Abstract
Purpose:
To investigate the biomechanical, histological, and radiological effects of sildenafil and pentoxifylline on femoral fracture healing in rats.
Methods:
Forty-eight Sprague-Dawley rats were divided into three groups equally according to the pharmacological agents to be investigated. Femoral shaft fractures were formed in the left side. Group 1 (control group), group 2, and group 3 were administered with saline, sildenafil, and pentoxifylline during the fracture healing process, respectively. Eight rats from each group were euthanized on days 15 and 30. X-ray images of the rats were taken after euthanasia for radiographical examination. Femur samples were subjected to histopathological and biomechanical (three-point bending) examinations.
Results:
Radiologically, no difference between the Goldberg scores of the groups was found for day 15 (p > 0.05), while higher Goldberg scores were obtained from group 2 than that of group 1 (p > 0.05) and group 3 (p < 0.05) for day 30. In the biomechanical analysis, higher mean breaking forces were found both for day 15 and day 30 from group 2 than those obtained from group 1 (for day 15 p > 0.05 and day 30 p > 0.05) and group 3 (for day 15 p < 0.05 and day 30 p < 0.01). Higher mean absorbed energy values were obtained from group 2 than those obtained from group 1 (for day 15 p > 0.05 and day 30 p < 0.05) and group 3 (for day 15 p < 0.01 and day 30 p < 0.01). A significant difference was not found between the histological scores of all groups (p > 0.05) for day 15, while the histological score of group 1 on day 30 was found to be significantly lower than that of sildenafil and pentoxifylline groups (p < 0.05).
Conclusion:
Sildenafil had a positive effect on fracture healing, while pentoxifylline did not provide consistent positive effect.
Introduction
In the fracture healing process, vascularization of the tissue is a prerequisite for successful bone healing. 1 Decreased vascularity at the fracture site is one of the most important parameters causing delay in fracture healing and the formation of atrophic nonunion. Pentoxifylline is a competitive nonselective phosphodiesterase (PDE) inhibitor that reduces inflammation and increases microcirculation, blood flow, and tissue oxygenation. 2,3 In addition, pentoxifylline improves the ability of red blood cells to deform and reduce the potential for platelet aggregation and thrombosis. In a previous study, daily pentoxifylline injections have been shown to stimulate bone formation and increase systemic bone mass in mice, therefore it can be regarded as a valid approach to the management of osseointegration. 4 Moreover, many studies have shown positive effects of pentoxifylline on the healing of the mandible. 5,6 The therapeutic efficacy of pentoxifylline is mainly due to its hemorrhagic effects and the potential to increase blood flow and tissue oxygenation.
Sildenafil, a cyclic guanosine monophosphate (cGMP)-dependent PDE5 inhibitor, has been shown to be an important stimulus of angiogenesis through the upregulation of pro-angiogenic factors and the control of cGMP concentration. 7,8 Earlier studies have shown that angiogenic and osteogenic factors, vascular endothelial growth factor (VEGF), and cysteine-rich angiogenic inducer 61 (CYR61) are involved in bone formation and fracture healing. 9 –11
Previous studies evaluating the effects of pentoxifylline and sildenafil on bones have been conducted to investigate the effects of the two drugs separately in a closed fracture model. 12,13 Moreover, these studies did not include the histopathological, biomechanical, and radiological investigations all together. Unlike these research, since the vascular response is a prerequisite for successful bone repair physiology, the role of the two PDE inhibitors, which increase blood flow, in open bone repair has been extensively investigated in this study.
Materials and method
All experimental procedures were approved by the ethical committee of the Istanbul Bağcılar Training and Research Hospital (project no: 2013-30). The experiments were carried out by taking the animal rights into consideration. A total of 48 adult, male, 7-month-old Sprague-Dawley rats with an average body weight of 350 g were included in the study. After randomization, 16 rats were assigned as the control group (group 1, n = 16) and were administered with saline (1 cc intraperitoneal) during the fracture healing process. Two study groups were formed to administer sildenafil (group 2, n = 16; Viagra 1 mg/d, Pfizer, New York City, New York, USA) and pentoxifylline (group 3, n = 16; Trental 100 mg, Sanofi-Aventis, Gentilly, France). In each group, the rats were further divided into two subgroups, equal in number, to be euthanized on day 15 and day 30. Table 1 presents a summary of the definitions of all the groups.
All groups of animals organized in the study.

The treatment was started on the day of surgery and continued to be administered at the same time every day until the day that the rats were euthanized. Sildenafil and pentoxifylline were administered by oral gavage (10 mg/kg per day) and intraperitoneal injection (50 mg/kg per day), respectively. Since only oral substrates of sildenafil are available in Turkey, oral administration was carried out for group 2. After 15 days (early period) and 30 days (late period), eight rats in each group were euthanized to evaluate the bone healing process.
All rats received antibiotic prophylaxis as a subcutaneous dose of gentamicin 8 mg/kg before surgery. After administering general anesthesia (isoflurane 4% induction, 2% idiopathic inhaler), the rats were placed in the supine position. Under sterile conditions, the left knee regions of the rats were anteromedially skinned with a 2-cm longitudinal incision. The joint capsule was opened through the patella medial. Patella was misaligned to the lateral side and the knee was kept in the flexed position. A femur canal was prepared using a 1 mm Kirschner wire and electric drill through the femur condyle. Then the prepared channel was placed in a 0.8 mm Kirschner wire. At the place where the wire was stuck, the wire was pulled back about 3–4 mm and the femur was cut from the level of the condyle. The remaining wire in the canal was pushed back into the canal in such a way that the wire would not be out of the condyle. The knee was then kept in extension position and the patella reduction was carried out. The joint capsule was closed. Once the wire was placed, to form a standard open femur shaft fracture, the femur was cut through the middle of the shaft transversely. The fracture was radiographically confirmed with a portable X-ray. Following the surgical procedure, carprofen (3 mg/kg) was administered to provide postoperative analgesia. Following radiological examination (Figure 1), the rats were administered isotonic saline (1 cc) intraperitoneally, sildenafil (10 mg/kg) by oral gavage, and pentoxifylline (50 mg/kg) intraperitoneally, according to their groups. These medications were continued as a single dose daily for 4 weeks. After the operation, the animals were allowed to move with full weight. Half of each group was euthanized under high-dose anesthesia on the 15th day following the operation (early period) and the other half on the 30th day (late period). The left femurs of all rats were then amputated.
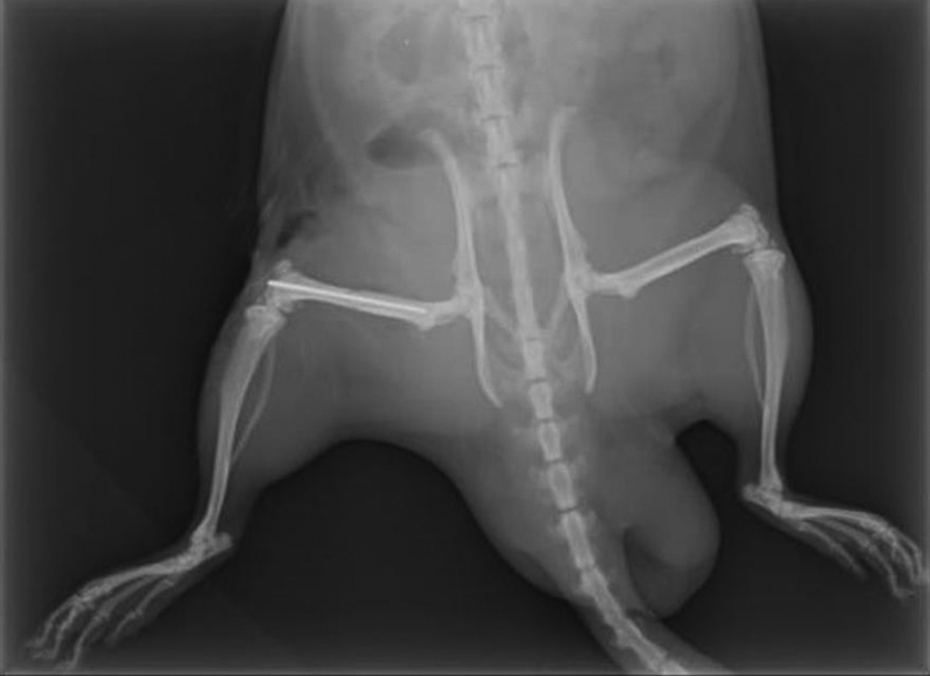
A representative X-ray image of a rat included in the study.
Radiological evaluation
Direct X-ray images taken from all euthanized and surgically treated groups were evaluated in terms of fracture healing according to the classification procedure recommended by Goldberg et al. 14 Radiological evaluations of all animals were performed independently by two orthopedists who were not included into the study (Figure 1).
Histopathological testing
Three femur samples in each group that was euthanized on days 15 and 30 were subjected to histopathological examination. All femurs were fixed in a 10% buffered formalin solution for 2 days. After fixation, the femurs were decalcified in a 10% hydrochloric acid solution for 2 h. The samples were then dehydrated by passing through alcohol, acetone, xylene, and paraffin stages in the closed system tissue monitoring device. Then paraffin blocking was done. Longitudinal sections of 4 µm thickness were cut and stained with hematoxylin–eosin staining, and examined by light microscopy (Olympus BX51, Tokyo, Japan).
On histopathological examination, healing and maturation of the bone were evaluated. Vascularity was not included in the histopathological examination. The histological classification of healing was made according to the healing scale by Huo and Troiano. 15 According to this scale, high scores indicate that the bone healing process progresses positively. The numerical scoring used for the histological evaluation of fracture healing was as follows: score 1: fibrous tissue, 2: mainly fibrous tissue and little cartilage tissue, 3: equal amount of fibrous tissue and cartilage tissue, 4: cartilage tissue, 5: mainly cartilage and a small amount of immature bone, 6: equal amount of cartilage and immature bone, 7: mainly immature bone and little cartilage, 8: totally immature (woven) bone, 9: immature bone and a small amount of mature bone, 10: mature (lamellar) bone.
Biomechanical testing
The remaining samples (five femurs) in each group were subjected to biomechanical examination. The extracted femurs were wrapped in a saline-soaked gauze bandage to prevent dehydration and stored at −20°C in small, sealed freezer bags until the day of biomechanical testing. Femurs were exposed to three-point bending test to determine the biomechanical effects of sildenafil and pentoxifylline on the bone tissues during the fracture healing process.
All mechanical bending tests were performed on a testing frame (Instron 5982, Norwood, Massachusetts, USA) having a 100 kN load cell with a load accuracy of ±0.5%. The deflection along the anteroposterior axis was induced at the center of the diaphysis of the femurs at a constant speed of 10 mm/min until failure. The bending tests were carried out with a constant span length (distance between the supports) of 25.7 mm. The press head, as well as the two support points, was rounded to avoid shear load and cutting. The bone was positioned horizontally with the anterior surface upward, centered on the supports, and the pressing force was directed vertically to the mid-shaft of the bone. At the start of the test, the press head contacted with the bone surface with a small preload (<1 N) to keep the bone stable between the contact points of the testing machine and at this instant, the deflection value along the anteroposterior axis was set to 0. The force and deflection data were simultaneously recorded at 1 kHz using Bluehill 3 software program consistent with the testing machine. The breaking load, which was determined as the highest point of the force–deflection curve (failure point), and the energy absorption, which was obtained by calculating the area under the load–deformation curve until the failure point (the point at which the first breakage occurred within the specimen), were obtained from the three-point bending tests.
Statistical analysis
The statistical significance analysis of the radiographical scores was done with the Kruskal–Wallis test. To observe whether the breaking force and absorbed energy differences between the groups are statistically significant, a one-way analysis of variance was employed. For statistical analysis of the histopathological examination, mean, standard deviation, and lowest and highest median values were used in the descriptive statistics of the data. The distribution of the variables was measured by the Kolmogorov–Smirnov test. Kruskal–Wallis and Mann–Whitney U tests were used in the analysis of quantitative data. Wilcoxon test was used in the analysis of repeated measurements. IBM SPSS Statistics (version 21; SPSS Inc., Chicago, Illinois, USA) software was used for statistical analysis. The differences were evaluated at a level of significance of 0.05.
Results
In all groups, a progression of consolidation can be observed in radiographical scores over time (Table 2). Radiologically, no statistically significant difference between the Goldberg scores of group 1, group 2, and group 3 was found for the 15th day. On the other hand, a significant difference between group 2 and group 3 for the 30th day was observed (p = 0.02). Although the sildenafil group provided more complete healing than the control group for the 30th day, this difference was not statistically significant (p > 0.05).
Summary of the Goldberg scoring results of the femur samples.

In the biomechanical analysis, it was found that the mean breaking forces obtained from group 2 were higher than those obtained from the control (for day 15 p > 0.05 and day 30 p > 0.05) and pentoxifylline (for day 15 p = 0.049 and day 30 p = 0.01) groups (Figure 2). The control group provided higher mean breaking forces than the pentoxifylline group, but the difference was only statistically significant for day 30 (p = 0.047). The mean absorbed energy values obtained from group 2 were higher than those of group 1 (for day 15 p > 0.05 and day 30 p = 0.02) and group 3 (for day 15 p = 0.008 and day 30 p = 0.01) (Figure 3). The control group provided higher mean absorbed energy values than the pentoxifylline group, but the difference was only statistically significant for day 15 (p = 0.001).

Mean and standard deviation of the breaking forces: (a) 15th day and (b) 30th day (*p < 0.05 and **p < 0.01).

Mean and standard deviation of the absorbed energy: (a) 15th day and (b) 30th day (*p < 0.05 and **p < 0.01).
Although the means of the histological scores obtained from group 2 and group 3 were higher than that of the control group for day 15, a statistical significance was not found between the scores (p > 0.05; Table 3). For day 30, the histological scores obtained from group 2 and group 3 were significantly higher than that of the control group (p = 0.03). The histological score of the fractured regions on the 30th day from the sildenafil and pentoxifylline groups did not differ significantly (p > 0.05). When the intragroup changes in the histological scores were analyzed, it was found that the means of the histological scores obtained at the 30th day of fracture were higher than those obtained at the 15th day of fracture, indicating that a better improvement in fracture healing was observed at the 30th day than at the 15th day for all the groups. But these intragroup differences were not statistically significant (p > 0.05). Figure 4 presents the representative images of the histology of the samples.

Representative images of the histology of the samples: (a) equal amount of cartilage and immature bone, hematoxylin and eosin, ×100, control group (sample number 2) on day 30; (b) mainly immature bone and less cartilage, hematoxylin and eosin, ×100, sildenafil group (sample number 3) on day 30; (c) totally immature bone, hematoxylin and eosin, ×100, pentoxifylline group (sample number 3) on day 30.
Histological findings at the fracture site (significant results at 0.05% in bold).

SD: standard deviation; min: minimum; max: maximum.
K Kruskal–Wallis (Mann–Whitney U test).
W Wilcoxon test.
Discussion
Rapid bone fracture healing after trauma and surgery is crucial to regain normal functions of the bone and surrounding structures. 16 Because of the vascularity of the bone, angiogenesis plays a very important role in bone formation, both during bone development and fracture healing. 17,18 Previous studies have shown that angiogenic and osteogenic factors associated with VEGF and CYR61 proteins are involved in fracture healing 19 and that reduced vascularity is one of the most important risk factors for delayed fracture healing. 20
During the bone healing process, nitric oxide (NO) increases blood flow. NO is known to play a regulatory role in blood flow and perfusion pressure in vascular beds in response to appropriate physiological stimuli. 21 For this reason, the treatment methods applied to improve blood circulation can improve bone healing.
Our study focused on the effects of pentoxifylline and sildenafil as peripheral vasodilators on the healing of open bone fractures. Unlike most peripheral vasodilators, pentoxifylline reduces blood viscosity. The effectiveness of pentoxifylline in treatment is mainly due to hemorrhagic effects and the potential to increase blood flow and tissue oxygenation. 22 Bone repair mediators and cytokines are thought to be transferred to the fracture site, thanks to the increase in blood flow, and pentoxifylline causes an increase in their concentration. Kinoshita et al. showed in their animal study that pentoxifylline improves bone formation in rats. 23 It is unclear whether pentoxifylline increases osteoblasts or osteoclasts. Takami et al. showed that PDE inhibitors both increase osteoclasts and turn osteoclasts into osteoblasts. 24 However, Horiuchi et al. examined the effects of pentoxifylline on new bone formation in an animal model and showed that pentoxifylline increased bone formation with increasing bone morphogenetic protein 2. 25,26 Aydin et al. suggested that pentoxifylline could raise the healing of the hematoma, the first stage of fracture healing. 12 They claimed that the anti-inflammatory effects of pentoxifylline delayed fracture healing on day 21. In the study of Aydin et al., histological bone healing in the pentoxifylline group was higher in the first week, while the amount of healing in the control group was higher in the third week. 12 However, in another study, the positive results of pentoxifylline on bone healing on day 21 were also obtained. 27
Pentoxifylline, a PDE inhibitor, specifically reduces the production of chemotactic mediators such as interleukin (IL)-1 and IL-6 by reducing tumor necrosis factor alpha, thereby suppressing inflammatory reactions. 22 The first phase of fracture healing, hematoma phase, lowers blood viscosity due to pentoxifylline and its rheological effects, and in turn, promotes an increase in the amount of hematoma formed at the fracture site. For the late period, it is thought that the anti-inflammatory effects of pentoxifylline may delay fracture healing similar to other nonsteroidal anti-inflammatory drugs. 12 It is known that infection in the fracture zone is among the most important reasons for nonhealing. In the study of Aydin et al., higher rates of infection were found in the pentoxifylline group than the control group. 12 This situation can also be considered as another factor that may cause the delay of fracture healing. In our study, approximately 50% infection rate was seen in the pentoxifylline group despite antibiotic prophylaxis. We attributed relatively more infections occurred in the pentoxifylline group to the open fracture model. In our study, the histopathologic analysis revealed that the pentoxifylline group provided higher histological scores for the open femur fractures than the control group both on the 15th (p > 0.05) and 30th (p < 0.05) days. However, in terms of biomechanical and radiological points of view, pentoxifylline did not ensure better fracture healing when compared with the control group. We consider that this insufficient performance of pentoxifylline may be attributed to the high infection rate.
Pentoxifylline has also a broad range of effects. 28 Although the clinical trials with pentoxifylline have often been too small in size to reach statistically significant findings regarding the impacts on hard end points, a review of the existing literature suggests that pentoxifylline may have the potential for slowing the progression of atherosclerosis, stabilizing plaque, reducing risk for vascular events, improving the outcome of vascular events, dampening the systemic inflammatory response following cardiopulmonary bypass, providing symptomatic benefit in angina and intermittent claudication, enhancing cerebral blood flow in patients with cerebrovascular disease while slowing the progression of vascular dementia, improving prognosis in congestive heart failure, and aiding diabetes control. 29
Sildenafil, a cGMP-dependent selective PDE5 inhibitor, started clinical development as an agent for the treatment of hypertension and angina, and subsequently evolved into a revolutionary new oral treatment for erectile dysfunction. Sildenafil was then further developed to become a much-needed new oral treatment for pulmonary arterial hypertension, and has also been shown to be effective in treating severe Raynaud’s phenomenon associated with systemic sclerosis and digital ulceration. Later studies have suggested that sildenafil has also promise in the treatment of respiratory disorders with ventilation/perfusion mismatch, congestive cardiac failure, hypertension, and stroke. 30
Sildenafil has been shown to be an important stimulus of angiogenesis through the upregulation of pro-angiogenic factors and control of cGMP concentration. 31 It has been shown that sildenafil uses the angiogenic factors through the upregulation of different pro-angiogenic growth factors. 32 Sildenafil affects the metabolism by means of NO. It was reported that sildenafil accelerates the healing of bone fractures and defects. 13 It is known that the positive effect of PDE5 inhibitors on bone healing is related to the increase of NO synthase (NOS) enzymes and CYR61 in the healing fracture tissue. 33 Angiogenic and osteogenic factors associated with VEGF and CYR61 proteins are involved in fracture healing, 19 and reduced vascularity at the fracture site has been shown to be one of the most important risk factors for delayed fracture healing. 13 Lienau et al. concluded that the reduced cartilage expression of CYR61 resulted in less effective or suboptimal chondrocyte differentiation, thereby resulting in delayed healing. 19 CYR61 also has a role in promoting osteoblast proliferation and differentiation 34 and inhibits bone-resorbing osteoclasts. 35 Thus, the stimulating effect of sildenafil on CYR61 may accelerate cartilage resorption, promote osteoblast proliferation and differentiation, and inhibit osteoclast activity, thereby enabling bone fracture healing. Angiogenic processes play an important role in the early stages of fracture healing, affecting both endocardial and intramembranous pathways of osteogenesis. 36 Hausman et al. reported that antiangiogenic agents severely impair fracture healing, since they cause defective granulation tissue, absence of cartilage differentiation, and endochondral ossification. 37 VEGF activity is crucial for proper callus structure and mineralization in response to bone injury as well as normal angiogenesis. Sildenafil has been shown to induce VEGF expression in human coronary artery endothelial cells as an angiogenic response. 38,39 However, the same effect on fracture healing was not observed by Histing et al. 13 Their results might have been due to the time when the analysis was performed. Local levels of endogenous VEGF peak at 5 days and decrease toward normal levels at day 10 after fracture or bone injury. 12 However, analysis of Histing et al. occurred on day 14 after fracture. 13 Corbett et al. reported that two reversed NOS molecules were involved in fracture repair. 21 They observed high endothelial NOS (eNOS) activity and low inducible NOS activity in the early phase of fracture repair (first day after fracture), and vice versa in the second week of fracture repair. Decreased eNOS levels observed in the study of Histing et al. may be due to accelerated fracture healing by means of sildenafil. 13 Histing et al. have shown that sildenafil accelerates fracture healing in the first 2 weeks. 13 However, at the end of the fifth week, they reported that the results obtained from sildenafil were similar to those from the control group.
In our study, we deduced from the radiological evaluation that sildenafil provided more complete healing than the control group for both day 15 and day 30, although differences between the control and sildenafil groups were not statistically significant. In the biomechanical analysis, we observed that the mean breaking forces obtained from the sildenafil group were higher than those obtained from the control group; however, the differences were not statistically significant (p > 0.05). The mean absorbed energy values obtained from the sildenafil group were higher than those of the control group for both day 15 (p > 0.05) and day 30 (p < 0.05). Furthermore, higher histological scores were obtained from the sildenafil group than the control group for day 15 (p > 0.05) and day 30 (p < 0.05). Intragroup comparisons of the histological scores pointed out that the scores obtained at the 30th day were higher than those obtained at the 15th day for all three groups, indicating that a better improvement in fracture healing was observed at the 30th day than at the 15th day; however, these differences were not statistically significant (p > 0.05).
It can be deduced from the radiological, histological, and biomechanical results that the sildenafil group showed better recovery than the control group. Biomechanical and histopathological tests provide macro- and microlevel evaluations of the bone tissues, respectively. Obtained results indicated that the biomechanical and histopathological effects of pentoxifylline on bone tissue were not in agreement, namely when comparing with the control group, the histopathological effect of pentoxifylline was obviously clearer than the biomechanical effect, suggesting that pentoxifylline had a positive effect at microscale, but not at macroscale, at least, within 30 days of the treatment process.
Due to ethical concerns, the number of animals (n = 48) included in the study was kept relatively low, which can be seen as one of the limitations of the study. Moreover, the difference in the administration routes of sildenafil and pentoxifylline can be considered as another limitation of the study. Multicenter studies would increase the number of samples and provide a more certain way to evaluate the effectiveness of PDE inhibitors on bone fracture healing.
Bone healing continues to be one of the important orthopedic issues for which details are not fully understood. The effects of different chemicals on fracture healing are important in the literature, and the effects of some drugs on fracture healing are almost certain. 40 In related studies, we are increasingly aware of the effects of the use of PDE inhibitors on bone healing metabolism.
Conclusion
Sildenafil provided higher positive biomechanical, radiographical, and histological effects on the healing of open femoral fracture when compared with the control group. Although pentoxifylline had a positive histopathological effect when compared with the control group, since the biomechanical and radiographical results obtained from the control group were better than those of the pentoxifylline group, it was concluded that pentoxifylline does not have a consistent positive effect on femoral fracture healing.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by Istanbul Bağcılar Training and Research Hospital, Turkey.
