Abstract
Aim:
To assess if milled cobalt chromium (Co-Cr) alloy offers significantly better marginal accuracy than cast Co-Cr alloy for screw-retained long-span dental implant framework.
Materials and Methods:
A search PICO was formulated using suitable keywords and an electronic search was initiated. The databases of PubMed, Cochrane Library, Google Scholar and Embase were searched for related articles. Bibliographies of randomised control trials and reviews, identified in the electronic search, were analysed for studies published outside the electronically searched journals. Electronic search identified 26 studies. A total of 16 studies were eliminated after reading the abstracts. Out of the remaining 10 studies, 3 were eliminated based on the inclusion and exclusion criteria, and finally 7 studies were finalised for systematic review.
Results
Data were extracted from the included studies and analysed. The obtained data were suitable for meta-analysis, which showed an overall effect size z = 4.97 (P < .001) at 95% CI showing a significant statistical difference between milled and cast Co-Cr frameworks.
Conclusion:
Milled cobalt chromium frameworks are significantly more accurate than cast frameworks for long-span implant-supported frameworks used in dental prosthetic rehabilitation. More randomized controlled trials need to be conducted with a larger sample size to get a more authentic conclusion in a clinical scenario.
Keywords
Introduction
Accuracy, marginal adaptation, aesthetics, biocompatibility and mechanical strength are important determinants of successful implant prosthesis. 1 Fabrication of an implant-supported prosthetic framework is a technique-sensitive treatment with the probability of maximum lab errors.2,3 The survival of the implant following placement and the post-operative care of the patient also determines the future marginal bone loss around the implant as well as post loading of the implant.4,5
The stress on the bone–implant interface can be reduced by fabrication of passive frameworks using digital impression to achieve accuracy.6,7 Digital impressions can be recorded by intraoral scanners as well as lab scanners, both of which are highly accurate. 8 Prostheses which lack a passive fit do not marginally adapt with the abutment precisely and thus lead to a marginal gap > 50 m between the prosthesis and the abutment interface. 9 The long-term survival of the restoration also depends on the material used for the prosthesis. 10 Adequately recorded tooth preparation margins and healthy tissues surrounding the implant improve the longevity of the prosthesis.11,12 Retention of the prosthesis is another extremely important factor to be considered which would improve the survival and reduce the failure rates of the restoration. 13
Theoretically, the framework must induce absolutely no strain on the implant or its components and the surrounding bone in the absence of any external load. 14 The accuracy may also depend on many other factors including the location, direction and magnitude of applied load on the implant, design of the superstructure and the interpretation of the nature of stresses around the load-carrying implant. 15
Many systematic reviews have supported the use of computer-aided designing and computer-aided manufacturing (CAD/CAM) over cast frameworks for short-span bridges. 16 CAD/CAM techniques are reported to provide prostheses with marginal discrepancy less than 80 µm.17,18
Most commonly used materials for fabrication of these implant-supported frameworks are cobalt chromium, pure titanium and titanium alloys, zirconia and PEEK. However, the extent of marginal accuracy of milled frameworks over cast frameworks is not clearly reported in the literature and needs to be explored further. Hence, this systematic review was done with the aim to assess whether milled cobalt chromium alloy offers significantly better marginal accuracy than cast cobalt chromium alloy for screw-retained long-span dental implant framework.
Material and Method
This systematic review has been registered with PROSPERO registration number: 168618. This review was conducted from January 2019 to January 2020.
The review included articles from the year 2000 to 2019. RevMan data analysis software was used to analyse this study as well as perform the meta-analysis. The Quality Assessment of Diagnostic Accuracy Studies (QUADAS) checklists were used to assess the quality of the study. The final data extraction was done manually by two different observers and recorded. The Kappa score was 0.65 suggesting good inter-observer agreement. AND/OR/NOT were the Boolean operators used in PubMed to narrow or broaden the search to include as many relevant articles as possible.
Literature Search Protocol
The search for the articles was done by three reviewers independently. Publications of interest within the scope of this focused systematic review were searched in the electronic database National Library of Medicine (MEDLINE/ PubMed), Google Scholar, Cochrane Library, Embase, and by hand searching.
Inclusion criteria were randomized controlled trials evaluating marginal accuracy of cobalt chromium long-span dental implant frameworks, controlled clinical trials evaluating marginal accuracy of cobalt chromium long-span dental implant frameworks, in vitro trials evaluating marginal accuracy of cobalt chromium long-span dental implant frameworks and intra-oral implant frameworks in both maxilla and mandible. Exclusion criteria were finite element analysis studies, studies done on extraoral implant frameworks, zygomatic implant frameworks, orbital implant frameworks, auricular implant frameworks, transitional implant frameworks and implant frameworks in maxillofacial defects.
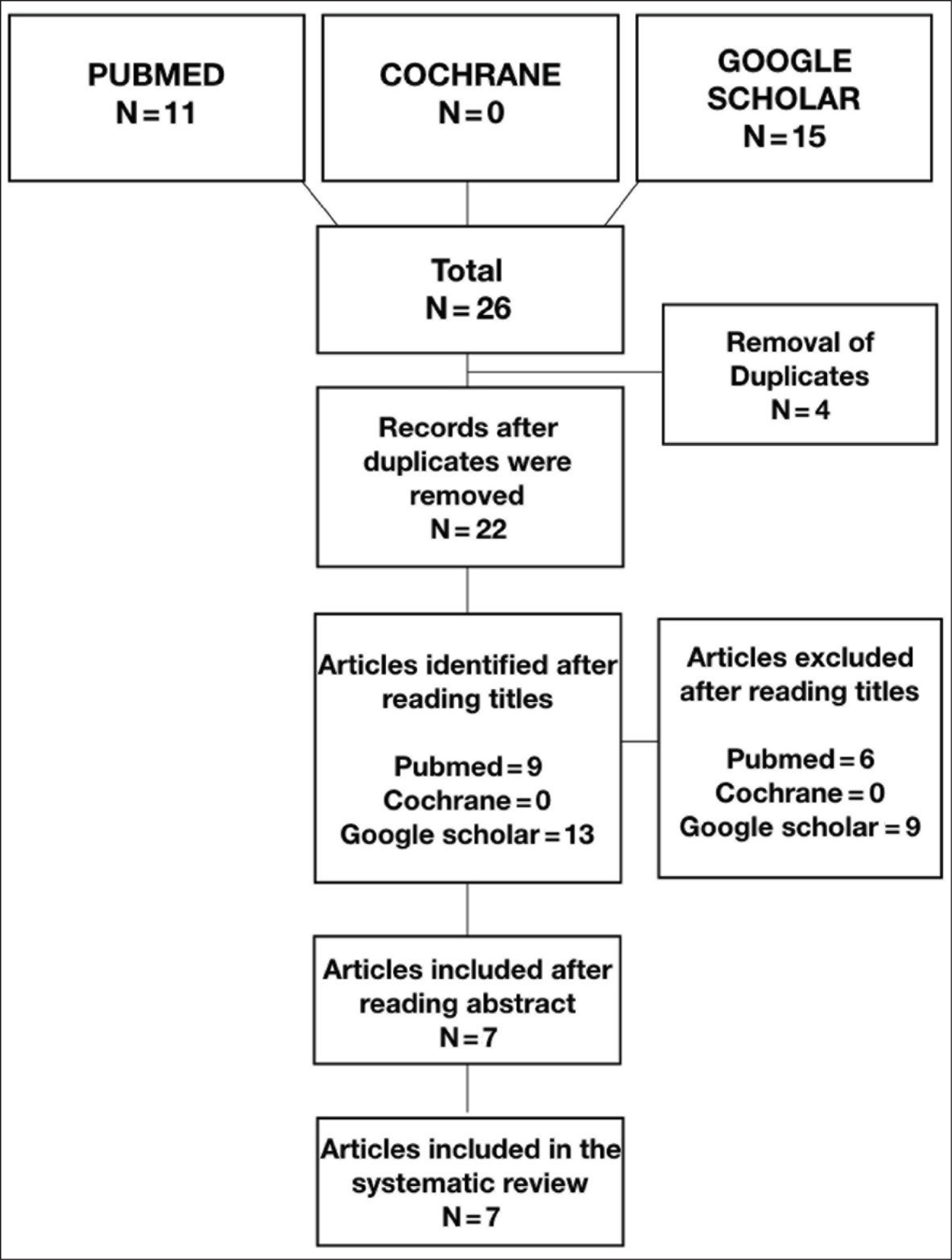
The initial search yielded 26 articles in the PubMed database, Google Scholar, Embase, Cochrane library, and hand-searched articles. Excluding all animal studies, case series, case reports, systematic review and duplicate studies, 10 articles were selected. These articles were screened based on the relevance of the title and abstract to the topic of interest. A total of 16 articles were excluded based on the exclusion criteria of this systematic review and full texts of 10 articles were analysed. Finally, 7 articles were chosen and 3 were excluded due to different comparison groups (Table 1, Figure 1).
Included Studies for the Systematic Review
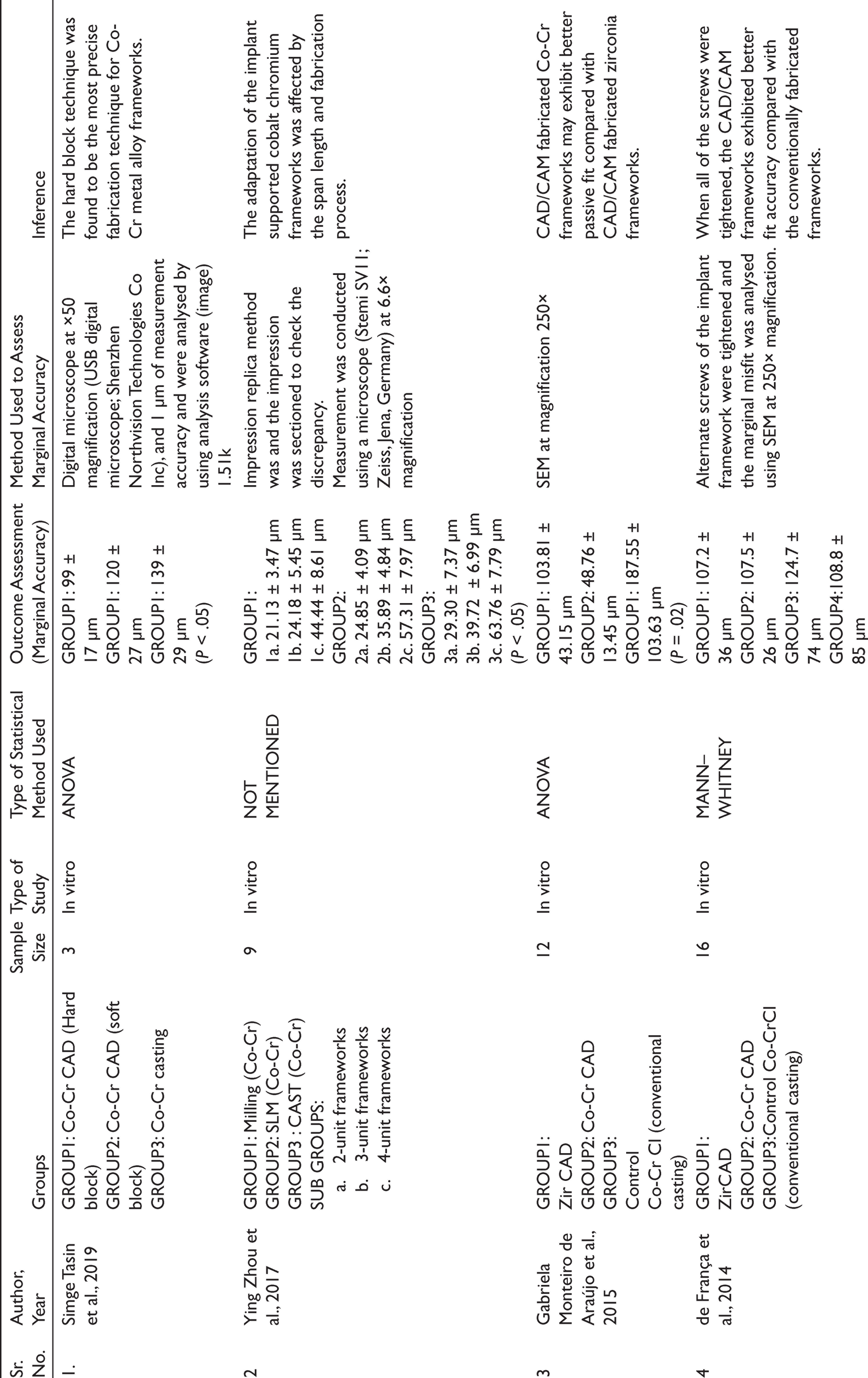
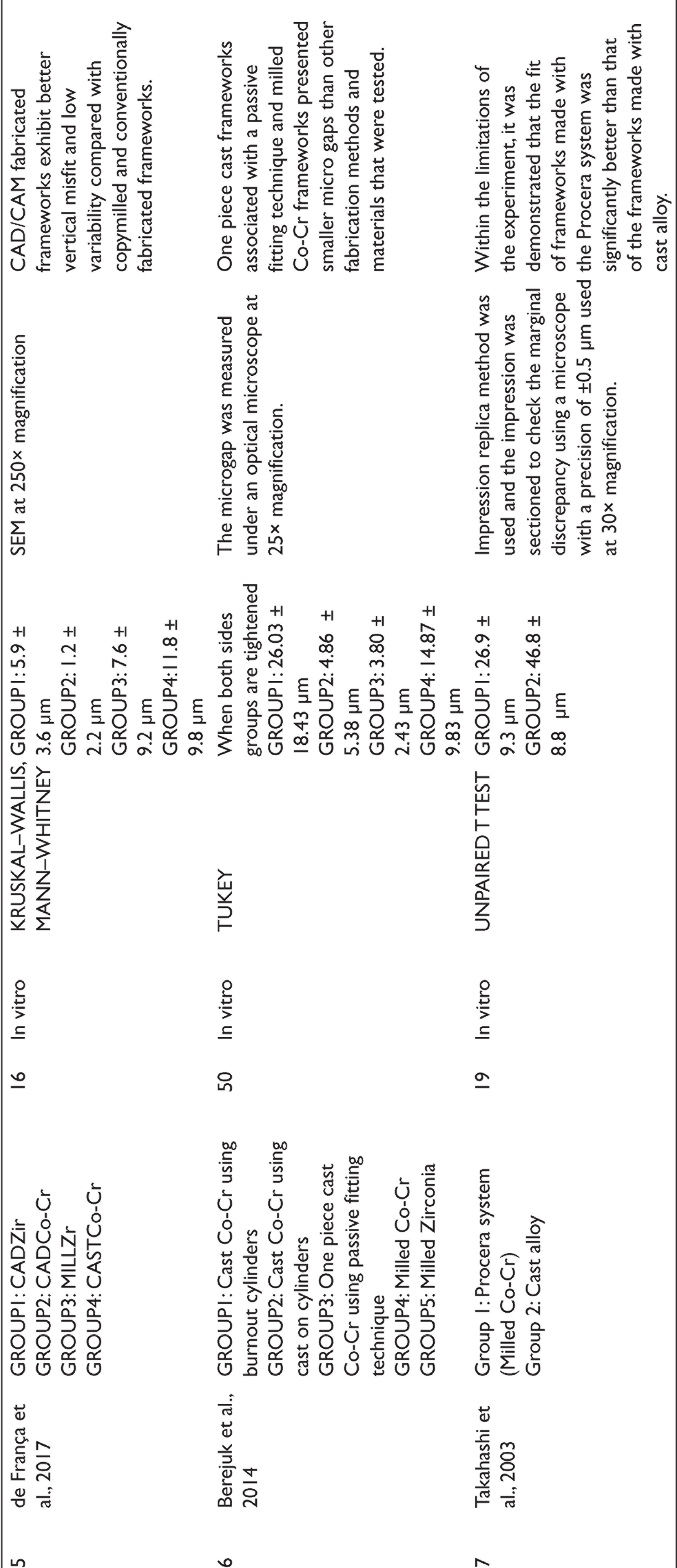
Image Representing the PRISMA Flow Chart for Search Methodology
Results
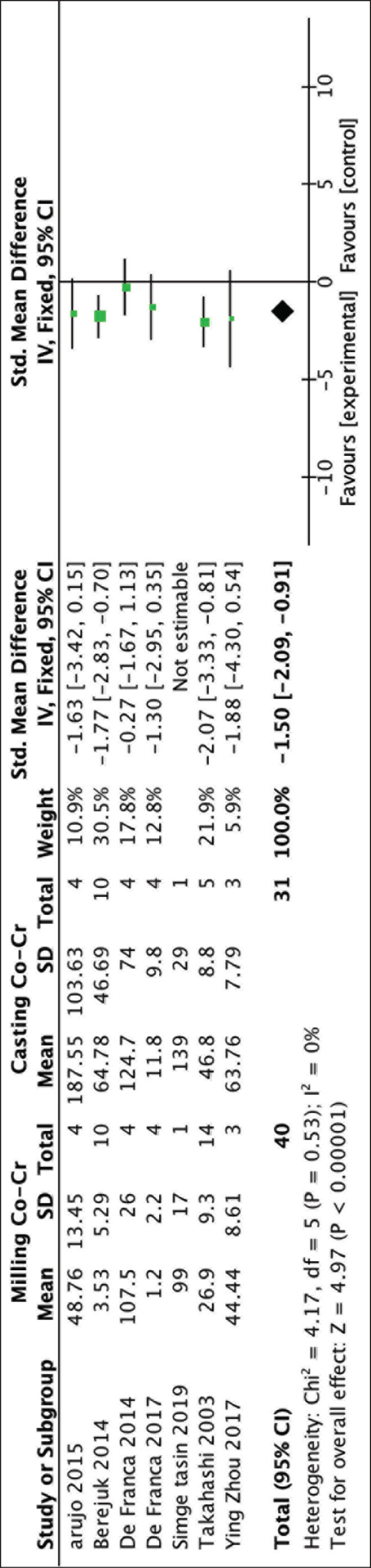
Data from the included studies were consolidated and the studies were not heterogeneous (Chi2 test = 4.17. df = 5 [P = .53] I2 = 0, α = 0.5). Hence, a meta-analysis with a fixed effects model was done (Figure 2). The software used to derive the result was RevMan 5.3 developed by the Cochrane Information Management System in Copenhagen, Denmark. The independent variables were the publication year, country and study size, whereas the dependant variables were the type of fabrication method, the instrument used for the measurement of the dimensional accuracy as well as the intervention it was compared to. Milled Co-Cr implant framework was the experimental intervention and cast Co-Cr was the control. The outcome measure was marginal accuracy expressed as mean difference was calculated. The pooled effect size, in this case the mean difference, was –1.50 (–2.09 to –0.91) and the overall treatment effect of Z = 4.97 showed a high statistically significant difference between the experimental and control groups (P < .001) with a confidence interval of 95%. Hence, it can be concluded that the experimental intervention milled Co-Cr implant framework showed less marginal discrepancy and more marginal accuracy than the cast Co-Cr which is the control intervention.
Image Representing the Pooled Estimate of Mean Difference in Marginal Accuracy Between Milled and Cast Co-Cr Long Span Dental Implant Framework

Discussion
In this systematic review, a total of seven in vitro studies were evaluated. All the seven studies evaluated the marginal fit and accuracy of the long-span implant supported frameworks fabricated by CAD/CAM and casting. Only two studies determined marginal accuracy along with the strain development in the framework. From this available evidence, the CAD/CAM-fabricated cobalt chromium frameworks showed the least marginal discrepancy between the implant and the framework interface in long-span implant-supported prosthesis. The meta-analysis favoured the milled cobalt chromium long-span implant frameworks.
In the included articles, it has been reported that scanning electron microscopy (SEM) imaging was better than light microscopy to evaluate marginal gap of class II CAD/CAM inlays. 19 Digital microscopy with different magnifications was the common method used to assess the vertical misfit of the frameworks in the above-reviewed studies.20,21 Araujo et al. and de Franco et al. used SEM at 250× magnification to estimate the micro-gap between the implant and abutment interface.22,23 Tasin et al. evaluated the marginal discrepancy using a digital microscope with 50× magnification.24,25 Zhou et al. evaluated the marginal accuracy using a microscope with 6.6× magnification. 26 Berejuk et al. used an optical microscope with a magnification of 25×, whereas Takahashi et al. used a microscope with a magnification of 30×.27,28 Zhou et al. and Takahashi et al. used the impression replica method followed by measurement with a microscope. 29
Zhou et al. had the maximum accuracy of the marginal fit amongst the studies reviewed. It can be suggested that Bego EOS M280 (Germany) milling machine used in this study produced the most accurate results compared to the other machines like Yenadent, Neoshape and Procera 30 used in the other studies. This cannot be generalized because Bego EOS was used only in one study for the fabrication of milled cobalt chromium long-span implant frameworks. 31 Two studies showed the strain development using a strain gauge stress analysis technique and photo elastic test.
Strain gauge was the sensor used; it provides resistance with applied force. The strain gauge stress analysis technique converts the force, pressure, tension and weight into a change in electrical resistance which can be measured in kilopascals. The strain development was analysed at the implant and framework interface as well as around the implant using a strain gauge stress analysis technique in the study by Tasin et al. Photo elasticity test studies the stress field around bi-material notches. Bi-material notches exist in many engineering applications like welded or adhesively bonded structures, interfaces of two surfaces, etc. It is popularly being used in dentistry. This technique was used to measure the strain around the implants by Araujo et al. 32
Both the studies showed a significant difference in the strain development around the implant and framework interface (P < .05). The strain development was less around the milled cobalt chromium frameworks than the casted frameworks. The cobalt chromium hard blocks with the lowest misfit values had the lowest strain values—81.1 ± 54 MPa after torque application. 33 Casted cobalt chromium implant framework presented the significant difference and had the highest average strain around the implants 17.19 ± 7.22 kPa using the photo elastic test (P < .020). The risk of bias of the included studies was high—Level 5 as analysed by the CEBM levels of evidence.
The limitations of the studies included in this review are discussed as follows. In the study by Tasin et al., the misfit and strain values were measured at only 1 prosthesis for each technique, which might not be representative of the technique’s overall accuracy. Furthermore, a single type of metal alloy was used for each technique; different types of alloy systems might reveal different results. The possible limitation of Araujo et al., however, is related to the number of specimens. The inclusion of more specimens would have posed significant practical and financial difficulties. In the study by De Franco et al., Zhou et al. and Berejuk et al., the number of specimens and the number of measurement points were less. Takahashi et al. had disproportionate samples in different groups; out of 19 frameworks, 14 made with the Procera system (type 1) and 5 made of a cast gold alloy (type 2) were fabricated.32,33
In this systematic review, only the in vitro studies have been used to formulate meta-analysis. More research is required to clarify practical matters using different methods to anticipate the maintenance level and the costeffectiveness of any system used for the fabrication of the prostheses. As for the clinical perspective, milled implant frameworks, especially for a long-span prosthesis, must be made a gold standard treatment due to its multiple advantages over cast frameworks.
Conclusion
This systematic review concludes that CAD/CAM fabricated long-span implant-supported frameworks are significantly more accurate than the casted long-span frameworks for implant-supported prostheses. Thus, milling must be opted as the recommended technique for the fabrication of implant-supported long-span cobalt chromium frameworks due to their high marginal accuracy.
Footnotes
Acknowledgements
I would like to acknowledge my colleagues who helped in the search for the final articles to be included in this study. I would like to thank my university for providing me with the opportunity to conduct this study.
Authors’ Contributions
All the authors contributed in the collection and analysis of the data.
Clinical Significance
Milled Co-Cr frameworks are recommended than cast frameworks in dental long-span screw-retained implant framework in clinical situations for better performance.
Data Availability Statement
All data generated or analysed during this study are included in this published article (and its supplementary information files).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
