Abstract
Study Design:
Systematic literature review with meta-analysis.
Objective:
Thoracolumbar (TL) fractures can be treated conservatively or surgically. Especially, the treatment strategy for incomplete and complete TL burst fractures (A3 and A4, AOSpine classification) in neurologically intact patients remains controversial. The aim of this work was to collate the clinical evidence on the respective treatment modalities.
Methods:
Searches were performed in PubMed and the Web of Science. Clinical and radiological outcome data were collected. For studies comparing operative with nonoperative treatment, the standardized mean differences (SMD) for disability and pain were calculated and methodological quality and risk of bias were assessed.
Results:
From 1929 initial matches, 12 were eligible. Four of these compared surgical with conservative treatment. A comparative analysis of radiological results was not possible due to a lack of uniform reporting. Differences in clinical outcomes at follow-up were small, both between studies and between treatment groups. The SMD was 0.00 (95% CI −0.072, 0.72) for disability and −0.05 (95% CI −0.91, 0.81) for pain. Methodological quality was high in most studies and no evidence of publication bias was revealed.
Conclusions:
We did not find differences in disability or pain outcomes between operative and nonoperative treatment of A3 and A4 TL fractures in neurologically intact patients. Notwithstanding, the available scores have been developed and validated for degenerative diseases; thus, their suitability in trauma may be questionable. Specific and uniform outcome parameters need to be defined and enforced for the evaluation of TL trauma.
Keywords
Introduction
Burst fractures of the thoracolumbar spine account for approximately 45% of all major thoracolumbar injuries. At least half of the patients with thoracolumbar burst fractures maintain full neurological function. 1 In spite of the high incidence of thoracolumbar burst fractures without neurological deficit and the extensive reporting on this topic in the literature, the optimal treatment strategies for this type of injury remain controversial.
Many reviews have compiled information to compare different treatment modalities. Since 2000, reviews and meta-analyses on surgical strategies have been published on fusion versus nonfusion, 2 minimally invasive surgery versus open surgery, 3,4 anterior versus posterior approach, 5 early versus late treatment, 6,7 or looked at a specific treatment types in itself, for example, pedicle screw fixation 8 or surgical treatment in general. 9 Fewer reviews have been published about conservative treatment options, for example, on the usefulness of orthoses. 10,11
Likewise, the amount of reviews with the aim of directly comparing operative to non-operative treatment is scarce. Gnanenthiram et al 12 published a meta-analysis in 2012, which identified 4 comparative primary studies published in 1998, 13 2001, 14 2003, 15 and 2006. 16 A Cochrane review, published in 2006 17 and updated in 2013, 18 focused on randomized clinical trials (RCTs). In the update, 2 primary studies were deemed eligible, 15,16 which were also included in the aforementioned meta-analysis. Another systematic review by Thomas et al 19 in 2006 identified 21 studies of which only half were considered having a quality score of 50% or more. The 7 studies that achieved a quality score of greater than 50% dated from 1993 to 2004 and were presented in greater detail while the majority of the lower quality studies dated from the 1990s.
Ghobrial et al 20 published a review on adverse events related to operative or nonoperative treatment in 2014. In contrast to our review, they excluded noncomparative studies and 63% of the operatively treated patients had a neurological deficit.
None of the aforementioned reviews comparing surgical with nonsurgical treatment narrowed the target population to AO A3 and A4 fractures 21,22 in neurologically intact patients, although these are the most controversial fracture types with regard to treatment. In the AOSpine classification, the A3 type represents an incomplete burst fracture with involvement of the posterior wall but only one endplate, while the A4 fracture, a complete burst fracture, is characterized by an involvement of the posterior wall and both endplates.
General consensus exists that in less severe fractures (A0-A2) conservative treatment has the best risk/benefit ratio and that very severe fractures (B and C type) as well as patients with neurological compromise should be treated surgically. However, no such consensus exists in patients with incomplete (A3) and complete (A4) thoracolumbar burst fractures without neurological deficit. 23,24
The most recent comprehensive systematic review with the aim of determining whether surgical or nonsurgical treatment achieves better results in these fracture types has been performed nearly 10 years ago. 19
Therefore, the purpose of our review was to generate the best available evidence on the clinical outcomes achieved with current operative and nonoperative treatment modalities in A3 and A4 fractures in neurologically intact patients by performing a meta-analysis.
Materials and Methods
Search Strategy
A literature search was performed in PubMed and the Web of Science on April 7, 2015. Since the terminology used to describe thoracolumbar fractures is extremely varied, the search strings were deliberately kept general to avert the risk of missing eligible publications. The search strategy is depicted in Table 1.
Search Strategy.

Study Selection
In order to obtain results with a high reproducibility, the minimum population size per treatment group was set at 20 patients and only A3 and A4 fractures according to the present AOSpine classification, published by Vaccaro et al 21 and Reinhold et al 22 in 2013, were considered. Of note, the definition of A3 fractures according to Vaccaro et al 21 and Reinhold et al 22 is identical to the one of A3.1 fractures and the definition of A4 fractures according to Vaccaro et al 21 and Reinhold et al 22 is identical to A3.2 and A 3.3. fractures according to the previous AOSpine classification, published by Magerl et al 25 in 1994, which got substituted with the present classification in 2013.
Titles and abstracts of the initial matches were independently screened by 2 reviewers to identify potentially eligible primary studies. In cases where the title or abstract did not allow determining eligibility, the full text was obtained in order to make a valid decision. In case of discrepancies, consensus was sought through discussion and in case of doubt, a third reviewer was consulted. Inclusion and exclusion criteria are presented in detail in Table 2. Additionally, the references of reviews and meta-analyses identified in this search were screened for further potentially eligible primary studies.
Inclusion and Exclusion Criteria.

Data Extraction
Information collected included inclusion and exclusion criteria of the respective study, demographic and injury characteristics, treatment details, outcomes concerning clinical, radiological and perioperative parameters, return to activity, adverse events, reoperations, follow-up (FU) time, and the proportion of patients lost to FU. This was completed via a standardized data extraction form.
Whenever comparative studies presented results of several groups and not all groups conformed to the minimum group size of 20 patients, only the group that contained a minimum of 20 patients was included in this analysis.
In case of missing information concerning parameters of interest, for example, outcome mean values at last FU or standard deviations, authors of the respective publications were contacted by email with the request to provide the missing information.
Data Synthesis
With regard to all measured indices of (a) disability and (b) pain, the pooled estimate of standardized mean difference (SMD) and 95% confidence intervals (CIs) were calculated by combining the SMD of each individual study that compared operative and nonoperative outcomes based on the mean, standard deviation, and sample size. SMD for disability was calculated based on the Roland Morris Disability Questionnaire (RMDQ) 26 and the Low Back Outcome Score (LBOS), 27 while pain was calculated based on pain visual analog scale (pain VAS) results. Missing values for standard deviation were imputed based on values from other studies in the analysis. Heterogeneity among studies was estimated by chi-square test and Cochran Q score (reported as I 2 ). An I 2 of 0% denotes no heterogeneity while an I 2 of 100% denotes maximum heterogeneity. The statistical significance level for heterogeneity was set at P < .05. In the presence of high heterogeneity, the random effects model was used. An SMD < 0 favored operative treatment when compared with nonoperative treatment. Publication bias was assessed by Egger’s regression and visual inspection of the funnel plots. The results of the meta-analyses were graphically presented as forest plots. The analysis was performed in the statistical software STATA version 13 (STATA Corp, College Station, TX, USA).
The mean values of clinical outcome parameters that were available for a minimum of 125 patients in both surgical and conservative treatment groups were depicted graphically to give an overview about results that also include the noncomparative studies.
Assessment of Methodological Quality
The quality of all studies was evaluated using a quality assessment tool previously used in similar publications. 19 This tool is based on guidelines suggested by the Cochrane Collaboration Back Review Group 28 and the University of British Columbia Department of Epidemiology “Evaluating Therapeutic Interventions” criteria. It contains 13 questions, which can be scored with “yes,” “no,” “unsure,” or “not applicable.” In prospective studies, 0 to 7 check marks denote a study of poor quality and 8 to 13 check marks indicate a study of good quality. In retrospective studies, 0 to 5 check marks denote a study of poor quality and 6 to 10 check marks indicate a study of good quality. A list of the respective items is given in Table 3.
Questions for Quality Rating According to Thomas et al (2006). 19

Risk of bias of studies directly comparing conservative to surgical treatment was evaluated with the Newcastle-Ottawa Quality Assessment Scale (NOS). 29 This methodological rating scale was originally developed to rate the risk of bias in nonrandomized comparative studies. It rates the methodological quality of the 3 domains “selection,” “comparability,” and “outcome.” The maximum attainable ratings are 4 stars for selection, 2 stars for comparability, and 3 stars for outcome. Rather than defining absolute values denoting the methodological quality level, the authors advise to present the ratings as a visual comparison combined with the target outcomes of each study included in a review. This allows readers to make their own decision on the validity of respective outcomes. 29
Ethical Aspects
No institutional review board approval is needed for systematic literature reviews and meta-analyses.
Results
Eligible Literature
The searches in PubMed and the Web of Science resulted in a total of 1929 matches (Figure 1).
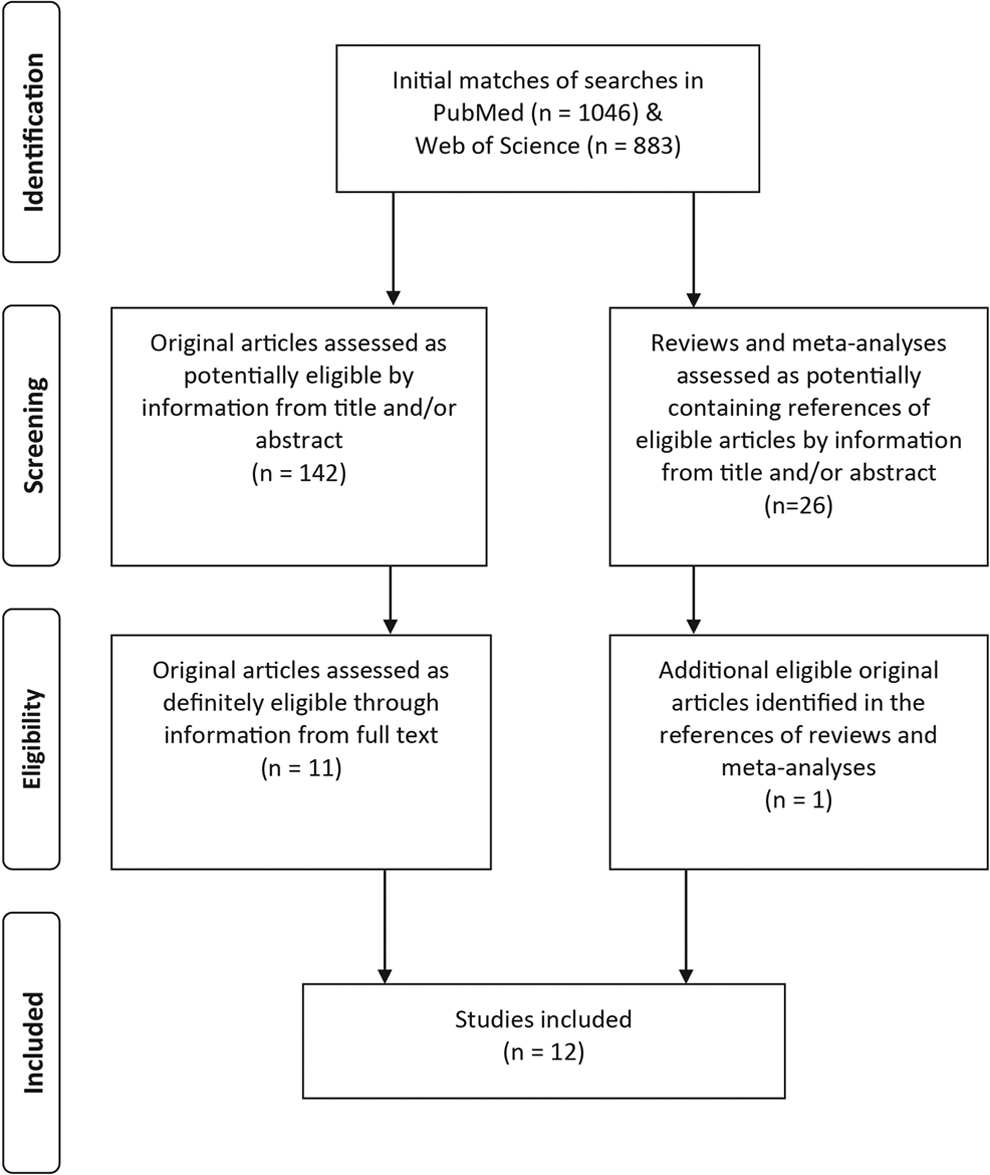
Study inclusion flow diagram.
After screening of titles and abstracts by two independent reviewers, 142 primary studies were considered potentially relevant. After full text assessment, 11 articles were deemed eligible. 14,15,30 –38 Additionally, 26 reviews and meta-analyses were screened for further potentially eligible references, which led to the identification of another primary study. 39
Overall, 4 studies directly compared surgical with conservative treatment. 14,15,33,35
One of them was an RCT. 15 Six additional comparative studies had a different focus, and 3 studies compared different types of surgical treatment. 34,37,38 Another 2 studies compared the outcome of patients with different degrees of injury severity, 31,36 and 1 study, designed as an RCT, compared 2 types of conservative treatment. 30
Finally, 2 case series were identified. One presented results of surgical treatment 39 and the other analyzed results of patients treated nonoperatively. 32
A total of 656 patients were included within these studies. No overlapping patient populations were identified. Overall, studies presented a high heterogeneity with regard to inclusion and exclusion criteria and the level of detail reported, particularly in the parameters used to evaluate treatment success. A summary of study characteristics for baseline data is given in Table 4 and for clinical outcome data in Table 5 and for radiological outcome data in Table 6.
Study Characteristics—Baseline.

Abbreviations: LoE, level of evidence; CT, computed tomography; RCT, randomized controlled trial; ICBG, iliac crest bone graft; SI, sagittal index; pts, patients.
Study Characteristics—Clinical Outcome.
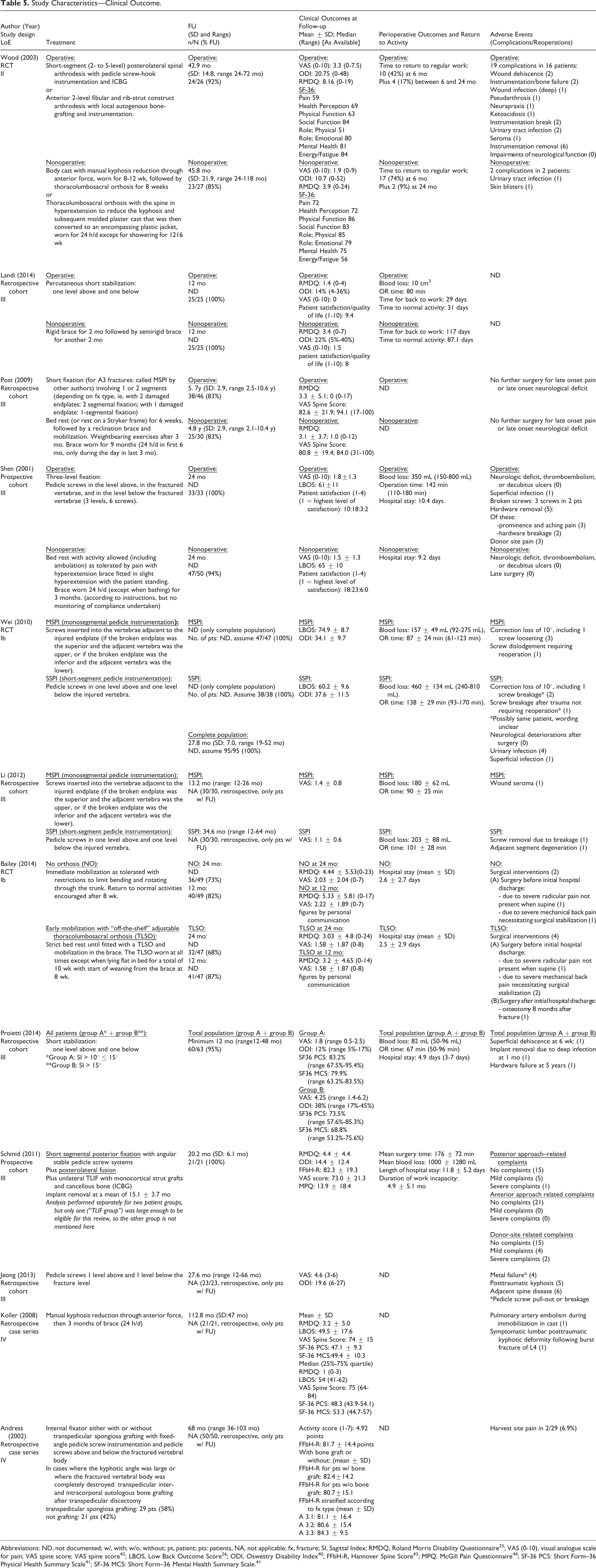
Abbreviations: ND, not documented; w/, with; w/o, without; pt, patient; pts: patients, NA, not applicable; fx, fracture; SI, Sagittal Index; RMDQ, Roland Morris Disability Questionnaire 25 ; VAS (0-10), visual analogue scale for pain; VAS spine score: VAS spine score 42 ; LBOS, Low Back Outcome Score 26 ; ODI, Oswestry Disability Index 40 ; FFbH-R, Hannover Spine Score 43 ; MPQ, McGill Pain Questionnaire 44 ; SF-36 PCS: Short Form–36 Physical Health Summary Scale 41 ; SF-36 MCS: Short Form–36 Mental Health Summary Scale. 41
Study Characteristics—Radiological Outcomes.

Abbreviations; ND, not documented; w/, with, w/o; without, pt, patient; pts, patients; NA, not applicable; fx, fracture, FU, follow-up; SI: Sagittal Index, LSC: Load Sharing Classfication. 53
The major reasons for exclusion after full text screening were (a) the use of a different classification to describe the fracture type, which did not allow to determine whether the fractures could have been classified as A3 or A4 acc. to AOSpine 21,22 ; (b) populations consisting of a mix of fracture types in which A3 and A4 were indeed contained, however not analyzed separate from other fracture types; (c) populations including patients with a neurological deficit; and (d) group size below threshold.
Outcomes
A wide range of different clinical outcome parameters were presented in the eligible publications: Most frequently reported was the pain VAS (7 studies), followed by the Roland Morris Disability Questionnaire (RMDQ) 26 and Oswestry Disability Index (ODI) 40 (6 studies each) and Short Form–36 (SF-36) 41 (4 studies). The VAS functional spine score, 42 LBOS, 27 and patient satisfaction were reported in 3 studies each; the Hannover Spine score (FFbH-R), 43 was reported in 2 studies, whereas the McGill Pain Questionnaire (MPQ), 44 and an unspecified Quality of Life (QoL) scale were reported in 1 study each.
Nearly all publications presented results in which both A3 and A4 fractures were contained without stratification. 14,15,30,31,33 –38 Only Andress et al 39 presented results stratified for fracture type and Koller et al 32 presented results and fracture type for each individual patient. 32 Based on the lack of stratified results, we were unable to evaluate results of A3 and A4 fractures separately.
SMDs were calculated for all studies directly comparing operative with nonoperative treatment. 14,15,33,36 All 4 of these studies reported on disability but only 3 reported on pain. 14,15,33
Heterogeneity assessment of the studies combined to calculate the SMD for disability revealed an I 2 of 86.3% (P = .000), whereas for the studies combined to calculate the SMD for pain, the I 2 was 93.0% (P = .000). Based on the high heterogeneity, a random effects model was used to calculate the SMD. Estimation of the SMD for disability was based on RMDQ and LBOS scores, while for pain it was based on the pain VAS.
For disability, the overall SMD was 0 (95% CI −0. 72, 0.72) (Figure 2) and for pain it was −0.26 (95% CI −1.47, 0.95) (Figure 3). An SMD of less than 0 favors operative treatment whereas SMD values greater than 0 favor nonoperative treatment.
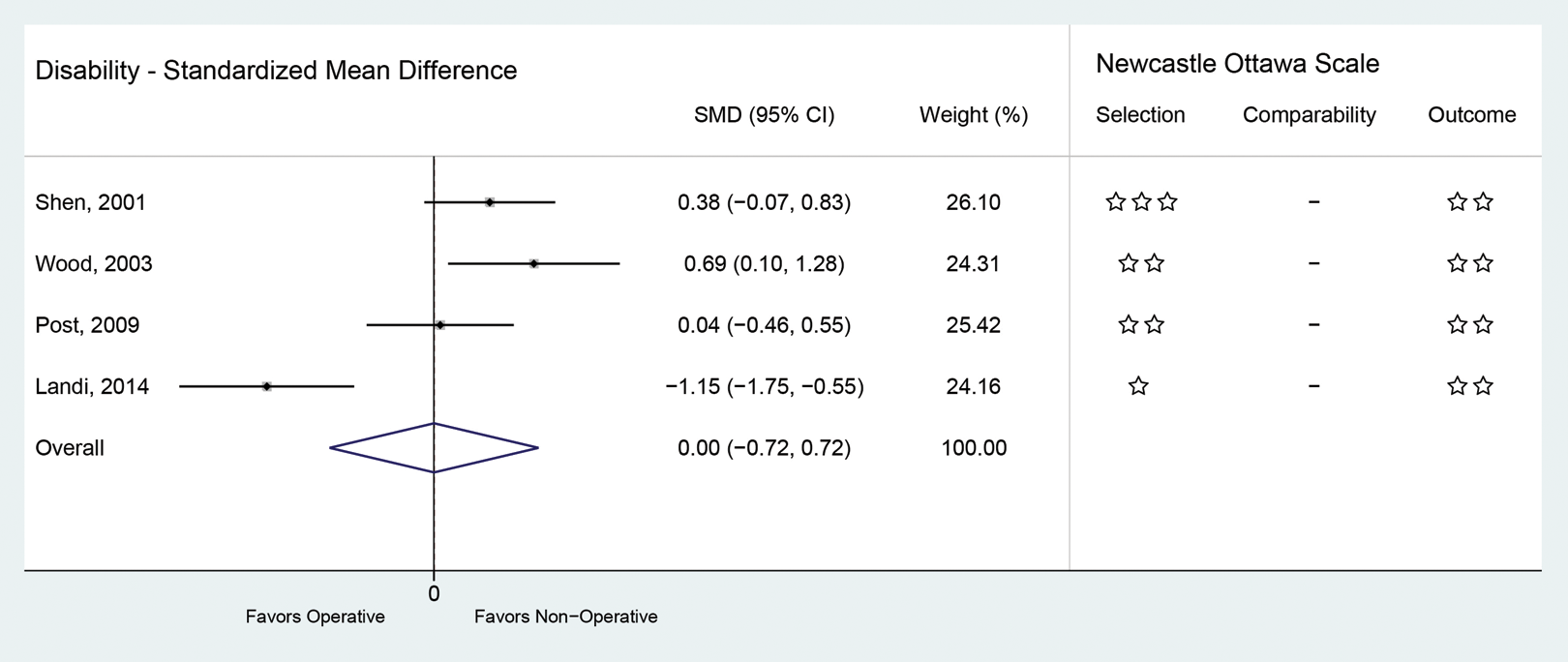
Standardized mean difference for disability combined with Newcastle-Ottawa Scale for bias rating.
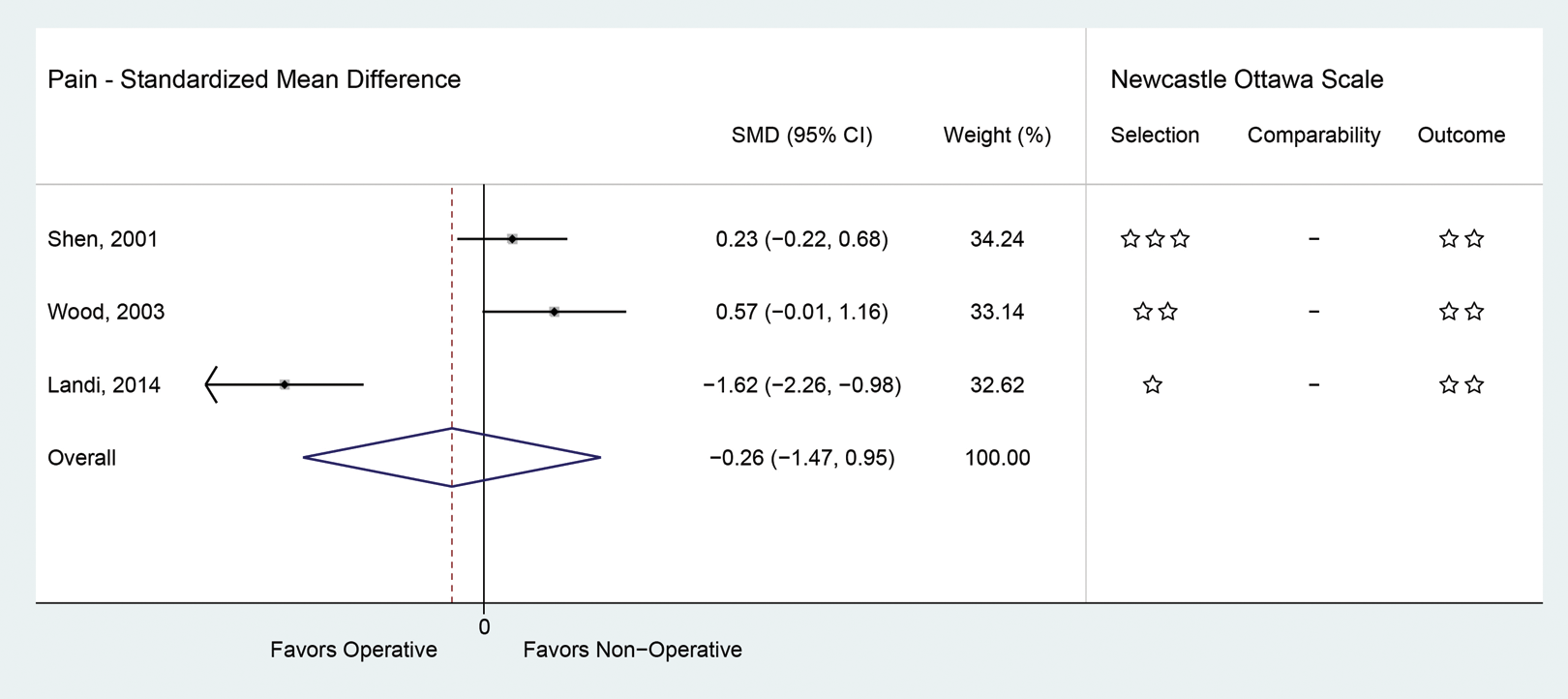
Standardized mean difference for pain combined with Newcastle-Ottawa Scale for bias rating.
Egger’s regression did not reveal any evidence of publication bias with coefficients of −8.75 for studies pooled for disability SMD (P = .553) and −11.81 for studies pooled for pain (P = .591).
In addition to the meta-analysis performed with studies directly comparing operative with nonoperative treatment, clinical outcome parameters that were available for a minimum of 125 patients for each of the target treatment modalities were analyzed descriptively for all studies. This was done for RMDQ and pain VAS. Since some of these studies comprised more than 1 patient group, results are presented per treatment group rather than per study (Figures 4 and 5).
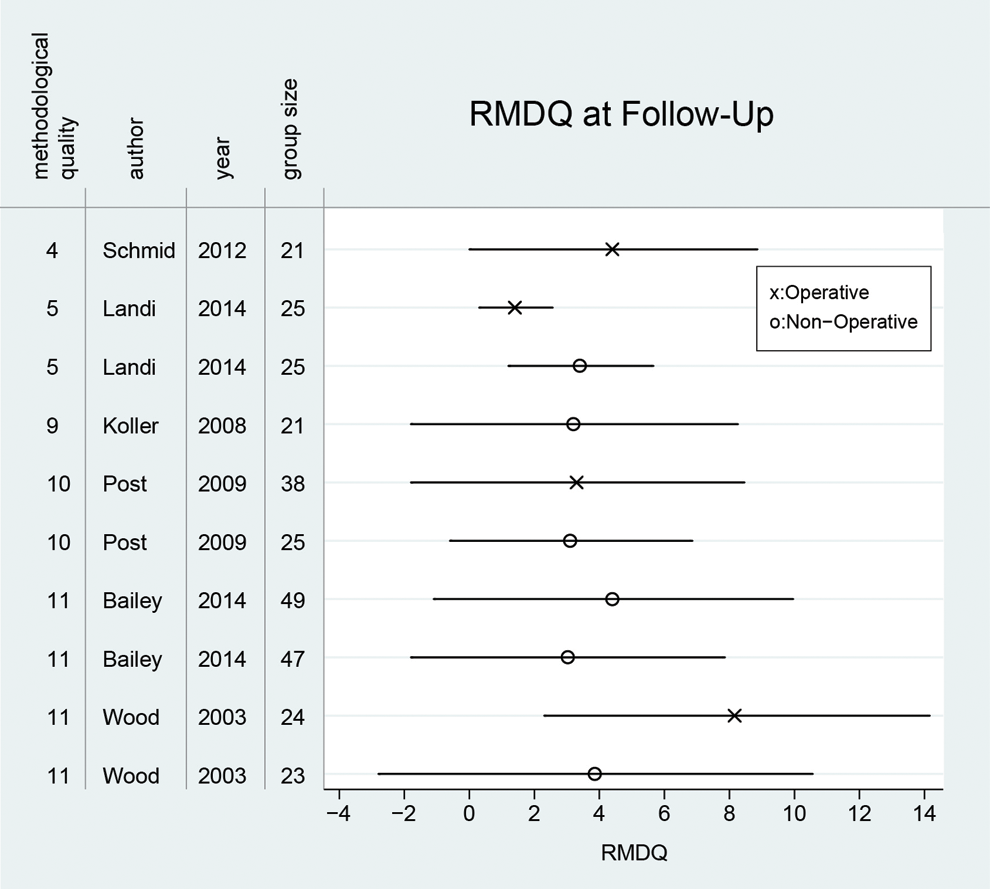
Results and treatment group sizes of all studies reporting Roland Morris Disability Questionnaire (RMDQ) presented in the order of methodological quality. X and Ο represent the RMDQ mean values and the bars represent the standard deviation.
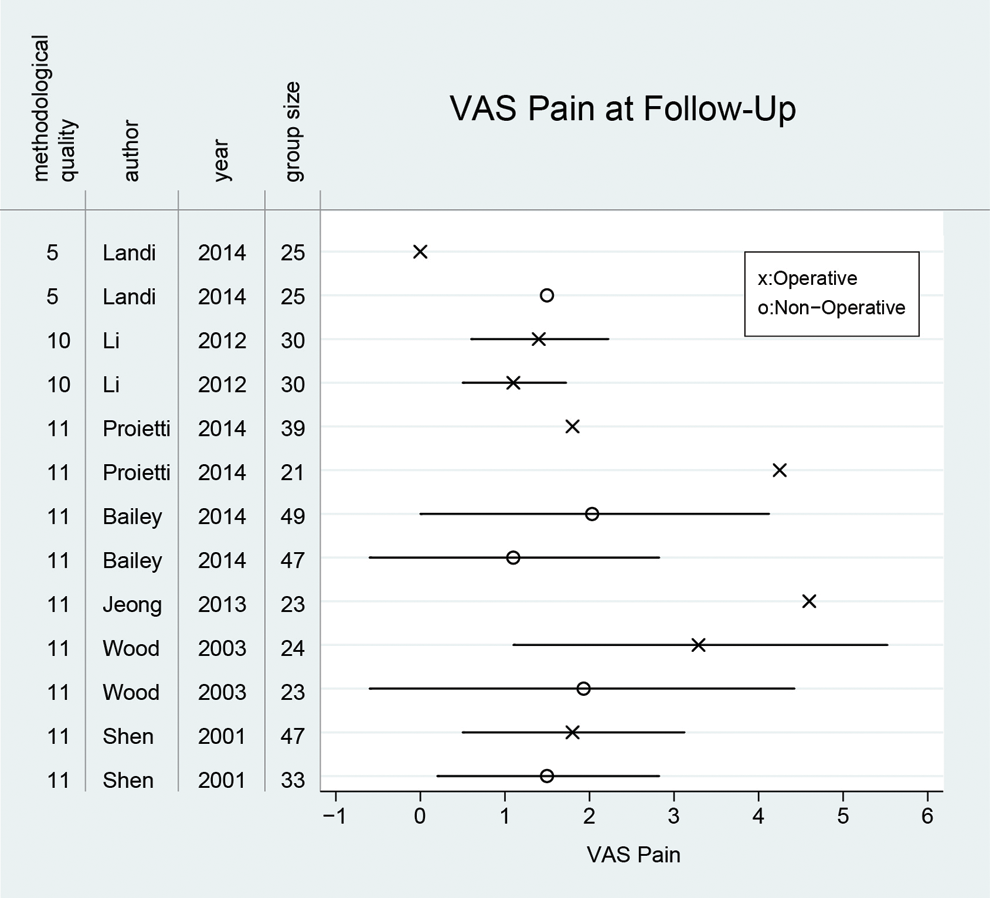
Results and treatment group sizes of all studies reporting pain visual analog scale (VAS) presented in the order of methodological quality. X and Ο represent the pain VAS mean values and the bars represent the standard deviation (as far as reported).
Generally, the differences in the respective outcome parameter results at FU were small, both between studies and between treatment groups. Nine of 13 treatment groups that presented pain VAS reported mean values between 1 and 2 at FU, with the most extreme values coming from operatively treated patients. The best pain VAS results were published by Landi et al 33 for the surgical treatment group, where none of the patients reported any pain at FU. They had only included patients with a McCormack score of 6 or less and a maximum spinal canal invasion of 25%. The worst pain was reported by Jeong et al 31 who surgically treated patients with a McCormack score of 7 or higher and reported a mean pain VAS of 4.6 at FU for this group. Similar pain values were reported for patients with a Sagittal Index (SI) >15°, treated surgically by Proietti et al. 36 At FU, they reported a mean pain VAS of 4.3.
Likewise, 8 of 10 treatment groups with RMDQ results reported mean values between 3 and 4.4 at FU, also with the most extreme values coming from operatively treated patients. The best RMDQ results were reported by Landi et al, 33 whose surgically treated patients reported a mean of 1.4 at FU while the worst RMDQ values were reported by Wood et al, 15 whose surgically treated patients reported a mean of 8.2 at FU.
Only 3 studies provided information about the time after which their patients returned to normal work. Landi et al 33 reported that patients treated operatively were back to work after 29 days while patients undergoing nonoperative treatment needed 117 days. Wood et al 15 reported contrasting results: In the group treated operatively, 6 months after surgery 42% of patients were back to work while in the nonoperatively treated patients this proportion was 74%. After 2 years, 59% of the operatively treated patients were back to work whereas this was the case for 83% of the nonoperatively treated patients. 15 Schmid et al 37 treated patients operatively and reported a mean time for back to work of 4.9 months.
Complication outcomes are listed in Table 5 and were clearly in favor of nonoperative treatment since the majority of possible complications are related to surgery. The most important local adverse events reported in nonoperatively treated patients were the need for surgery due to persisting complaints. Interestingly, surgery after initial conservative treatment was only reported in patients from one study. 30 In this study, which comprised 96 nonoperatively treated patients, 5 patients required surgery while still in hospital; 2 for severe radicular pain, and 3 for mechanical back pain. Another patient from this study required an osteotomy 8 months after her fracture. In operatively treated patients, instrumentation failure and donor site morbidity were the most significant adverse events. None of the included studies reported a neurological deterioration in any of their patients.
Most studies reported radiological outcomes with the target to describe the magnitude of kyphosis. However, a wide range of methods was used to measure it. Three studies provided no exact 34 or an unclear 33,37 description. Another 3 studies used the SI. 36,38,39 The Cobb angle was presented in 3 studies. 30 –32 One of these studies additionally presented the anterior vertical compression ratio 31 as described by Jiang et al. 45 One study each 14,15 used kyphosis measurement methods as described by Knight et al 46 and Atlas et al, 47 respectively. One study measured the segmental kyphosis angle (SKA), 32 another study measured the sagittal plane kyphosis (SPK). 39 The lack of uniform reporting made it impossible to pool the radiological results, which are listed in Table 6.
Quality Assessment
The quality assessment scores ranged from 4 to 11 on the 13-point scale. Two studies were rated low quality 33,37 with scores of 5 and 4, respectively, 1 study scored 9, 32 4 studies scored 10, 34,35,38,39 and 5 studies scored 11. 14,15,30,31,36
Risk of bias in the studies comparing conservative to surgical treatment was evaluated with the NOS. 29 The highest risk of bias was found in the domain “comparability” since none of the studies had matched the treatment groups or controlled for potential confounders in the analysis. The lowest risk of bias was seen in the domain “outcome” since FU was sufficiently long with an acceptable rate of drop-outs.
Discussion
In this systematic review and meta-analysis, we attempted to generate the best available evidence to support either operative or non-operative management of AO A3 and A4 thoracolumbar burst fractures in patients without neurological deficit.
Since we identified a number of primary studies that compared operative with nonoperative treatment, we were able to pool the respective results to generate SMDs for disability and pain. No difference between the operative and nonoperative management was revealed for any of these parameters. This finding is also supported by the results reported in the studies not comparing operative to non-operative treatment, even though no analytical statistics could be performed with these results.
Two RCTs that just missed inclusion in this review are worth mentioning: In 2015, Wood et al 48 published long-term results of the same patient cohort that is included in this review and was not included here because the number of patients available for analysis had fallen below our group size limit. However, the long-term results confirmed the earlier findings, which were strongly in favor of nonoperative treatment, becoming even more pronounced in the 20-year follow-up. The other RCT that just missed inclusion was published by Siebenga et al 16 in 2006 and was clearly in favor of operative treatment. Its group size was below our limit and some patients with fractures other than A3 or A4 had been included.
Generally, the differences in clinical outcomes of the included publications were small, both between studies and between treatment groups. In the vast majority of treatment groups, pain VAS results ranged from 1 to 2 on a 0 to 10 scale and RMDQ results ranged from 3 to 4.4.
In the context of chronic low back pain, the minimally important change (MIC) of RMDQ has been suggested to be defined as 5. 49 For back pain VAS on a scale of 0 to 100, values of 15 (see Ostelo et al 49 ) and 18 and 19 (see Hagg et al 50 ) have been suggested. Assuming that the MIC is similar for trauma patients, hardly any of the treatment groups included in this review present clinically relevant differences.
Previous attempts to synthesize the available clinical evidence have produced similar results: The systematic literature review conducted by Thomas et al 19 in 2006 included 21 studies with a total of 564 patients but a recognized overall low quality. The authors concluded that in spite of the wealth of published studies on thoracolumbar burst fractures, methodological limitations were pervasive such that at the time, the available evidence to justify the additional risks of surgery in neurologically intact patients with thoracolumbar junction burst fractures was minimal.
In 2012, a meta-analysis published by Gnanenthiram et al 12 based their main analysis on 2 randomized trials that yielded contrasting results and comprised heterogeneous patient populations. They concluded that “operative management of thoracolumbar burst fractures without neurologic deficit may improve residual kyphosis, but does not appear to improve pain or function at an average of 4 years after injury and is associated with higher complication rates and costs.” 12
Abudou et al 18 performed a Cochrane review in 2013, which included the same 2 trials with a total of 79 participants on which Gnanethiram et al 12 had published a meta-analysis in the year before. Abodou et al 18 summarized that the contradictory evidence provided by 2 small and potentially biased randomized controlled trials was insufficient to conclude whether surgical or nonsurgical treatment yielded superior pain and functional outcomes for people with thoracolumbar burst fractures without neurological deficit. However, they acknowledged that surgery was associated with more early complications and the need for subsequent surgery, as well as with greater initial health care costs.
In the absence of any evidence that would clearly favor one of the treatment options with regard to clinical outcome, on one hand, considerations on complication incidence, cost of intervention and time until full recovery gain importance. On the other hand, surgical treatment may well be considered for patients with unsatisfactory clinical outcomes after conservative treatment and further studies are needed to identify subgroups of patients who would benefit from early surgery.
The occurrence of complications in the studies included in this review is clearly in favor of nonoperative treatment. The most important local adverse events reported in nonoperatively treated patients were the need for surgery due to persisting complaints, while in the operatively treated patients, this concerned instrumentation and donor site morbidity.
These findings are well in line with results reported by other researchers. In 2014, Ghobrial et al 20 published a review specifically targeted at adverse events in the operative and nonoperative management of thoracolumbar burst fractures. They found significant differences in the incidence of infection (5.5% vs 0%, P = .0009) and instrumentation failure leading to revision surgery (4.4% vs 0%, P = .004). The incidence of all other types of complications as well as the overall complication rate was always higher in the operatively treated patients, but this never reached statistical significance. 20
The time required to go back to work reported in the studies included in our review is inconclusive due to contradicting results of the individual studies.
The major limitation of this review is the heterogeneity of included studies, which was present in various aspects such as FU time, study population, treatment modalities, and outcome parameters. The FU times ranged from 1 year to 10 years. However, since the clinical results were fairly uniform independent of FU time, we believe this had only a minor influence. On the other hand, the heterogeneity concerning the study populations was striking and certainly limited the comparability of studies in general. Nonetheless, the effect on clinical outcomes was primarily visible in the studies that had the most extreme differences in in- and exclusion criteria. For instance, Landi et al 33 only included patients with a McCormack score of ≤6 and reported a mean pain VAS of 0 at FU, 33 while Jeong et al 31 report a mean VAS of 4.6 at FU in patients with a McCormack sore of ≥7. This highlights how heterogeneous patient populations hamper the comparability among trials. The aforementioned differences in the included populations also show that the focus on AO A3/A4 fractures alone as an inclusion criterion may not be sufficient to define a uniform population for a systematic review. And yet, given that the 12 primary studies found eligible for this review were derived from 1929 initial matches in the literature databases, stricter inclusion criteria might have led to even less eligible studies.
A further important source of heterogeneity was the lack of uniformity amongst treatments. For instance, all studies analyzing non-operative treatment used different treatment modalities. The same applied to the studies analyzing operative treatment, but several studies used short segment stabilization or mono segmental stabilization techniques with pedicle screws. 33 –35,38
Another limitation of our review is the choice of target outcome parameters. We focused on the most common clinical outcome scores, but all of these were initially developed and validated for patients with chronic low back pain caused by degenerative diseases. Hence, these scores may not be suitable instruments to measure the success of spinal interventions after trauma. However, since no such instruments exist yet, we did not have an alternative.
Additionally, it was not possible to evaluate the radiological outcomes due to the lack of uniform reporting. However, several studies have demonstrated superior radiological results after operative treatment. 14,16,33 Nonetheless, the clinical relevance of radiological outcome in itself is unclear - no studies are known to us that demonstrate an unequivocal association of radiological and clinical outcomes after A3 and A4 fractures. On the other hand, many physicians are familiar with reports of patients who initially underwent conservative treatment and later in life present with significant global alignment and/or severe adjacent level issues requiring far more substantial surgery than initial surgical treatment would have involved. Further long-term studies employing uniform radiological outcome measures in combination with appropriate clinical scores are needed to address this important topic.
Finally, for calculation of the disability SMD, we pooled the functional scores RMDQ and LBOS. Even though the very concept of SMD relies on pooling different scores that are aimed at measuring the same outcome for the purpose of synthesizing evidence from different studies, pooling of these 2 scores is precarious. Both scores measure pain and the ability to perform activities of daily living, but while RMDQ measures the pain aspect purely in terms of duration, LBOS measures pain in terms of intensity.
Conclusion
This systematic review and meta-analysis did not reveal any difference in disability or pain outcomes between operative and nonoperative treatment of A3 and A4 thoracolumbar fractures in neurologically intact patients.
Unfortunately, it is currently unclear if the scores used to evaluate disability are indeed suitable for the evaluation of thoracolumbar trauma, which essentially implies that we are not sure whether we measure the right things. A new project has been initiated by AOSpine to define a thoracolumbar trauma score, which will hopefully solve the issue. 51
Although previous studies have shown a possible benefit of surgical treatment of A3 and A4 fractures with regard to radiographic outcomes, a structured analysis of radiological outcomes was not possible in this review due to the wide range of different measurement techniques employed.
Furthermore, this review demonstrated that so far, the majority of studies have not differentiated between incomplete (A3) and complete (A4) burst fractures, leaving potential outcome differences between the 2 entities undetected. The new AOSpine classification aims to overcome this drawback by emphasizing this difference with a clear distinction between these fracture types in the classification labels.
In the future, it will be important for the spine community to define and enforce the use of specific and uniform outcome parameters that should be applied in all studies evaluating thoracolumbar trauma.
Footnotes
Acknowledgments
The authors thank the AO Foundation TK System for funding this work and AOCID staff, in particular Anahí Hurtado-Chong and Alexander Joeris for critical review and helpful discussions.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Three authors (Elke Rometsch, Brigitte Sandra Gallo-Kopf, and Vasiliki Kalampoki) are employees of AO Foundation in the Department of Clinical Investigation and Documentation (AOCID). Concerning the work under consideration, Frank Kandziora has received travel support and honorary for board meetings by AO Spine. Financial activities outside the submitted work within the preceding 36 months are reported by Maarten Spruit for his activities as Chairman of AO TK Spine, by Frank Kandziora for his activities as a consultant for DePuy-Synthes, Siemens, and Silony, by Roger Härtl for his activities as a consultant for Brainlab, Lanx, Depuy-Synthes and AOSpine, and by Robert Alton McGuire for review of medical records for Rehab, Inc.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by the AO Foundation TK System.
