Abstract
Background/Purpose
The purpose of this study was to compare the joint awareness and knee function after unicompartmental knee arthroplasty (UKA) and total knee arthroplasty (TKA) for the management of isolated medial compartment osteoarthritis.
Methods
Patients who underwent UKA or TKA at our institution for isolated medial compartment osteoarthritis from 2015 to 2020 with a minimum follow-up of 1 year were screened. 116 eligible patients were invited and 94 volunteer patients participated. All patients were evaluated with The Forgotten Joint Score-12 and Lysholm Knee Scale.
Results
Average follow-up period was 29.13±15.48 months for UKA and 31.66±2.91 months for TKA groups (p=0.292). FJS-12 of the UKA group was significantly higher than that of the TKA group (79.74±15.06 and 63.25±19.86, respectively; p=0.024). The Lysholm Knee Scale score was also significantly higher in the UKA group compared with the TKA group (92.94±8.74 and 78.34±14.99, respectively; p = 0.002).
Conclusion
Our findings suggest that patients who underwent UKA were less aware of their artificial joints and had better knee function compared to patients who underwent TKA for medial osteoarthritis of the knee.
Keywords
Introduction
Unicompartmental (UKA) or total knee arthroplasty (TKA) are successful surgical options used to reduce pain and improve function in patients with isolated medial knee osteoarthritis.1,2 However, there is still a discrepancy regarding optimal arthroplasty surgery options, but both TKA and UKA approaches are logical and have self-supporting data. 3
One of the primary goals of joint arthroplasty is to restore the natural feel of the joint. However, reducing joint awareness is a complex process that requires comprehensive consideration of the physical and psychological perception of a foreign object in the novel joint. 4 Joint awareness has recently been introduced as a patient-reported outcome concept that allows distinguishing patients with high functional levels and little or no pain. 5 Evaluation methods for postoperative outcomes of joint arthroplasty generally focus on objective clinical evaluations such as postoperative activity, quality of life, complication and revision rate, but the ability to forget the artificial joint in daily life can be considered the ultimate goal in joint arthroplasty, which results in the highest patient satisfaction. 6
Due to the potential benefits of UKA in functional outcomes and the ongoing debate about postoperative residual complaints following TKA, interest in comparing UKA with TKA has recently increased. Also, the current literature has only shown an insufficiency of outcome studies in which the Forgotten Joint Score-12 is considered. 2 Therefore, the aim of the present study was to compare joint awareness and knee function in patients who underwent TKA or UKA after isolated medial knee osteoarthritis.
Methods
Patients who underwent UKA or TKA for isolated medial compartment osteoarthritis from 2015 to 2020 were screened from the local university hospital registry system. A total of 116 eligible patients were called and invited to participate in this study, and 94 volunteer patients participated. The study was approved by the Clinical Research and Ethics Committee of the authors’ affiliated institution (approval no. 19.03.2019/06). Informed consent was obtained from all patients.
The inclusion criteria were as follows; having undergone unilateral UKA or TKA surgery due to isolated medial compartment primary osteoarthritis at least a year ago and having age >45 years. Exclusion criteria were as follows; the presence of anterior knee pain and pre-operative Kellgren-Lawrence grade III–IV of the lateral or patellofemoral compartments, bilateral knee arthroplasty, rheumatoid arthritis, malignancies, revision surgery, post-surgical infection, history of prior knee surgery and body mass index (BMI) > 40 kg/m2.
Surgical technique
All the operations were performed by the same surgeon using the same brand and type of prosthesis through 8–12 cm of longitudinal medial parapatellar approach. Patients received fixed bearing UKA (Unicompartmental High Flex Knee, Zimmer-Biomet Inc., Warsaw, Indiana 46,580, ABD), and high viscosity polymethyl methacrylate (PMMA) bone cement (Oliga- G21 srl-Vias. Pertini, 8- 41,039 San Possodonio (MO)-Italy) or posterior stabilized fixed bearing TKA (NexGen Legacy®, Zimmer-Biomet Inc., Warsaw, Indiana, USA), and high viscosity polymethyl methacrylate bone cement (Oliga-G21 srl-Via S.Pertini, San Possidonio (MO), Italy). All the operations were performed without using tourniquet.
Evaluations
Demographic (age, gender, education, occupation) and clinical data (BMI, average follow-up of period, dominant and operated extremity) of all patients were recorded.
Forgotten Joint Score-12 is a recently developed scoring system that assesses how natural the prosthesis feels after total joint arthroplasty. The scale assessing patients’ awareness of the joint during different activities of daily living. It consists of 12 questions with a five-point Likert format (0–4) and the total sum score is converted into a scale ranging from 0 to 100, with a higher score indicating a more natural or forgotten joint. 5
Lysholm Knee Scale is an 8-item tool that evaluates knee joint pain, instability, locking, swelling, limping, climbing stairs, squatting, and the need for walking support. Total score ranges from 0 to 100 and higher scores indicates better knee function. 7
Statistical analysis
The data was analysed using SPSS 24.0 (IBM Corp. Released 2016. IBM SPSS Statistics for Windows, Version 24.0. Armonk, NY: IBM Corp.) package program. Continuous variables were given as mean±standard deviation and categorical variable values are presented as absolute numbers (n) and percentages (%). Normality of data distribution was assessed by the Shapiro-Wilk test The data was not normally distributed. Mann-Whitney U test was used to compare the groups. Spearman's correlation coefficient was used to assess the correlation between Forgotten Joint Score-12 and Lysholm Knee Score. The statistical significance level was set as p<0.05.
Results
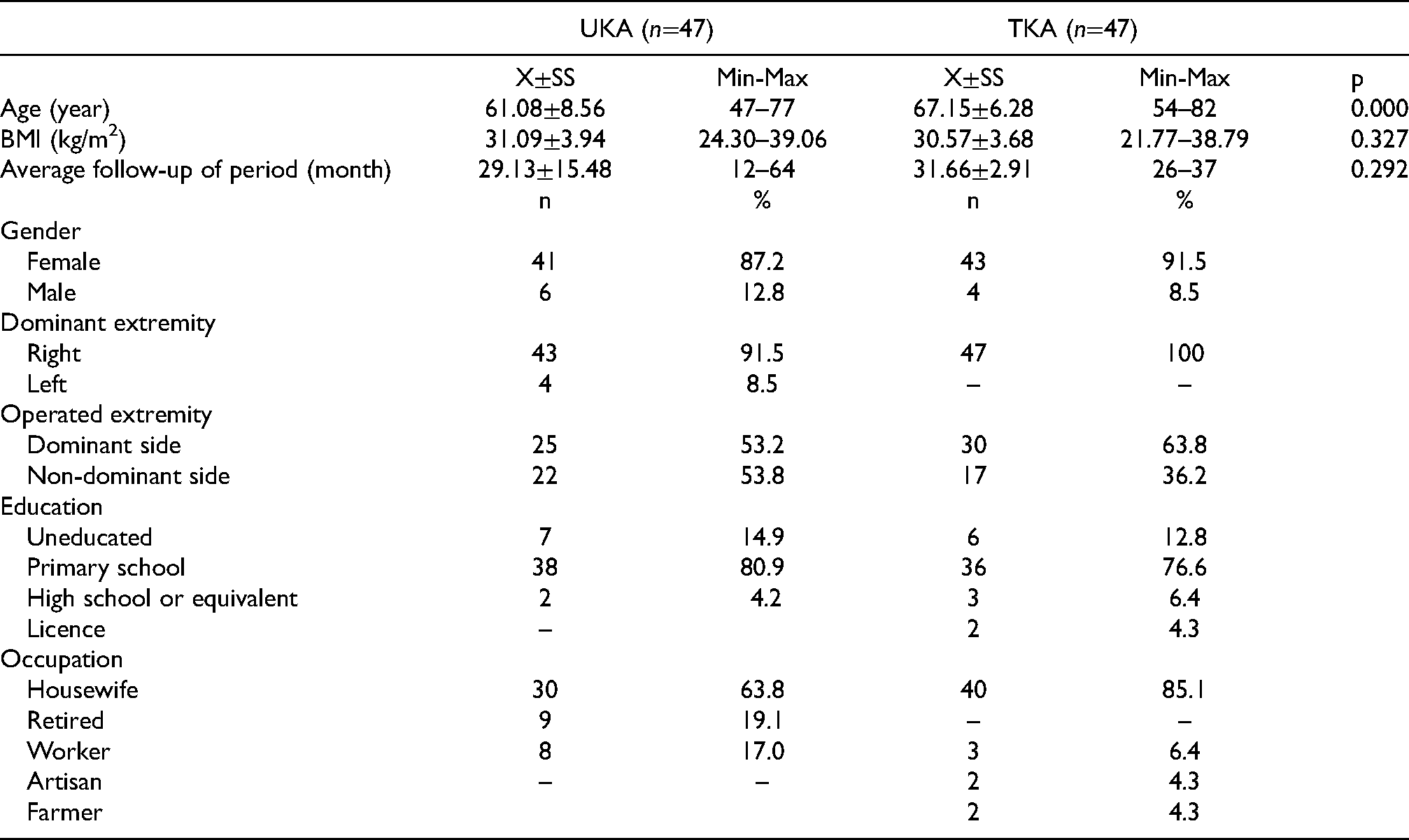
The UKA group consisted of 47 patients (mean age, 61.08±8.56 years; 41 women and 6 men) and TKA group consisted of 47 patients (mean age, 67.15±6.28 years; 43 women and 4 men). Average follow-up period was 29.13±15.48 months for UKA and 31.66±2.91 months for TKA groups (p=0.292). 25 (53.2%) patients from UKA and 30 (63.8%) from TKA group underwent dominant-side total knee arthroplasty surgery. Descriptive characteristics of patients are provided in Table 1.
Demographic characteristics of the groups.
The comparison of clinical outcome scores of the groups is shown in Table 2. Forgotten Joint Score-12 and Lysholm Knee Score of the UKA group were statistically significantly higher than TKA group (p≤0.001).
Comparison of Forgotten Joint Score-12 and Lysholm Knee Score of the groups.
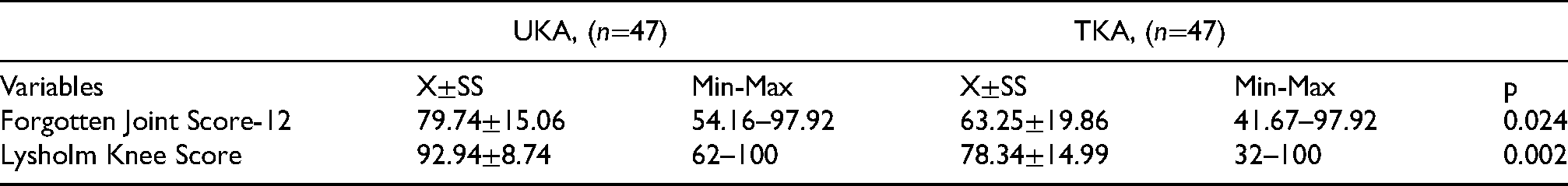
The relationship between Forgotten Joint Score-12 and Lysholm Knee Score is presented in Table 3. There was no correlation between Forgotten Joint Score-12 and Lysholm Knee Score in both groups (p>0.05).
Correlations between Forgotten Joint Score-12 and Lysholm Knee Score.

Discussion
Evaluation of joint feel after joint arthroplasty has become spreading focus of measurement in recent years, and the main finding of our study was that the UKA patients feel the artificial knee joint more natural than TKA patients. In addition, UKA patients had better knee function than TKA patients. There was no relationship between knee joint feels and knee functions in both groups.
A recent meta-analysis presented that UKA patients are better able to forget their artificial joints compared to TKA patients. According to the results the difference in joint awareness in UKA and TKA patients is maximum at 6 months, and this may decrease over time and reach a minimum level in 2 years. Therefore, the evaluation of joint awareness in 2 years can accurately reveal the artificial joint perception of the patients. 8 Our study shows that UKA patients (79.7) are better able to forget their artificial joints in an average of 2.5–3 years of follow-up compared to patients who underwent TKA (63.2). The results of this study are in correspond well with those obtained by studies with similar follow-up period in the literature. Thienpont et al. 9 found better Forgotten Joint Score-12 with UKA compared to TKA, although there was no statistically significant difference (76.4 vs. 73.2, p=0.4356). However, Zuiderbaan et al. 10 (74.3 vs. 59.8, p=0.004), Kim et al. 11 (67.3 vs. 60.6, p=0.011), Fabre-Aubrespy et al. 12 (93.9 vs. 88.6, p<0.0001), Blevins et al. 13 (90.5 vs. 79.5, p<0.0001) documented significant differences in Forgotten Joint Score-12 between UKA and TKA patients. A high Forgotten Joint Score-12 score indicates how the individual is of his/her joints awareness were little during activities of daily living. In other words, there are no significant subjective disorders such as pain, instability, or limitation of range of motion in the joint, and therefore the joint can be considered forgotten. 9 Although the reasons for a more natural joint feeling in UKA compared to TKA are not known, UKA surgery preserves more soft tissue and bone, possibly preserving proprioceptive fibres, may be among the reasons why these patients are less aware of their artificial joints in daily life.10,11
Meta-analysis results comparing UKA and TKA in terms of knee function differ from past to present. Arirachakaran et al. 14 reported that there was no difference in postoperative function, but in a very recent meta-analysis, Deng et al. 15 showed that UKA effectively improved knee function more than TKA at early and mid-term follow-up, with no significant difference in postoperative revision rate. Therefore, researchers recommended UKA instead of TKR in patients with late-stage isolated medial knee osteoarthritis. Although UKA had better postoperative knee function than TKA in our study, we could not find a relationship between knee function and joint awareness. However, joint awareness is one of the issues to be considered in gaining a high level of activity in young patients with high expectations.11,16 In this respect, UKA is advantageous in terms of enabling patients to forget the joint more, and it was also supported in our study that knee functionality increased. The reason why we could not detect a relationship may be the size of the population.
The present study has some limitations. Many factors such as preoperative variables including functional status suggested affecting postoperative outcomes were not included in the current analysis. Although the preoperative demographic outcomes differed significantly only in an age in this study, comparison with the age-matched group in further studies may be more accurate for patient-reported outcomes interpretation.
Conclusion
In conclusion, we found that patients who underwent UKA were less aware of their artificial joints in daily life and had better knee function compared to patients who underwent TKA for medial osteoarthritis of the knee. These findings may provide useful information for surgeons counselling patients considering TKA or UKA for the treatment of isolated medial compartment osteoarthritis.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
