Abstract
Purpose:
The purpose of this study is to evaluate the outcome and prognosis of complete synovectomy performed under arthroscopic surgery in the treatment of diffuse pigmented villonodular synovitis (DPVNS) of the knee.
Methods:
We retrospectively reviewed 7 cases (6 female and 1 male) diagnosed with diffuse pigmented villonodular synovitis (DPVNS) of knee from 2013 to 2017. All of these cases were treated with knee arthroscopy-assisted complete synovectomy. The follow-up period ranged from 36 months to 60 months (average: 48.0 months). The pain score, range of motion and functional outcome of the knee joint were evaluated after surgery. Symptoms and signs were monitored and magnetic resonance imaging (MRI) were routinely requested to note for possible recurrence during clinical follow up.
Results:
During and after the surgeries of complete synovectomy under arthroscope by the same surgeon, no complications were noted in the ward or the clinic. Significant improvements were achieved in terms of the range of motion and Lysholm knee function score. There was no recurrence of DPVNS observed in our patients during a follow-up of 4 years.
Conclusions:
Intra-articular DPVNS of the knee can successfully be treated by complete synovectomy under arthroscope. This case series emphasized the technique of multiple portals and cycling different shavers to achieve satisfactory outcomes.
Introduction
Pigmented villonodular synovitis (PVNS), also known as tenosynovial giant cell tumor, is a rare synovial proliferative disease. PVNS typically presents with single joint involvement, and most often involves the knee joint. 1,2 In the general population, the incidence is estimated to be approximately 2 cases per million per year. 1 The sex predominance still remains controversial. Some studies have reported a male predominance; however, others have shown no difference between males and females. 3 –7 Two subtypes have been introduced based on the affected lesion. 8 Localized pigmented villonodular synovitis (LPVNS) has been noted to be a focal lesion, while diffuse pigmented villonodular synovitis (DPVNS) often has infiltrative synovial proliferation with hemosiderin deposition involving both the anterior and posterior compartments around the knee joint.
The clinical presentation is different between LPVNS and DPVNS. In the localized type, patients usually present with painless swollen joints. The anterior compartment over the knee is the most involved region. Episodes of trauma might be elicited from history. Due to the unspecific symptoms, the diagnosis is sometimes incidentally found. Patients with DPVNS tend to have more concerning symptoms than patients with LPVNS. Effusion, swelling and joint tenderness are most common. The diffuse lesion might induce limitations of motion over the joint. Due to the difficulty of clinical diagnosis, magnetic resonance imaging (MRI) plays an important role in lesion confirmation. A well circumscribed soft-tissue mass is visualized in LPVNS, whereas an ill-defined mass is more often revealed in diffuse types. 9,10 MRI can also be used to evaluate the extra-articular extension of an intra-articular process.
The general principle for the treatment of PVNS is complete excision of the proliferative synovium. Partial synovectomy has been demonstrated to be effective in LPVNS with either an open procedure or arthroscopy. 11 –13 However, the optimal method for complete synovectomy in DPVNS remains controversial. Even with an open method, the prognosis is unsatisfactory with recurrence rates as high as 33%. 14 –16 With the development of the arthroscopic technique, combined arthroscopic anterior with open posterior compartment synovectomy has been reported to have a similar recurrence rates compared to the use of open procedures alone. 15,17
The complication rate after the treatment of DPVNS is relatively high with open synovectomy. To eradicate diffuse lesions with a good surgical field, a large open wound is often inevitable. The incidence of wound complications is thus elevated. Other complications include hemarthrosis, knee stiffness and prolonged rehabilitation. 6 Arthroscopic synovectomy is a good alternative method for avoiding the problems described above. 18 Recently, there have been a few studies on complete synovectomy under arthroscopy for the treatment of DPVNS with satisfying prognosis. 18 –20 In this study, we aim to investigate the clinical outcome and prognosis for treating intra-articular DPVNS of the knee with complete synovectomy under arthroscopy.
Material and method
Study design
A retrospective study was conducted in our institution with approval of the Institutional Review Board. From January 2013 to 2017, all patients diagnosed with diffuse pigmented villonodular synovitis involving the knee joint treated with complete synovectomy using purely arthroscopic techniques were reviewed. Patients with recurrent DPVNS, those with extra-articular extension and major degenerative joint changes were excluded in our research. Seven patients, one male and six females, with one patient having bilateral knee lesions diagnosed in different years, were included in the study.
General data and clinical presentation were collected from the charts. All patients had X-rays of the knee (AP, lateral view and merchant view) and MRI done (Figure 1). Pain scores and knee function, including the range of motion and Lysholm score, were evaluated preoperatively and after the surgery. Patients were clinically followed every 3–6 months after the operation. Suspected recurrence was based on the clinical presentation. MRI were taken in all patients in the final follow-up (Figure 2). The data collection was done by an independent examiner.

Pre-operative MRI (left: T2-weighted sagittal, right: Proton density weighted sagittal) revealed a low-signal lesion of diffuse pigmented villonodular synovitis over right knee.

The same patient with follow-up MRI (left: T2-weighted sagittal, right: Proton density weighted sagittal) after the operation for 36 months. There was no intra-articular lesion noted.
Surgical technique
All surgeries were performed by the senior author (Y.S.C.). Under general anesthesia, the patient was placed in the supine position with 90 degree flexion of the knee. First, standard anteromedial and anterolateral portals with the combination of superomedial and superolateral portals were created for debridement of the anterior compartment. Anterior synovectomy always systemically begins with the suprapatellar pouch and then progresses to the medial and lateral gutters. Using arthroscopes set at 30 degrees and 70 degrees alternatively is quite important for a wide field of view.
Debridement over the posterior compartment is highly challenging due to the neurovascular structures. A modified Gillquist maneuver was performed to approach the posteromedial and posterolateral corners. To visualize and completely debride the compartment, posteromedial and posterolateral accessory portals were always created (Figure 3). Similar to the anterior region, the regular use of arthroscopes set to 30 and 70 degrees and the cycling of different shavers with radiofrequency (Arthrocare, Sunnyvale, California, U.S.A.) were the mainstays of thorough synovectomy. Finally, a trans-septal approach was used for further visualization of the two posterior corners.
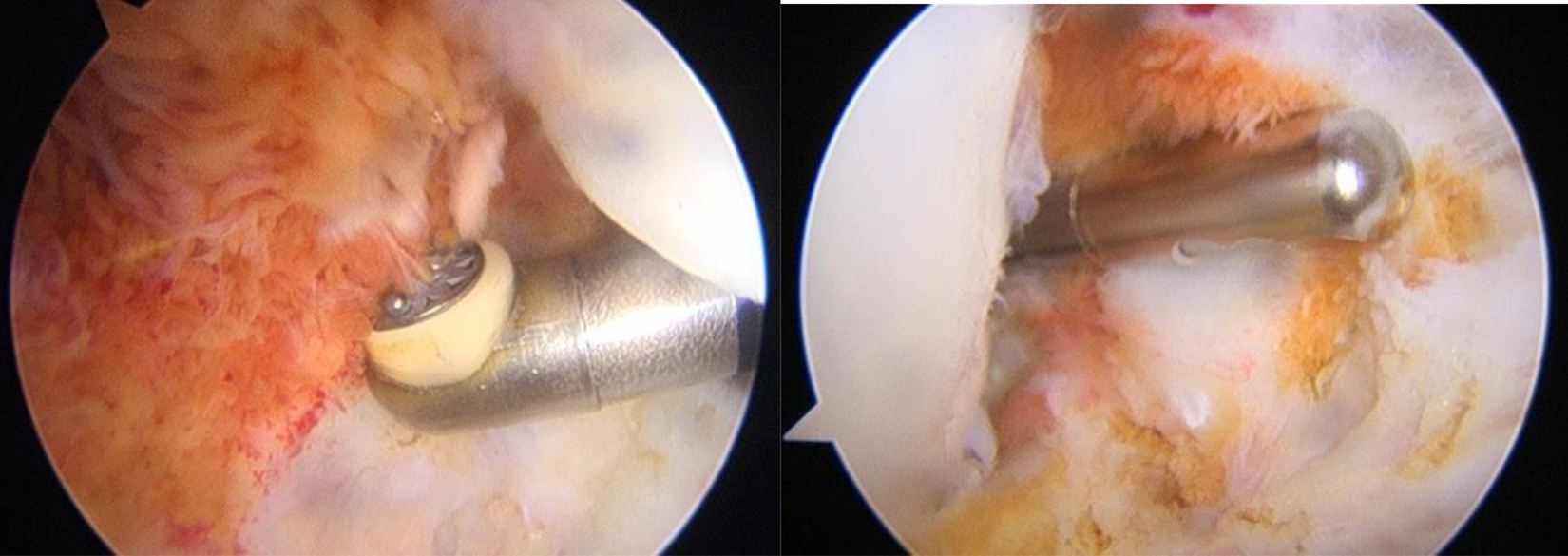
Posteromedial (left) and posterolateral (right) portals were created for debridement over the posterior compartment.
Statistical analysis
Statistical data were analyzed utilizing the SPSS software. Due to the small sample size, the data were analyzed with Wilcoxon’s test. Preoperative and postoperative pain scores over the knee and Lysholm knee scores were compared. P values smaller than 0.05 were considered significant.
Results
Data from 7 patients were collected from 1 male and 6 female patients. The average age of the patients was 29.4 years (range from 15 to 48 years). One patient was diagnosed with DPVNS over the right knee in 2014 and the left knee in 2017. The mean follow-up period was 48.0 months (36–60 months). The major symptoms were effusion and swelling over the knee joint, with 71% of the patients having one of the clinical presentations described above. Five of the seven patients had tenderness. Only one patient had a trauma history with knee contusion due to falling down. The general data for the patients are listed in Table 1.
General data of patients with intra-articular DPVNS of the knee.

Pre-OP ROM: pre-operative range of motion; Post-OP ROM: post-operative range of motion
There were no major complications, such as neurovascular injury or wound infection, during or after the surgery. The pain scores and range of motion scores (Table 2) improved significantly after arthroscopic synovectomy. All the patients had “fair” and “poor” Lysholm knee joint function scores before the treatment. After surgery, 6 of 7 patients achieved “excellent” and “good” results with significant improvement. Only one patient had a “fair” Lysholm score and had undergone secondary arthroscopic surgery due to an anterior cruciate ligament and meniscus tear. There were no recurrent lesions seen on follow-up MRI in all the cases.
The average range of motion, pain score and Lysholm knee score before and after the operation.

* Significantly different from Wilcoxon’s test
Discussion
PVNS is an uncommon proliferative disease involving the synovial joint, bursa and even the tendon sheath. It was first reported in 1852 by Chassaignac and was then introduced with the current terminology “pigmented villonodular synovitis” by Jaffe et al. in 1941. 2,21 The classification of localized and diffuse types was defined by Granowitz and Mankin in 1967 and is currently well accepted. 22
The etiology of pigmented villonodular synovitis remains unclear. It is considered to be an inflammatory disease due to the presence of proliferative lesions and might be induced by trauma or abnormal lipid metabolism. 23 However, many studies have demonstrated that rearrangement of chromosome 1p11-13 is highly correlated with pigmented villonodular synovitis. 24 A neoplastic origin for this disorder was supported with the presence of an aneuploid DNA pattern, trisomy 7 and 5 and a clonal rearrangement of chromosomes 1,3 and 15 in genetic investigations. 3,25 Perka et al. postulated that DPVNS is potentially a more neoplastic type due to the characteristic of invasiveness, high recurrence rate, malignant transformation, metastasis and chromosomal abnormalities mentioned above. 26 Recently, the role of the molecular pathway inducing pigmented villonodular synovitis, such as colony stimulating factor-1 (CSF-1), was also developed. 27,28 Novel insight into the disease might challenge the concept of therapy in the future.
The treatment of PVNS is slightly different based on the presence of the localized or diffuse type. Regular follow-up in nonsymptomatic patients can be considered for LPVNS, while the protocol for conservative treatment is still not well documented. However, in most cases, patients suffer from pain and effusion of joints, and would require surgical treatment. Excision with the open approach is routinely used, but many studies have reported excellent prognosis for the arthroscopic procedure in LPVNS. 12,13 Partial synovectomy under arthroscopy might be a preferable method in most patients.
Treatment for the diffuse type of PVNS is more difficult than that for LPVNS due to the high recurrence rate. Complete synovectomy via open arthrotomy has been the gold standard for DPVNS in the past. 10,29 Previous studies have shown variations in the recurrence rate for open procedures from 8% to 46%. 6,30,31 The diversity in prognosis might be due to the development of techniques for open synovectomy. Flandry and Hughston reported the most satisfactory recurrence rate of 8% with the open method in 25 patients; however, 24% of them complained of knee stiffness. 6 Manipulation was required with long rehabilitation for these cases.
Arthroscopic surgery is an alternative treatment for intra-articular PVNS lesions to prevent wound complications or a limited range of joint motion. Studies comparing the traditional open method and arthroscopic surgical technique have been performed. Gu et al. demonstrated that the recurrence rate among open and arthroscopic synovectomy procedures was not significantly different. Comparing the 2 groups, patients receiving arthroscopic surgery had significantly shorter hospital stay and operation time than those who have undergone the open method. The postoperative function of the knee joint was also improved. 7 Auregan et al. in a systematic review that included 60 studies reported no difference in local recurrence rates after open or arthroscopic surgery for either LPVNS or DPVNS. A lower rate of postoperative complications was also found for DPVNS patients undergoing arthroscopic surgery. 32
Recently, the prognosis for arthroscopic technique in treating DPVNS was improved (Table 3). However, the recurrence might be under-estimated as the prognosis was based on clinical symptoms in some studies. In our study, 7 cases of DPVNS showed satisfactory range of motion of the knee joint. The Lysholm knee function score also improved significantly with “excellent” and “good” result. All patients underwent MRI in their final follow-up. No major complications nor signs of recurrences were found.
Literature review of DPVNS treated with complete arthroscopic synovectomy.

Because arthroscopic synovectomy is a technically demanding procedure, the treatment of DPVNS remains difficult. 18,33 The combination of additional portals with the use of multiple shavers and radiofrequency for complete synovectomy has been introduced for sophisticated synovectomy. 38 Our experience also proved the benefits of using a surgical tip. Due to the risk of neurovascular injury and the easily missed lesions between the meniscus and cruciate ligament, the achievement of an excellent prognosis requires skillful technique with a steep learning curve.
The good prognosis in our study may be due to the adequate skills and training of the surgeon performing the technique. Another reason might be the rigorous inclusion criteria used for our study where DPVNS cases with extra articular extension, who may not be appropriately treated with purely arthroscopic techniques, were excluded. In this case series, the absence of signs of recurrence in the follow-up radiographic images, and the significantly improved functional scores support the use of complete synovectomy with arthroscopic techniques for the thorough treatment of intra-articular DPVNS of the knee.
There are limitations in our study. Even though Ushijima reported that the mean time of recurrence was 24 months, 9 the follow-up period (average 48 months) was relatively short. More complications or instances of recurrence might occur with longer follow-up periods. Second, this was a retrospective study. Lastly, because of the relative rarity of DPVNS of the knee joint, the number of cases in these series are few.
In conclusion, complete synovectomy using purely arthroscopic techniques could be achieved safely in intra-articular DPVNS of knee joint with excellent result. We recommended using multiple portal technique with cycling of different shavers to achieve satisfactory outcomes.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
