Abstract
Purpose
In the setting of sacral fractures, percutaneous screw fixation is a reliable, safe, and minimally invasive method for managing most stable and unstable fractures. However, significant variations in sacral anatomy due to sacral dysmorphism (SDM) could prevent safe implementation. This scoping review aimed to highlight such a detrimental yet under-reported variable in managing sacral fractures.
Methods
A scoping review was conducted following the Arksey and O’Malley framework for scoping studies. A comprehensive literature search of four electronic databases was conducted to identify relevant peer-reviewed studies. Data were extracted from eligible articles to summarize, collate, and create a narrative account of the findings.
Results
Twenty-one articles were included in our review (18 level III, two level II, and one level I). Studies were categorized into three main groups based on the investigated outcomes: prevalence and determinants of SDM, effect of SDM on the surgical corridor, and efficacy of different intra-operative imaging modalities. The prevalence of SDM ranged from 10 to 85%. The presence of SDM decreased the available surgical corridor at S1, with a compensated increase at S2 and S3. Mixed results regarding accuracy and revision rate were identified between different intra-operative imaging techniques.
Conclusion
SDM represents consistent yet atypical “safe zone,” sizes, and angles that require careful analysis and technique alterations when placing upper and second sacral segment screws. Considering their limited availability, high cost, and mixed results, navigated imaging systems represent a promising technique that requires more rigorous examination of its efficacy before widespread adoption.
Introduction
The sacrum is the keystone of the pelvic girdle and is responsible for 60% of pelvic stability. 1 Considering the relatively low incidence and significant heterogenicity of sacral fractures, the management of such fractures has always been controversial. 2 As the trend in managing unstable pelvic fractures has shifted towards surgical fixation in the past few decades, considering the clear impact on both morbidity and mortality, several techniques, both open and percutaneous, have been proposed to treat such complex injuries.3–6
With technical improvement, widespread practice, and advances in surgical imaging, percutaneous screw placement has become a reliable method that provides stability with minimal soft tissue insult.7,8 However, safe percutaneous screw placement is technically demanding and requires a considerable understanding of the complex three-dimensional anatomy of the posterior pelvis. The trajectory of the long screw and proximity of critical neurovascular structures makes any cortical penetration dangerous. 9 Moreover, the significant variation in sacral anatomy, including sex-specific differences, adds to this complexity. 10
Sacral dysmorphism (SDM) or upper sacral dysplasia refers to a variation of the “normal” sacral anatomy. 11 The prevalence of SDM varies significantly between different studies and ranges between 10 and 85%.12,13 This variation is due to significant discrepancies in the definitions of SDM in the literature, regarding both qualitative and quantitative parameters.
Routt et al. identified five qualitative radiographic signs of upper SDM on pelvic outlet and lateral plain films (residual disc space S1/S2, collinearity, mammillary bodies, dysmorphic sacral neuroforamina, and upper sacral segment not recessed in the pelvis). 11 Since then, most studies have focused on whether the sacrum was normal or dysmorphic based on these signs.14,15 However, little is known regarding the reliability and clinical value of these signs for the preoperative planning of iliosacral/trans-sacral screw fixation.13,16 Moreover, there is no agreement on how many of these signs are needed to label a sacrum as dysmorphic or which signs are more specific for SDM. Quantitative definitions of SDM are based on the determination of trans-sacral osseous corridors on computed tomography (CT).10,17 The sacrum is defined as dysmorphic if no corridor with a certain minimum diameter threshold is found in S1.18,19
The importance of identifying SDM becomes more evident when managing certain unstable fracture patterns that have a higher risk of displacement, such as vertical and bilateral sacral fractures. 20 In these cases, obtaining purchase in the contralateral trans-sacral cortex can increase the strength of fixation.7,21 In dysmorphic sacra, however, the ability to place a transverse screw at S1 is limited by the more cephalad and anterior position of the upper sacral segments in relation to the iliac crests and is impossible in most cases.14,22–24 In such situations, a transverse screw in S2 and S3 is crucial to restore stability. Several reports have demonstrated that the decrease in the available osseous fixation pathway (OFP) at S1 in dysmorphic sacra is compensated by an increase in OFP at S2 and S3.14,17,22,23,25 However, questions have arisen regarding the strength of fixation at S2 and S3 owing to the reported decrease in bone mineral density (BMD) in both normal and dysmorphic sacra.26,27 Interestingly, SD is independent of sex despite significant differences in sacral morphology. 10
Considering the narrow corridor for screw placement, especially in the setting of SDM, different intra-operative navigation systems have been proposed as guides for “safer” screw placement as opposed to conventional fluoroscopy.28,29 However, the high cost and limited data regarding their efficacy in the setting of SDM remain an obstacle to determining the best intra-operative guiding system.19,30
Despite the prevalence of SDM and the challenges it presents, the ideal approach to manage sacral fracture in such cases remains unclear. Scoping reviews are effective strategies to aggregate and categorize heterogeneous research activity, and areas of focus for future research can be determined by identifying gaps and points of conflict in existing literature. This scoping review aimed to highlight this prevalent morphological variant and to examine the existing evidence in efforts to determine: (1) the prevalence and determinants of SDM; (2) the influence of SDM on the sacral surgical corridor and hardware choice; and (3) if navigation increases the accuracy of screw placement in the setting of SDM.
Materials and methods
A systematic literature review of SDM was conducted. The numerous variables, methodologies, results, and outcomes in the available SDM literature suggest the use of a scoping review as described by Arksey and O’Malley.31,32 A scoping review includes a broader search strategy while maintaining transparency, reliability, and reproducibility.
Search strategy
Excerpta Medica Database (EMBASE), Medical Literature Analysis and Retrieval System Online (MEDLINE/PubMed), Cochrane Central Register of Controlled Trials (CENTRAL), and Cumulative Index to Nursing and Allied Health Literature (CINAHL) databases were searched from date of inception to May 10, 2021.
The search strategy was adapted to each database. MeSH and EMTREE terms were used in several combinations to increase search sensitivity. The search strategies for the databases are presented in Appendix 1. A manual search of related references and cited articles was also performed.
Eligibility criteria
All studies that investigated SDM, either alone or in comparison with the normal sacrum were included. To maximize potentially eligible data, there were no restrictions on publication date or language. We excluded studies that did not account for SDM as a distinct group. We also excluded case reports, surgical technique articles, reviews, editorials, and basic science papers.
Study screening
Study selection was performed by two authors (FNA, OAM) using the Covidence systematic review software (Veritas Health Innovation, Melbourne, Australia). The selection of studies was performed in a stepwise manner, first by title and abstract, then by full-text review. A resolve-by-consensus strategy was utilized for all discrepancies. If consensus could not be reached, a third senior researcher (HJ) was consulted. The references of the included studies were manually screened to identify additional articles that may have been missed using the initial search strategy.
Extraction of data
Data were extracted by two reviewers (FNA, OAM) independent of each other using electronic data sheets. To ensure accuracy, the results were audited by both reviewers and reviewed by the senior researcher (HJ).
The extracted data included information on basic study characteristics, demographic data (age, sex, sample size, and prevalence of SDM), determinants of SDM, characteristics of S1/S2/S3 in normal and dysmorphic sacra, safe zone for S1 screw, feasibility of trans-sacral screw at S1/S2/S3 in normal and dysmorphic sacra, feasibility of the oblique screw at S1 in the dysmorphic sacrum and angle of insertion, BMD, method of intra-operative imaging, number of misplaced screws, complications, and revision rate.
Risk of bias and quality assessment
Risk of bias at the individual study level was independently assessed by two reviewers (FNA, OAM) using the ROBINS-I tool (Risk of Bias in Non-randomised Studies of Interventions). 33 Risk of bias is assessed within specified bias domains, and review authors are asked to document the information on which judgements are based. In this context, bias focuses on studies’ internal validity and is defined as a tendency for study results to differ systematically from the results expected from a randomized trial that is conducted with the same participant group, without flaws in its conduct. Seven domains were assessed: confounding, selection, departures from intended interventions, missing data, outcome measurement, selective reporting, and overall bias. As most of the identified studies had a single-arm design, bias specific to this review included the likelihood that the findings would differ from a well-designed randomized controlled trial (RCT).
Statistical analysis
Using Cohen's Kappa (κ), inter-reviewer agreement at each stage of the screening process was calculated. Agreement was categorized a priori, as per Landis and Koch, 34 with κ of 0.81–1.0 for near-perfect, 0.61–0.80 for substantial, 0.41–0.60 for moderate, and 0.21–0.40 for fair agreement. Inter-observer agreement for methodologic quality assessment was calculated using the intraclass correlation coefficient; a value of ≥0.65 was considered adequate. 35 We used descriptive statistics to summarize all data. For continuous data, we reported the mean and standard deviation or median and interquartile range based on the data distribution. We used counts and proportions to describe all other data. No inferential statistical testing was performed.
Results
Study selection
Using the search strategy described above, 395 relevant citations were identified from the electronic databases. These 395 articles underwent title and abstract screening. Following the removal of duplicates (n = 22), irrelevant articles, and articles with incomplete data, 44 articles remained. These 44 articles underwent full text review, ultimately producing 21 articles that met the inclusion criteria for this report.10,12–19,22–26,28–30,36–39 Figure 1 shows the PRISMA flow diagram. There was perfect agreement for both the title and abstract screening (κ = 0.92) and full-text review (κ = 0.96).
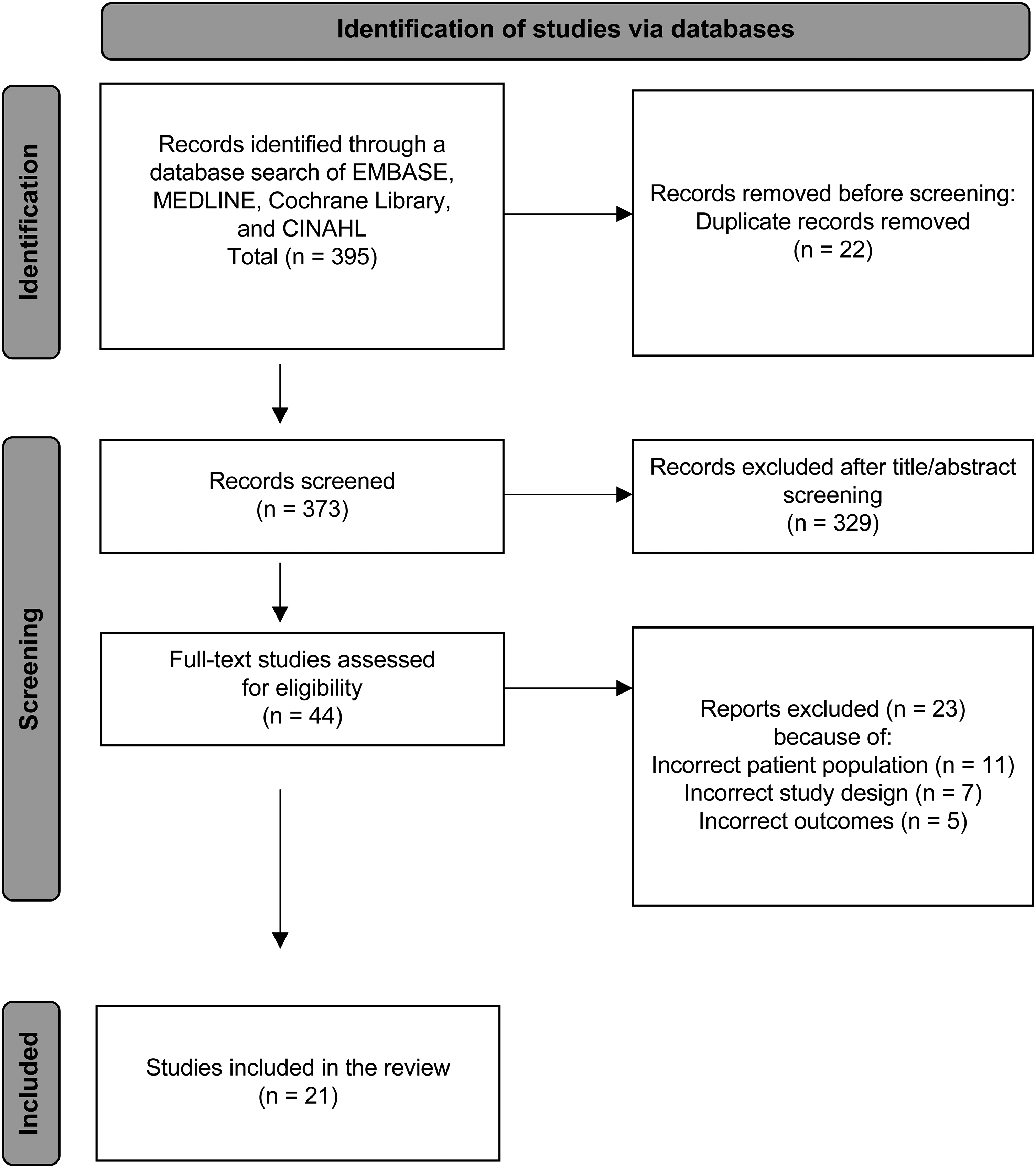
PRISMA flow diagram which included searches of databases and other sources.
Study characteristics
The included studies were conducted between 2010 and 2020, with 13 (62%) studies published within the past five years of our search. Majority (18/21) were level III evidence (number of patients, n = 3180),10,12–18,22–24,28–30,37–39 two were level II evidence (n = 392),25,26 and one was level I evidence, 19 (n = 130). Table 1 shows the characteristics of the included studies.
Baseline characteristics of the included studies.
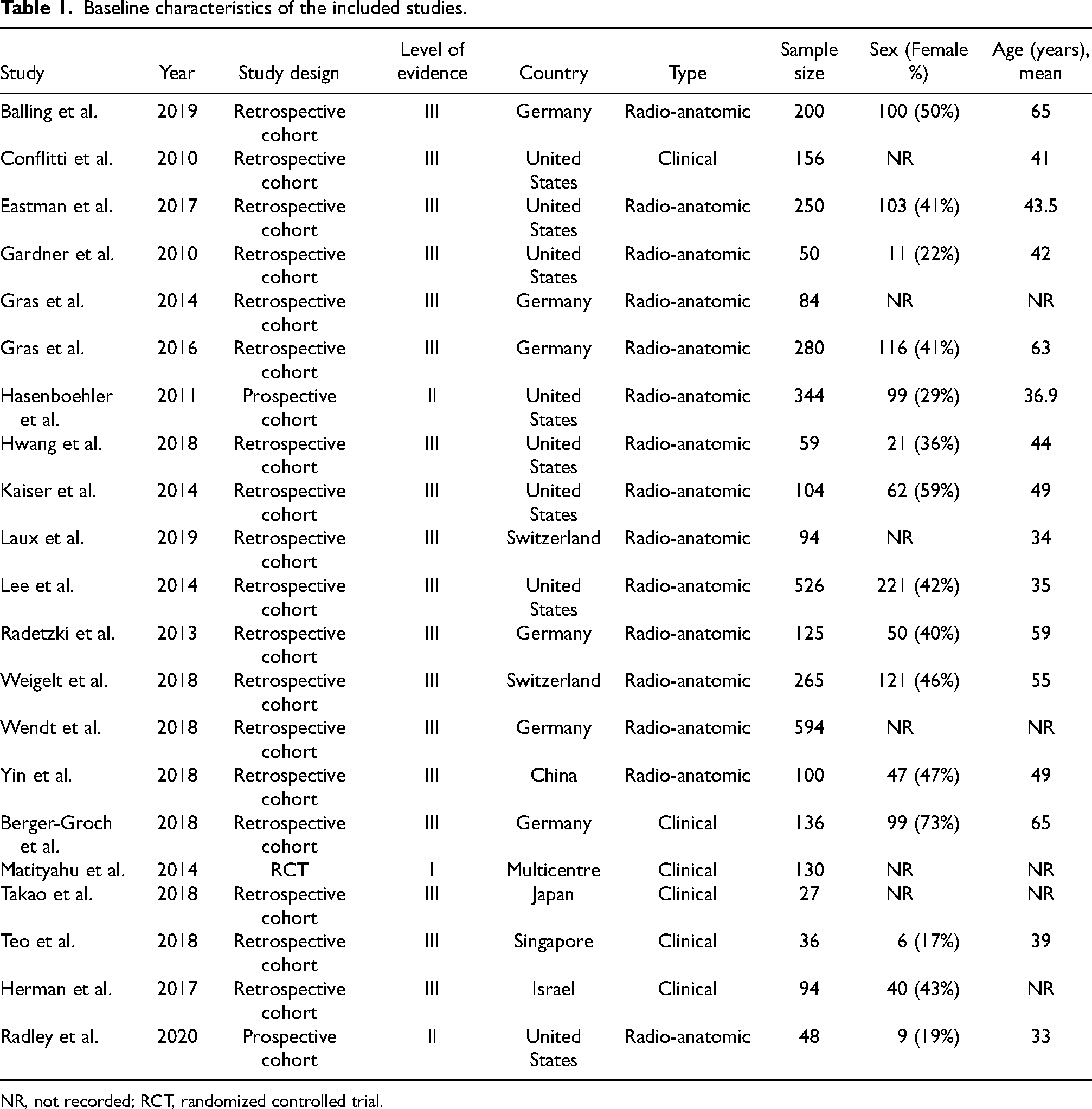
NR, not recorded; RCT, randomized controlled trial.
This review included 3702 patients; 1639 (44.1%) were female, with a mean participant age of 47 ± 10.1 years. Most of the studies included were radio-anatomic (15/21),10,12–18,23–26,36–38 and six were clinical papers.19,22,28–30,39 Studies can be categorized into three main groups based on the investigated outcomes: studies that investigated the prevalence and determinants of SDM (21/21) (Table 2), studies that investigated the effect of SDM on sacral surgical corridors and screw feasibility (15/21) (Table 3), and studies that investigated different intra-operative imaging modalities and their efficacy in the setting of SDM (6/21) (Table 4).
Prevalence and determinants of sacral dysmorphism per study.
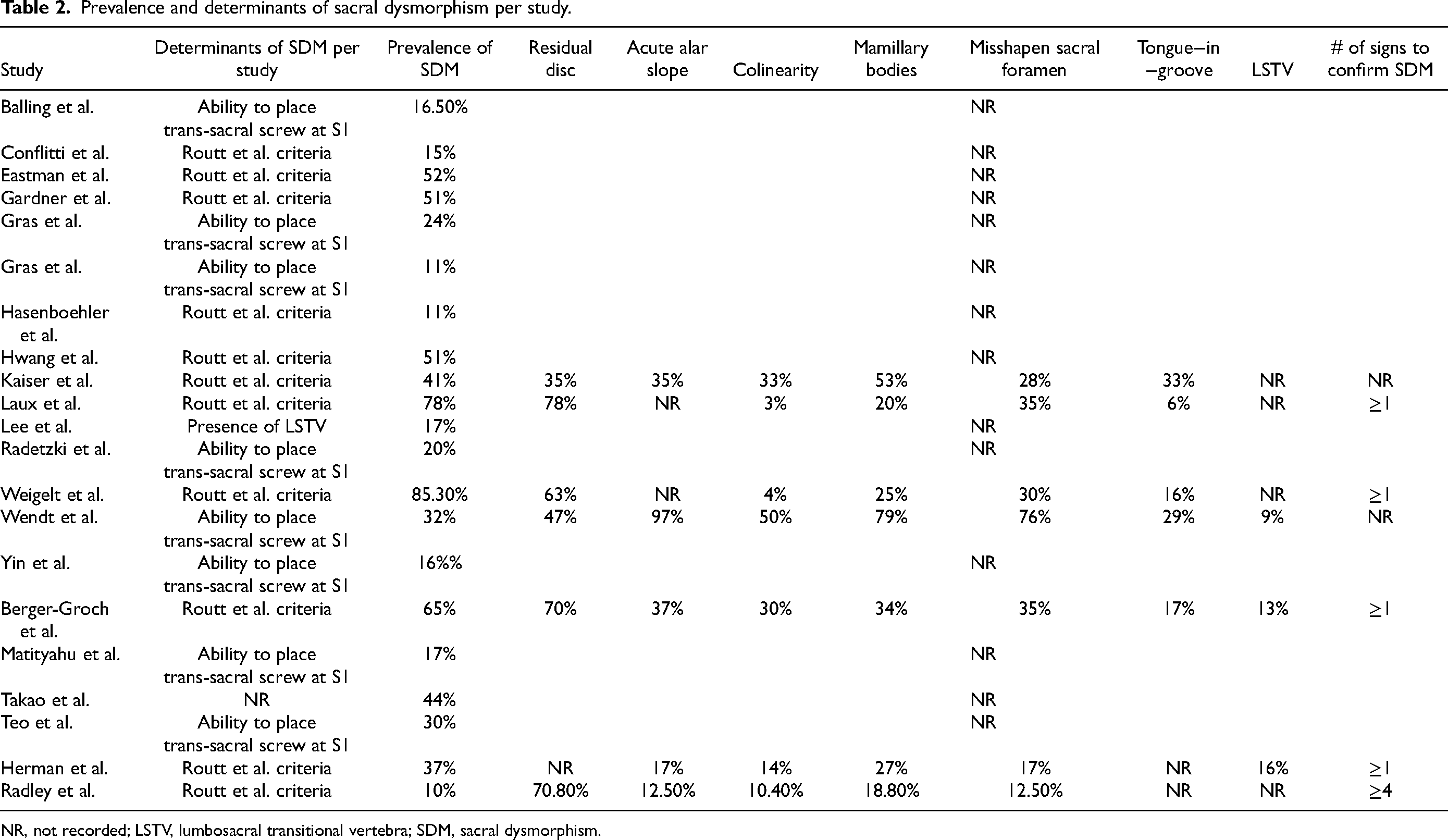
NR, not recorded; LSTV, lumbosacral transitional vertebra; SDM, sacral dysmorphism.
Surgical corridor diameter in NS and DS and screw feasibility.
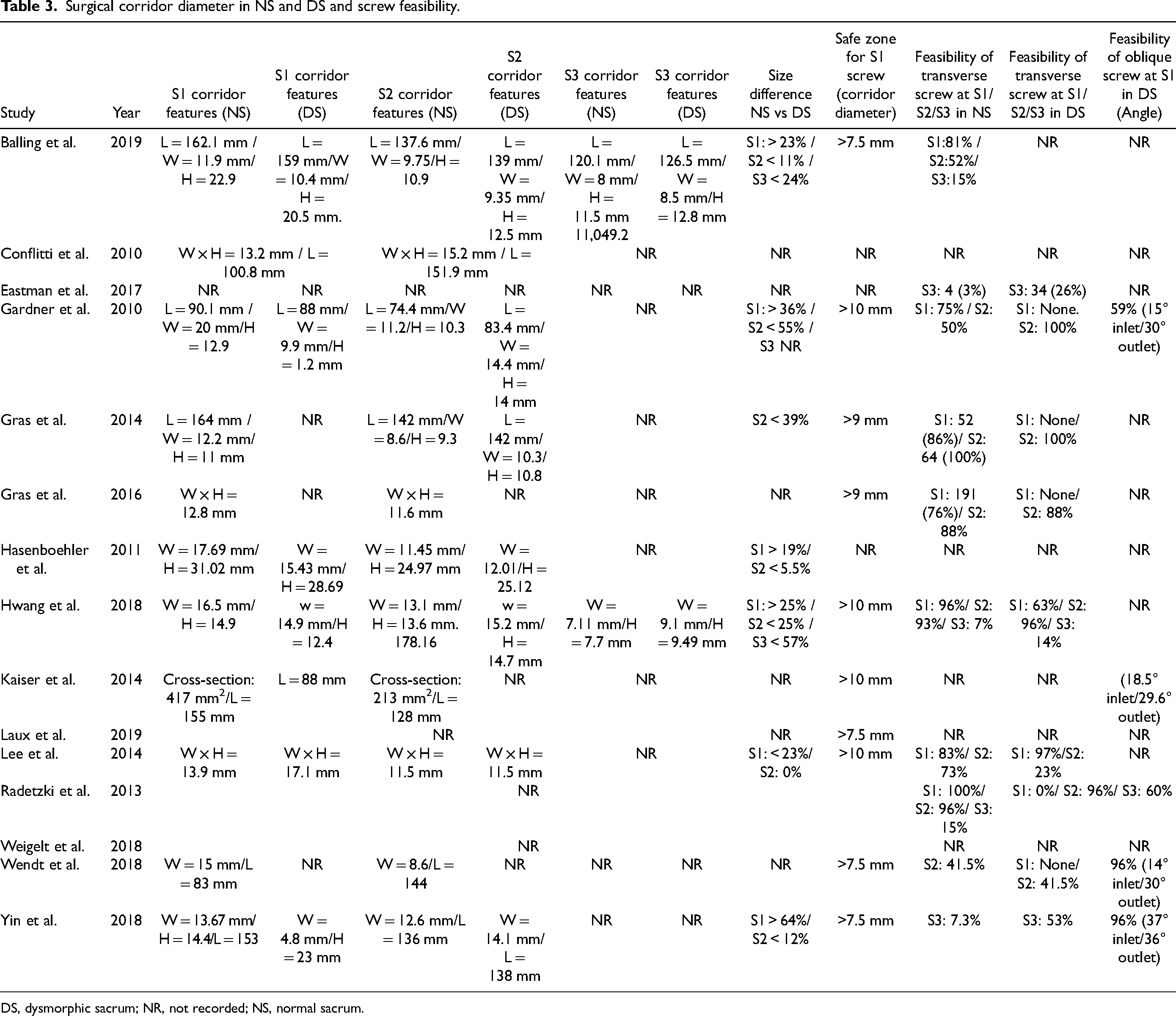
DS, dysmorphic sacrum; NR, not recorded; NS, normal sacrum.
Accuracy, complications, and revision rates in Conventional Fluoroscopy Vs Navigated fluoroscopy in SD.
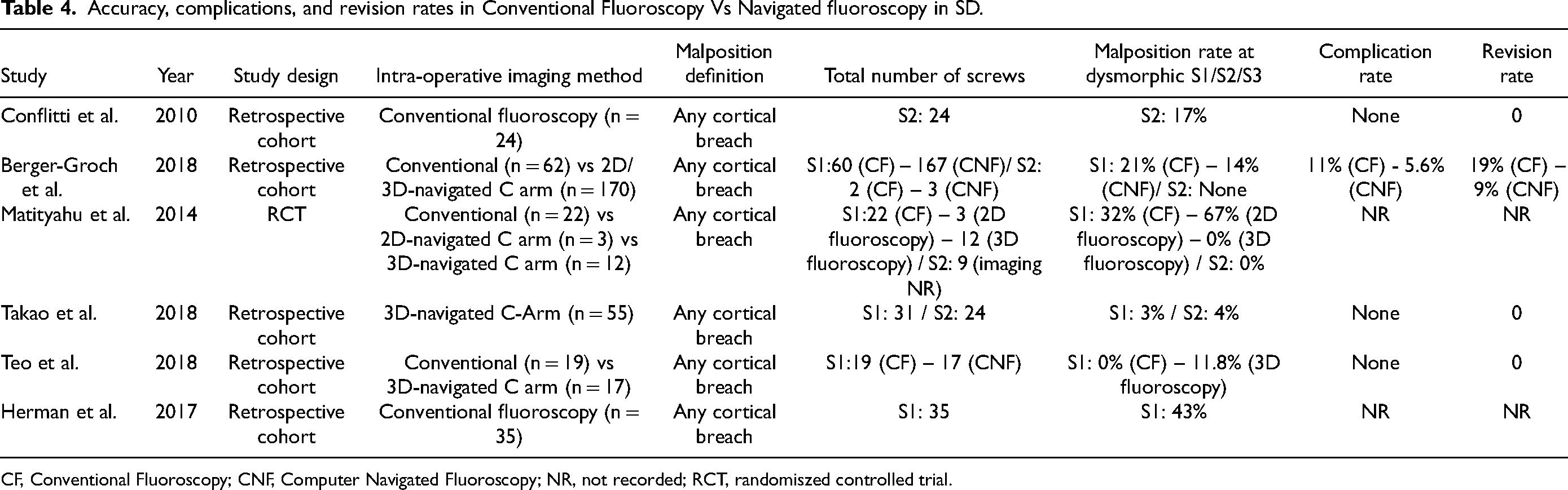
CF, Conventional Fluoroscopy; CNF, Computer Navigated Fluoroscopy; NR, not recorded; RCT, randomiszed controlled trial.
Prevalence and determinants of sacral dysmorphism
The prevalence of SDM in the included studies ranged from 10 to 85%. Studies included in our systematic search mainly defined SDM based on qualitative or quantitative criteria. Qualitative criteria (11 studies) were based on the previously mentioned radiographic characteristic identified by Routt et al. on an outlet view in addition to the “tongue-in-groove” sacroiliac morphology on axial CT.13–16,22–23,25–26,28,36,37,39 Majority of the studies either did not report (16/21)10,12,14–15,17–19,22–25,29,30,36,38 or required at least one sign to label a sacrum as dysmorphic (4/21).13,16,28,39 Only the study by Radley et al. required at least four signs to confirm SDM. 26 The most prevalent dysmorphic sign reported in all the included studies was the presence of a residual disc at S1 (61%), followed by acute alar slope (40%), presence of mamillary bodies (36%), dysmorphic foramen (33%), collinearity (21%), tongue-in-groove (20%), and lumbosacral transitional vertebra (LSTV) (19%).
Quantitative criteria (10 studies)10,12,17–19,30,37,38 were based on whether a transverse trans-sacral screw could be safely placed in the S1 corridor. The cut-off S1 corridor diameters for “safe” screw placement were 7.5 mm (4/10 studies), 9 mm (2/10), and 10 mm (4/10).
Studies with qualitative criteria had a higher average prevalence of SDM with 45.5% (range: 10–85%) compared to studies with quantitative criteria [20.3% (range: 11–32%)].
Influence of sacral dysmorphism on the sacral surgical corridor and hardware choice
Nine retrospective and one prospective cohort study directly compared the effect of SDM on the S1/S2/S3 surgical corridor (Table 3).10,12–18,22–25,36–38 At S1, all dysmorphic sacra had a smaller available surgical corridor at all diameters (height, width, and length) compared to normal sacra. The average reduction in the available OFP was 33.4% (range: 19–64%). The exception was the Lee et al. study which evaluated sacral segmentation variation as a predictor of dysmorphism, in which S1 corridor was 23% larger in dysmorphic sacra. 24 This effect SDM has on the available corridor translates into limited feasibility for a trans-sacral screw at S1. Compared to normal sacra (in which the feasibility of a trans-sacral S1 screw ranged from 75 to 100%), only Hwang et al. reported the feasibility of a trans-sacral screw in a dysmorphic S1, while the remaining studies reported that it was impossible in any of the dysmorphic groups. Regarding the optimum angle for an oblique iliosacral screw at S1, the average angle ranged from 14 to 37° on inlet view and from 30 to 36° on outlet view.
Considering the available surgical corridor at S2 and S3, the decreased diameter of dysmorphic S1 vertebra was compensated by an increase in the available corridor at S2 and S3 in all the included studies. The average increase in available OFP was 21% (range: 5.5–55%) at S2 and 40.5% (range: 24–57%) at S3. Moreover, despite not having a significant effect on the feasibility of a trans-sacral screw at S2, the presence of SDM increased the feasibility of a trans-sacral screw at S3 from 3–15% in normal sacra to 26–60% in dysmorphic sacra.
Considering these results, the strength of fixation at dysmorphic S2 was investigated by Radley et al. based on BMD. They reported that dysmorphic S2 had 28% less BMD compared to S1, highlighting the importance of S1 screw. 26
Accuracy of screw placement in sacral dysmorphism using navigation systems
Although extensive research exists comparing conventional vs. navigated fluoroscopy in the setting of sacral fracture and the accuracy of S1 screw placement, only a few studies considered SDM as a confounding variable. Our systematic search revealed two retrospective studies that investigated the accuracy of conventional fluoroscopy,22,39 one retrospective paper that assessed the use of 3D-navigated fluoroscopy, 29 and three studies including a multicentre RCT that compared conventional fluoroscopy to 2D/3D-navigated fluoroscopy.19,28,30 Tables 4 and 5 summarize the findings in the included papers. The conventional and navigated groups utilized 135 and 156 screws, respectively, considering all included studies. Screw misplacement was defined as any cortical breach in all included studies. The navigated group had a higher accuracy rate (88% vs. 76%). However, the complication (5.1% vs. 5.7%) and revision (5% vs. 5.7%) rates were similar between the conventional and navigated groups.
Accuracy, complication, and revision rates in Conventional Fluoroscopy Vs Navigated fluoroscopy in SD.

Discussion
With the advances in surgical imaging, manipulative reduction techniques, and increased experience, percutaneous Sacroiliac (SI) and trans sacral fixation has seen a widespread dissemination in use and now represent a staple technique in managing sacral fracture. Arguably, no patient group has benefited from such minimally invasive methods as patients with sacral fractures as these methods are reliable and safe in managing most stable and unstable fractures.7,8 However, the significant variation in posterior pelvic anatomy owing to SDM represents one of the most difficult obstacles in standardizing a fixation protocol. This review aimed to highlight such a common and detrimental variable in managing sacral fractures.
Since Routt et al. first described the qualitative characteristics of dysmorphic sacra, several other studies have investigated the prevalence and determinants of SDM in the general population. 11 Depending on how SDM is defined in available literature, the prevalence of SDM is variable, ranging from 10 to85%.13,26 Studies using a qualitative definition, defined SDM based on the presence of the qualitative characteristics of SDM as described by Routt et al. on radiography and CT. Quantitative definitions, however, are based on whether a trans-sacral screw can be safely placed in the upper sacral segment. SDM prevalence was higher using qualitative criteria since most required the presence of one sign to label a sacrum as dysmorphic. However, the prevalence in the quantitative group also ranged from 11 to 32% since there is no clear consensus on the cut-off for a “safe” corridor diameter for trans-sacral screw placement. The safe cut-off in majority of the studies was defined as an S1 corridor diameter of >10 mm, while 40% considered a 7.5-mm diameter to be a safe cut-off. However, all these studies were radio-anatomic papers. Also, having only a 0.2-mm margin to safely place a 7.3-mm screw, although clinically feasible, requires the use of sophisticated navigated systems and tremendous experience. 40
Few studies have investigated if any of the qualitative dysmorphic signs were more predictive of SDM as it pertains to a safe sacral screw at S1. Weiglet et al. concluded that the presence of a residual disk space at S1, which was the most prevalent sign (70%) in their study group, is significantly associated with a smaller available sacroiliac joint surface and thus a higher risk of screw misplacement. 13 However, Lee at al., who studied the effect of LSTV on the available surgical corridor, concluded that the presence of LSTV and four sacral neuronal foramina increased the safe zone at S1 while decreasing it at S2. 24 In an attempt to provide a more objective definition for SDM, Kaiser et al. proposed a sacral dysmorphism score. 23 It is based on the axial and coronal angulation of S1 on CT scans [(S1 coronal angle) X 2(S1 axial angle)]. The higher the score the less likely a transverse S1 screw was feasible with no safe screw possible if the score was >70. This was further validated by Teo et al.. 30
Regardless of prevalence and definition, SDM has a detrimental effect on the available surgical corridor compared to normal sacra. Dysmorphic sacra have a smaller OFP at S1, with a compensated increase in the available OFP at S2 and S3. These changes require adapting a new strategy in managing sacral fractures. This becomes more evident in managing unstable sacral fractures in which, routine iliosacral screw fixation is associated with the risk of implant failure and residual deformity.41,42 In such cases, trans-sacral screws have been proposed as a more robust technique for managing unstable sacral fractures. 7 In dysmorphic sacra, however, the more cephalad and anterior position of the upper sacral segments in relation to the iliac crests makes a trans-sacral screw at S1 impossible in most cases. To overcome this, it has been proposed that an increased OFP in both S2, and even S3 in certain cases, can be utilized for placing trans-sacral screws.7,22,36 Few reports have shown that the increase in the OFP at S2 in dysmorphic sacra was able to accommodate two trans-sacral screws.7,10 This becomes of importance as more reports are showing an increased rate of implant failure when utilizing a single trans-sacral screw in vertical shear fractures. 43 However, the quality of S2 and S3 screws have been questioned considering the reported decreased BMD at these levels. 27 Radley et al. investigated the BMD at different sacral levels and found that, similar to normal sacra, a dysmorphic S2 was 28% less dense compared to a dysmorphic S1. Moreover, a dysmorphic S1 was less dense compared to a normal S1. 26 This highlights the importance of maximizing fixation at S1 before considering fixation at other levels.
Considering the narrow corridor for screw placement and the proximity of neurovascular structures, different intra-operative navigated systems have been proposed as guides for “safer” screw placement as opposed to conventional fluoroscopy. A systematic review that compared CT-navigated systems and 2D/3D-navigated fluoroscopy to conventional fluoroscopy concluded that the screw misplacement rate was significantly lower in the CT group (0.1%) compared to conventional fluoroscopy (2.4%) and 2D/3D-navigated fluoroscopy (1.3%). However, there was no significant difference in complication and revision rates between the groups. 44 Moreover, there are few studies that consider SDM as a variable that might affect screw placement accuracy. Among the available data, mixed results exist regarding the optimal imaging modality. Matityahu et al. conducted a multicentre RCT that compared conventional fluoroscopy to 2D- and 3D-navigated systems in dysmorphic sacra and concluded that 3D navigation had a higher accuracy compared to 2D navigation and conventional fluoroscopy. However, complication and revision rates were unreported. 19 On the other hand, Berger-Groch et al. and Teo et al. concluded that there was no significant difference between conventional and 2D/3D-navigated fluoroscopy regarding accuracy, complication, and revision rates.28,30
Strengths and limitations
This scoping review has several factors that contributed to its strength and quality. First, a research librarian with expertise in the area designed the search strategy and conducted the search. Additionally, all the articles were independently screened by two reviewers who had expertise regarding both content and methodology. Finally, to the best of our knowledge, this scoping review is the first to assess SDM. Despite these strengths, our scoping review was limited by the restriction of our search to published literature. This may have introduced publication bias into our results as it is possible that a higher proportion of studies with neutral or negative results were unpublished compared to positive ones. Additionally, the heterogeneity of the study design and interventions introduced challenges with respect to capturing all of the details of each included study.
Conclusion
SDM represents consistent yet atypical ‘‘safe zone’’, sizes, and angles that require careful pre-operative and intra-operative analysis combined with technique alterations when placing upper and second sacral segment screws. Fixation should be maximized in S1 in the form of iliosacral screws prior to fixation in other levels. This should be combined with a trans-sacral screw at S2 and, when anatomically feasible, at S3 especially in the setting of unstable sacral fractures. Considering the limited availability, high cost, and mixed results, navigated imaging systems represent a promising technique that requires more rigorous research into its efficacy before widespread adoption.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
Each author certifies that his institution waived approval for the reporting of this investigation and that all investigations were conducted in conformity with ethical principles of research. Investigation performed at Division of Orthopaedic Surgery, Department of Surgery, McMaster University, Hamilton, ON, Canada
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
