Abstract
Purpose:
Proper placement of infra-acetabular screws is technically demanding; there is a limited safe zone for screw fixation because of the complexity of the bone anatomy around the hip joint and the vulnerability of the major neurovascular bundles in the pelvic cavity. We aimed to present the obturator hook technique as a surgical technique for infra-acetabular screw placement in acetabular and pelvic fractures and report its radiological outcomes.
Methods:
Patients treated with infra-acetabular screw placement using the obturator hook technique between January 2015 and August 2020 were enrolled in this study. We collected data on demographics, surgical approach, reduction status, complications, and outcomes. The radiological outcomes of infra-acetabular screw placement based on computed tomography findings were evaluated as follows: success, articular penetration, or out of the bone.
Results:
Thirty-five patients underwent infra-acetabular screw placement (26 men, 9 women; mean age, 55 years; range, 27–90 years). One patient underwent bilateral infra-acetabular screw placement; therefore, 36 infra-acetabular screws were inserted in all patients. An ideal placement was achieved with 27 infra-acetabular screws (27/36, 75%). Seven infra-acetabular screws (7/36, 19%) showed articular penetration, and two infra-acetabular screws (2/36, 6%) were placed outside the bone. One patient with articular penetration and mechanical symptoms of the hip joint required screw replacement. No other complications, including obturator nerve and vascular injuries, were observed.
Conclusion:
The obturator hook technique could be a favorable and individualized method for infra-acetabular screw placement in patients with acetabular and pelvic fractures.
Level of Evidence:
IV, retrospective descriptive study.
Introduction
An acetabular fracture is among the most challenging fractures in orthopedic trauma. The clinical outcomes of an acetabular fracture are influenced by multiple factors, including the patient’s preexisting conditions, injury-related elements, surgical factors, and postoperative management. Among the surgical factors, anatomical reduction of the articular surface and stable fixation permit an early range of motion and weight-bearing to ensure better outcomes regarding the management of acetabular and pelvic fractures. Numerous studies have reported a favorable prognosis for acetabular fractures after following these principles, 1 –4 and insufficient fixation around the pelvis and acetabulum may result in reduction loss, osteosynthesis failure, and osteoarthritis. 5,6 However, it is difficult to achieve stable fixation because of the limited safe zone for screw fixation owing to the complexity of the bone anatomy around the hip joint and vulnerability of vital organs and the major neurovascular bundles in the pelvic cavity.
The infra-acetabular screw was first introduced by Culemann et al. in 2011 7 ; since then, it has been used as a viable option for transfixation of the anterior and posterior columns. However, an improperly placed screw, such as a screw penetrating the hip joint or causing injury to the neurovascular bundles during acetabular fixation, can cause hazardous complications. 8,9 In addition, a three-dimensional computed tomography (CT)-based study demonstrated that the infra-acetabular corridor has a double-cone shape with a narrow isthmus and that infra-acetabular screws could be inserted at consistent angles in only 64% of the acetabulum. 10 These factors make the proper placement of infra-acetabular screws technically demanding. To the best of our knowledge, no specific technique has been designed to guide the proper placement of infra-acetabular screws. Therefore, we aimed to introduce a novel surgical technique for infra-acetabular screw placement in acetabular and pelvic fractures and report its radiological outcomes.
Materials and methods
Patients
This study was approved by our Institutional Review Board. We retrospectively reviewed the data of patients with acetabular or pelvic fractures who underwent open reduction and internal fixation between January 2015 and August 2020. We included patients who underwent infra-acetabular screw placement using the obturator hook technique (described below), which has been used since 2015. Patients with incomplete radiological and/or clinical data were excluded from the study. Data on demographics, acetabular fracture patterns, and associated injuries were collected from medical and radiological records and evaluated. We also collected data on infra-acetabular screw profiles, such as surgical approach, reduction status, complications, and outcomes.
Anatomical and radiographic landmarks
As infra-acetabular screws were inserted, the corridor was contained in a “teardrop” formed medially by the quadrilateral plate, laterally by the medial acetabular fossa, and basally by the acetabular notch in the inlet view (Figure 1). In addition, the following structures were visible on the radiographic images: superior and inferior walls of the acetabulum, subcotyloid groove, ischial tuberosity, and obturator crest (Supplementary Material 1).

Boundaries of the teardrop and radiological landmark. Boundaries of the teardrop are formed (a) medially by the quadrilateral plate, (b) laterally by the medial acetabular fossa, and (c) basally by the acetabular notch. (a) Quadrilateral plate forming the medial border: plates on the quadrilateral plate (black arrow) and dental hook hooking in the quadrilateral plate through the obturator groove from the outside. (b) Medial acetabular fossa forming the lateral border: plate on the medial acetabular fossa (black arrow). (c) Acetabular notch forming the base: dental hook-pointing acetabular notch (black arrow). (d) The outlet view clearly demonstrates the relationship between the medial and lateral boundaries of the infra-acetabular corridor in the coronal plane. A 3.2-mm S-pin was inserted from the pectineal surface to the ischial tuberosity.
Indications
For acetabular fractures, infra-acetabular screw placement was indicated in fractures that could benefit from additional infra-acetabular screw fixation via the anterior approach, which involves a fracture line descending along the acetabular fossa and reaching the obturator foramen, resulting in separation of both columns (anterior column, anterior column and posterior hemitransverse, transverse, T-type, and both column fractures).
For pelvic ring injuries, infra-acetabular screw placement was indicated in any fracture pattern where an augmentation of stability was needed with a long screw length (mean, 85.8 mm; range, 65–100 mm). First, it was indicated when the operator performed symphyseal plating and wanted to achieve maximal fixation strength through the Stoppa approach without a lateral window. Second, it was an available screw option when fixation of both pelvic ring injury and acetabular fracture was needed using a single plate. Third, when screw fixation on the pubic ramus was necessary but difficult because of fracture comminution, an infra-acetabular screw was placed to achieve stable purchase through the use of long screws without elongation of the plate to the posterior side and without a lateral approach.
Preparation
The patients were placed in the supine position on a radiolucent table that allowed easy access to the C-arm image intensifier. The affected limb was draped freely to allow hip and knee motions that are required during surgery. The screw could be placed through the pararectus approach, second window in the ilioinguinal approach, and lateral corner in the modified Stoppa approach.
Decision on the starting hole
After the plate was placed along the pelvic brim, pectineal eminence, and superior aspect of the pubic ramus, the location of the starting hole could be determined. The screw was placed on a plate. The starting hole location was determined on the basis of two points: the nearest hole from the center of the circle in the “teardrop” in the inlet view and the hole closest to the hooked finger.
Obturator hook technique
This technique has been described for a right-handed operator. Herein, the operator performs drilling with trajectory control using the right hand while receiving tactile feedback from the left hand.
Right acetabulum or pelvis
The operator can insert the infra-acetabular screw, standing on the right or left side of the patient, depending on the surgical situation. After the location of the starting hole was determined, the ulnar border of the distal phalanx of the index finger of the left hand was placed in the obturator groove with supination of the left hand. Thereafter, the index finger of the left hand was advanced along the obturator groove from the inner surface to the outer side, and the ulnar border of the middle phalanx of the index finger of the left hand was placed on the quadrilateral plate. As the hooked finger encircles the trunk of the pubic ramus, we named this technique the obturator hook technique. The ulnar border of the distal phalanx of the index finger of the left hand was placed at the superolateral shoulder of the outer surface of the obturator canal. Thereafter, the ulnar border of the middle phalanx of the left hand was placed on the superoanterior edge of the quadrilateral plate (Figures 2 and 3).

Illustration of the obturator hook technique performed in the right acetabulum or pelvis. In this technique, the index finger is hooked in the obturator notch and quadrilateral plate. (a) The ulnar border of the distal phalanx of the index finger is placed in the obturator notch. (b) The ulnar border of the middle phalanx of the index finger is placed on the quadrilateral plate. (c) The markings copied on the finger from the pelvic bone model demonstrate the tactile areas of the finger.

Intraoperative image of the obturator hook technique performed in the right acetabulum. Drilling using a K-wire by the right hand was performed with the hooked index finger of the left hand in the obturator notch through the pararectus approach on the acetabulum.
Left acetabulum or pelvis
We recommend standing on the left side of the patient when inserting the infra-acetabular screw on the left acetabulum or pelvis. With pronation of the left hand and flexion of the left wrist, the radial border of the index finger of the left hand was placed in the obturator groove. This hooked finger allowed palpation of the outer, inner, and anterior surroundings of the bony margin of the safe corridor, which aided in controlling the trajectory of the drill bit and protected the obturator nerve and artery by pulling them away from the superolateral corner of the obturator foramen (Figure 4). If the operator places the left index finger with supination, which is a posture similar to that when performing the surgery at the right acetabular or pelvis, the right hand must cross the left hand because the drilling (which is performed using the right hand) is placed on the left side of the obturator groove. This position can make the operator uncomfortable.

Intraoperative image of the obturator hook technique performed in the left acetabulum. Left acetabulum surgery through the pararectus approach and the upper part of the image is the foot direction. (a) With pronation of the left hand and flexion of the left wrist, the radial border of the index finger of the left hand is placed in the obturator notch and quadrilateral plate during drilling performed with the right hand. (b) The hooked index finger protects the obturator nerve (white arrow) by pulling it away from the superolateral corner of the obturator foramen. The white asterisk indicates the left quadrilateral plate, and the black asterisk indicates the left superior ramus.
Drilling and screw insertion
The space between the medial acetabular fossa and quadrilateral plate is approximately 4 mm in the Asian population. 11 Thus, a 3.5-mm cortical screw was used through the plate in all surgeries. As a 2.4-mm K-wire is flexible and its trajectory is easy to control, we routinely used this type of K-wire instead of a drill bit to identify the available intramedullary corridor. After the sharp end of the K-wire was advanced in the near cortex, intraoperative fluoroscopy in the obturator outlet view was performed to confirm the sagittal trajectory. The fluoroscopy view was then changed to the outlet view, wherein the coronal trajectory was controlled, keeping the sagittal trajectory unchanged. As the K-wire advanced slowly in the oscillation mode, the operator could feel the vibration, which was transmitted to the hooked finger, and could estimate and control the trajectory of the K-wire.
After the K-wire crossed the fracture line along the proper corridor, it could be advanced into the ischial tuberosity. The location of the K-wire was checked in the inlet, iliac wing outlet, and obturator outlet views of the image intensifier. Thereafter, the K-wire was replaced with 3.5-mm cortical screws. Finally, the position of the screw was confirmed in the inlet, iliac wing outlet, and obturator outlet views (Figure 5).

Intraoperative and postoperative radiographic images and postoperative CT scan of infra-acetabular screws. (a) The K-wire is advanced under the outlet view of the image intensifier demonstrating the K-wire passing between the acetabular fossa and the quadrilateral plate. (b) Postoperative radiographic image and (c) CT scan present the ideal placement of the infra-acetabular screw. CT, computed tomography.
Evaluation
Matta’s criteria, which were based on radiographic findings, were applied to the CT scans. 12 Gap or step displacement in the weight-bearing dome was measured in the axial, sagittal, and coronal planes independently on the CT scans, and the quality of reduction was graded as anatomic (0–1 mm of displacement), imperfect (2–3 mm), or poor (>3 mm). The length of the infra-acetabular screw was measured on the postoperative CT scan, which was reconstructed with a plane with the infra-acetabular screw used as an axis using a standard Digital Imaging and Communications in Medicine (DICOM) viewing software (RadiAnt DICOM Viewer Version 2020.1.1). The outcome of infra-acetabular screw placement was described as successful, hip joint penetration, or out of the bone based on the CT findings (Figure 6). The outcome was described as successful in cases wherein the infra-acetabular screws were located within the double-cone-shaped corridor on every axial CT scan. Articular encroachment of the hip joint and out-of-the-bone screw placement were evaluated. The causes of failure were analyzed by two senior authors from the postoperative CT scan, which was reconstructed with a plane with the infra-acetabular screw used as an axis. Complications, such as mechanical symptoms after joint encroachment, obturator nerve injury, and vascular injury, were evaluated using information from the patients’ medical records.
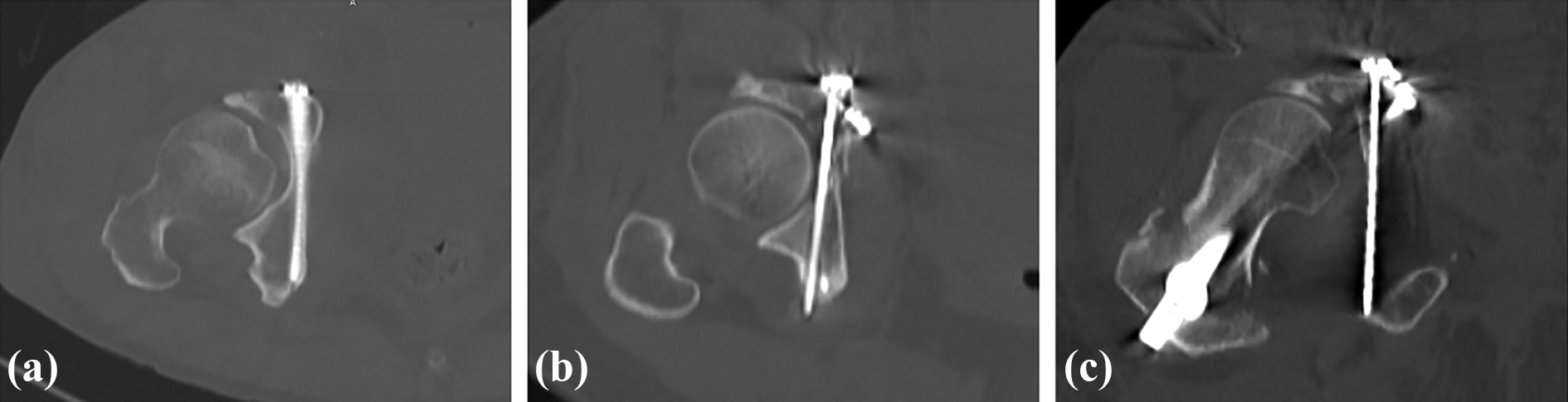
Outcomes of infra-acetabular screw placement described as success, hip joint penetration, or out of the bone. (a) Success: ideal placement of infra-acetabular screws; (b) hip joint penetration: any articular penetration; and (c) out of the bone: screws extending out of the bone.
Results
Thirty-five patients underwent infra-acetabular screw placement at our institution (Table 1). One patient underwent bilateral infra-acetabular screw placement, one for an acetabular fracture and the other for an anteroposterior compression injury. Therefore, 36 infra-acetabular screws were inserted in all patients. Twenty-nine patients had acetabular fractures and needed open reduction for insertion of the infra-acetabular screw, and six patients were treated for a pelvic ring injury. The quality of reduction for the acetabular fractures was anatomical in 7 patients (24%), imperfect in 11 (38%), and poor in 11 (38%).
Demographics, fracture patterns, associated injuries, surgical approaches, reduction status, complications, and outcome of the obturator hook technique (36 infra-acetabular screws; 35 patients).

a Calculated based on 35 patients.
b Calculated based on 29 acetabular fractures.
The mean length of the infra-acetabular screws was 85.8 mm (range, 65–100 mm). Twenty-seven of the 36 infra-acetabular screws (75%) were placed in the proper location. Seven screws (19%) showed hip joint penetration on the CT scan, and the remaining two (6%) were placed out of the bone. One patient with mechanical symptoms of the hip joint that required screw replacement presented with articular penetration. The other patients did not present any mechanical symptoms of hip joint penetration and signs of neurovascular involvement on physical examination.
The causes of failure could be classified into three scenarios. Three patients demonstrated persistent displacement of the quadrilateral plate, which hindered the passage of the infra-acetabular screw. Four patients presented “too narrow corridors,” defined as corridors sized <3.0 mm. 11 In the remaining two patients, the cause was related to technical failure, which was the selection of a wrong starting hole or wrong direction of the infra-acetabular screw, even though there was neither persistent displacement of the quadrilateral plate nor too narrow corridor. No other complications, including obturator nerve and vascular injuries, were observed. The profiles of the individual patients who underwent infra-acetabular screw placement are described in detail in Supplementary Material 2.
Discussion
The role of the infra-acetabular screw as a barrier for preventing quadrilateral plate redisplacement is well known. This encourages surgeons to perform infra-acetabular screw placement, despite technical difficulties. May et al. reported that the placement of additional periarticular screws along the quadrilateral plate increased the fixation strength and that the effect of a buttress plate alone might be questionable in a biomechanical study of an anterior column and posterior hemitransverse fracture model. 13 Meanwhile, other biomechanical studies have shown a significant reduction in maximum fracture displacement with additional infra-acetabular screws, independent of the use of implants, in anterior column fracture models. 14,15
The infra-acetabular corridor has been widely studied owing to its unique characteristics related to the transfixation of the anterior and posterior columns. Baumann et al. proposed the following optimal starting point for intra-acetabular screws: 10.2 mm caudal and 10.4 mm medial to the iliopectineal eminence and suggested sex-based differences in the starting angle. 16 Gras et al. reported that the corridors in men are larger and approximately parallel to the sagittal midline plane and that those in women are tilted from the medial to the lateral direction, based on their CT-based analysis findings. 10 However, in actual surgical situations, the starting point for infra-acetabular screws is clinically decided on the basis of the plate position. Inter-individual adjustment of the corridor angle is then required according to the starting point (Figure 7). From this point of view, our technique could be an option for fine-tuned placement of infra-acetabular screws. The drilling direction could be approximately estimated through the hooked index finger, and fine tuning would be possible in response to tactile feedback from the quadrilateral plate and obturator groove.

Examples of the coronal direction and angle of the infra-acetabular screw decided according to the plate hole. (a) With the medial starting point on the plate, the screw direction should be from the medial to the lateral direction. (b) The screw direction is decided on the basis of the lateral starting point and intrinsic medial direction of the quadrilateral plate.
In our study, 27 infra-acetabular screws (27/36, 75%) were appropriately inserted using the obturator hook technique, as observed on the CT scans; however, the actual success rate could be lower because other cases might have ended up as empty holes, which were not counted. To the best of our knowledge, no published study has assessed the success rate or clinical complications of infra-acetabular screw placement; therefore, it is difficult to compare our results with those of other studies. A CT-based study in an Asian population showed that 20% of the infra-acetabular corridors were not feasible for the placement of infra-acetabular screws. 11 Considering the previously reported percentage of uninjured corridors, our study suggests that the obturator hook technique is a reliable method for infra-acetabular screw placement. The hooked finger in this technique is useful for the placement of infra-acetabular screws in several manners: 1) it facilitates the selection of the starting hole in the plate; 2) it estimates the anterior, inner, and outer boundaries of the available corridor and reduces the risk of disastrous perforation into the pelvic cavity or hip joint; and 3) the obturator nerve and artery can be protected by pulling them away from the superolateral corner of the obturator foramen.
It would be beneficial to statistically analyze the causes of placement failure. However, as we included only a few cases, we can only define the causes of failure based on the discussion of senior authors. First, there was persistent displacement of the quadrilateral plate after reduction, which hindered the passage of infra-acetabular screws. Especially in fractures with displacement at the acetabular fossa, the infra-acetabular screw, which is usually well contained in the infra-acetabular corridor of the anterior column, could exit the bone or penetrate the hip joint in the posterior column. Second, patients who have a corridor that is too narrow for infra-acetabular screws are ineligible for the procedure. Regardless of the inclination of the infra-acetabular screw (more caudal or more cranial), there is no space for fixation of the infra-acetabular screw. Third, technical factors, such as incorrect choice of the entry hole and insufficient proficiency in this technique, can make it difficult to insert infra-acetabular screws. A detailed description of these factors is provided in Supplementary Material 3.
There are concerns on the reproducibility of our technique, which is affected by several factors, such as the size of the individual fingers, approaches, local anatomy, soft tissues, and body habitus. Several prerequisites should be considered to increase its reproducibility. The presence of an available corridor is required, i.e., sufficient width of the infra-acetabular corridor and acceptable or anatomical reduction of the quadrilateral plate, which makes insertion of the infra-acetabular screw amenable. In addition, an approach that offers sufficient space and soft tissue tension for positioning the index finger, selecting the ideal entry point, and handling the trajectory is needed. The reproducibility of our technique would be considerable if these conditions were achieved beforehand.
To overcome the causes of failure and factors related to reproducibility, we suggest several methods. Accurate reduction is important to achieve successful insertion of infra-acetabular screws, and the width of the corridor can be checked from the contralateral intact corridor using a preoperative CT scan. Estimation of the appropriate entry hole considering the coronal direction of the quadrilateral plate is also required. Practice using a sawbone or cadaver is recommended to increase the proficiency for our technique. We believe that the success rate will increase with thorough accurate reduction, preoperative planning, and sufficient practice.
The iliac wing outlet view proposed by Culemann et al. would be advantageous for visualizing hip joint penetration because the fluoroscopic beam of the iliac wing outlet view is in the same plane as the quadrilateral plate. 7 In our technique, we recommend placing the infra-acetabular screws under the outlet fluoroscopic view, as it is more intuitive than the under the iliac wing outlet view to adjust the position of the single coronal plane, while the position of the sagittal plane is fixed. We then confirmed hip joint penetration of the infra-acetabular screws under the iliac wing outlet view and out of the bone under the obturator outlet view, although these views could not completely predict the malposition of the infra-acetabular screws.
This study has several limitations. First, owing to the retrospective study design, it was not possible to evaluate the reproducibility of our findings accurately, although we thoroughly examined all surgical records, fluoroscopic images, and postoperative CT scans. In addition, missing “attempted” cases could contribute to overestimation of the success rate. Second, statistical analysis of the factors affecting the failure of infra-acetabular screw placement and reproducibility was not performed owing to the small sample size in this study. These factors can be affected by other unrevealed confounding factors that were not mentioned above, which warrant further research.
Conclusion
The obturator hook technique described herein is a favorable and individualized method for infra-acetabular screw placement in patients with acetabular and pelvic fractures.
Supplemental material
Supplemental Material, sj-docx-1-osj-10.1177_2309499021996838 - Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement
Supplemental Material, sj-docx-1-osj-10.1177_2309499021996838 for Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement by Eic Ju Lim, Seungyeob Sakong, Whee Sung Son, HanJu Kim, Jae-Woo Cho and Jong-Keon Oh in Journal of Orthopaedic Surgery
Supplemental material
Supplemental Material, sj-docx-2-osj-10.1177_2309499021996838 - Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement
Supplemental Material, sj-docx-2-osj-10.1177_2309499021996838 for Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement by Eic Ju Lim, Seungyeob Sakong, Whee Sung Son, HanJu Kim, Jae-Woo Cho and Jong-Keon Oh in Journal of Orthopaedic Surgery
Supplemental material
Supplemental Material, sj-docx-3-osj-10.1177_2309499021996838 - Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement
Supplemental Material, sj-docx-3-osj-10.1177_2309499021996838 for Usefulness of the obturator hook technique for guiding the initial trajectory control in infra-acetabular screw placement by Eic Ju Lim, Seungyeob Sakong, Whee Sung Son, HanJu Kim, Jae-Woo Cho and Jong-Keon Oh in Journal of Orthopaedic Surgery
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by a grant from Korea University (Grant Number K1609761).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
