Abstract
This case report presents a rare instance of solitary endobronchial plasmacytoma in a 58-year-old male, who had progressively worsening shortness of breath and a productive cough. The patient, who had a smoking history, was found to have a large, hypervascular mass completely obstructing the right main bronchus, confirmed as a plasma cell tumor via endoscopic biopsy. Further diagnostic imaging, including positron emission tomography-computed tomography (PET-CT) and chest CT, revealed a mass measuring 1.7 cm with abnormal fluorodeoxyglucose (FDG) uptake. The bone marrow biopsy ruled out multiple myeloma. The patient underwent challenging endoscopic debulking of the tumor, although margins were not well defined due to its size. Post-operatively, the patient showed significant symptomatic improvement and was discharged home on post-operative day 4. Two months after the procedure, follow-up with a chest CT scan and bronchoscopy showed no evidence of residual tumor or local recurrence, and the patient reported significant respiratory improvement. The literature review revealed that extramedullary plasmacytoma (EMP) is uncommon and often occurs in the upper aerodigestive tract. The diagnostic workup generally involves histopathological analysis, bronchoscopy, and imaging studies. Treatment is tailored to the patient’s condition and the characteristics of the tumor. This case underscores the need for a high index of suspicion and comprehensive diagnostic evaluation of patients presenting with obstructive bronchial mass. Furthermore, it highlights the importance of considering endobronchial plasmacytoma in the differential diagnosis of obstructive bronchial masses and the value of early intervention in achieving favorable outcomes. Regular follow-up is crucial to monitor recurrence and ensure ongoing patient well-being.
Introduction
Extramedullary plasmacytoma (EMP) is a type of plasma cell tumor that originates from mucosal plasma cells. 1 It may be associated with chronic irritation caused by chemicals or viral infections.1,2 The EMP accounts for approximately 3% of all plasma cell tumors, with an incidence in the United States (2003-2016) of 0.09 per 100 000 people.3,4 It commonly occurs in the elderly, with an average age of 55 years and predominantly affects males, with a 3:1 male-to-female ratio. 1
The EMP commonly occurs in the aerodigestive tract in about 80% of the cases. However, it can also occur in the gastrointestinal tract, breast, testis, skin, and lungs, 2 and it is referred to as primary pulmonary plasmacytoma (PPP).
The PPP is considered an extremely rare tumor 5 and can originate from different parts of the airway, such as the trachea, bronchi, or pulmonary parenchyma. Patients typically present with nonspecific symptoms related to tumor size and location, such as dyspnea, cough, and hemoptysis.6,7 The literature on endobronchial plasmacytoma is limited, with few reported cases. Surgical resection is often the first-line treatment approach. In addition, radiotherapy has a role in the treatment of some cases either as an adjunct or as a standalone treatment. 5
In this report, we present a case of a 58-year-old male diagnosed with endobronchial plasmacytoma who presented with respiratory distress and oxygen desaturation, which was successfully resected endoscopically with no evidence of local recurrence on follow-up. This case report has been reported in line with the CARE (CAse REport) reporting guidelines. 8
Case Presentation
A 58-year-old male patient, a heavy smoker (approximately 2 packs per day), who had quit smoking 3 months ago. The patient was referred to our hospital by clinicians from another facility. His condition worsened en route, prompting an emergency evaluation upon arrival. He presented with severe respiratory distress, and desaturation down to 60’s with minimal effort outside the hospital; his main presenting complaint was shortness of breath (SOB) for the last 6 months, which was progressive in course, occurs at a small distance, increases by lying down and on exertion, relieved by rest, and associated with productive cough containing whitish sputum. There was no history of other complaints or other symptoms in his systemic review, such as weight loss, hemoptysis, hematemesis, pleuritic chest pain, hoarseness, decreased oral intake, abdominal pain, or arthralgia. The patient had no other past medical conditions or any previous surgeries, and he did not take any previous medications with no known drug or food allergies. According to the patient, there’s no known cancer history in his family, or other inherited disorders.
The patient was initially suspected of having allergic rhinitis and was treated accordingly, but he did not improve and his symptoms became more severe. Given the significant SOB and progressive respiratory deterioration, the patient admitted had an urgent bronchoscopy to identify the cause of his symptoms.
On admission, the patient’s vital signs were as follows: SPO2:85% on room air; temperature (axillary): 36.5°C; blood pressure: 132/64 mm Hg; pulse: 67 bpm; and pain score 2/10. Oxygen support of 3 L per minute was provided, raising his SPO2 to 96%. The patient’s physical examination revealed a well-appearing man, with decreased air entry on the right side and good air entry on the left side with vesicular breathing, no added sound, and no murmur; the reminder of the physical examination was unremarkable. Laboratory results showed a slight increase of white blood cell (WBC) count to 11 290 per microliter (normal range = 4500 to 11 000 per microliter); his other blood tests, serum electrolytes (sodium, potassium, chloride), liver and kidney function tests were within normal ranges. In addition, the patient’s serum free light chain (FLC) ratio was tested as part of the initial workup, and the results did not show a significant elevation, remaining well below the threshold of 100 that would indicate multiple myeloma (MM). A chest radiography was done and showed no obvious abnormalities.
Further imaging contrast-enhanced chest computed tomography (CT) showed a well-defined smoothly marginated, enhancing mass lesion seen at the right main bronchus at the level of carina, causing a complete obstruction in the intraluminal space of the right main bronchus; the axial view showed how the tumor was extended and partially obstructing the trachea (Figure 1A-D).

(A) Axial view chest computed tomography (CT), revealed a marginated enhancing mass obstructing the right main bronchus just below the carina. (B) Axial view CT (lung window), showing the tumor was extending and partially obstructing the trachea at the level of the carina*. (C) Coronal view CT (lung window), showing the tumor completely obstructing the right main bronchus and protruding into the main carina*. (D) Sagittal view CT (lung window), showing the tumor is completely obstructing the bronchial wall*. *Notice the motion artifact explained by the severe respiratory distress of the patient.
Urgent bronchoscopy revealed a normal nasal cavity, vocal cords, larynx, trachea, carina, and left bronchial tree. However, a large, well-defined, rounded, hypervascular mass was observed in the right main bronchus, completely occluding the airway. The mass was well defined, rounded, mobile with respiration, and hypervascularized that easily bleed with manipulation (Figure 2), after irrigation with cold normal saline and adrenaline, a biopsy was attempted, multiple fragments of grayish tissue measuring 3 × 2 × 1 cm in aggregate were obtained, in which they received in formalin, but the mass started to bleed, a suitable controlling measure was applied with intermittent cold saline irrigation, diluted adrenaline, and with intravenous (IV) and local tranexamic acid (Hexacarbon). A post-procedure chest radiography was performed and showed no pneumothorax.
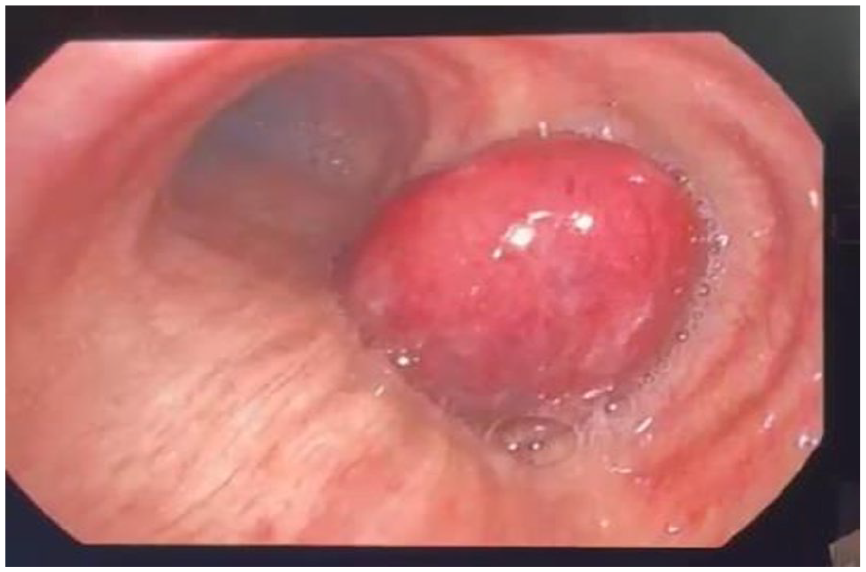
Fiberoptic bronchoscopy revealed a protruding huge endobronchial mass in the right main bronchus.
Given the presence of an endobronchial mass, a differential diagnosis of lipoma, leiomyoma, carcinoma, and secondary malignant metastasis was suspected. The biopsy results revealed that it is a plasmacytoma, kappa restricted, and the tumor is composed of sheets of mature and immature plasma cells that are positive for CD138 and Kappa immunostaining and negative for lambda immunostaining. Therefore, a correlation with bone marrow biopsy was recommended to rollout MM, which was subsequently excluded. The bone marrow biopsy showed no evidence of clonal plasma cells, confirming the absence of MM. No minimal marrow involvement (<10%) was identified either, supporting the diagnosis of a solitary plasmacytoma. In addition, the workup included SPEP, quantitative immunoglobulins, and serum FLC assays, all of which were within normal limits, further reinforcing the exclusion of multiple myeloma.
Although cytogenetic testing, fluorescence in situ hybridization (FISH), and immunotyping were not performed during the bone marrow biopsy due to the negative results of the initial workup and lack of clinical signs of systemic disease, we agree that these tests could have provided additional information. However, the negative bone marrow biopsy and absence of clonal plasma cells supported our diagnosis of an isolated plasmacytoma.
To further assess the mass’s localization, extension, and spread, the patient underwent positron emission tomography-computed tomography scan (PET-CT), which showed evidence of endocranial soft tissue mass protrusion from the right posterior-lateral wall, demonstrating abnormal fluorodeoxyglucose (FDG) uptake, measure 1.7 cm in the longest axis diameter (LAD) with a maximum standardized uptake value (SUVmax) of 8.7.
Following diagnosis, the patient underwent endoscopic maximum debulking and complete removal of the endobronchial tumor by our thoracic surgeon in the operation room. The procedure was challenging due to the inability to identify clear mass margins, necessitating endoscopic division of the tumor using the hot snare prior to removal because of its large size. The tumor was removed endoscopically with the use of both the rigid and the flexible bronchoscopy, and using the hot snare and the biopsy forceps, complete removal of the tumor was confirmed, and hemostasis was achieved using the cold saline and local adrenaline. Postoperatively, he was transferred to the surgical intensive care unit (SICU) for observation and kept fasting (NPO—Nothing by Mouth) on the first postoperative day; he gradually resumed an oral diet and tolerated it without nausea or vomiting. The next day, the patient was transferred to the surgical ward; the patient showed significant respiratory symptoms improvement, and he was discharged home on postoperative day 4.
One poor prognostic factor that should be mentioned is the advanced age of the patient (58 years old). However, at 2 months of follow-up, the patient reported significant improvement in symptoms, including SOB and easy fatigability. The patient underwent CT with contrast on follow-up, which showed both lungs appear normal without evidence of masses, no significant hilar, or mediastinal lymph node enlargement (Figure 3).

Axial (right) and coronal (left) views of chest CT with IV contrast revealed both lungs appear normal without evidence of masses with no hilar or mediastinal lymph node enlargements.
Discussion
Extramedullary plasmacytoma is an uncommon plasma cell tumor condition that affects organs outside the bone marrow. Involvement of the endobronchial area is uncommon, with potential involvement of the trachea, mainstem bronchi, or more distal airway structures. Most of the pulmonary plasmacytomas are treated surgically, with radiation therapy, or by palliative bronchoscopic interventions. 5 In this case report, we describe a solitary endobronchial plasmacytoma detected in a 58-year-old male that is maximally debulked by bronchoscopy with no evidence of recurrence.
A review of the literature on EMP reveals that it occurs predominantly in males aged 40 to 77 years old. The site of EMP occurs predominantly in the upper aerodigestive tract (UADT). The therapeutic options for the treatment of EMP include radiation therapy alone used in 44.3% of cases, surgery and radiation in 26.9% of cases, and surgical intervention alone in 21.9%. For patients who underwent surgery and radiation, the median survival rate was greater than 300 months; comparing to patients who underwent surgery alone, the median survival was 156 months; and who underwent radiation alone, the median survival was 144 months. Overall, the rate for the patients who were treated for EMP in the UADT, 61.1% of them had no recurrence or multiple myeloma; 22.0% had a recurrence; and 16.1% had a conversion to MM. 9 Our case was discussed in a multidisciplinary team including an oncologist, hemato-oncologist, radiation oncologist, pathologist, and thoracic surgeon; the decision was to follow the patient up closely with no need for adjuvant radiation at this point, providing the complete removal of the tumor, and to keep the radiation option for any future local recurrence.
This case presents a primary endobronchial plasmacytoma, in which the patient presented to our hospital with rare complaints, severe respiratory symptoms and distress, and desaturation down to 60’s with minimal effort. An urgent bronchoscopy and further workup were performed to decide the treatment plan because of his progressive SOB and location of the mass in the bronchus. Bronchoscopy showed huge endobronchial mass with complete obstruction of the right main bronchus. The subsequent biopsy confirmed the presence of a plasma cell tumor. Therefore, it is important to consider endobronchial plasmacytomas in the differential diagnosis of an endobronchial mass.
Diagnosis of EMP requires a comprehensive workup, including radiological studies, bronchoscopy, and histopathological examination. Treatment options are different and depend on the patient’s condition and health status; it includes surgery or radiotherapy, which considers as a valid option for elderly patients. Careful monitoring and regular follow-up are essential to detect possible recurrence and ensure optimal patient outcomes.
Conclusion
In this case report, we presented a rare instance of solitary endobronchial plasmacytoma in a 58-year-old male, characterized by complete airway obstruction and progressive respiratory symptoms. This case highlights the importance of considering endobronchial plasmacytoma in the differential diagnosis of endobronchial masses, especially in patients with obstructive symptoms and no other identifiable etiologies.
The successful management of this patient with an endoscopic tumor resulting in significant improvement in respiratory symptoms underscores the efficacy of surgical intervention in such cases. Given the rarity of endobronchial plasmacytoma and its potential for severe clinical presentation, it is crucial for clinicians to maintain a high index of suspicion and conduct thorough diagnostic evaluations including bronchoscopy, imaging studies, and histopathological analysis. The favorable outcomes observed in this patient suggest that early diagnosis and intervention are key to effective management. Regular follow-up is essential to monitor recurrence or progression, ensuring continued patient well-being and a timely response to any emerging issues.
Footnotes
Acknowledgements
The completion of this case could not have been possible without the participation and assistance of many people whose names may not be enumerated like our patient’s parents; their contribution is sincerely appreciated and gratefully acknowledged.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
