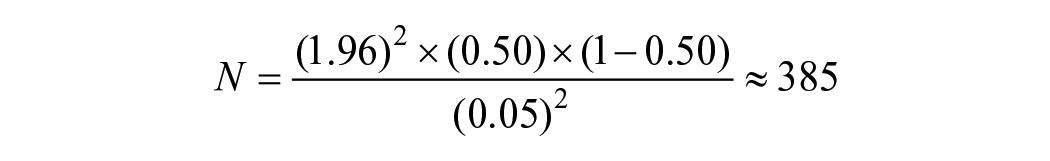Abstract
Background:
AI tools are transforming diagnosis, treatment planning, and patient care in healthcare. However, adoption in resource-limited settings like Bangladesh remains slow. Therefore, this study aims to investigate the knowledge, attitudes, and practices of registered physicians in Bangladesh regarding AI tools in medical practice, contributing to a growing but underexplored body of literature on digital health readiness in Bangladesh.
Design and methods:
A cross-sectional study was conducted over 6 months (September 2023 to February 2024), involving 398 doctors with MBBS or BDS degrees across Bangladesh. Participants were selected using a convenience sampling method. Data were collected through paper surveys, assessing knowledge, attitudes, and practices. Cronbach’s alpha for each section was above 0.70, with an overall model consistency of 0.79, indicating very good reliability. Statistical analysis was performed using Stata 17.
Results:
Among the study participants, 78.39% had poor knowledge. Attitudes were almost evenly split, with 48.74% having a negative attitude and 51.26% having a positive attitude. In terms of practice, 65.58% exhibited poor practice. In multivariate analysis, female physicians had a significantly higher likelihood of having good knowledge (AOR = 3.56, CI: 2.11–6.03, p < 0.001) and good practice (AOR = 2.89, CI: 1.73–4.83, p < 0.001) compared to male physicians.
Conclusion:
While awareness of AI tools is high among Bangladeshi physicians, actual integration into practice remains limited. The cautiously positive attitudes—especially toward AI’s educational and diagnostic potential—indicate an opportunity for targeted training and user-centered AI tool development. Strengthening AI literacy and addressing concerns such as job displacement could enhance future adoption and optimize healthcare delivery.
Introduction
Artificial intelligence (AI) technologies are transforming the way healthcare is delivered to individuals, and currently, they are revolutionizing medical practices with their quick and accurate data analysis capabilities.1,2 These technologies are enhancing disease diagnostics, treatment planning, and patient care management in faster and more precise ways. 3 GPT-based tools, known as Generative Pre-trained Transformers, are AI models that can understand and create text that resembles human writing.4,5 These tools offer promise in supporting healthcare professionals with decision-making, personalized medicine, and patient education. 6
The global research on the integration of AI in healthcare has extensively explored its benefits. A comprehensive review underscores how AI can enhance precision, predict outcomes, and tailor treatment strategies effectively in healthcare settings. 2 From analyzing images to forecasting disease outbreaks, AI applications demonstrate the versatility and Promise for enhancing healthcare delivery.7,8 As for AI tools, studies have showcased their ability to generate contextually appropriate information to aid various tasks, such as drafting reports, addressing patient inquiries, and formulating research hypotheses in the medical field.9,10 By incorporating these tools into practice, physicians can reduce burdens while enhancing communication with patients and improving healthcare outcomes.
Despite the progress made in utilizing AI in the healthcare sector, there are still obstacles to overcome. Research has highlighted challenges, such as a lack of understanding among healthcare providers, concerns about data security, and the potential disruption of clinical processes by AI technologies.11,12 These hurdles are particularly pronounced in countries like Bangladesh, where limited healthcare resources and infrastructure pose barriers, as issues such as a patient-to-physician ratio, restricted access to medical equipment, and disparities in healthcare services between urban and rural areas have been identified, which underscores the potential benefits of integrating AI tools into the healthcare system.13 –15
Comparative studies from neighboring South Asian countries offer valuable perspectives that contextualize the challenges faced in Bangladesh. For instance, a cross-sectional study in Pakistan revealed that while 91.2% of doctors had a good level of knowledge about AI in medicine, only 30.6% were actively using AI tools in practice—highlighting a gap between awareness and practical implementation. 16 Similarly, a study in India identified significant barriers such as lack of structured training, limited institutional support, and concerns over reliability, despite an overall positive attitude among physicians toward AI integration. 17 These regional parallels reinforce the urgency of tailored training and policy efforts to bridge the implementation gap in resource-limited healthcare settings.
Various studies have delved into how healthcare professionals perceive AI technologies. Findings indicate curiosity among physicians regarding AI applications, but significant concerns about its implications for clinical practice and job stability.18,19 Insufficient training and education in AI have been identified as major obstacles to its integration into medical practice. 20 These results emphasize the importance of implementing programs to improve AI understanding among healthcare providers. However, implementing such technology may face resistance from traditional physicians, potentially leading to financial losses.12,21 Therefore, understanding current knowledge, attitudes, and practices toward AI tools is crucial for early adoption.
In Bangladesh, digital health efforts have gradually expanded under the umbrella of national health sector programs and digital governance initiatives. Notable examples include the introduction of the District Health Information Software 2 (DHIS2) for real-time health data management, the National eHealth Strategy endorsed by the Ministry of Health and Family Welfare, and the rollout of telemedicine services at Upazila Health Complexes as part of the Digital Bangladesh Vision.22,23 The Directorate General of Health Services (DGHS) has also facilitated platforms such as Shastho Batayon (Health Call Center 16263) and mobile-based pregnancy tracking systems to support maternal and child health. 24 These policy-driven interventions underscore the country’s commitment to leveraging digital tools for universal health coverage. Despite this progress, the digital health ecosystem remains fragmented in terms of infrastructure, interoperability, and human resource readiness. There is no dedicated AI governance framework or ethical guideline for clinical use, and AI-specific capacity-building is not yet embedded in undergraduate or postgraduate medical curricula. These gaps suggest that while the foundation for digital health has been laid, Bangladesh remains at an early stage of AI-readiness in healthcare, particularly at the point-of-care level.
A thorough review of existing literature revealed a lack of studies examining physicians’ knowledge, attitudes, and practices regarding AI use in medical practice in Bangladesh. Given this backdrop of emerging digital health capacity but limited structured AI implementation, it becomes imperative to explore whether Bangladeshi physicians face similar or distinct challenges compared to neighboring countries. Therefore, this study aims to fill that gap by evaluating these aspects among Bangladeshi physicians, offering insights that can guide healthcare policy and AI integration efforts in Bangladesh. Specifically, the study hypothesizes that physicians with higher levels of knowledge about AI will exhibit more positive attitudes related to its clinical application.
Study materials and method
Study design and data collection methods
In Bangladesh, approximately 186,000 healthcare professionals hold MBBS and BDS degrees, and they are registered under the Bangladesh Medical and Dental Council (BMDC). 25 Through a cross-sectional study, we captured a comprehensive and representative overview of doctors’ views and behaviors regarding AI tools within a specific timeframe. The entire research lasted half a year (from September 2023 to February 2024), allowing for a dive into the current status of AI-related knowledge, attitude, and practice in medical settings, which highlights both the potential benefits and existing challenges faced by healthcare professionals in integrating these technologies into their routine clinical work.
To calculate the sample size, we employed the formula, with a standard normal deviation (z) of 1.96 for a 95% confidence interval, a proportion (s) of 50%, and a margin of error (e) of 0.05.
This calculation resulted in a minimum required sample size of 385 participants.
This study included 398 registered physicians with MBBS or BDS degrees (both male and female), selected from a pool of 414 respondents. Sixteen responses were excluded from the analysis due to incomplete or missing critical information needed for accurate assessment. This ensured that the final dataset was complete and reliable for analysis. Participants from medical and dental colleges and hospitals across the eight divisions of Bangladesh (Dhaka, Mymensingh, Chattogram, Sylhet, Rajshahi, Khulna, Rangpur, and Barisal) were selected using a convenience sampling technique. This method was chosen for its practicality and efficiency in quickly gathering a diverse sample of male and female physicians. However, we acknowledge that convenience sampling may limit the generalizability of our findings, as it might overrepresent certain subgroups, such as younger or more urban-based physicians. While the overall research process spanned 6 months, the data collection phase specifically took place over 2 months, starting from 20th September 2023.
Data collection was conducted using a single paper-based survey format administered in person. Trained data collectors visited multiple hospitals, diagnostic centers, and private chambers across the eight divisions to distribute and collect the surveys directly from physicians. This approach ensured direct engagement, enhancing both the reliability and consistency of responses. Participants received clear instructions on how to complete and submit the questionnaire to maintain reliability. The identification of suitable hospitals, chambers, and diagnostic centers, along with selecting convenient times for physicians, was crucial in gathering comprehensive and accurate data. This also allowed for immediate clarification of any questions participants had, further ensuring the quality of the responses.
Participants for the study were required to have completed at least their MBBS or BDS degree and be registered with the BMDC. Inclusion was contingent upon obtaining informed consent from each participant, ensuring voluntary participation. Excluded from the study were intern doctors and any incomplete survey responses, to maintain the integrity and quality of the data collected.
To ensure the reliability of the questionnaire, three experts reviewed the entire questionnaire set. These included two senior public health researchers, both holding PhDs with extensive experience in quantitative survey design and validation, and one experienced clinician with a postgraduate diploma in medical education and a strong background in integrating health technologies into clinical practice and teaching. The development of survey items was guided by existing validated tools from global literature assessing AI-related knowledge, attitudes, and practices among healthcare professionals. After adapting these items to the local context, expert feedback was sought for content relevance, clarity, and cultural appropriateness. After a thorough review process, the questionnaire was finalized and translated into Bangla. A pilot test involving 30 physicians was conducted to statistically assess the reliability and clarity of the questionnaire. Participants also reviewed the content for relevance, wording, and comprehensibility. As all items were found to be appropriate and clearly understood, no modifications were necessary following the pilot. The survey questionnaire was split into three parts: one focusing on knowledge, another on attitude, and the last on practice, with each section having its own questions. We calculated Cronbach’s alpha (α) for each section to evaluate reliability and consistency. All sections showed an alpha value greater than 0.70, indicating acceptable reliability. The overall model consistency was found to be 0.79, which is considered statistically very good.
Data analysis
After gathering the data, an authorized individual carefully reviewed it to ensure that it was complete and suitable. This involved refining and organizing the data to preserve its accuracy and reliability. Any missing or duplicated data was removed before finalizing the dataset. Stata software version 17 was utilized for this process. The analysis commenced with verifying that all gathered data aligned with the study’s criteria, for both inclusion and exclusion. The demographic characteristics of the participants were categorized and presented as frequency and percentage. Additionally, participants’ knowledge, attitude, and practice were also shown as frequency percentages.
To facilitate analytical comparison, participant responses in the knowledge, attitude, and practice (KAP) sections were converted into composite scores and categorized into meaningful groups using established KAP assessment principles. Specifically, respondents were labeled as having “good” or “poor” knowledge, “positive” or “negative” attitudes, and “good” or “poor” practices based on predefined scoring thresholds. These thresholds were derived from the total score distribution for each domain and were designed to reflect meaningful distinctions in understanding, perception, and behavior. For instance, a “good knowledge” classification indicated that a respondent correctly answered more than half of the relevant knowledge items, aligning with widely accepted practices in health behavior research where a 50%–60% score cut-off is used to indicate adequate knowledge or awareness. Similarly, for attitude and practice domains, Likert-scale responses were summed and interpreted using cut-offs validated in comparable studies. This binary categorization enabled the use of inferential statistics (e.g. Chi-square tests, logistic regression) to explore patterns and associations within the dataset. The full coding scheme, item-level scoring structure, and categorization logic are presented in Supplemental Appendix 1, and all survey questions used to generate these scores are detailed in Supplemental Appendix 2.
After completion of labeling, bivariate analysis was conducted, which included the Chi 2 test to explore potential associations between these factors and the knowledge, attitude, and practice variables. Statistical significance for the Chi-square test results was indicated as follows: Ψ for a p-value less than 0.05, ΨΨ for a p-value less than 0.01, and ΨΨΨ for a p-value less than 0.001. Moreover, binary logistic regression was conducted to determine the Adjusted Odds Ratio (AOR), which measures the strength of the influences. The statistical significance of the logistic regression results was indicated by p-value notations: * for a p-value less than 0.05, ** for a p-value less than 0.01, and *** for a p-value less than 0.001. These statistical methods allowed for a thorough analysis, identifying important factors and assessing the strength of the associations.
Results
The study includes 398 registered physicians in Bangladesh. The majority of participants were aged 21–30 years (55.53%), followed by the sexual categorical distribution showed that the majority were 65.58% females. Most participants were MBBS/BDS graduates (67.59%), and the majority of the participants were currently working in private hospitals (27.39%). All this information is shown in Table 1.
Demographic characteristics of the participants.

Knowledge of AI tools
In Table 2, A significant majority of participants had heard of AI (90.45%) and AI-based tools (76.88%). Knowledge about the application of AI in the medical field was low, with only 20.35% knowing such applications. Instructions for learning prompt generation for using AI tools were also minimal, with 1.01% receiving comprehensive instructions and 81.16% receiving no instructions. Regarding the knowledge of the application of AI in diagnostic decisions, this also showed a poor outcome, as 56.78% showed no knowledge, 17.34% had very limited knowledge, and 17.84% had limited knowledge.
Physicians’ knowledge, attitudes, and practices regarding AI tools in medical practice.

Attitudes toward AI in medical practice
Attitudes toward AI’s role in the medical system varied: 43.22% were neutral, 25.13% agreed, and 4.77% strongly agreed. Positive attitudes toward AI in medical education were observed, with 40.70% agreeing and 12.31% strongly agreeing. For AI’s role in early diagnosis, 45.98% agreed and 10.80% strongly agreed. Regarding those who think AI will replace doctors, 30.65% disagreed and 18.84% strongly disagreed. For AI’s essentiality in clinical practice, 34.67% were neutral, 30.65% agreed, and 4.02% strongly agreed. The necessity of AI for diagnosis was acknowledged by 36.93% who agreed and 4.52% who strongly agreed, with 32.16% remaining neutral. Concerning AI as a burden for practitioners, 40.95% were neutral, and 34.92% disagreed.
Practice of using AI tools
In practice, 73.87% of participants had not used AI tools in clinical areas. The ease of using AI was found majority as neutral by 70.35%, with 18.84% finding it easy and 3.02% very easy. Regarding the perception of whether AI tools made their job easier, 60.30% were neutral, 25.38% agreed, and 5.78% strongly agreed. Physicians’ roles in AI application and evaluation were positively perceived, with 40.20% agreeing and 19.35% strongly agreeing. Looking ahead, 41.96% agreed and 10.55% strongly agreed on the future adoption of AI diagnostic aids.
Prevalence of knowledge, attitude, and practice
After scoring and categorization based on participant responses, Figure 1 shows that 78.39% of participants demonstrated poor knowledge, while 21.61% demonstrated good knowledge. Attitudes were almost evenly split, with 48.74% having a negative attitude and 51.26% having a positive attitude. In terms of practice, 65.58% exhibited poor practice, while 34.42% had good practice.

Prevalence of knowledge, attitude, and practice levels among physicians in Bangladesh. The bar chart illustrates the prevalence of different levels of knowledge, attitude, and practice among 398 physicians in Bangladesh. Categories include poor and good knowledge, negative and positive attitudes, and poor and good practices. Each bar represents the number of participants and the corresponding percentage. The chart highlights that the majority of participants have poor knowledge and practice levels, while attitudes are nearly evenly split between positive and negative. The main categories (Knowledge, Attitude, Practice) are indicated below their respective subcategories for clarity.
Bivariate analysis of knowledge, attitude, and practice
In Table 3, Out of the total 398 participants, 312 (78.4%) were classified as having poor knowledge, and only 86 (21.6%) demonstrated good knowledge regarding AI in clinical practice. in terms of knowledge, the Sexual category showed a highly significant association with both knowledge (p < 0.001) and practice (p < 0.001). No significant associations were found in both knowledge and practice between other demographic variables like age group, education level, current role, or workplace. Also, attitude doesn’t have any significant associations with any demographic variables.
Association between demographic factors and knowledge, attitude, and practice regarding the use of AI tools in medical practice.

Note. Chi² significance: ΨΨΨp-value < 0.001.
Multivariate analysis
In multivariate analysis, there’s a higher likelihood (AOR = 3.56, CI: 2.11–6.03, p < 0.001) of having good knowledge among females compared to male physicians, and it is highly significant. gender was a significant predictor of good knowledge. Similar things were found in practice, where the female was also a highly significant predictor of good practice (AOR = 2.89, CI: 1.73–4.83, p < 0.001) compared to male physicians.
However, in terms of Postgraduate positions, those who were Assistant professors had a lower likelihood of having good knowledge (AOR = 0.21, CI: 0.04–0.93, p < 0.05) compared to those who didn’t have any postgraduation. Participants working in “others” workplaces had higher odds of a positive attitude toward AI (AOR = 1.97, CI: 1.06–3.64, p < 0.05) compared to those who worked in govt hospitals. Additionally, those who were working in a private hospital had a higher likelihood of having good practice (AOR = 2.16, CI: 1.11–4.20, p < 0.05) compared to those who were working in a government hospital. More information can be seen in Table 4.
Demographic factors associated with knowledge, attitude, and practice regarding the use of AI tools in medical practice.

Note. *CI: 95% confidence Interval; AOR: adjusted odds ratio.
AOR significance: *p-value < 0.05, ***p-value < 0.001.
Discussion
The study among registered physicians in Bangladesh provides significant insights into the demographics, knowledge, attitudes, and practices concerning AI tools in medical practice. Most participants were young (21–30 years) and predominantly female, aligning with global trends indicating an increasing presence of young professionals and females in the medical workforce. 26 Most participants worked in private hospitals, reflecting the diverse employment distribution within the healthcare sector. While this reflects the growing number of early-career physicians in Bangladesh, it may also result in an overrepresentation of individuals with more recent exposure to AI technologies through medical education or personal interest. Consequently, the findings may not fully capture the perspectives and practices of more experienced or senior physicians, potentially skewing the results toward higher AI awareness or acceptance.
A notable finding was that over 90% of the participants had heard of AI, and 76.88% had knowledge of AI-based tools, but detailed knowledge about AI applications in medicine was limited. This limited knowledge can be attributed to the lack of structured AI education in medical training programs, as supported by studies emphasizing the need to integrate AI education into medical curricula to enhance understanding and application.27,28 Furthermore, only 1.01% of participants received comprehensive instructions on using AI tools, highlighting a significant gap in getting training and professional development. 29 This mirrors findings in international contexts where lack of formal training remains a critical barrier to AI adoption among clinicians. 30 In contrast, some high-resource settings have reported early integration of AI modules in medical training, suggesting the need for localized curriculum reform to bridge this gap.
The attitudes toward AI revealed a mixed perspective. While a substantial proportion of participants held neutral views on AI’s role in the medical system, a positive attitude was observed toward AI’s potential in medical education and early diagnosis. This is shown in an existing study that suggests a cautious yet optimistic outlook among healthcare professionals regarding AI’s role in improving medical education and diagnostic accuracy. 31 The apprehension about AI replacing doctors, with many participants disagreeing with this notion, reflects concerns about job security and the perceived threat of AI to professional roles, a sentiment echoed in several studies on AI adoption in healthcare. 19
The practical use of AI tools in clinical settings was less common, with 73.87% of participants not having used AI tools, and the neutral stance on the ease of using AI tools indicates a need for more intuitive and user-friendly AI systems, as well as better training to facilitate ease of use. 32 Interestingly, this neutral stance contradicts studies in other LMICs where younger physicians reported more proactive experimentation with AI tools. 33 This divergence may point to cultural and institutional hesitations specific to Bangladesh, such as administrative resistance or regulatory ambiguity. This aligns with findings from other research, which suggests that user-friendly interfaces and comprehensive training programs are crucial for enhancing the adoption of AI technologies in clinical practice. 32 The study also found that while a majority had poor knowledge about AI, their practices were relatively poor as well, with 65.58% exhibiting poor practices. Studies have shown that without sufficient hands-on experience, healthcare professionals may struggle to integrate AI tools effectively into their practice. 34
Sex-based differences were found to be statistically significant in both knowledge about AI tools and the practical application of these tools in clinical settings, as demonstrated by both bivariate and multivariate analyses. Multivariate analysis revealed that female physicians had a significantly higher likelihood of having good knowledge and practicing well compared to male physicians. This is because female physicians may be more likely to participate in continuing education and professional development activities, which can enhance their understanding and utilization of AI tools. 35 Also, this may be influenced by several interlinked factors. In Bangladesh, female medical professionals often engage more actively in academic training and workshops related to emerging technologies due to greater institutional encouragement and peer engagement opportunities. 36 Additionally, gendered expectations in professional roles may result in women seeking out AI-related education to overcome perceived disadvantages in leadership or clinical authority, thereby contributing to higher AI literacy. 37 These trends are reflective of wider global shifts, where female healthcare professionals increasingly adopt digital health tools to enhance both efficiency and patient engagement. However, those in assistant professor positions had a lower likelihood of having good knowledge regarding the use of AI. This may be due to the demanding nature of their roles, which might limit their engagement with new technologies. 38
Furthermore, participants working in “other” workplaces exhibited higher odds of a positive attitude toward AI compared to those in government hospitals. Research facilities or specialized workplaces often provide more exposure to cutting-edge technologies and innovations, fostering a culture of continuous learning and adaptation. 39 These environments are typically equipped with better resources, training programs, and support systems for integrating new technologies, which can positively influence attitudes toward AI. 39 Additionally, those working in private hospitals had a higher likelihood of demonstrating good practice, likely due to better access to resources and training opportunities in private settings compared to government hospitals in Bangladesh. 40 Ethical concerns, especially regarding job displacement and de-skilling, also emerged in participant responses. These themes have been echoed globally, where physicians express ambivalence about AI tools substituting human judgment. 30
Limitations and strengths
Despite the efforts made to ensure the validity and reliability of the survey, some limitations may relate to how questions were worded and the response options provided. These can influence how participants understand and answer the questions, potentially impacting the accuracy of the data collected. Furthermore, these studies’ cross-sectional design offers a snapshot of physicians’ current knowledge, attitudes, and practices at a moment in time. However, this design doesn’t allow for tracking changes or trends over time, making it challenging to establish cause-and-effect relationships or understand how AI adoption evolves longitudinally. Additionally, measuring attitudes and awareness involves subjectivity, as participants’ interpretations can vary, potentially affecting the results. Another limitation is the potential for response bias, where physicians with a prior interest in AI may have been more motivated to participate. This could result in an overestimation of awareness and positive attitudes toward AI among the general physician population. Recognizing these limitations is essential for understanding the study’s findings and guiding future research. Despite these limitations, the study provides valuable insights into the knowledge, attitudes, and practices of physicians in Bangladesh regarding AI tools. The large and diverse sample enhances the generalizability of the findings and highlights the current state and potential areas for development in AI adoption among healthcare professionals. Furthermore, the study identifies critical gaps in AI knowledge and practice, offering a foundation for targeted educational and policy interventions.
Conclusion
This study highlights key insights into the knowledge, attitudes, and practices of physicians in Bangladesh regarding the use of AI as a medical assistant. The findings show high awareness but limited detailed knowledge. Most participants, despite their awareness, lacked comprehensive instruction on AI usage, indicating a need for improved training programs. Attitudes were cautiously optimistic, especially about AI’s role in medical education and diagnosis, though concerns about job displacement by AI were noted. Practical use of AI tools was limited, emphasizing the need for more user-friendly systems and better training. To address these gaps, AI training programs should be embedded into both undergraduate and continuing medical education. These programs could include hands-on modules, case-based simulations, and real-world use scenarios, ideally delivered by interdisciplinary teams combining clinicians and AI specialists. User-friendly AI systems should prioritize intuitive interfaces, minimal technical jargon, and seamless integration with existing hospital information systems, allowing physicians to adopt them without disrupting workflow. It is crucial to integrate AI education into medical curricula, offer ongoing professional development, and communicate AI’s supportive role clearly. Encouraging research and innovation in AI applications will further enhance its adoption. Future studies should consider longitudinal research designs to track changes in AI literacy and adoption over time. Additionally, interventional trials aimed at evaluating the effectiveness of specific AI training models—such as simulation-based learning or hybrid online modules—would provide valuable evidence to guide curriculum development. These steps will enable physicians to effectively utilize AI technologies, ultimately improving healthcare outcomes.
Footnotes
Acknowledgements
We would like to express our gratitude to all the physicians for their participation. Without their support, it would be difficult to get the data. We also acknowledge the use of AI-based language tools for minor editing and grammatical refinement of the manuscript; however, all content, analysis, and interpretations were solely developed by the authors.
Abbreviations
Abbreviation Full Form
AI Artificial Intelligence
AOR Adjusted Odds Ratio
BDS Bachelor of Dental Surgery
BMDC Bangladesh Medical and Dental Council
CI Confidence Interval
DHIS2 District Health Information Software 2
GPT Generative Pre-trained Transformer
KAP knowledge, attitude, and practice
MBBS Bachelor of Medicine, Bachelor of Surgery
p-Value Probability Value
Ethical consideration
The study received approval from the Institutional Review Board (IRB) of North South University (IRB #2023/OR-NSU/IRB/0806), which was mandated by regulatory requirements. The ethical guidelines specified in the 1964 Declaration of Helsinki and its later amendments were adhered to wherever applicable. Before participation, all eligible respondents were provided with a detailed explanation of the study’s purpose, procedures, potential risks, and benefits.
Consent to participate
Written informed consent was obtained from each participant. The respondents were assured that their privacy and confidentiality would be strictly protected, and no part of their responses would be disclosed to unauthorized individuals under any circumstances. This commitment to ethical standards ensured the protection and respect of all participants throughout the study.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data that support the findings of this study are available from the corresponding author (Md Nahid Hassan Nishan), upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.