Abstract
Pulmonary autograft, or Ross procedure, is performed by supplanting a diseased aortic valve with the patient’s own pulmonary valve. Reconstruction of the right ventricular outflow tract is then completed using a pulmonary homograft. To our knowledge, infective endocarditis occurring decades after the Ross procedure has not been reported. Diligent echocardiographic examination can be crucial to ensure prompt treatment and avoid the 25% mortality rate associated with infective endocarditis. Clinical suspicion should remain high in those with a pulmonary autograft history. In this article, we report the case of a 39-year-old patient with infective endocarditis presenting 22 years after Ross procedure.
Introduction
The pulmonary autograft, or Ross procedure, was initially performed in 1967 by cardiothoracic surgeon Dr Donald Ross. 1 The patient’s own pulmonary valve supplants the diseased aortic valve. Following pulmonic excision, the right ventricular outflow tract is reconstructed with a pulmonary homograft. 1
Pulmonary autografts have demonstrated superior resistance to early and late infections as compared with other traditional aortic replacement procedures.2,3 By preserving the endothelium and endocardium, the autograft maintains the ability to fight infection leading to lower rates of infective endocarditis (IE). 1
Infective endocarditis is an infection of the endocardium with predilection for heart valve involvement. Early diagnosis and prompt intervention are crucial to avoid an approximate mortality rate of 25%. 4 Predisposing risk factors include structural heart disease, presence of a prosthetic valve or cardiac device, intravenous drug use, immunosuppression, or recent invasive procedures. 4
Diagnosis is satisfied through a combination of clinical presentation, positive blood cultures, and echocardiographic characteristics. 5 The current diagnostic gold standard is established with the modified Duke criteria. It is sensitive and specific for IE based on major and minor criteria categorizing patients as either definite, possible, or rejected. 6
To our knowledge, IE occurring 2 decades after pulmonary autograft has not been documented. We report the case of a 39-year-old patient with IE presenting 22 years after Ross procedure.
Case
A 39-year-old female presented to the emergency department with 4 days of fever and stabbing, nonradiating right flank pain. The patient self-treated a reported 101.7 °F temperature at home with acetaminophen. Her history was significant for a bicuspid aortic valve corrected with aortic balloon valvuloplasty followed by Ross procedure at age 17. She denied intravenous drug use, recent dental treatment, or other invasive procedures.
On physical examination, the patient was febrile (102.9 °F), tachycardic (101 beats per minute), and hypertensive (174/103 mm Hg). A grade 4/6 holosystolic ejection murmur was heard in all cardiac windows on auscultation. Electrocardiogram was negative for abnormalities or acute ischemic changes. Mild cardiomegaly and evidence of previous sternotomy were seen on chest radiography (Figure 1). A bedside transthoracic echocardiogram (TTE) was completed revealing an ejection fraction of 65% and elevated right ventricular systolic pressure of 71 mm Hg. No definitive lesions were identified. Two sets of blood cultures were collected in addition to a urine specimen before the patient was discharged home. The following day, blood cultures were found to be positive for Streptococcus anginosus, while urinalysis was negative. The patient was immediately informed of the results and returned for admission and initiation of empiric intravenous therapy with vancomycin pending sensitivity results. Fever, positive blood cultures, and a predisposing cardiac condition met the clinical diagnostic threshold for possible IE.
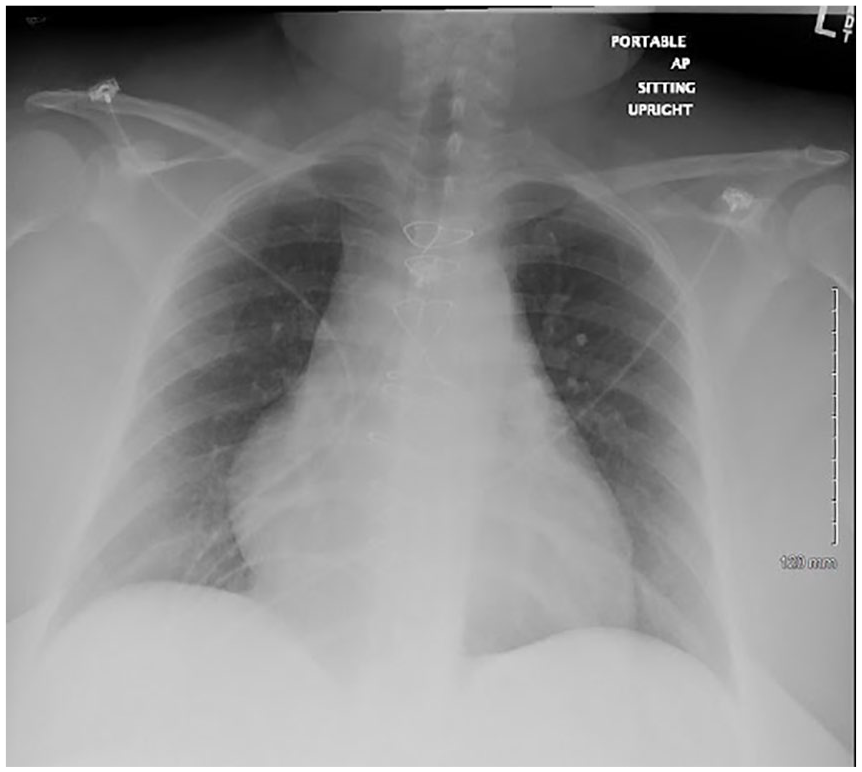
Chest radiograph demonstrating mild cardiomegaly and previous sternotomy.
Cardiology was consulted to complete a transesophageal echocardiogram (TEE) given her history of a bioprosthetic valve. TEE indicated severe pulmonic stenosis with an elevated right ventricular systolic pressure of 90 mm Hg, pulmonary artery maximum velocity of 4.7 m/s, and peak gradient of 88 mm Hg. Left ventricular ejection fraction was similar to the previous TTE at 60%. Moderate aortic and tricuspid regurgitation was appreciated along with a dilated right ventricle. No vegetations were noted; however, the pulmonary valve was not well visualized. A cardiac computed tomography scan identified severe pulmonic stenosis; 5 mm right-outflow tract narrowing of the proximal main pulmonary artery and 25 × 12 mm pulmonary annulus narrowing. Orthopantomography was negative for acute disease or significant periodontal disease.
Sensitivity results to ceftriaxone, cefotaxime, and benzylpenicillin had minimum inhibitory concentrations of 0.5, <0.12, and <0.06 mg/L, respectively. Her antibiotic regimen was modified accordingly for optimal treatment. She began a 6-week course of intravenous ceftriaxone and gentamicin.
The patient continued medical management and was transferred to a tertiary care center with cardiac surgery expertise. Ultimately, she underwent successful Melody transcatheter pulmonary valve replacement after completing her course of antibiotics without complication. As of June 2020, the patient remains in good health.
Discussion
The diagnostic challenge in our case was maintaining suspicion for IE with our patient’s pulmonary autograft history further augmented by the inability to identify vegetations on echocardiogram. Diagnostic delays may prevent prompt antibiotic treatment and contribute to a prolonged hospital course.
Careful echocardiographic evaluation should be conducted in all patients with suspected IE, especially those with a history of pulmonary autograft surgery. With a TTE sensitivity of 75%, a definitive diagnosis is concluded in the majority of patients. 7 However, a negative examination does not rule out disease and may be observed in up to 15%. 7 Adding difficulty, some vegetations are not yet present or too small to be visualized early in the disease process. 8
The European Society of Cardiology recommends a second examination be performed 7 to 10 days after initial negative results if a high index of suspicion persists. 7 One report in France identified pulmonary homograft infection occurring 2 years after Ross procedure. 9 Similar to our case, the patient initially presented with fever of unknown origin and negative TEE. Blood cultures were positive for Enterococcus faecalis. A septic pulmonary embolism prompted a second TEE, which revealed large vegetations on the pulmonary valve. In our case, a repeat examination was not performed that may have revealed a vegetation not previously identified.
While pulmonary autograft surgery is presumed to have a lower incidence of IE, it is not negligible. A review of the literature identified limited cases occurring decades after Ross operation. In a 25-year longitudinal study, Martin and colleagues reported 3 patients (1.0%) out of 310 who developed IE following Ross procedure. 10 Unfortunately, the time since operation was not available. India confirmed a case involving the homograft of a 54-year-old patient presenting 10 years since pulmonary autograft. He was treated conservatively with 6 weeks of antibiotics. 11 Late-onset endocarditis occurring 7 years post-Ross was reported in a 40-year-old male without history of intravenous drug use or recent dental treatment, as in our patient. 2 Diagnosis was established with positive blood cultures isolating Staphylococcus aureus and large vegetation on echocardiography. Their patient underwent urgent vegetectomy and cryopreserved homograft replacement with a stable hospital course. Smeets et al published the case of a 38-year-old male with pulmonary homograft IE and aortic root dilation that occurred 13 years after Ross procedure. 12 He was managed surgically with a double stentless bioprosthesis approach. Closest temporally to our patient, a case occurring 19 years after surgery was reported in London. 13 Streptococcus agalactiae was identified and attributed to a cat bite. The patient tolerated surgical excision and replacement of the infected valve without complication.
Our case serves to encourage clinicians to maintain suspicion of IE in patients with a pulmonary autograft history despite negative echocardiographic results. In addition, a secondary TEE should be performed in accordance with cardiology recommendation if suspicion persists.
Conclusion
To our knowledge, an IE diagnosis 2 decades after undergoing Ross procedure has not been reported. Our case highlights the importance of diligent echocardiographic examination to ensure prompt identification and treatment. Clinical suspicion should remain high, inclusive of those with a pulmonary autograft history and negative echocardiogram.
Footnotes
Acknowledgements
We would like to thank the patient for allowing us permission to publish this case report. Additionally, we would like to thank the American Federation for Medical Research where the abstract of this paper was presented during the 2019 Western Medical Research Conference.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval to report this case was obtained from the Institutional Review Board #18105.
Informed Consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
