Abstract
Study Design
Rat subjects were randomly assigned to control, local, and systemic esomeprazole groups (n = 4-6 per group).
Objective
Excessive scar formation after laminectomy can cause nerve entrapment and postoperative pain and discomfort. A rat laminectomy model determined whether topical application and systemic administration of esomeprazole can prevent epidural fibrosis.
Methods
Laminectomy alone was performed in the control group. Topical esomeprazole was introduced to the laminectomy area in the local esomeprazole group. Intraperitoneal esomeprazole was introduced in the systemic esomeprazole group following laminectomy. Macroscopic and histopathologic examinations were performed four weeks after laminectomy.
Results
In the systemic esomeprazole group, the macroscopic epidural fibrosis score was less than the control group (P < 0.001). Microscopic epidural fibrosis score and fibroblast cell density classification scores in local and systemic esomeprazole groups did not significantly differ. Fibrosis thickness was significantly lower in the local and systemic esomeprazole groups compared to the control group (P < 0.01, P < 0.001, respectively).
Conclusions
Esomeprazole reduced the formation of epidural fibrosis in the rat laminectomy model.
Introduction
Epidural fibrosis (EF), the excessive proliferation of fibrous tissues in the epidural space, is a common complication associated with laminectomy. 1 Often leading to symptoms that include pain, nerve root compression, and inflammation, it reduces the quality of life and potentially results in failed back surgery syndrome. Reduced tissue cellularity and excessive extracellular matrix deposition contribute to the etiopathogenesis of EF. 2 Reparative inflammation, exceptionally severe cicatrization, and adhesions resulting from the fibrotic process all contribute to the pathogenesis of EF. 3 Transforming growth factor β (TGFβ) production is another key mechanism initiating EF formation.4,5
Proton pump inhibitors (PPIs) are primarily used for treating peptic ulcers and gastroesophageal reflux disease; they also possess anti-inflammatory and anti-oxidative properties. 6 Esomeprazole is a PPI with well-known anti-inflammatory, antioxidant, and antiapoptotic properties.7,8 Many previous studies have also shown that esomeprazole has antifibrotic activity.9-11
Given esomeprazole’s antioxidant, anti-inflammatory, and anti-apoptotic activity and the fact that it has been shown to suppress TGFβ and fibroblasts and to show anti-fibrotic activity, we hypothesized that esomeprazole may also play a therapeutic role in EF. In this study, we investigate the possible action of esomeprazole in attenuating EF after laminectomy in rats. We hypothesize that systemic and local application of esomeprazole could limit the extent of EF and contribute to better post-operative outcomes. The results of our investigation may provide novel insights into strategies to prevent EF, enhancing the quality of life for patients undergoing laminectomy.
Materials and methods
Experimental Animals
This study, which obtained approval from the University of Health Sciences’ regional animal research ethics committee (20.11.2020, 06.09), adhered strictly to the European Union Council Directive (86/609/EEC) of November 24, 1986 addressing the protection of animals used in studies. The study followed all the directives of animal care and testing. A total of 18 female Sprague Dawley rats, each weighing between 150 and 250g, were the subjects of the experiment. They were housed under optimal conditions with a 12-hour light cycle, controlled humidity, and temperatures maintained between 22 and 25°C. They had unrestricted access to food and water throughout the experiment.
These animals were randomly divided into three groups for the study:
Laminectomy Group (n = 6)
The rats underwent the laminectomy procedure described below. After ensuring adequate hemostasis at the site of surgery, no topical or systemic medication was administered. The subjects were euthanized 30 days post-surgery using the detailed procedures.
Local Esomeprazole Group (n = 4)
Following laminectomy and hemostasis, these rats received a topical application of esomeprazole (30 mg/kg) directly to the dura at the laminectomy site. The process was finished once it was established that the applied solution was on the field for at least five minutes. The subjects were euthanized 30 days post-surgery.
Systemic Esomeprazole Group (n = 6)
These rats underwent laminectomy with no post-surgical topical treatment. A single intraperitoneal dose of 30 mg/kg of esomeprazole was given immediately after the operation. The subjects were euthanized 30 days post-surgery. The dosage of esomeprazole was obtained from a previous study. 10
Surgical Procedure
To prevent infection, each rat received an intramuscular 20 mg/kg sodium cephazolin injection before surgery. Intraperitoneal injections of 50 mg/kg ketamine (Ketalar, Parke Davis, Turkey) and 10 mg/kg xylazine (Rompun, Bayer, Turkey) induced anesthesia. Rat body temperatures were maintained at 37°C using a heating pad and a rectal probe.
The rats were placed in a supine position during surgery. Their lower backs were shaved, the surgical sites were cleaned with povidone and a sterile field was established. A midline incision was made over the L1-L3 levels and laminectomy at the L2 level then exposed the dura mater and epidural spaces, with careful removal of the ligamentum flavum and epidural fat tissue. Topical treatments were applied in the relevant groups and the wounds were sutured with 4-0 prolene polypropylene sutures. The same surgeons meticulously carried out each surgery under a surgical microscope to protect the neurological structures (BG, PKB).
Post-surgery, the rats had unrestricted access to food and water for four weeks. Euthanasia was performed via cervical dislocation following an intraperitoneal injection of 50 mg/kg ketamine (Ketalar, Parke Davis, Turkey). The laminae, dural sacs, nerve roots, and paravertebral tissues, along with the muscles and skin, were excised from the first to the third vertebrae.
Macroscopic Assessment of Epidural Fibrosis
A neurological surgeon blind to the treatment groups carefully re-opened the surgical sites and macroscopically evaluated the existing epidural fibrosis according to the Rydell classification, 12 which includes four distinct grades based on scar tissue adherence to the dura mater and the difficulty of dissection. The details of Rydell classification scoring were published recently. 13
Histopathological Evaluation
For histological analysis, the laminectomy region was separated by cutting the upper L1 to lower L3 levels of the spine axially. Pathology procedures were published previously. 13 For histological analysis, the samples were immersed in a 10% buffered formalin solution. The specimens were separated into 2-3 mm thick axial slices and then preserved in formalin for 48 hours. A decalcification solution (BiocalC, Code: RRDC3/G, Specifications: EDTA1%, Pot. Sod. Tartate1%, Sodium Tartate1%, Hydrochloric acid1%, Biostain-U.K.) was used to decalcify each tissue sample for 72 hours. Hematoxylin and eosin (H&E, Shandon Harris Hematoxylin-Eosin Y -UK) and Masson trichrome (Bio-Optica special stains kit, Milan, Italy) were used to stain serial slices that were four μm thick after a paraffin-embedded block was prepared from formalin-fixed, paraffin-embedded tissues. Bozkurt et al. 14 ’s parameters for the microscopic assessment of EF were used to assess the extent of inflammation, scar tissue formation, fibrosis, and other histological changes. The classification scheme for fibroblast cell density was published recently. 13
Statistical Analysis
GraphPad Prism 8.0 (GraphPad Software Inc, La Jolla, CA, USA) was used for data analysis. A one-way analysis of variance was used to examine the variations between the groups, followed by a Tukey posthoc test. The threshold for statistical significance was a P value of 0.05.
Results
Wound Healing and Complications Related to the Procedure
In the local esomeprazole group, 2 unfortunate instances of mortality were recorded. As the dosage was arranged accordingly and even no slight systemic symptoms were observed in other animals in this group, we speculate that these instances may have been caused by animal-related reasons. The local effects of esomeprazole need further investigation to have a conclusion. There were no procedural complications such as hematomas, erythema, infections, or leaks of cerebrospinal fluid reported across all groups. At the time of sacrifice, all animals retained unhindered mobility.
Macroscopic Assessment of Epidural Fibrosis
Severe epidural adhesions were observed in the majority of cases in the laminectomy group (n = 5 grade 3 and n = 1 grade 2). Moderate to severe epidural adhesions were observed in the local esomeprazole group (n = 3 grade 3 and n = 1 grade 2). Only mild to moderate epidural adhesions were observed in the systemic esomeprazole group (n = 3 grade 1, n = 1 grade 2). Notably, the epidural fibrosis severity score was statistically significantly decreased in the systemic esomeprazole group compared to the laminectomy group (P < 0.001). However, no statistically significant difference was found in comparing the local esomeprazole group to the laminectomy group (Figure 1). Macroscopic assessment of epidural fibrosis score of study groups. Data are presented as mean ± SD. Post-laminectomy, severe epidural adhesions were observed in the laminectomy group. (A). Macroscopic epidural fibrosis score decreased significantly in the local esomeprazol group compared with the laminectomy group (***: P < 0.001). (B). The local and systemic esomeprazol group’s fibrosis thickness scores decreased significantly compared with the laminectomy group (**: P < 0.01; ***: P < 0.001). L: local, Lam: Laminectomy, S: Systemic, ESO: Esomeprazol.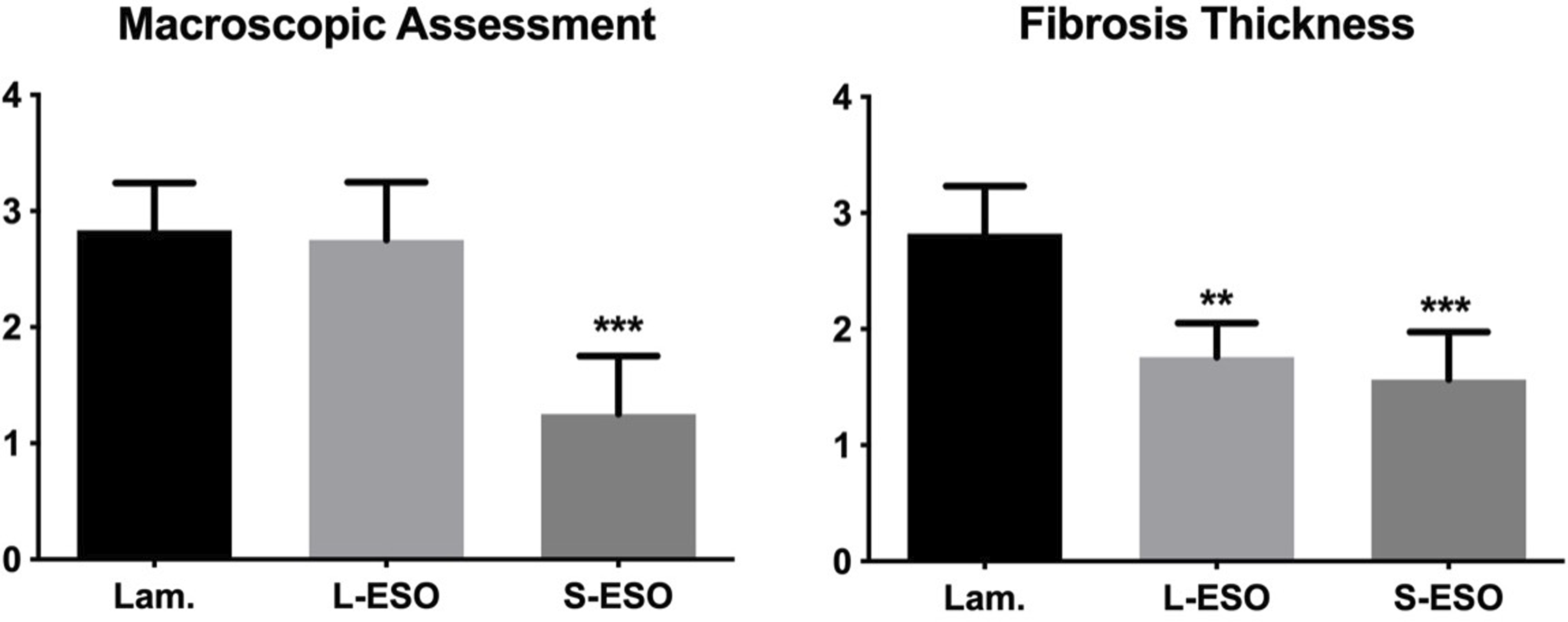
Histopathologic Assessment
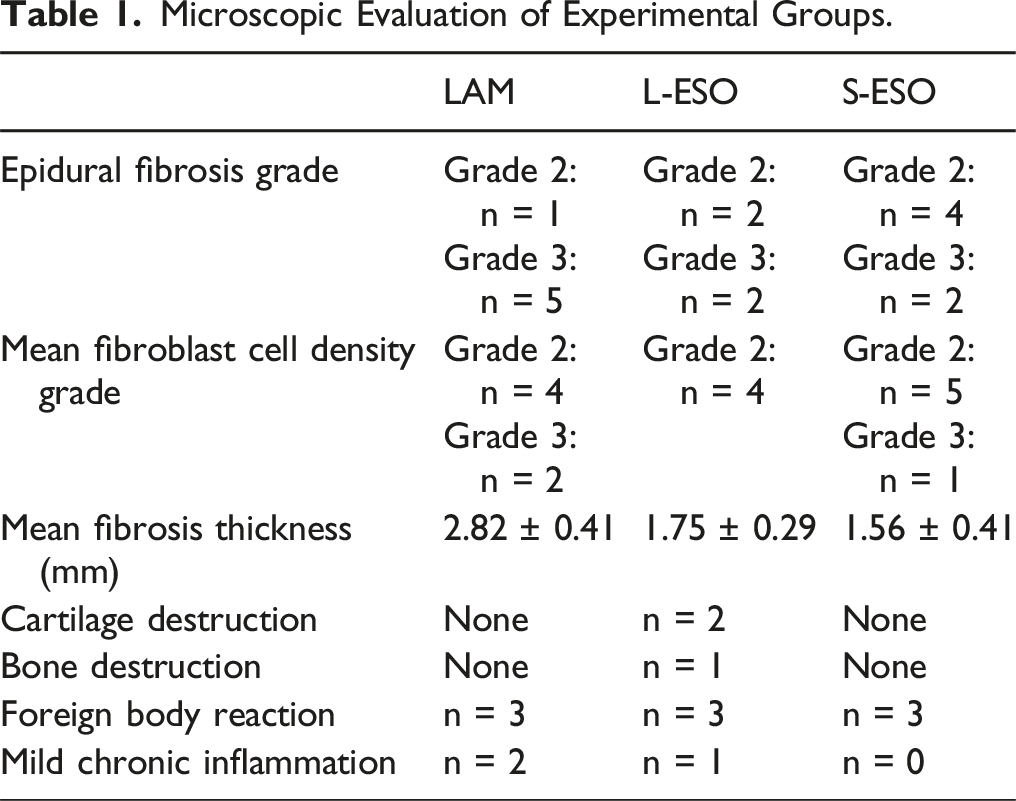
Microscopic Evaluation of Experimental Groups.
Discussion
After laminectomy EF results in physical disability and recurring radicular discomfort due to adherent scar tissue compressing the nerve root. 15 EF procedures have a low success rate and a significant complication rate.16,17 As a result, research on prevention has gained attention and various alternatives to surgical treatment have been investigated.1,13,14,18-21 The major objective is to inhibit the process that causes fibrosis to develop.
The primary contributors to EF development are chemotactic factors, which emerge in the epidural region of patients after laminectomy due to the breakdown of erythrocytes and thrombocytes following bleeding, and fibroblastic cell migration brought on by paraspinal muscles. 22 Dermatan sulfate, fibronectin, and collagen are extracellular matrix components produced by excessively high fibroblast stimulation and proliferative activity. 4 Excessive generation of these components promotes scar tissue development, compressing neural structures. 23
Esomeprazole is a safe PPI that is used effectively in the clinical treatment of peptic ulcer and related diseases. Compared to other PPIs, the molecule is more metabolically stable and more bioavailable. 24 Eltahir et al. 10 demonstrated the reducing effect of esomeprazole administration on TGFβ levels. In reducing the expression of collagen that is triggered by TGFβ, 25 esomeprazole has antifibrotic efficacy. 26 By macroscopic analysis, the current study found that systemic esomeprazole administration lowered EF. In addition, both the local and systemic esomeprazole groups showed a statistically significant reduction in fibrosis thickness scores.
Esomeprazole exhibits acid-suppressing, acid-dependent activity. It is also known to have acid-independent activity and carries anti-inflammatory, antioxidant and anti-apoptotic properties.8-10 When antioxidant properties are compared, esomeprazole demonstrates more effective antioxidant activity than other PPIs. 27 Cho et al. 28 revealed the reducing effect of esomeprazole on TGF-β1 levels. In a randomized clinical study, esomeprazole treatment was found to be effective and well-tolerated for the healing of gastric ulcers who continued daily nonsteroidal anti-inflammatory drug usage.29,30 It was also found to be effective in the treatment of gastroesophageal reflux disease. 31 The beneficial effects of esomeprazole were also noted in erosive esophagitis. 32 Human data is needed for EF.
There are limitations to this study. The small number of animals per group, particularly in the local esomeprazole group, restricts our ability to conclude, as does the fact that we did not conduct biochemical tests. Adding biochemical investigation will strengthen the data and help the researchers to be able to explain the mechanism of action for esomeprazole in EF.
Conclusions
Esomeprazole, well-known for its anti-inflammatory and antioxidant capabilities, arrested the synthesis of EF macroscopically and microscopically. The outcomes of our investigation offer the first experimental proof of esomeprazole’s EF protective effects. (Figure 2). Representative photomicrograph of the epidural fibrosis analysis of the study groups. (A)-(B): The control group exhibits severe epidural fibrosis (Fibrosis score: 3). L: Laminae, F: Fibrosis, SC: Spinal Cord, Arrow: Dura Mater (A) hematoxylin and eosin: H&E, x40. (B) MT: Masson trichrome, x40. (C)-(D): The local esomeprazol group exhibits severe epidural fibrosis (Fibrosis score: 3). L: Laminae, F: Fibrosis, SC: Spinal Cord, Arrow: Dura Mater. (C) H & E, x40, (D) MT, x40, (E)-(F): The systemic esomeprazol group exhibits moderate epidural fibrosis (Fibrosis score: 2). L: Laminae, F: Fibrosis, SC: Spinal Cord, Arrow: Dura Mater. (E) H & E, x40, (F) MT, x40.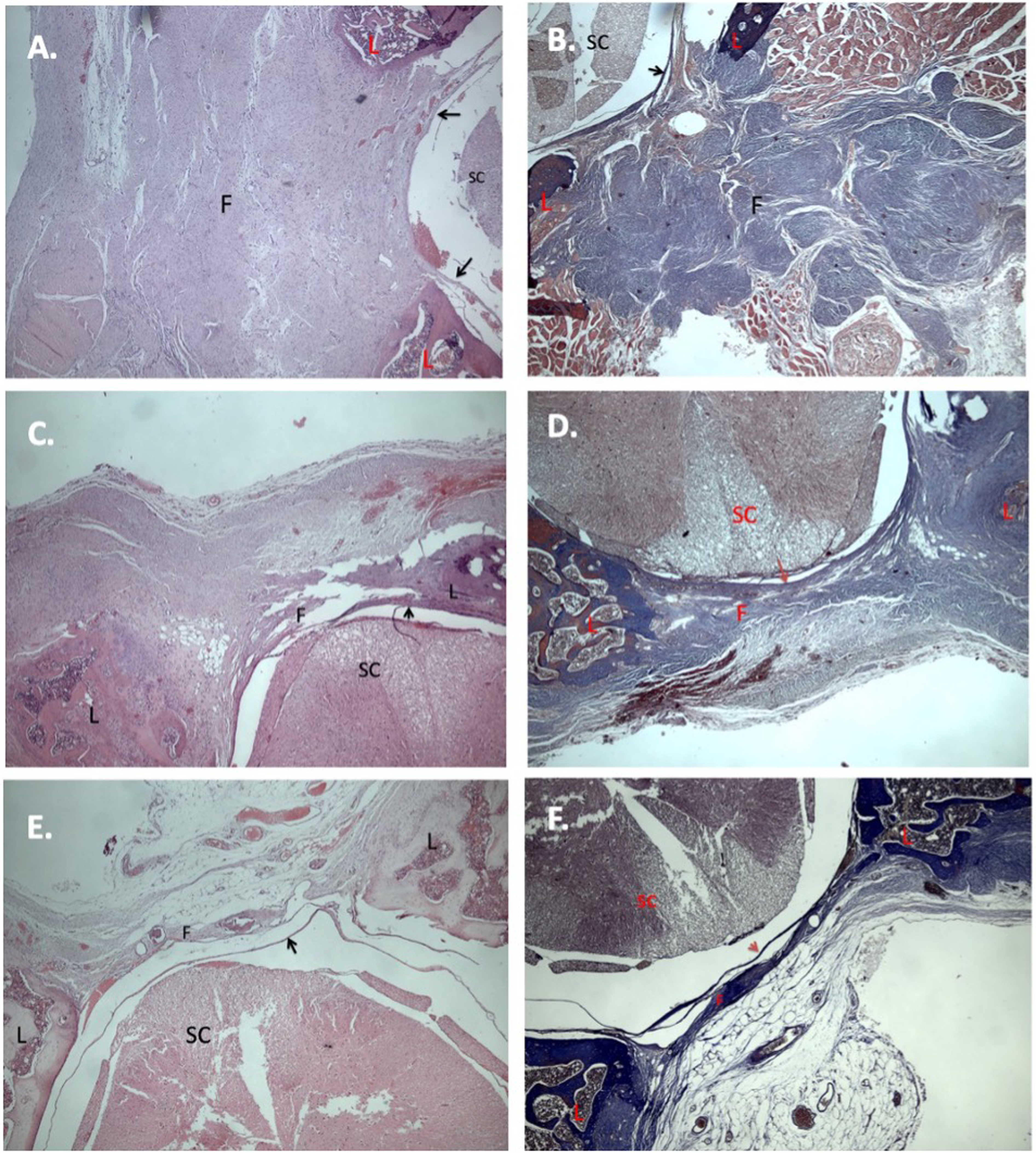
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
