Abstract
A barium esophagram is a diagnostic test used for the evaluation of dysphagia. However, this test has the potential risk for aspiration of the barium contrast. Barium aspiration typically localizes to the right lower lobe or left lingular lobe. We present a case of barium aspiration localized to the right middle lobe that persisted on chest X-ray. A 62-year-old male with a past medical history of hypertension, long-term back pain, gastritis, and anxiety presented with the complaints of hoarseness of voice, dysphagia, and weight loss for several months. During the esophagram, the patient aspirated the barium contrast. Chest X-ray confirmed the aspiration in the right middle lobe with a tree in bud appearance suggesting involvement of bronchioles. Three months later, a repeat chest X-ray revealed residual contrast. Pulmonary complications are directly related to the amount of aspirated barium and can include hypoxia, respiratory failure, secondary aspiration pneumonia, shock, and acute respiration distress syndrome. The prognosis of a barium aspiration is dependent on the amount of barium aspirated.
Background
A barium esophagram is a common diagnostic tool to visualize the digestive system in complaints of dysphagia. Barium sulfate, an insoluble agent, is ingested, and radiographic images are obtained during this process. 1 This procedure carries a risk of barium aspiration with deposition most commonly present in the right lower lobe and left lingular lobe. 1 This particular aspiration poses several pulmonary complications and has a varying prognosis.1,2 We present a case of barium aspiration to the right middle lobe with residual contrast present in the lung 3 months later.
Case Presentation
A 62-year-old male with past medical history of hypertension, long-term back pain, gastritis, anxiety had complaints of hoarseness of voice, weight loss, and dysphagia for several months. The patient was followed for this chief complaint by a physician outside the presenting hospital, several imaging tests as well as the discussed emergency room (ER) visit occurred at our facility. A computed tomography (CT) of the neck soft tissue revealed 5.6 cm × 3.7 cm × 4.9 cm heterogeneously enhancing soft tissue mass, which involved the left pharyngeal wall, left pharyngeal tonsil, the hypopharynx with erosion of the posterior aspect of the glenoid cartilage noted. In addition, the CT revealed a necrotic, 16 mm right level V lymph node and a 18 mm left level III lymph node. A barium swallow study was indicated for the complaint of dysphagia. During the study, the patient aspirated barium. The X-ray showed the contrast in the right middle lobe confirming the aspiration of barium along with a tree in bud appearance (red arrow; Figure 1). The patient presented to the emergency room following the barium aspiration with a blood pressure (BP) of 162/87 mm Hg, heart rate 71 bpm, respiratory rate (RR) 18, Temp 98.2°F, and oxygen saturation was 97% on room air. His physical exam in the ER was significant for cervical lymphadenopathy. The patient was placed on 2 L of supplemental oxygen while under observation in the ER. The patient was offered bronchoscopy, but he refused. The patient remained stable, and he wished to leave against medical advice after the risks were explained. He was advised to follow-up with his primary-care physician and pulmonologist. The patient was lost to follow-up. Following the barium aspiration, at a separate institution, the patient was diagnosed with squamous cell carcinoma of the hypopharynx after an esophagogastroduodenoscopy, and biopsy revealed a large hypopharyngeal mass partially obstructing the upper esophagus. He subsequently had a tracheostomy placed. Repeat chest X-ray 3 months later showed residual barium contrast in the right middle lobe (Figure 2).

Barium contrast aspiration in the right middle lobe.
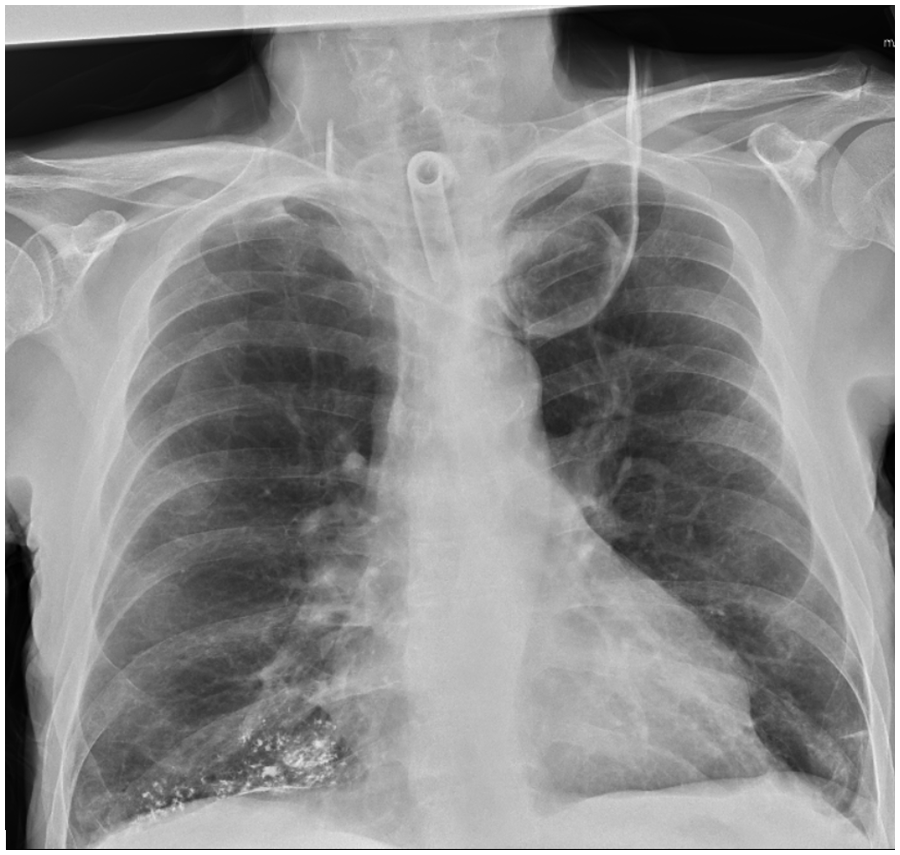
Residual barium contrast in the right middle lobe.
Discussion
Barium is a foreign body in the lung, which causes chronic pulmonary inflammation. 3 Barium studies are indicated for any digestive complaints centering around dysphagia. Barium sulfate is an insoluble agent that is used to visualize the gastrointestinal (GI) tract via a bolus that is ingested and later excreted in the feces undigested. 1 Although this is a common diagnostic test, there is a potential risk of aspiration. Our patient with no pertinent GI past medical history and no neurological deficits aspirated the barium contrast during his study. Established risk factors for barium aspiration include dysphagia, esophageal obstruction due to tumor, esophageal foreign body, elderly, history of oropharyngeal dysphagia, head and neck malignancy, decreased level of consciousness, neuromuscular dysfunction, alcoholism, and a bronchoesophageal fistula.1,4,5
Prognosis of barium aspiration depends on the amount aspirated. Barium aspiration can be localized in both lungs. Our patient aspiration event localized to his right middle lobe which is rare because lower lobe followed by the lingual area is typically more common. 1 In addition, a patient’s position during the test determines where the barium deposition occurs. For example, if a patient is in the recumbent position, the posterior segments of upper lobes or superior segment of the lower lobes are affected; if upright, the basal segments of lower lobes; and finally, if inclined forward, the middle lobe is affected.2,5,6 Based on the chest radiograph seen in Figure 1, our patient’s barium deposition occurred in the middle lobe which corresponds to a leaning forward position for his esophagram. Therefore, chest radiographs can confirm diagnosis of barium aspiration whereas a high-resolution CT is reserved for severe cases for determination of long-term prognosis. 4 Our patient’s chest X-ray showed a tree in bud appearance after this event, which was likely due to the barium deposition in the lower parts; therefore, he did not require a CT scan.
Pulmonary complications are also directly related to the amount of aspirated barium. Complications vary from hypoxia, respiratory failure, secondary aspiration pneumonia, shock, and acute respiration distress syndrome.1,2 The highest dose of barium associated with aspiration mortality was seen with Gray el al 7 at 250% weight/volume. The current recommended barium concentration for barium studies is 100 g barium in every 100 ml of solution. 1 The exact amount of contrast agent was not known for this case, but it was suspected to be less than 30 g, as the patient started to cough immediately after drinking it. Most patients are asymptomatic with no intervention needed. 2 Treatment is mainly supportive including oxygen supplementation, anti-reflux medications with proton pump inhibitors, dopamine 2-receptor agonist, and chest physiotherapy.1,2 Our patient was treated with supplemental oxygen but left abruptly from the emergency department. If aspiration occurs consequently with aspiration of gastric contents, there is a concern for aspiration pneumonia, which necessitates the initiation of anaerobic antibiotic coverage. In Tamm and Kortsik’s study, 6 a patient exhibited progressive dyspnea after barium aspiration. The patient was requiring 6 L/min and eventually bronchoscopy was performed. The patient subsequently developed signs of an infection including fever, an increase in inflammatory markers, and a leukocytosis which led to the initiation of antibiotics. Tamm and Kortsik 6 also discussed a second case presentation in which a patient was hypoxemia on room air after barium aspiration and a bronchoscopy was performed immediately. The chest radiograph 6 days later showed a significant reduction of barium deposition; although long-term resolution could not be followed because the patient expired. In Kumar et al’s study, 4 the patient was intubated due to hemodynamic instability and underwent bronchioalveolar lavage to remove the barium contrast. The patient was extubated after 24 hours. However, other studies caution against bronchoalveolar lavage to avoid further distribution of barium.2,6
As barium can be visualized on radiograph, the timing of when it is cleared can vary. For our patient, his chest radiograph 3 months later still showed barium, although it was improved. In Voloudaki et al’s study, 5 a year later after the barium aspiration, a high-resolution CT scan suggested fibrosis from the barium deposition with thickened interlobular septa, subpleural cysts, and subpleural lines even though the patient was clinically asymptomatic. In Tamm and Kortsik’s study, 6 one of the patients described was also clinically stable a year and a half after the aspiration event with plain radiograph showing persistent barium deposition with only slight improvement. Therefore, resolution of barium can also be affected by the amount of barium aspirated.
With the long-term residence of barium deposition, the question remains if it continues to act as a foreign body within the body system. In Ueha et al’s study, 3 60 uL of 60% weight/volume barium suspension was injected to mimic aspiration in rats which is equivalent to 10 mL barium aspiration in humans to study the effects of barium after 30 days. Within 30 days, histopathological findings showed thickened bronchiolar walls with staining positive for CD3+ lymphocytes and thickened alveolar walls staining positive for myeloperoxidase (MPO) (+) granulocytes and macrophages for continued chronic inflammation of the respiratory system.3,4
Although incidence of barium aspiration can be rare with varying prognosis, prevention should always be considered. Alternative diagnostic work up in those with risk factors for aspiration include ultrasound, endoscopy, magnetic resonance imaging (MRI), CT, positron emission tomography (PET) scan, functional endoscopic evaluation of swallowing, or even video fluoroscopic modified barium swallow.1,2 Another source of prevention is the use of contrast agents that do not affect the lung including iopydol, hytrast, and iodixanol.1,4,6 Finally, positioning during the swallow exam can be beneficial by chin touching the neck if done upright or rotating the head if lying on the side.1,8 In Belafsky et al’s study, 9 the use of retro-esophageal suction catheters in those with oropharyngeal dysphagia was studied to determine if its use can reduce aspiration events. The study found that the use of a retro-esophageal suction catheter greater than 12 French with negative pressure at the upper esophageal sphincter reduced aspiration events by 100% by increasing the opening at the upper esophageal sphincter. 9 It is already known that those with oropharyngeal dysphagia have an increased risk of aspiration. Although, this study was used to determine if this ideation can be applied to percutaneous enterogastric tubes. It is uncertain if this can prevent aspiration events that occur before and during the act of swallowing but can be eliminated in those with hypopharyngeal residue. 9 The clinical significance of these findings is uncertain as their study was done on cadavers; hence, comfort and tolerability of the catheter is not clearly established.
Conclusion
Barium aspiration is a rare complication of a barium esophagram. Complications of the aspiration event include respiratory failure, shock, and acute respiratory distress syndrome.1,2 Prognosis varies but seems to be dependent on the amount of barium aspirated.
Footnotes
Acknowledgements
None.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Informed consent for patient information to be published in this article was not obtained because the patient has expired.
