Abstract
The Tityus trinitatis, a black scorpion species endemic to the fauna of Trinidad, has been implicated in envenomation with devastating clinical sequelae such as acute pancreatitis and major adverse cardiovascular events. We present the first in-Caribbean case of a 59-year-old Caribbean South Asian male with human immunodeficiency virus who presented with a non-ST-segment-elevation acute coronary syndrome after being stung, which was managed with comprehensive, guideline-directed medical therapy. The clinician should be cognizant of scorpion-induced acute coronary syndrome (ACS) as a potential sequela of envenomation and its clinical management.
Keywords
Introduction
The Tityus trinitatis scorpion species (family Buthidae) is recognized for its potentially lethal venom, primarily attributed to its potent cardiotoxic and neurotoxic properties. It is endemic to Trinidad and Tobago, and envenomed patients typically present with a constellation of clinical features such as hypersalivation, intractable emesis, agitation, tachypnea, and cerebral edema. 1 In addition, pulmonary edema, hypovolemic shock, and convulsions can occur. This species is notorious for being implicated with fulminant myocarditis and pancreatitis as deleterious complications.2,3
Postenvenomation systemic responses are resultant of either immediate hypersensitivity, direct toxic effects of the venom on various organs, or a combination of both, likely mediated by catecholamines. 3 While electrocardiographic and biochemical evidence of myocarditis following T. trinitatis envenomation have been described, the specific association with non-ST-segment elevation acute coronary syndrome (NSTE-ACS) has not yet been reported to our knowledge. Herein, we present this case report of a middle-aged Caribbean South Asian with human immunodeficiency virus (HIV) who experienced an NSTE-ACS after being afflicted with a Tityus trinitatis scorpion sting.
Case Presentation
The patient is a 59-year-old Caribbean South Asian male with a medical history of HIV infection, well controlled on a combination antiretroviral therapy (ART) regimen (cluster of differentiation-4 count of 673 cells/mm3 [normal < 200 cells/mm3]) and undetectable HIV ribonucleic acid levels who presented with a scorpion sting on his left medial foot (Figure 1) at approximately ~4

The patient’s afflicted foot and Tityus trinitatis, a black scorpion. (a) Site of the patient’s left medial foot sting (encircled in red) with resolving erythema. (b) A sample picture of the Tityus trinitatis, a black scorpion endemic to Trinidad. This photograph was taken by co-author Dr. Stanley Giddings and is not the actual scorpion that stung the patient.
His vital signs on admission (midnight) were blood pressure of 169/94 mm Hg, heart rate of 52 beats per minute, pulse-oximetry 98% on room air, random blood glucose 116 mg/dL, and temperature of 36.4°C. The patient was alert and coherent, with a Glasgow Coma Scale score of 15/15, indicating no apparent neurological deficits. Cardiovascular examination revealed normal heart sounds with no detectable murmurs. Respiratory auscultation yielded clear breath sounds bilaterally without wheezing or crackles. Abdominal examination revealed a soft, mildly tender abdomen in the epigastric region with normal bowel sounds present. His admission electrocardiogram (ECG) reflected marked sinus bradycardia with hyperacute T-waves and secondary ST-segment depression suggestive of ischemia (Figure 2). His initial diagnostic data (Table 1) indicated an abnormal, positive high-sensitivity troponin I of 0.322 (normal 0.0 – 0.10 ng/mL) (~1 am the next day) with normal amylase and lipase levels.
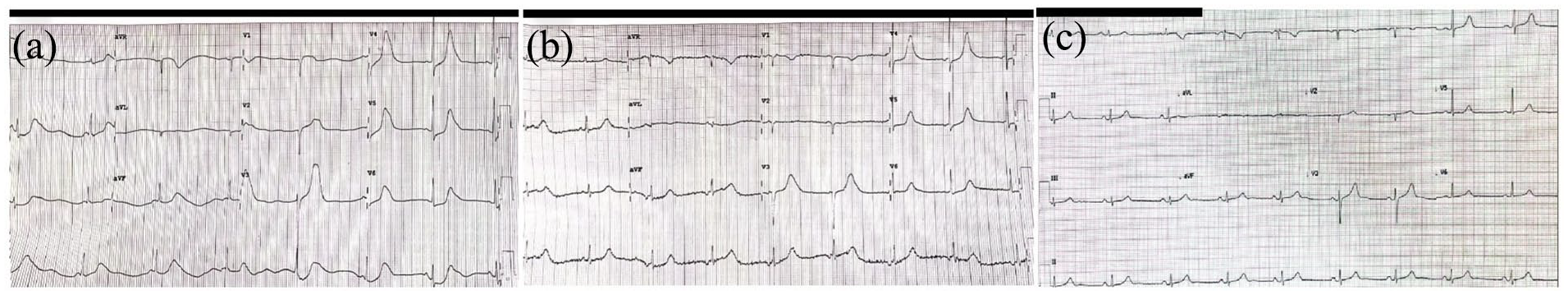
The patient’s 12-lead electrocardiogram (ECG). (a) This admission ECG revealed a marked sinus bradycardia with hyperacute T-waves and ST-depression in leads V4–V6 suggestive of dynamic, ischemic changes. (b) The postcoronary angiogram (CAG) ECG indicated sinus bradycardia with less acute T-waves and subtle resolution of the depressed ST-segments. c. The patient’s discharge ECG demonstrating marked improvement with respect to T-waves and ST-segments.
The Patient’s Initial Diagnostic Data.

Abbreviations: WBC, white blood cells; RBC, red blood cells; HCT, hematocrit; MCV, mean corpuscular volume; MCH, mean corpuscular hemoglobin; MCHC, mean corpuscular hemoglobin concentration; RCW, red cell distribution width; PLT, platelet; MPV, mean platelet volume; BUN, Urea; AST, aspartate transferase; ALT, alanine transaminase; ALP, alkaline phosphatase; GGT, gamma-glutamyl transferase; TP, total protein; ALB, albumin; GLB, globulin; CRP, c-reactive protein; LDH, lactate dehydrogenase; BNP, b-type natriuretic peptide; LDL, low-density lipoprotein; HDL, high-density lipoprotein; TG, triglycerides; HIV, human immunodeficiency virus; CD, cluster of differentiation; RNA, ribonucleic acid.
The patient was subsequently admitted to the cardiac ward, where he underwent bedside 2-dimensional transthoracic echocardiography (2D-TTE), which revealed a normal left ventricular ejection fraction (LVEF) of 55% to 60%, with no evidence of regional wall motion abnormality. In addition, the study confirmed normal valve function and no pericardial effusion (Figure 3). An abdominopelvic computed tomography scan was performed for his severe epigastric pain, which identified features suggestive of gastritis; however, there was no radiologic evidence of acute pancreatitis.
2
He was then initiated on a comprehensive, guideline-directed medical therapy (CGDMT) for his tentative diagnosis of NSTE-ACS, which included aspirin, ticagrelor, enoxaparin, rosuvastatin (low dose), ramipril, carvedilol, spironolactone, and empagliflozin, in addition to his pre-existing ART. His hs-cTnI remained persistently elevated the following day at 0.18 (normal 0.0–0.10 ng/mL) (~9

The patient’s 2-dimensional transthoracic echocardiogram (2D-TTE). (a) The parasternal long-axis view demonstrates normal left ventricular structure and function. (b) The apical 4-chamber view also demonstrates preserved left ventricular function.

The patient’s coronary angiogram (CAG). (a) A left anterior oblique (LAO) view of the patient’s right coronary artery (RCA) demonstrates an angiographically normal vessel. (b) A left anterior oblique-cranial view of the patient’s left anterior descending artery (LAD) demonstrates an angiographically normal vessel. (c) Left anterior oblique-caudal view of the patient’s left circumflex artery (LCx) demonstrating an angiographically normal vessel.
Discussion
Scorpion envenomation can have a broad spectrum of clinical manifestations, ranging from localized pain and swelling to severe systemic complications and even death. 4 The Tityus trinitatis (family Buthidae) are hazardous and can cause lethal complications.5,6 A series from the University of the West Indies estimated a case fatality rate of 0.9-1.5%. 7 Their distribution is more abundant in rural and subtropical regions than in temperate climates. 8 The severity of symptoms is contingent on the amount of venom injected, which is influenced by factors like the size and age of the scorpion, duration of the sting, and depth of penetration. 9 Tityus trinitatis holds the distinction of being endemic to the twin-island republic of Trinidad and Tobago, and due to climate changes, there has been a recent surge in scorpion stings both locally and internationally.7,9
The key components of scorpion venom often comprise cardiotoxins, neurotoxins, nephrotoxins, and biogenic amines. Other elements include phospholipases, hyaluronidases, and hemolysins.10,11 The toxic compounds can elicit mild to severe symptoms. The venom is capable of causing coronary artery spasm, platelet aggregation and thrombosis, reduced Na-K-ATPase activity, increased endogenous epinephrine, norepinephrine, bradykinin levels and anaphylaxis.11,12 These symptoms reported are emesis, diaphoresis, hypersalivation, tachy-, bradyarrhythmias, and convulsions. 11 The most reported cardiac manifestations are hypertensive crises (30-77%), T1MI, T2MI, myocarditis, heart failure with pulmonary edema (25%), and cardiogenic shock. 13 A systematic review of 703 cases identified sinus tachycardia (82%) and ST-T wave changes (64.6%) on ECGs as the most frequent electrocardiographic abnormalities, which represent cardiac injury, ischemia or myocardial strain. On 2D-TTE, there is regional or global hypokinesia with a depressed LVEF and dilated cardiac chambers. 14 Interestingly, the clinical presentation of the patient was significant for marked sinus bradycardia with ST-changes, unremarkable 2D-TTE and CAG. The pathophysiology of myocardial oxygen supply-demand mismatch resulting from tachycardia, hypotension, or hypertension is the maladaptive mechanism of T2MI according to the Fourth Universal Definition of Myocardial Infarction. 15 Unfortunately, there remains ambiguity with respect to certain facets of characteristics and management strategies of T2MI versus T1MI.15,16 We ascertained his final diagnosis to be a T2MI in the setting of a precipitating sting, abnormal electrocardiographic changes, and cardiac biomarkers with an unremarkable coronary angiogram. Cardiovascular medications such as nifedipine, a dihydropyridine calcium channel blocker, can vasodilate and attenuate myocardial oxygen demand. Prazosin, an alpha-adrenergic receptor antagonist, can reduce peripheral vascular resistance (PVR). In addition, angiotensin-converting enzyme inhibitors improve perfusion and mitigate against pulmonary edema. 11 In cases of cardiogenic shock, dobutamine is preferred as it augments myocardial contractility with minimal effect on PVR in a high catecholaminergic state. 14
Patients who have HIV and are prescribed ART display an accentuated cardiovascular burden. 17 There is an intricate milieu of chronic inflammation, endothelial dysfunction, ART-induced dyslipidemia, insulin resistance, and thrombophilia that is atherogenic. 17 Our patient’s low-density lipoprotein level of 76 mg/dL (normal 60-130 mg/dL) was not substantially elevated during his index ACS and was initiated on low-dose rosuvastatin to attenuate any drug-drug interaction with his ART. His glycosylated hemoglobin was 5.3% (normal < 5.7%), which did not suggest any metabolic component or endocrinopathy despite being on long-term ART.
Our case report contributes valuable insights into the potential spectrum of envenomation by Tityus trinitatis. It must be acknowledged that although the patient presented with a hypertensive crisis and T2MI, an HIV-associated major adverse cardiovascular event could have obfuscated the diagnosis, hence the rationale for CAG. As mentioned, this specific species envenomation has not been previously linked with either an ACS or T2MI, to our knowledge. Most envenomation-related Takotsubo cardiomyopathy (TTC) has been attributed to scorpion bites due to the mechanisms of fear, anxiety, direct catecholamine toxicity, and administration of exogenous beta-adrenergic agents. The majority of these patients do not fully meet international diagnostic criteria for TTC.18,19 With respect to our patient, while we did not image any transient reversible left ventricular systolic dysfunction, there were electrocardiographic changes and cardiac troponin release in the absence of coronary artery disease, myocarditis, or pheochromocytoma. 20 While TTC may be tentatively suspected, our patient did not completely fulfill diagnostic criteria with the caveat of his delayed presentation.
Conclusion
We present the case of a 59-year-old Caribbean South Asian male infected with HIV who presented with a T2MI post-Tityus trinitatis black scorpion envenomation. He was successfully managed with CGDMT. Clinicians should have a high index of clinical suspicion of cardiovascular sequelae in patients presenting with scorpion stings.
Footnotes
Author Contributions
AK, KA, AB, VC, PR, VS, RS, SG, and NAS all contributed substantially to the conception or design of the work and assisted with the acquisition, analysis, or interpretation of data. All authors also drafted the work and revised it critically for important intellectual content. There was final approval of the version to be published by all authors and consensus to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Compliance With Ethics Guidelines and Standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
The patient has provided verbal and written informed consent to have the details and images of his case published. Our institution does not require ethical approval for reporting individual cases or case series.
Data Sharing Statement
All available data can be obtained by contacting the corresponding author.
