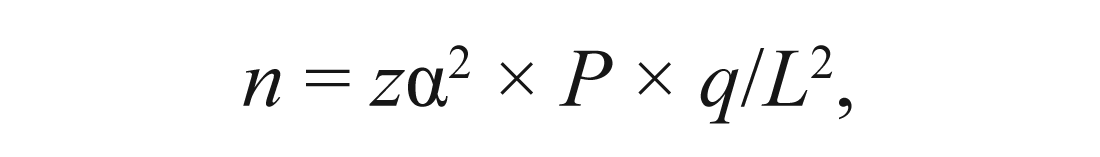Abstract
Aims and Objectives:
The practice of self-medication may lead to lack of clinical evaluation by a trained medical professional and delay in effective therapy. This study was aimed to find the prevalence of self-medication and identify the common causes of illness/symptoms that necessitate self-medication awareness and develop perception regarding methods to prevent the growing trend of self-medication and associated factors among population those who visit a community outreach programme in Madurai, India.
Material and Methods:
A cross-sectional, questionnaire-based survey in which a semi-structured questionnaire was used to collect data. A total of 238 participants were included in the study with respect to the final sample size. Data were analysed using SPSS software with a significance level of 0.05, and statistical relationship between the variables was analysed using chi-square test.
Results:
The prevalence of self-medication is 69.32 per cent. Headache (59.6%), fever (60%), cough (51%) and toothache (25%) were the most common symptoms for self-medication. The most commonly used drugs/substances were analgesics (65.54%), warm saline (38.23%) and hot drinks (27.73%). The most common reason for resorting to self-medication practice was previous experience of successfully treating a similar illness. The majority of the participants (56.97%) were in their third–fourth decade of life. The association of self-medication with characteristics such as male gender, urban locality, and upper-and lower-middle class was statistically significant at a p-value of 0.005.
Conclusion:
Self-medication practices were quite high in this study, and these practices were also prevalent among the educated people. The physicians and health professionals have to spend some extra time in educating patients regarding the same. Improved knowledge and understanding about self-medication may result in rationale use and thus limit emerging microbial antibiotic resistance issues.
Introduction
Self-medication is the use of medicinal products by people to treat self-recognized disorders or symptoms, or the intermittent or continuous use of a medication prescribed by a medical physician for a chronic or recurring symptom. 1 It also includes acquiring medicines without a valid prescription, giving old prescriptions to purchase the medicines, sharing medicines among relatives or members of one’s social circle or using leftover medicines which are stored at home. 2 With the increase in awareness and knowledge related to medications, self-medication practice is widely spreading in developing countries like India. For years, the Indian healthcare system has been plagued with unrestricted use of analgesics and antibiotics prescriptions and sales, resulting in the emergence of resistant microbial strains for antibiotics.
Major disadvantages of practising self-medication are the lack of clinical evaluation of the condition by a physician, which could result in missed diagnosis and delaying of appropriate treatments, and increased risk of drug toxicity as a result of overdosing and adverse drug interactions. 3 Many researchers have shown that self-medications can increase the wastage of medicinal resources and the risk of microbe’s resistance.
To our best available knowledge, only few studies were conducted at community level in India to assess the magnitude and factors associated with self-medication practices. Studies of such nature have useful insight on the reasons for which patients opt this practice and might help the regulatory authorities to streamline the process of drug regulations, updating the list of essential medicines and safety issues of over-the-counter drugs. 4 With this background, the present study was done to assess the prevalence and attitude of self-medication practice among people attending oral health outreach programmes in Madurai East, Tamil Nadu.
Materials and Methods
The study population included people of age more than 18 years, who visited community outreach programmes in Madurai East, Tamil Nadu. Following simple random samp-ling, Madurai East has been selected for the study by lottery method. The synopsis of the proposed research was prepared and submitted to the Institutional Review Board, Best Dental Science College and Hospital, Madurai, for ethical approval (BDSC/29-7-15). After the review and scrutiny by the board members, approval was granted to conduct the research. Based on the prevalence rate of pilot study, sample size required for this study was calculated using the following formula:
where n = number of subjects required, zα = confidence level at 95 per cent (standard value of 1.96), P = 83% (prevalence of self-medication), q = 1 – P = 17%, L = allowable error = 5% (power of 95%) Non response rate of 10 per cent was expected.
The study consisted of 238 participants. The survey was conducted for a period of three months from August 2015 to October 2015. A detailed schedule of the survey was prepared well in advance. A pilot study was carried out with 20 subjects in order to test items’ understandability and content validity. The internal consistency was assessed by Cronbach’s α. The results of the pilot study showed a good consistency with α-values higher than 0.9.
A pretested questionnaire containing items to assess the practices, determinants and attitudes of the sampled population towards self-medication was interviewed after obtaining informed consent. The participants were given assurance on the confidentiality of their personal information. The study population comprised of people who visited community outreach programme conducted by the Department of Public Health Dentistry, Ultra Best Dental Science College and Hospital, Madurai. The questionnaire consisted of six sections (A, B, C, D, E and F). Details of this questionnaire are as follows: Section A, containing eight items, assessed the demographic details, including age, sex, education, employment, monthly income and address. These were all open-ended questions. Section B comprised of nine questions related to health conditions to which they opt for self-medication. Section C consisted of six items related to drugs and other substances used for self-medication. Section D consisted of 10 questions with respect to the reasons for opting self-medication. Sections E and F consisted of questions related to self-awareness and methods of preventing self-medication respectively.
Results
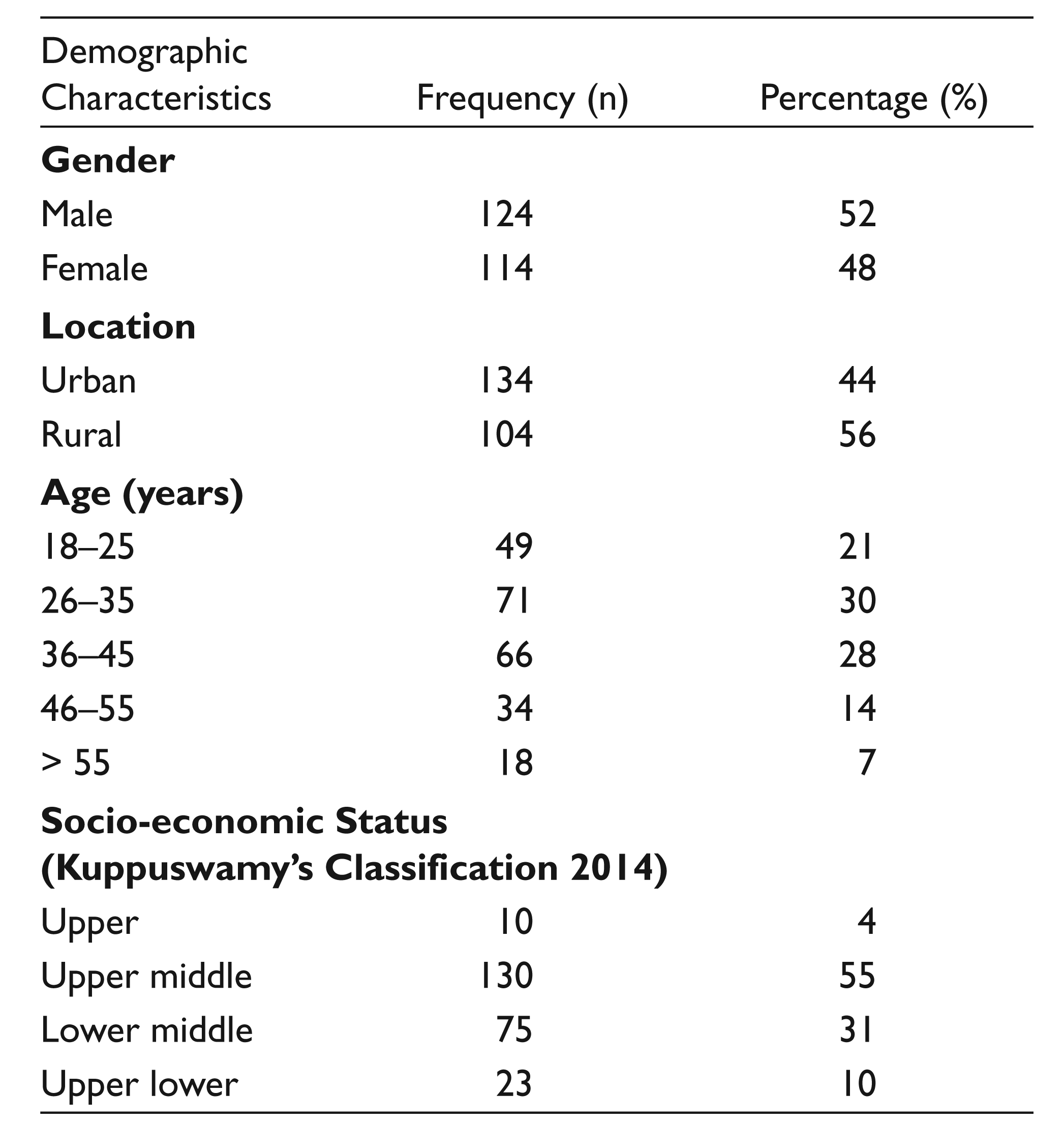
The prevalence of self-medication in our study was 69.32 per cent (n = 238). Socio-demographic data revealed that the age of the participants ranged from 18 to 60 years, out of which females were 48 per cent (n = 114) and males were 52 per cent (n = 124). Majority of the participants belonged to the adult age group of 26–45 years and were 58 per cent (n = 137) (Table 1).
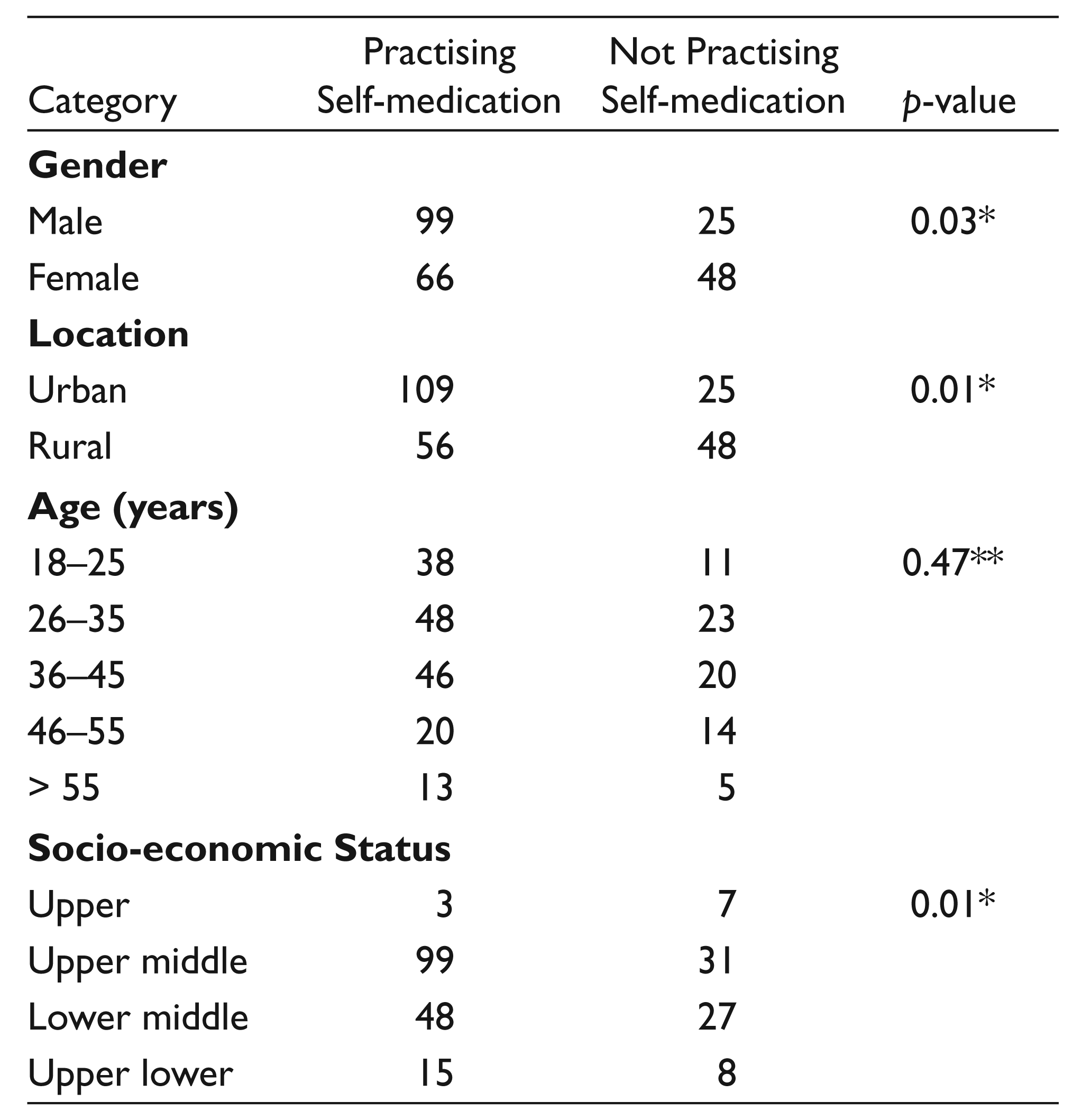
The comparative evaluation of the practice of selfmedication with the socio-demographic factors revealed that the males (52%; n = 124) were practising more than the females (48%; n = 114) and the difference was found to be statistically significant (p < 0.05) (Table 2).
Socio-demographic Details of the Study Population
Comparative Evaluation of Self‑medication Practice in Relation to Socio-demographic Characteristics
Discussion
In this study, the prevalence of self-medication practice among the participants was 69.32 per cent. Many studies are conforming to present study results such as Samuel et al. (62%) 5 and Joshi et al. (75%). 6 This may be due to easy availability of the drugs without a prescription or with an old prescription from the pharmacy and the availability of these drugs as over-the-counter drugs for perceived symptoms. The wide difference in practice of self-medication may be due to difference in socio-economic status, education and awareness of dangers of self-medication among people. 7
Subjects of more than 18 years of age participated in this study. There was no statistical difference observed between the different age groups and the practice of self-medication, which is similar to studies conducted by Simon et al., Gupta et al. and Shankar et al.8-10 A possible implication of this is that all adult people who practise selfmedication may have unrestricted access to drugs and this may lead to misuse of drugs.
The present study detected an association between gender and self-medication practices, where males were more likely to indulge in them. This finding is consistent with other studies which demonstrated a high prevalence of self-medication among males.11,12 The probable reasons for higher prevalence in males could be they being economically stronger; their increased outdoor activities; free movement outside and easy accessibility to pharmacies; to avoid loss of wages by spending time in hospitals; and the neglecting nature of mild illnesses by males.
The majority of the subjects involved in self-medication belonged to upper middle (55%) and lower-middle classes (31%). Practice of self-medication was least among upper-class (4%) subjects. The study conducted by Selvaraj et al. is conforming to our study. 13 The probable reason may be that upper-and lower-class people seek treatment from the private and public hospitals respectively. The lower-and upper-middle-class people practise self-medication may be due to financial burden and indirect social pressure to not to seek treatment from government hospitals.
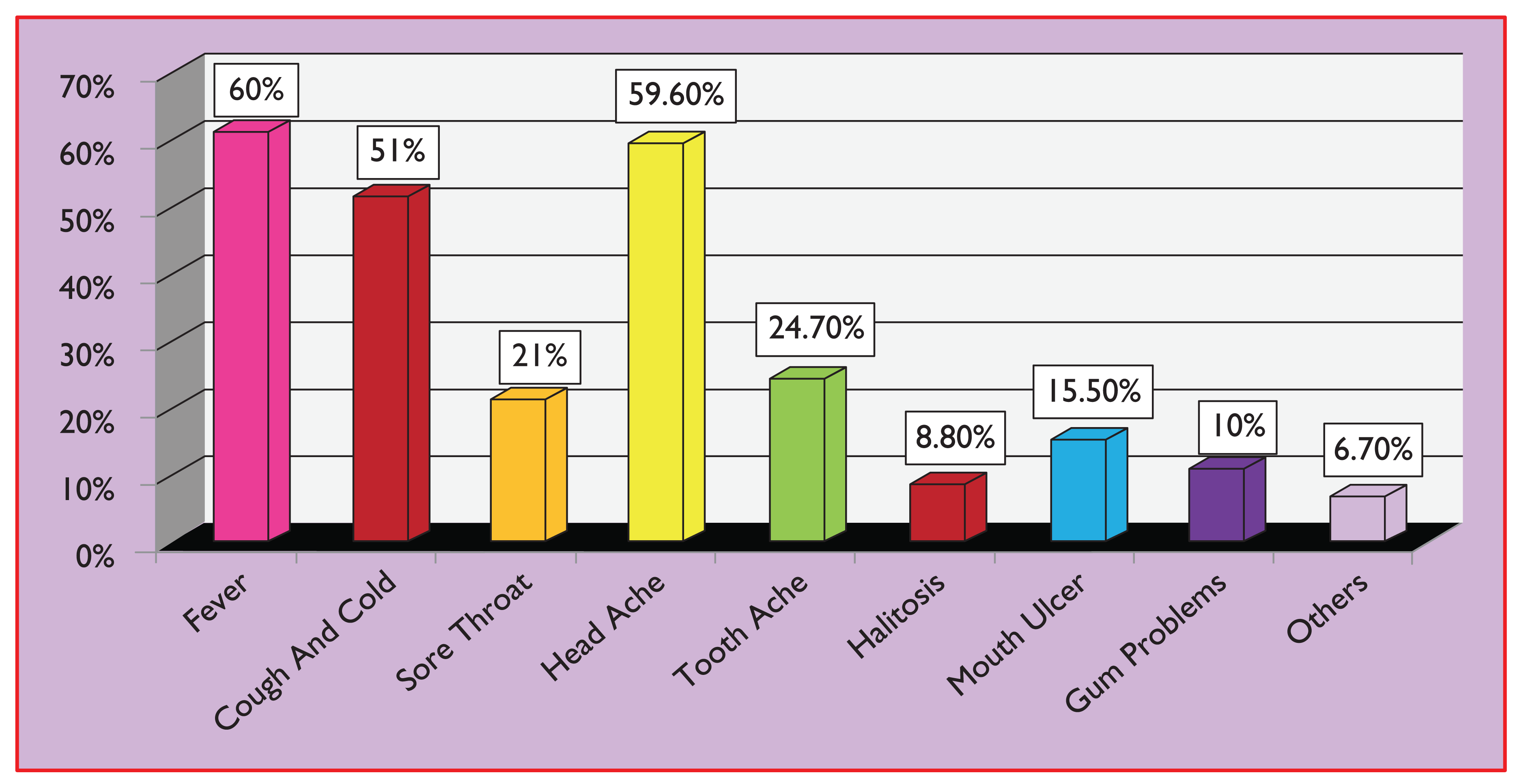
In this study, fever (60%), headache (59.6%) and cough and cold (51%) were the most common symptoms for which self-medication was practiced (Figure 1). The study conducted by Gupta et al. is conforming to our study. 9 The probable reason for indulging in self-medication for these conditions is the fact that they are considered minor illnesses, self-limiting in nature and doctor’s consultation is not necessary for them. The other oral conditions such as toothache, sore throat, mouth ulcer, gum problems and halitosis are considered less symptomatic and do not have much effect on their health. The reason could be the fact that people give more importance to the general health than oral health.
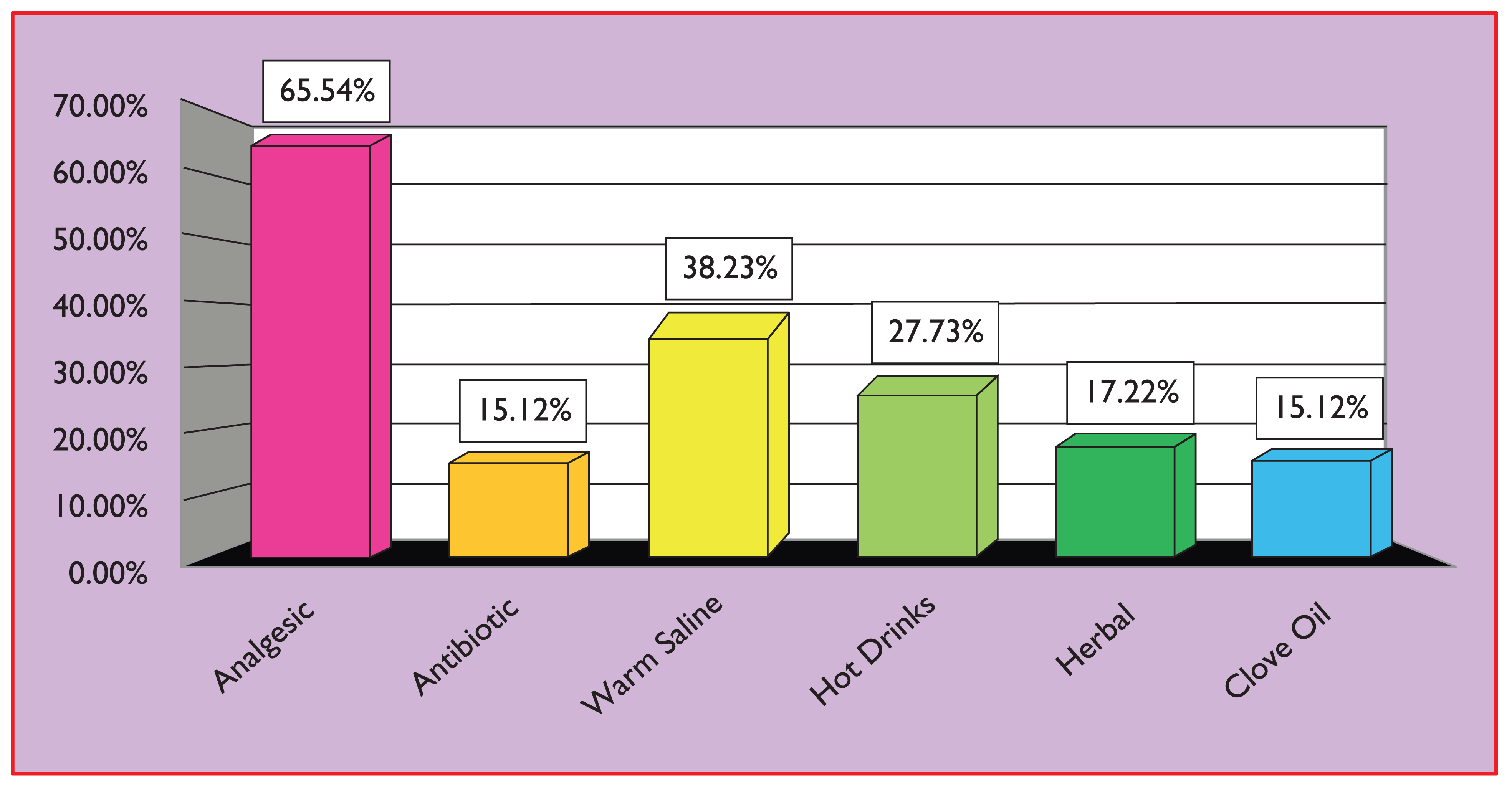
In this study, analgesics were the most common group of drugs opted for self-medication by the respondents (Figure 2). This is similar to other studies conducted by Aqeel et al., Baig et al. and KomalRaj et al.14-16 Antipyretics were the most common medications used for selfmedications in studies conducted by Sandeep et al. and Rajput et al.12,17 This is because analgesics and antipyretics are widely available and easily procured over the counter in our environment. The major problems associated with the use of analgesics include increased risk of nephropathy, drug-induced gastric ulceration and chronic toxicity leading to renal failure.
The most common reason for practising self-medication in this study was previous experience of treating a similar illness (47.89%) (Table 3). This could be explained by the ability of people to remember medications whether prescribed or over the counter used for similar previous conditions. Second major reason mentioned by 47 per cent of respondents was that subjects felt that the illness was too mild, whereas easy accessibility to over-the-counter drugs was the common factor reported by Adedapo et al. and Abid et al.3,18 Joshi et al. concluded that economic constraints were the most common reason for opting self-medication. 6 Baig et al. reported laziness as the most common reason associated with self-medication in their study. 15
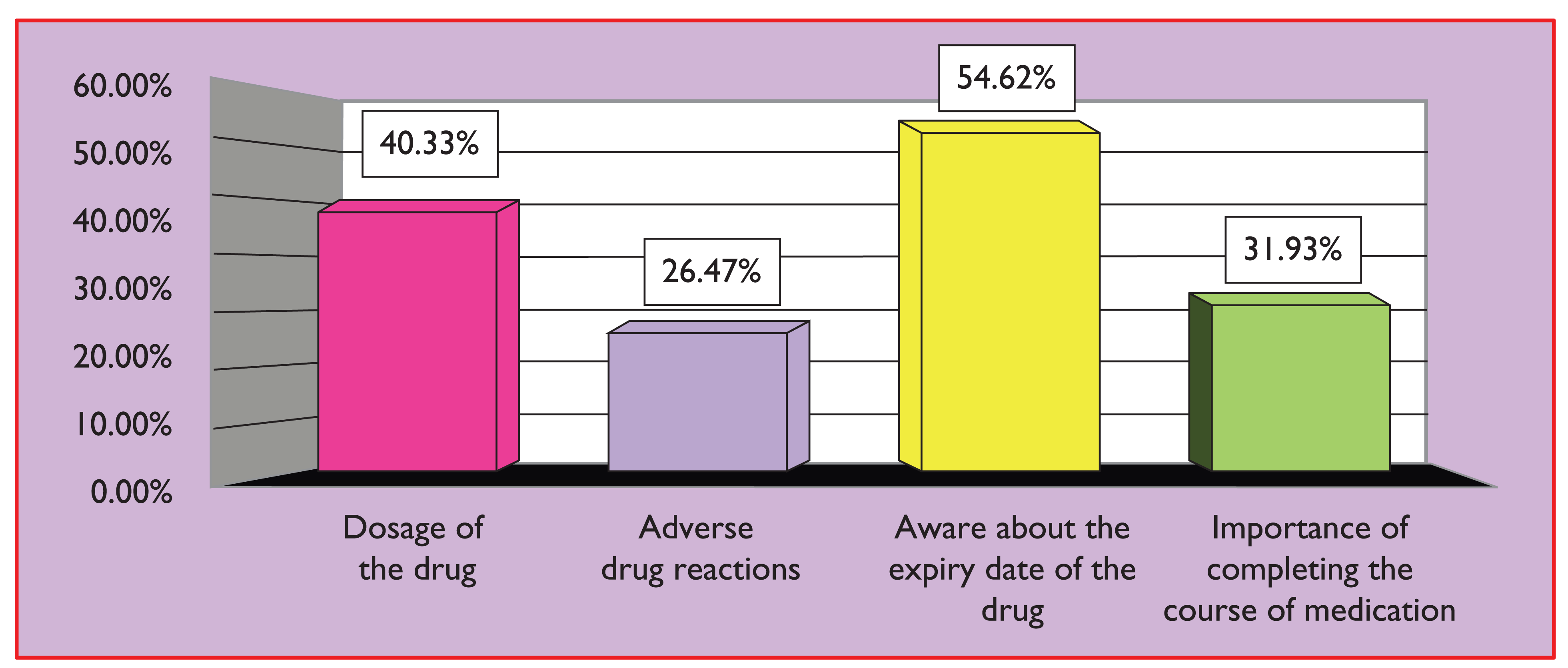
When the study subjects were enquired about the awareness of self-medication practices, the participants were more aware about the expiry date (54.62%) (Figure 3). Similar finding was seen in studies conducted by Jain et al. and Shah et al.19,20 This finding may be due to the fact that majority of study participants in the present survey had level of education which made them to read the label instructions on the medication including expiry date.
Percentage of Various Factors Associated with Self-medication Practice

Conclusion
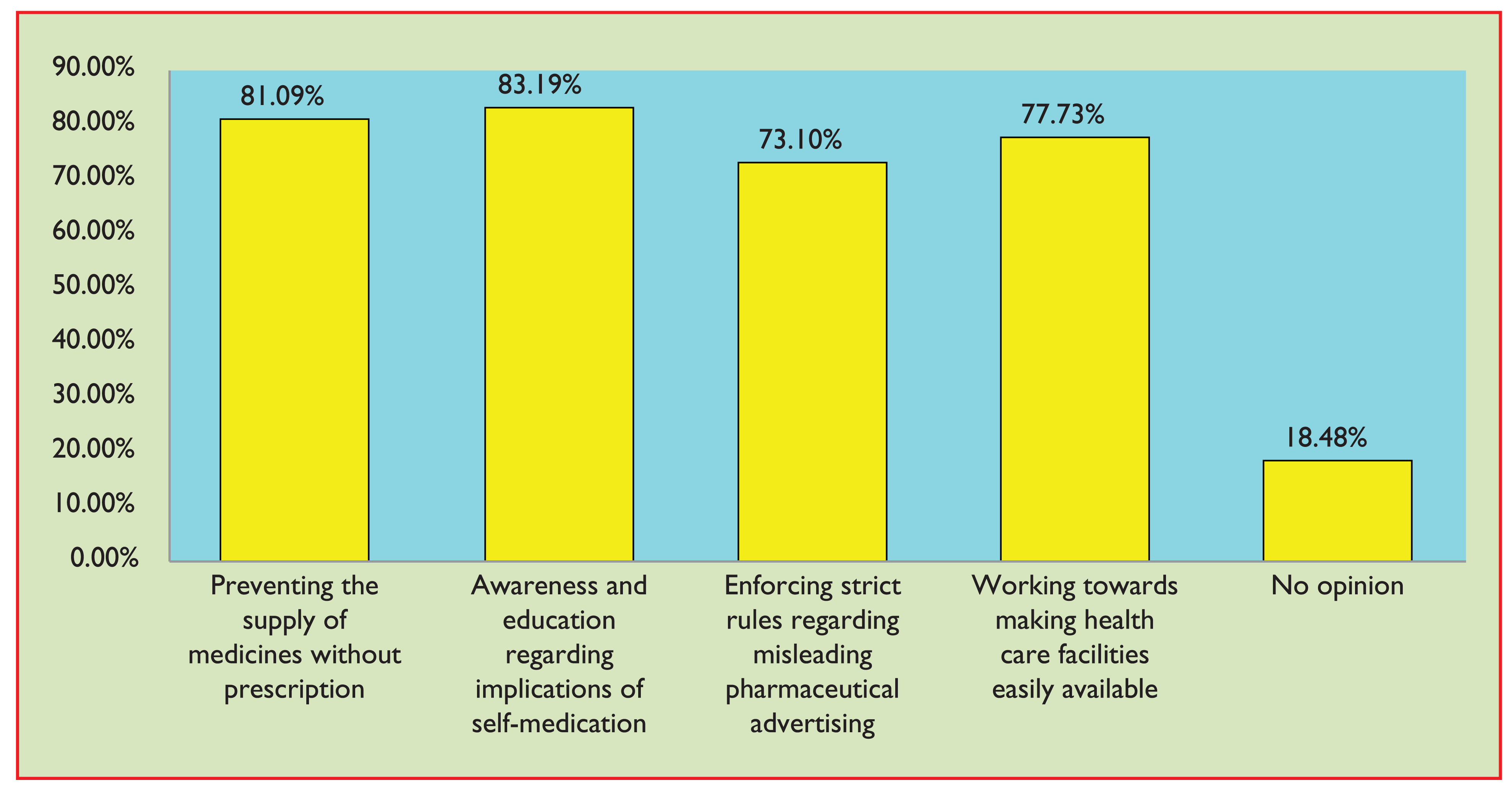
Results showed that self-medication and non-doctor prescription was found to be obvious and at an alarming rate of 69.32 per cent. In this survey, people of all socio-demographic categories approve of self-medication, giving reasons of previous experience of treating a similar illness, non-seriousness of their condition, followed by lack of time as a major reason. In addition, analgesics were often used for treating their problems. Fortunately, majority of respondents were aware of the adverse effects regarding the drug prescribed including expiry date of medication used. Self-medication has to be used within the limits and treated along with proper consultation from a registered pharmacist, if possible. It would be safe if the people who are using it have sufficient knowledge about the dose, side effect on overdose and time of intake. Due to lack of information, it can cause dangerous effects such as microbial resistance to antibiotics, skin disorders, hypersensitivity and allergy to medicines. So, in developing countries like India where we have poor economic status and poor health care facilities, people have less knowledge regarding risks associated with their self-medication practice. We are on the edge of sword whether to promote or stop self-medication practice. So, a holistic approach should be undertaken to prevent this problem, which includes proper education and awareness regarding self-medication and strictness regarding pharmaceutical advertisements. The physicians and health professionals have to spend some extra time in educating patients regarding the same. Improved knowledge and understanding about self-medication may result in rationale use and thus limit emerging microbial antibiotic resistance issues.
Footnotes
Acknowledgements
None
Declaration of Conflicting Interest
The authors declare that there is no conflict of interest.
Funding
None