Abstract
Introduction
Osteoarthritis (OA) of the knee is a common disease globally. The lifetime risk of developing symptomatic knee OA is estimated to be up to 47%, which further increases after the age of 60. 1 Total knee arthroplasty (TKA) is an effective treatment for treating patients with end-stage osteoarthritis of the knee.2–4 In the US alone, more than 600,000 TKA were performed in 2010. 5
According to local published statistics in 2017, the elderly (age >65) is expected to increase from 16% of the total population in 2016 to 29% by 2036. 6 This ageing population are expected to present with symptomatic knee OA indicated for TKA. Due to increasing age and medical morbidities, TKAs in octogenarian have been shown to be associated with higher post-operative complications, mortality and longer length of stay in comparison with younger patients.7–9 At the same time, patients aged 80 and over would still benefit greatly from the improved pain, function and quality of life. This has been well supported by current literature regarding short term benefit,10–15 however, mid-to long-term results of TKA in octogenarian have been scarcely reported.
This study aims to compare the safety and outcomes of TKA in the octogenarian population.
Patients and method
Ethics approval was obtained from the Research Ethics Review Board (CREC Ref. No. 2015.433). All methods in the study were carried out in accordance with the Helsinki guidelines and declaration or any other relevant guidelines.
This was a retrospective review of all patients aged 80 years old and above who underwent elective TKA between December 2005 and August 2013 in the orthopaedic unit of a tertiary hospital. All patients attended a pre-operative assessment clinic 1 to 2 months before the date of the surgery. During the pre-operative assessment clinic, patients were reviewed by orthopaedic surgeons, anaesthetists, nursing staff, physiotherapists and dietitians. This pre-habilitation exercise aimed to optimise patients’ clinical condition before surgery. There was no difference in clinical management during surgery and after surgery in either group. The patients followed the same post-operative rehabilitation program and attended their regular follow-up sessions at the clinic. The data for this study were retrieved from the electronic record system from the hospital. Pre-operative, peri-operative and post-operative factors were collected. A sex-matched group of patients aged 70–80 years, from a total of 950 TKAs performed within the same period, was selected as a comparison.
Pre-operative factors included comorbidities, indications of surgery (e.g. OA, rheumatoid arthritis, post-traumatic arthritis, etc.), Knee Society Score (KSS) and Functional Score (KFS), age at time of surgery, history of knee surgery, steroid usage, smoking status, pre-op knee range and fixed flexion deformity. Peri-operative factors included the type of anaesthesia, American Society of Anaesthesiologists (ASA) grading, the model of implant, duration of surgery, length of stay (LOS), ambulatory status on discharge and discharge status (direct home or to convalescence). Post-operative factors included implant survivorship, KSS and KFS, range of motion, Charnley Functional Score, 16 as well as rate of revision, infection or aseptic loosening. Intra- and post-operative complications were also recorded and divided into major and minor complications. Major complications included deep infection of implant, vascular injury, myocardial infarction, fast atrial fibrillation, stroke, pulmonary embolism and cardiac arrest. Minor complications included superficial wound infection, acute retention of urine, deep vein thrombosis, pneumonia and urinary tract infection. The primary outcome is the survivorship of TKA in this age group. Complications such as aseptic loosening, infection and revision TKA were considered a failure of TKA. Secondary outcomes include the functional benefit and rate of complication following TKA.
Statistical analysis
Pre-, peri- and post-operative factors between the above-80 and the control group were compared using Student’s t-test. Pre- and post-operative functional score, flexion range were compared using paired t-test. Kaplan–Meier survival analysis was done comparing the above-80 and control groups. Revision TKA was considered as the end-point. Patient mortality was also an end-point to investigate the viability, longevity and success of TKA in their 80’s. Data analysis was performed using IBM SPSS 26.0 (Armonk, New York). A p-value of ≤0.05 was considered statistically significant.
Results
Pre-operative factors between the two groups of patients.

Intra- and post-operative outcomes.

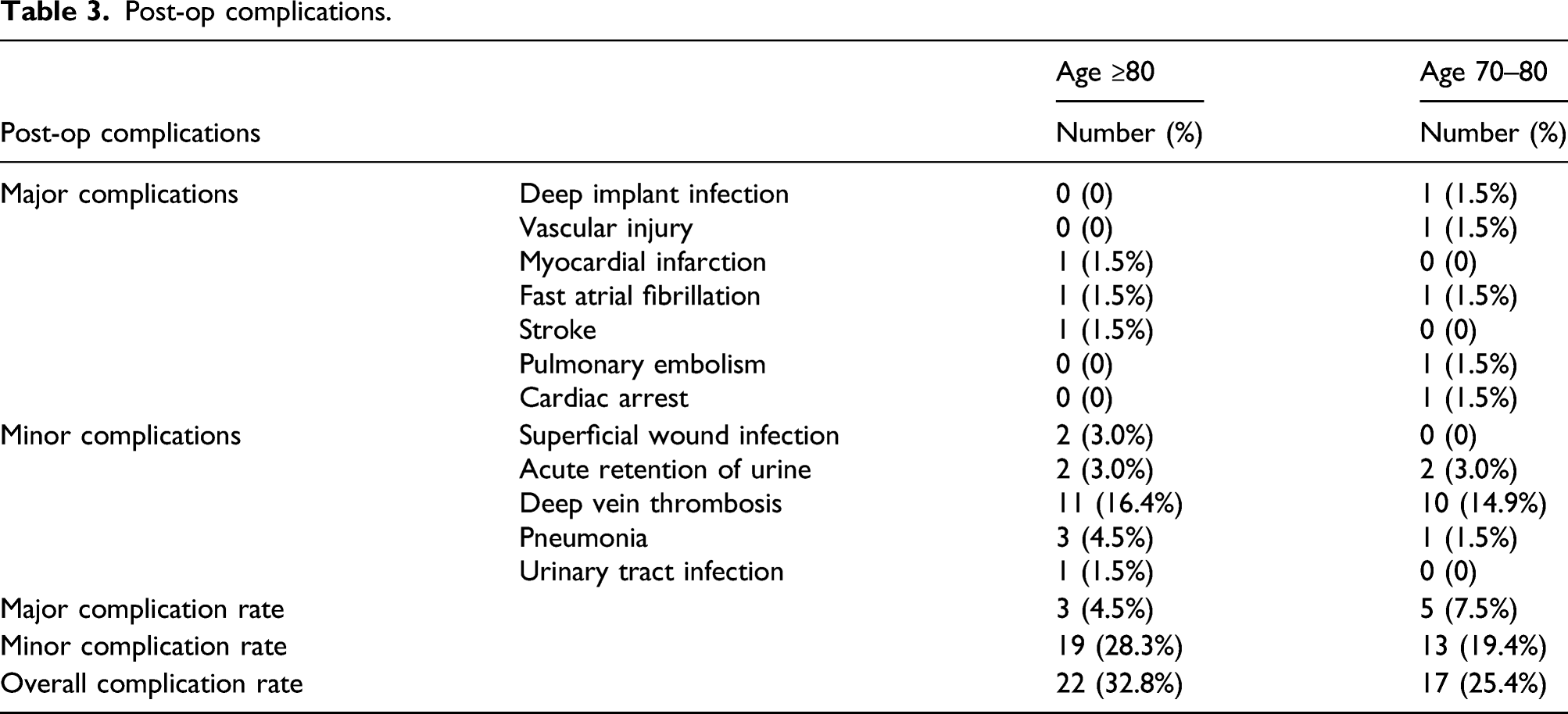
Post-op complications.
Functional outcomes between the octogenarian and control groups.

KSS: Knee Society Score, KFS: Knee Society Function Score.
*Student’s T-test.
Comparison of functional outcomes pre- and post-operatively.

KSS: Knee Society Score, KFS: Knee Society Function Score.
*Paired T-test.
Patient survival rate and standard error (SE) of the two groups using Kaplan–Meier product limit method.


Kaplan–Meier curve of patient survival time in above-80 and control groups.
Implant survival rate and standard error (SE) of the two groups using Kaplan–Meier product limit method.


Kaplan–Meier curve of implant survival time in above-80 and control groups.
Discussion
TKAs are a common, safe and effective procedure. However, some healthcare providers may be averse to offer TKAs in patients aged above 80 due to concerns of higher risk of surgery as well as patient survivorship. Many studies in different specialties have shown the pervasiveness of ageism in healthcare systems around the world resulting in poorer patient outcomes.17–21 With better healthcare and longer average life expectancy, 22 we can anticipate more and more healthy and active elderly who would benefit from the improved function that TKAs can provide. Here, we have shown that TKAs are safe and effective in the octogenarian population with comparable rate of revision and post-operative outcome. To the authors’ best knowledge, this was the first study to investigate the long-term results of TKA in octogenarian.
In terms of implant survival, our study correlates with Klasan et al., who looked at the medium-term outcomes of TKAs in octogenarians in Australia. 23 Implant survivorship at 10 years was reported at 99.5%, and patient survivorship was 26% at 10 years; mean follow-up was 7.76 years. Joshi 15 reported a 10-year patient survival of 34% in octogenarian TKAs in 2003. Our study observed a 10-year implant and patient survivorship of 100% and 54.6%, respectively. As expected, the elderly enjoyed excellent implant survival but had poorer patient survival. The difference in patient survival between our study and Klasan’s may be explained by our higher life expectancy than Australia. 24
Tay et al. 25 found the 2-year revision rate was higher in octogenarians (2.9% vs 1.4%), but this was not statistically significant (p = 0.31). Klasan 23 reported a revision rate of 0.46% (versus 1.55% in younger patients, p = 0.51) with mean follow-up of 7.76 years. The lower rate of revision is likely due to lower functional demand and higher threshold for performing revision arthroplasty in the elderly. In our study, the rate of revision was comparable to the younger cohort; only one patient in the control group required revision TKA, which may be due to smaller sample size.
Multiple studies have shown a correlation between advanced age with increasing LOS.25,26 Tay et al. reported a mean LOS of 6.3 vs 5.4 days in octogenarian versus younger cohort. Austin et al. reported a mean LOS of 3.30 vs 2.91 days, with 37% requiring facility discharge. In comparison, our LOS was 9.55 ± 3.28 vs 9.23 ± 3.19 days (octogenarian vs control), with 87% discharged to convalescent hospital. This is likely due to old practice; with introduction of newer surgical practice and accelerated rehabilitation protocols, 27 most our patients currently have shorter length of stay and are discharged home directly.
Yohe et al. studied the complication rate of octogenarians according to the American College of Surgeons National Surgical Quality Improvement Project (ACS-NSQIP) database in USA. 28 Rate of major complications such as stroke, myocardial infarction, sepsis and revision surgery was found to be 3.5%, with overall rate of revision 1.2%. 4.7% patients presented with unplanned readmissions within 30 days. In comparison, our rate of major complications in octogenarian was 4.5%, and revision rate was 0%. The slightly higher complication rate and difference in rate of revision may be due to small sample size or overall low TKA volume at our hospital. We report a high minor complication rate in our study (28.3%), with a majority due to deep vein thrombosis (DVT). This is due to the lack of modern multi-modal DVT prophylaxis such as early mobilisation, thromboembolism-deterrent stockings, sequential compression devices and direct oral anticoagulants which are now routine in our unit. Overall mortality rate in Yohe’s study was found to be 0.3%, which was increased in patients with dependent functional status and ASA > 2 (OR 8.94 and 6.11, respectively). This was comparable with our findings of 0%.
Cher et al. studied the functional scoring between octogenarians and younger patients in TKA at 6 and 24 months. 29 Both groups showed statistical improvement in KSS and KFS post-operatively. In the octogenarian group, mean KSS improved from 36.77 to 84.44 (p < 0.05), while mean KFS improved from 39.50 to 55.77 (p < 0.05). In our study, mean KSS in octogenarian improved from 34.48 to 94.22 (p < 0.01) which was comparable. This improvement was maintained during the lifetime of the prosthesis as well as the patient. KFS in our study was not significantly improved, this may be due to deterioration in our patients’ overall ambulatory status with longer follow-up and increasing age.
There are limitations in our study. This study was retrospective in nature; octogenarians with poor premorbid status and deemed surgically unfit would naturally not be included. There would also be inherent bias from healthcare providers and relatives to opt for a more conservative management in marginal patients. Using revision as an end-point for TKA survivorship in these patients may therefore underestimate the true figure. In this study, our control group was chosen to be aged between 70 and 80. This was intentionally done to provide a more comparable cohort to the above-80 group. We would anticipate a larger difference in pre-operative functional score, post-op improvement as well as complication rate with a control group that included all ages. Our moderate sample size of 67 patients at a single centre may also affect the power of our study. This study was performed more than a decade ago; evolving surgical methods, different surgeons as well as introduction of multi-disciplinary approach to accelerated TKA rehabilitation may also introduce heterogeneity between earlier and later cases in our study.
Here, we have shown that TKA in octogenarian has similar complication rate and functional outcome compared to a younger age group. Despite the higher ASA grading overall, post-operative complications were comparable to those aged between 70 and 80 years old. While there was a lower patient survivorship in the elderly group due to age difference, implant survivorship was comparable. Function score remains poor in octogenarian without significant difference in comparison to the younger cohort; this is to be expected as they often have impaired muscle strength, coordination and balance. However, patients are still able to benefit from TKA with improved knee range of movement and pain which is reflected in KSS. Clear surgical objective, addressing patients’ concern and expectation is paramount in order to achieve good outcome following TKA.
Conclusion
TKA can be performed in patients with age above 80 years old with comparable post-op knee range, complication rate and long-term functional score. Advanced age should not be a limiting factor for TKA.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
