TI ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) OR AB ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) MH Therapeutics OR MH Rehabilitation OR MH “Diagnostic Imaging” OR TI ((therap* or rehab* or manag* or interven* or imag*)) OR AB ((therap* or rehab* or manag* or interven* or imag*)) MH “Recovery of Function” OR MH “Sports Medicine” OR TI ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) OR AB ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) S1 AND S2 AND S3 AND S4 Narrow by language – English |
|
|
|
(MH “hamstring muscles” OR MH thigh OR TI ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh))) OR AB ((hamstring* or (biceps N2 femoris) or semimembranosus or semitendinosus or thigh or (posterior N2 thigh)))) NOT TI ACL NOT TI cruciate MH (“Wounds and Injuries”) OR MH (“Sprains and Strains”) OR MH “Pain” or TI ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) OR AB ((injur* or (leg N2 injur*) or (sports N2 injur*) or (athletic N2 injur*) or strain* or sprain* or tear* or rupture* or trauma* or pain* or dysfunction*)) MH Therapeutics OR MH Rehabilitation OR MH “Diagnostic Imaging” OR TI ((therap* or rehab* or manag* or interven* or imag*)) OR AB ((therap* or rehab* or manag* or interven* or imag*)) MH “Recovery of Function” OR MH “Sports Medicine” OR TI ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) OR AB ((recover* or progress* or convalescen* or outcome* or “return to play” or “return to sport” or “return to competition” or “return to participat*” or “return to train*” or “return-to-play” or “return-to-sport” or “return-to-competition” or “return-to-participat*” or “return-to-train*”)) S1 AND S2 AND S3 AND S4 Narrow by Language – English Limiters – Full Text |
