Abstract
Aim:
Natural antioxidants were offered as the answer of dentin adhesion issue. The aim of this study is to investigate the effects of proanthocyanidin and lycopene as pretreatment agents on the sound and caries-affected dentin surface on microtensile bond strength and microleakage.
Materials and Methods:
This study was designed as in vitro because of that 84 mandibular molar teeth were collected. Forty-two of the included teeth were carious teeth, while the other 42 were without caries. Sixty of them were used for microleakage and 24 for microtensile bond strength testing and scanning electron microscopy analysis. The samples were divided into six subgroups randomly according to dentin pretreatments: 5% proanthocyanidin, 5% lycopene, and no antioxidant application. After the restorative procedures, samples were attached to the microtensile tester. Samples were subjected to tensile stress in the load cell until they broke at a speed of 0.5 mm per min. Microtensile bond strength (µTBS) and microleakage test data were analyzed with two-way analysis of variance, Bonferroni correction, and Tamhane’s T2 tests.
Results:
Two-way variance analysis showed that dentin pretreatment applications, dentin substrate, and the interaction between these two parameters had statistically significant effects on µTBS values (P < .001). There was no difference between dentin pretreatment applications in terms of microleakage scores (P > .05).
Conclusion:
The application of dentin pretreatment with proanthocyanidin is a successful procedure that increases the bond strength in both dentin substrate, while pretreatment with lycopene in caries-affected dentin reduces it.
Introduction
The development of effective adhesive systems and procedures has brought the term minimally invasive approach to today’s literature. 1 It is aimed to treat the carious lesion of the dentin conservatively, not to expand the cavity margins with macromechanical retention and to protect the sound dental substrate in this approach. 2 Dentin caries consist of two separate layers: externally infected dentin and internally affected dentin. 3 Many researchers agree that the caries-affected dentin (CAD) layer, when bacterial contamination is not observed and has a remineralization capacity, should not be removed in a conservative cavity preparation.4,5
CAD exhibits a different chemical and physical characteristic than sound dentin (SD) because of the cyclic repetitions of remineralization and demineralization occurring during the caries process. 6 Because CAD is a more porous, partially demineralized, and modified ultrastructural collagen tissue, it exhibits lower bond strength compared to SD, and the adhesive interface is more sensitive to hydrolytic/enzymatic degradation. 7 Water absorbed by the polymers initiates hydrolytic degradation, leading to the destruction of adhesion monomers that are not capable of fully encapsulating the collagen matrix. 8 Thus, collagen fibrils in the hybrid layer are exposed and undergo enzymatic destruction by metalloproteinases (MMPs) in the dentin matrix. 9
Although MMPs are secreted as inactive proenzyme, they are involved in the breakdown of extracellular matrix, elastin, and collagen fibrils when activated. 10 The activation of these enzymes takes place at low pH, and the acidification process of dentin, which is carried out during restorative processes prepares the ground for pH decrease. 11 However, later research has shown that the acid-etching process is not the only responsible and that the pathogenicity experienced in the dental caries process triggers the activation mechanism by causing low pH.12,13 Nishitani et al. demonstrated that collagen fibrils in the hybrid layer, which cannot be fully covered after the application of adhesive to the dentin, are spoiled or destroyed. They interpreted this as an indirect indicator of the presence of MMPs with the realization of collagenolytic and gelatinolytic activity in partially demineralized dentin. 14 However, the zymography and Western Blot techniques developed afterward provided the direct detection of stromelisin-1 (MMP-3), collagenase (MMP-8), gelatinase A (MMP-2), gelatinase B (MMP-9), and enamelize in the dentin pulp complex.15,16 This development was followed by the discovery of MMP-2 and MMP-9, which are heavily expressed in the CAD tissue. 17 Pashley et al. suggested that dentin-derived MMPs caused disruption in the hybrid layer of weak resin infiltration and that this deterioration could be prevented by MMP inhibitors. 18 Based on this idea, many strategies have been developed, called dentin pretreatment or dentin biomodification, for both SD and CAD substrate to prevent the disruption of adhesion attachment and to prolong the life of restorations. 19
The purpose of the dentin pretreatment application is to apply the components with MMP inhibition feature after acid etching, to protect or increase the bond strength of the hybrid layer. 20 For this aim, many synthetic agents such as chlorhexidine, tetracycline, ammonium compounds, ethylenediaminetetraacetic acid (EDTA), and chitosan have been used and the effectiveness of the inhibition has been demonstrated.10,20,21 However, because of the synthetic nature of these chemicals, the cytotoxic effects that dentin has on odontoblast cells and the structural changes of its components in the tooth have led researchers to seek alternatives.22,23 Natural antioxidant substances have the ability to inhibit MMP synthesis and the catalytic activity of the existing MMPs. 24 Successful results on MMP-2, -8, and -9 have been reported in studies where proanthocyanidin rich grape seed extract was used as a pretreatment agent on the SD surface.24,25 Lycopene is an important carotenoid in red fruits and vegetables such as tomato, watermelon, papaya, pink grapefruit, and guava. 26 In preclinical experimental studies, multiple biological functions such as antioxidant activity, and MMP-2 and -9 inhibition activity have been demonstrated.26,27 However, as far as we know, there is no study investigating its use as intact dentin or CAD as a pretreatment agent.
For this reason, the aim of this study is to investigate the effects of proanthocyanidin and lycopene, which are natural antioxidant agents, as pretreatment agents on the SD and CAD surface on microtensile bond strength (µTBS) and microleakage. The null hypotheses tested in our study are as follows: (a) There will be no difference in bond strength between the tested dentin substrates. (b) There will be no difference in bond strength between the pretreatment agents tested. (c) There will be no difference between the tested groups in terms of microleakage.
Materials and Methods
Preparation of Samples
Eighty-four mandibular molar teeth were collected for our study. Teeth were extracted after obtaining informed consent from patients as part of the original treatment plan, and stored in 0.5% chloramine T solution until completely used after removing organic residue. Forty-two of the included teeth were carious teeth with ICDAS II (International Caries Detection and Assessment System) score five, while the other 42 were teeth without caries. Sixty of them were used for microleakage, and 24 of them for microtensile bond strength testing and scanning electron microscopy (SEM) analysis.
The occlusal surfaces of the teeth were cut with a low-speed precision cutting machine (Isomet 1000, Buehler, Lake Bluff, IL, USA) and the dentin surface was exposed. The roots of the teeth were removed to be 2 mm below the enamel–cement boundary. Different dentin tissues were defined using the visual and tactile method. Caries marking dye (Caries Marker, VOCO GmbH, Cuxhaven, Germany) was used to properly separate the CAD and SD substrates. The dye was applied to the flat dentin surface for 10 s with the help of an applicator and washed for 5 s. Then it was gently air dried for 5 s. The areas painted in dark red were infected dentin, the pink stained areas were considered to be the dentin affected by caries and the non-stained areas were considered as sound dentin. The infected dentin area, painted in dark pink, was removed with the help of a partial sharp-tipped excavator (Fischer’s Ultrapak Packers, Ultradent, UT, USA). After the procedure, the residual dentin thickness was measured with the aid of calipers and the ones 2 mm and above were included in the study. Surfaces were abraded with 600 grit SiC papers and formed a standard smear layer. Afterward, the samples rinsed under water were air dried for 15 s.
Restorative Procedures
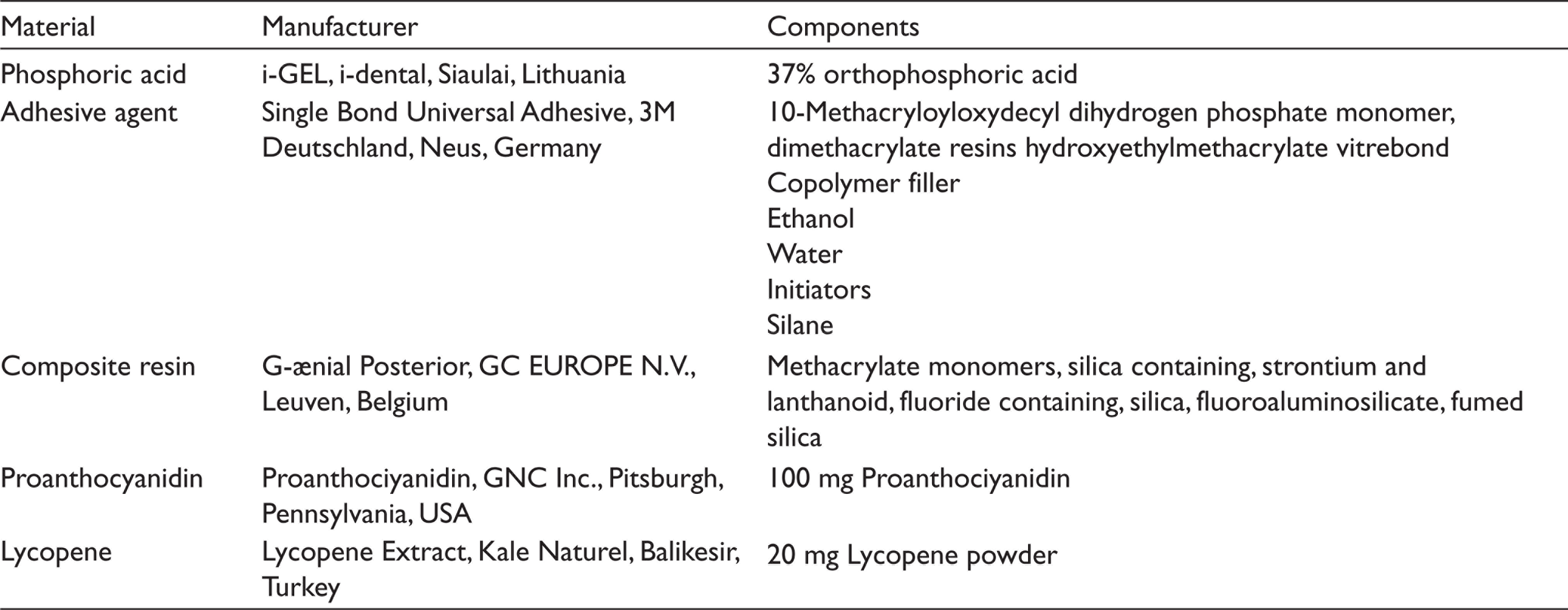
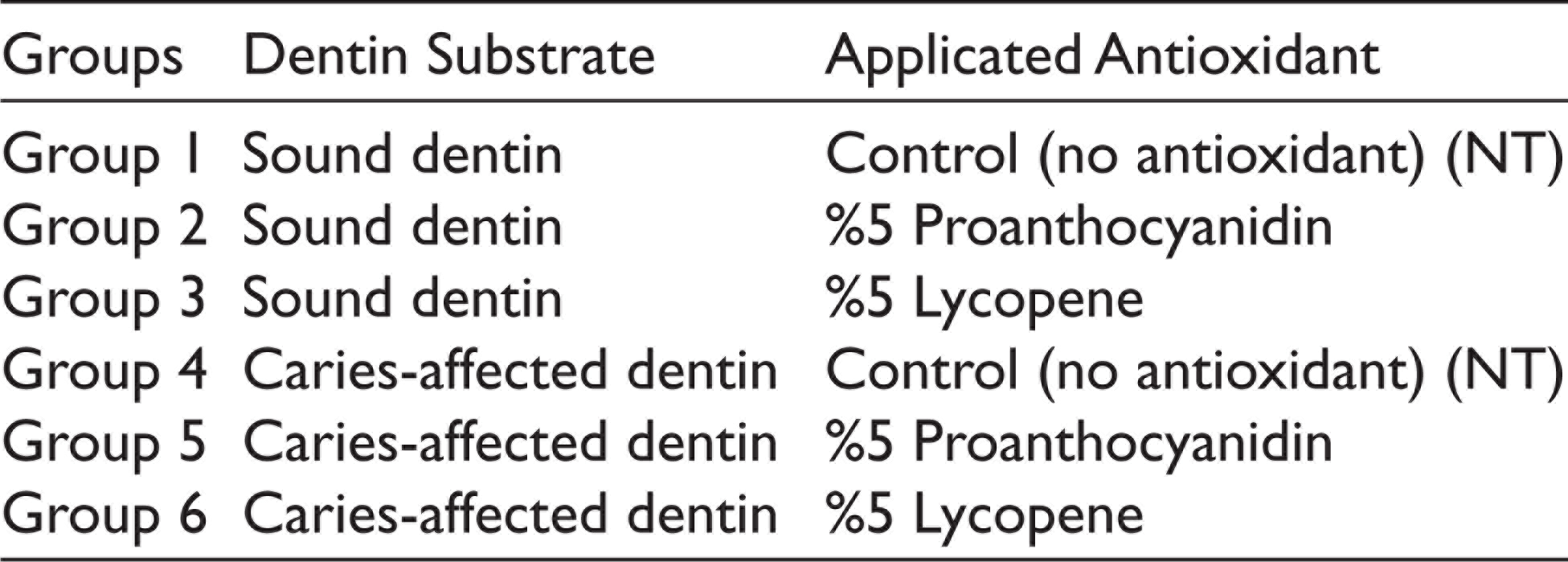
The materials and their chemical compositions used during restorative procedures are shown in Table 1. SD and CAD sample surfaces were etched for 15 s with 37% phosphoric acid and washed with water for the same period of time. The samples were then divided into six subgroups, with three different dentinal pretreatments: 5% proanthocyanidin, 5% lycopene, and NT (no antioxidant application was performed and used as control group; Table 2). Pretreatment applications were passively applied to SD and CAD surfaces for 10 min and the dentin surfaces were dried with the help of an absorbent paper. Subsequently, the adhesive system of etch and rinse was applied to the dentin surface for 20 s, and excess adhesive was removed with the aid of air spray for 5 s and polymerized at a distance of 1 mm for 20 s with a high-performance light-emitting diode. The final height of the complex, whose restoration was completed with a microhybrid composite resin, was standardized as 4 mm.
The resin–dentin complexes were kept in distilled water at 37°C for 24 h. Low-speed precision cutting device sections were taken with perpendicular position to the adhesion interface and sticks were obtained. Two sticks from each resin–dentin complex were separated for scanning the hybrid layer by SEM. The area of each stick was measured as 1.0 mm2 (± 0.2 mm2). On average, 18 sticks were obtained from a resin–dentin complex.
Microtensile Test Procedure
Samples were attached to the microtensile tester (microtensile tester, BISCO Inc., Schaumburg, IL, USA) with cyanoacrylate adhesive. Samples were subjected to tensile stress in the load cell until they broke at a speed of 0.5 mm/min. The bond strength values were obtained in kgf/cm2 and converted to MPa after measuring the cross-sectional area in the fracture area by a digital caliper (Model CD-6BS, Mitutoyo, Tokyo, Japan).
The Materials and Their Chemical Compositions Used in Restorative Procedures
Study Groups
After the microtensile test, the broken surfaces of all samples were examined using a stereomicroscope (TM-505, Mitutoyo, Tokyo, Japan) to determine the failure mode at 60× magnification. The refraction pattern was divided into three failure groups as follows: cohesive (within dentin or composite structure), adhesive (at the interface of the junction), and mix (fracture line with multiple substrates).
Microleakage Test
Thirty occlusal caries and 30 caries-free mandibular molar teeth were used for microleakage testing. Before the test, class I cavities were opened on the occlusal surfaces of carious teeth with a depth of 3 mm, 3 mm buccolingual width, and 6 mm mesiodistal width. In carious teeth, the caries were removed with the help of a high-speed hand tool, the infected dentin was cleaned with a sharp excavator. The preparation was continued with the help of caries fixing dye until the CAD was obtained. Later on, the dentin pretreatment process was applied to the teeth and their restorations were completed. The root tips of the teeth were covered with a composite material and two layers of nail polish were applied, 1 mm outside the restoration. After the nail polish was dried, all samples were kept in an incubator containing 0.5% basic fuchsin solution at 37°C for 24 h. Teeth were washed under running water to remove any remaining dye and then dried at room temperature. To detect microleakage, the teeth were cut from the roots with a low-speed precision cutting device in the buccolingual direction and evaluation sections were obtained.
Dye penetration in sections was examined using a stereomicroscope (TM-505, Mitutoyo, Tokyo, Japan) at 20× magnification. It was made according to the following criteria determined by scores of Milleding et al.:
0 = No microleakage 1 = Microleakage throughout the enamel 2 = Microleakage that extends beyond the enamel–dentin junction 3 = Microleakage along the cavity base 4 = Microleakage reaching the pulp
28
Statistical Analysis
Microtensile bond strength test (µTBS) and microleakage test data were analyzed with IBM SPSS v23 program (IBM Corp, Armonk, NY, USA). The relationship between µTBS data and dentin pretreatment applications and dentin tissue was examined by two-way analysis of variance. It was decided to use Bonferroni correction and Tamhaneʼs T2 in order to determine the source of the main effects and interactions determined as a result of variance analysis. Statistical significance of the data was accepted at P < .05 significance level.
Results
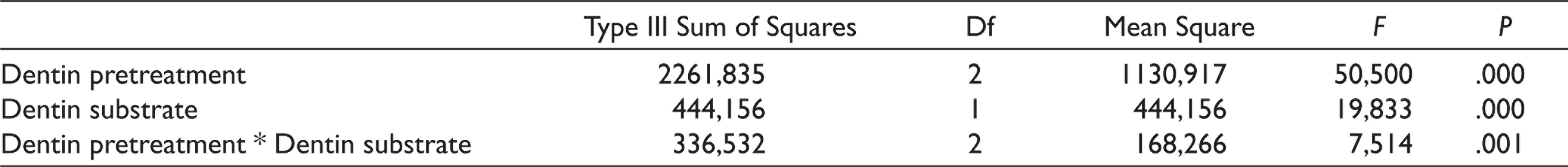
Descriptive statistics including mean and standard deviations of µTBS data are shown in Table 3. Two-way analysis of variance showed that dentin pretreatment applications, dentin tissue, and the interaction between these two parameters had statistically significant effects on µTBS values (P < .001; Table 4). Accordingly, µTBS values obtained in SD tissue were found to be statistically significantly higher than CAD µTBS values (P < .001). In addition, the application of dentin pretreatment with proanthocyanidin significantly increases the µTBS values of the samples (42,35), while pretreatment with lycopene shows the opposite effect and causes a serious decrease (32,86; P < .001). SEM microphotographs of the adhesive–dentin interfaces of the groups are shown in Figure 1. Resin monomer infiltration was detected in both SD and CAD interfaces, where dentin pretreatment was performed with proanthocyanidin, with a more uniform, regular, and deeper penetration in dentin tubules compared to other groups. On the other hand, on the SD and CAD surfaces, where lycopene was applied, an irregular, short or no resin tag formation was detected. In parallel with these results, in our study, the highest µTBS value was obtained in SD tissue treated with proanthocyanidin, while the lowest value was observed in CAD which was pretreated with lycopene.
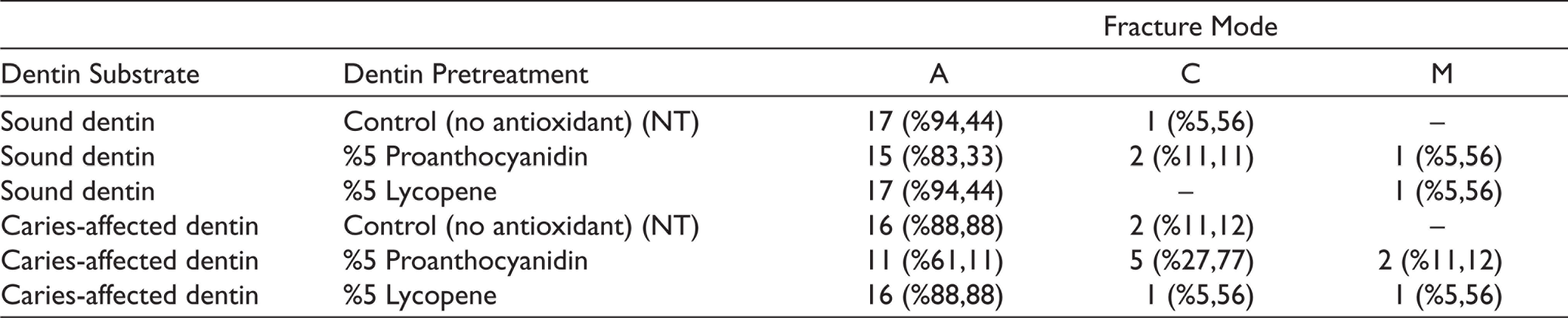
Failure modes of the samples after the microtensile bond strength test are shown in Table 5. When all groups were evaluated, the most common failure mode was 85.18% with adhesion failure, followed by cohesive (10.18%) and mixed (4.64%) failure types, respectively. In addition to this, the major failure mode is adhesives in CAD tissue, but it has been found that the cohesive failure type increases compared to SD tissue. From the point of view of dentin pretreatment, it was observed that the rates of cohesive failure in proanthocyanidin groups were relatively increased.
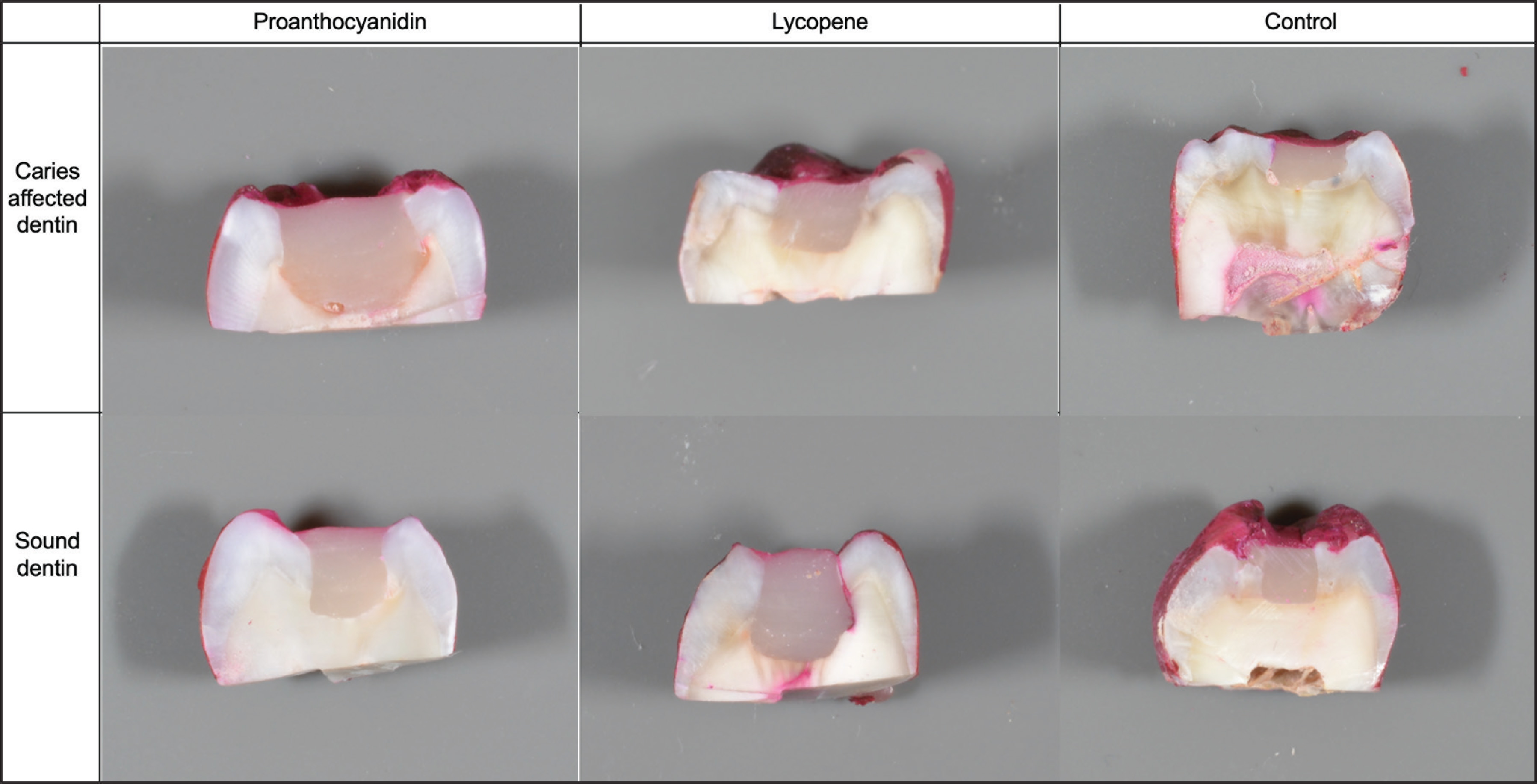
The images of microleakage scoring of the samples are shown in Figure 2. There was no difference between dentin pretreatment applications in terms of microleakage scores (P > .05). It was observed that dye penetration was limited to the exterior wall of the restoration and there was no microleakage as a major in both the control group and the surfaces where pretreatment was applied with antioxidant. However, considering the dentin tissue, it was determined that the samples with microleakage observed throughout the enamel were relatively more independent of pretreatment applications in CAD groups; however, this difference was not statistically significant (P > .05).
Descriptive Statistics of µTBS Values

Effects of Dentin Pretreatment and Dentin Substrate on µTBS
SEM Microphotographs of the Adhesive-Dentin Interfaces of the Groups

Failure Modes of Groups
Discussion
Because of the abundant water content and large volume of intertubular dentin structure, ensuring adequate adhesion to the dentin tissue is still a problem that restorative dentistry is still trying to overcome. 29 CAD is the most common tissue in the preparation performed with a minimally invasive approach, but it has a lower bond strength compared to SD. 30 Many researchers offer different adhesive strategies to deal with this issue. 31 Based on this problem, our study is one of the first studies to investigate the effects of proanthocyanidin and lycopene, which are natural antioxidants, as pretreatment agents on the SD and CAD surface on microtensile bond strength and microleakage.
The Images of Microleakage Scoring of the Samples
In our study, the microtensile bond strength of CAD and SD tissues were compared and significantly higher values were obtained in SD substrate (P < .001). Therefore, the first null hypothesis of our study was rejected. In some of the researches that deal with the bond strength of SD and CAD tissues, the CAD substrate obtained by using natural or different methods is compared with SD, 32 while in some of them the long-term continuity of the bond strength is evaluated in terms of substrate difference. 26 As a result of many studies, it has been emphasized that there is a difference between artificially obtained CAD and natural CAD texture, but it has been reported that the microtensile bond strength in SD is higher both in the short and long terms.4,26 The demineralisation cycle experienced in the caries process causes the mineral content to decrease in the dentin, increase the intertubular dentin porosity, 3 dissolve the apatite crystals, 33 and degrade the unprotected collagen with bacterial or host-derived enzymes. 27 The researchers agree that all these morphological changes are the main cause of both poor dentin hybridization and low connectivity.29,34 In addition, the literature has shown that collapsed collagen fibrils interfere with adhesive resin penetration, demonstrating that this is a distinct behavior for CAD tissue in all adhesive systems. 30 Our results are in line with the literature in the light of all these findings. In addition, shorter resin tag formation and irregular hybrid layer were detected in the SEM microphotographs of the CAD adhesive interface, confirming the mechanical results and the researchers’ comments.
The second null hypothesis tested in our study is that there will be no difference between proanthocyanidin and lycopene and dentin pretreatment in terms of bond strength. Our data showed that the application of proanthocyanidin dentin pretreatment increases the bond strength and lycopene causes a decrease. Therefore, our second null hypothesis was also rejected. Proanthocyanidin is a natural polyphenols and is also called tannin. 31 MMP inhibition and collagen are used because of their cross-linking properties in dentistry. 16 When combined with proteins, covalent, ionic, hydrogen bonding, and hydrophobic interactions are observed, and it is believed that it performs its functions.32,35 There are many studies reporting an increase in bond strength with proanthocyanidin in SD tissue.33,36 Many of these studies focused on their long-term success as they examined their effectiveness as an MMP inhibitor. However, a more limited number of studies have examined its interaction with CAD and has been proven to have a positive effect on immediate bond strength as a result.12,37 They even emphasized that after the pretreatment, the CAD bond strength approached SD values and observed a more homogeneous layer in SEM microphotographs and observed a more frequent and thick resin infiltration in the tubule. 33 Both the increase in the bond strength and the findings of SEM analysis confirm our study. However, the increase rate seen in these studies is much higher than our results. This may be because of the difference in application time and application concentration. However, as the other researchers stated, the application time was used only 10 min in our study because the prolongation of the application time would make it practically impossible. 35 In addition, only one study reported that there was no increase in µTBS values after pretreatment with proanthocyanidin in the literature. 24 However, this difference may be because of the fact that the restorative material evaluated for bond strength is a resin cement containing polyacrylic acid. Lycopene is another natural antioxidant with MMP inhibition feature proved in the laboratory environment, but its effectiveness in dentistry only on periodontal diseases has been discussed. There is only one study investigating the effectiveness of its use as an antioxidant on bond strength. 38 Although the research is focused on radicular dentin, it is noteworthy that the results of lycopene pretreatment groups were lower in the immediate, one week, and one month connection values compared to the control group. In our study, pretreatment with lycopene negatively affected the bond strength in CAD substrates and lower values were obtained from the control group. This may be because of the fact that lycopene has the ability to eliminate free radicals and has a more limited effect in MMP inhibition compared to proanthocyanidin. However, literature that examines the interaction of lycopene and CAD and where we can compare our results has not been found.
The major failure mode for the control and all our experimental groups after the µTBS test was adhesion failure. However, there was some increase in CAD tissue and groups treated with proanthocyanidin pretreatment, but this increase was not statistically significant (P > .05). Carvalho et al. reported that 63% of the major failure was adhesive in their studies evaluating failure modes after µTBS test in CAD tissue using different MMP inhibitors, but the coherent failure rate increased after green tea application. 4 Similarly, Costa et al. reported that the major failure type in all time periods was adhesion for both tissues in the µTBS test performed by CAD and SD samples after short- and long-term water storage. 26 Our results are in line with the general literature. However, Nakajima et al. reported that the major failure in CAD tissue is the cohesive type observed in dentin in their study comparing the failure mode difference between SD and CAD tissues. 3 This difference can be explained by the fact that the researchers obtained a thicker hybrid layer even it is porous and rich in collagen, and this maintained the continuity of the connection interface after the test. However, as it is known, while thicker hybrid layer is expected to be obtained in CAD texture, mineral accumulation in the tubule, namely whitlockite crystals, restricts this situation and, contrary to expectations, a thinner hybrid layer is obtained. 4
The third null hypothesis tested in our study is that there will be no difference in terms of microleakage between both pretreatment application groups and CAD and SD. In our findings, no difference was found between all groups in terms of microleakage. It was found that dye penetration was limited to the outer wall of the restoration and there was no microleakage, but there were relatively more samples in the CAD groups where microleakage was observed throughout the enamel in all groups. A single study that comparatively examined CAD texture and SD in terms of microleakage was found. It was reported that there was no difference in terms of microleakage between CAD obtained after chemomechanical caries cleaning and SD tissue obtained after drilling in research conducted by Hafez et al. In addition, in the SD group, there were no samples with microleakage, whereas it has been reported that there are microleakage samples seen along the enamel in CAD substrate. 39 However, there are no studies examining the effects of pretreatment applications on leakage at micro level and there are limited number of nanoleakage studies.13,40
The main purpose of dentin pretreatment processes is to increase the bond strength and to maintain this condition for a long time. However, in our study, only immediate bond strength was evaluated. In addition, leakage studies were carried out only at the micro level. Its effects on nanoscale have not been evaluated. For this reason, long-term clinical studies of the bond strength obtained are required.
Within the limitations of this study, the following conclusions can be drawn:
µTBS bond strength in CAD substrate is lower than SD (P < .001). Application of dentin pretreatment with proanthocyanidin is a successful procedure that increases the bond strength in both dentin tissues. While pretreatment application with lycopene does not affect the bond strength in SD, in CAD it reduces the bond strength of µTBS.
Footnotes
Acknowledgements
The authors wish to thank Dr Selçuk Gümüş for their assistance in generating SEM microphotographs and Dr Naci Murat for statistical analysis.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
