Abstract
Odontogenic bacteremia, most commonly involving gram-positive oral flora, can result from daily self-care practices or professional dental procedures. Though usually transient and quickly cleared by the immune system, the presence of periodontal disease increases the frequency of exposure and risk of persistence of oral-systemic infections. Comorbidities such as asplenia, alcoholism, and immunocompromise increase the risk of complications of hematogenous spread and severe systemic illness.
Introduction
Bacteria of the genus
Capnocytophaga spp have a worldwide distribution across all ages as normal flora of the oral cavity. Pathologically, they can cause nonfulminant diseases such as periodontitis, caries, and plaque across all ages.
4
Comorbidities such as diabetes and malignancies in children increase the oral bacterial burden of
In contrast,
Case Presentation
A 70-year-old man presented with 3 days of loose watery stool, worsening generalized weakness, 1 day of confusion, and inability to walk. He had a history of chronic medical problems including asthma/chronic obstructive pulmonary disease (COPD) requiring 4 L of home oxygen therapy, rheumatoid arthritis, sarcoidosis, and chronic kidney disease. He was on long-term 17.5 mg methotrexate weekly and 10 mg prednisone daily.
Vital signs recorded on admission included normal temperature with normal heart rate and blood pressure. On initial physical examination, he was noted to be awake but lethargic and had poor oral hygiene with multiple dental caries. On auscultation, there was reduced air entry into his lungs, and bilateral wheezing, and his abdomen was tender to palpation. He was noted to have extensive bruising over his left hand and bilateral pitting pedal edema. He was admitted and managed for COPD exacerbation and dehydration due to diarrhea.
On admission, he was started on intravenous methylprednisolone and bronchodilator treatments; on day 2, his mental status became more altered. He was later intubated urgently after failure of bilevel positive airway pressure (BiPAP) trial for acute on chronic hypercapnic respiratory failure. He was also started on diuretics initially and later hemodialysis for acute kidney injury. After 3 days of intubation, his mental and respiratory status had improved remarkably, and he was successfully extubated on day 5 of admission.
On day 9 of admission, he developed fever of 38.7 °C. Blood and urine cultures were collected, and he was promptly started on empiric vancomycin, cefepime, and metronidazole.
By day 10, his mental status declined, and he was again in hypercapnic respiratory failure. He failed BiPAP trial again and had to be re-intubated. At time of intubation, a pool of blood was noted in mouth and hypopharynx and 2.5 L of bloody fluid suctioned from his stomach. He was placed on pantoprazole infusion for suspected gastrointestinal (GI) bleeding and aspiration was strongly suspected. Broad antibiotics that had been started the prior day were continued. A few hours later, norepinephrine infusion and stress-dose hydrocortisone were started due to persistent hypotension. Esophagogastroduodenoscopy revealed esophageal erosion, gastric, and duodenal ulcers.
On day 11, he still required high doses of norepinephrine despite resolution of fever. Urine culture obtained on day 9 had >100 000 colony forming units/mL of
Blood cultures obtained on day 9 became positive on the fourth day of culture, with Gram-negative bacilli in one anaerobic bottle of 4 culture bottles, his antibiotic was switched to piperacillin-tazobactam and tobramycin. The isolate was identified 2 days later, on hospital day 14, as
The patient was taken off vasopressors on hospital day 16 and extubated on day 17. The patient was treated for 4 weeks with renally dosed intravenous ampicillin-sulbactam for endovascular infection due to the occlusive thrombosis detected while patient had bacteremia.
Using 16s rRNA gene sequencing,
Discussion
Bacteremia resulting from a break in mucosal barrier is common: from the oral cavity, routine activities such as brushing and flossing regularly cause transient bacteremia with oral flora. Odontogenic diseases pose an increased risk of persistent bacteremia due to undrained foci of infection. Bioburden, such as in extensive dental plaques, or mucosal disruption in gingivitis, oral ulcers, gastritis, colitis, peptic ulcer disease, and inflammatory bowel diseases can also increase the risk of microbial gut translocation.10-12 Our patient had been on methotrexate and prednisone for rheumatoid arthritis causing him to be immunocompromised. Prolonged use of glucocorticoids and methotrexate have individually been shown to lower the integrity of the gut mucosa leading to ulcerations, perforations, and increased risk of bleeding.13-15
Only one case of bacteremia due to
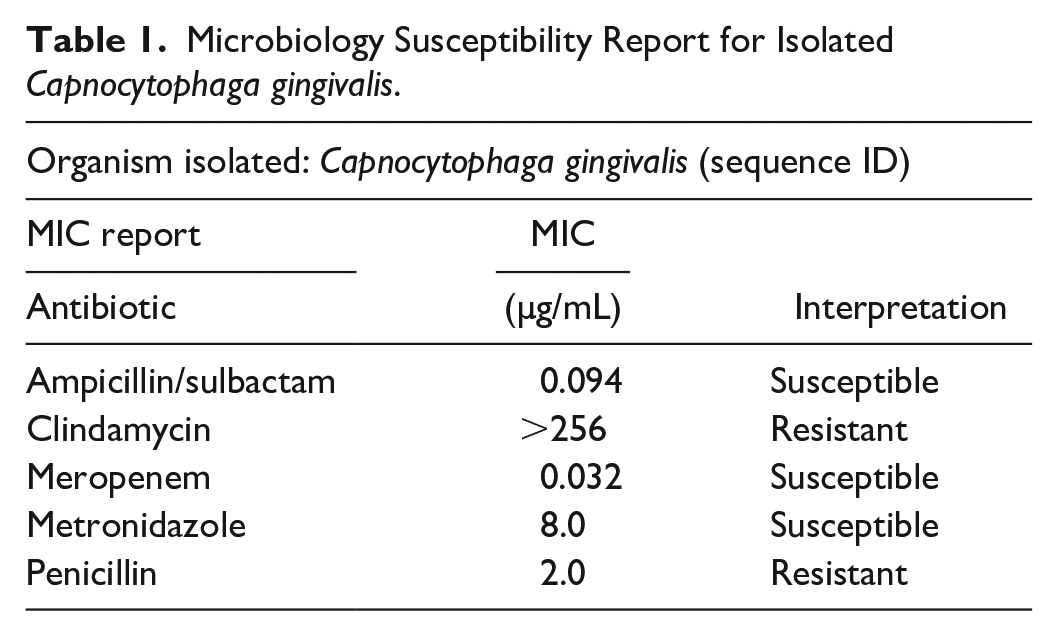
Microbiology Susceptibility Report for Isolated
A detailed literature search was conducted using the search words “

Case reports search flow diagram.
Polymicrobial and primary oral/periodontal abstracts were excluded from this review. Five case reports of human non-oral

Abbreviation: COPD, chronic obstructive pulmonary device.
Antimicrobial susceptibilities in the identified cases followed no specific pattern as 4 of the 5 cases had class resistance reported, with only one multi-drug resistant case resistant to 4 classes of antibiotics. As in our case, many of the
In conclusion, in this case, poor dental hygiene with periodontitis posed an increased risk of infection with human oral strains of genus
Footnotes
Authors’ Note
The contents of this article do not represent the views of the Department of Veterans Affairs or the US government. This work was previously presented at the Southern Regional Meeting, New Orleans, Louisiana, 2019.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The material is the result of work supported with resources and the use of facilities at the Charlie Norwood VA Medical Center. The funding organizations had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication. The contents of this publication are solely the responsibility of the authors and do not represent do not necessarily reflect the views, opinions or policies of The Department of Veterans Affairs, or the the U.S. Government. Mention of trade names, commercial products, or organizations does not imply endorsement by the U.S. Government.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Verbal informed consent was obtained from the patient for their anonymized information to be published article.
