Abstract
Introduction
Breast reconstruction is considered an important element of breast cancer care, aiming to restore the natural appearance of the breast and improve well-being following mastectomy.1,2 Immediate breast reconstruction (IBR) is associated with an increased quality of life, satisfaction with breasts, and physical, psychosocial, and sexual well-being BREAST-Q scores.3–8 Immediate breast reconstruction is becoming more common than delayed reconstruction in Canada, the United States, United Kingdom, Germany, Italy, and Australia, partially attributed to improved aesthetic outcomes, the need for fewer surgical procedures, faster recovery, reduced hospitalizations, earlier postoperative mobilization, and lower costs.9,10 Notwithstanding recognized benefits of breast reconstruction, there are persistent disparities in the availability of IBR. Racial disparities have been well-reported in the United States and Europe with respect to who receives breast reconstruction.5,11,12 Geographic location, socioeconomic status (SES), cancer stage, and age may further contribute to variations in IBR access. 12
Rural residents often experience limited healthcare access and worse health outcomes compared to their urban counterparts.13,14 Age, race, healthcare costs, travel time, and distance to academic centers may contribute to these differences.15,16 Vangsness et al 12 and Retrouvey et al 15 found that women in rural locations were less likely to receive breast reconstruction at any point in their treatment course compared to urban patients. In a systematic review of studies based in the United States, Australia, United Kingdom, and Canada, potential reasons for this disparity included reduced plastic surgeon density in rural communities, greater travel distances/costs to receive reconstruction, less patient education about reconstruction, and differences in surgical oncologist referral patterns. 15 A Canadian retrospective cohort study reported that IBR patients traveled significantly farther than patients who underwent mastectomy alone, supporting that rural patients may face compounded barriers to surgical care. 17
While geographic disparities in access to breast reconstruction regardless of timing have been established, no meta-analysis has specifically investigated and quantified disparities in IBR rates between rural versus urban patients. This analysis is critical to identify geographic inequities and inform policy development and resource allocation to improve access to this valuable component of breast cancer care in underserved populations. Therefore, we aimed to (1) compare rates of IBR among patients from rural and urban locations; and (2) identify sociodemographic and economic factors associated with breast reconstruction rates.
Methods
Requirement for institutional review board approval was waived. This work relied entirely on published primary research. This study followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses 18 and Meta-Analysis of Observational Studies in Epidemiology guidelines. 19 This work abided by the Tenets of the Declaration of Helsinki. The study was prospectively registered on PROSPERO (CRD420251106592).
Search Strategy and Study Selection
We systematically searched MEDLINE (Ovid), Embase, Web of Science, and CENTRAL from inception to May 15, 2025, without language restrictions. Database search strategies were designed with an expert medical librarian (see Appendix, Supplemental Digital Content 1). The yield of screened studies was limited by the specificity of our research question involving defined populations and outcomes. Citations were manually reviewed to identify studies missed in the initial search.
Studies were included if they (1) reported primary data on mastectomy patients; and (2) reported IBR rates for patients living in both urban and rural communities. Studies were excluded if they (1) were published as an abstract, review, meta-analysis, case report, or conference report or (2) did not specify the immediate timing of breast reconstruction.
Two independent reviewers performed title and abstract screening, full-text screening, data extraction, and risk of bias (ROB) assessment. Discrepancies were resolved via discussion with a third reviewer (AM
Data Extraction and ROB Assessment
Extracted data included study descriptors (publication year, design, data collection years), participant characteristics (mean age, population), IBR rates and rural or urban residence, and adjusted odds ratios (ORs), if reported. The ROB was evaluated using the Risk of Bias in Non-Randomized Studies - of Exposures tool. 20 The evidence certainty of study outcomes was evaluated using the GRADE tool. 21
Definition of Exposure
The U.S. Rural-Urban Continuum Codes are widely used in the literature, indicating that urban areas have populations of at least 5000, and rural areas contain less than 5000 people. 22 However, given the heterogeneity in definitions across studies, we accepted each study's classification of rural versus urban (eg, “rural” vs “urban,” “remote” vs “non-remote,” “major city/metropolitan” vs “non-major city/non-metropolitan”). We extracted rural-urban categorizations as reported to reflect real-world differences in geographic classification.
Data Synthesis and Statistical Analysis
The primary outcome measure was the literature-pooled OR of rural patients receiving reconstruction compared to their urban counterparts with a 95% confidence interval (CI). Given the international scope of this review, IBR rates were pooled across countries. A random-effects model with restricted maximum likelihood estimation (REML) was performed to estimate the pooled OR with a 95% CI (α = 0.05) and to account for system-level and population-level heterogeneity. Pooled estimates may not be fully comparable across countries. Statistical heterogeneity was measured using the I2 value, which was interpreted according to Cochrane-endorsed thresholds: (i) might not be important (0%-40%); ii) moderate (30%-60%); substantial (50%-90%); and considerable (75%-100%) heterogeneity. 23 Sensitivity analyses were conducted to assess whether including crude ORs influenced the pooled results and to determine the impact of including studies that defined rural populations as communities with fewer than 10 000 people. A leave-one-out analysis was performed to evaluate the influence of individual studies on the pooled ORs and heterogeneity. Analyses and figure syntheses were conducted in R (version 4.3.0; R Foundation for Statistical Computing).
Univariate meta-regression was conducted with REML estimation to explore study-level covariates (mean age, SES, race, cancer stage, Charlson Comorbidity Score, mean distance to hospital, hospital type, data collection year) that might explain heterogeneity. Covariates with at least 10 studies were included in the meta-regression to prevent overfitting. 23 Covariates with less than 10 studies were descriptively summarized. Meta-regression results were presented as coefficients and intercepts, 95% CIs, and P-values. The proportion of heterogeneity explained by covariates and the goodness of fit was evaluated using the R2 value. Multivariate meta-regression was conducted if there were at least 10 included studies per aforementioned variable to prevent overfitting. 23
The midpoint data collection year (mean of the start and end of data collection) was analyzed categorically and continuously to explore temporal changes in IBR rates. Subgroup analysis included studies reporting geographic IBR rates using data between 2004 to 2008, 2009 to 2012, and 2013 to 2017. Univariate meta-regression used midpoint data collection year as a continuous covariate to assess temporal trends.
While SES was reported in tertiles, quartiles, or quintiles across studies, we collapsed this data into 3 SES levels: low (tertile 1, quartile 1, and quintiles 1 and 2), mid (tertile 2, quartile 2, quintile 3), and high (tertile 3, quartiles 3 and 4, and quintiles 4 and 5). High SES served as the reference group, and low and mid SES proportions were considered continuous covariates.
Exploratory country-specific subgroup analysis and univariate meta-regression by reconstructive type (implant, autologous, combined implant and autologous) were conducted.
Results
The search yielded 815 unique studies (see Figure 1). Citation screening identified 2 additional studies; 15 studies met inclusion criteria.17,24–37 These studies were published between 2013 and 2025 and originated from the United States (predominantly private, multipayer system) (n = 9), Canada (public system) (n = 2), Australia (public-private system) (n = 3) and Japan (public system) (n = 1) (see Table, Supplemental Digital Content 2). Most IBR was tissue expander/implant-based (n = 103 431), followed by autologous (n = 79 260) and combined tissue expander/implant and autologous (n = 29 796). Most patients were White (n = 1 551 771), followed by Black (n = 199 321), Asian (n = 63 688), and Hispanic (n = 50 028); 72 427 patients did not identify as these races.
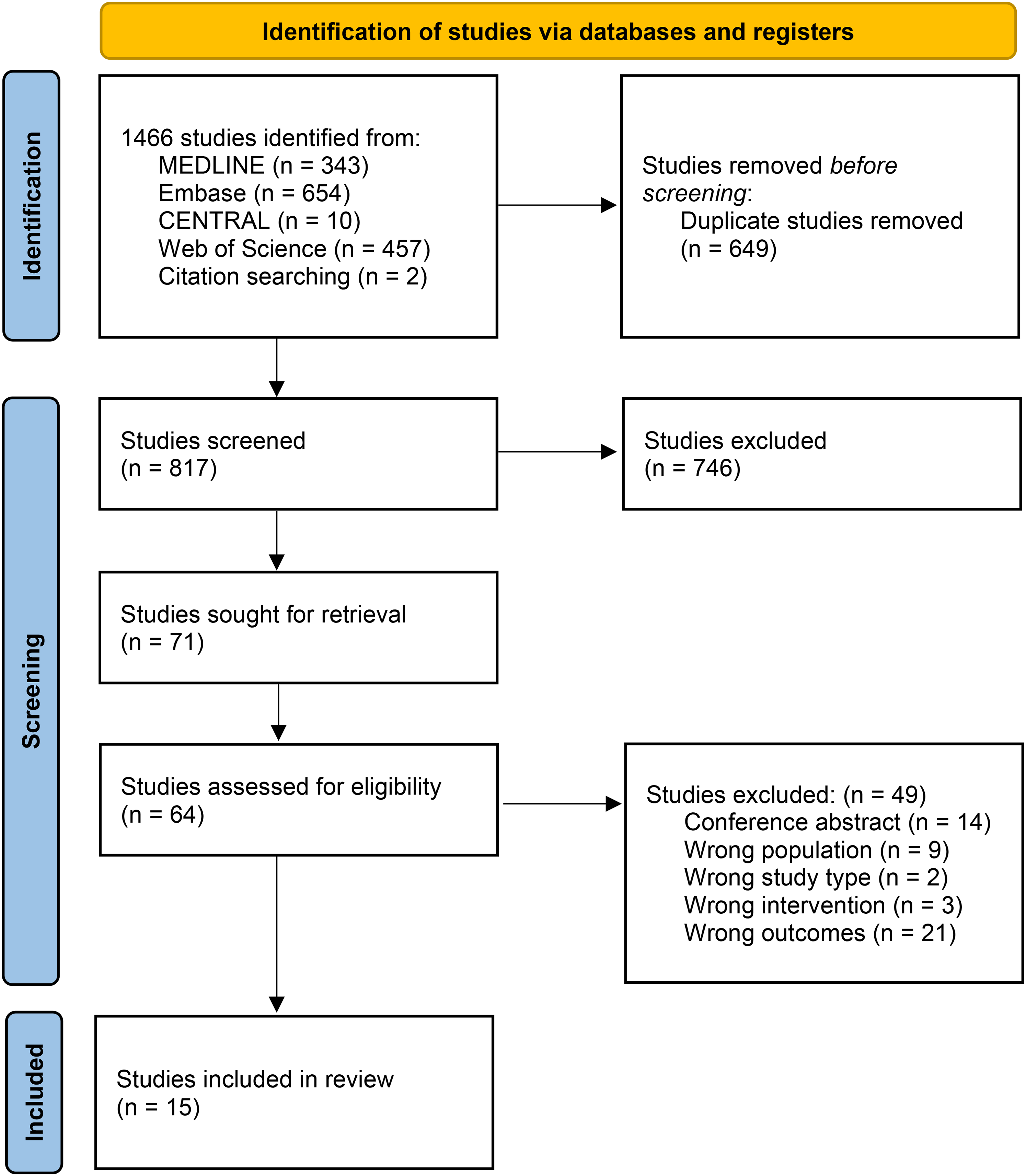
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram.
Risk of Bias
All included studies were observational cohort designs with low ROB (n = 13) and moderate ROB (n = 2), predisposing to low GRADE certainty evidence (see Table, Supplemental Digital Content 3). Study weaknesses included potential confounding (n = 2) and missing data (n = 1). Studies reliably measured the outcome with low ROB in selecting participants into the study (n = 15) and selecting the reported result (n = 15).
Meta-Analysis
Across 15 studies, there were 46 986 rural patients and 1 833 906 urban patients who underwent mastectomy, of whom 8179 rural patients and 658 342 urban patients underwent IBR. The rate of reconstruction in rural patients was 13.44% (95% CI [9.69-18.35], I2 = 99%). The rate of reconstruction in urban patients was 21.95% (95% CI [16.35-28.82], I2 = 100%). Rural patients were significantly less likely to undergo IBR compared to urban counterparts (OR 0.67; 95% CI [0.57-0.79]; P < .001; I2 = 97%) (see Figure 2).
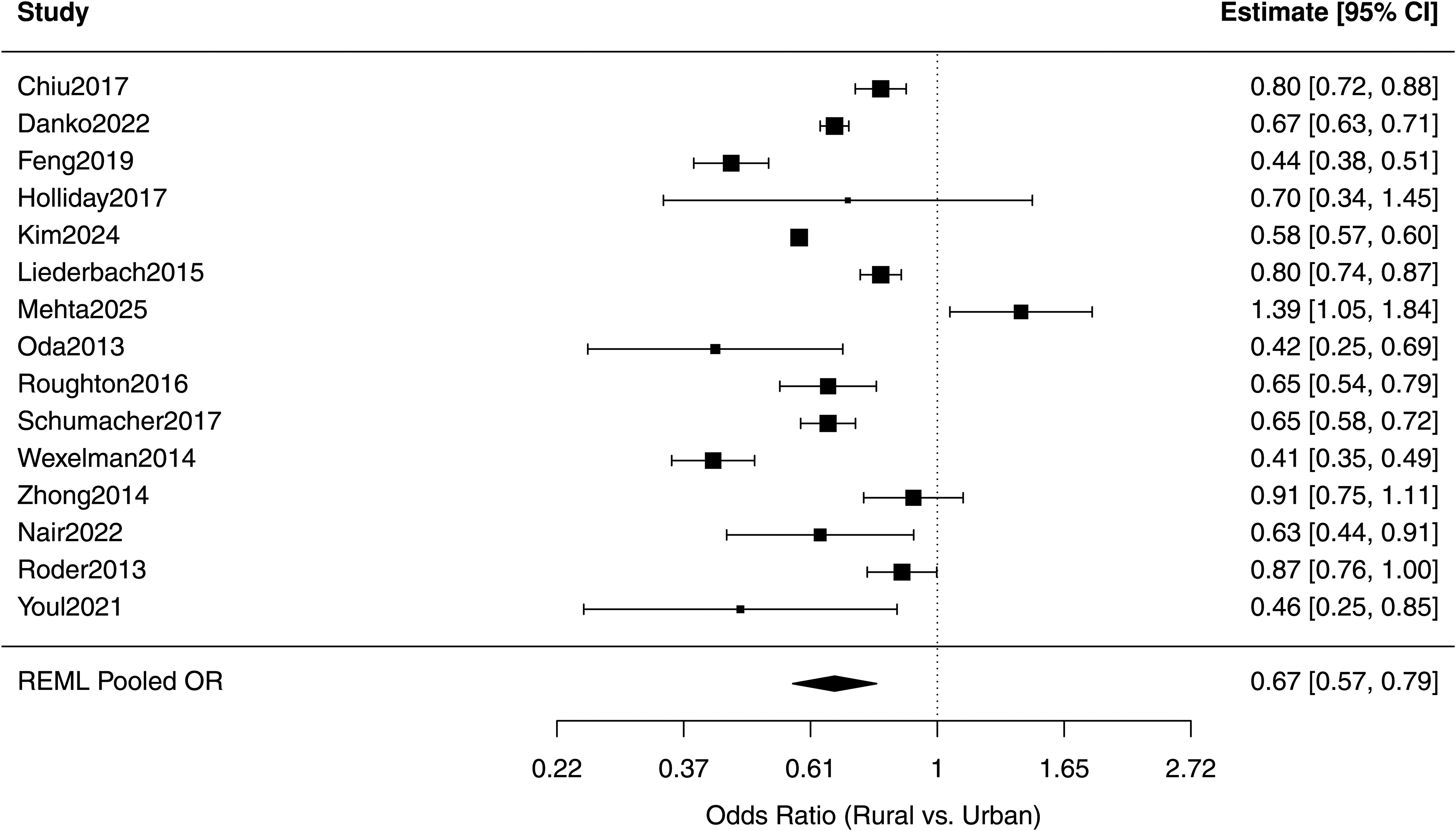
Forest plot summarizing the pooled odds ratio (OR) of immediate breast reconstruction (IBR) in rural versus urban patients.
Sensitivity analysis showed a slightly reduced effect size in adjusted-only studies (n = 12) compared to all studies (OR 0.73; 95% CI [0.63-0.84]) (n = 15). The direction and statistical significance of the association remained consistent, suggesting that the inclusion of crude ORs did not introduce meaningful bias.
Two studies defined rurality using a strict threshold (communities with <10 000 people),17,27 while the remaining 13 applied broader criteria. When excluding the 2 strict-definition studies, the pooled OR remained consistent (OR 0.65; 95% CI [0.54-0.78]).
Across all iterations of the leave-one-out analysis, the pooled ORs remained within a narrow range with CIs overlapping the pooled estimate. No study disproportionately influenced heterogeneity.
Subgroup analysis using data collection period stratification and univariate meta-regression based on data collection year found that the pooled ORs across the 3 intervals (2004-2008, 2009-2012, 2013-2017) were consistently below 1 (P < .0001), indicating a persistent disparity affecting rural populations across all periods. The pooled ORs were 0.66 (95% CI [0.50-0.87]) for 2004 to 2008, 0.70 (95% CI [0.62-0.78]) for 2009 to 2012, and 0.64 (95% CI [0.38-1.09]) for 2013 to 2017 (all P < .001). Confidence intervals between the groups overlapped considerably. There was no clear trend suggesting temporal changes in geographic disparities. Heterogeneity remained high within each period (I2 = 94%, 69%, 98%).
Meta-Regression
Univariate meta-regression analyses were conducted for mean age (n = 14), SES (n = 12), and midpoint year of data collection (n = 15). Mean age variability did not significantly explain the observed rural-urban disparity (regression slope 0.0139, P = .57) and did not explain between-study variance (R2 = 0). Significant residual heterogeneity remained (QE = 170.50, P < .0001), further suggesting that mean age alone did not account for inter-study differences in ORs. The pooled OR comparing low versus high SES was 0.69 (95% CI [0.13-3.63]), and for mid versus high SES was 0.29 (95% CI [0.06-1.60]). Socioeconomic status did not significantly explain variability in ORs (QM = 2.0647, P = .36) and did not account for between-study heterogeneity (R2 = 0). The regression slope for data collection year was nonsignificant (β = 0.0026, P = .92), with an R2 value of 0. This covariate did not explain between-study heterogeneity in effect sizes. Substantial residual heterogeneity remained (τ2 = 0.0978, I2 = 96.34%, QE = 131.95, P < .0001). Data collection year did not significantly explain the observed rural-urban disparity (QM = 0.0114, P = .92).
Exploratory Analyses
Country-specific analyses showed consistently lower odds of undergoing IBR among rural patients in the United States, Australia, and Japan. In Canada, while rural patients were similarly less likely to undergo IBR, the CI crossed 1 (see Table, Supplemental Digital Content 4). Univariate meta-regression by reconstructive type (n = 7 studies) indicated a nonsignificant trend toward greater disparity in settings where implant-based reconstruction predominated (P = .19). These findings are considered exploratory given the limited number of studies.
Descriptive Statistics
The most frequent hospital type was academic (n = 449 355), followed by community (n = 360 445), and comprehensive programs (n = 286 645). Most patients had a Charlson Comorbidity Score of 0 (n = 1 052 893); scores 1 (n = 168 609) and 2 (n = 37 374) were less common. Most patients were stage II (n = 520 648), with fewer being stage I (n = 431 617), in situ (n = 140 532), and stage III (n = 60 762). The mean distance to hospital ranged from 11.71 to 24.68 miles. Most patients were privately insured (n = 1 096 521), followed by publicly insured (n = 735 832), and uninsured (n = 36 814).
Discussion
In this systematic review and meta-analysis, rural patients undergoing mastectomy were significantly less likely to receive IBR compared to urban counterparts. This significant association remained robust after sensitivity analysis using adjusted effect sizes, restricting the “rural” population threshold, and leave-one-out analysis. Mean age, SES, and year of data collection did not significantly impact the pooled effect size.
No meta-analysis to date has quantified geographic disparities in IBR. Yet, the observed disparity is consistent with systematic reviews investigating breast reconstruction regardless of timing, which have reported that rural residence is associated with reduced access to breast reconstruction.12,15,38 The persistence of this disparity that we found over time has also been shown in other studies.12,39,40 DeCoster et al 40 found that while breast reconstruction rates increased between 2006 and 2015 across all geographic groups, utilization among urban patients increased at a greater rate. Similarly, Vangsness et al 12 noted consistent rural-urban disparities in breast reconstruction over time.
While insufficient data on other factors precluded their inclusion in the meta-regression, distance to plastic surgeon, plastic surgeon density, hospital type, comorbidities, stage, and race may contribute to geographic disparities. Two American studies had a greater proportion of publicly insured versus privately insured patients. However, most patients were privately insured in the remaining 13 studies. Residents are more likely to be un- or underinsured in countries without universal healthcare and subsequently have lower rates of healthcare utilization. 41 Rural communities may have fewer plastic surgeons, requiring patients to travel further for care.42–44 Distance exceeding 10 miles between a patient's home and a plastic surgeon has been identified as a significant predictor of no reconstruction. 32 Referral patterns may further explain disparities. 40 General surgeons who refer to reconstructive surgeons commonly work in high-volume centers. Hence, surgeons in rural areas with less resource are less likely to refer to plastic surgeons. 40 Differences in cancer care may also contribute. Rural patients have demonstrated higher mastectomy rates, whereas urban populations undergo breast-conserving surgery more frequently.45,46 Breast-conserving surgery is often followed by adjuvant therapy that necessitates frequent healthcare visits. Interestingly, rural patients are more likely to undergo contralateral prophylactic mastectomy than urban counterparts, potentially reflecting the greater travel burden associated with multiple operations.47,48 Despite higher mastectomy rates, rural patients may experience a reduced likelihood of undergoing IBR due to limited plastic surgeon access.
In our study, academic centers were most often utilized. Vangness et al 12 and Retrouvey et al 15 found that the likelihood of breast reconstruction was lower in non-teaching, lower volume hospitals, and higher in teaching hospitals. Because most academic centers are found in urban regions, their services may be less accessible to rural patients. 49 Our exploratory subgroup analysis suggested a consistent disparity across countries. Furthermore, rural patients are more likely to experience multiple morbidity and advanced staging due to limited healthcare resources, preventative care, transportation demands, and socioeconomic disadvantage.50,51 Three included studies found a significant negative association between advanced staging and receipt of breast reconstruction, potentially reflecting the prioritization of aggressive adjuvant therapy in these patients.28,32,37 Moreover, non-White patients are less likely to undergo IBR compared to White counterparts.5,11,12 While Onega et al 52 found that rural patients had lower reconstructive odds than urban patients across locations, this difference was more pronounced in rural racial minorities, likely due to compounded barriers to IBR access, including structural racism and geographic isolation. Exploratory analyses revealed nonsignificant pronounced disparities in settings where implant-based reconstruction predominated. Future research comparing IBR rates by reconstructive type among geographic populations can further elucidate whether reconstructive type contributes to disparities.
Proposed solutions to reduce geographic disparities in IBR access include increased plastic surgeon density in rural communities and ride-sharing programs or transportation company partnerships to reduce travel barriers and promote social accountability.38,40,51 Restructuring referral systems to ensure rural patients are referred to their closest plastic surgeon with adequate travel arrangements may further improve IBR access.38,51 Telemedicine can significantly reduce commuting time. 53 Virtual seminars about breast reconstruction may augment IBR access through mitigating established barriers to reconstruction, including travel requirements, lack of high-quality information, and IBR awareness. 15 Xue et al 54 proposed a telemedicine model involving a referral from a breast surgeon, virtual consultation, visual exam, and discussion with a plastic surgeon, an in-person meeting with breast and plastic surgeons and anesthesiologists, and virtual postoperative follow-up. Expanding primary care access may help address other patient-related and socioeconomic factors contributing to the disparity. Nonetheless, a holistic approach considering clinical, socioeconomic, and geographic factors should be used to inform efforts to improve IBR rates among rural patients.
This study has limitations. Many included studies lacked consistent definitions/criteria for rural versus urban status, resulting in potential misclassification bias and reduced comparability of IBR rates. The inclusion of less stringent definitions of “rural” population size may have reduced the observed pooled OR, potentially underestimating the true effect size of IBR rates between rural and urban patients. High heterogeneity was present. Subgroup analysis revealed a reduction from considerable to substantial heterogeneity for Canadian studies versus American and Australian studies, offering one potential heterogeneity source. Ultimately, our meta-analysis summarizes geographic disparities in IBR rates across heterogeneous settings, while recognizing that healthcare system context, clinical and individual factors likely influence the magnitude of this disparity. Findings were based on study-level data, limiting our ability to adjust for individual-level confounding variables. Insufficient studies precluded meta-regressions for race, stage, comorbidities, mean distance to hospital, and hospital type, which may confound the relationship between rurality and IBR rates. The international scope of this review included countries with different healthcare systems, which may limit between-study comparability.
Given the unique barriers associated with immediate versus delayed reconstruction, we studied IBR separately. While IBR requires multidisciplinary surgical coordination, one's eligibility for delayed reconstruction may be impeded by comorbidities and complications of mastectomy, such as fibrosis and chest wall changes. 55 Geographic disparities may be obscured when all breast reconstruction timelines are investigated simultaneously.
Accordingly, future studies should evaluate whether geographic disparities exist in delayed reconstruction and long-term reconstructive outcomes. The use of standardized definitions of rural and urban populations can reduce misclassification bias and improve heterogeneity. If feasible, using patient-level data can reduce residual confounding.
Conclusion
Rural patients exhibited approximately 33% lower odds of receiving IBR compared to urban patients. This disparity did not significantly improve over time. Mean age, SES, and data collection year did not explain heterogeneity nor rural-urban differences in IBR access. Geographic disparities may be multifactorial. Altogether, targeted interventions are needed to improve breast cancer care for individuals living in underserved areas. Future research should aim to characterize the impact of other factors contributing to this disparity and inform strategy development to promote access to IBR.
Supplemental Material
sj-docx-1-psg-10.1177_22925503261436341 - Supplemental material for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis
Supplemental material, sj-docx-1-psg-10.1177_22925503261436341 for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis by Alexis E. Mah, Damoon Ranjbar, Brandon Chai and Laura M. Snell in Plastic Surgery
Supplemental Material
sj-docx-2-psg-10.1177_22925503261436341 - Supplemental material for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis
Supplemental material, sj-docx-2-psg-10.1177_22925503261436341 for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis by Alexis E. Mah, Damoon Ranjbar, Brandon Chai and Laura M. Snell in Plastic Surgery
Supplemental Material
sj-docx-3-psg-10.1177_22925503261436341 - Supplemental material for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis
Supplemental material, sj-docx-3-psg-10.1177_22925503261436341 for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis by Alexis E. Mah, Damoon Ranjbar, Brandon Chai and Laura M. Snell in Plastic Surgery
Supplemental Material
sj-docx-4-psg-10.1177_22925503261436341 - Supplemental material for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis
Supplemental material, sj-docx-4-psg-10.1177_22925503261436341 for Comparing Immediate Breast Reconstruction Rates in Rural and Urban Populations: A Global Systematic Review and Meta-Analysis by Alexis E. Mah, Damoon Ranjbar, Brandon Chai and Laura M. Snell in Plastic Surgery
Supplemental Material
Footnotes
Authors’ Note
Study Registration Number: CRD420251106592.
Author Contributions
Alexis E. Mah contributed to concept and design development, data acquisition and interpretation, and manuscript writing. Damoon Ranjbar contributed to data acquisition, statistical analysis, data interpretation, and manuscript writing. Brandon Chai contributed to concept and design development, data acquisition and interpretation, and manuscript writing. Laura M. Snell contributed to concept and design development, critical manuscript revision, and manuscript writing.
Consent to Participate
Not applicable. Requirement for institutional review board approval was waived as this work relied entirely on published primary research. The results will neither disseminate nor generate patient identifiable information.
Data Availability Statement
Datasets generated and/or analyzed during this review are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Considerations
Requirement for institutional review board approval was waived as this work relied entirely on published primary research. The results will neither disseminate nor generate patient identifiable information.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
