Abstract
Introduction:
Social networking sites (SNSs) are increasingly used as sources of health and medicine-related information, offering accessible communication but raising concerns about misinformation and its impact on medication-related behaviors. This study examined public views, patterns of use, and factors associated with using SNSs for medicine-related information in Saudi Arabia, as well as the perceived impact on medication-related decisions.
Methods:
A cross-sectional study was conducted among adults aged ≥18 years residing in Saudi Arabia who used at least one SNS. An online self-administered questionnaire was distributed via multiple social media platforms using a secure web-based survey (QuestionPro). Data were analyzed using SPSS version 29. Bivariate and multivariate analyses were conducted, with statistical significance set at
Results:
Of 651 participants, 60.2% used SNSs to seek medicine-related information. YouTube was the most commonly used platform, followed by X (formerly Twitter) and Instagram. Commonly searched topics included medication side effects, long-term effects, and mechanisms of action. Nearly one quarter reported altering or discontinuing medications, 25.0% initiated treatments based on SNS information, and 14.5% experienced adverse effects. Higher SNS use was associated with residence outside the Eastern Province, whereas retired participants and those using prescription or over-the-counter medications were less likely to rely on SNSs.
Conclusions:
SNSs are widely used by the Saudi public for medicine-related information and significantly influence medication-related behaviors. Despite their convenience, these platforms pose risks related to misinformation. Greater involvement of healthcare professionals, particularly pharmacists, is needed to provide evidence-based medication information and enhance medication literacy and patient safety.
Keywords
Introduction
Social networking sites (SNSs) are internet-based communication technologies that enable the exchange of information, ideas, and messages through virtual communities and networks. 1 SNSs facilitate user interaction, including the sharing of multimedia content, personal experiences, and social engagement across geographic boundaries. Globally, social media adoption has increased rapidly over the past decade, with more than 5.6 billion social media user identities worldwide in 2025, representing over two-thirds of the global population and continuing to grow annually. 2
Saudi Arabia has experienced a similar increase in digital connectivity and SNSs use. Recent digital reports indicate that nearly 99.6% of the Saudi population are active social media users, with more than 34 million social media accounts reported in early 2025.3,4 Social media platforms such as WhatsApp, Snapchat, YouTube, and Instagram are widely used for communication, networking, and content sharing within the Kingdom.3,4
SNSs initially emerged as tools for social interaction, reconnecting with family and friends, and discovering new contacts worldwide. 1 Over time, these platforms have evolved into powerful communication tools that enable real-time interaction and the dissemination of information to millions of users simultaneously. 1 SNSs continue to expand with the introduction of new applications, such as TikTok and Clubhouse, alongside established platforms including Twitter (X), Instagram, Snapchat, Facebook, WhatsApp, and YouTube, reflecting their dynamic and evolving nature. 2
In recent years, SNSs have increasingly served as sources of health- and medicine-related information due to their accessibility, convenience, interactivity, and low cost. 5 Individuals with chronic conditions often form online groups or follow dedicated pages to share experiences and advice in supportive environments. 6 Healthcare professionals (HCPs) also use SNSs to disseminate health- and medicine-related information through educational posts, images, and videos that can be accessed at any time. 5 However, reliance on social media for health information may increase exposure to inaccurate, misleading, or unverified content, potentially leading to inappropriate medication use and adverse health outcomes. 7
During the COVID-19 pandemic, SNSs played a central role in disseminating public health updates, vaccine information, and coping strategies. 8 The pandemic accelerated social media engagement across different demographic groups, including older adults, who became more active users and contributors of online content. 9 Social media platforms were widely perceived as accessible sources of timely health information during this period, highlighting their potential to support patient-centered and affordable healthcare delivery.8,10
Previous studies in Saudi Arabia have reported substantial use of the internet and social media for obtaining health-related information, while also highlighting concerns regarding information reliability and its potential consequences. A study by Sumayyia et al. found that patients and their companions commonly encountered health information on social media platforms, and many perceived it as useful; however, participants expressed varying levels of trust in its accuracy and emphasized the need for verification by healthcare professionals. 11 The study also found that social media influenced health-related perceptions and decisions, underscoring its growing role in patient information-seeking.
Similarly, AlMuammar et al. demonstrated that a considerable proportion of the Saudi population relied on the internet and social media as sources of health information. 12 While participants reported benefits such as improved awareness and understanding of health conditions, the study also identified negative consequences, including confusion, anxiety, and misinterpretation of medical information. Importantly, many respondents indicated that information obtained online influenced their health-related decisions, sometimes without consulting healthcare professionals, highlighting the potential risks associated with unregulated health and medicine-related content on social media. 12
These findings suggest that the Saudi population is highly motivated to seek health-related information online, often to gain reassurance, learn from others’ experiences, and manage uncertainty. However, reliance on non-professional sources may increase the risk of misinformation dissemination, which can contribute to irrational medicine use, adverse drug reactions and interactions, therapeutic failure, disease progression, and poor health outcomes. 7 These concerns highlight the importance of understanding how SNS use influences medicine-related decision-making and the extent to which such platforms contribute to behavioral changes.
The increasing reliance on SNSs for medicine-related information can be interpreted within the broader framework of eHealth literacy and medication literacy. eHealth literacy refers to individuals’ ability to seek, understand, appraise, and apply health information obtained from electronic sources to make appropriate health decisions. 13 Similarly, medication literacy encompasses the knowledge and skills required to safely use medicines, including understanding dosing, risks, and therapeutic outcomes. 14 Variations in these competencies may influence how individuals interpret medicine-related information encountered on SNSs and whether they apply such information to modify medication use. Anchoring the present study within this conceptual framework provides a theoretical basis for examining the relationship between SNS use and medication-related behaviors.
To date, no study in Saudi Arabia has comprehensively examined the proportion, frequency, platforms used, types of medicine-specific information sought, and the behavioral impact (including medication initiation, discontinuation, and adverse effects) associated with SNS use. Existing Saudi studies have primarily focused on general health information-seeking behaviors, perceived usefulness, or trust in online sources, without detailed assessment of medicine-specific content or its direct influence on medication-related decisions.
Accordingly, the primary objective of this study was to assess the prevalence, patterns, and frequency of SNS use for obtaining medicine-related information among adults in Saudi Arabia. Secondary objectives were to (1) examine the types of medicine-related information sought, (2) evaluate the perceived reliability and usefulness of SNS-derived information, (3) assess the behavioral impact of SNS use on medication initiation, discontinuation, and adverse effects, and (4) identify sociodemographic factors associated with reliance on SNSs for medicine-related information.
Specifically, this study sought to address the following research questions:
What proportion of the Saudi public uses SNSs to obtain medicine-related information?
What types of medicine-related information are most frequently sought?
Does SNS use influence medication-related behaviors, including initiation, discontinuation, or adverse outcomes?
Which demographic or health-related characteristics are associated with SNS reliance for medicine-related information?
Material and methods
Study design
A descriptive cross-sectional study was conducted in the Kingdom of Saudi Arabia.
Study population, participant identification, and recruitment
Adults aged 18 years and above who resided in Saudi Arabia, were able to read and write in Arabic or English, and reported using at least one social media network were eligible to participate in the study. Physicians, pharmacists, and individuals who did not meet the inclusion criteria were excluded.
Data were collected between June and August 2022 through a self-administered online questionnaire hosted on QuestionPro and distributed to a convenience sample of participants via multiple social media platforms, including Facebook, Twitter, WhatsApp, Telegram, and LinkedIn. The questionnaire required approximately 5–10 min to complete.
Prior to the initiation of the study, participants were provided with a participation information sheet outlining the study objectives, the voluntary nature of participation, and assurances of data confidentiality and anonymity. Informed written consent was obtained from all participants before completing the questionnaire. No incentives or compensation were offered for participation. Ethical approval was obtained from the Institutional Review Board of Imam Abdulrahman Bin Faisal University (IRB-UGS-2022-05-199).
Study instrument
The study instrument was a semi-structured questionnaire developed in English and adapted from previously published work to meet the objectives of the current study. 15 The questionnaire comprised 29 items organized into two sections. Although described as semi-structured, the instrument primarily consisted of close-ended questions, with a limited number of open-ended items included to provide additional contextual insights. The study design remained quantitative and was not intended as a formal mixed-methods approach. The full questionnaire is provided as Supplemental File 1.
The first section consisted of 10 questions collecting participants’ sociodemographic characteristics, including age, gender, education level, occupation, and place of residence. The second section included 29 questions exploring participants’ use of social media to seek medicine-related information, including the platforms used, the types of information sought, and the reasons for use.
Most items were close-ended multiple-choice questions, allowing either single or multiple responses where applicable. Consequently, percentages for some questions may exceed 100% during analysis. An “Other” option was included where appropriate to allow participants to provide additional responses. Several items used a five-point Likert scale ranging from 1 (strongly agree) to 5 (strongly disagree) to assess participants’ agreement with statements about social media as sources of medicine-related advice.
For the purposes of this study, behavioral outcomes were defined as self-reported changes in medication-related practices following exposure to medicine-related information on social media. “Altering or stopping medications” was defined as any self-reported modification, dose adjustment, temporary interruption, or discontinuation of a prescribed or non-prescribed medication based on advice or advertisements encountered on social media platforms. “Initiating medications” referred to starting any medication, supplement, or treatment following exposure to social media content. “Experiencing adverse effects” was defined as any self-reported unpleasant or unexpected symptom that participants attributed to following medicine-related advice obtained from social media. These outcomes were measured using direct yes/no questionnaire items and, where applicable, supplemented by open-ended responses for contextual clarification.
Questionnaire validation and translation
The questionnaire underwent a systematic validation and translation process to ensure clarity, relevance, and cultural appropriateness. Content validity was established through review by three pharmacists with expertise in academia, hospital practice, and community pharmacy, who assessed the questionnaire for clarity, relevance, completeness, and suitability for the Saudi context. Minor wording refinements were discussed, and the instrument was deemed appropriate for the study objectives. A formal quantitative Content Validity Index (CVI) was not calculated, as the validation process was conducted through qualitative expert assessment and consensus. The questionnaire was pilot tested prior to the launch of the main study with five individuals from the target population who were not included in the final study sample. Feedback from the pilot testing confirmed that the questionnaire items were clear, easy to understand, and appropriately structured, and no substantial modifications were required. The pilot responses were reviewed and removed prior to data collection for the main study, and these participants were not included in the final analysis dataset.
For linguistic validation, the questionnaire was translated from English into Arabic using a parallel blind translation approach. 16 Two bilingual researchers independently translated the questionnaire into Arabic, and the resulting versions were compared and harmonized through consensus to produce a single consolidated version. An Arabic-speaking pharmacist reviewed the finalized translation to ensure linguistic accuracy and conceptual equivalence. The Arabic version was then tested with five native Arabic-speaking individuals from the target population to confirm clarity, comprehensibility, and cultural appropriateness before final deployment. The internal consistency reliability of perceptions toward social media use for medicine-related information was assessed using Cronbach’s alpha and demonstrated acceptable reliability (α = 0.70).
Sample size
The required sample size was calculated using the Raosoft online sample size calculator 17 at a 95% confidence level, a 5% margin of error, and an assumed response distribution of 50%. Considering an adult population of 34,566,328 individuals aged ≥18 years living in Saudi Arabia, 18 the minimum required sample size was estimated at 385 participants. This sample size was deemed sufficient to detect potential differences in outcomes based on participants’ characteristics. Although the minimum required sample size was 385 participants, 651 complete questionnaires were collected and included in the final analysis.
Data management and analysis
Data were analyzed using the Statistical Package for the Social Sciences (SPSS), version 29 (IBM Corp., Armonk, NY, USA). Descriptive statistics were used to summarize the data, including frequencies and percentages for categorical variables. Bivariate analysis was conducted using the Chi-square test to examine associations between participants’ sociodemographic characteristics and the use of social networking sites (SNSs) as a source of medicine-related information. Statistical significance was set at a
A multivariate logistic regression model was subsequently performed to assess the independent association between participants’ characteristics and the likelihood of using SNSs for medicine-related information. All explanatory variables were entered into the model as categorical variables. Adjusted odds ratios (AORs) with 95% confidence intervals (CIs) were calculated. Participant characteristics with a
Multicollinearity among independent variables was assessed using variance inflation factors (VIF), with values greater than 5 considered indicative of concern. Model fit was evaluated using the Hosmer–Lemeshow goodness-of-fit test and pseudo
Responses to open-ended questions were analyzed using thematic content analysis. Two researchers independently coded responses, and discrepancies were resolved through discussion. Themes were quantified to provide descriptive frequencies.
The reporting of this study conforms to the STROBE Statement guidelines for cross-sectional studies 19 (Supplemental File 2).
Results
Questionnaire response and participants’ characteristics
A total of 651 completed questionnaires were included in the analysis. Most participants were Saudi nationals (98.3%) and resided in the Eastern Province (74.3%). The majority were female (76.2%) and aged 18–24 years (46.2%). Over half of the participants reported very good general health (53.8%), held a university degree (56.2%), and were students (41.2%).
Most respondents reported prior use of prescription-only medicines (POMs; 85.1%), while 62.7% reported prior use of over-the-counter (OTC) medications. The most common conditions for which prescription medicines were used included infections (31.6%), skin conditions (23.8%), and allergies (19.4%). A detailed summary of participants’ characteristics is presented in Table 1.
Participants’ characteristics (

The percentages add up to more than 100% because participants could select multiple responses.
Use of social media for medicine-related information
Detailed distributions of platform use and frequency are presented in Table 2. WhatsApp, Instagram, and X (formerly Twitter) were the most commonly used social media platforms overall. Approximately, 60.2% of participants reported using at least one social media platform to search for medicine-related information. Among these users, YouTube was the most frequently used platform for medicine-related content, followed by X and Instagram.
Social media platforms, patterns of use, types of medicine-related information sought, and reasons for using social networking sites.
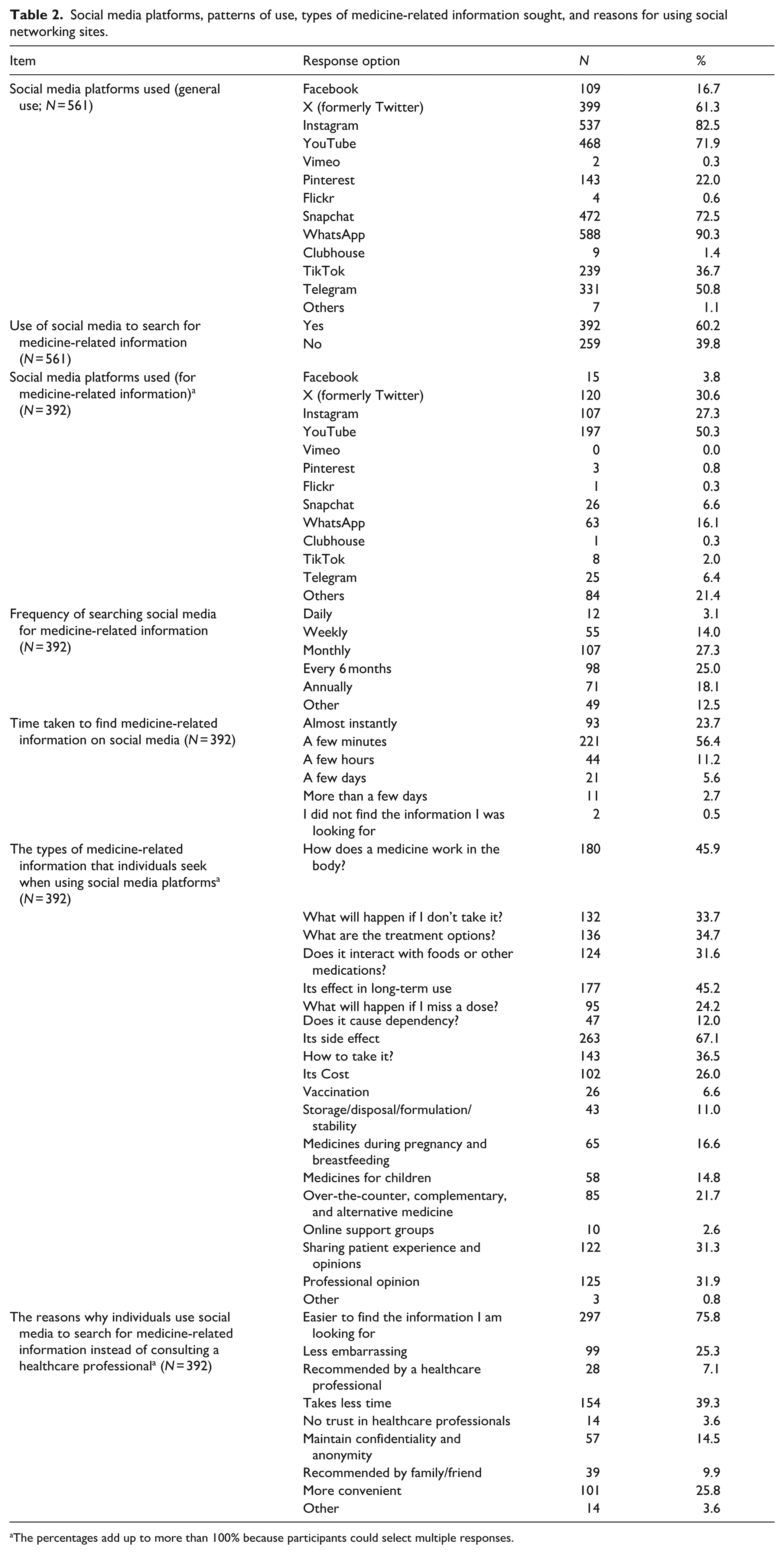
The percentages add up to more than 100% because participants could select multiple responses.
Most participants reported searching for medicine-related information monthly or semi-annually. The majority indicated that they were able to find the desired information quickly, often within minutes or almost instantly (Table 2). The most frequently searched topics were medication side effects and mechanisms of action (Table 2). Participants reported multiple reasons for using social media to search for medicine-related information instead of consulting a healthcare professional (
YouTube was also most commonly perceived as the most beneficial platform for medicine-related information (31.6%, 124/392). When asked to explain why they perceived a particular social media platform as the most beneficial source of medicine-related information (Question B11), some participants cited that healthcare professionals, including doctors and pharmacists, shared medication-related details on these platforms. Others valued the comprehensiveness and depth of the information provided, while some highlighted the usefulness of video and audio explanations. Ease and speed of access were also commonly reported, and others emphasized the information’s trustworthiness and credibility. Additional perceived benefits included learning from other users’ experiences, access to multiple viewpoints, as well as convenience and flexibility.
Impact of social media on medication-related behavior
Among participants who used SNSs for medicine-related information, 65.1% reported sometimes discussing the information they found online with a healthcare professional, while 14.8% reported never doing so. Among participants who discussed medicine-related information obtained from SNSs with a healthcare professional (
Behavioral outcomes and decision-making related to medicine-related information obtained from social networking sites.

The percentages add up to more than 100% because participants could select multiple responses.
Approximately half of the participants were unaware of the original sources of the information encountered on SNSs (Table 3). Among those who reported being aware of the information sources and provided further details in Question B21, the most frequently cited sources were official governmental health authorities, particularly the Saudi Ministry of Health (MOH) and the Saudi Food and Drug Authority (SFDA). Participants also reported professional and charitable health organizations, such as the Saudi Heart Association, the Saudi Charitable Association of Diabetes, and the Saudi Initiative for Asthma, as sources of medicine-related information. A smaller proportion referred to verified social media accounts of healthcare professionals, including physicians and pharmacists.
Notably, 23.2% of SNS users reported altering or stopping medication use based on advice or advertisements encountered on social media (Table 3). Analysis of responses to Question B25 indicated that participants reported a wide range of medicines that were started, altered, or discontinued following such advice. These medicines included over-the-counter products, such as analgesics, vitamins, and dietary supplements, as well as herbal and complementary remedies. Participants also reported medicines commonly used for chronic conditions or acute symptoms, including treatments related to gastrointestinal, dermatological, respiratory, or metabolic conditions.
In comparison, 25.0% of participants reported starting a medication or treatment after receiving advice or seeing advertisements on social media. Responses to Question B27 revealed that medication initiation similarly involved a variety of products, predominantly over-the-counter medicines, dietary supplements, skincare treatments, and herbal remedies. Some participants also reported initiating medicines used for managing acute symptoms or chronic conditions. Several responses indicated the initiation of multiple medicines, suggesting a repeated or cumulative effect of social media advice on medication-related decisions.
Additionally, 14.5% of participants reported experiencing unpleasant or unexpected side effects after following advice obtained from social media (Table 3). Analysis of open-ended responses to Question B23 revealed a range of adverse experiences, including gastrointestinal disturbances, dizziness, headaches, fatigue, and skin reactions, as well as allergic manifestations such as itching, rashes, and swelling. These reactions were particularly reported following the use of supplements, herbal products, or other treatments promoted online. Some participants also described worsening of existing conditions or the emergence of new symptoms, which they attributed to the lack of individualized medical assessment and consideration of personal health history.
Among participants who did not use SNSs for medicine-related information, the most commonly reported reasons included a preference for consulting healthcare professionals (97.7%) and lack of trust in social media content (88.8%), Table 3. Overall, 77.3% of all participants indicated that they would be willing to use a social media page maintained by healthcare professionals for medicine-related information (Table 3).
Participants’ confidence in, and application of, medicine-related information obtained from social media
Figure 1 illustrates participants’ agreement with statements related to the reliability, usefulness, accessibility, and confidentiality of medicine-related information obtained from social media. For interpretative clarity, Likert-scale responses were collapsed into three categories (agree/strongly agree, neutral, disagree/strongly disagree). A substantial majority of participants agreed that medicine-related information obtained from social media was useful (79.5%), easy to access (77.6%), and free (87.6%). Agreement regarding confidentiality was also high (68.0%). However, uncertainty remained regarding practical application, as 55.9% of participants were neutral or disagreed that they felt confident applying the information to their personal situation. Additionally, 53.0% were neutral or disagreed with the statement that they would recommend using social media for medicine-related information.

Participants’ agreement with statements regarding the reliability, usefulness, accessibility, confidentiality, and applicability of medicine-related information obtained from social media.
Factors associated with the use of social media for medicine-related information
Bivariate chi-square analysis demonstrated statistically significant associations between the use of social networking sites (SNSs) for medicine-related information and province of residence (
Participant characteristics associated with the use of social media for medicine-related information (Chi-square test).

df: degrees of freedom;
In the multivariate logistic regression analysis, the overall model was statistically significant (Omnibus χ2 = 40.040, df = 9,
Participants residing in provinces other than the Eastern Province had 67% higher odds of using social media for medicine-related information compared to those in other Provinces (AOR = 1.67, 95%CI: 1.17–2.39,
Multivariate analysis of participant characteristics associated with the use of social media for medicine-related information.
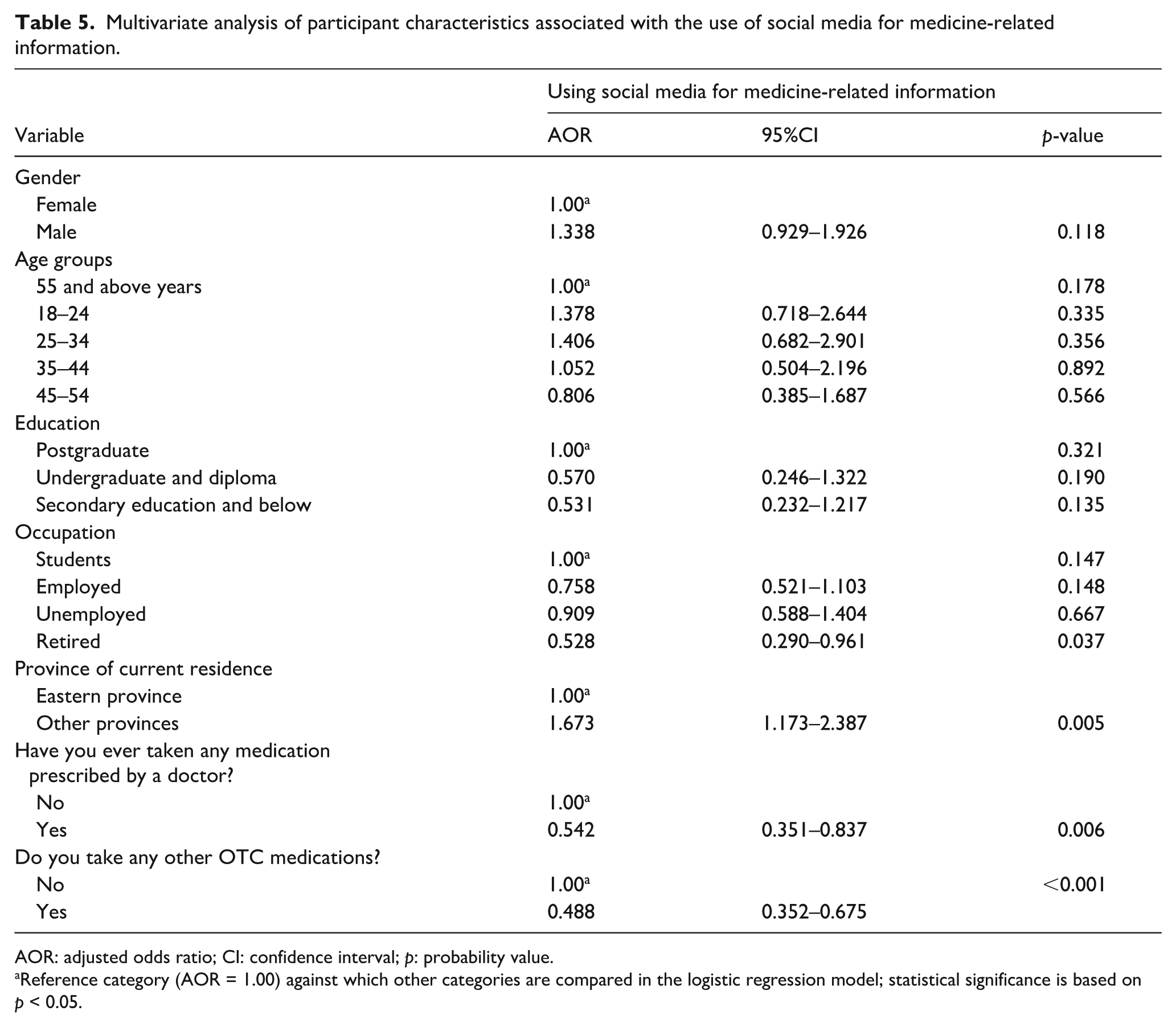
AOR: adjusted odds ratio; CI: confidence interval;
Reference category (AOR = 1.00) against which other categories are compared in the logistic regression model; statistical significance is based on
Discussion
This study provides a comprehensive assessment of public use of social networking sites (SNSs) for medicine-related information in Saudi Arabia and highlights both the opportunities and risks associated with this growing phenomenon. The findings demonstrate that SNSs are widely used for seeking medication-related information, with approximately 60% of participants reporting reliance on at least one social media platform. This prevalence reflects the rapid expansion of digital connectivity and social media penetration in Saudi Arabia, where social network sites have become integral to everyday information-seeking behaviors, with nearly universal internet access and social media use reaching more than 99% of the population.3,4
The observed level of SNSs use for medicine-related information is consistent with prior studies conducted in Saudi Arabia and internationally, which report increasing reliance on online platforms for health-related knowledge.11,12,20 However, unlike earlier work that focused primarily on general health information,11–13,20–22 the present study provides novel insights into medicine-specific information-seeking behaviors, addressing a critical gap in the literature. These findings can be interpreted within the framework of eHealth and medication literacy, as individuals’ ability to critically appraise online information may influence whether SNS-derived content leads to safe decision-making or inappropriate medication modification.13,14
YouTube emerged as the most commonly used and most highly valued platform for medicine-related information. Participants highlighted the advantages of audiovisual content, including clarity, depth of explanation, and ease of understanding. This finding may reflect the perceived advantages of audiovisual content, such as improved clarity and ease of understanding reported in previous studies.5,23 Nevertheless, the reliance on YouTube also raises concerns, as studies have repeatedly demonstrated substantial variability in the quality, accuracy, and balance of medication-related content available on this platform. 24
The types of medicine-related information most frequently sought—such as side effects, long-term effects, and mechanisms of action—underscore persistent gaps in patient counseling and medication education. These information needs are consistent with findings from international studies, which suggest that patients often feel inadequately informed about medication risks during clinical encounters and subsequently seek clarification online. 15 While such proactive information-seeking may reflect patient engagement, it also exposes individuals to misinformation and non-contextualized advice.
Importantly, this study demonstrates that SNS use is not limited to passive information-seeking but is associated with observable medication-related behavioral changes. In our sample, 23.2% of participants reported altering or discontinuing prescribed medications, and 25.0% reported initiating treatments based on advice encountered on social media. These proportions are consistent with findings from previous research conducted in Saudi Arabia and internationally, where exposure to online health information has been associated with self-medication, changes in prescribed therapy, and increased use of supplements or alternative remedies.12,25 While earlier studies primarily examined general health decision-making, the present findings extend this evidence to medicine-specific behaviors, which carry direct implications for patient safety.
Compared with prior Saudi research exploring general online health information–seeking behaviors,12,26 the proportion of participants in the present study reporting medication modification appears notably high. This may reflect the medicine-specific focus of our questionnaire, the increasing normalization of self-directed health decision-making in digital environments, or growing trust in peer-shared experiences and influencer-driven content. 26 The diversity of products initiated or discontinued, including prescription medicines, over-the-counter products, and herbal remedies, suggests that social media exposure may influence both acute and chronic therapy decisions.
Notably, 14.5% of participants reported experiencing adverse effects after following social media advice. While this proportion may indicate a potential safety concern associated with exposure to online medicine-related information, the finding should be interpreted with caution. The cross-sectional design cannot establish causal inference, and the reported outcomes represent self-perceived temporal associations rather than clinically confirmed adverse drug reactions. Participants may have retrospectively attributed symptoms to social media–derived advice, introducing attribution and recall bias, while underlying health conditions, concurrent medication use, or inappropriate self-medication practices unrelated to SNS exposure may also have contributed to these events. Nevertheless, the observed rate remains clinically relevant and aligns with existing literature suggesting that unverified digital health content may contribute to medication errors, inappropriate dosing, drug interactions, and adverse outcomes.7,27 Although most users did not report harm, even a modest proportion experiencing potential adverse effects represents an important public health concern given the widespread use of social media platforms in Saudi Arabia. Collectively, these findings underscore the need for strengthened digital health governance and proactive involvement of healthcare professionals to mitigate risks associated with medicine-related misinformation, while warranting further longitudinal investigation to clarify causal relationships. Despite these risks, SNSs were not used in isolation. A substantial proportion of participants reported discussing online medication information with healthcare professionals, and over half indicated that providers sometimes agreed with the information found online. This suggests that SNSs may function as a supplementary information source rather than a complete substitute for professional advice, as observed in previous studies. 15 However, the high proportion of healthcare professional disagreement further highlights the inconsistency and questionable reliability of social media content.
The multivariate analysis revealed that participants residing outside the Eastern Province were more likely to use SNSs for medicine-related information, potentially reflecting regional differences in healthcare access, service availability, or continuity of care. In contrast, participants who reported using prescription or OTC medications demonstrated substantially lower odds of relying on SNSs for medicine-related information. This finding may reflect greater engagement with healthcare professionals among medication users, as ongoing treatment often involves regular clinical consultations that reduce unmet informational needs. Individuals actively using medications may also possess heightened awareness of medication-related risks, including adverse effects and drug interactions, which may encourage reliance on professionally validated sources rather than user-generated online content. Alternatively, SNS use may primarily serve individuals without ongoing therapeutic management who seek preliminary or exploratory medication information prior to consulting healthcare professionals.
Similarly, retired participants were significantly less likely to use SNSs, consistent with evidence of digital disparities and lower online engagement among older adults. 9 Collectively, these moderate effect sizes highlight meaningful differences in information-seeking behaviors across geographic, clinical, and demographic groups, with important implications for targeted digital health education strategies.
These findings highlight a complex relationship between SNSs use, medication literacy, and healthcare engagement. While SNSs offer accessible and convenient avenues for medication information, they also introduce substantial risks related to misinformation, inappropriate medication use, and adverse outcomes. Encouragingly, the strong willingness of participants to use healthcare professional–managed SNS pages indicates a clear opportunity to use these platforms for safe, evidence-based medication education.
Implications for practice and policy
Given the descriptive cross-sectional design of this study, the following implications should be interpreted as hypothesis-generating rather than prescriptive policy recommendations. The findings have important implications for healthcare practice in Saudi Arabia. Pharmacists and other healthcare professionals should routinely inquire about patients’ use of SNSs for medication-related information and address misinformation proactively during consultations. Creating a non-judgmental environment may encourage patients to disclose online information sources and facilitate corrective counseling.
Pharmacists may represent a promising group to lead future digital medication education initiatives; however, the effectiveness of such approaches should be examined through controlled or intervention-based studies. Previous research supports the role of pharmacists as trusted sources of medication information, both offline and online. 28 The high public willingness to engage with healthcare professional–managed social media pages suggests that pharmacist-led SNS accounts may have the potential to improve medication literacy, counter misinformation, and promote rational medicine use, pending evaluation through implementation research.
From a policy perspective, while causal inferences cannot be drawn from this descriptive study, the findings highlight areas that may warrant consideration in future intervention or policy research. Regulatory authorities such as the Saudi Ministry of Health and the Saudi Food and Drug Authority may explore the potential value of developing national frameworks or guidance governing medicine-related content on social media. Any such approaches should be evaluated through implementation and impact studies prior to large-scale adoption. Policies supporting verified healthcare professional accounts, monitoring misleading medication advertisements, and collaboration with SNS platforms could be investigated as potential strategies to enhance public safety and trust in digital health communication.
Strengths and limitations
This study has several strengths, including a large sample size, representation from multiple regions, and a rigorously validated bilingual questionnaire. The use of both bivariate and multivariate analyses strengthens the robustness of the findings by identifying independent predictors of SNSs use for medicine-related information.
However, the study has limitations. The cross-sectional design limits causal inference. Self-reported data are subject to recall and social desirability bias, and individuals with higher SNS engagement may have been more likely to participate. In addition, the use of convenience sampling via social media platforms may have led to the overrepresentation of younger, digitally engaged, and female participants. Given that 76.2% of respondents were female and nearly half were aged 18–24 years, the findings may not be fully generalizable to older adults or individuals with lower levels of digital engagement. Because the study employed a non-probability sampling strategy without a defined sampling frame, post-stratification weighting was not performed, as it would not eliminate underlying selection bias. Therefore, the results should be interpreted as representative of socially connected and digitally active adults rather than the entire Saudi population. This demographic distribution also reflects potential demographic skewness within the study sample, including a higher representation of participants from the Eastern Province, which may be attributable to differential social media engagement patterns and online survey participation across regions and population groups.
Moreover, the study did not objectively assess the accuracy of information accessed on SNSs, focusing instead on participant perceptions and behaviors. As participation was voluntary and recruitment occurred through social networking platforms, self-selection bias may have occurred, whereby individuals with greater interest in medicine-related information or higher digital literacy were more likely to participate, potentially overrepresenting active online health information seekers.
Furthermore, although internal consistency was assessed, formal construct validation and test–retest reliability were not performed. Also, the study did not conduct subgroup analyses by medication type, chronic disease status, or age group; therefore, potential differential patterns of medication alteration or initiation across clinical subgroups could not be examined. Thus, future studies should conduct stratified or longitudinal analyses to better understand differential risk patterns. In addition, recruitment through shared social media networks introduces the possibility of clustering effects, whereby participants connected through similar online communities may share comparable demographic characteristics, health literacy levels, or information-seeking behaviors. Because recruitment chains and network structures were not identifiable, potential intra-network correlations could not be formally evaluated.
Finally, although the sample size calculation was based on assumptions of simple random sampling, recruitment was conducted using a non-probability convenience sampling strategy. Therefore, the calculated margin of error and confidence level should be interpreted as indicative of sample size adequacy rather than strictly representative population parameters. Additionally, although participants reported exposure to medicine-related information on SNSs, the study did not independently verify the accuracy or quality of the online content encountered. Accordingly, findings reflect perceived exposure and self-reported behavioral responses rather than objective assessment of information validity.
Suggestions for future research
Future research should employ longitudinal designs to explore causal relationships between SNSs use and medication-related outcomes. Qualitative studies could provide deeper insights into how individuals assess credibility and apply online medication information. Intervention studies evaluating the effectiveness of pharmacist-led or institutionally managed SNS platforms are also warranted. Finally, research assessing the impact of regulatory policies and verification mechanisms on the quality of medicine-related content on SNSs would further inform evidence-based digital health strategies.
Conclusion
This study demonstrates that SNSs are widely used by the Saudi public as sources of medicine-related information and that such use significantly influences medication-related behaviors. While SNSs are valued for accessibility, convenience, and perceived usefulness, they also present substantial risks related to misinformation and inappropriate medication use. Regional and demographic differences in SNSs reliance highlight the need for targeted, context-specific interventions.
Greater involvement of healthcare professionals—particularly pharmacists—in digital health communication is urgently needed. Using SNSs as platforms to deliver accurate, evidence-based medication information is a promising strategy to enhance medication literacy and patient safety in an increasingly digital healthcare environment.
This study demonstrates that social networking sites (SNSs) are widely used by the Saudi public as sources of medicine-related information and that such use significantly influences medication-related behaviors. While SNSs offer accessibility and convenience, they also contribute to the spread of misinformation that may result in inappropriate medication use and adverse outcomes.
However, SNSs themselves also present an opportunity to combat health misinformation. When appropriately regulated and utilized, these platforms can serve as powerful tools for disseminating accurate, evidence-based medication information to large populations. Strengthening collaboration between healthcare professionals, regulatory authorities, and social media platforms is essential to improve content verification and reduce misleading medicine-related advertisements.
In addition, integrating digital health literacy education and structured training on responsible social media use within healthcare systems, universities, and community outreach programs may empower individuals to critically evaluate online medication information. Developing pharmacist- and healthcare professional–led social media initiatives, as well as incorporating social media education modules into health curricula, could further support safe medication practices in an increasingly digital environment. Incorporating SNSs into a coordinated public health strategy offers a promising pathway to enhance medication literacy, reduce misinformation-related harm, and improve patient safety in Saudi Arabia.
Supplemental Material
sj-docx-1-phj-10.1177_22799036261444088 – Supplemental material for Public views, patterns, and impacts of social networking site use for medicine-related information in Saudi Arabia: A cross-sectional study
Supplemental material, sj-docx-1-phj-10.1177_22799036261444088 for Public views, patterns, and impacts of social networking site use for medicine-related information in Saudi Arabia: A cross-sectional study by Faten Alhomoud, Farah Kais Alhomoud, Amal Al Muslim, Sarah Altheeb, Rana Al Subait, Hawra Alsadah, Bayan Alsultan, Marwah Alamer, Aymen Ali Alqurain, Basmah Alfageh and Hailah Almoghirah in Journal of Public Health Research
Supplemental Material
sj-docx-2-phj-10.1177_22799036261444088 – Supplemental material for Public views, patterns, and impacts of social networking site use for medicine-related information in Saudi Arabia: A cross-sectional study
Supplemental material, sj-docx-2-phj-10.1177_22799036261444088 for Public views, patterns, and impacts of social networking site use for medicine-related information in Saudi Arabia: A cross-sectional study by Faten Alhomoud, Farah Kais Alhomoud, Amal Al Muslim, Sarah Altheeb, Rana Al Subait, Hawra Alsadah, Bayan Alsultan, Marwah Alamer, Aymen Ali Alqurain, Basmah Alfageh and Hailah Almoghirah in Journal of Public Health Research
Footnotes
Acknowledgements
The authors would like to thank all study participants for their valuable contribution to this research.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
