Abstract
Given the reasonably low COVID-19 vaccine rates (e.g., <60% fully vaccinated) among Canadian young adults (18–29), we sought to understand the factors that motivated this demographic to get vaccinated. Fifteen post-secondary students and graduates participated in semi-structured interviews about the type of health information they received during the pandemic, and their communication preferences. Analysis of interview data revealed four themes: (1) Participants had high science and health literacy which equipped them to identify and dismiss misinformation; (2) Participants expressed high trust in official sources which positively impacted their confidence in the vaccines; (3) Participants exhibited a low perceived risk from COVID-19 infection and got vaccinated for reasons beyond personal protection; and, (4) Participants responded best to communication that was targeted and tailored towards them. These themes form a foundation for effective vaccine communication campaigns targeted and tailored toward young adults, which is essential for acceptance of future vaccine recommendations.
Keywords
Introduction
Canada’s COVID-19 Vaccine Landscape
Mass vaccination has been a primary strategy to mitigate severe illness and death from COVID-19 in Canada. The country’s vaccine rollout has been relatively successful, with more than 88% of Canada’s adult population having completed their primary COVID-19 vaccine series (Public Health Agency of Canada, 2022c). However, for optimal protection against emerging COVID-19 variants and waning immunity, booster doses have been recommended (Public Health Agency of Canada, 2022c). Booster dose rollout began in late 2021, but coverage remained particularly low compared to the primary series, with only 60% of adults having received their first booster dose and 26.7% their second (Public Health Agency of Canada, 2022c).
Although COVID-19 vaccine uptake has waned across all Canadian adult demographics, 18-to-29 year-olds have the lowest coverage (Public Health Agency of Canada, 2022c), and represents one of the most hesitant Canadian adult demographics to get vaccinated (Burns, Dubé, Godinho Nascimento, & Meyer, 2024). As of December 2022, 83% of this age group had received their primary COVID-19 vaccine series; however, only 37% had received a first booster and 6.5% had received a second booster (Public Health Agency of Canada, 2022c). Further, national polls suggest that within the 18-to-34-year-old age group, 34% of vaccinated men and 19% of vaccinated women will refuse another COVID-19 booster dose if they are made available (Korzinski, 2022). This low uptake is a cause for concern as young adults have driven much of the transmission during the 2021 and 2022 waves (Public Health Agency of Canada, 2022b) and thus, without optimal vaccine coverage, are at a greater risk for developing and spreading severe illness. To address this gap in COVID-19 vaccination uptake, the priorities, attitudes, needs, and concerns of young adults must be understood to better meet their needs and influence vaccine uptake across all vaccine series.
The 5C Model for Vaccine Hesitancy and Acceptance
The 5C model is a theoretical framework that was designed to understand the psychological antecedents of vaccination (Betsch et al., 2018), and has been used to explore COVID-19 vaccine intention in several studies (Machida et al., 2021; Thier et al., 2022; Wismans et al., 2021). This model has condensed the factors associated with vaccine acceptance and hesitancy into the following five predictors: confidence, complacency, collective responsibility, constraints, and risk calculation. Confidence refers to an individuals’ trust in the safety and efficacy of the vaccine and those with high confidence are more likely to get vaccinated. Complacency describes an individual’s perceived risk of getting severely ill from the virus − those who are highly complacent do not see themselves at risk and are therefore less likely to get vaccinated. Collective responsibility covers the societal benefits of vaccination, including herd immunity and protecting vulnerable populations. Individuals who feel a strong collective responsibility are more likely to get vaccinated. Constraints are any physical or psychological barriers that make it difficult to get vaccinated. Finally, risk calculation describes the ability of an individual to weigh the risks of getting the vaccine against the risks of getting severely ill from the virus − exposure to vaccine-related misinformation creates a false narrative that can greatly impact risk calculation and reduce an individual’s willingness to vaccinate (Betsch et al., 2018).
Vaccine Attitudes and Intentions Among Young Adults
Several studies have been conducted to understand the specific factors that influence young adult decisions to get vaccinated against COVID-19. One study exploring vaccine intention among post-secondary students found confidence and collective responsibility had the strongest relationship to the sample’s intention to get vaccinated against COVID-19 (Wismans et al., 2021). The authors determined students with a high degree of trust in the vaccine and public health officials and a strong desire to protect those around them are more likely to get vaccinated, and public health campaigns targeted at this age group should aim to address these factors (Wismans et al., 2021). Another study found that post-secondary students who had confidence in health authorities were more likely to get the COVID-19 vaccine compared to students who were concerned about the vaccines’ safety, efficacy, and rapid development (Tam et al., 2022). Similarly, authors exploring vaccine hesitancy among Canadian young adults found that vaccine hesitancy can be driven by a distrust of political and scientific figures (Santavicca et al., 2023); and an American study cited that vaccine-hesitant young adults expressed a lack of trust in COVID-19 vaccine development and approval process (Szilagyi et al., 2021). Thus, understanding levels of trust and instilling confidence in the vaccine through effective communication campaigns is essential for improving acceptance.
In addition to COVID-19 vaccines, studies exploring young adult attitudes towards other routine vaccines can be used to understand their overall intentions to get vaccinated. For example, the human papillomavirus (HPV) vaccine is highly recommended in young people to prevent several cancers (World Health Organization, 2022). One study on the self-reported barriers and facilitators to receiving the HPV vaccine determined that young women who felt the vaccine was not important were less likely to receive it. Furthermore, another study on HPV vaccines in post-secondary students found that risk denial was associated with a lower intention to get vaccinated (Dempsey et al., 2014). Thus, effective vaccine communication for young adults should consider the holistic body of evidence for the barriers, facilitators, priorities and preferences of this demographic.
Tailoring Vaccine Communication for Young Adults
As a strategy to encourage vaccine uptake and reduce vaccine hesitancy, the Public Health Agency of Canada has recommended healthcare providers structure their communication about vaccines to address the 5Cs (Public Health Agency of Canada, 2021). However, different populations have different priorities, and the decision to get vaccinated is highly personal. As such, some studies have aimed to identify the impacts of the 5Cs on decisions to get the COVID-19 vaccine based on demographic characteristics like age, race and gender (Machida et al., 2021; Thier et al., 2022; Wismans et al., 2021), suggesting that COVID-19 vaccine communication must be tailored to meet the varying needs of target audiences. Additionally, the National Academies of Sciences, Engineering, and Medicine (NASEM) has published guidelines for communicating about vaccines with the public, citing that a targeted and tailored approach is needed (Brunson et al., 2021). They suggest that data from qualitative research on the target population be used to build the vaccine communication and meet the needs of the audience (Brunson et al., 2021). Another study on targeting pandemic communication towards young adult needs was conducted in Canada, however data was collected prior to the COVID-19 vaccine rollout, and thus the findings do not focus on vaccine-specific messages (Cheng et al., 2021). However, while some qualitative research has explored the priorities to vaccinate among young adults, gaps in understanding how to effectively integrate these findings and communicate with this demographic remain.
Objectives
1. To explore the major drivers for young adults in Canada to get vaccinated against COVID-19 including personal priorities and external influences; 2. To explore the communication needs and preferences of young adults receiving COVID-19 vaccine information; and 3. To understand how to effectively build vaccine communication campaigns that meet the needs of young adults.
Methods
Participant Recruitment
Eligible participants were 18-to-29 years old and living in any Canadian province or territory. No parameters were set on gender, education level or COVID-19 vaccination status. Convenience sample recruitment was conducted through social media channels including Instagram, LinkedIn, Facebook, and Twitter. The open call for participants was posted on the personal accounts of the research team and subsequently amplified by their networks. A $20 gift card was offered in recognition for participation.
Interviews
The Incorporation of Young Adult Communication Preferences for COVID-19 Vaccine Messages.

Demographic Survey
Immediately following the completion of the interview, participants were sent an online survey (supplementary material (2) developed through Qualtrics software (Qualtrics, Provo, UT, USA) asking questions about their age, race, gender, education level, and province of residence. The survey was optional, and responses were used solely to contextualize interview findings and were not linked in any way to interview data. Participants’ decision to complete the survey did not impact their overall participation or their eligibility for the gift card.
Data Analysis
Upon completion of the interviews, two researchers independently reviewed the transcripts and used an inductive approach to develop an initial list of codes for commonalities across the dataset. Codes represented interesting and important aspects of the data that provided the basis for theme development. The researchers then collaboratively developed a final codebook consisting of thirteen distinct codes (supplementary material 3). The researchers collaboratively coded a portion of the dataset using NVivo 12 Plus (QSR International, Doncaster, Australia) until agreement had been reached, and one researcher independently coded the remainder of the dataset. Next, reflexive thematic analysis was used to generate the initial list of themes (Braun & Clarke, 2006, 2019). Themes generated represented combinations of codes that shared meaning and are organized to describe the relationship between themes. The themes were discussed collaboratively by the research team to generate the final list of themes.
Ethics
Ethical approval was provided by the University of Guelph Research Ethics Board #22–08-004 on October 20, 2022. Prior to the interview, each participant reviewed a consent agreement form and expressed explicit verbal consent to participate.
Results
Participants
Fifteen young adults participated in the semi-structured interviews and thirteen participants completed the demographic survey (age range = 20–25 years, mean age = 23 years). The survey respondents consisted of four men and nine women, with eight who identified as white, three who identified as southeast asian, and two who identified as a mixed-ethnic background. Eleven respondents resided in Ontario, one lived in Alberta and one in British Columbia. All respondents reported using at least one form of social media every day including Instagram (n = 12), YouTube (n = 10), Twitter (n = 5), Facebook (n = 11).
All participants identified in the interviews that they were vaccinated against COVID-19, with survey results determining that three respondents received two doses, five participants with three doses, and five participants having received four or more doses. All participants identified in the interviews that they were enrolled in or had previously completed a post-secondary education program and the survey responses indicated that this included a college diploma (n = 1), bachelor’s degree (n = 6), or graduate degree (n = 6).
Priorities
Participants were asked to rank the importance of each construct of the 5C model (Betsch et al., 2018) on their decision to get vaccinated. The rank order for each participant was given a score of 1 (lowest priority) to 5 (highest priority). The total sum of the score given to each category across all participants was reportedー where the highest sum indicated the highest priority across all participants. Based on these rankings, collective responsibility had the greatest influence on decisions to get vaccinated (n = 60), followed by confidence (n = 54), risk calculation (n = 51), complacency (n = 42) and constraints (n = 18).
Themes
Across the fifteen interviews, four themes surrounding the decision to get vaccinated against COVID-19 emerged (Figure 1): (1) participants had perceived high science literacy which positively influenced their decision to vaccinate; (2) participants had high trust in official sources including government and public health which positively influenced their decision to vaccinate; (3) personal perceived risk from COVID-19 infection was low among participants and their decisions to get vaccinated were influenced by factors beyond personal protection; and (4) public health messages that met the communication needs and preferences of participants were most influential over decisions to vaccinate. Positive influences on young adults’ decision to get vaccinated against COVID-19.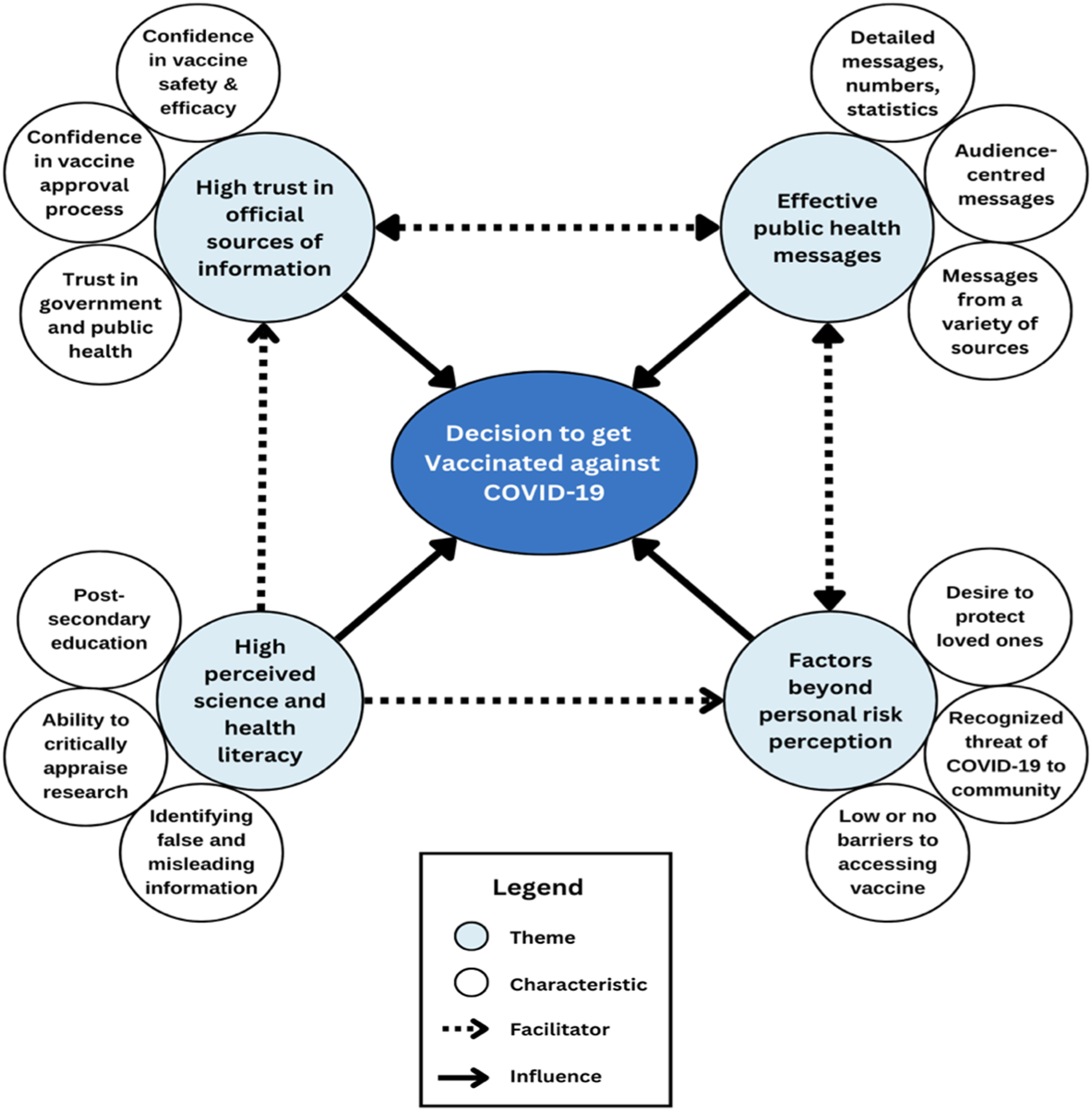
Theme 1: Perceived High Science and Health Literacy Positively Influenced Decision to Vaccinate
All participants identified themselves as acceptant of the COVID-19 vaccine, having received at least two doses at the time of the interviews. Participants commonly referenced their academic backgrounds and felt their post-secondary experiences (i.e., college and/or university courses), regardless of their majors, had prepared them to critically appraise evidence. “I would say in my post-secondary education there was emphasis on analyzing, critiquing, and discussing various forms of scientific journals throughout undergrad. So previous to the pandemic I did have a fair amount of experience reading them and comprehending them. Taking the necessary talking points out of a journal and trying to understand what setbacks a specific experiment could have, you know, and if there are any inherent biases.” – Participant 1
Furthermore, participants felt comfortable sifting through scientific information, claiming that the ability to ‘do their own research’ helped them make the decision to ultimately get vaccinated against COVID-19. This scientific and health literacy seemed protective against mis- and disinformation and led them towards accurate and trustworthy scientific information. Participants acknowledged that misinformation exists, however felt equipped to identify and disregard these false claims online because they had the ability to cross-reference with accurate and scientifically grounded information. Participants ultimately felt that their decision to get the COVID-19 vaccine was not impacted by misinformation that was circulating during the vaccine rollout. “Because of my background being able to do research with my Master’s, it’s helped me to be able to read some of those more complicated studies and the science that’s out there and look at maybe those news articles and actually figure out where the true science lies within that.” – Participant 11 “There’s lots of misinformation we can factor in, but there is also a lot of good, factual information that combats that. And it really depends on the person, because they are the one who’s filtering the information, and if they end up just focusing more on the misinformation then I don’t know [if they would get vaccinated].” – Participant 15
Theme 2: High Trust in Official Sources and the Influence of Personal Relationships Positively Impacted Vaccine Decision-Making
Participants discussed their trust in Canada’s government, healthcare, and public health professionals. Participants received their information from a range of sources including news media, government websites and social media accounts (e.g., @HealthyCdns on Instagram), healthcare professionals and personal relationships (e.g., family members, colleagues), and felt that these sources were promoting pro-vaccines sentiments, which influenced their decision to get vaccinated. They also stated that they did not feel that any of these sources had any ‘ulterior motives’ for promoting COVID-19 vaccines, which increased their level of trust. “I've always just trusted the fact that the government approved these vaccines. And the World Health Organization and all these medical professionals are saying it's a good thing. I always trusted that.” – Participant 9 “I just don’t think I ever had a reason to not trust [the vaccine], I don’t think anybody has really anything to gain from making it untrustworthy or unethical.” – Participant 2 “I believe the outlets that I followed were very positive about the vaccine whenever [I saw] negative news for the vaccine I’d make sure to double check.” – Participant 3
In addition, participants felt the COVID-19 vaccine development process was transparent, and they felt confident in the science, safety, and efficacy of the vaccines. “I have a lot of trust in the medical community and the people that created the vaccine and so I never once doubted that it would be detrimental in any way to my health […] I had so many conversations about the vaccine, with my physician and with other people in the medical community, I definitely had built a lot of trust and safety in the vaccine based on talking to these experts. So I had a lot of confidence in it.” – Participant 10
Theme 3: Personal Risk Perception from COVID-19 Infection was Low, and Decisions to Get Vaccinated Were Influenced by Factors Beyond Personal Protection
Participants did not feel they were at high risk for severe COVID-19 infection based on their age and health status. Their personal feeling of risk decreased as they witnessed people close to them contracting mild cases of COVID-19. “I don’t think I would be at severe risk of COVID. Obviously, you can’t say, you know, ‘I have no risk of being hospitalized or dying of COVID’. But I do understand that for me personally, as a young person, it’s pretty low.” – Participant 5 “From the research that I’ve done, it typically looks like young, healthy individuals are usually not at [high] risk, also, my father is immunocompromised, so I’m looking at that and seeing him as a much higher risk population than someone like me.” – Participant 13
However, despite their low perceived risk, all participants decided to get vaccinated against COVID-19 for external reasons. While some cited government mandates as a reason to get vaccinated, most participants recognized COVID-19 as a threat to older adults and immunocompromised individuals and wanted to get vaccinated to protect those members of the community. Participants also felt getting vaccinated would help protect their loved ones from COVID-19 infection and getting vaccinated would help the world return to normal life. “I just knew that [getting the COVID-19 vaccine] was something that I was going to do, mostly for those around me. I have older grandparents that I see, and my parents, I wanted to protect those around me and as well I just thought it was doing my part of being part of society and doing it for everyone. That is definitely a big part of it.” – Participant 14 “I mean, I have a lot of people around me who are elderly or have some underlying health conditions. And I think a large factor of me getting the vaccine was because I didn’t want to spread or give it to someone else.” – Participant 12 “I just decided to get vaccinated because at the time, COVID had been around for a while, and it seemed like almost a cure. Also, it was needed to enter certain public spaces or to go on vacation so yeah, those are the main reasons and I thought it would protect myself against COVID and spreading it to others.” – Participant 8
Participants did not experience any major barriers to getting vaccinated beyond the high demand for first-dose vaccine appointments. Some had a fear of needles, but most participants felt that the process was convenient, and they were able to get vaccinated without any issue. “I think it was a pretty seamless process, I just had to go online and sign up. I think it was surprisingly easy and just the fact that the government’s been pretty diligent about putting clear and factual information out there on how on, you know all the steps to get the vaccine, you know, encouraging people to get one.” – Participant 15
Theme 4: Public Health Communication that met the Needs and Preferences of Participants was Most Influential over Decisions to Vaccinate Compared to Non-targeted Communication
Participants preferred vaccine communications that specifically mentioned their demographic and addressed their personal concerns surrounding the COVID-19 vaccine. They liked messages that were highly detailed – for example with the inclusion of statistics, links to more information, and personal testimonies. Participants preferred messages that did not use excessive scare tactics and wanted to see accurate representations of risk in crisis communication. This was consistently mentioned during interviews when participants were shown the message: “Myth: young people always experience milder COVID-19 symptoms. Fact: young people can still become very ill and are at a risk for long-term effects after a COVID-19 infection. The best way to protect yourself from a severe infection is to get vaccinated against COVID-19,” (supplementary material 1). “I don’t think [this message is] overblowing the fact that young people [can get severely ill from COVID-19 infections], they’re not like, ‘young people will get sick’ and it’s like ‘it’s possible, it’s not like a guarantee’, but I think it’s good for people who maybe are kind of just thinking like, ‘I’m 22 and healthy’. To know that they can still get quite sick and that getting the vaccine is a good idea. So yeah, I like this just kind of [message] targeting.” –Participant 4 “[Messages that are targeting young adults] sort of make you think, ‘oh yeah, that is me and I personally could get sick.’ So, I think that’s good with some of the messages, make them less general and if you target people specifically then it makes it more personal, and I think then young people are more inclined to pay attention. When it’s addressing everyone it’s easier to just put it out of mind.” –Participant 7 “I’m a stats person. I like looking at numbers and real data, so if there was a way of putting, ‘X amount of young people get COVID with severe symptoms’, let's say, it would make it sound more believable.” –Participant 6
Participants felt the quality and quantity of COVID-19 vaccine communications declined as the pandemic progressed which impacted their personal feeling of risk from the virus. They felt that the news was no longer emphasizing the risks associated with COVID-19 infections, and that vaccine promotion had declined. Overall, participants felt crisis communication was not well targeted to them, as the overwhelming message participants heard was that they were a very low risk group and COVID-19 vaccination was to protect others and not themselves. “COVID seems like a long-gone thing in the news. It was literally just a running headline, every single news source, you open the TV and I’ll tell you the cases that day. But now they don’t. They no longer say that, now it’s just a passing by comment.” –Participant 6 “I think [communication was effective] maybe a year ago, less so now. I mean a year ago we were told that the vaccines are not for yourself, but for the community, and we had the vaccine passport which really emphasized that. It’s all gone away now and it’s more of just a “let it go” type feeling, so I think that notion has kind of gone away.” –Participant 11
Discussion
As outlined in Figure 1, four themes emerged from the interview data, which contributed to positively influencing participants to get vaccinated against COVID-19: high trust in official sources, high science literacy, low personal risk perception from COVID-19, and audience-centred messaging. Underpinning each of these themes were the following 5C factors: high confidence, high complacency, high collective responsibility, and low constraints.
High Trust and Confidence in the Vaccines
Participants stated that they had a high trust in the COVID-19 vaccines, and were confident that the vaccines were a safe and effective way to prevent severe COVID-19 infections. The participants cited their experiences in post-secondary programs had prepared them to critically appraise research, which helped them sift through any information that was posted about COVID-19 vaccines. Previous research found individuals with higher levels of education (e.g., post-secondary education) are more likely to trust and accept the COVID-19 vaccine (Kricorian et al., 2022; Santavicca et al., 2023). Further findings suggest those without a post-secondary education had lower confidence in the safety and efficacy of the COVID-19 vaccine, and were more likely to believe vaccine misinformation compared to the post-secondary-educated counterparts (Kricorian et al., 2022). It is known that misinformation and COVID-19 conspiracy theories can drive vaccine hesitancy in young adult populations (Santavicca et al., 2023), and as such, the current research participants’ decisions to ultimately get vaccinated could be attributed in-part to their higher education levels.
The study participants also expressed trust in government, public health, and the vaccine development process. In general, lower levels of trust in institutions has been associated with lower vaccine intentions (de Coninck et al., 2021; Humprecht et al., 2020); and a previous study on vaccine hesitancy among Canadian young adults found that a distrust of political and scientific figures can contribute to vaccine hesitancy (Santavicca et al., 2023). Lack of trust in vaccine development and approval was found to be one of the main drivers in vaccine hesitancy among young adults and other subpopulations (Szilagyi et al., 2021). However, the study participants trusted the experts to develop a vaccine that is safe and effective and viewed the COVID-19 vaccines in the same positive light as other vaccines, such as childhood immunizations. This high degree of trust and confidence is a predictor for vaccine acceptance as outlined in the 5C model (Betsch et al., 2018), and has echoed previous study findings (Santavicca et al., 2023; Szilagyi et al., 2021; Tam et al., 2022; Wismans et al., 2021).
High Complacency was Balanced with High Collective Responsibility
Despite choosing to get vaccinated, all participants expressed low risk perception for COVID-19. They did not feel at-risk of severe COVID-19 infection, and the main driving force to get vaccinated was not the prevention of severe illness. This is consistent with findings from a previous survey which indicate young adults exhibit the lowest perceived severity and susceptibility to a COVID-19 infection compared to all other age demographics (Rosi et al., 2021). Contributing to their low-risk-perception, many participants stated they felt pandemic communication campaigns have been centred around ‘high-risk’ and ‘vulnerable’ populations, and young and healthy individuals were more likely to experience milder COVID-19 symptoms if any. In terms of the 5C model, this high complacency should align with low vaccine uptake (Betsch et al., 2018); however, this was not the case in our study sample, as everyone was vaccinated. Instead, the participants’ high complacency was outweighed and modified by a strong feeling of collective responsibility. Previous research has found that young adults felt that protecting their community was the most important reason for getting vaccinated, and they chose to do so as a means of societal good (Wismans et al., 2021). Similarly, another study found university students had low COVID-19 risk perception and did not follow preventative behaviours to protect themselves, but instead for vulnerable populations around them (Kollmann et al., 2022).
However, while promoting the societal benefit of vaccination is a key priority when addressing COVID-19 vaccine uptake in this group, it is unclear whether collective responsibility would have an equally strong impact on non-emergency vaccine campaigns. For example, prior research on young womens’ intentions to get vaccinated against HPV also determined that many felt they were not at risk from the virus, which negatively impacted their decision to get vaccinated (Rambout et al., 2014). The study participants expressed a sensitivity and responsiveness to the example messages that they were shown about personal risks associated with contracting COVID-19, and as such, along with promoting collective responsibility, it remains highly important to tailor health messages to address young adults’ complacency surrounding infectious diseases.
Low or No Constraints to Vaccination
None of the participants identified any major barriers that prevented or made it difficult to get vaccinated. Instead, most participants stated the process for booking and receiving the COVID-19 vaccines was seamless, aside from the high demand for appointments in the initial rollout stages. This convenience can be attributed to Canada’s rapid COVID-19 vaccine procurement and rollout, which ensured that all Canadians would have access to a completed primary vaccine series in 2021 (Public Health Agency of Canada, 2022a). Furthermore, young adults may have had positive experiences with navigating online booking systems due to their high digital literacy skills, and ability to navigate websites and applications.
Building Effective Vaccine Communication Campaigns
As National Academies of Sciences, Engineering, and Medicine (NASEM) guidelines have stated, a targeted and tailored approach to communication, using findings from qualitative research should be used to build effective vaccine messages (Brunson et al., 2021). Thus, the research findings build on previous studies that identified young adult priorities for vaccination (Wismans et al., 2021; Tam et al., 2022), and message tailoring (Cheng et al., 2021) to inform best practices and guide future vaccine communication campaigns to increase uptake among young adults. In general, the participants identified their preference for messages that: (1) mention their demographic; (2) are highly specific; and (3) are communicated on a variety of channels. Together these four strategies can be used to build and improve upon vaccine communication (Table 1).
Our findings suggest that the strong sense of collective responsibility should be a focus of communication to young adults, in addition to instilling confidence in the safety and efficacy of the vaccines. While not a priority for this age group, efforts should also be made to influence risk perception so young adults are aware they are at risk from negative consequences from a COVID-19 infection (Lockerd Maragakis, 2020).
The participants expressed their preference for messages that were highly specific and addressed their age-group directly. Targeting and tailoring messages is an important strategy for crisis communication broadly (MacKay et al., 2022), and it appears that this is especially important for young adults. This population expressed that when they felt that their age-group was reflected in a message, they would be more compelled to follow the public health advice, which is an important consideration for developing communication campaigns. The interviewees also stated they preferred communications that included statistics, numbers, figures and examples, rather than broad, general statements made to the general public. Finally, there was also a desire for the messages to clearly cite their sources to improve the credibility of the message.
In terms of communication channels, the study population identified several platforms from which they receive information about the COVID-19 vaccines. The most cited sources were news outlets, social media, government websites, and friends and family. However, the most used social media platform among the study participants was Instagram. It is known that in Canada, young adults constitute the primary user group on this social media platform (Gruzd & Mai, 2020) and as such, public health should leverage their presence on Instagram, and tailor their messages to incorporate the preferences, priorities and concerns of young adults around vaccination (table 1).
Limitations and Future Research
The current research had high homogeneity across the study population and was derived by a convenience sample, and self-selection bias likely contributed to the sample characteristics. Since the fifteen participants were all vaccinated against COVID-19, had a high digital literacy, and had some level of post-secondary education the results may not be generalizable to a broader Canadian or global population. Furthermore, the participants were not asked about specific disciplines of education and since these details were not collected, the results may have been skewed towards a higher health or science literacy. Instead, this work can be used to inform best practices for general communication with post-secondary students about vaccines, as this population was represented in the study.
There also exist limitations in the data analysis process. During transcript de-identification, demographic characteristics (e.g., age, ethnic background) were not linked with direct quotes. Given our small sample, this process was completed to ensure anonymity in participants, however it may have led to inaccuracies in interpretation. Furthermore, despite codebook agreement being met by the research team, the bulk of the dataset was coded independently which could lead to biases in the coding process.
Future studies should focus on using research findings to develop public health messages and subsequently test them with young adult focus groups. Given the limited generalizability of these results, further research should also be conducted on broader young adult demographics, including those without formal education and/or unvaccinated populations, to better understand how to promote vaccination. In addition, future studies should explore the interactions of various psychosocial factors that influence the decision of young adults to get vaccinated.
Conclusion
Our findings show that this sample of Canadian post-secondary students exhibit high levels of confidence, collective responsibility, and complacency towards the COVID-19 vaccines. Their perceived scientific literacy and trust in government and public health led them to accept the COVID-19 vaccines as safe and effective public health measures; and while they did not feel COVID-19 was a serious threat to their own health, they chose to get vaccinated to protect others. The findings also suggest building public health messages that instill confidence, collective responsibility and address the threat that a COVID-19 infection can pose to this age group will increase vaccine uptake. Finally, we found highly specific public health messages that include statistics and specific details, are perceived as the most effective and trustworthy messages. Although the study sample contained all vaccinated individuals, understanding the knowledge, attitudes and perceptions of this group will be important for tailoring future vaccine communication campaigns. Specifically, these findings will be useful for health promotion teams on post-secondary campuses as they promote vaccine uptake for illnesses that can have major implications on the young adult population (e.g., HPV, influenza, Meningitis B).
Supplemental Material
Supplemental Material - Communicating about COVID-19 Vaccines: A Qualitative Study on Preferences, attitudes, and Influences on Canadian Post-secondary Student Decisions to Get Vaccinated
Supplemental Material for Communicating about COVID-19 Vaccines: A Qualitative Study on Preferences, attitudes, and Influences on Canadian Post-secondary Student Decisions to Get Vaccinated by Caitlin Ford, Melissa MacKay, Jennifer McWhirter, and Andrew Papadopoulos in Emerging Adulthood
Supplemental Material
Supplemental Material - Communicating about COVID-19 Vaccines: A Qualitative Study on Preferences, attitudes, and Influences on Canadian Post-secondary Student Decisions to Get Vaccinated
Supplemental Material for Communicating about COVID-19 Vaccines: A Qualitative Study on Preferences, attitudes, and Influences on Canadian Post-secondary Student Decisions to Get Vaccinated by Caitlin Ford, Melissa MacKay, Jennifer McWhirter, and Andrew Papadopoulos in Emerging Adulthood
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
