Abstract
Study Design
Cross-sectional survey study.
Objective
To investigate factors affecting decision-making in thoracolumbar burst-fractures without neurologic deficit.
Methods
A 40-question survey addressing expert-related, economic, and radiological factors was distributed to 30 international trauma experts. Descriptive statistics were used to assess the impact of these factors on operative or non-operative management preferences.
Results
Out of 30 experts, 27 completed the survey. The majority of respondents worked at level 1 trauma centers (81.5%) within university settings (77.8%). They were primarily orthopedic surgeons (66.7%) and had over 10 years of experience (70.4%). About 81% found distinguishing between A3 and A4 fractures relevant for decision-making. Most experts (59%) treated A3 fractures non-surgically, while only 30% treated A4 fractures conservatively. Compensation systems did not influence treatment recommendations, and hospital measures promoting surgeries did not significantly affect distribution. Radiological factors, such as local kyphosis (25/27), fracture comminution (23/27), overall sagittal balance (21/27), and spinal canal narrowing (20/27), influenced decisions.
Conclusion
Incomplete burst fractures (A3) are predominantly treated non-surgically, while complete burst fractures (A4) are primarily treated surgically. Compensation, third-party incentives, and outpatient care did not significantly impact decision-making. Radiological factors beyond the AO Spine thoracolumbar classification system seem to be essential and warrant further evaluation.
Keywords
Introduction
Thoracolumbar burst fractures without neurologic deficit are frequent and their treatment still poses a controversy.1–6 The AO Spine thoracolumbar injury classification differentiates between incomplete (A3) and complete (A4) burst type fractures and their possible treatment options.7,8 However, global clinical consensus remains elusive and treatment pathways diverse. This state of equipoise accentuates a critical clinical conundrum that necessitates a nuanced understanding of the multifarious factors influencing therapeutic decisions. Uniquely combining an equipoise study with an expert survey, our research addresses this gap, providing unparalleled insight into the intricate variables steering surgeons’ choices. This blend of expert opinions and empirical data allows a thorough exploration of prevailing uncertainties in treating such fractures, facilitating a closer alignment of clinical practice with evidence-based guidance. The objective of this study was to explore a broad spectrum of factors—encompassing not only radiological considerations but also extending to personal factors such as background, professional training, experience, remuneration, OR availability, hospital setting etc.—that influence decision-making in managing neurologically intact thoracolumbar burst fractures.
Methodology
Employing a meticulously crafted questionnaire, we engaged an international cadre of spine surgery experts (the Equipoise Group who crafted and produced this special issue), dissecting the manifold influences inherent in decision-making processes related to A3/A4 thoracolumbar fractures. The questionnaire was drafted and defined through a discussion process within the AO Spine Knowledge Forum Trauma. This integrative tool was pivotal in unraveling the intertwined elements influencing clinical decisions, offering a panoramic view of the factors steering treatment paths. The survey along with additional insights will be provided as supplemental material to this editorial.
Findings
Expert Group Demographics and Background
A thorough analysis garnered insights from international 27 experts, predominantly stationed at Level 1 trauma centers and immersed in university settings. Most experts exhibit profound experience, with two-thirds being orthopedic surgeons. A significant 80% of these experts have engaged in AO Spine trauma courses. The professional background of the expert group is illustrated in the tables within the supplemental material.
A3 Fractures: Expert Preferences and Influences
Crosstabulation of Therapy Recommendation for A3 Fractures With Annually Treated Fractures.
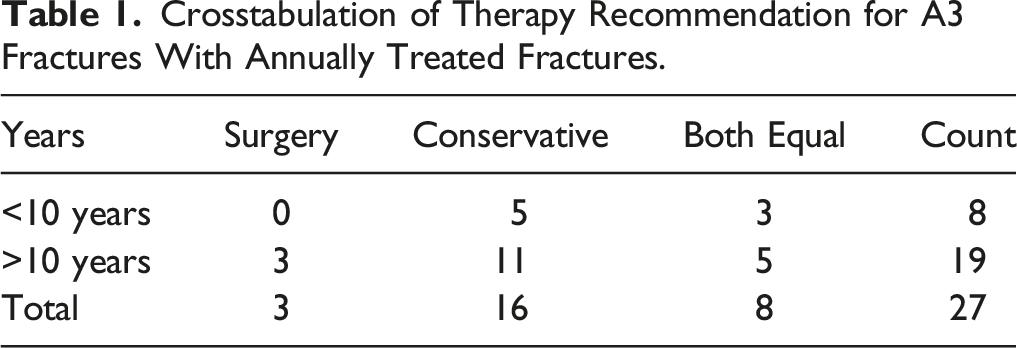
We looked at how different economic factors like the hospital setup, how doctors are paid, and the risks of legal issues might affect treatment decisions for A3 fractures. However, these factors did not change the treatment recommendations. The findings show a steady preference for non-surgical treatments for A3 fractures, regardless of these economic factors.
A4 Fractures: Inclination Towards Surgical Therapy
Crosstabulation of Operation Room Availability and Treatment Recommendation for A4 Fractures.
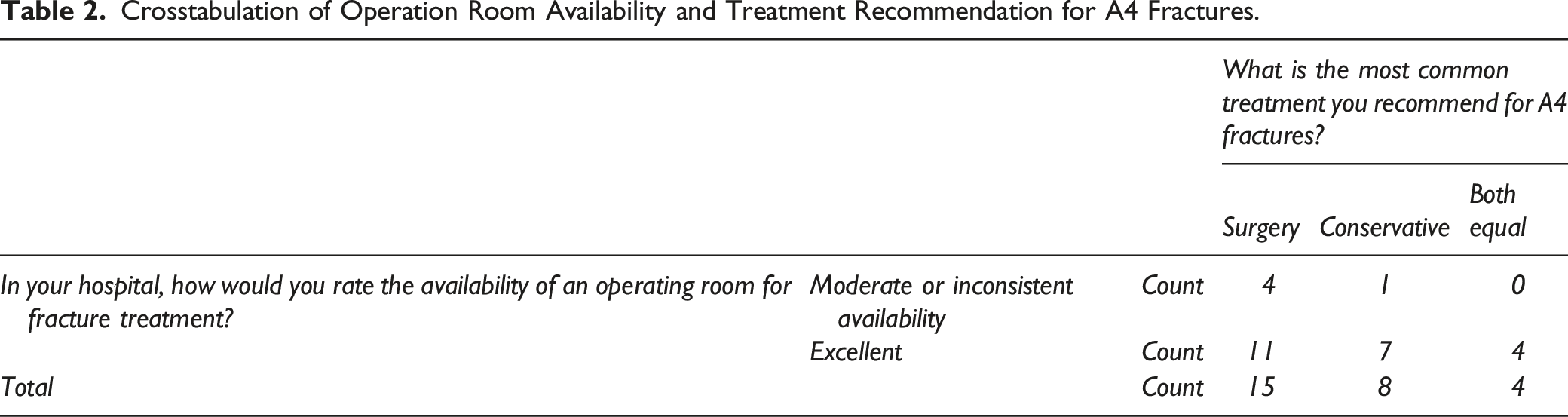

Crosstabulation of Level of Insurance and Treatment Recommendation for A4 Fractures.

Crosstabulation of Perceived Reimbursement and Treatment Recommendation for A4 Fractures.

Radiological Influences: Consensus and Divergences
The differentiation between A3 and A4 fractures was deemed crucial by the overwhelming majority of experts in determining treatment plans. In decisions related to A3 fractures, 81% of experts incorporated considerations for potential long-term complications such as post-traumatic kyphosis and implant failure, though this did not significantly sway the overall distribution of treatment recommendations.
Regarding A4 fractures, 81% of experts expressed that long-term complications like kyphosis or material failure do play a pivotal role in influencing treatment decisions.
Radiological Factors Influencing the Therapy Recommendation for A3 and A4 Fractures.

Conclusion
This study aimed to understand how factors related to clinician expertise, economic interests, and radiological features influence therapy recommendation for AO Spine A3/A4 thoracolumbar fractures without neurological deficit. The majority of experts (81%) found distinguishing between A3 and A4 in neurologically intact patients to be relevant for decision-making. Accordingly, most of the experts (59%) treat A3 fractures without surgery, while only 30% treat A4 fractures conservatively. Most experts are concerned about long-term complications such as implant failure or future kyphosis. Radiological factors, such as local kyphosis, fracture comminution, overall sagittal balance, and spinal canal narrowing strongly influence the treatment decision by the experts, while remuneration pattern does not.
Supplemental Material
Supplemental Material - What Factors Influence Surgeons in Decision-Making in Thoracolumbar Burst fractures? A Survey-Based Investigation of a Panel of Spine Surgery Experts
Supplemental Material for What Factors Influence Surgeons in Decision-Making in Thoracolumbar Burst fractures? A Survey-Based Investigation of a Panel of Spine Surgery Experts by Klaus J. Schnake, Marcel F Dvorak, Cumhur F Öner, Charlotte Dandurand, Sander Muijs, and Sebastian F. Bigdon in Global Spine Journal
Supplemental Material
Supplemental Material - What Factors Influence Surgeons in Decision-Making in Thoracolumbar Burst fractures? A Survey-Based Investigation of a Panel of Spine Surgery Experts
Supplemental Material for What Factors Influence Surgeons in Decision-Making in Thoracolumbar Burst fractures? A Survey-Based Investigation of a Panel of Spine Surgery Experts by Klaus J. Schnake, Marcel F Dvorak, Cumhur F Öner, Charlotte Dandurand, Sander Muijs, and Sebastian F. Bigdon in Global Spine Journal
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was organized and funded by AO Spine through the AO Spine Knowledge Forum Trauma, a focused group of international Trauma experts. AO Spine is a clinical division of the AO Foundation, which is an independent medically-guided not-for-profit organization. Study support was provided directly through AO Network Clinical Research.
Supplemental Material
Supplemental material for this article is available online
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
