Abstract
Introduction
The ongoing COVID-19 pandemic has had a substantial impact on the North American healthcare systems.1,2 Shortly after the pandemic was declared by the World Health Organization on March 11, 2020, 3 The American College of Surgeons (ACS) and Centres for Medicare and Medicaid Services (CMS) recommended reducing the number of elective surgical procedures performed during the initial shutdown period.4,5 During this time, the total number of procedures performed in the United States decreased by 48% when compared to the corresponding time period in 2019. 2 The COVID-19 pandemic has had a similar impact to the Canadian healthcare system.6,7 As reported by the Canadian Institute for Health Information, during the first wave of the COVID-19 pandemic, there was a 17% to 21% decline in life-saving and urgent surgeries in Canada. 6 The impact of the pandemic on elective surgeries in North America is far greater. 6 Elective surgeries have been defined by the Anesthesia Quality Institute as procedures that can be scheduled in advance and take place at any time. 8 However, the ACS statement provides additional context to this definition by outlining the varying degrees of urgency of the different types of elective procedures. 5
Decreasing the total quantity of surgical procedures performed can lead to longer wait times for patients who are awaiting surgery. For instance, a study published by Jain et al 9 in 2020 projected a backlog of one million elective orthopedic surgery cases over the first two years of the pandemic, requiring approximately 16 months to resolve the backlog. Wait times for elective surgeries in Canada reached a record high in 2020, with an average of 22.6 weeks between the time the referral was sent by the family physician to the time of surgery. 10 Long wait times can be particularly challenging for individuals awaiting a surgery that will improve their quality of life, such as in the case of elective hand surgery.11–13
Carpal tunnel syndrome (CTS), Dupuytren's disease (DD) and stenosing tenosynovitis, are common medical conditions of the hand, with high prevalence rates across the world.14–16,17,18 For instance, the prevalence of CTS has been stated to be between 1% and 5%.14–16 CTS, DD and stenosing tenosynovitis can significantly impact the quality of life of patients, as symptoms related to these conditions include pain, and decreased hand function.11–13 The initial treatment for these hand conditions is often medical management.19–21 However, failed medical management and worsening symptoms can lead to surgical management (carpal tunnel release (CTR) for CTS), fasciotomy/subtotal palmar fasciectomy for DD and pulley release/tendon release for stenosing tenosynovitis).19–21 Long wait times for surgical management of CTS, DD and stenosing tenosynovitis can result in decreased quality of life for patients who experience pain and decreased hand function associated with these conditions.11–13 The purpose of this retrospective chart review study was to evaluate the number of surgical procedures performed for CTS, DD and stenosing tenosynovitis during the COVID-19 pandemic, compare it to a corresponding time period prior to the pandemic and evaluate its impact on wait times.
Materials and Methods
This was a descriptive retrospective chart review study conducted in accordance with the REporting of studies Conducted using Observational Routinely-collected Data (RECORD) checklist 22 (Supplemental Material 1). Research ethics board approval for this project (Project ID: 2021-14107-C)) was obtained.
All health records for individuals who underwent surgery in the main operating room or minor procedure room for elective CTS, DD or stenosing tenosynovitis were retrieved from the Health Information Systems from two university affiliated hospital systems, for the time horizon of the study: March 11, 2018 to July 1, 2019 (Pre-Pandemic time period) and March 11, 2020 to July 1, 2021 (Covid-19 time period). These time periods were selected to allow for trends to be compared between a COVID-19 pandemic time period (March 11, 2020, July 1, 2021) to a corresponding time period prior to the pandemic (March 11, 2018, to July 1, 2019). The two university affiliated hospital systems involved with this study were subjected to Ontario elective surgery shutdowns. 23 Surgical management of CTS, DD and stenosing tenosynovitis were selected as the most common elective hand surgeries at the local institutions.
The primary outcome was defined as number of procedures performed for CTR, fasciotomy/subtotal palmar fasciectomy and pulley release/tendon release during the COVID-19 pandemic (March 11, 2020 to July 1, 2021) compared to prior to the pandemic (March 11, 2018 to July 1, 2019).
Secondary outcomes included the mean wait time (days) for CTR, fasciotomy/subtotal palmar fasciectomy and pulley release/tendon release during the COVID-19 pandemic (March 11, 2020 to July 1, 2021) compared to prior to the pandemic (March 11, 2018 to July 1, 2019). Wait time was defined as the time-period between the surgeon's decision to treat surgically and the time of surgery (Wait 2). 24 It should be noted that Wait 1 (the time period between the date the referral request is sent by the family physician and later received by the specialist's office 24 ) was not captured, as confounding variables at the institution impacted this wait time. The cumulative percentage of cases achieving target wait times as set by the Wait Time Alliance 25 was also calculated for each procedure type for each time period. Potential variables as predictors of wait times were determined a priori, including: a) age 26 ; b) gender 27 ; c) socioeconomic status (determined by postal code) 28 ; d) geographic location (rural vs urban) 29 ; and e) comorbidities. 30 Socioeconomic status was determined by cross-referencing patient postal codes with data from the Government of Canada on average household income by postal code. 31 A geographical region was defined as urban if it fell within a census metropolitan area (CMA) as defined by the Government of Canada. 32 Comorbidities included number of known medical conditions that increased likelihood of morbidity and mortality in the patient. Hand comorbidities were number of other conditions of the hand (including but not limited to previous trauma, CTS, DD, stenosing tenosynovitis, condition(s) affecting the joint(s) of the hand).
A search strategy was designed to capture cases of patients who underwent surgery for CTS, DD and stenosing tenosynovitis in the aforementioned time periods. To identify patients who met inclusion criteria, a list (removed of patient identifiers) of potential eligible patients was requested from Research Decision Support at the university affiliated hospital systems included in this study. For individuals who underwent CTR, fasciotomy/subtotal palmar fasciectomy or pulley release/tendon release on both hands (2 distinct surgeries), only the first surgery was extracted. The health record data, including outcomes and patient demographics, was extracted by four study team members (KU, SL, RD, SJ) from the health record information systems. Patient records that had a wait time (between decision to treat and surgery date) that exceeded more than one year (365 days) were omitted as per care guidelines, as patients would require re-referral to the operating surgeon. This was chosen to mitigate any potential bias that may be to 1) scheduling their procedure from their second referral (re-referral) or 2) due to other potential confounding variables not related to the healthcare system, but due to patient factors.
Statistical Analysis
Descriptive statistics and between group comparison was performed for each of the pre-pandemic and pandemic groups, for each surgical procedure type (CTR, fasciotomy/subtotal palmar fasciectomy and pulley release/tendon release). Continuous variables were reported as mean with standard deviation. Cumulative percentage tables were generated to determine the proportion of patients that fell above a pre-determined cut-off of 182 days based on Health Quality of Ontario target wait time (Priority 4). 33 A One-Way ANOVA (Kruskal-Wallis test) was conducted as data was non-parametric. This analysis was used to determine if there was a statistically significant difference in the pre-pandemic and pandemic groups for CTR, fasciotomy/subtotal palmar fasciectomy and pulley release/tendon release. A univariate regression analysis of wait times and the variables determined a priori a) age 26 ; b) gender 27 ; c) socioeconomic status (determined by postal code) 28 ; d) geographic location (rural vs urban) 29 ; and e) number of comorbidities) 30 was completed. IBM SPSS Statistics for Macintosh, Version 27.0 (Armonk, NY: IBM Group 34 ) software was used for statistical analysis.
Results
The charts searched between March 11, 2018 to July 1, 2019 (Pre-Pandemic time period) and March 11, 2020 to July 1, 2021 (Covid-19 time period) retrieved and outlined in Figure 1. 906 patient records were identified from the database. There were 41 patient records that were pulled in duplicate for CTR, 5 for fasciotomy/subtotal palmar fasciectomy, and 8 for pulley release/tendon release, as those individuals had surgery bilaterally. Patient records that exceeded more than one year (365 days) were omitted as per care guidelines (n = 137). Therefore, a total of 715 cases were included (447 CTR cases, 135 fasciotomy/subtotal palmar fasciectomy cases and 133 pulley release/tendon release cases). Patient demographics are listed in Table 1.
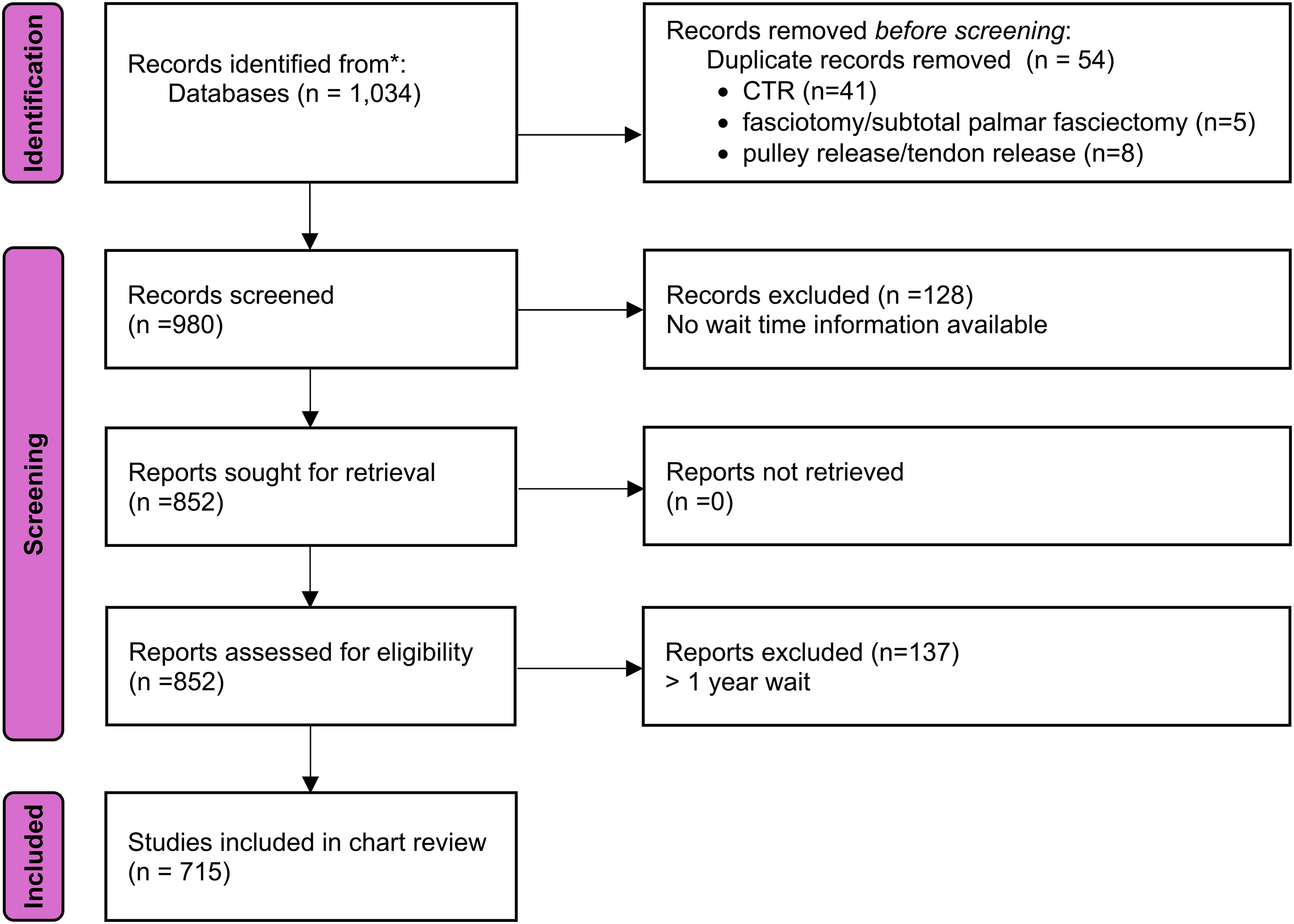
Consort diagram of patient charts.
Patient Demographics.
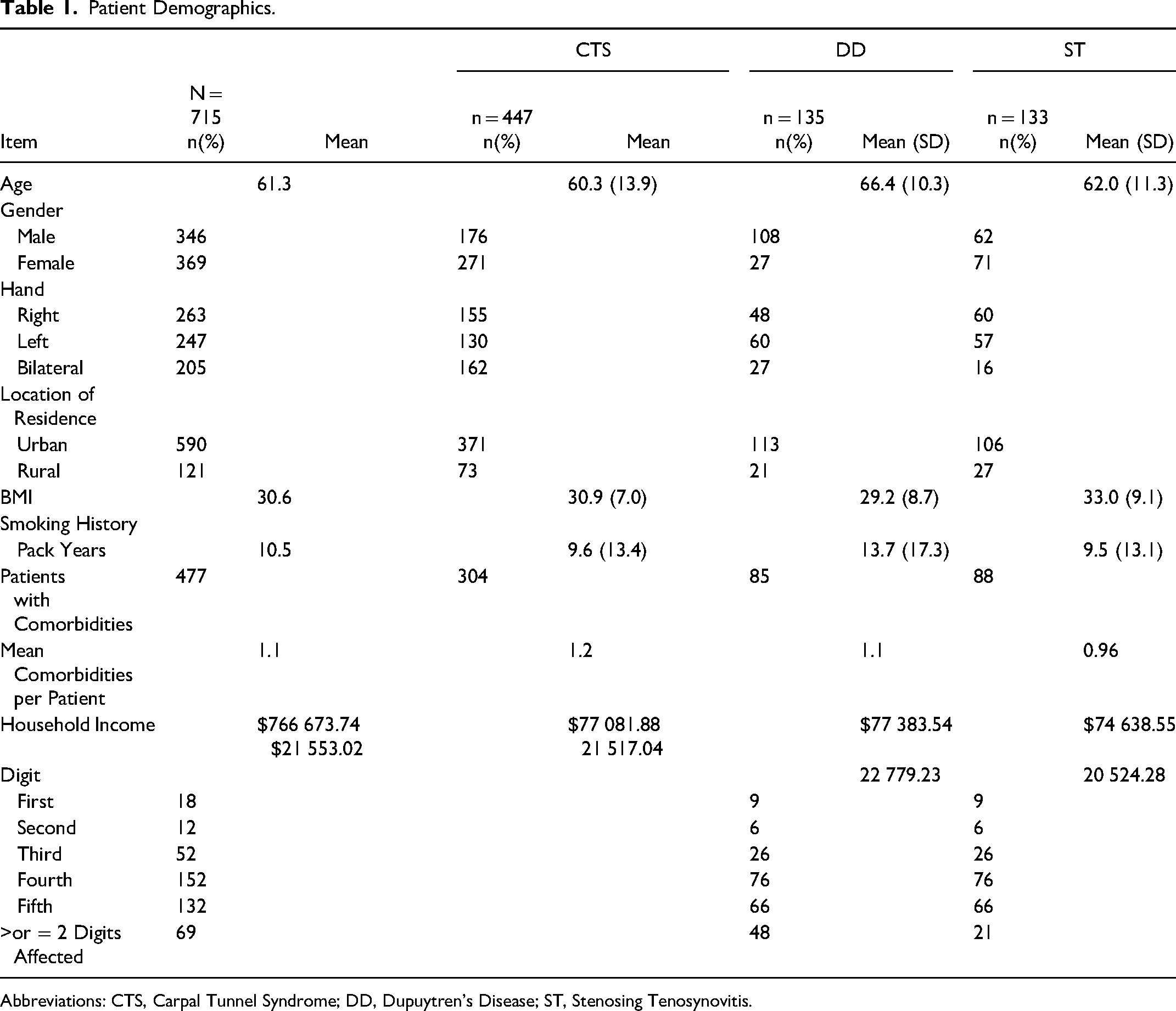
Abbreviations: CTS, Carpal Tunnel Syndrome; DD, Dupuytren's Disease; ST, Stenosing Tenosynovitis.
Case Loads
Overall, a total of 264 elective hand procedures were performed during the COVID-19 time period, compared to 451 in the pre-pandemic time period (Figure 1); a reduction of 187 surgeries (41.5%). The number of surgeries for CTS reduced the most, with 291 surgeries during the pre-pandemic time period compared to 156 performed during the pandemic (n = 135, 45.5%). The number of surgeries for stenosing tenosynovitis was reduced as well (86 surgeries pre-pandemic, compared to 47 during the pandemic (n = 39, 45.3%)). For DD, 74 surgeries were performed in the time period prior to the pandemic, compared to 61 during the pandemic, (n = 13, 17.6%).
Wait Times
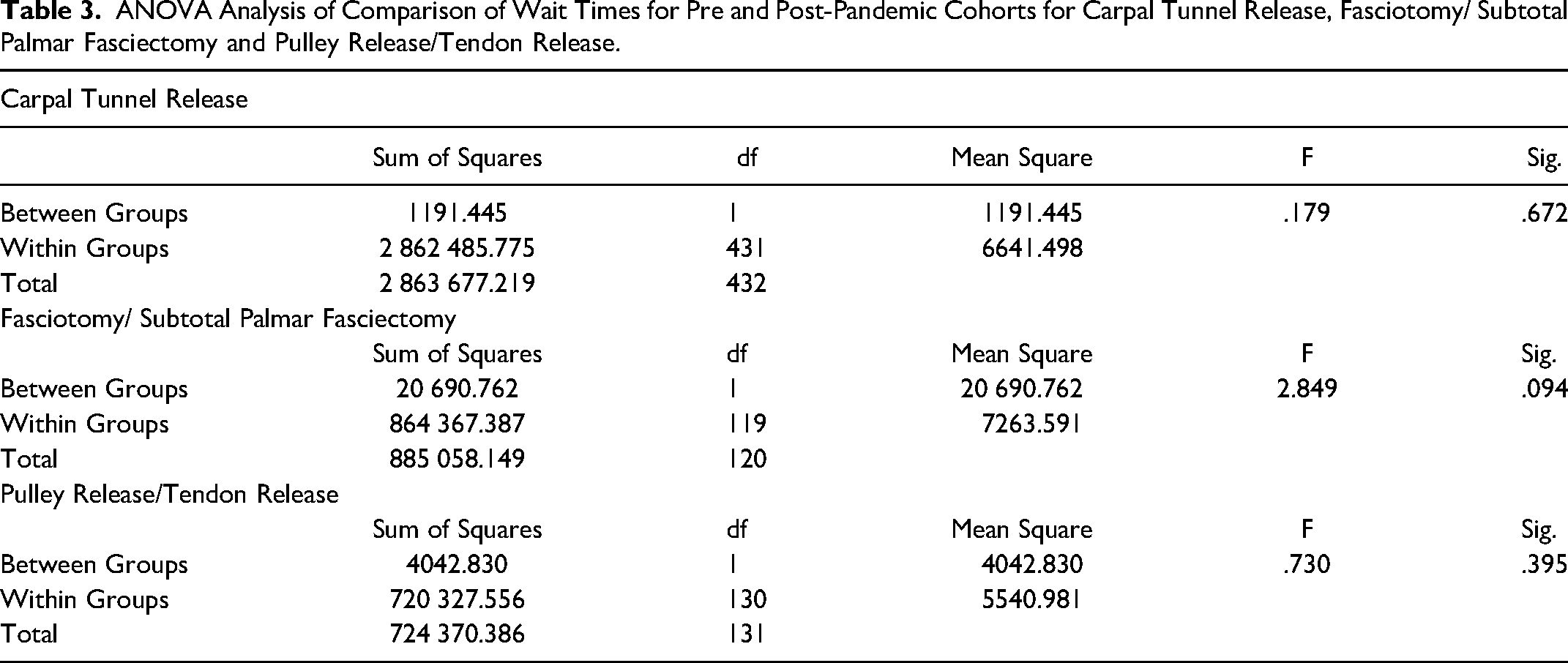
Comparisons of mean wait times for CTR, fasciotomy/ subtotal palmar fasciectomy and pulley release/tendon release are reported in Table 2. Mean wait times for CTR during the pandemic period were found to be 105.97 days (SD: 88.71), compared to the pre-pandemic time period average wait time of 109.43 (SD: 77.15). For fasciotomy/subtotal palmar fasciectomy, the average wait time for the pandemic period was 105.72 (SD: 92.58), compared to the pre-pandemic average wait time of 132.07 (SD: 79.05). The average wait time for pulley release/tendon release during the COVID-19 pandemic was found to be 95.51 (SD: 92.07), compared to the average wait time period prior to the pandemic, of 83.95 (SD: 62.71). None of these were found to be statistically significant. See Table 3 for an ANOVA analysis of comparison of wait times for each group.
Comparison of Wait Times for Carpal Tunnel Release, Fasciotomy/ Subtotal Palmar Fasciectomy and Pulley Release/Tendon Release.

ANOVA Analysis of Comparison of Wait Times for Pre and Post-Pandemic Cohorts for Carpal Tunnel Release, Fasciotomy/ Subtotal Palmar Fasciectomy and Pulley Release/Tendon Release.
Cumulative percentages achieving wait-time targets for each surgery group are presented in Table 4. For CTR, 84.1% of patients underwent surgery before the cut-off in the pre-pandemic period compared with 78.1% of patients in the pandemic period. For fasciotomy/subtotal palmar fasciectomy, 75.0% of patients underwent surgery in the pre-pandemic period compared with 81.1% of patients in the pandemic period. For pulley release/ tendon release, 92.9% of patients underwent surgery before the cut-off in the pre-pandemic period compared to 83.0% of patients in the pandemic period.
Cumulative Percentages Achieving Wait-Time Targets Determined by Ontario Health.

Predictors for Surgery
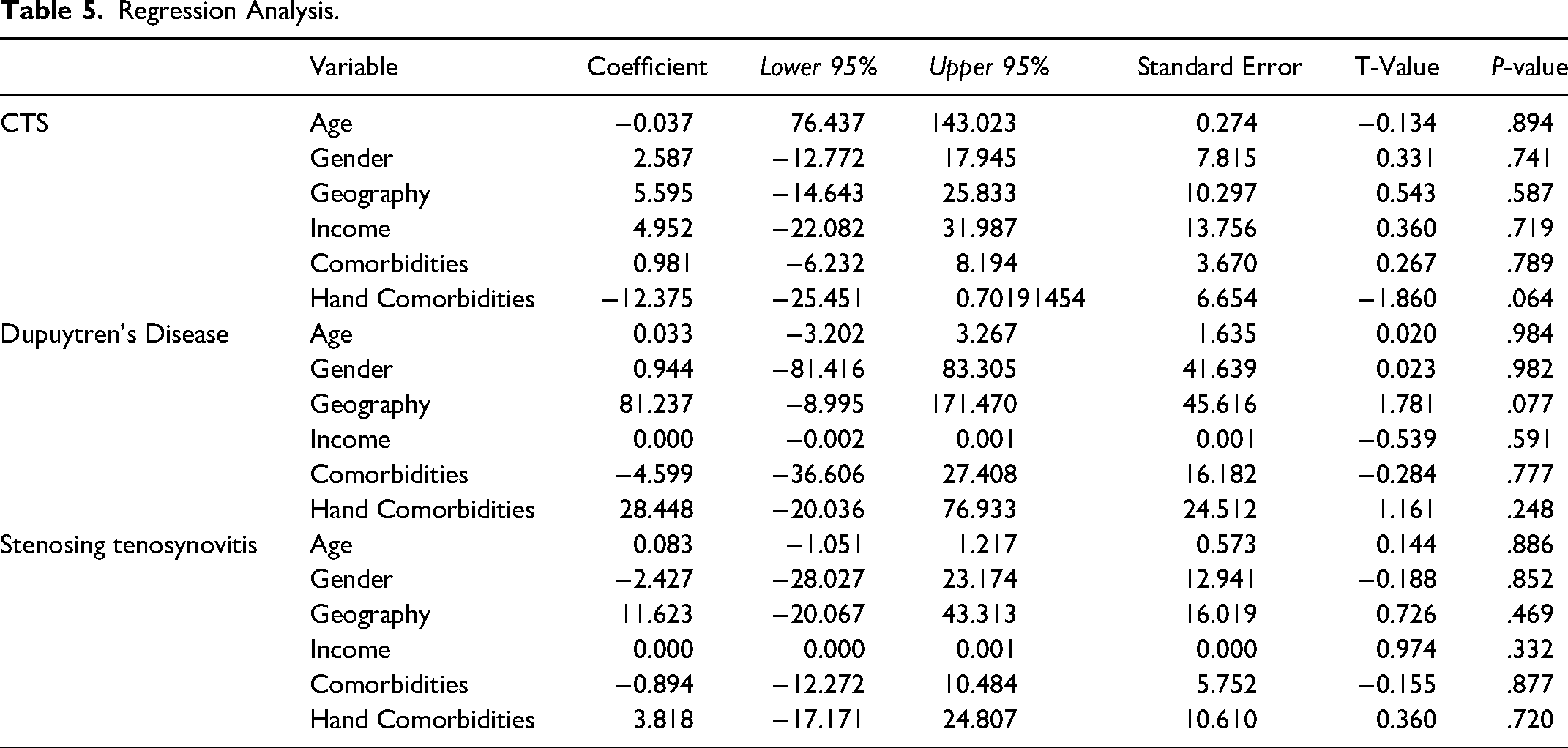
Univariate regression analysis showed that age, gender, geography (urban vs rural), income, comorbidities or hand comorbidities were not significant predictors for wait times (See Table 5).
Regression Analysis.
Discussion
After the onset of the COVID-19 pandemic, both the United States and Canada implemented policies to limit elective surgical procedures with the aim to free up resources to aid in the care of patients with COVID-19.4,5,7 This study found that in the 16 months after the COVID-19 pandemic was declared, the total number of elective hand surgeries performed reduced by 41.5% compared to the corresponding time period prior to the pandemic. For CTS and stenosing tenosynovitis, the cumulative percentages achieving wait-time targets went down during the 16 months following the start of the pandemic, when compared to the corresponding pre-pandemic time period.
The impact that the pandemic had on the number of surgeries performed was similar to previously published studies.2,35,36 However, it should be noted that previous studies have evaluated the impact of the pandemic on numbers of surgeries performed in the main operating room environment.2,35,36 The surgical procedure volume evaluated in this study also takes place in minor procedure rooms (CTS and Stenosing Tenosynovitis). A study by Saggaf et al 36 evaluating the impact of the pandemic on plastic and reconstructive surgery in Ontario found a 43% decrease in surgical case volume during the pandemic period compared to the pre-pandemic baseline. The 43% average decrease in all plastic and reconstructive surgical cases is consistent to the 41.5% decrease of elective hand surgery found in this study.
The COVID-19 pandemic has impacted the quantity of surgeries performed in North America. A study by Mattingly et al 2 found that the quantity of surgeries performed in the United States decreased by 48% during the initial shut down period. 2 Although details were not included specific to hand surgery, the authors did include a surgical category of musculoskeletal (MSK) procedures and found that the number of MSK procedures reduced by 64%. 2 Interestingly, Mattingly et al 2 found that after the initial shut down period, surgical procedure numbers quickly increased back to baseline 2019 levels throughout the rest of 2020. In contrast, the findings of this study show intermittent decreased volume of elective hand surgeries performed throughout 2020 and 2021 (see Figures 2 and 3). It should be noted, however, that the Mattingly et al 2 study included all surgical procedures, and was not limited to only elective surgical procedures.
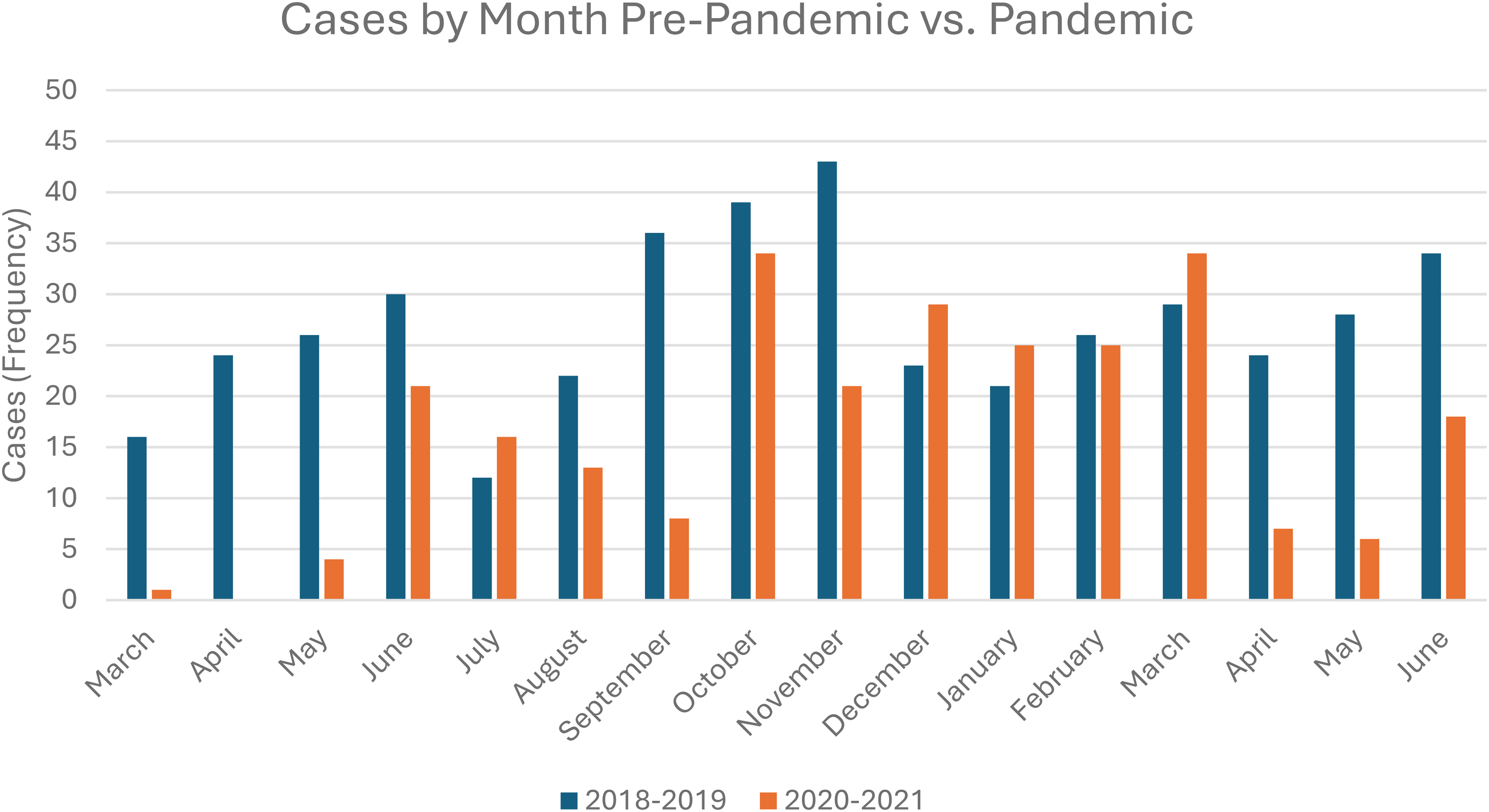
Elective hand surgical cases per month 2018-2019 versus 2020-2021.
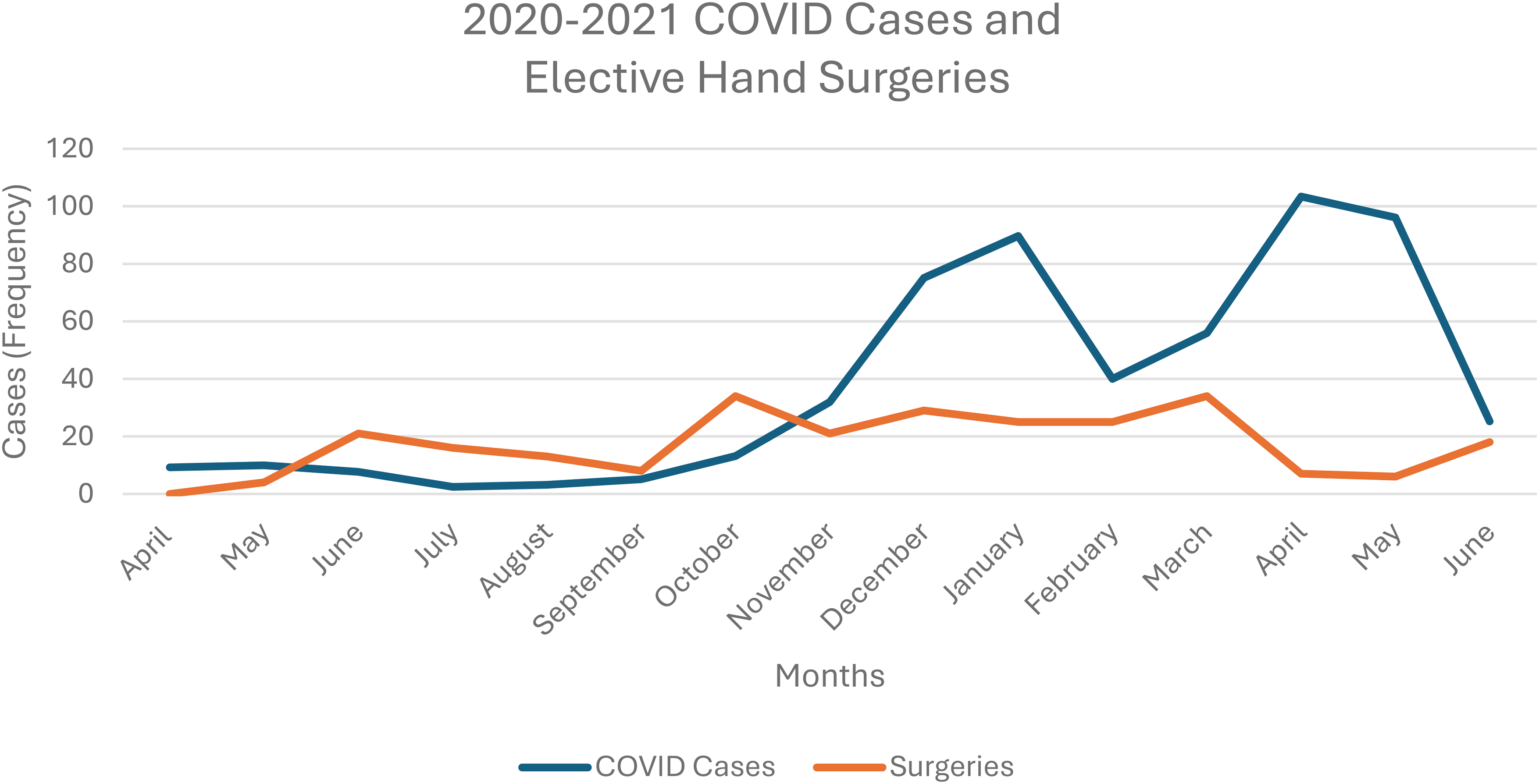
2020-2021 COVID cases and elective hand surgeries.
Decreased surgical volume can lead to an increase in backlog of surgical procedures. 7 A Canadian study published by Wang et al 7 in 2020 found a total estimated backlog of 148 364 surgeries in Canada for the time period between March 15 to June 13, 2020. The authors 7 estimated that the time to clear the backlog would be 84 weeks. It was estimated that during this period, an average of 719 operating room hours must be dedicated per week in each province to clear the backlog. 7
The decreased surgical case volume during the pandemic, without a significant increase in measured wait times can be explained by fewer patients being seen in consultation for issues pertaining to CTS, DD or stenosing tenosynovitis during the pandemic. This could lead to higher wait times for Wait 1 (the time period between the date the referral request is sent by the family physician and later received by the specialist's office 24 ) which was not measured in this study. For patients with hand conditions such as CTS, DD or stenosing tenosynovitis, increased wait times can lead to continued symptoms of pain and decreased hand function.11–13 This can have an impact on the quality of life for patients with these hand conditions.11–13 Furthermore, delayed surgery can lead to adverse outcomes for patients.37,38 As described by the ACS, elective surgeries have varying degrees of urgency. 5 To assist in the surgical decision making process, the ACS statement includes an elective surgery acuity scale from St. Louis University. 5 Each surgical specialty also has guidelines that are specialty-specific to help in the prioritization of elective surgical procedures. 5 The prioritization of cases can impact and improve the overall quality of life for patients.
Limitations
The findings of this study must be interpreted in the context of the retrospective study design, a limitation of the study. In most cases, wait time data was not available. However, this study was also limited by potential confounding factors. For example, data may not be available in the health record of a patient that asked to delay surgery for personal reasons. However, the large sample size mitigates the confounding effect. It should be noted that sample size was limited for the surgical management of DD and stenosing tenosynovitis when evaluated independently. Statistical significance (P < .05) of results was not achieved.
Conclusion
To mitigate the backlog of elective surgical procedures, potential solutions have been proposed, such as centralized wait list systems, and optimizing operating room (OR) time to improve efficiencies and increase effective capacity.7,39,40 Several strategies have been shown to increase OR efficiency, such as standardized OR practices, decreased OR turnover time, and case duration estimation accuracy.7,41 Healthcare institutions could increase average OR and minor procedure room (MPR) operating time per week to reduce the backlog of surgical cases.7,41 Other creative solutions could be evaluated, such as increasing the healthcare workforce and investing in healthcare infrastructure to increase OR and MPR capacity.7,30,41 An argument against the investment of additional healthcare resources includes the costs associated in an already economically-stretched healthcare system.42–44 A cost-benefit analysis should be performed in the future to determine the costs associated with prolonged wait times of elective surgeries. Efforts made to reduce wait times could lead to decreased healthcare spending by mitigating costs associated with longer wait times for both healthcare institutions and patients.
Supplemental Material
sj-docx-1-psg-10.1177_22925503241276544 - Supplemental material for The Impact of the COVID-19 Pandemic on Case Volume and Wait Times of Elective Hand Procedures: A Retrospective Chart Review Study
Supplemental material, sj-docx-1-psg-10.1177_22925503241276544 for The Impact of the COVID-19 Pandemic on Case Volume and Wait Times of Elective Hand Procedures: A Retrospective Chart Review Study by Kathryn Uhlman, MD, MBA, Isabella Churchill, MSc, Robert Dydynsky, BSc, Stepfanie Johnston, MD, Cameron Leveille, MD, Mark McRae, MD, MSc, and Matthew McRae, MD, MHS in Plastic Surgery
Footnotes
Author Contributions
All authors verify that they have made substantial contributions to: 1) conception and design, acquisition of data, or analysis and interpretation of data; 2) drafting the article or revising it critically for important intellectual content; 3) final approval of the version to be published; 4) agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Data Availability
Accessibility of supplemental information such as the study protocol, raw data, or programming code is available upon request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Hamilton Integrated Research Ethics Board Approval Project ID: 2021-14107-C. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Informed Consent
This was a retrospective review study and therefore, informed consent was not obtained.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
