Abstract
Introduction
Total hip arthroplasty (THA) is one of the most common and successful orthopedic operations for the treatment of hip disease. It can significantly eliminate hip pain, restore hip function and substantially improve quality of life. 1 The main clinical indications to perform a THA are pain and a reduced range of motion of the hip joint. Patients with osteoarthritis (OA) comprise 87% of all indications for THA. 2
As for all surgical procedures, THA presents a risk of complications such as infection, aseptic loosening, Trendelenburg gait, leg length discrepancy, periprosthetic fractures, or dislocation of the joint. The risk of dislocation is the highest in the first few months after surgery. 3 In primary THA, the incidence of joint dislocation ranges between 0.3% and 10%, but in revision THA this can even go up to 28%. 3 Most dislocations are isolated events and can be treated non-operatively; however, some cases will require hip revision surgery to prevent recurrent dislocations and are performed in approximately one-third of the patients after dislocation following THA. 4
There are different surgical approaches for THA, without a particular predisposition given the current literature.5,6 Although the posterolateral approach is still the most frequently used approach, the direct anterior approach (DAA) is gaining popularity. 7 In the DAA, the hip joint is replaced with reduced soft tissue trauma, theoretically reducing the risk of dislocation.8,9 Alternatively, the supine positioning may allow for better cup inclination and anteversion.10,11 In the literature, however, there is no consensus on which surgical approach has the lowest risk of dislocation. Throughout the literature, both a lower12,13 and higher14,15 dislocation rate have been reported for the DAA compared to other approaches. However, regardless of the surgical approach that is used, the incidence of dislocation was low in these studies.12,14,15 Given the inconsistent results regarding dislocation rates, aggregated evidence is desired. Therefore, we performed a systematic review with meta-analysis to assess (a) the risk of dislocation for different surgical approaches and (b) the relative risk of dislocation of the DAA compared to other surgical approaches, for patients after THA.
Materials and methods
This study was conducted using methods from the Cochrane Handbook 16 and in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) 2020 statement. 17 The study protocol was registered on PROSPERO (registration ID: CRD42019121619).
Search strategy
Six electronic databases (PubMed, Embase, Central, Cochrane Library, PEDro, and Trip) were searched on 11 January 2022. The search strategy (Appendix 1) was developed in consultation with an information specialist and combined search terms for three major themes: ‘total hip arthroplasty’, ‘dislocation’, and ‘approach’. Key terms were mapped to controlled headings and expanded to include free-text terms, as appropriate for the specific database. Since we aimed to observe the modern DAA technique and current component sizes, the search was limited to studies published since 2009. Grey literature was also assessed through Greylit and OpenGrey. After the removal of duplicates, three reviewers (MK, AL and JB) independently reviewed all studies on title/abstract and subsequently reviewed eligible studies in full text using RAYYAN. 18 Furthermore, references of included studies were manually searched for additional studies. Disagreement on eligibility was resolved amongst the reviewers and consensus was reached on the inclusion and exclusion of all studies.
Study selection
A study was included if it (a) was a randomized controlled trial (RCT) or prospective observational study, (b) included adult participants undergoing primary THA because of osteoarthritis, (c) reported data on dislocation, and (d) – in case of an RCT – compared DAA with another approach. Studies were excluded if they (a) were retrospective or (b) included patients with other operation indications than osteoarthritis. Furthermore, only studies written in English, German, French, Spanish, and Dutch were included.
Methodological quality
Methodological quality of the included studies was independently graded with the Cochrane risk of bias (RoB) 2.0 tool 19 for RCTs and with the Methodological Index for Non-Randomized Studies (MINORS) criteria 20 for the prospective observational studies. The level of evidence was determined using the Grades of Recommendation Assessment, Development and Evaluation (GRADE) approach. 21
Data extraction
All data were collected in Excel 365 (Microsoft Corp., Redmond, USA). From each study, we extracted the following information: first author, publication year, country, study design, number of patients (per group), sample characteristics, surgical approach, and follow-up length. Then, we extracted the main clinical outcome and the number of dislocations.
Statistical analysis
Statistical analysis was performed using the ‘meta’ package in R version 1.4.1717 (R Foundation for Statistical Computing, Vienna, Austria). First, we calculated the overall mean dislocation rate using a single proportion meta-analysis. Subgroup analyses were performed based on the surgical approach. Then, the relative risk (RR) of dislocation for the DAA compared to other surgical approaches was calculated by means of meta-analysis for binary outcome data. Random-effect models were used. All tests were two-sided, and significance was attributed to a p-value of <0.05. Results of the meta-analyses are presented in forest plots. Finally, a funnel plot was created to visually assess for publication bias.
Results
Study selection and characteristics
The initial search yielded 868 records. After removal of duplicate studies, 703 studies remained. Another 594 studies were excluded based on their titles and abstracts, 11 reports could not be retrieved, thus 98 studies were read in full. Subsequently, 87 were excluded because they failed to meet the inclusion criteria. In the end, 11 studies were included in this systematic review and meta-analysis: eight RCTs and three prospective observational studies. Details of the study selection are presented in Figure 1.
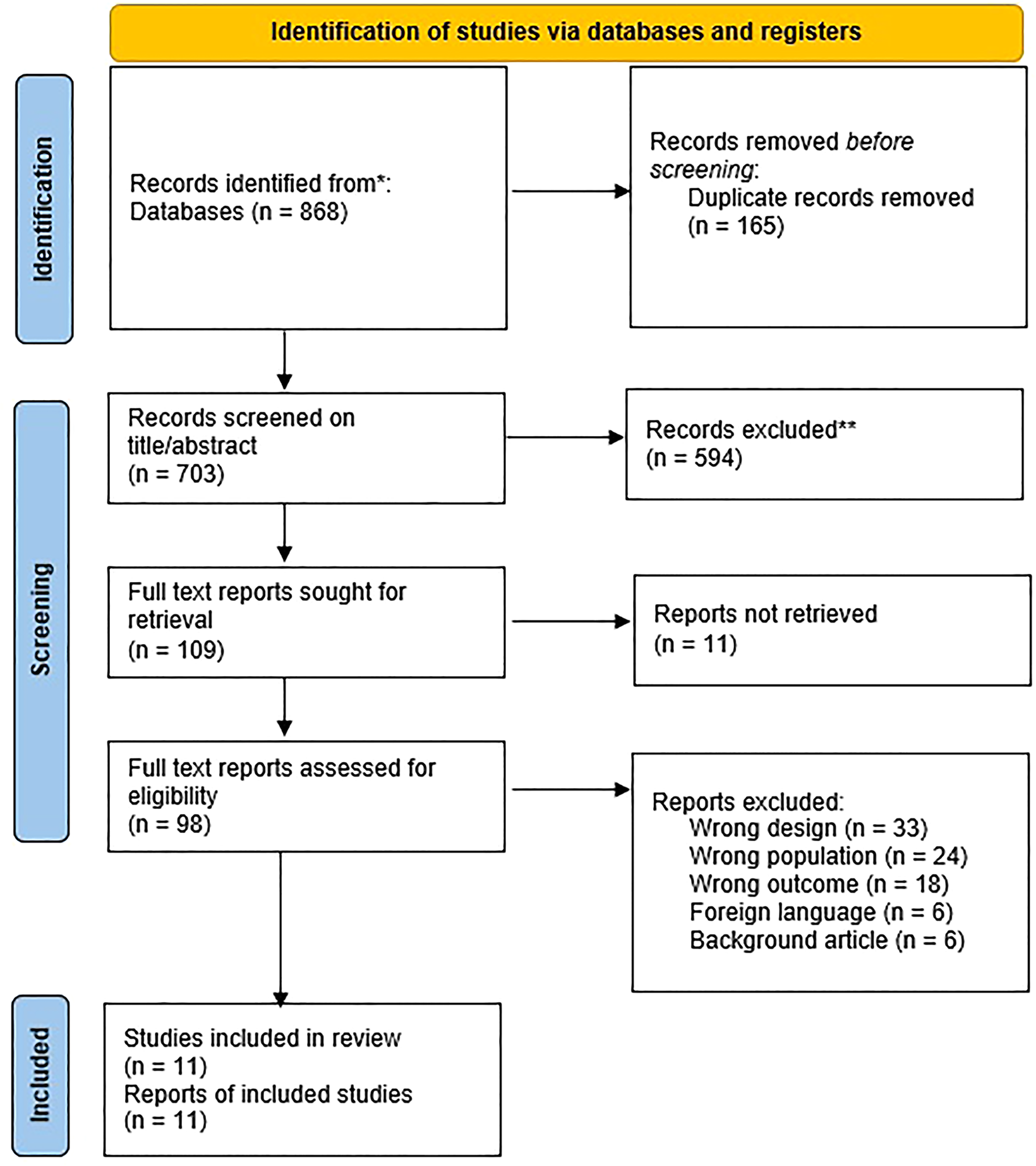
PRISMA flowchart of study selection.
There were no indications for publication bias, as can be observed in the funnel plot (Figure 2).
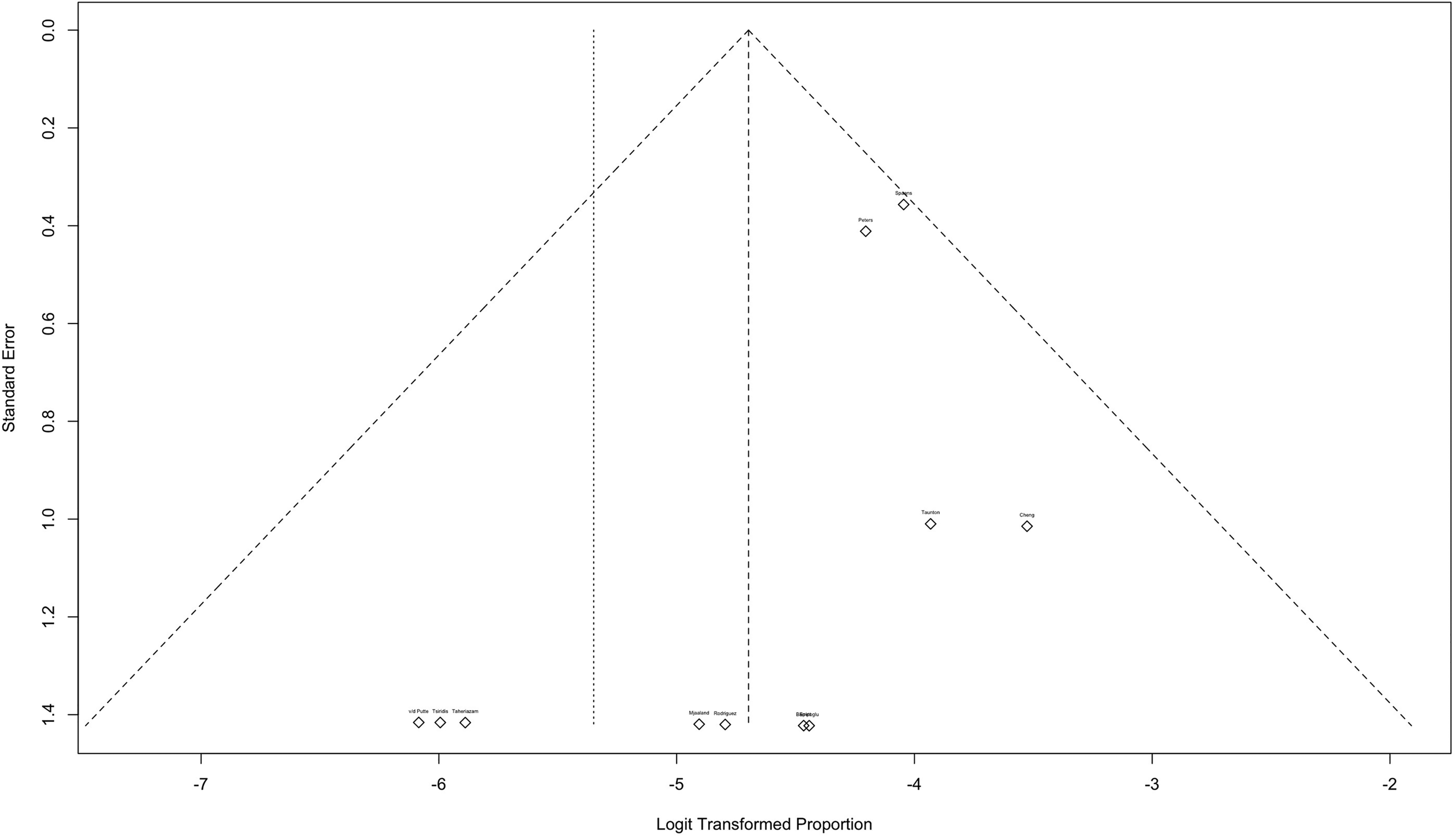
Funnel plot of included studies.
The included studies included a total of 2025 patients, involving 1306 in the posterior subgroup (respectively presented as 189 posterior (PA), 917 posterolateral (PLA), and 200 direct superior (DSA)), 476 direct anterior (DAA), and 243 direct lateral (LA; Table 1). Four of the eight RCTs were considered as prospective observational because the contrast within the study was not the surgical approach. For these studies,10,22–29 subgroups of patients were merged to conduct the appropriate meta-analysis. Accordingly, all studies were included in the meta-analysis to determine overall mean dislocation, whereas only four RCTs30–33 were analyzed to determine the RR of DAA compared to other approaches.
Study and participant characteristics of included studies.
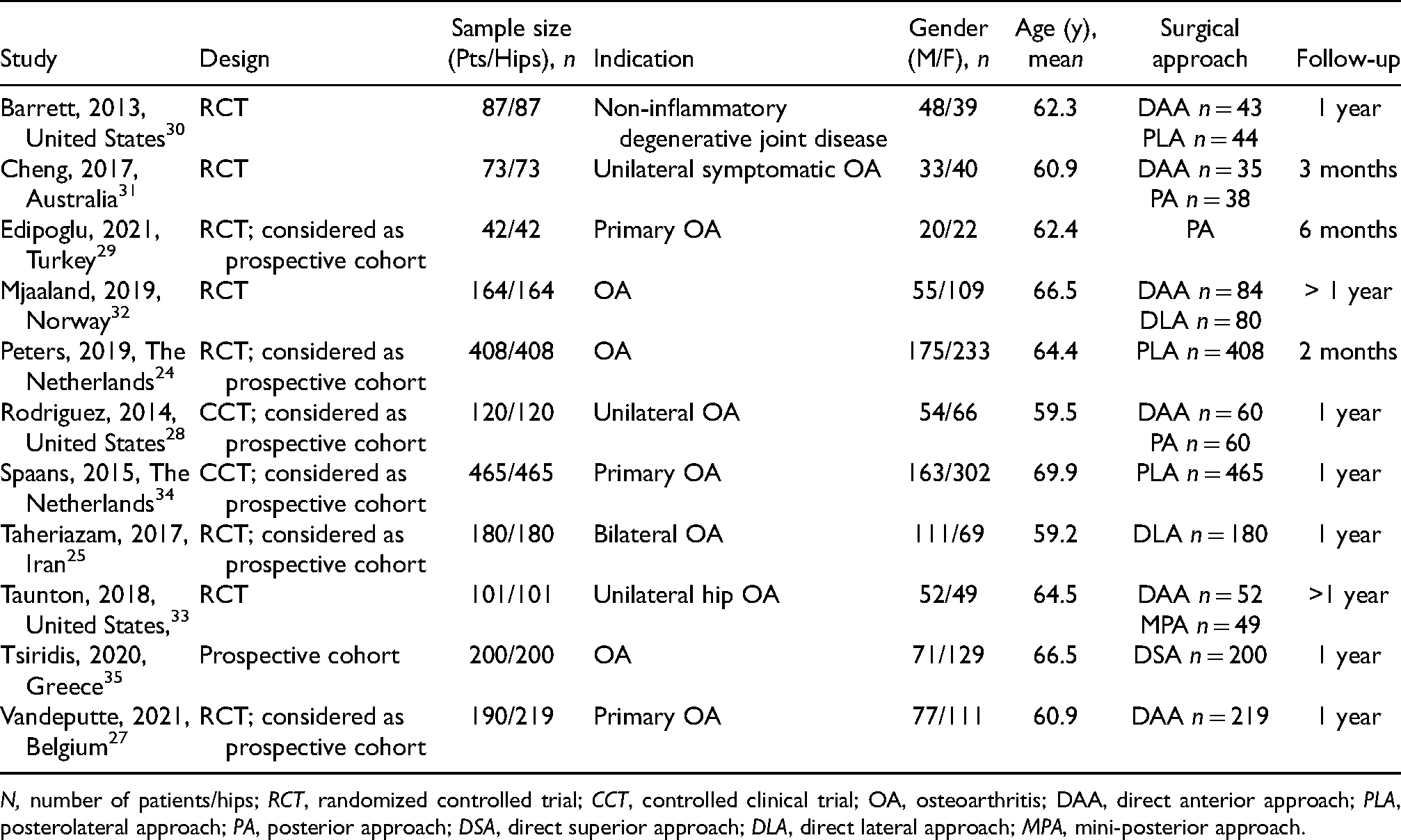
N, number of patients/hips; RCT, randomized controlled trial; CCT, controlled clinical trial; OA, osteoarthritis; DAA, direct anterior approach; PLA, posterolateral approach; PA, posterior approach; DSA, direct superior approach; DLA, direct lateral approach; MPA, mini-posterior approach.
Quality
Summary of methodological quality appraisal is provided in Appendix 2, all four RCTs30–33 showed an overall low risk of bias. For the prospective observational studies, or considered as, the quality scores ranged from 6 to 14 out of 16 with a mean score of 11.1 ± 2.9 (70% of maximum), according to the MINORS criteria (Appendix 3). Using the GRADE approach, the overall level of evidence was rated as low, mainly based on broad confidence intervals.
Dislocation rate
A total of 2025 patients were included with a mean age of 64.6 years, 44% male, and a mean follow-up of 10.5 months (range 2–24). The overall dislocation rate was 0.79% (95% CI 0.37–1.69). Subgroup analyses showed that the most dislocations were in the posterior approaches group (18 dislocations/1306 patients, 1.38% (95% CI 0.87–2.18)). There were no significant differences between subgroups of the surgical approach (p = 0.42; Figure 3).
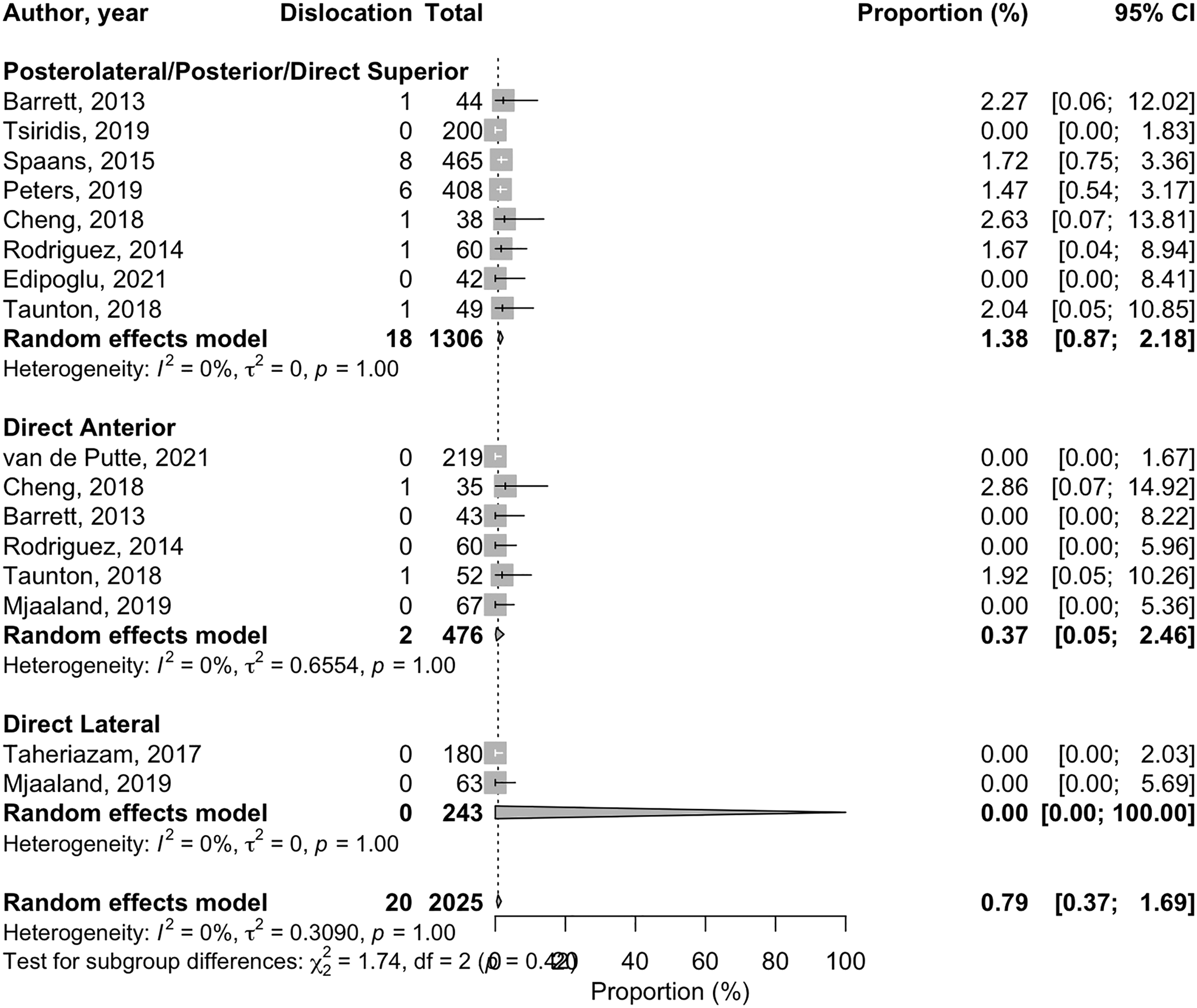
Forest plot of surgical approach subgroup analysis.
Relative risk of dislocation in the direct anterior approach
An RR of 0.75 (95% CI 0.14–3.93) was observed in favour of the DAA (Figure 4). However, this difference was not statistically significant (p = 0.85).
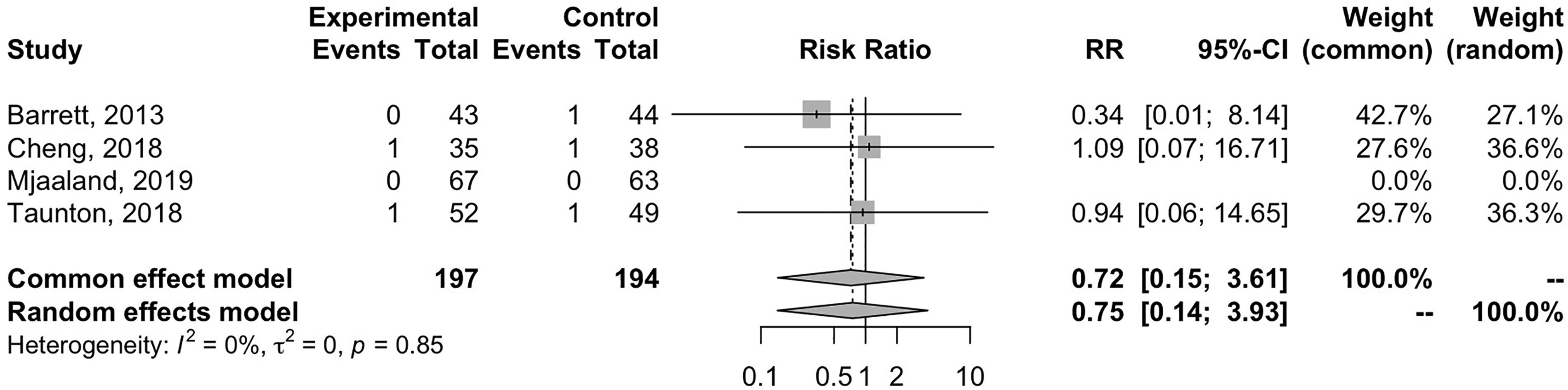
Forest plot of risk ratio DAA vs. other surgical approaches.
Discussion
The main findings of this systematic review with meta-analyses were that the posterior approaches group for THA provides the highest risk of dislocation (1.38%), whilst the direct anterior approach emerges with a non-significant lower risk of dislocation (RR 0.37) compared to other surgical approaches for THA. In 2025 patients treated with primary THA for osteoarthritis, the overall dislocation rate was 0.79%. It should be noted, however, that the overall level of evidence was rated as low.
When reviewing the literature on complications amongst different approaches for THA, most recent studies report no differences in major postoperative complications between various approaches. Gazendam et al. 5 found no significant differences in dislocation between the anterior, posterior, or lateral approaches. Unlike the present study, their network meta-analysis focused on RCTs but observed similar results. Another systematic review by Miller et al. 6 showed an RR of 0.65 (95% CI 0.44–0.95) in favor of the DAA compared to the PA. They only assessed these two approaches, without making further distinctions, but the inference is similar. Docter et al. 36 showed a similar RR of 0.66 (95% CI 0.56–0.77), demonstrating that the direct anterior approach has a significantly lower risk of dislocation compared to the posterior approach. However, retrospective cohort studies were also included in their study. Since these studies had the largest samples, they received more weight in their meta-analysis. Huerfano et al. 37 showed a non-significant difference in dislocation between the DAA and PA, however, they also included retrospective studies in their meta-analysis, and included all surgical indications. Miller et al. 6 and Docter et al. 36 did not include the DSA, but it appears to be a promising technique based on the findings, and literature is emerging.35,38 Above all, the risk of dislocation following THA is generally low according to recent literature. Nonetheless, all reviews show a similar trend, namely that the DAA for THA has a low risk of dislocation compared to other surgical approaches, although non-significant.
Dislocation risk may differ between subgroups of patients based on certain characteristics. Indeed, Gausden et al. 39 showed that more dislocations occur in females and also in people with older age. A population-based study by Hermansen et al. 40 also reported a higher risk of dislocation in patients older than 75 years, and the same was observed in a registry study by Peters et al. 24 These characteristics could not be weighted in this review because the dislocations are not specifically reported in terms of characteristics, but may have influenced the observed RR. For example, Barrett et al. 30 had a less favorable male/female ratio in the PA group, potentially leading to an overestimation of the RR in favor of the DAA compared to the PA. Regarding age, we found the largest age difference between treatment groups in the study of Cheng et al. 31 However, although the PA group had higher age, the difference (3.2 years) was rather small thus overestimation of the RR would be minimal. Most studies included in this review included patients of the same age category (elderly), making risk assessment less biased by age. Furthermore, as this age group is representative of patients receiving THA due to severe osteoarthritis, 2 the current results are clinically relevant.
Besides patient-related characteristics, other factors could also influence the risk of dislocation, such as the surgeon's experience, component size, or patient positioning. Kyriakopoulos et al. 41 indicated that several studies showed both significant and non-significant differences in other complications such as intraoperative fractures in the DAA, depending on the surgeon's learning curve. They did not mention the combination of dislocation and learning curve, but it could be interesting to know whether the experience of the surgeon plays a role in the risk of dislocation in the various surgical approaches. In recent years, larger component sizes like femoral head diameter are being used, 42 which can have a decreasing risk of dislocation since larger component sizes naturally provide more stability to the joint. Furthermore, the use of intraoperative fluoroscopy in recent years for more accurate component positioning may decrease the risk of dislocation for several approach techniques. 43 Regarding patient positioning, approaches that are being performed in a supine position allow for better inclination and anteversion within previously established safe zones, therefore minimizing dislocation risk. 10 On the other hand, the use of a traction table does not seem to affect this risk. 44 Lastly, the included studies were performed in different countries. Whether the risk of dislocation is influenced by different specialist care and rehabilitation protocols is unclear, almost all included studies were conducted in Western countries and therefore comparability is likely.
There are limitations to this review. First, selection bias may be present owing to certain exclusion criteria. We excluded retrospective studies due to their low level of evidence, and only included studies performed from 2009 onwards, due to compare the new DAA technique including modern used component sizes. Despite possible bias resulting from this decision, the results of this review are more useful for today's clinical care as only currently applied surgical techniques were included. Furthermore, some studies were excluded based on the language criteria, making the results more relatable to the Western clinic. Another limitation is the variability amongst the length of follow-up between the included studies. Some studies reported the timing of the complication, but most reported only the final follow-up lengths, which ranged from 2 to 24 months. Subgroup analysis for follow-up length had no added value because only two studies24,31 reported a follow-up length of 3 months or less. However, dislocations are known to occur most frequently within the first 3 months after surgery, with around 70% in the first month. 45 Finally, including prospective observational studies reduced the level of evidence compared to only including RCT studies. However, the amount of high-quality comparative RCTs assessing dislocation risk for the DAA was limited. A strong point of this review, however, is that prospective data was used in combination with a clear outcome measure, preventing the risk of misclassification.
Conclusions
In conclusion, this systematic review with meta-analysis showed no difference between surgical approaches in view of the risk of postoperative dislocation. The choice of approach is determined by a risk-benefit analysis, and recommendations for this analysis regarding the risk of dislocations cannot be made based on the present review. The overall level of evidence for this review, as qualified by GRADE, was low. More high-quality large RCTs are needed to further identify the effects of the surgical approach technique on the risk of postoperative dislocation of the hip joint. Furthermore, to perform a subgroup analysis, important parameters such as surgical experience and the primary indication to perform THA should be recorded per subgroup.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Appendix 1. PubMed search

| # | |
|---|---|
|
|
Hip Dislocation [Mesh] |
|
|
hip dislocat*[tiab] OR hip displac*[tiab] OR hip dysplas*[tiab] OR disloc*[tiab] |
|
|
#1 OR #2 |
|
|
Arthroplasty, Replacement, Hip [Mesh] |
|
|
total hip arthroplast*[tiab] OR THA[tiab] OR total hip replacement*[tiab] OR hip prosthesis implantation*[tiab] OR arthroplasty hip replacement*[tiab] OR hip replacement arthroplast*[tiab] |
|
|
#4 OR #5 |
|
|
Approach*[tiab] OR posterior approach*[tiab] OR anterior approach*[tiab] OR anterolateral approach*[tiab] OR lateral approach*[tiab] |
|
|
#3 AND #6 AND #7 |
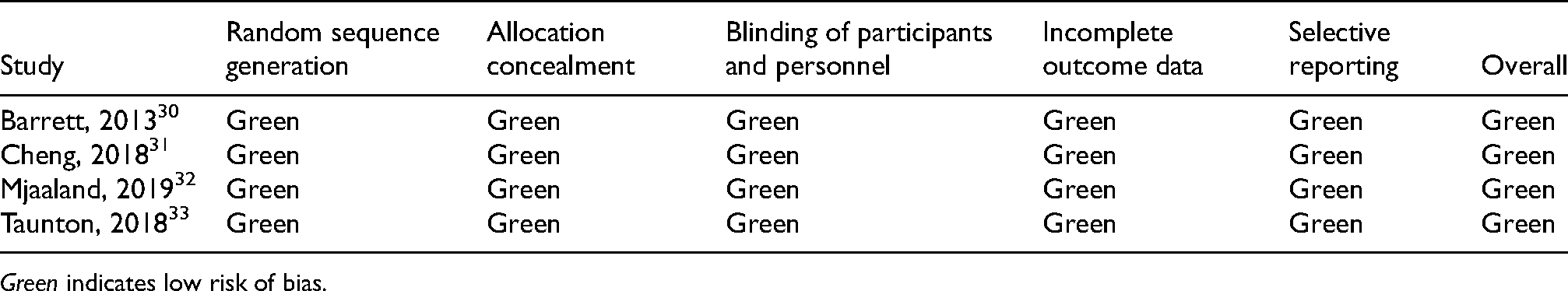
Appendix 2. Risk of bias summary (RoB 2.0 tool) for randomized controlled trials
| Study | Random sequence generation | Allocation concealment | Blinding of participants and personnel | Incomplete outcome data | Selective reporting | Overall |
|---|---|---|---|---|---|---|
| Barrett, 2013 30 | Green | Green | Green | Green | Green | Green |
| Cheng, 2018 31 | Green | Green | Green | Green | Green | Green |
| Mjaaland, 2019 32 | Green | Green | Green | Green | Green | Green |
| Taunton, 2018 33 | Green | Green | Green | Green | Green | Green |
Green indicates low risk of bias.
Appendix 3. Risk of bias summary (MINORS criteria) for non-randomized prospective studies
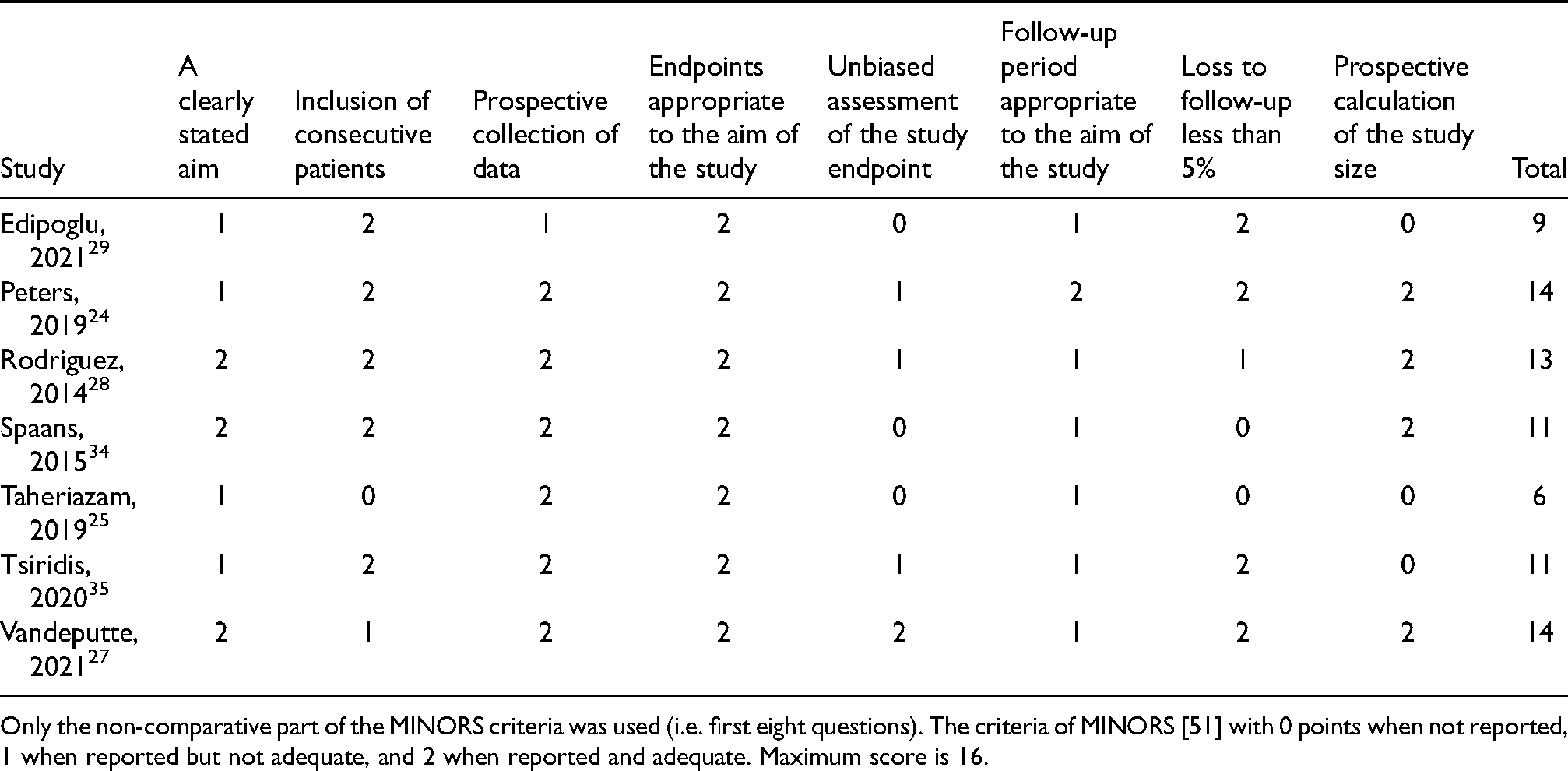

| Study | A clearly stated aim | Inclusion of consecutive patients | Prospective collection of data | Endpoints appropriate to the aim of the study | Unbiased assessment of the study endpoint | Follow-up period appropriate to the aim of the study | Loss to follow-up less than 5% | Prospective calculation of the study size | Total |
|---|---|---|---|---|---|---|---|---|---|
| Edipoglu, 2021 29 | 1 | 2 | 1 | 2 | 0 | 1 | 2 | 0 | 9 |
| Peters, 2019 24 | 1 | 2 | 2 | 2 | 1 | 2 | 2 | 2 | 14 |
| Rodriguez, 2014 28 | 2 | 2 | 2 | 2 | 1 | 1 | 1 | 2 | 13 |
| Spaans, 2015 34 | 2 | 2 | 2 | 2 | 0 | 1 | 0 | 2 | 11 |
| Taheriazam, 2019 25 | 1 | 0 | 2 | 2 | 0 | 1 | 0 | 0 | 6 |
| Tsiridis, 2020 35 | 1 | 2 | 2 | 2 | 1 | 1 | 2 | 0 | 11 |
| Vandeputte, 2021 27 | 2 | 1 | 2 | 2 | 2 | 1 | 2 | 2 | 14 |
Only the non-comparative part of the MINORS criteria was used (i.e. first eight questions). The criteria of MINORS [51] with 0 points when not reported, 1 when reported but not adequate, and 2 when reported and adequate. Maximum score is 16.
