Abstract
Introduction
In 2007, Hseih et al
4
investigated 122 patients with culture-proven bacterial brain abscess in a retrospective study and discovered that
Case Presentation
A 62-year-old male with a history of hypertension, paroxysmal atrial fibrillation on rivaroxaban, and obstructive sleep apnea on home continuous positive airway pressure (CPAP) presented to an outside hospital with frontal lobe headaches, left-sided vision loss, and nausea for 1 week. He also endorsed a 2-month history of fevers, night sweats, generalized weakness, and 40-pound weight loss. Computed tomography (CT) head showed a 2.4-cm right occipito-parietal mass which led to transfer to our hospital for urgent neurosurgical evaluation. On admission, initial vital signs were stable with temperature of 37.7°C, heart rate 92 bpm, blood pressure 131/86 mm Hg, and respiratory rate of 22 breaths/minute on room air. Lab tests were significant for a white blood cell (WBC) count of 10 100/mm3, hemoglobin of 12.2 g/dL, platelet count of 262 000/mm3, creatinine of 0.63 mg/dL, lactic acid of 0.8 mmol/L, Hgb A1c of 5.4%, erythrocyte sedimentation rate (ESR) of 130 mm/h, c-reactive protein (CRP) of 18.925 mg/dL, and HIV antigen/antibody nonreactive (Figure 1). Magnetic resonance imaging (MRI) brain confirmed a right parietal-occipital lobe abscess with vasogenic edema (Figure 2A). Levetiracetam was initiated for seizure prophylaxis and broad-spectrum antibiotics (vancomycin, ceftriaxone, and metronidazole) were started. The neurosurgery service performed a right parietal burr hole for stereotactic biopsy and drainage. His cerebral abscess cultures grew

Initial laboratory tests.

(A) MRI brain with and without IV contrast showing a right parietal-occipatal lobe brain abscess (red arrow) with vasogenic edema (orange arrow). (B) MRI brain with and without IV contrast showing post-surgical changes and edema (red arrow) at the right parietal burr hole without evidence of residual right parietal-occipital brain abscess.

Gram stain from brain abscess showing thin fusiform gram-negative rods.
Given his night sweats and weight loss, additional imaging was obtained to rule out malignancy or other sites of infection. The CT scans of the chest, abdomen, and pelvis identified a colovesical fistula extending from the sigmoid colon into the bladder dome, an intramural bladder wall abscess (2 × 2.5 cm), and 2 focal liver lesions. General surgery and urology deferred surgical intervention in the absence of active gastrointestinal issues or voiding dysfunction and recommended outpatient follow-up with cystoscopy and colonoscopy. The MRI liver imaging confirmed 2 sizable intrahepatic abscesses, each 5 cm in size (Figure 4). An infective endocarditis workup was initiated, and a transthoracic echocardiogram (TTE) showed thickening of the noncoronary cusp on the aortic valve. Follow-up transesophageal echocardiogram (TEE) detected a 1-cm mobile vegetation on the aortic valve (Figure 5A). Interventional radiology (IR) performed CT-guided percutaneous drainage with multiple hepatic drain placements; however, all his liver abscess cultures remained negative. He was discharged home to complete a 6-week course of oral metronidazole 500 mg thrice daily and intravenous ceftriaxone 2 g twice daily to address his brain abscess, liver abscess, and aortic valve endocarditis.
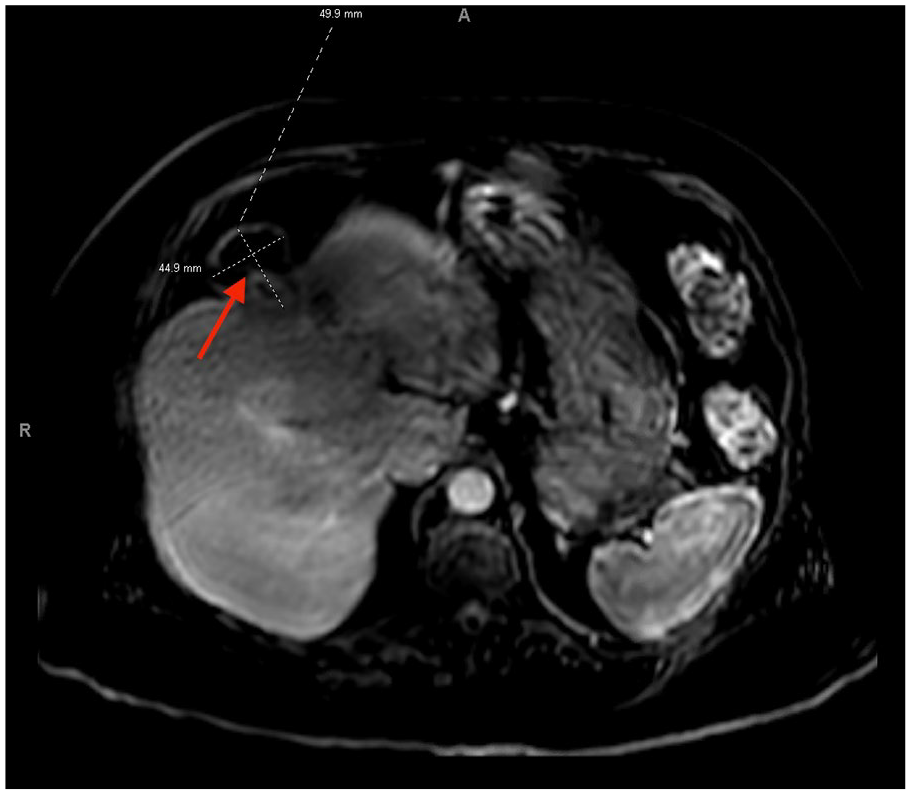
MRI liver shows a 5 × 5.5-cm subcapsular lesion in the anterosuperior subsegment of the right lobe (red arrow) and a 4.5 × 5-cm lesion in medial superior subsegment of the left lobe with an exophytic component and mild surrounding inflammation.

(A) Transesophageal echocardiogram showing a 1 cm vegetation on the aortic valve (red arrow). (B) Repeat transesophageal echocardiogram showing resolution of aortic valve vegetation after antibiotic treatment.
One week later, the patient underwent an outpatient cystoscopy which confirmed a trabeculated bladder with 2 diverticula but showed no evidence of a communicating colovesical fistula. The IR performed a hepatic drainage catheter check and subsequent removal given his liver abscesses had substantially decreased in size on repeat CT imaging. He developed elevated hepatic transaminases of unknown etiology on his outpatient surveillance labs, and his antibiotics were briefly held for possible concern of drug-induced liver injury (DILI). Our patient’s liver enzymes improved, but he then developed acute renal failure with eosinophilia and a widespread maculopapular rash affecting his neck, trunk, and upper and lower extremities. He was readmitted 3 weeks later for further workup, and both Dermatology and Nephrology were contacted for further assistance. The Dermatology service suspected the patient had experienced drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome, so his antibiotics were stopped, and corticosteroids were initiated for treatment. His renal function and eosinophilia improved; repeat TEE and MRI of the brain performed 7 weeks after the beginning of antibiotic treatment showed completed radiographic resolution of his cerebral abscess and aortic valve vegetation (Figures 2B and 5B). Repeat CT abdomen and pelvis revealed a persistent fistulous tract extending from the sigmoid colon into the bladder dome with near resolution of his bladder wall abscess and decreased size of his hepatic abscesses. The patient restarted oral metronidazole while inpatient and continued on discharge given his persistent hepatic abscesses. He continued metronidazole for approximately 13 weeks until he ran out of refills and did not show up to his outpatient ID clinic appointment.
Unfortunately, the patient developed a seizure episode at home 4 days later after stopping his antiepileptic therapy for 2 weeks and was re-evaluated in the emergency department (ED). Initial CT brain in the ED showed no evidence of recurrent brain abscess, and he was restarted on levetiracetam for secondary seizure prophylaxis. However, he presented again to the ED 1 week later as a code stroke when he was found to be nonverbal with new left-sided weakness. The CT brain on admission revealed a ring-enhancing lesion in the subcortical occipital lobe, concerning early abscess reaccumulation (1.9 × 1.1 cm). The ID service restarted the patient on intravenous metronidazole pending further workup. Subsequent MRI of the brain confirmed his ring-enhancing right occipital lobe lesion with surrounding vasogenic edema. The neurosurgery service attempted another stereotactic biopsy and drainage but was unsuccessful in return of abscess fluid. The catheter was removed, and a small sample of brain tissue was sent for gram stain and culture. Both aerobic and anaerobic cultures remained negative from his intraoperative brain tissue and catheter. Brain tissue cytology ruled out malignancy, and broad-range 16S rRNA bacterial polymerase chain reaction (PCR) testing returned negative for any bacterial infection. His recurrent brain lesion was determined to be due to fibrinous scar tissue from his prior cerebral abscess, and his metronidazole was discontinued after receiving another 3-week course, completing a 16-week total duration of antibiotics.
Discussion
The incidence of brain abscesses is 0.3 to 0.9 per 100 000 population and usually occur in patients with predisposing risk factors such as severe immunocompromised conditions (malignancy, connective tissue disease, organ transplantation, use of immunomodulating therapies, and HIV/AIDS), dental infection and surgery, severe head trauma or neurosurgery, diabetes mellitus, alcohol abuse, and ear, nose, and throat infections.7,8
In 2003, Han et al
11
analyzed 5 patients with
This case illustrates an uncommon presentation of brain and liver abscesses in an immunocompetent adult with colovesical fistula as the probable primary source of disseminated infection. After further interview, the patient admitted to heavy alcohol consumption in the distant past, but denied engaging in high-risk sexual behavior, smoking, or intravenous drug use. The patient had no recent travel history or sick contacts, and his age-appropriate cancer screenings were up to date. He disclosed his last colonoscopy was performed 5 years ago and a personal history of colon polyps and diverticulitis in the past. He initially denied any recent dental surgery or infection, but later disclosed poor oral hygiene with his dental appliances. Periodontal disease was ruled out with negative CT maxillofacial imaging.
Our patient received combination therapy with metronidazole and ceftriaxone for 6 weeks to target his cerebral abscess due to
In conclusion,
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases.
Informed Consent
Verbal informed consent was obtained from the patient for their anonymized information to be published.
Prior Presentation of Abstract
This work was presented as a poster at the ACP Internal Medicine Meeting in Boston, MA, on April 19, 2024.
