Abstract
The aim of this mixed-studies systematic review was to synthesise existing research to identify if the five features of emerging adulthood (identity exploration; instability; self-focus; feeling in-between; possibilities) were evident in the self-management of long-term physical conditions by emerging adults (aged 18 – 29 years old). Five databases were systematically searched. Thirty papers met the eligibility criteria and were included. The synthesis identified that the five features of emerging adulthood are present in the self-management strategies and tasks of emerging adults living with long-term physical conditions. Due to numerous transitions, that characterise this unstable developmental period, emerging adults encounter specific self-management challenges. However, a greater understanding of the extent to which each of the five features are present and the challenges posed to the self-management of a long-term physical condition in emerging adults is required. This will inform targeted self-management supports and interventions in the future.
Keywords
Introduction
Long-term physical conditions (LPTC) last for more than six months; therefore, are persistent and seldom cured completely, for example, diabetes, asthma and epilepsy (Stanton et al., 2006; World Health Organisation, 2014). In addition to ongoing physical symptoms, LTPC can be a source of stress leading to an increased risk of psychological issues such as anxiety, depression which may impact a person growing up (Compas et al., 2012) and poorer educational and vocational outcomes (Maslow et al., 2011). Over time, due to medical advancements, some LTPC (e.g., some heart conditions and cancers) can be detected and treated early, leading to longer survivorship from the condition. While other LTPC such as asthma and diabetes can be monitored and treated long-term with various medical and non-medical treatments extending life expectancy (McCorkle et al., 2011). This means that more children and adolescents who experience LTPC are reaching emerging, young, middle and older adulthood which has led to an increased burden on health services (Barlow et al., 2002; Dowrick et al., 2005). This increase in people living into adulthood prompted the need to move to a collaborative, patient-centred model of healthcare with a focus on self-management (Dowrick et al., 2005). Indeed, a systematic review found that self-management can benefit people living with LTPC through improved quality of life, learning to manage physical and psychological symptoms, how to utilise healthcare resources and to manage overall attitudes to living with LTPC (De Silva, 2011).
Self-management places the patient at the centre of managing their LTPC and usually involves collaboration with families and healthcare professionals (Dowrick et al., 2005; Ryan & Sawin, 2009). In this review, self-management is defined as a dynamic process of self-regulation (Schulman-Green et al., 2012) by a person to manage the day-to-day effects of living with LTPC (Barlow et al., 2002), using core self-management skills that should be individually tailored, that is; problem-solving; decision-making; resource utilisation; forming of a patient/healthcare provider partnership; and taking action (Lorig & Holman, 2003). Different LTPC can require varying approaches to self-management, for example, some techniques might focus on generic cognitive and behavioural changes, while others might also require, more in-depth technical information about physical activity, nutrition, and medication (De Silva, 2011). This process of self-management changes over time as and when needed and affects both the individual and families in different ways (Ryan & Sawin, 2009).
Within the self-management literature, age has been highlighted as both a risk and protective factor for self and family management of LTPC identifying that different developmental ages/periods may need different support levels from others (Grey et al., 2006). The transfer of self-management between parent and child is a socially complex process and may become more so, with the transfer to adult services between the ages of 16–21 years and as the person with the LTPC becomes legally responsible for their own healthcare decisions (Giarelli et al., 2008). In addition, at this age, the individual may be expanding their social and support network beyond the family, as they transition to college or the workplace; increasing contact with peers and developing long-term romantic relationships (Wiebe et al., 2016), trying to establish a community of peers and forging strong emotional ties (Hopmeyer et al., 2022). For example, in addition to parents continuing to provide support, romantic partners were deemed as important for support by emerging adults living with diabetes. Both parents and partners provided multiple support functions, but the key difference was who acted as the primary support during emerging adulthood (Campbell et al., 2022).
The Five Features of Arnett’s Emerging Adulthood (Arnett, 2004a; 2004b).

Overall, emerging adulthood is a time of many aspirations while also a time of instability and uncertainty (Arnett, 2004a; 2004b). Possibly more so for emerging adults living with LTPC, as research has found that those with chronic paediatric physical illness when entering emerging and full adulthood have delays with some psychosocial developmental milestones (Maurice-Stam et al., 2019). This research found less participation in sports, less likely to have paid employment and later sexual intimacy (Maurice-Stam et al., 2019). There may also be challenges to self-management due to the navigation of changing support systems, shifting interpersonal influences and competing priorities as emerging adults find their feet in the adult world (Audulv et al., 2009) that is, finding their identity and exploring possibilities (Arnett, 2004b). Additionally, as the self-regulatory parts of the brain are still maturing, the susceptibility during this period to taking risks with self-management may lead emerging adults living with LTPC to take risks that affect health and development in the longer term (Arain et al., 2013).
Three recent review papers on emerging adults living with LTPC have highlighted the importance of considering self-management within emerging adulthood (Rasalingam et al., 2021; Shelley et al., 2020; Wentzell et al., 2020), however, none focused solely on self-management. Wentzell et al., (2020) examined how challenges or transitions during emerging adulthood added to the understanding of diabetes distress. They found levels of diabetes distress to be highest in emerging adulthood compared to other age groups. In terms of issues relevant to self-management, they found that changes to personal and professional support networks were a challenge for emerging adults and this contributed to diabetes distress. Shelley et al. (2020) examined how emerging adults living with and at risk of genetic conditions experience the five features of emerging adulthood. They found five themes; independence, education/career/employment, relationships/social life, family planning and life perspective. Each of these themes was congruent with two or more of the five features of emerging adulthood. In relation to findings relevant to self-management, the researchers found differences in independence, such as those living with conditions, had more reliance on family and medical professionals for supports (e.g., physical and financial), were influenced in making college and career decisions (e.g., to be near medical care or family), were cautious of social environments and activities (e.g., smoking and alcohol) and that the higher the severity of a condition the lesser the autonomy reported. Finally, in their review of how individuals with LTPC experience emerging adulthood, Rasalingam et al. (2021) highlighted some themes relating to self-management; the importance of support networks (e.g., worry of loss of support from family members or financial dependence); working towards independence which depends on the severity of LTPC (e.g., adjusting career goals to specific health needs); issues with systemic resources (e.g., access to reliable personal care assistants); psychosocial challenges (e.g., limitations to socialising making it difficult to build friendships or dealing with anxiety related to condition); and keeping a positive attitude (e.g., not engaging with negative thoughts).
While these reviews have yielded some important information about the self-management experiences of emerging adults who are living with or at risk of conditions, to date there has been no systematic review that has been undertaken to specifically examine self-management within the period of emerging adulthood nor within the context of Arnett’s theory of emerging adulthood. Therefore, the aim of this review is to synthesise existing research on emerging adults (aged 18 – 29 years old) to identify if the five features of emerging adulthood (i.e., the age of; identity exploration; instability; self-focus; feeling in-between; possibilities) are evident in the self-management of LTPC. By undertaking this systematic review, a greater understanding will be gained of the impact of this diverse period of change and exploration on the self-management of LTPC. This can help healthcare professionals in understanding the unique challenges that emerging adults face as they transition to adulthood and improve the development of care strategies.
Method
This mixed studies systematic review includes quantitative, qualitative and mixed methods studies (see Pluye & Hong, 2014). It was conducted and reported in accordance with the standards of the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) Statement (Moher et al., 2009; Page et al., 2021; Sarkis-Onofre et al., 2021).
Search Strategy
A systematic search was conducted across five electronic databases (PubMed, Medline, PsycINFO, CINAHL and Web of Science) up to 15th of February 2022. The search strategy combined controlled vocabulary and free-text search terms which were adapted to each database. One category was “Emerging Adult*” to capture papers relating to emerging adulthood and the second category related to self-management terms, using Boolean terms “OR” and “AND” to combine the two together (see supplementary file for example). A further search of the reference lists of three review papers and all the final included papers supplemented the search.
Inclusion and Exclusion Criteria
Papers were included if they (1) were empirical, peer-reviewed papers published in English up to 15th February 2022; (2) had participants with a long-term physical condition and were aged 18–29 years of age (or where data for this group could be clearly disaggregated from other data reported); (3) discussed Arnett’s theory of emerging adulthood; (4) included research data relating to the self-management of a long-term physical condition; and (5) study design included qualitative, quantitative or mixed method data.
Screening and Data Extraction
All titles and abstracts were imported into Covidence (www.covidence.org) and screened by one reviewer (OM). Titles/abstracts identified as potentially eligible were sourced and screened as full-text by one reviewer (OM). Queries were discussed and resolved through consensus with a second and third reviewer (PG, VL) and reasons for exclusion recorded (see Figure 1). Data extracted from the papers were author; country of study; study aim; method of data collection; type of long-term physical condition; sample size; age range and which of the five features of emerging adulthood was evident in the self-management findings of each paper (see Table 2). Extracted data were cross-checked by the second and third reviewers (PG, VL) and any discrepancies were resolved through consensus. PRISMA 2020 flow diagram for systematic reviews which included searches of databases and other sources.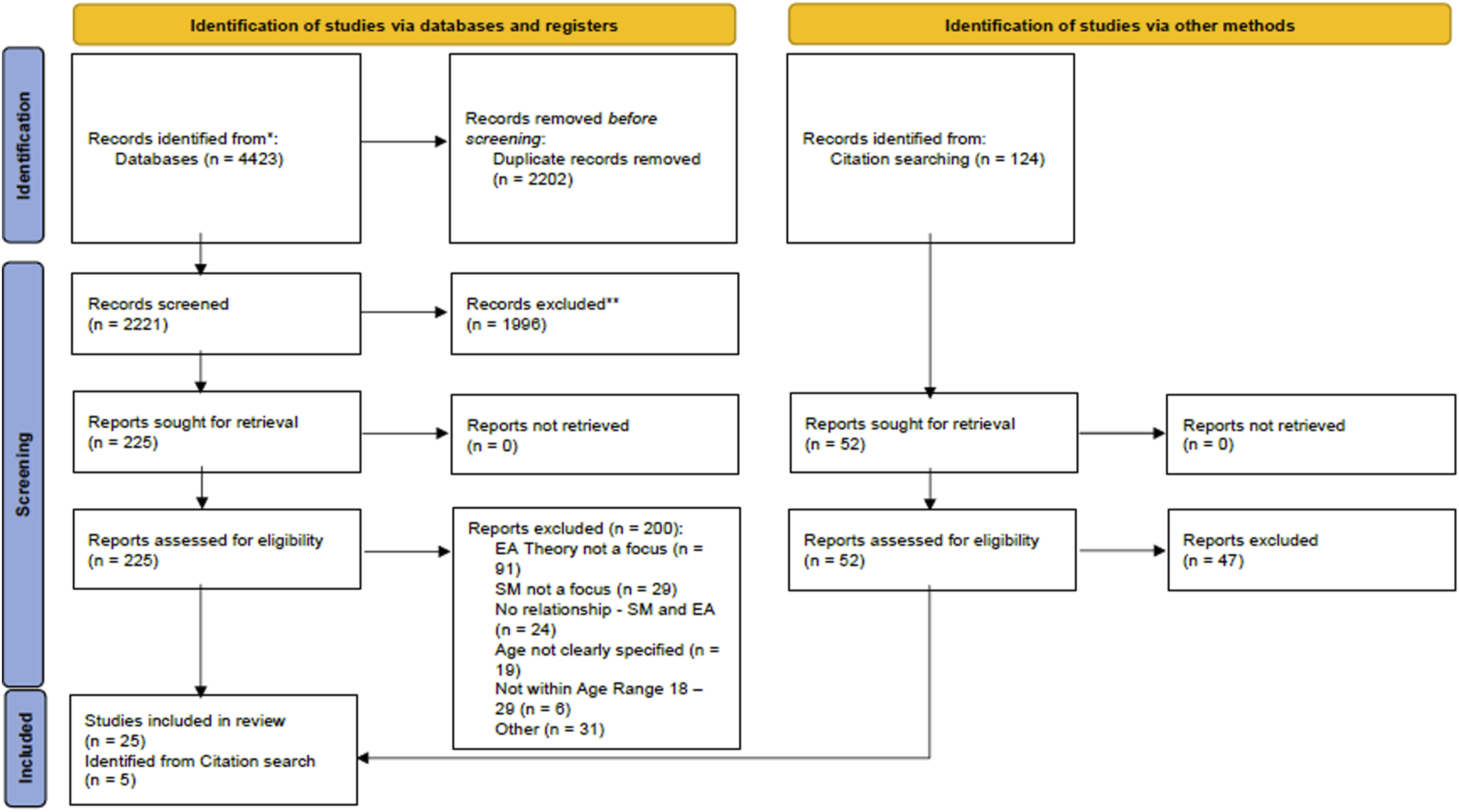
Quality Appraisal
Characteristics of Papers Included.
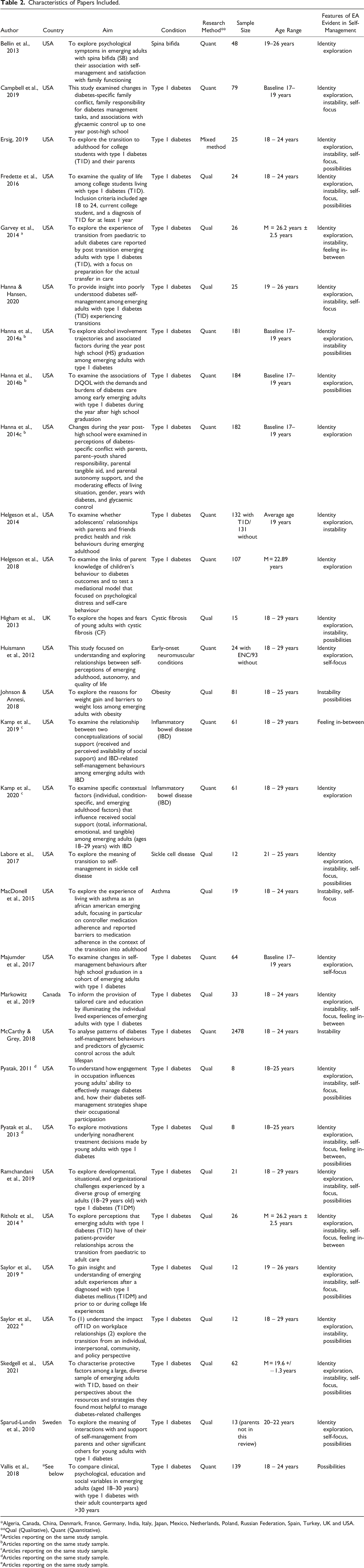
*Algeria, Canada, China, Denmark, France, Germany, India, Italy, Japan, Mexico, Netherlands, Poland, Russian Federation, Spain, Turkey, UK and USA.
**Qual (Qualitative), Quant (Quantitative).
aArticles reporting on the same study sample.
bArticles reporting on the same study sample.
cArticles reporting on the same study sample.
dArticles reporting on the same study sample.
eArticles reporting on the same study sample.
Data Synthesis
In synthesising the data from the included studies, a data-based convergent QUAL synthesis design (Hong et al., 2017; Pluye & Hong, 2014) was adopted in this systematic mixed studies review. In this synthesis design, the data from all included studies, whether qualitative, quantitative or mixed method in design, were considered equally important for answering the research question. This involved data transformation and for the purposes of this systematic mixed studies review, quantitative data were transformed into qualitative data (Pluye & Hong, 2014). To wholly convert the quantitative data to qualitative, the researcher (OM) followed the recommendations of Gough et al., (2017) and included the broader perspective of the authors’ conclusions to report the results for these studies as part of the results.
Thematic synthesis (Thomas & Harden, 2008) was the method of synthesis following the transformation of data. Thematic synthesis has many forms, ranging from a “deductive” model, where the codes and/or themes are identified in advance, to an “inductive” model where the codes and/or themes are generated through the process and can have elements of both (Gough et al., 2017). This systematic review combined both deductive and inductive models (Gough et al., 2017). The free codes and descriptive themes were developed inductively by analysing the self-management findings in combination with the definitions of each of the five features of emerging adulthood. The analytical themes were pre-defined as the five features of emerging adulthood, that is the age of; identity exploration; instability, self-focus; feeling in-between; and possibilities (Arnett, 2004a; 2004b).
There are three stages to Thomas and Harden’s framework of thematic synthesis; free line-by-line coding of the findings of primary studies (in this case, self-management findings); organising of these free codes into descriptive themes (stages one and two can overlap); and generating analytical themes (Gough et al., 2017; Thomas & Harden, 2008). In this review, all relevant self-management data from the included papers was read and free-coded line-by-line and subsequently organised into one or more of the 14 descriptive themes that were developed inductively (see Figure 2). In addressing the aim of this systematic review, the analytical themes were pre-defined as the five features of emerging adulthood and the descriptive themes were mapped onto these five features of emerging adulthood. The five emerging adulthood analytical themes and mapped descriptive themes.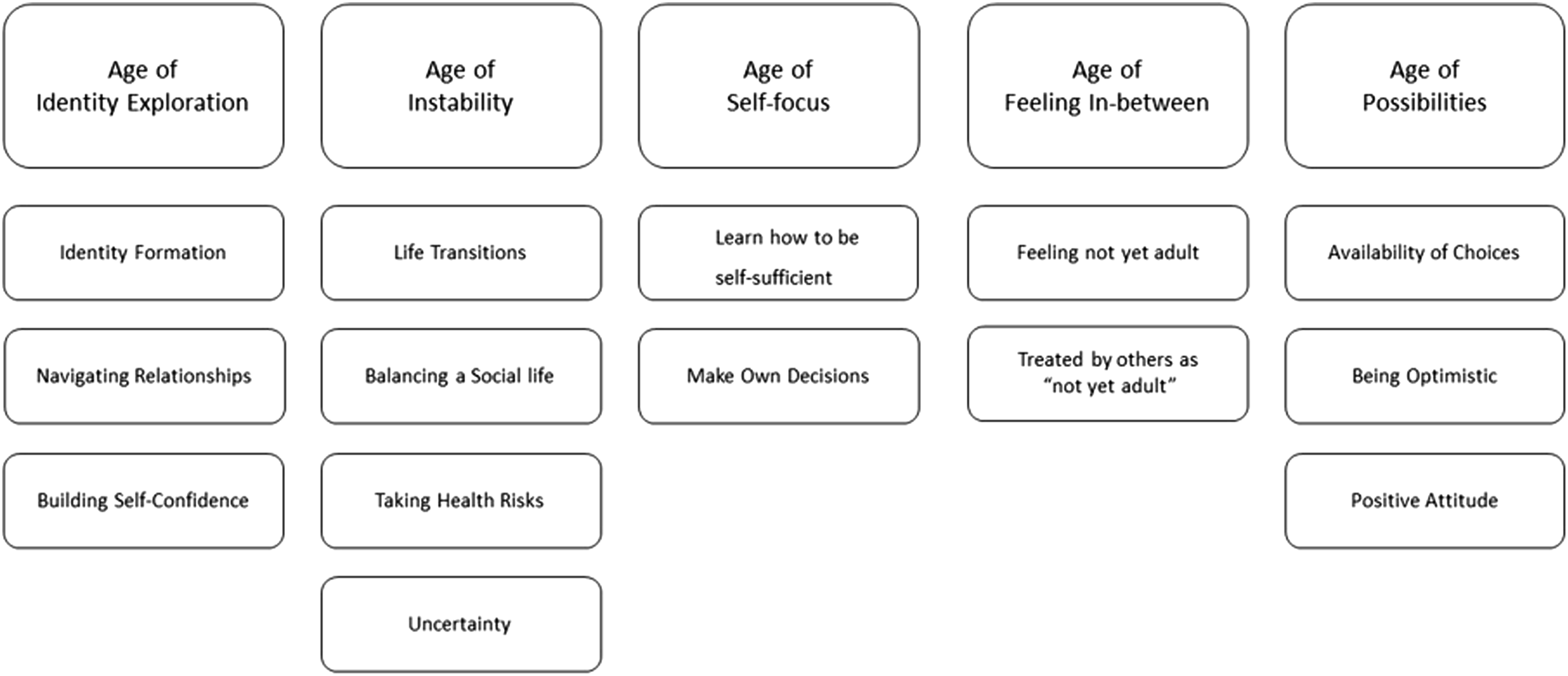
Results
Database searches yielded 4423 results, with 2221 papers remaining after duplicates were removed. Following the initial screening of titles and abstracts, 1996 papers were removed, with 225 papers remaining for full-text screening and of these 25 papers were identified for inclusion. The reference lists of these 25 papers and three review papers were reviewed with a further 124 papers for full-text screening identified, of which five additional papers were included. Overall, a total of 30 papers were included in this review (see Figure 1).
Characteristics of Included Papers
MMAT Quality Appraisal.
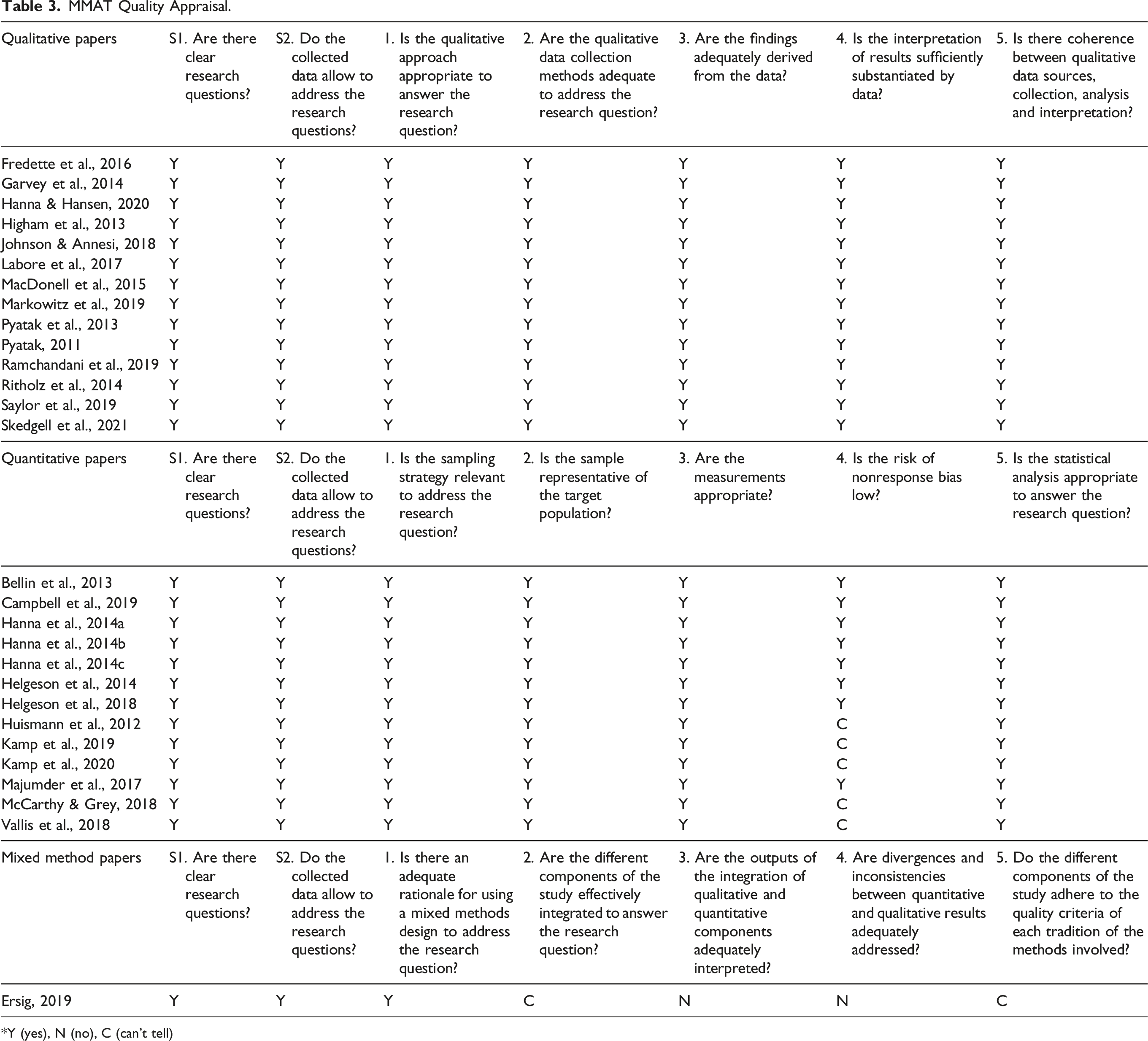
*Y (yes), N (no), C (can’t tell)
Thematic Synthesis Results
Illustrative Quotations and References for Each Descriptive Theme.

Analytical Theme 1: The Age of Identity Exploration
The Age of Identity Exploration is reflected in how emerging adults living with and self-managing LTPC are in the process of identity formation, exploring and navigating relationships and building self-confidence in their self-management ability. Exploring and forming their own identity is concerned with questions such as “who am I, who and what do I identify with?”. The process of navigating relationships such as peer and romantic others helps an emerging adult to identify and solidify what qualities are important to them in themselves and others and helps them to gain a broad range of life experiences (e.g., new relationships at college and work). Similarly, navigating changing relationships with parents and healthcare professionals helps them to become more independent and take more responsibility for their own decisions and actions, for example, those related to healthcare and self-management. As they become more independent and take on these responsibilities, this builds self-confidence in their ability to self-manage their condition further solidifying their sense of self. The Age of Identity Exploration theme was evident in the self-management of LTPC across 25 papers (Bellin et al., 2013; Campbell et al., 2019; Ersig, 2019; Fredette et al., 2016; Garvey et al., 2014; Hanna et al., 2014a, 2014b, 2014c; Hanna & Hansen, 2020; Helgeson et al., 2014, 2018; Higham et al., 2013; Huismann et al., 2012; Kamp et al., 2020; Labore et al., 2017; Majumder et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019, 2022; Skedgell et al., 2021; Sparud-Lundin et al., 2010).
Descriptive Theme: Identity Formation
Across 16 papers identity formation was evident in participants’ self-management strategies and tasks (Fredette et al., 2016; Garvey et al., 2014; Hanna et al., 2014a, 2014b; Hanna & Hansen, 2020; Higham et al., 2013; Huismann et al., 2012; Labore et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019, 2022; Skedgell et al., 2021; Sparud-Lundin et al., 2010), for example, being able to accept LTPC as part of identity or struggling, even refusing to accept it as so. For some participants, it was important to be normal (Higham et al., 2013) with some participants feeling so strongly about this, they would fight against anything that might affect their “normality” (Higham et al., 2013). Some participants feared stigma about their condition, leading them to hide their condition and their self-management tasks from others (Hanna & Hansen, 2020). However, others were able to accept it as part of their identity. For example, increasing self-care responsibility did not increase worry or decrease life satisfaction for participants who had lived with diabetes for at least nine years, indicating an acceptance of diabetes management as part of their identity and therefore a part of normal life (Hanna et al., 2014b). Some even indicated how their condition has helped to define and improve who they are “I’ve thought a lot about how I wish that I didn’t have diabetes. But at the same time, I’ve also thought about how it has made me stronger as a person… if I did get the chance to change it, I don’t think I would” (Skedgell et al., 2021, p. 348).
Descriptive Theme: Navigating Relationships
Navigating relationships as emerging adults leave behind adolescence and journey towards full adulthood helps emerging adults identify what qualities are important, both in themselves and in others. This helps emerging adults to understand who they are or whom they want to be and whom they want in their networks. Changing relationships (e.g., parental, healthcare) also helps emerging adults to begin to take responsibility for themselves, further building their identity. Efforts to navigate new, current, and changing relationships were evident in self-management strategies and tasks across 22 papers (Bellin et al., 2013; Campbell et al., 2019; Ersig, 2019; Fredette et al., 2016; Garvey et al., 2014; Hanna et al., 2014c; Hanna & Hansen, 2020; Helgeson et al., 2014, 2018; Higham et al., 2013; Kamp et al., 2020; Labore et al., 2017; Majumder et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019, 2022; Skedgell et al., 2021; Sparud-Lundin et al., 2010).
Navigating newer personal relationships (e.g., building networks) across college or the workplace had an impact on self-management. In navigating new relationships in the college environment, participants found themselves having to rely on people they may have just met for support, like roommates. (Ersig, 2019). Sometimes this was a positive experience, however, sometimes not knowing people well enough meant not knowing if they understood the seriousness of a condition “I keep Glucagon in my dorm room. I actually don’t think my roommates know how to use it, but I’ve told them it treats low blood sugar” (Ersig, 2019, p. 15). In relation to the new classroom environment at college, some participants were not always comfortable to carry out essential self-management tasks (Ramchandani et al., 2019) and this also lent itself to the workplace, with self-consciousness evident for working participants (Saylor et al., 2022). Fear of stigma was often reported as a reason for being uncomfortable “I get self-conscious, because I’m like I don’t want people looking at it [glucose level], like they’re going to judge me … oh, you’re doing a bad job” (Saylor et al., 2022, p. 153). Positively, other participants highlighted the importance of educating work colleagues to reduce this stigma and to advocate for themselves and their condition (Saylor et al., 2022).
Navigating changing and new “adult” relationships with healthcare professionals that involve new adult self-management responsibilities (e.g., no parents in appointments, being responsible for medication) was difficult for many participants in the transition from paediatric to adult care and “one of the hardest things … about adult care is rebuilding that relationship” (Ritholz et al., 2014, p. 43). Emerging adults importantly highlighted a need for more developmentally appropriate care (Garvey et al., 2014). Sometimes there was a perceived lack of insight from healthcare professionals into the lifestyle issues facing emerging adults, such as moving away to college and experiencing a social life (Pyatak et al., 2013). However, some participants had a more positive experience, where finding a collaborative approach was implemented by their new healthcare team helping them to develop their new identity as an emerging adult (Markowitz et al., 2019). One participant even went to several endocrinologists until they found one specifically for young adults that understood emerging adulthood “everyone actually knew … that I drink, and I don’t always eat what I should. There are just things that are realistic, that kids do, and so many doctors act like it doesn’t happen” (Pyatak, 2011, p. 466).
Becoming independent from parents and/or family is important for emerging adults, particularly in developing their own self-management strategies that fit with whom they are when becoming their own adults. In relation to navigating familial relationships and the self-management of their LTPC, experiences were mixed. Becoming independent in self-management during emerging adulthood was supported by parents for some participants (Labore et al., 2017). However, others wanted to continue to rely on parents even when they had moved out of home “she’s been by my side since the start, she comes with me to the doctors and she knows what it’s all about…” (Sparud-Lundin et al., 2010, p. 133). Other participants found their parents unable to let go and stifling their need to become independent by continuing to attend medical appointments and monitoring self-management tasks to ensure they are done correctly (Pyatak et al., 2013). Furthermore, it was found that for some participants, more diabetes-specific conflict and parental responsibility were associated with worse glycaemic control (Campbell et al., 2019). For a smaller number of participants, more fractured family relationships led to poorer self-management (Pyatak et al., 2013).
For emerging adults who are navigating relationships with significant others while carrying out self-management of LTPC, they are often exploring what qualities are important to them in other people, while also considering what that person values in them. For some in relationships with significant others it was highlighted that it was important that the partner show interest (Sparud-Lundin et al., 2010) but participants were not expecting them to become responsible for them (Sparud-Lundin et al., 2010). One participant felt bad for her partner due to being sick, maybe challenging her identity as a significant other “I’ve been really poorly, it hasn’t made anything bad between my partner and our relationship, but I just feel awful sometimes because…I can’t do anything and he has to do everything” (Higham et al., 2013, p. 378).
Descriptive Theme: Building Self-Confidence
Self-confidence comes as emerging adults become more certain about who they are. Feeling not confident or confident in self-management tasks was evident across 13 papers (Fredette et al., 2016; Hanna et al., 2014a, 2014b; Hanna & Hansen, 2020; Higham et al., 2013; Huismann et al., 2012; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Saylor et al., 2019, 2022; Skedgell et al., 2021; Sparud-Lundin et al., 2010). Not feeling confident to carry out self-management tasks stemmed from various reasons, such as no support from family (Pyatak et al., 2013). Some participants did not have the confidence yet to risk drawing attention to themselves (Higham et al., 2013), while participants with a stronger sense of identity, were more confident in carrying out their tasks, especially in public “I’ve gotten to a point where I’m comfortable sitting down at a table and just taking insulin” (Hanna & Hansen, 2020, p. 451). Furthermore, self-confidence also allowed participants to speak up for themselves, for example when dealing with peer pressure to socialise (Saylor et al., 2019).
Analytical Theme 2: The Age of Instability
The Age of Instability is reflected in how emerging adults living with and self-managing LTPC are planning how to get from adolescence to adulthood and making that transition. This plan is subject to the instability of different life transitions, trying to balance a social life, taking health risks and uncertainty. During this period there can be numerous life transitions (e.g., starting college or a new job) which can mean revisions to the plan (e.g., changing college major or dropping out, changing jobs, moving homes). Important to note is that many of these transitions happen due to identity explorations (e.g., moving in with roommates or a significant other) which means that identity exploration and instability often go hand in hand. The transitional nature of this period can also mean emerging adults have more opportunities to socialise (e.g., college) and now have the freedom to decide if to socialise more frequently. Emerging adults with LTPC may have an extra challenge in trying to balance their social life with their self-management tasks. The combination of life transitions and increased socialising makes it an unstable period culminating sometimes with decisions that take risks with health (e.g., missing medication) and for some emerging adults it creates further uncertainty (e.g., relationships, finances, future). This theme of instability was reflected across 20 papers (Campbell et al., 2019; Ersig, 2019; Fredette et al., 2016; Garvey et al., 2014; Hanna et al., 2014a; Hanna & Hansen, 2020; Helgeson et al., 2014; Higham et al., 2013; Johnson & Annesi, 2018; Labore et al., 2017; MacDonell et al., 2015; Markowitz et al., 2019; McCarthy & Grey, 2018; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019, 2022; Skedgell et al., 2021).
Descriptive Theme: Life Transitions
Life transitions, such as moving out of home, going away to college, starting work and moving to adult healthcare make emerging adulthood a highly unstable period during which, the self-management of LTPC needs to continue. This may even involve some emerging adults taking on this responsibility solely for the first time. The interaction between life transitions and self-management is evident across 14 papers (Ersig, 2019; Fredette et al., 2016; Garvey et al., 2014; Hanna & Hansen, 2020; Johnson & Annesi, 2018; MacDonell et al., 2015; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019, 2022; Skedgell et al., 2021).
In relation to college, this transition was important for many participants in relation to learning how to fit their self-management tasks (old and new) into their new schedule. In participants living with obesity, 44% of participants reported that they experienced significant weight gain when they transitioned to college, due to busy schedules, increased access to poor food choices, overeating, and a reduction in extracurricular activities such as sports (Johnson & Annesi, 2018). In those living with diabetes, similar diet and lifestyle issues led to blood sugar issues (Ersig, 2019), and the impact of blood sugar issues led to issues such as impaired cognition, missing classes and assignments, even skipping tests (Fredette et al., 2016).
Similarly, in transitioning into the workplace, while some experiences were positive, again emerging adults had to figure out how to fit their self-management tasks into their new schedule while also considering how it might impact colleagues. One issue was worrying about the impact of carrying out their self-management tasks on colleagues “brings on a whole new anxiety, because you realize you’re impacting everyone else around you” (Saylor et al., 2022, p. 155). In situations, where there was a lack of accommodations in the workplace, this also led to anxiety for some participants about asking for support even leading to one participant feeling the need to lie to their employer from fear of being judged for not managing their diabetes properly “I lied, because I was embarrassed, because I was like I feel like I should be more prepared” (Saylor et al., 2022, p. 155).
In healthcare, changes in self-management targets and the transition from child to adult healthcare impacted overall self-management. Changes in healthcare targets could mean constantly chasing good control (Pyatak et al., 2013), while others felt the changes from paediatric to adult care created instability (Ritholz et al., 2014). For one participant, the independence gained from transitioning to adult healthcare coupled with moving away from home to college, meant that they were able to “get away” with a minimum amount of self-management “during college, I went to the endocrinologist once a year, and I didn’t really do much with the information, and nobody really noticed” (Garvey et al., 2014, p. 194).
Descriptive Theme: Balancing a Social Life
The many transitions during emerging adulthood, such as college and work can lead to an increase in the opportunities to socialise outside of college and work schedules. The freedom and independence gained during emerging adulthood means that those living with LTPC often face challenges in balancing their social lives with managing their condition, often due to competing needs and wants which can create a lack of consistency, that is, instability. This was evident across four papers (Garvey et al., 2014; Hanna & Hansen, 2020; Saylor et al., 2019; Skedgell et al., 2021). For instance, the need to carry out self-management tasks (e.g., taking medication, resting) competed with the desire to socialise with others (e.g., alcohol, late nights) (Garvey et al., 2014). A key reason reported for prioritising socialising over self-management was wanting to fit in and be normal which links back to identity exploration (Skedgell et al., 2021). For certain LTPC such as diabetes when socialising, alcohol is an important consideration but even without drinking alcohol, other issues such as staying up late is also a risk factor when trying to balance socialising and self-management, for example “Even without alcohol partying is dangerous. I can live without alcohol, but got to be like everybody else” (Saylor et al., 2019, p. 76).
Descriptive Theme: Taking Health Risks
There are several reasons why emerging adults may take risks with their health and it is not always done purposely. Consistency is important for the self-management of LTPC, for example, taking daily medication or regular sleep. A lack of consistency is a health risk and creates instability in carrying out ongoing self-management tasks. Burnout, poor planning and stigma are some of the reasons that emerged in the literature, that led to taking health risks. Taking health risks was reflected in 11 papers (Hanna et al., 2014a; Helgeson et al., 2014; Higham et al., 2013; Labore et al., 2017; MacDonell et al., 2015; Markowitz et al., 2019; McCarthy & Grey, 2018; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Saylor et al., 2019).
Being tired or reaching burnout in carrying out self-management tasks such as checking blood sugars or taking medication was mentioned by a number of participants and led to rebelling and missing such tasks and risking their health (Pyatak et al., 2013). Alternatively, some participants living with diabetes decided to rely on their bodies to tell them how their blood sugar was, even when they knew it was not reliable (Pyatak, 2011). Anxiety caused others to be non-adherent and in denial about health consequences “I know what will happen … [But] for some reason, it doesn’t hit me. It’s like I know it, but I won’t accept that it’s going to happen” (Pyatak et al., 2013, p. 714). While others missed carrying out self-management tasks due to poor planning, for example, when socialising (MacDonell et al., 2015). Additionally, with socialising, for example, for some living with diabetes, the desire to be normal sometimes meant sacrificing the perfect A1C to be with friends (Ramchandani et al., 2019). For other participants, fear of stigma and being self-conscious was also highlighted as a reason “it’s just that little aspect of social anxiety, that sometimes keeps me from measuring it in class” (Ramchandani et al., 2019, p. 488). Finally, one paper found that emerging adults more than any other age group have the lowest percentage of achieving the recommended haemoglobin A1c, report the fewest blood glucose checks per day and were more likely to report missing an insulin dose (McCarthy & Grey, 2018, p. 1610).
Descriptive Theme: Uncertainty
Uncertainty of a situation or the future is unsettling and this lack of knowledge or certainty about an outcome can bring instability to a person’s ability or confidence to self-management now or possibly in the future. For example, uncertainty in familial relationships was reflected in one paper where more family conflict and more parental responsibility were associated with worse glycaemic control (Campbell et al., 2019, p. 7). Financial uncertainty and self-management were highlighted in three papers (Ersig, 2019; Labore et al., 2017; MacDonell et al., 2015), with insurance being the main concern for affording treatments, such as medications (MacDonell et al., 2015). Additionally, some participants highlighted overall uncertainty about their future due to living with LTPC across three papers (Ersig, 2019; Fredette et al., 2016; Higham et al., 2013), such as how their health will be in the future “knowing that “…even though I take care of myself and am active, eventually the disease will overcome me” (Ersig, 2019, p. 15).
Analytical Theme 3: The Age of Self-Focus
The Age of Self-Focus is reflected in how emerging adults who are living with and self-managing LTPC have the greater freedom to make own decisions (e.g., what to eat, when to socialise) and learn how to be self-sufficient. A freedom which allows emerging adults to focus on themselves. This means that emerging adults, as independence is gained, have an opportunity to develop or try to improve life skills and for those living with LTPC, self-management skills. Being self-focused was evident in self-management strategies and tasks across 16 papers (Campbell et al., 2019; Ersig, 2019; Fredette et al., 2016; Hanna & Hansen, 2020; Huismann et al., 2012; Labore et al., 2017; MacDonell et al., 2015; Majumder et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019; Skedgell et al., 2021; Sparud-Lundin et al., 2010).
Descriptive Theme: Learn how to be Self-Sufficient
Learning how to be self-sufficient within self-management was evident across 15 papers (Campbell et al., 2019; Ersig, 2019; Fredette et al., 2016; Hanna & Hansen, 2020; Huismann et al., 2012; Labore et al., 2017; MacDonell et al., 2015; Majumder et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Ritholz et al., 2014; Saylor et al., 2019; Skedgell et al., 2021). Some participants were at the beginning of becoming self-sufficient and voiced how they needed to learn more about taking care of themselves (Pyatak et al., 2013) and others were learning to become more sufficient by learning from past mistakes, like trial and error (Saylor et al., 2019). For some participants it was the collaborative relationships with healthcare professionals that spurred them on (Ritholz et al., 2014) and for others it was the realisation that their parents were not around anymore that they needed to take responsibility for themselves (Ramchandani et al., 2019).
Many participants reported taking responsibility for themselves in the realisation of the seriousness of their condition, for example “it’s not a game. [Diabetes] is real for me, it’s like life or death kind of a situation. So, I really just have to do right by it” (Skedgell et al., 2021). Therefore, planning ahead became an important task and could be as simple as setting phone reminders, checking blood sugar regularly and ensuring to carry the correct insulin doses (Skedgell et al., 2021), or developing a routine (Hanna & Hansen, 2020). Importantly, some participants expressed frustration in how they were being self-sufficient but still experiencing issues and uncertainty (Ersig, 2019). The importance of advocating for oneself was also important to be able to carry out some self-management tasks “that’s where I think you have to advocate for yourself and say I need a lunch break” (Saylor et al., 2019, p. 78).
Descriptive Theme: Make Own Decisions
Making decisions is an important part of self-focus and self-management as emerging adulthood is a time of taking responsibility for oneself; this was evident across five papers (Huismann et al., 2012; MacDonell et al., 2015; Pyatak, 2011; Pyatak et al., 2013; Saylor et al., 2019). For participants living with early onset neuromuscular conditions, attitudinal autonomy which is associated with goal setting and decision making was positively correlated with quality of life (Huismann et al., 2012). An example of decision-making for participants living with diabetes was whether to opt for insulin pump treatment. For one participant, it meant a difficult decision on whether to leave a clinic with healthcare professionals who were trusted but did not provide this treatment option, for another participant, the pump would be a reminder of their illness, yet for another participant, they found it was the best decision as the pump enabled self-control and efficiency (Pyatak, 2011).
In general, non-adherence to medication was common for many participants, and a variety of reasons led to this decision. As mentioned previously, rebelling was a common reason for participants non-adherence (MacDonell et al., 2015), while some others felt they could control their condition without medication (MacDonell et al., 2015). Making decisions is a way of focusing on what is important to emerging adults with LTPC, regardless of whether this results in self-management decisions that have a negative or positive impact. For example, one participant who took “vacation” from treatments “at this point, I make it such a small part of my life, that I can’t do this minimal amount of care forever. It wouldn’t be healthy” (Pyatak, 2011, p. 464).
Analytical Theme 4: The Age of Feeling In-Between
The Age of Feeling In-Between is reflected in how emerging adults living with and self-managing LTPC, during emerging adulthood, can often feel “in-between” adolescence and adulthood, and feeling not yet adult. In addition, it is a time when they may be treated by others as “not yet an adult” in the carrying out of their self-management tasks. The age of feeling in-between was evident in self-management strategies and tasks across five papers (Garvey et al., 2014; Kamp et al., 2019; Markowitz et al., 2019; Pyatak et al., 2013; Ritholz et al., 2014).
Descriptive Theme: Feeling Not Yet Adult
Feeling not yet like an adult and its interaction with self-management was evident in four papers (Garvey et al., 2014; Kamp et al., 2019; Markowitz, 2019; Ritholz et al., 2014). Some participants felt intimidated by the change to adult healthcare and the expectation that they are now expected to be fully responsible for themselves, for example “It’s [college] a vulnerable time […] whoever your doctor is, just because you’re assigned as an adult doesn’t mean you’re necessarily ready to face adult situations” (Garvey et al., 2014, p. 194). In addition, feeling in-between was found in one paper to correlate with medication adherence. Kamp et al., (2019) used the Inventory of Dimensions of Emerging Adulthood scale (Baggio, et al., 2014) and found that those with lower levels of feeling in-between tended to have better medication adherence while those with higher levels of feeling in-between were more likely to be non-adherent.
Descriptive Theme: Treated by Others as “Not Yet an Adult”
Some participants found themselves not being treated like an adult in relation to their self-management, sometimes by healthcare professionals and other times by family; this was highlighted in two papers (Garvey et al., 2014; Pyatak et al., 2013). Participants reported some healthcare professionals lecturing them if they reported non-adherence and highlighted that the responses were often not relevant to emerging adults’ lifestyle (Pyatak et al., 2013). In relation to family, one participant highlighted how their mother was still attending medical appointments and monitoring them at home even though they were in adult care (Garvey et al., 2014, p. 714).
Analytical Theme 5: The Age of Possibilities
Emerging adulthood while being a time of instability is also the time of greatest opportunity for emerging adults living with LTPC. It is full of possibilities, has an availability of choices about the future and filled with high hopes and expectations. In relation to self-management, there is the freedom to choose to do what suits them in relation to their lifestyle at a moment in time, even if it may negatively affect their health in the future. There is the ability to be optimistic about a future full of possibilities even living with LTPC which can encourage emerging adults to develop a positive attitude about their condition and the self-management of said condition. The age of possibilities was evident in self-management strategies and tasks across 16 papers (Ersig, 2019; Fredette et al., 2016; Hanna et al., 2014a, 2014b; Higham et al., 2013; Johnson & Annesi, 2018; Labore et al., 2017; MacDonell et al., 2015; Pyatak, 2011; Pyatak et al., 2013; Ramchandani et al., 2019; Saylor et al., 2019, 2022; Skedgell et al., 2021; Sparud-Lundin et al., 2010; Vallis et al., 2018).
Descriptive Theme: Availability of Choices
Being a time of many possibilities can provide choices for emerging adults, before making the self-management decision that suits them. This was evident across five papers (Johnson & Annesi, 2018; MacDonell et al., 2015; Pyatak, 2011; Pyatak et al., 2013; Saylor et al., 2019). It may be as simple as the choice to take medication or not (MacDonell et al., 2015) or for others, feeling overwhelmed by having too many choices available which often led to poor self-management decisions. For example, in participants living with obesity, being away from home meant they could eat what they wanted when they wanted or being on “all you can eat” meal plan at college “it is easy to just go to the commons [dining hall] and eat all the unhealthy food” (Johnson & Annesi, 2018, p. 7).
Descriptive Theme: Being Optimistic
Being optimistic about living with LTPC and in carrying out self-management strategies and tasks was evident across seven papers (Ersig, 2019; Fredette et al., 2016; Pyatak, 2011; Pyatak et al., 2013; Skedgell et al., 2021; Sparud-Lundin et al., 2010; Vallis et al., 2018). Being hopeful can help emerging adults living with LTPC be confident about the possibility of managing their condition in the future and about their overall future (Skedgell et al., 2021). Several participants identified optimism as helping them to change from negative to positive ways of thinking leading to them to be successful with their goals, such as improved glycaemic control (Fredette et al., 2016). However other participants tended to be overly optimistic about the possible consequences of poor self-management behaviour, even when they knew the most probable outcome was negative, for example, being in denial about the consequences of high blood sugar or “hoping that should an emergency arise, emergency medical services will be able to assist me” (Ersig, 2019, p. 15).
Descriptive Theme: Positive Attitude
Having a positive attitude allowed participants to not catastrophise about their condition which allowed them to stay open to possibilities and be hopeful. This was evident across eight papers (Fredette et al., 2016; Higham et al., 2013; Labore et al., 2017; Markowitz et al., 2019; Pyatak, 2011; Ramchandani et al., 2019; Saylor et al., 2019; Skedgell et al., 2021). This positive attitude was often seen in self-talk by participants, to stay in the present moment, which is an important self-management tool, rather than worrying or catastrophising about the future (Higham et al., 2013; Labore et al., 2017). For one participant their positive attitude has come from learning about diabetes and allows them to view their condition in a positive light “I donate to the cause and I do walks and I have been able to meet a lot of people too … it seems that’s been a positive … a network and feeling like I have a cause I care about” (Fredette et al., 2016, p. 1604).
Discussion
This review found that the five features of emerging adulthood are present in the self-management strategies and tasks of emerging adults living with LTPC. Furthermore, emerging adulthood is an unstable and diverse time, with many life transitions for those living with an LTPC that requires a balancing act which can pose challenges to successful self-management, sometimes increasing the risks to current and long-term health.
In this review, the emerging adulthood feature, the age of identity exploration, was strongly evident in self-management, as emerging adults with LTPC found out who they were while navigating relationships and building their self-confidence. Exploring one’s identity is a complex process that can be further challenged with LTPC. Some emerging adults living with LTPC strived to “feel” normal (Higham et al., 2013) and of these, some felt it was important to fight against being different (Higham et al., 2013) sometimes making decisions that led to poorer self-management. For others, the stigma of living with LTPC led to hiding self-management tasks from view, even at times, missing carrying them out altogether (Hanna & Hansen, 2020). Importantly however, being accepting of their condition and incorporating it into their identity had a positive impact on self-management for some emerging adults (Hanna et al., 2014b; Skedgell et al., 2021).
Emerging adulthood is a period during which emerging adults are exploring and expanding their networks beyond the family (Hopmeyer et al., 2022; Wiebe et al., 2016). Previous research has highlighted that in addition to being important for the transition to adulthood, navigating shifting interpersonal influences and changes to support systems (e.g., familial support) is also important for the self-management of LTPC during emerging adulthood (Rasalingam et al., 2021; Shelley et al., 2020; Wentzell et al., 2020). This review provides support for this in highlighting the changes in support systems (e.g., college peers) and how relationships, especially family, can act either as a facilitator or as a barrier to self-management. It also finds that for emerging adults with LTPC, their ability to self-manage is key to building their confidence and further developing their sense of self. Emerging adults reflected on positive facilitators that allowed them to take on more self-management responsibilities with increased confidence as they became more independent, such as supportive parents (Labore et al., 2017), peers taking on more important support roles (Ersig, 2019) and new healthcare relationships with professionals that understand the lifestyle issues of emerging adulthood (Markowitz et al., 2019; Pyatak, 2011). On the other hand, other emerging adults highlighted relationship barriers that affected their ability and confidence to self-manage such as too much parental control (Campbell et al., 2019; Pyatak et al., 2013), continued reliance on parents to carry out self-management tasks (Skedgell et al., 2021; Sparud-Lundin et al., 2010) and some highlighted their need for more developmentally appropriate healthcare (Garvey et al., 2014; Pyatak et al., 2013). Future research on emerging adults living with LTPC should consider how navigating relationships may impact the ability of an emerging adult to take on responsibility for self-management tasks and the important role this plays in forming their identity as an adult.
The age of instability brings numerous life transitions, as emerging adults are transitioning to college or the workplace, moving out of home and expanding social and support networks (Wiebe et al., 2016). Previous research has found that during this period emerging adults have many competing priorities (Audulv et al., 2009) and those living with LTPC need to consider and be cautious of their social environment and balance it with their treatment regime (Shelley et al., 2020). The findings of this review highlight that emerging adults living with LTPC also have many life transitions and that these transitions and new schedules (e.g., college, work, moving out of home), can have a negative effect on the ability to carry out self-management tasks (e.g., taking medication, eating habits, rest and exercise) (Ersig, 2019; Johnson & Annesi, 2018; Saylor et al., 2019, 2022). Furthermore, the newfound independence and freedom to socialise can make this a time of experimenting and taking risks (Arnett, 2004a; 2004b) which can also impede the carrying out of self-management tasks (e.g., drinking alcohol and/or staying up late) and may pose a risk to health (Garvey et al., 2014; Hanna & Hansen, 2020; Saylor et al., 2019; Skedgell et al., 2021). The existing evidence does not elucidate how instability might vary between emerging adults; however, the findings suggest that it is important to consider how unstable this period may be and how it is a time of heightened experimentation and risk-taking, in order to develop a more developmentally appropriate level of support for self-management.
The age of self-focus allows emerging adults the freedom from restrictions and obligations to focus on themselves and learn how to become self-sufficient (Arnett 2004a, 2004b). Reflective of this period of self-focus is that the two most valued criteria regularly reported in previous research by emerging adults for becoming an adult are accepting responsibility for themselves and making independent decisions (Arnett, 1997, 1998; Sharon, 2016). Accepting responsibility and making decisions are also both important skills for successful self-management (Lorig & Holman, 2003). In line with this, this review highlighted the relevance of this feature of emerging adulthood in the self-management strategies and tasks for people with LTPC. For example, the findings provide evidence that emerging adults living with LTPC know that they need to take responsibility for their own healthcare and self-management as they become more independent from their parents (Ramchandani et al., 2019), and often begin a trial-and-error process (Saylor et al., 2019) that enables them to begin to implement plans and routines that fit in with their busy lives (Hanna & Hansen, 2020; Skedgell et al., 2021). However, others are at the beginning of learning how to become self-sufficient in their self-management and may not be sure of where or how to start (Pyatak et al., 2013), thus requiring more support. Similarly, this review shows that for decision-making related to implementing self-management strategies, emerging adults often need non-judgmental support that considers their lifestyle, such as considering the reasons behind the decision to be non-adherent to medication, for example, the experiences of side effects and signs of burnout (MacDonell et al., 2015). Understanding how self-sufficient an emerging adult is in their ability to self-manage and furthermore, considering what their lifestyle needs are (e.g., schedules, socialising) for their self-management decision-making process can help healthcare professionals to determine what level of self-management support is necessary.
The age of feeling in-between is about how emerging adults feel “on the way” to adulthood but not quite there, feeling “in-between” adolescence and full adulthood (Arnett, 2001; Reifman et al., 2007). The findings of this review show that emerging adults living with LTPC feel “in-between” and can feel intimidated and not fully ready for the challenges of adult healthcare and taking on self-management responsibilities (Garvey et al., 2014; Ritholz et al., 2014). Only one study (Kamp et al., 2020) used a designated emerging adult measure, a shortened version of the Inventory of Dimensions of Emerging Adulthood scale (Baggio et al., 2014) and importantly found those who scored higher on “feeling in-between” had higher levels of non-adherence to medication. In addition to feeling in-between, some emerging adults found themselves not being treated as adults by parents and/or some healthcare professionals which could also act as a barrier to taking on self-management responsibilities (Garvey et al., 2014; Pyatak et al., 2013). Future research should consider using an emerging adulthood scale to examine to what extent an individual might be experiencing each of the five features and how this relates to taking on self-management responsibilities.
While emerging adulthood is an unstable developmental period it is also a time of possibilities with many choices available to emerging adults for how to live their lives and what paths to take to get to adulthood (Arnett 2004a, 2004b). This review found that emerging adults with LTPC can face a range of choices in relation to how they proceed with self-management strategies and tasks. Some emerging adults make their choice based on what fits their busy lifestyle which might lead to a risky decision, such as not taking medication (MacDonell et al., 2015). Others, when faced with a range of choices can feel overwhelmed, resulting again in a poor decision (Johnson & Annesi, 2018). However, this is also a time for optimism and positivity. This review found that optimism for emerging adults living with LTPC can work in two ways in relation to self-management. Firstly, some emerging adults were optimistic about their future and believed that self-managing LTPC would not hold them back nor narrow their future possibilities (Skedgell et al., 2021). While secondly, other emerging adults tended to be in denial about the consequences of risky health choices in their self-management, being overly hopeful and optimistic about a positive outcome (Ersig, 2019; Pyatak et al., 2013). In line with previous research (Rasalingam et al., 2021), this review found that having a positive attitude, particularly by focusing on staying in the present moment helped emerging adults worry less about living with and managing their LTPC into the future and kept possibilities open (Higham et al., 2013; Labore et al., 2017). It might be beneficial for healthcare professionals to capitalise on emerging adults’ ability to see this period positively as a time of opportunity and work to create positive attitudes around self-management and the future.
Limitations
There were a number of limitations to this review. Firstly, only English language papers were included which means some important results may have been missed through publication bias. Secondly, as it is recommended by Hong et al., 2018, in the quality appraisal, papers are not assigned grades for how low or strong they are methodological-wise. This may mean that some low-quality papers may have contributed little to the overall aim. Thirdly, we chose only to include papers on emerging adults aged 18 – 29 years, it is possible that parents, peers and healthcare professionals may have useful information to add. Finally, the quantitative papers had limited data which may have limited their contribution to the synthesis.
Conclusion
This systematic review highlights the importance of researching emerging adults living with LTPC as a group that is distinct from adolescence or adulthood, as many of the challenges faced, fall “in-between” those experienced by either adolescents or full adults. It found that emerging adults living with LTPC experience the five features of emerging adulthood within the context of their self-management. Emerging adults living with LTPC engage with self-management strategies but can face challenges due to the many transitions that make this a highly unstable development period. A greater understanding of how much an emerging adult living with LTPC is experiencing emerging adulthood, in that, to what extent each of the five features are present and of the challenges posed to self-management (e.g., social support) would inform and assist healthcare professionals in providing support and designing more targeted self-management supports or interventions in the future.
Supplemental Material
Supplemental Material - Self-Management of Long-Term Physical Conditions During Emerging Adulthood: A Systematic Review
Supplemental Material for Self-Management of Long-Term Physical Conditions During Emerging Adulthood: A Systematic Review by Orla Mooney, Veronica Lambert, and Pamela Gallagher in Emerging Adulthood.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Transparency and Openness Statement
As this is a systematic review there is no raw data collected and this review was not pre-registered.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
![]() ).
).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
