Abstract
Aim:
The study aims to describe a less invasive technique for displaced tibial intercondylar eminence fractures, using only one bone tunnel with suture anchor and EndoButton system.
Methods:
Seventeen patients were followed up after arthroscopic fixation for tibial eminence fractures using suture anchor and EndoButton. The patients were followed with clinical examinations such as Lysholm, Tegner, and International Knee Documentation Committee (IKDC) rating scales. Radiographic assessments were also performed during the follow-up for evaluating the healing of the fracture.
Results:
There were 14 male patients and 3 female patients with 10 right knees, and 7 left knees included. All the fractures healed anatomically at final follow-up. Also, no clinical signs of anterior cruciate ligament deficiency were detected. The mean Lysholm score improved significantly from 74.72 ± 3.24 (range from 70 to 79) to 96.2 ± 2.54 (range from 89 to 98) (
Conclusion:
The study demonstrated that the procedure is safe and effective, which can be another option for tibial intercondylar eminence fractures.
Introduction
Intercondylar eminence avulsion fractures or tibial eminence fractures, first described by Poncet in 1875, are relatively uncommon in clinic. 1 Tibial eminence fractures can occur in adults in association with other concomitant intraarticular pathologies such as injury of the menisci, articular cartilage, and tibial plateau fracture. 2 –5 Tibial eminence fractures have been classified into four types according to Meyers and McKeever, 6,7 type I for minimal displacement fracture, type II for elevation of one-third or a half of the eminence, type III for complete separation of the fragment to the bony bed, and type IV for comminuted fracture. Displaced fractures of the intercondylar eminence will result in nonunion or malunion and cause instability or loss of knee extension. 8 Therefore, surgical reduction and fixation is commonly recommended.
The application of arthroscopic procedures to intraarticular fracture treatment has expanded during the past decade, with regard to the surgical morbidity, time of hospital stay, recovery, and complications such as infection and loss of knee motion. 1,9 –11 Several arthroscopic fixation techniques have been reported, such as crossed percutaneous pin fixation, 10 metal screws fixation, 12 –16 staple fixation, 17 suture fixation, 18 –25 and K-wire folded fixation. 26 Here, we describe a new technique using only one bone tunnel with suture anchor and EndoButton system, which is believed to be effective and may be another option for arthroscopic reduction and fixation of displaced tibial intercondylar eminence fractures.
Patients and methods
The study included 17 consecutive adult patients who underwent arthroscopic treatment of displaced intercondylar eminence fractures at the Changzhou No. 2 People’s Hospital between May 2008 and September 2012. The patients with anterior instability (grade II or more) results from displaced intercondylar eminence fractures (Figure 1) in skeletally mature patients were included. Avulsion fracture of the intercondylar eminence is diagnosed by anterior instability examination and radiographic evidence of bone fragmentation. Anterior instability was determined by performing the anterior drawer test and the Lachman test. The anterior drawer test was performed at 90° of knee flexion and was graded according to the extent of anterior translation (grade I, translation <5 mm; grade II, translation of 5 to 10 mm; and grade III, translation >10 mm). The exclusion criteria were as follows: tibial plateau fracture, nerve or vessel damage, multiligament injury, knee dislocation, or less than 10 months of follow-up. The study was approved by the Changzhou No. 2 People’s Hospital. Written informed consent was obtained from all participants.

Anteroposterior and lateral radiographs of tibial eminence fracture before and 3 months postoperatively.
Surgical technique
All patients were operated on by the same surgeon. The arthroscopic procedure was performed under general or epidural anesthesia and the patients were placed in supine position with the knee in 90° of flexion. A pneumatic tourniquet is typically used to control bleeding and improve visualization. The arthroscopic view is obtained from an anterolateral portal. The hematoma is debrided to expose the fracture site using a shaver. The fracture type and concomitant pathologies were evaluated. Interposed tissue such as fracture debris, fat pad, and transverse ligament is removed so that the avulsed bone fragment can be easily reduced in its bony bed with a probe.
After the trial reduction, a suture hook (Linvatec, Largo, Florida, USA) loaded with No. 2–0 polydioxanone suture (PDS; Ethicon, Somerville, New Jersey, USA) was introduced through the anteromedial portal and pierced the fibers of the anterior cruciate ligament (ACL). The PDS was then advanced into the joint while the suture hook was removed. A suture grasper was used to retrieve the end of the PDS out of the joint through the anteromedial portal.
A 3-cm longitudinal incision was made over the proximal anteromedial tibia, and by use of the ACL tibial guide, a 5-mm bone tunnel was drilled toward the fracture site. Then, the displaced fragment was reduced and temporarily fixed with a 0.8-mm Kirschner wire (K-wire), which also acted as a guide for the screw. The cannulated suture anchor was then placed through the K-wire (Figure 2(a)).
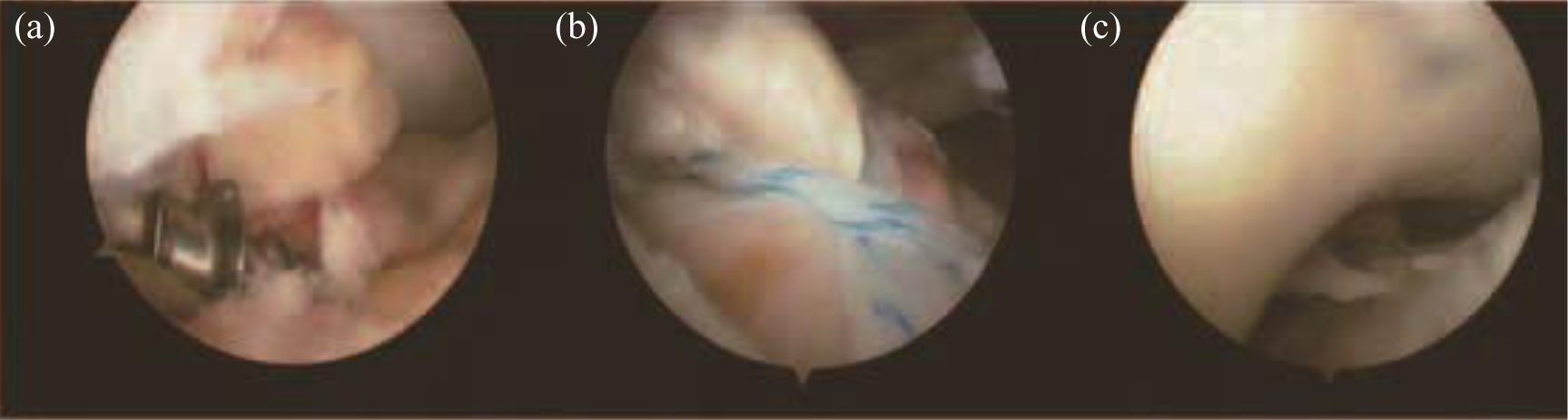
Surgical procedure under arthroscopy. (a) The cannulated suture anchor was placed to reduce and fix the fracture fragment. (b) The PDS was used as a guide suture to deliver the suture of the anchor through the base of the ACL. (c) The fragment was held reduced and the sutures were kept under tension until all sutures were tied. PDS: polydioxanone suture; ACL: anterior cruciate ligament
The PDS described above was used as a guide suture to deliver the suture of the anchor through the base of the ACL (Figure 2(b)). The medial and lateral limbs of the suture were then brought out of the bone tunnel using a suture grasper through the anteromedial portal to deliver the suture limbs to the suture retriever that was introduced through the tunnels. Finally, the sutures were tied over with the EndoButton system with the knee in 30° of flexion. The fragment was held reduced with the probe or blunt trocar, and the sutures were kept under tension until all sutures were tied (Figure 2(c)). The surgeon then reexamined the reduced fragment with the probe, checking the reduction and stability of the fragment throughout knee flexion and extension. ACL tension was also checked with the probe. Postoperative radiographs were used to confirm anatomic reduction of the fragment.
Postsurgery rehabilitation
All patients underwent the same rehabilitation program. During the first postoperative week, each patient was immobilized using a full-extension knee brace. Quadriceps-strengthening, isometric exercises, and straight-leg raises were allowed immediately after surgery. A brace was used for the first month and the patients were encouraged to bear weight as tolerated. Among the first 4 weeks, the range of motion (ROM) patients was limited to 45° in flexion. At week 6, ROM was 0° to 90° in flexion, and at week 8 was more than 120° in flexion.
Follow-up evaluation
All the patients were evaluated with clinical and radiographic assessments (Figure 1) during the follow-up. The Lysholm scoring was used to describe the subjective symptoms, and the Tegner activity score and the International Knee Documentation Committee (IKDC) were also used. The IKDC score combines the assessment of both symptoms and signs. Each category is assigned an overall grade of A (normal), B (nearly normal), C (abnormal), or D (severely abnormal).
Statistical analysis
The Statistical Package for Social Sciences software (SPSS version 16.0, Inc., Chicago, Illinois, USA) for Windows was used for statistical analysis. The clinical data were presented as mean ± SD and compared by the Student’s
Results
There were 14 male patients and 3 female patients with 10 right knees and 7 left knees included. The mean age was 39.3-years old (range from 19 to 57). And the average period between injury and operation is 14.5 days (range from 4 days to 31 days). According to the Meyers and McKeever classification, there were eight type II fractures, eight type III fractures, and one type IV fracture. There were 6 sports accidents and 11 traffic accidents in regard with the injury mechanism. Among the patients, a total of 12 patients presented with a combined injury, including 8 meniscal tears and 6 articular cartilage damages. The mean follow-up is 14.0 months (range from 10 months to 24 months). The basic characteristics of the patients included are shown in Table 1.
The basic characteristics of the patients included.

No major complication such as nerve and vessel injury, infection, or deep venous thrombosis happened preoperatively. All the fractures healed anatomically at final follow-up, as shown in radiologic assessments. The visual analog scale score improved significantly 3 days after surgery (3.5 ± 1.0) in comparison with the score before surgery (7.7 ± 1.2). And from 2 weeks after surgery, the pain remains slight and stable. ROM measurement showed that 16 of all the patients achieved normal flexion degree when compared with the unaffected side, with the exception of 1 patient with the flexion degree of only 0° to 110°. At the final follow-up, no clinical signs of ACL deficiency were detected as shown with Lachman and drawer tests. Also, there were no signs of impingement. The mean Lysholm score was 74.72 ± 3.24 (range from 70 to 79) preoperatively, and the Lysholm score improved significantly postoperatively with the mean score of 96.20 ± 2.54 (range from 89 to 98) (
Statistical analysis of clinical evaluations.

IKDC: International Knee Documentation Committee.
Discussion
The study describes a less invasive technique for arthroscopic reduction and fixation of displaced tibial intercondylar eminence fractures, using only one bone tunnel with suture anchor and EndoButton system. The clinical and radiographic results demonstrated that this procedure is safe and effective, which can be another option for tibial intercondylar eminence fractures.
Tibial eminence fractures involve bony avulsion of the ACL from its insertion on the tibial spine. Treatment of the fracture includes both operative and nonoperative methods, which is always dependent on the degree of trauma, namely, dependent on the Meyers and McKeever classification. Conservative treatment (immobilization with the knee fully extended) is enough for patients with type I fractures. For type II fractures, both operative and nonoperative methods were widely used, but the ideal treatment remains unclear. And surgical treatment is usually indicated for type III and IV fractures. 27
When operative treatment is utilized, methods of fixation vary; multiple surgical methods of reduction and fixation for displaced tibial eminence avulsion fractures have been described. Since open surgery has a higher incidence of postoperative stiffness than arthroscopic techniques and the advances in arthroscopic techniques and devices, the application of arthroscopic procedures to intraarticular fracture treatment has become increasingly popular during the past decade. 1,10 Also as the arthroscopic reduction and fixation method has the advantages such as the evaluation and treatment of the concomitant lesions including meniscal tears, it is less invasive with regard to the decreased exposure of the posterior capsule or muscle. As a result, the arthroscopic methods are most commonly applied to stabilize the displaced bony fragment of the tibial eminence nowadays. 28
Much has been published about the different techniques for arthroscopic-assisted reduction and internal fixation for tibial eminence fractures, including absorbable surgical suture of the fragment, fixation with a wire knot, fixation with a cannulated screw, fixation with K-wire, stabilization using absorbable elements, and so on. However, two modes of fixation, suture and screw drilled through bone tunnels are most commonly described, with both satisfactory postsurgery outcomes. However, the ideal method of fixation, suture versus screw, has not been defined. 29
The screw fixation technique provides stable fixation and allows for early ROM, as well as the advantage of direct reduction and compression of the fracture fragment. 30 For example, the use of cannulated screws can achieve a rigid fixation of the fracture fragment and potentially earlier weight-bearing. However, the limited space makes the arthroscopic fixation with a screw difficult, in regard with the challenge of achieving a satisfactory angle of placement. On the other hand, the screw methods can easily crush bony fragments and cut ligaments, and the screw head impingement on the intercondylar notch can decrease terminal knee extension, increasing the likelihood of damaging the open physis and requiring a second procedure to remove the implant. Also, concerns about the screw purchase with fragment comminution, as well as the transphyseal fixation in the skeletally immature patient, are increasingly common.
Arthroscopic suture fixation has also evolved over the years, including suture loop transporters, retrograde guides, multiple drill tunnels, and various tissue penetrators for suture passage, which is fundamentally divided into two classes. One is based on the ACL itself (ligament suture methods, when the fracture of the intercondylar eminence of the tibia is comminuted or small in size), and the other is based on the avulsed bone fragment (avulsed bone fragment suture methods). 31 One distinct advantage of suture fixation is that it obviates a future operation for hardware removal in regard with its bioabsorbable ability and serves to minimize damage to the growth plate. Bong et al. have shown that suture fixation is biomechanically stronger than screw fixation. The primary problem with suture fixation technique is the difficulty in performing the arthroscopic procedure. Also, the drill holes in the tibia for suture fixation may produce a second damage. And significant soft tissue reactions were reported with biodegradable implants. Suture anchors also do not provide a direct reduction of the fracture fragment, which is based on a tension band effect, though healing times and functional outcomes appear comparable with those of other treatment techniques. 32 On the other hand, biomechanical study with a single-cycle test and cyclic loading test showed no significant difference in maximal load, yield load, and stiffness between Ethibond suture (Ethicon, Somerville, New Jersey, USA) fixation and screw fixation for tibial eminence fractures.
The technique described here is safe and suitable for all types of fractures, with the advantages of easy surgery procedure, rigid fixation, rapid recovery, and so on. The technique is easy to perform as only one bone tunnel for suture fixation is needed, and more importantly, less bone tunnel means less invasive when compared with the traditional suture techniques, which may be the greatest advantage of the technique. And both the application of screw and suture techniques results in a double protection for fragment fixation. Similarly, in comparison with the traditional screw technique, there is less incidence of impingement and causing bone fragments as the screw here is much smaller. Also, there is no need for implant removal. However, the present technique also has some limitations. The most important limitation is the absence of the biomechanical evaluation of the above fixation technique in optimizing fracture fixation. Also, the study was only performed in 18 patients though the outcomes seem perfect. And the above fixation technique used metal cannulated suture anchor and not the bioabsorbable anchor, which may be more suitable for the patients. On the other hand, as both the suture anchor and the EndoButton system were employed, the total cost is expensive, which may be the most disadvantage that limits the technique. Moreover, although the method has the advantages of both the suture and screw techniques, it also has the drawbacks of both techniques, like the limited space of arthroscopic fixation with a screw and the need for removing EndoButton.
Conclusion
In conclusion, the present study describes a less invasive technique for displaced tibial intercondylar eminence fractures, using only one bone tunnel with suture anchor and EndoButton system. The clinical and radiographic results demonstrated that this procedure is safe and effective, which can be another option for tibial intercondylar eminence fractures.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grants from the National Natural Science Foundation of China (81171680 to Y.W.), the science and technology support of Changzhou (CE20135054 to Y.W.). The project of Jiangsu province (BE2015632 to Y.W), and the National Natural Science Foundation of China (81601919 to Q.Z.).
