Abstract
Background:
Overweight and obesity are increasingly prevalent among HIV-infected populations. We describe their prevalence and associated risk factors among HIV-infected adults in Dar es Salaam, Tanzania.
Methods:
A cross-sectional study was conducted to determine the proportion of patients who were overweight or obese at enrollment to care and treatment centres from 2004 to 2011. Multivariate relative risk regression models were fit to identify risk factors.
Results:
A total of 53 825 patients were included in the analysis. In all, 16% of women and 8% of men were overweight, while 7% and 2% were obese, respectively. In multivariate analyses, older age, higher CD4 count, higher hemoglobin levels, female sex, and being married were associated with obesity and overweight. World Health Organization HIV disease stage, tuberculosis history, and previous antiretroviral therapy were inversely associated with obesity and overweight.
Conclusion:
Overweight and obesity were highly prevalent among HIV-infected patients. Screening for overweight and obesity and focused interventions should be integrated into HIV care.
Keywords
Introduction
The prevalence of overweight (body mass index [BMI] 25 to <30 kg/m2) and obesity (BMI ≥ 30kg/m2) is an increasingly important public health concern in sub-Saharan Africa, especially in urban areas. 1 In Tanzania, overweight and obesity were previously associated with persons with diabetes and high-ranking executives; however, these conditions are becoming more common in the general population. 2,3 In the decade from 1995 to 2004, the prevalence of obesity among women attending antenatal clinics in Dar es Salaam, an urban center, increased from 3.6% to 9.1%. 4 The Tanzania Demographic and Health Surveys (TDHS) similarly show an increase in the nationwide prevalence of overweight and obesity, from 18% in 2004/2005 to 22% in 2010. 5,6 In 2010, the prevalence of overweight and obesity in Dar es Salaam was 28.1% and 16.4%, respectively, double and triple the national figures. 6 Recent changes in Tanzanians’ lifestyles, including migration to urban areas, an increasingly Western-style diet, and a shift away from manual work, are associated with overweight and obesity. 7,8 Social perceptions, such as the belief that overweight is symbolic of health and beauty, also contribute to the increasing prevalence of overweight and obesity. Furthermore, some Tanzanians believe that overweight is a sign of not being infected with HIV. 9 –11 Such beliefs contribute to a preference of overweight and obesity over normal weight.
Obesity is associated with metabolic abnormalities including insulin resistance, 8 dyslipidemia, 8,12 and kidney disease, 13 which can lead to chronic diseases such as hypertension, 14 diabetes, 15 cardiovascular disease, 16,17 and some cancers. 18 Although obesity is the underlying cause of several chronic diseases and imposes an economic burden to individuals and to Tanzania as a whole, 19 limited resources are available to address the condition and associated consequences.
Obesity is relatively common among people infected with HIV, 20,21 a disease once defined by “wasting” and “slimming.” 22 Recent studies have reported a high prevalence of obesity among antiretroviral therapy (ART)-naive populations 23 in both developed 24 –26 and developing 27 countries, including Tanzania. 28 Some authors have projected that the proportion of patients on ART who are overweight or obese will soon be similar to or higher than that of the general population. 26,27 As in the general population, overweight and obesity have been found to be associated with hypertension and dyslipidemia, risk factors for cardiovascular diseases. 24,27,29
There are limited published studies on the prevalence and predictors of overweight and obesity among HIV-infected adults in Tanzania. Most previous studies were composed of small samples and compared overweight and obese participants to nonoverweight and nonobese participants, which included underweight rather than only normal-weight participants. 23,25,26,29,30 We conducted a study of participants in care and treatment centres (CTCs) to describe the prevalence of overweight and obesity in HIV-infected patients and compared overweight and obese participants to normal-weight participants to identify factors associated with overweight and obesity at CTC enrollment.
Methods
Study Site and Population
This cross-sectional study uses data on HIV-infected patients who enrolled in HIV/AIDS CTCs in Dar es Salaam, Tanzania, between November 2004 and December 2011. These CTCs were supported by Management and Development for Health (MDH), one of the recipients of the US President’s Emergency Plan for AIDS Relief. All nonpregnant patients aged 15 years and older whose weight and height were recorded at program enrollment were included.
Standard practice dictates that all patients attending MDH-supported HIV CTCs receive comprehensive care and support per Tanzanian national guidelines. 31
Data Collection
Physicians and nurses at the CTCs complete standard forms to record demographic, clinical, laboratory, and medication information. Weight and height are measured using standardized protocols, which include measuring height to the nearest 0.1 cm using a stadiometer and weight to the nearest 0.1 kg on a calibrated scale. 32 Clinical data collected include history of tuberculosis (TB) and medication data collected include previous use of ART. Laboratory data collected include CD4 count and hemoglobin. All patients are referred for general nutrition education provided by a trained nurse counselor and nutrition counseling provided by the nutritionist. Additional sessions of nutrition counseling and therapeutic food are provided to those undernourished until they graduate from malnutrition. Clinical and laboratory data are entered into a national standard case report form, reviewed at site level for accuracy and completeness, and then entered into a protected computerized database which is updated daily and undergoes weekly quality assurance audits.
The study protocol was approved by the Institutional Review Boards of the National Institute of Medical Research, Muhimbili University of Health and Allied Sciences, and the Harvard School of Public Health.
Outcomes and Risk Factors
The primary outcome in this cross-sectional study was the prevalence of overweight or obesity at enrollment. Normal weight was defined as 18.5 to <25 kg/m2, overweight as 25 to <30 kg/m2, and obese as ≥30 kg/m2. For each risk factor studied, two comparisons were made: overweight versus normal weight and obese versus normal weight. 32
We examined the following potential baseline risk factors for overweight and obesity: age, sex, marital status, parity, functional status (categorized as confined to bed, limited ambulation, or able to work), CD4 count, World Health Organization (WHO) HIV staging, hemoglobin concentration, previous ART use, and history of TB at enrollment. We also assessed the relationships between overweight or obesity and opportunistic infections (diarrhea, oral candidiasis, and other AIDS-defining illnesses).
Statistical Analyses
A total of 90 118 patients aged 15 years and older were enrolled in the MDH program between 2004 and 2011. We excluded 36 293 patients, because of pregnancy (11 674), missing height or weight (3998), or being underweight (20 621; BMI < 18.5 kg/m2).
Chi-square tests were used to test for differences in the prevalence of obesity and overweight by potential risk factors. Univariate and multivariate relative risk models were used to assess the associations between overweight and obesity compared to normal weight (18.5 kg/m2 ≤ BMI < 25.0 kg/m2) and baseline risk factors. 33 Log-binomial regression was used for all univariate regressions. Poisson regression was used for the multivariate regressions because the multivariate log-binomial regressions did not converge. All variables in the univariate analyses were included in the multivariate models. We used the missing indicator method and set continuous variables to the mean value for missing covariates. Wald tests were calculated for median scores of categorical variables and for binary variables. Based on known differences in the proportion of and risk factors for overweight and obesity between men and women, we tested for an interaction between sex and each risk factor associated with overweight and obesity.
We examined the possibly nonlinear relation between age and CD4 count with the relative risks of obesity and overweight nonparametrically with restricted cubic splines. 34 All analyses were performed using SAS software version 9.3 (SAS Institute, Inc, Cary, North Carolina). P values less than .05 were considered statistically significant.
Results
Demographic characteristics of the 53 825 patients included in the analyses are shown in Table 1. Among the patients, 69% were female, the median age was 35 years (interquartile range [IQR], 30–42 years), and the median BMI was 22 (IQR 20–25 kg/m2). The female and male patients who were overweight was 16% and 8% and obese was 7% and 2%, respectively.
Baseline characteristics of the study population.a

Abbreviations: BMI, body mass index; Hgb, hemoglobin; TB, tuberculosis; WHO, World Health Organization.
aN = 53 825.
bExcept where otherwise noted, data represent n (%) of patients.
cNot all numbers add up to 53 825 because of missing data.
dChi-square test.
Associations between individual risk factors and obesity are reported in Table 2. Compared to the reference group (<30 years), patients aged 30–40 years, 40–50 years, and those aged 50 and older had 2.12 (95% confidence interval [CI], 1.93–2.32), 3.19 (95% CI, 2.90–3.51) and 3.62 (95% CI, 3.22–4.06) times the risk of being obese (trend test P value <.001). The prevalence of obesity was 4-fold higher in women than in men, that is, in women with no children, the prevalence ratio (PR) was 4.39 (95% CI, 3.97–4.87); in women with 1 child the PR was 4.38 (95% CI, 3.93–4.88); in women with 2 children the PR was 4.20 (95% CI, 3.73–4.74); and in women with 3 or more children the PR was 3.98 (95% CI, 3.50–4.51). Relative to patients with CD4 counts greater than 200 cells/mm3, patients with CD4 counts between 50 and 99 cells/mm3 had a reduced risk of obesity (PR, 0.64; 95% CI, 0.56–0.72). Lower hemoglobin concentrations were associated with a lower risk of obesity. Compared to patients with normal hemoglobin concentrations (>11 g/dL), patients with hemoglobin concentrations of <8.5 g/dL were less likely to be obese (PR, 0.32; 95% CI, 0.27–0.37). The risk of being obese was lower in patients diagnosed with WHO stage IV compared to those with stage I disease (PR, 0.28; 95% CI, 0.24–0.32). History of TB was associated with a decreased risk of obesity (PR, 0.70; 95% CI, 0.62–0.78).
Risk Factors for Obesity (BMI ≥ 30) among Obese and Normal-Weight Patients Enrolled for Care and Monitoring at MDH-PEPFAR-Supported Facilities in Dar es Salaam, Tanzania.a

Abbreviations: BMI, body mass index; CI, confidence interval; Hgb, hemoglobin; PR, prevalence ratio; TB, tuberculosis; WHO, World Health Organization; MDH, Management and Development for Health; PEPFAR, President’s Emergency Plan for AIDS Relief.
aN = 43 986.
bWald test for trend for median scores of categorical variables. Wald test for binary variables.
Older age, female sex, being married, higher CD4 count, higher hemoglobin levels, lower WHO stage, no history of TB at enrollment, and history of antiretroviral (ARV) drug use were found to be risk factors for overweight after adjustment for covariates (Table 3). Relative to patients aged <30, patients aged 30–40, 40–50, and those aged 50 and older had 1.31 (95% CI, 1.25–1.38), 1.73 (95% CI, 1.64–1.82), and 1.86 (95% CI, 1.74–1.99) times the risk of being overweight. The prevalence of overweight was twice as high in women compared to men: 2.05 (95% CI, 1.95–2.16) in women with no children, 2.13 (95% CI, 2.02–2.25) in women with 1 child, 2.07 (95% CI, 1.94–2.29) in women with 2 children, and 1.87 (95% CI, 1.73–2.01) in women with 3 or more children. High CD4 counts were associated with a high risk of overweight, while lower hemoglobin concentrations were associated with a lower risk of overweight. Compared to patients with CD4 counts greater than 200 cells/mm3, patients with CD4 counts between 50 and 99 cells/mm3 had a reduced risk of overweight (PR, 0.84; 95% CI, 0.79–0.90). Compared to patients with normal hemoglobin concentrations (>11 g/dL), patients with hemoglobin concentrations of <8.5 g/dL were less likely to be overweight (PR, 0.53; 95% CI, 0.49–0.57). The risk of being obese was lower in patients diagnosed with WHO stage IV than in those with stage I disease (PR, 0.47; 95% CI, 0.43–0.51). History of TB at enrollment was associated with a decreased risk of overweight (PR, 0.82; 95% CI, 0.77–0.87) and history of previous ARV medication use was associated with increased risk of overweight (PR, 1.12; 95% CI, 1.06–1.18).
Risk Factors for Overweight (25≤ BMI < 30) among Overweight and Normal-Weight Patients Enrolled for Care and Monitoring at MDH-PEPFAR-Supported facilities in Dar es Salaam, Tanzania.a

Abbreviations: BMI, body mass index; CI, confidence interval; Hgb, hemoglobin; RR, risk ratio; TB, tuberculosis; WHO, World Health Organization; MDH, Management and Development for Health; PEPFAR, President’s Emergency Plan for AIDS Relief.
aN = 49 982.
bWald test for trend for median scores of categorical variables. Wald test for binary variables.
Sex modified the association between the following risk factors and overweight and obesity: age (obese, P = .0002; overweight, P < .0001), marital status (obese, P < .0001; overweight, P < .0001), and WHO stage (obese, P < .0001; overweight, P = .0001). Married men were more likely to be obese (PR, 1.68; 95%CI, 1.37–2.05) and more likely to be overweight (PR, 1.47; 95% CI, 1.34–1.60) than men who were not married. The association between marital status and weight was weaker in women. Married women were more likely to be obese (PR, 1.09; 95% CI, 1.02–1.16) and overweight (PR, 1.05; 95%CI, 1.01–1.10) than unmarried women.
In both men and women, the risk of being overweight decreased significantly with higher WHO stage. Compared to men with WHO stage I, the risk of being overweight in men with WHO stage II was lower (PR, 0.72; 95% CI, 0.65–0.80) as was the risk in men with WHO stage IV (PR, 0.44; 95% CI, 0.37–0.53). Compared to women with WHO stage I, women with WHO stage II were less likely to be overweight (PR, 0.82; 95% CI, 0.78–0.87) as were women with WHO stage IV (PR, 0.48; 95% CI, 0.43–0.52; P for trend<.0001).
The relative risk curves for overweight and obesity by age (Figure 1) show that the risks of both overweight and obesity reach a maximum point in the mid-50s and then decline. The curves for overweight and obesity by CD4 count (Figure 2) show that the risks of both overweight and obesity increase rapidly up to approximately 500 cells/mm3 and then continue to increase but at a lower rate.

Multivariate relative risks and 95% confidence intervals (CIs) of overweight (25 ≤ BMI < 30) and obesity (BMI ≥ 30) as a function of age (years); 95% CIs are indicated by the gray area.
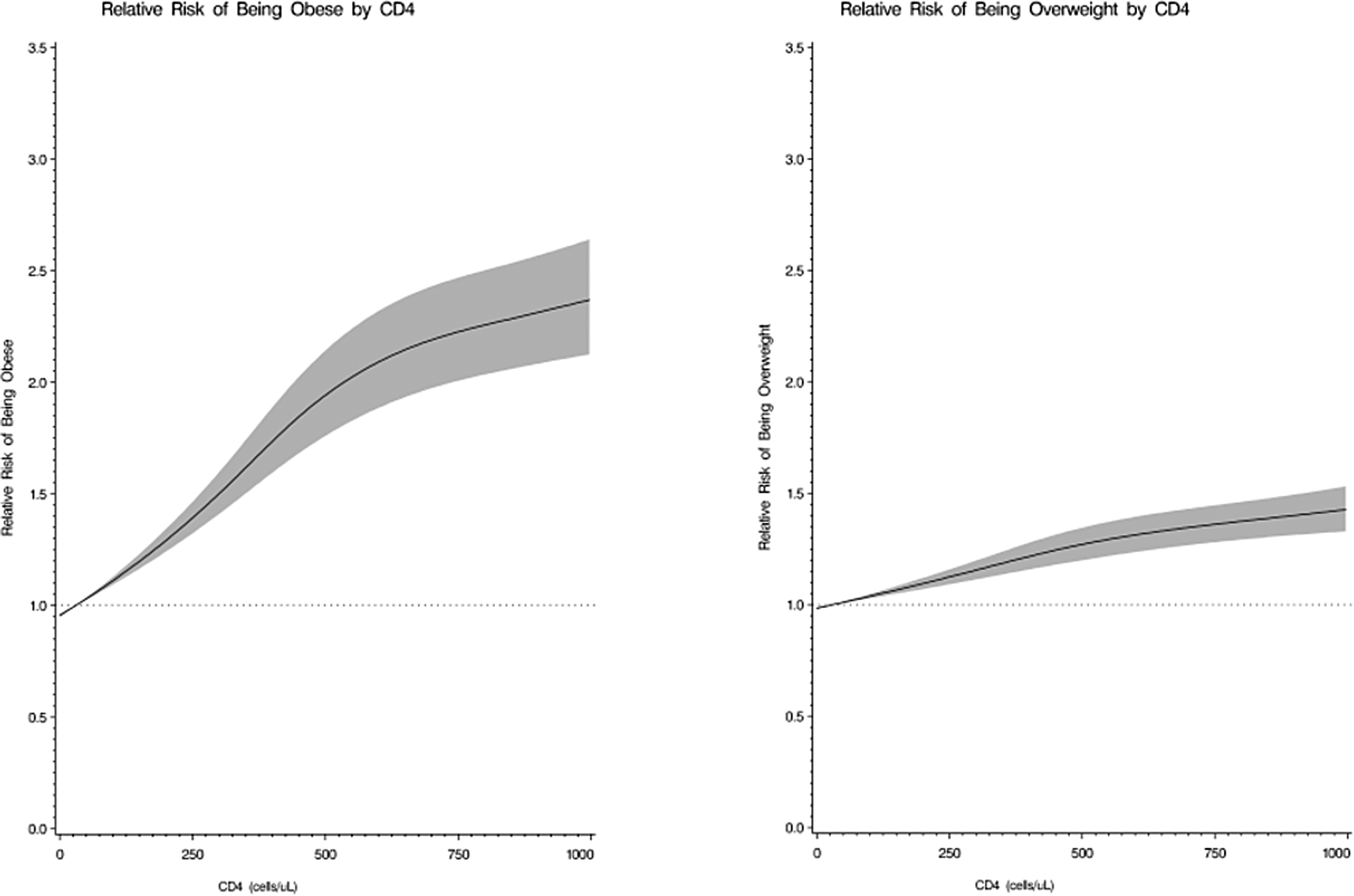
Multivariate relative risks and 95% confidence intervals (CIs) of overweight (25 ≤ BMI < 30) and obesity (BMI ≥ 30) as a function of CD4 count (cells/mm3); 95% CIs are indicated by the gray area.
Discussion
This article identifies risk factors for overweight and obesity and describes their prevalence among adult HIV-infected patients in Dar es Salaam. This is the first study to report on overweight and obesity among people infected with HIV at enrollment to CTCs in Tanzania. It is also the first study of this population that excluded underweight participants from the reference group when looking at predictors of overweight and obesity. Exclusion of underweight patients from the reference group was important to identify factors associated with being overweight or obese compared to a healthy weight, and we did not want our findings to be potentially distorted by underweight caused by the HIV disease process itself.
Our data suggest 4 major findings. First, there was a substantial proportion of people infected with HIV who were overweight or obese at enrollment to the CTCs. We found that 8% of male patients and 16% of female patients were overweight, while 2% of male patients and 7% of female patients were obese. These numbers are approximately 10 percentage points below the prevalence of overweight and obesity of the general population, based on comparisons to data from the 2010 TDHS, which reported a prevalence of 28% and 16% of overweight and obesity, respectively, among women aged 15–49 years, in Dar es Salaam. 6 A comparison of our results with a study conducted in the Kinondoni district, Dar es Salaam, in 2007–2008 found that the prevalence of obesity in HIV-infected men was 7.2 percentage points lower than that in the general population (1.8% versus 9%). 35
It is worth considering that the prevalence of overweight and obesity among HIV-infected people in Dar es Salaam may be higher than that observed by us. Our patients’ nutritional status was measured at the time of enrollment to the CTC. We did not have data on reasons for enrollment at that particular time. Persistent and frequent sickness could have compromised individuals’ nutrition and weight and led to CTC enrollment. It is important to monitor the BMI in patients after ART initiation, as patients’ health hopefully improves and they potentially gain weight. Furthermore, our study was limited to government-supported facilities where the majority of patients were of low socioeconomic status. In Dar es Salaam, the prevalence of overweight and obesity is higher among the middle and upper classes compared to the poor, and thus our population may have reflected the lower weights among the poor. 6,35
A high prevalence of obesity at the time of enrollment in HIV clinics, at levels comparable to the general population, has been noted in the United States. 23 –25,36 Our study adds evidence that, in Tanzania where wasting and underweight remain highly prevalent in the HIV-infected population, the prevalence of obesity among people infected with HIV at CTC enrollment is high but lower than that of general population. 37,38
Second, we observed that overweight and obesity were more prevalent in older patients, with the oldest age-group (>50 years) having the highest burden. A similar trend has been observed in the general Dar es Salaam population where the highest prevalence of obesity was among those aged 45–55 and slightly lower in those aged 55+. 35 A study from the United States found a similar relationship between age and weight at HIV diagnosis. 24 The relative risk curves of overweight and obesity reache a maximum point in the mid-50s and then declines.
Third, this study builds on previous findings that, as in the general population, overweight and obesity among people infected with HIV is more prevalent in women than in men. 24 –26,29,30 However, this result conflicts with other data where no association was found between BMI and sex. A study of HIV-infected US military personnel found no association between sex and BMI, and a study of HIV-infected patients in Philadelphia found that the prevalence of obesity, but not overweight, was higher in women than in men. 24,26 In our study, the prevalence of overweight and obesity in women was double and triple that of men at the time of enrollment in the HIV CTC. A number of factors could contribute to these differences. In the general Dar es Salaam population, men are less likely than women to be overweight and obese. 35 Among those infected with HIV in sub-Saharan Africa, men tend to begin care later than women. 39,40 This delay may mean that by the time men begin care, they would have lost more weight than have women. This weight loss could be due to inadequate intake of food, malabsorption, frequent infection, or other, as of yet unknown, biological or physiological factors. We found that parity was inversely associated with overweight and obesity in women. Similar findings have been observed in the general population. 41
As in the general population, we found that overweight and obesity among people infected with HIV were significantly more common among the married. Married men were more likely to be overweight or obese than single men, but the association with marital status was not significant in women. This could partly be explained by the cultural differences in food consumption between men and women; household food distribution often favors men, and men are more likely to eat out regularly. It is also possible that women are likely to take adequate care of themselves whether they are married or not, while for men, marriage makes more of a difference. Married men may receive more care and food from their wives while unmarried men don’t have this advantage.
In Tanzania, excess weight continues to be perceived as a status symbol, a sign of being HIV free, and an indicator of good health. 11 Unless countrywide interventions and educational campaigns on obesity and associated consequences are implemented, overweight will continue to be perceived as a symbol of a properly cared for family and of beauty, especially among women. 11,42
Fourth, the prevalence of overweight and obesity at enrollment was significantly higher among those with the highest category of CD4 count. Similar to other studies in general and in HIV-infected population prior to ART initiation, we found that being overweight or obese was associated with higher CD4 count. 25,36,43 Our study found that overweight and obesity were more prevalent among the patients with higher CD4 counts. Other studies have reported that higher baseline BMI predicts greater gain in CD4 count, including maintenance of immune status and better recovery when patients initiated ART. 25,36,44
Although higher enrollment weight is associated with higher CD4 counts, this observation may be moderated by known associations of excess weight and negative health consequences. 45,46 Excess weight in HIV-infected patients has the potential to exacerbate higher rates of cardiovascular disease seen in HIV-infected patients who receive certain ART medications. 47 Thus, although nutritional status in HIV-infected patients may reflect larger national secular trends in obesity, specific obesity-related health issues require attention in HIV-infected patients.
Conclusion
The adverse health consequences of overweight and obesity are well described in the general population. 8,12 –16,18 In this study, we examined patients at enrollment to HIV CTCs in Dar es Salaam, Tanzania, and found that overweight and obesity were highly prevalent, although not as high as that found in the general population. Targeted dietary counseling and weight management should be integral components of care given to people infected with HIV.
Footnotes
Acknowledgement
We thank the Ministry of Health and Social Welfare (MOHSW) for their support in integrating HIV CTCs in Dar es Salaam. We also thank the MDH and all the patients and staff who have contributed to these findings.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This HIV intervention program in Dar es Salaam government facilities is funded by United States President’s Emergency Plan for AIDS Relief through Management and Development for Health in collaboration with the Ministry of Health and Social Welfare and the Harvard School of Public Health. RMZ is supported by a NIH T32 CA 09001 training grant.
