Abstract
Tracheobronchopathia osteochondroplastica (TPO) is a rare, benign condition characterized by the presence of submucosal cartilaginous and osseous nodules protruding into the anterior and lateral walls of the tracheobronchial lumen, sparing the posterior membranous wall. These nodules are incidentally discovered on imaging and bronchoscopy performed for unrelated respiratory symptoms. The exact etiopathogenesis is unclear, with various hypotheses proposed. The most widely accepted one is that chronic inflammation leads to cartilaginous and osseous metaplasia of the tracheobronchial submucosa. TPO is rare, with the prevalence further underestimated due to the incidental nature of the diagnosis. Clinically, patients may be asymptomatic or can have nonspecific symptoms such as chronic cough, dyspnea, and recurrent respiratory infections. Suspicion of the diagnosis arises upon incidental identification of nodules in the tracheobronchial lumen. Diagnosis is established through bronchoscopic visualization of characteristic nodular lesions sparing the posterior wall and can be confirmed by histopathologic examination showing submucosal cartilage formation and ossification. Management is generally conservative, focusing on symptomatic relief and treatment of infections. Severe cases with significant airway obstruction may warrant advanced bronchoscopic procedures or surgical interventions. Despite its benign nature, TPO can mimic other serious tracheal diseases. Awareness of this condition is essential for accurate diagnosis and appropriate management. We present a case of a 65-year-old asymptomatic chronic smoker who was found to have tracheal nodules on thoracic imaging. Bronchoscopic evaluation was consistent with TPO, with histopathology reaffirming the diagnosis.
Keywords
Introduction
Tracheobronchopathia osteochondroplastica (TPO) is a rare, benign condition characterized by the presence of submucosal cartilaginous and osseous nodules protruding into the anterior and lateral walls of the tracheobronchial lumen. Sparing of the posterior membranous wall is pathognomonic for this condition, distinguishing it from other tracheal diseases. 1 It is an uncommon condition identified incidentally in asymptomatic patients during thoracic imaging performed for other reasons or during bronchoscopy evaluation in patients presenting with chronic respiratory symptoms. Despite its benign course, the progressive growth of the nodules into the lumen can lead to significant airway obstruction, often raising an alarm due to its resemblance to malignant pulmonary processes. We present a case of an asymptomatic, chronic smoker who was found to have incidental endotracheal nodules on imaging performed for lung cancer screening, leading to a bronchoscopic evaluation and histopathologic evaluation confirming the diagnosis of TPO. Awareness of TPO among clinicians is crucial to prevent misdiagnosis and avoid unnecessary interventions.
Case Presentation
A 64-year-old female with a medical history significant for coronary artery disease, hyperlipidemia, and patent foramen ovale was referred to a pulmonologist for an evaluation of abnormal imaging findings. The patient was an active smoker with a 25-pack-year smoking history. Due to her age and extensive smoking history, she underwent low-dose computed tomography (LDCT) of the chest as part of lung cancer screening. She had no respiratory symptoms, including dyspnea, cough, hemoptysis, chest pain, or wheezing. She also denied palpitations, fevers, chills, or weight loss. While no nodules were identified in the lung parenchyma, the LDCT revealed nodular lesions within the lumen of the trachea, particularly in the anterior and lateral walls (Figure 1).

CT chest showing nodular lesions in the anterior and lateral walls of the trachea. CT, computed tomography.
Given the uncertain nature of the findings hinting at a broad differential diagnosis, a flexible bronchoscopic evaluation was performed to obtain a tissue diagnosis. Visualization by flexible bronchoscopy revealed multiple nodules protruding into the lumen from the anterior and lateral walls of the trachea, sparing the posterior wall (Figure 2). The findings were consistent with a diagnosis of TPO.
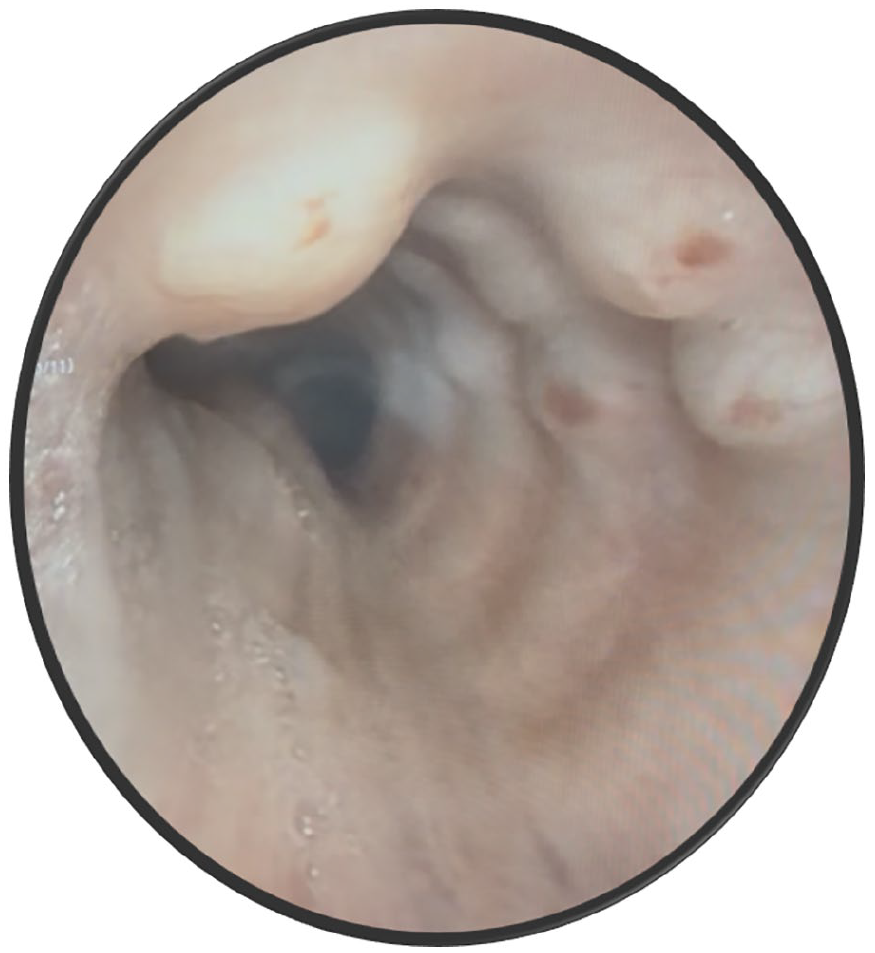
Bronchoscopic visualization revealing nodular appearance sparing the posterior wall of the trachea.
Endotracheal biopsies of the nodules revealed multiple benign fragments of hyaline cartilage, some associated with detached subepithelial stroma and benign respiratory epithelium on histopathologic examination (Figure 3). Additionally, intact fragments of unremarkable benign respiratory mucosa were identified. These findings further confirmed the diagnosis of TPO.

Histopathologic examination of endobronchial biopsies. (A) Benign hyaline cartilage fragments (red arrow), with adjacent detached subepithelial stroma and benign respiratory epithelial cells (asterisk). (B) Another section showing fragments of cartilaginous (red arrow) and osseous tissues (blue arrow).
The patient was reassured about the benign nature of these findings. As she had no respiratory symptoms, she did not require any further intervention or symptomatic management. Though the patient was initially concerned about malignancy on discovering the tracheal nodules, she expressed relief upon confirmation of the benign findings. Given her long smoking history, she was strongly advised to quit smoking and was referred to a smoking cessation program for support.
Discussion
TPO is an extremely rare condition with an estimated incidence of 0.11%. 2 However, its true prevalence is likely underestimated, as most cases are diagnosed incidentally in asymptomatic individuals. Although TPO can occur in younger patients, TPO is more commonly reported between the fourth and seventh decades of life, with no known gender predilection. 3 It is estimated that only 51% of the cases are predicted to be diagnosed within the patient’s lifetime. 4
The exact pathogenesis remains unclear, though several hypotheses have been proposed over the years. The most widely accepted hypothesis is that chronic inflammation and mechanical irritation of the tracheobronchial mucosa may trigger submucosal mesenchymal metaplasia into osteoblasts or chondrocytes, leading to ossification and cartilage formation. 3 Chronic smoking or long-term exposure to environmental or occupational pollutants like industrial dusts, chemicals can harbor conditions to trigger the submucosal mesenchymal metaplasia. Lesions typically arise in areas where the respiratory epithelium is thinned or absent, suggesting epithelial injury plays a role in disease development. The posterior membranous wall is typically spared, likely due to its distinct structural and embryological characteristics. 5 Degenerative changes in the tracheal cartilage due to local tissue ischemia or chronic damage may lead to dystrophic calcification, resulting in the formation of tracheobronchial nodules. 6 Other proposed mechanisms that are considered to have a role include developmental abnormalities of the tracheal cartilage, possible genetic predisposition, and the role of bone morphogenetic protein 2. 7
TPO is often asymptomatic or may present with nonspecific respiratory symptoms depending on the location and extent of the lesions. When symptomatic, patients can have chronic dry cough due to airway mucosal irritation, 8 exertional dyspnea due to partial airway obstruction, or mild hemoptysis. 9 Patients may also experience recurrent respiratory tract infections due to impaired mucociliary clearance. 9 Stridor and wheezing suggest severe narrowing of the airway. Voice changes are very rare and usually occur when proximal trachea or laryngeal structures are involved. Due to the nonspecific nature of the symptoms, patients are frequently misdiagnosed as having asthma, chronic obstructive pulmonary disease (COPD), bronchitis, etc, delaying appropriate diagnosis and management.
Radiographic findings are frequently overlooked and can be quite subtle. Chest X-rays are typically normal, but can reveal tracheal narrowing or signs of infection. CT of the chest typically reveals nodularity involving the anterior and lateral walls of the tracheobronchial tree, with characteristic sparing of the posterior membranous wall. 10 CT is also helpful to define the extent of stenosis if present and also identify complications such as postobstructive pneumonia, atelectasis, or bronchiectasis. A chest magnetic resonance imaging (MRI) scan may reveal intermediate signal intensity of widespread irregular thickening of the trachea and central bronchi, and punctiform low-signal intensity suggesting calcifications with no contrast enhancement. 11 Pulmonary function tests may be normal, or an obstructive pattern may be noted, especially in symptomatic patients. 12 Variable or fixed obstruction can be seen on flow-volume loops.
Bronchoscopy remains the gold standard for the diagnosis of TPO. A direct bronchoscopic visualization reveals a nodular, whitish or yellowish lesion projecting into the airway lumen. The hallmark feature remains the sparing of the posterior tracheal wall. 12 A histopathologic examination is not always required, as the classic appearance with posterior wall sparing is diagnostic of TPO, differentiating it from tracheal amyloidosis, tracheobronchial papillomatosis, relapsing polychondritis, malignancy, etc. Due to the ossification and calcification, it may sometimes be difficult to obtain a biopsy of the lesions. 12 Microscopically, TPO is characterized by the presence of ectopic submucosal cartilaginous and osseous nodules with the overlying epithelium intact, differentiating it from malignant and ulcerative lesions. 10 Zhu et al. have proposed a staging system for TPO based on the bronchoscopic and histopathologic examination (Table 1). 13
Staging of tracheobronchopathia osteochondroplastica.

There is no standardized treatment for TPO. Since the most accepted hypothesis suggests that chronic inflammation is the main trigger, avoidance of airway irritants remains the cornerstone of management. Smokers should be counseled regarding smoking cessation. Occupational exposures should be limited with the appropriate use of personal protective equipment, including face masks. Asymptomatic patients are managed with observation and periodic follow-up. Manageemnt is primarily symptomatic. Bronchodilators, inhaled corticosteroids, and antitussives are commonly used to relieve mild symptoms. Antibiotics are considered for secondary infections. 4 Efficacy is uncertain regarding the use of systemic corticosteroids. Difficult airway should be anticipated with adequate preparation, should intubation be required. 14 Surgical intervention is rare and is reserved for severe cases. In severely symptomatic patients and those with significant airway narrowing, endoscopic interventions such as mechanical debulking, laser ablation with (Holmium: YAG or Nd: YAG laser photoevaporation), or stenting may be necessary. Resection of the affected tracheal segment, or partial laryngectomy, may be considered depending on the extent of airway involvement. 3
Depending on the location and size of the nodular lesions, the prognosis is generally excellent due to the benign nature and slow progression of the disease. 3 Most patients remain stable for a prolonged period, with an indolent course. However, over time, significant airway narrowing can occur, leading to respiratory compromise and recurrent infections, necessitating the need for long-term follow-up. Although considered a benign condition with a generally favorable prognosis, some studies have noted a seemingly higher incidence of lung cancer among patients with TPO. In one such study, lung cancer was observed in 15 out of 40 patients (37.5%) diagnosed with TPO. 15 However, this association may be incidental rather than causal. A likely explanation is that TPO was identified incidentally during bronchoscopic evaluation performed for suspected or confirmed lung malignancy. Supporting this, Leske et al. found no significant link between TPO and an increased risk of malignant disease, suggesting that any observed association is coincidental rather than pathophysiologically related. 5
Although our patient did not have significant respiratory symptoms, the incidental finding of endotracheal nodules caused considerable anxiety and concern for the possibility of malignancy, especially since the imaging was performed for lung cancer screening. This highlights the psychological burden such findings can have on patients until histopathological confirmation rules out cancer. In this case, the biopsy confirmed the diagnosis of TPO, a benign condition, providng substantial relief to the patient. However, given her status as an active smoker, continued patient education remained crucial. She was counseled that while TPO is not malignant, ongoing airway inflammation from tobacco exposure could potentially exacerbate the condition. Smoking cessation was strongly advised as part of the long-term management plan.
Conclusion
TPO remains a rare and frequently overlooked condition that should be considered in the differential diagnosis of patients presenting with chronic cough, or vague respiratory symptoms, unexplained airway abnormalities, or pulmonary nodules. In this case, the identification of characteristic endobronchial lesions through bronchoscopy was key to reaching the correct diagnosis and avoiding more invasive procedures. A thorough understanding of the disease’s progression, from early inflammatory changes to significant airway remodeling leading to obstruction, can aid clinicians in recognizing and managing this entity more effectively. Although benign, findings such as TPO lesions can still lead to significant patient anxiety; clinicians should provide reassurance once malignancy is ruled out and emphasize modifiable risk factors such as smoking that may influence disease progression. With increased awareness and careful bronchoscopic evaluation, TPO can be diagnosed earlier, potentially improving patient outcomes, and reducing unnecessary diagnostic workups.
Footnotes
Acknowledgements
None.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Verbal informed consent was obtained from the patient for their anonymized information to be published in this article.
