Abstract
Purpose
This study aimed to evaluate the effectiveness of watching video records of their shoulder motion changes on functional outcomes and quality of life after arthroscopic rotator cuff repair (ARCR).
Introduction
Rotator cuff disorders impair the health-related quality of life, increase healthcare resources, and cause significant labor. 1 Rotator cuff tear (RCT) is reported as one of the most common shoulder disorders that cause pain, weakness, and disability. 2 Arthroscopic rotator cuff repair (ARCR) is a widely accepted treatment method for full-thickness rotator cuff tear (RCT) and is performed with increasing frequency. 3 The treatment goals are relief of pain, recovery of strength, increasing the range of motion (ROM), and returning function to daily activities. 1 Several patient-related factors were described associated with patient satisfaction following ARCR, such as age, gender, tear size, workers’ compensation status, marital status, employment, preoperative expectations, and medical comorbidities.4,5 However, recent evidence supports a biopsychosocial model in which psychosocial factors and certain constructs such as anxiety, depression, and fear-avoidance beliefs are associated with patient-reported outcomes. 6
Image capture is essential for recording, creating presentations, publications, documentation in patient registration and has traditionally played an essential role in academic orthopedic surgery practice. 7 Besides image capture, video records can be useful for lower literacy levels, as they do not rely on literacy areas for information. 8 Observational analysis without video may lack accuracy and fail to detect limitations of the joint motion. Video records can be reviewed with patients to increase and motivate shared decision making, understanding, and commitment and encourage self-management. Also, visual feedback of impaired movement patterns through recorded videos can increase patient motor learning and help them self-assess. 9 There are not many studies on video and its effect on results in orthopedic surgery. Besides, there are no studies in the literature regarding the effectiveness of video regarding functional outcomes and changes in patients’ quality of life after shoulder RCR and patients’ self-evaluation. In our study, we hypothesized that video recording of patients before and after RCR and sharing these images with patients could help improve the patients' clinical outcomes and quality of life.
Materials and methods
Patient selection
This is a retrospective study, including prospectively collected data. Patients who underwent ARCR surgery between October 2016 and March 2020 were evaluated after obtaining the institutional research ethics committee approval. The patients who had video records before and after the surgery were classified as Group 1, and the patients who did not receive video records as Group 2. The inclusion criteria were 1- patients received ARCR for full-thickness rotator cuff tear, 2- patients over the age of 18, 3- who had Goutallier grade 0.1 or 2 fatty degeneration at the supraspinatus muscle, 10 and small to large-sized full-thickness RCR in magnetic resonance imaging (MRI) according to DeOrio and Cofield classification. 11
The exclusion criteria for the study were 1- acute traumatic tears, 2- arthritic changes in the shoulder joint, 3- preoperative frozen shoulder, 4- previous surgery from the ipsilateral shoulder, 5- partial supraspinatus tear, 6- Goutallier grade 3 or 4 fatty degeneration at supraspinatus muscle, 7- concomitant subscapularis tendon tear, 8- open rotator cuff repair, 9- concomitant Bankart lesion, 10- concomitant Hill-Sachs lesion, 11- previous septic arthritis of the shoulder, 12- the presence of symptomatic acromioclavicular arthritis, 13- history of rheumatologic diseases, 14- loss of follow-up, and 15- previous shoulder fractures.
Of the 330 patients who operated for rotator cuff tear, 223 patients were eligible for the study. Twenty-seven patients were lost or refused to be included in the study. One hundred ninety-six patients were included in the study; 76 patients were in Group 1, and 120 patients were in Group 2.
Video recording procedure
Video records of the patients in Group 1 were obtained preoperatively and at the sixth-month follow-up visit. All video records were taken in the same room, by the same physiotherapist, at the same distance, and at the same light intensity with the Canon XF305 Professional 50 Mbps Camera. 12 All patients were informed about the video recording process. While taking video records, patients were asked to perform shoulder abduction, flexion, external rotation, and internal rotation movements as much as possible. Participants perform each of the four active shoulder movements with 1-minute rest intervals between consecutive video recordings.
Clinical evaluation
The Constant-Murley score (CS),
13
The American Shoulder and Elbow Surgeons (ASES) Score,
14
The Short-Form Health Survey (SF-36),
15
and active shoulder range of motion (ROM) were measured at the pre- and sixth postoperative month by a single physiotherapist. Shoulder flexion was assessed by asking the patient to raise the arm as much as possible over the head. Shoulder abduction was achieved by providing scapular stabilization (by an assistant) to the patient’s scapulothoracic movement by asking the patient to elevate his maximum arm laterally in the coronal plane. The external shoulder rotation was removed by placing the patient’s arm in 90 degrees of flexion and 90 degrees of abduction passively. The patient was asked to rotate the arm as far back as possible with the palm facing the ceiling. Shoulder internal rotation was obtained by placing the patient's arm in 90 degrees of flexion and 90 degrees of abduction passively. The patient was asked to rotate the arm forward as much as possible. Figure 1 shows preoperative and Figure 2 postoperative views of a sample patient (Figures 1 and 2). Preoperative images obtained from video of a patient in Group 1. Postoperative images obtained from video of a patient in Group 1.
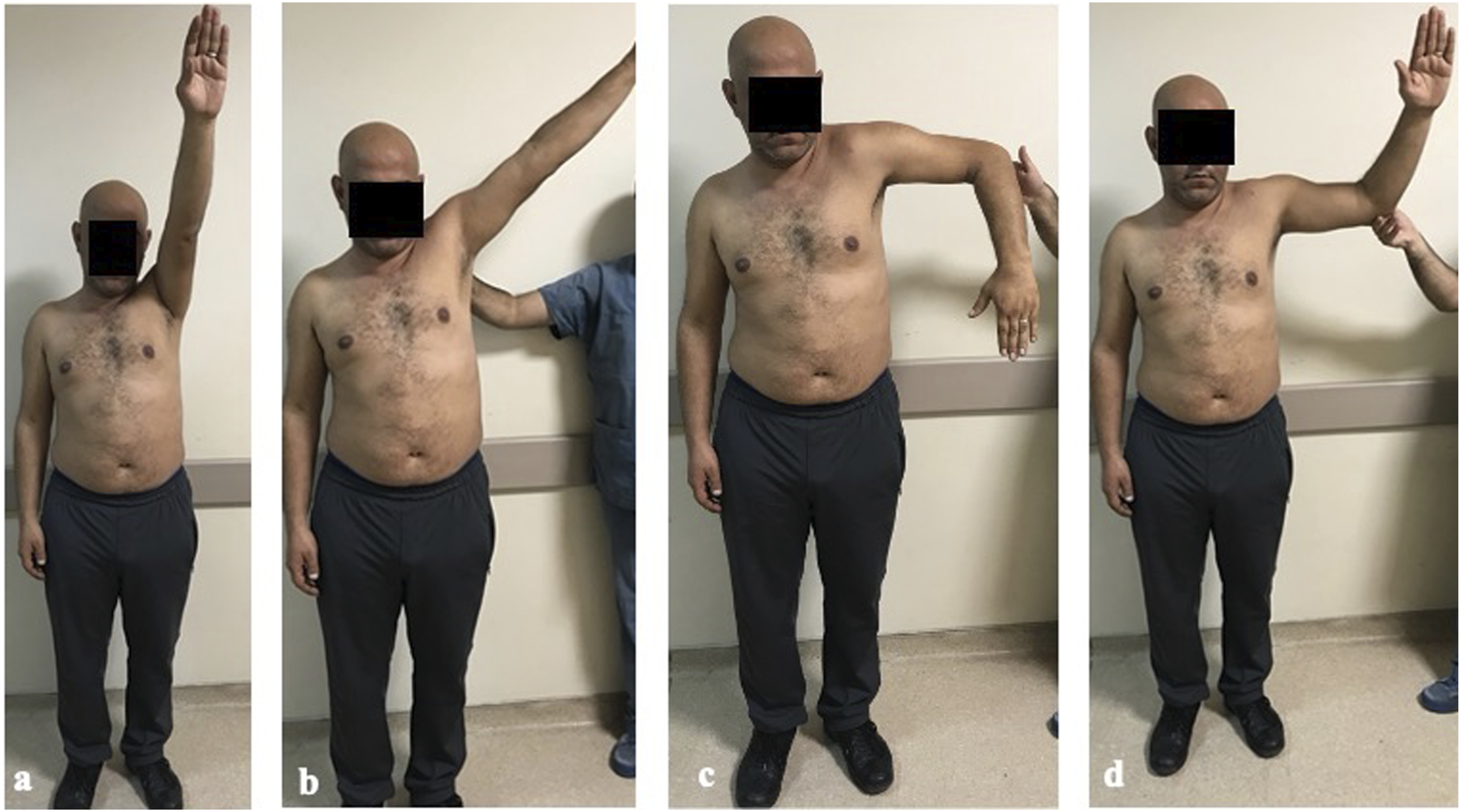
All postoperative measurements were done in the sixth postoperative month. In Group 1, all patients completed the ASES Score, the CS, and the SF-36 questionnaires first. Then, the patient’s active shoulder motions were recorded by a video camera. Then, the patients were invited again; preoperative and postoperative video records were shown to them, and they were asked to complete all questionnaires again. In all patients, the two postoperative scores were obtained at 10–20 days intervals.
Previously, minimal clinically important difference (MCID) values of ASES and CM had been reported. For ASES, 12 to 17 point change was reported. 16 For CM 15 point was reported. 17
Surgical technique
All patients were operated on by two experienced surgeons under general anesthesia in the beach chair position. Firstly, diagnostic arthroscopy was performed to evaluate the RCT’s extent, lesions of the biceps tendon, and other associated intracapsular pathologies. The ARCR was performed by placing one or two rows of suture anchors double-loaded in the footprint’s lateral aspect. The number of suture anchors varied with the tear’s size, the type of repair techniques, and the surgeon’s decision. Tenotomy was performed on all patients.
Postoperative rehabilitation
In all patients, the arm was immobilized in a neutral position with a shoulder sling for 6 weeks. Pendulum exercises were started five times a day on the first postoperative day. After 6 weeks, patients were allowed an active range of motion exercises. Strengthening exercises were started after the postoperative 3 months.
Age, gender, tear size, and demographic data of the patients were recorded. Preoperative and postoperative functional results, quality of life measures, and ROM were compared for each group. Postoperative first and second measures were also compared in Group 1 and Group 2, and those measures were compared between the two groups. Also, a subgroup analysis was performed to detect the effect of tear size on outcome measures in each group.
Statistical analysis
The data were presented as mean ± standard deviation, frequency, and ratio. The Kolmogorov–Smirnov test was used to determine the normality of the data. The Paired samples t-test and Wilcoxon test were used for the analyses of quantitative dependent data. The independent samples t-test and Mann–Whitney U test were used in the analyses of independent quantitative data. The Chi-square test was used in the evaluation of independent qualitative data. A p-value < .05 was considered statistically significant. According to the a priori sample size calculation, a total of 72 patients per group were needed to detect statistically significant difference in comparisons with 0.80 power and 0.05 type 1 error rate associated with the null hypothesis. Sample size calculation was performed using G-power (version 3.1.9.0, Franz Faul). All analyses were performed with SPSS IBM Statistics (version 23; IBM, Armonk, NY).
Results
Comparison of demographic variables between the two groups.

DM: diabetes mellitus.
aObesity defined as body mass index ≥ 30 kg/m2.
Comparison of preoperative and postoperative functional scores, quality of life measures, and ROM between two groups.

ASES: American Shoulder and Elbow Surgeons Survey, CM: Constant Murley Score, SF-36: Short-Form 36, SD: Standard Deviation. Bold values indicate statistical significance.
Comparison of postoperative first-time outcome values in both groups. (mean ± SD).

Abbreviations: ASES, American Shoulder and Elbow Surgeons Survey; CM, Constant Murley Score; SF-36, Short-Form 36; SD, Standard Deviation. Note: Boldface values indicate statistical significance.
Comparison of first postoperative (pre-video) measures and second postoperative (post-video) outcome values in the group 1. (mean ± SD).

Abbreviations: ASES, American Shoulder and Elbow Surgeons Survey; CM, Constant Murley Score; SF-36, Short-Form 36; SD, Standard Deviation. Note: Boldface values indicate statistical significance.
Comparison of first postoperative and second postoperative outcome values in the group 2. (mean ± SD).

Abbreviations: ASES, American Shoulder and Elbow Surgeons Survey; CM, Constant Murley Score; SF-36, Short-Form 36; SD, Standard Deviation. Note: Boldface values indicate statistical significance.
Comparison of postoperative post-video outcome scores in group 1 and second postoperative outcome scores in the group 2.

Abbreviations: ASES, American Shoulder and Elbow Surgeons Survey; CM, Constant Murley Score; SF-36, Short-Form 36; SD, Standard Deviation. Note: Boldface values indicate statistical significance.
Discussion
Our study’s most important finding was that video recording before and after RCR and showing it to the patients led to improvements in functional outcome scores and quality of life measurements.
It was shown that many factors might affect outcomes after rotator cuff repair. 18 Patient-related factors include age, gender, tear size, workers’ compensation status, marital status, employment, preoperative expectations, and medical comorbidities. 4 Surgeon-related factors that can affect healing include repair construction, single row, double row, and rehabilitation. 18 In our study, there was a significant improvement in ASES and some of the SF-36 scores (emotional role functioning, energy/fatigue, emotional well-being, health change, and pain subscales) of patients who watched the pre- and postoperative video records of their shoulder. Improvement in these subscales shows that emotional and painful feelings can improve by watching the video.
The patients in video group had improvement in ASES score but CS remained similar. We attribute this to the fact that the ASES score’s evaluation criteria are mostly subjective and depend on the patient. The questions in the CM score are more clinician-dependent and objective. Also, we observed improvements in emotional state, energy, pain, and health changes domain of SF-36 score. Based on our findings, physical abilities or ROM capacities of the patients remain unchanged after watching video. However, the difference between pre- and postoperative status, increases patient satisfaction, motivation, and perception of well-being are consistent with our study hypothesis.
Previous studies have shown that the surgeon’s efforts alone may not be sufficient for patients to remember all the information provided.19,20 Denny et al. found that an educational video is related to improved knowledge, recognition of specific symptoms, self-efficacy, and patient satisfaction. 21 In a previous study conducted on 100 patients, patients who watched an educational video on anesthesia had lower preoperative anxiety and higher perioperative satisfaction than patients whose standard anesthesia information was verbally performed. 22 It was shown that, majority of the patients obtained satisfactory clinical improvement at the postoperative sixth month after ARCR.23–25 Therefore, we measured outcomes at the postoperative sixth month visit.
Among the visual studies, there are a limited number of orthopedic studies investigating patient satisfaction following video watching. Apart from video, some studies investigate the effect of visual results on patient satisfaction and provide self-assessment. Of these, Misir et al. found that taking pictures before and after total knee arthroplasty and sharing these points with the patient positively affected the clinical scores, quality of life, and patient satisfaction. 26 Albayrak et al. reported increased patient satisfaction after showing pre- and postoperative photographs following surgical treatment in adolescent idiopathic scoliosis patients. 27 Besides, in another study, it has been shown that the photos were taken and shown to kyphosis patients before and after surgery to increase patient satisfaction regardless of the type of kyphosis.27,28 Matamalas et al. found a significant relationship between waist height angle and deformity perception in their photographic study on idiopathic scoliosis. 29
Contrary to these studies, in another study, 59 total knee arthroplasties were applied. There was insufficient evidence to conclude that the preoperative and immediate postoperative photographing affected the hospital stay or the rehabilitation process. 30 Apart from this, several studies in the literature compare surgeon and patient satisfaction using photographs before and after scoliosis surgery. 31 Quality of life outcomes were not directly evaluated in these studies.31,32 In previous studies, the procedures mainly based on deformity correction. The aim of ARCR is to relieve pain and improve both clinical and functional outcomes. Therefore, we preferred to record videos instead of photographs to show improvements more accurately. Based on our results, showing video records increases perception of well-being. As a result, it can be used as a simple and reliable way to increase patient satisfaction after ARCR.
There are some limitations to our study. First, we performed the second postoperative evaluation just after showing the video records. Improvements in the second evaluation may be temporary; differences may disappear in further follow-ups. Second, the sample size is relatively small. It would be appropriate to conduct similar studies with a larger number of patients. Third, we did not investigate video-based satisfaction in patients with postoperative complications. It will be essential to learn the contribution of a video-based study to patient self-assessment and satisfaction in postoperative complications. Fourth, psychosocial factors such as anxiety, depression, and fear-avoidance beliefs are associated with patient-reported outcomes of ARCR. Some residual symptoms at 6 months-postoperative time points, if any, may be affected by watching video.
Conclusion
When patients watch the pre- and postoperative video records of their shoulder ROM after ARCR, patients’ satisfaction and well-being perception increase in the short-term despite unchanged shoulder ROM.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Erciyes University Faculty of Medicine Ethics and Research Board approval date: 02/12/2020 number: 2020/608
