Abstract
Dementia is a growing challenge in Southeastern and Western Europe, with aging trends projected to accelerate in the former region. The region is facing critical gaps in dementia care due to rural-urban disparities, workforce shortages, and limited access to specialized services. Widespread reliance on informal caregiving and underdeveloped diagnostic infrastructure delay early diagnosis and equitable access to the healthcare system. This perspective article presents sustainable, regionally tailored solutions and innovative strategies from a multinational dementia network, which are aimed at improving care outcomes through collaboration, capacity building, and digital innovation. Tailored workshops and multilingual platforms have raised awareness and encouraged innovative care approaches. Meanwhile, mobile memory teams in underserved areas have been shown to enhance caregiver support and patient outcomes. The Circle of Care Hub framework was developed to bridge coordination gaps and promote equitable, integrated dementia care by linking healthcare providers, social workers, and families. Digital tools have been piloted to enhance professional training, interdisciplinary collaboration, and informal carer support. Addressing barriers such as limited services and workforce shortages is essential for sustainable improvements. Future initiatives should prioritize scalable interventions, such as mobile teams, digital platforms with evaluation mechanisms, and hybrid care models, while investing in early diagnosis, dementia centers and region-specific prevention strategies informed by robust epidemiological data. Achieving sustainable dementia care requires a combination of digital innovation and community-based solutions.
Keywords
Background
The rising prevalence of dementia is placing an ever-increasing burden on healthcare systems, challenging their ability to meet the complex needs of aging populations and adapt to the growing demand for specialized, multiprofessional care.1,2 This burden is expected to be particularly severe in Southeastern Europe, where rapid population ageing is projected to result in a faster increase in the proportion of older adults and persons living with dementia compared to Western Europe, putting additional pressure on already strained healthcare systems (see Figure 1 and Supplemental Table S1). 3 –5,65

Increase in dementia prevalence (2019–2050). The graph shows the projected percentage increase in the population aged 65 and over in the countries of Southeastern and Western Europe up to 2050 and reflect the different demographic trends in the region, with accelerated ageing expected to have a greater impact in some countries than in others.
Southeastern Europe – as defined for this analysis- encompasses nine EU and five non-EU countries, thus being home to over 100 million people. This region shows substantial diversity in economic, demographic, and population characteristics. Life expectancy ranges from 71.8 years (Moldova) to 82.9 years (Austria), and population sizes vary from 82.7 million (Germany) to 0.6 million (Montenegro; Supplemental Table S2). Some countries have “young” populations with a low share of people aged 65 and older (e.g. Moldova, Montenegro), while others, such as Austria, Bulgaria, and Croatia, have aging populations surpassing the EU average.6 –9 These demographic shifts are further complicated by rural-urban disparities, particularly in Bosnia-Herzegovina, Romania, and Moldova, where up to 57.5% of the population lives in rural areas, affecting access to health services, social support, and workforce development (see Figure 2, Supplemental Tables S2 and S3).

Demographic change and societal adjustment needs in European countries. A societal change index, calculated from the proportion of the population over 65, projected dementia increases, and life expectancy, highlights significant societal adaptation needs in countries with a very high index, such as Bosnia Herzegovina (BIH), North Macedonia (MKD) and Austria (AUT), while moderate to high index values are observed in Slovenia (SVN, Czech Republic (CZE), and Slovakia (SVK). In Bosnia-Herzegovina, Romania, Slovakia, Slovenia and Moldova, where up to 57.5% of the population lives in rural areas, these demographic constraints affect access to health services, social support and training of health workers. 5
While research on dementia is advancing, important gaps remain in understanding regional prevalence patterns and care needs – highlighting the importance of further system-level investigation.10 –16
Moreover, many healthcare systems lack standardized diagnostic tools and sufficient training for general practitioners.13,15,16 Expanding access to professional care, equipping caregivers with evidence-based interventions, and integrating person-centered therapeutic approaches are urgent priorities to better support persons living with dementia and their families.17 –21
Reliance on informal care is still widespread, especially in rural areas.12,22 –30 This dependency places substantial financial and emotional strain on caregivers, many of whom face inadequate formal support, mental health challenges, social isolation, and limited access to healthcare services.31,32 Additional barriers, including shrinking family sizes, the advanced age of caregivers, and low public awareness, contribute to delayed diagnoses and insufficient care.24 –26,33 Furthermore, formal care options, such as institutional care, continues to be underdeveloped, with primary care providers often failing to diagnose dementia and underutilizing available treatments.15,16,34 –36
Given dementia’s multifactorial etiology – including vascular, lifestyle, and environmental factors – comprehensive preventive strategies become increasingly relevant.10,14,37 Lifestyle modifications, comorbidity management, and early intervention offer significant opportunities to reduce dementia risk, especially since such preventive strategies are largely absent in the region.10,11,14,37 –42
Main text
To address these challenges, a multiprofessional network of dementia experts has been established to foster sustainable cross-border cooperation from Germany in the West to Bulgaria in the East and from the Czech Republic in the North to Albania in the South. The network focuses on promoting innovative interventions, including digital learning formats, caregiver support platforms and region-specific programs, aimed at improving prevention, diagnosis and long-term management of dementia. This article critically examines the ways in which these initiatives contribute to bridging the gaps and advancing equitable dementia care in the region.
Collaborative initiatives addressing dementia care
This multinational consortium of medical practitioners from Southeastern European countries systematically studied the key challenges in dementia care across their countries and integrated results of a previous survey. 43 The analysis highlighted critical areas for intervention, including rural-urban disparities, underdeveloped healthcare infrastructure, professional migration, and lack of specialized services. These findings were translated into regional initiatives and projects aimed at addressing gaps through interdisciplinary collaboration, digital innovations, and capacity building.
Core projects
The Danubian Network for Dementia Education and Care (DANDEC), active from 2014 to 2018, established a collaborative network of 12 partner institutions and Alzheimer organizations across six countries, later expanding to 10. The project developed a regionally tailored e-learning program and addressed unmet needs in dementia care through multinational meetings. These meetings focused on improving professional skills, integrating evidence-based care frameworks, and developing assistive technology strategies. The project emphasized interdisciplinary collaboration through initiatives like the Dementia Academy and introduced the Circle of Care Hub framework to coordinate services among healthcare providers, social workers, and families under the guidance of dementia coordinators (see Figure 3).
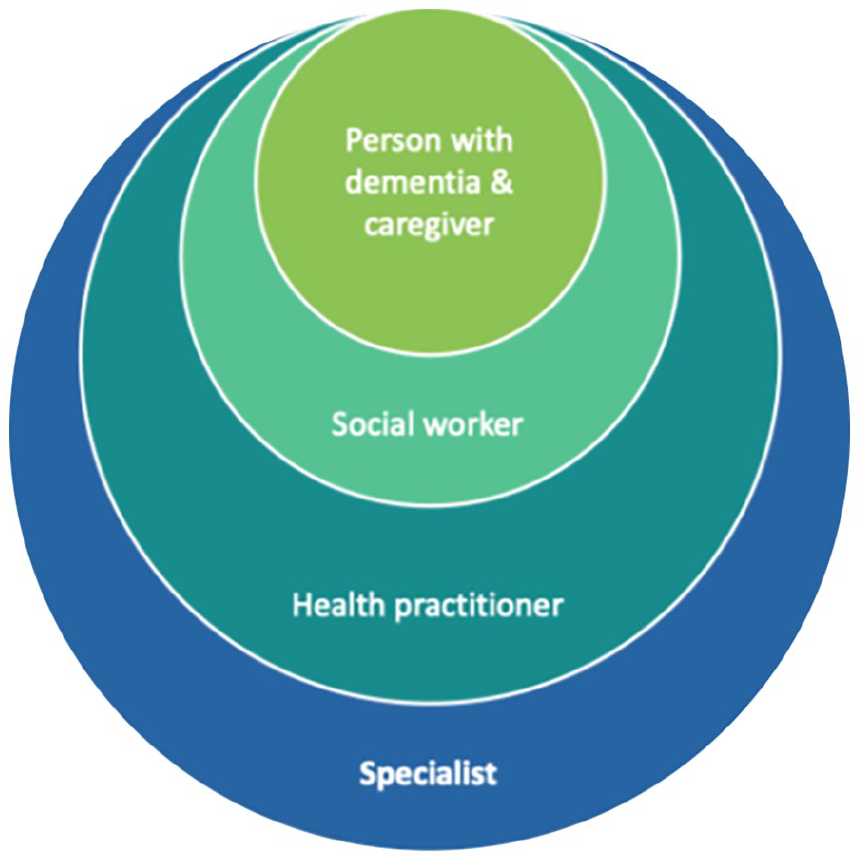
Circle of care hubs. The circle of care hub is a conceptual framework developed to demonstrate how dementia care could be improved through organized, multidisciplinary collaboration. At the heart of the model is the dementia coordinator, who connects healthcare providers, social workers, patient organizations and families to deliver coordinated, person-centered support. Although it is not a physical entity, the framework outlines mechanisms to bridge urban–rural divides, promote equitable distribution of resources, and foster dementia-friendly environments. By aligning local initiatives with transnational best practices, the model aims to reduce stigma, improve care outcomes and strengthen support systems, providing a vision for more inclusive and effective access to dementia care.
The INDEED (Innovation for Dementia in the Danube Region) project, launched in 2018, further expanded cross-border collaborations among 11 countries. Its web-based platform offered multilingual, mobile-accessible content for public awareness, professional training, and business development. By addressing infrastructure limitations, INDEED promoted scalable interventions tailored to diverse contexts, including early diagnosis, multidisciplinary care, and dementia-friendly communities. The development of the “Interprofessional Management on Dementia” workbook and regional training sessions demonstrated the impact of strong organizational collaboration on improving care outcomes.
Educational programs and digital solutions
A range of educational programs, including the Virtual Dementia Summer School and Dementia Master Classes, aimed to strengthen interdisciplinary dementia management through interactive sessions on person-centered care, treatment planning, and psychological support. The follow-up project STUDICODE (Stepping-Up Digital Competence in Dementia Education) improved the digital literacy of educators to develop online, flexible training modules for healthcare students and professionals. The modular structure, using interactive media such as videos and quizzes, ensured accessibility and relevance across different regions.
The ACCESS Dementia platform expanded these efforts by integrating features like an Easy Reading language version, simplified content, and sign language tools to improve accessibility for people with cognitive impairments, reading difficulties, or hearing loss. The platform’s community module connected users to organizations, dementia policies, and feedback mechanisms, while targeted workshops addressed the needs of 24-h caregivers. By combining digital flexibility with tailored content, ACCESS Dementia demonstrated the potential of hybrid solutions to address regional disparities and promote sustained learning.
Socio-psychiatric intervention
The North Macedonia Interprofessional Dementia Care (NOMAD) project (2021–2024) introduced mobile memory teams, consisting of nurses and social workers, to provide diagnostic, therapeutic, and community-based support in rural areas. 22 The project assessed the model’s feasibility through a cluster-randomized trial, demonstrating its effectiveness in improving access to care and strengthening national dementia strategies. 22 However, challenges related to staffing shortages and financial constraints highlighted the need for scalable hybrid models combining mobile teams with telehealth services to optimize resource use.
Key issues and future directions
Insights from the NOMAD project and related initiatives underline the need for broader analysis of care structures, diagnostic capacity, and implementation gaps to inform scalable strategies across the region.
A critical analysis of care infrastructure and implementation gaps
Building on prior findings, critical infrastructure deficits—including limited community services and diagnostic tools—continue to delay diagnosis and increase caregiver burden. Targeted interventions must now focus on strengthening formal services, especially in underserved rural areas.43 –47 These structural shortcomings are consistently reflected in regional research.12,16,34 Caregivers frequently report emotional strain, social isolation, and inadequate professional support, highlighting the urgent need to strengthen formal service networks.29,31 Tackling these deficits by expanding community-based services and mobile outreach is crucial to ensure sustainable and equitable dementia care infrastructure across the region, particularly in areas with shortages of specialists.48 –52
The importance of an early diagnosis
Even in high-income countries, dementia diagnoses are often delayed until the late stages of neurodegenerative diseases including Alzheimer’s disease. 53 The extended preclinical phase offers a key opportunity for prevention, planning and shared decision-making, yet it remains widely underused.3,54,55
Scalable innovations, such as blood-based biomarkers (e.g. phosphorylated tau and glial fibrillary acidic protein), demonstrate strong concordance with cerebrospinal fluid biomarkers, amyloid and tau PET imaging, and clinical progression.56 –59 This makes them promising tools for broader application, particularly when used alongside digital cognitive assessments or brief, validated questionnaires (e.g. the AD8, the IQCODE and the SCD-Q), as part of a stepwise diagnostic approach involving off-site screening and on-site confirmatory diagnostics, such as imaging or specialist evaluation.60 –62 These markers could facilitate the early detection of disease and risk stratification, even in settings with limited resources. They promote the judicious use of advanced tools and improve early access to the health care system.63,64
Prioritizing workforce development in dementia services
Primary care providers, especially general practitioners, are crucial in identifying persons with early cognitive decline and initiating preventive measures. Web-based training and continuing education programs help to close knowledge gaps and improve diagnostic work-up in both urban and rural settings, particularly because existing education and training programs of healthcare professionals remain disconnected from practical dementia care and lack standardized, evidence-based content.18,20,43,44 In order to address workforce shortages, efforts should focus on recruiting, training and retaining healthcare staff through targeted incentives and digital training platforms that enhance diagnostic capacity at the primary care level. 52
Highlighting differences in epidemiological trends
While some Western European countries report stabilizing or declining dementia incidence rates, which are likely linked to improvements in cardiovascular health, Southeastern Europe continues to experience an increase in prevalence driven by demographic aging, social disadvantage and a lack of adaptation in the health system.3 –5,65 Furthermore, the lack of robust, large-scale epidemiological data from Southeastern Europe hinders targeted and effective policy responses.10,11,13,14,25 Furthermore, although the interplay between vascular, genetic and psychosocial risk factors is well documented in the literature, this is rarely reflected in regional preventive strategies.37,40,66 These findings underscore the urgent need for regionally tailored prevention and diagnostic strategies that systematically address modifiable lifestyle risk factors and promote health literacy. 55
Hybrid care models as a strategic opportunity
In light of the structural challenges – including limited diagnostic infrastructure, regional disparities, and the reliance on informal care – hybrid care models emerge not only as a necessary adaptation but as a strategic approach to improving equity, scalability, and system resilience in dementia care. Instead of updating outdated systems, Southeastern European countries can transition directly to tiered models, which have been proposed as optimal solutions by healthcare market experts. 67 To have a sustained impact, such models must be embedded in robust evaluation frameworks and supported by cross-sector collaboration. Closing structural gaps and expanding access to targeted interventions is essential for achieving dementia care that is more equitable, cohesive and future-proof.
Conclusion
Southeastern Europe is facing the dual challenge of an increasing prevalence of dementia and limited healthcare resources. However, these gaps offer an opportunity to reimagine healthcare delivery by adopting sustainable, equity-focused strategies.55,68 –70 Digital innovation can help to bridge structural barriers by decentralizing information, supporting decision-making and improving knowledge transfer for patients, carers and providers.44,71 –74 Yet disparities in digital infrastructure and low digital literacy still pose major obstacles.75,76
Achieving sustainable dementia care in Southeastern Europe will depend on effectively integrating digital innovation with locally adapted, community-based solutions, supported by cross-sector commitment and informed by robust data.
Supplemental Material
sj-docx-1-phj-10.1177_22799036251361380 – Supplemental material for Bridging gaps in dementia care across southeastern Europe: Regional challenges, cross-border innovation, and implementation barriers
Supplemental material, sj-docx-1-phj-10.1177_22799036251361380 for Bridging gaps in dementia care across southeastern Europe: Regional challenges, cross-border innovation, and implementation barriers by Carolin Kurz, Ilir Alimehmeti, Marina Boban, Smiljana Kostic, Osman Sinanovic, Osman Kučuk, Shima Mehrabian, Latchezar Traykov, Ninoslav Mimica, Gabriela Novotni, Lea Pfaeffel, Vildan Dogan, Janine Diehl-Schmid, Panagiotis Alexopoulos, Christian Grünhaus, Zvezdan Pirtošek and Alexander Kurz in Journal of Public Health Research
Footnotes
Acknowledgements
The authors would like to thank Simona Krakovska and Mihai-Viorel Zamfir for contributing to the consortium. The authors would like to thank the respondents for their contribution and time. Graphs were created using R Studio version 2023.9.0.463 (RStudio, P., Boston, MA. RStudio: Integrated Development for R. 2020).
List of abbreviations
DANDEC – Danubian Network for Dementia Education and Care, EU – European union, GDP – gross domestic product, GP – general practitioner, INDEED – Innovation for Dementia in the Danube Region, n.a. – not applicable, STUDICODE – Stepping up Digital Competence in Dementia Education.
Ethical considerations
Ethical approval was obtained for the NOMAD study. The NOMAD study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethical Committee of the Medical Faculty at the University Ss Cyril and Methodius in Skopje, North Macedonia (Ref Number: 03-1260/5).
Informed consent
It was not necessary to obtain informed consent for this manuscript, as it does not contain original data from study participants.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Austrian Ministry of Social Affairs (ACCESS, grant number 2023-0.009.156), the German Federal Ministry of Education and Research (DANDEC and NOMAD, grant numbers 01DS13011 and 01DS21016), the European Union (INDEED, grant number DTP2-089-1. 2), European Union Erasmus+ Strategic Partnerships (STUDICODE, grant number 2020-1-DE01-KA226-HE-005786), German Academic Exchange Service (Dementia Masterclasses, 57367186, 57404449, 57461187 and Virtual Dementia Summer School/DAAD: 57527453) and Global Incentive Fund, Bavarian Research Alliance to support digital mobility (Bavaria-Québec/International).
Conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability
The data supporting the findings are available upon request. Interested individuals are welcome to contact the authors to gain access, subject to appropriate permissions and ethical considerations.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
