Abstract
Due to the psychological toll COVID-19 has had on emerging adults, as well as normative mental health challenges of this developmental period, emerging adults are struggling more than ever with depression and loneliness. The objective of this study was to assess feasibility, acceptability, and preliminary psychosocial outcomes of Embracing Your Life, a self-compassion program for emerging adults, as self-compassion is associated with better mental health. Thirty-nine emerging adults (Mage = 23.7, 67% female) enrolled in a 6-session online program from July 2020 to January 2022 participated in this study. Results indicated the program was feasible; 81% of participants attended at least five out of six sessions. Qualitative feedback indicated high acceptability, with recommended changes to make the program more interactive. Participants reported significant improvements in self-compassion, resilience, loneliness, depression, stress, and emotion regulation. Conclusions are that Embracing Your Life is a promising, accessible intervention to address the mental health of emerging adults.
Keywords
Introduction
Emerging adulthood is a transitional time in development in which one is faced with an array of normative challenges that present new demands and stressors (Arnett, 2000). As many emerging adults navigate the adjustment to this period of educational and professional growth, they face the challenges of gaining academic qualifications, preparing to enter the workplace, and often economic uncertainty. Additionally, emerging adults frequently are moving away from their family home for the first time, leading to greater responsibility to manage their own emotional and physical health in a new environment. Changes in relationships and access to social support during this transitional period contributes to cumulative stress and heightened expectations on emerging adults. Furthermore, research findings on mental health of emerging adults over the years from 2011-2018 demonstrates that mental health appears to be worsening, and elucidates a disturbing trend of increases in depression, anxiety, non-suicidal self-injury, suicidal ideation, and suicide attempts (Duffy et al., 2019).
Exacerbating this alarming trend, the recent coronavirus (COVID-19) pandemic introduced a context in which emerging adults suffered from the psychological impact of the pandemic due to the disruption to daily life and restrictions on professional and social activities (Killgore et al., 2020; Liu et al., 2020). In fact, according to a study of a cross-national sample assessed in the early months of the pandemic, loneliness, anxiety, depression, and stress were highest among emerging adults compared to middle-aged adults and older adults, and loneliness and lower resilience mediated the relationship between stress and both anxiety and depression (Varma et al., 2021). Thus, in the context of COVID-19, increased stress was linked to increases in loneliness and decreased resilience, which subsequently was associated with increases in anxiety and depression. Confirming these findings, another study conducted in the first week of the pandemic reported that 61.5% of adults (18–35 years old) felt “socially isolated much of the time,” and loneliness was linked to an increase in depression and higher levels of suicidal ideation (Killgore et al., 2020). As the pandemic progressed, related mental health challenges continued. According to a large, longitudinal study of a national sample of college students, in the 2020-21 academic year depressive symptoms increased by 135% and anxiety increased by 110% compared to 2013 rates (Lipson et al., 2022).
Social support has been shown to be instrumental in the protection against the impact of perceived stress and loneliness in young adults (Lee & Goldstein, 2016) and especially relevant in times of adversity and uncertainty (Schwarzer & Knoll, 2007). Yet clearly, face to face social support was less available during the pandemic. Social isolation, on the other hand, was pervasive throughout the pandemic (Kim et al., 2022); whether measured objectively (i.e., living alone, having infrequent social contact) or subjectively (i.e., the experience of feeling lonely), social isolation has been shown to not only be associated with poor mental health but also significantly increase the risk for mortality, comparable to the risk factors of smoking and alcohol use, and exceeding the effects of obesity (Holt-Lunstad et al., 2010). Thus, the impact of the pandemic on emerging adults was likely deleterious in terms of the psychological effects, perhaps more so than the physical effects of the coronavirus itself.
In addition to loneliness and social isolation, one factor that has long been associated with depression and anxiety is difficulty with emotion regulation. Emotion regulation has been broadly defined as one’s attempts to modulate one’s emotions (e.g., intensity, duration, or expression) using adaptive (helpful) or maladaptive (leading to prolongation or exacerbation of difficult emotions) strategies in the service of modifying emotional experiences (Aldao et al., 2010) For example, suppressing or avoiding emotions is a strategy considered maladaptive and linked to psychopathology, while cognitive reframing or problem solving are considered adaptive strategies used to modify emotions. Others have described emotion regulation in terms of specific skills, such as the ability to be aware of, label, understand the reasons for, and tolerate emotions (Berking et al., 2014). Difficulties with emotion regulation are considered key transdiagnostic factors (i.e., factors that are present across disorders) that involve challenges with both skills and strategies, including awareness, understanding, and acceptance of emotions, the ability to refrain from impulsive behavior in the context of negative emotions, and the flexible use of regulation strategies that may be helpful in any given context (Gratz & Roemer, 2004). In emerging adults, difficulties with emotion regulation are not only associated with anxiety and depressive symptoms, (Semborski et al., 2021) but have also been associated with unhealthy behaviors such as problematic alcohol use (Dvorak et al., 2014) and internet addiction (Hormes et al., 2014). Thus, resourcing emerging adults with emotion regulation skills and adaptive strategies may have broad implications on both mental health and functioning.
Given the pervasive deterioration of emerging adults’ mental health at a time of key developmental transition, there is an urgency to bolster the resources available to support this age group (J. Lee et al., 2021). Self-compassion is an internal resource that could be an accessible and effective transdiagnostic target of intervention for emerging adults. According to Neff (2023), self-compassion is a way of relating to oneself during difficult experiences that is defined by a dynamic interaction of three interconnected components: (1) mindfulness (i.e., viewing difficulty with an open, nonjudgmental perspective); (2) common humanity (i.e., holding one’s pain within the larger context of the shared human experience); and (3) self-kindness (i.e., demonstrating care and support toward oneself in difficult moments). Higher levels of these three adaptive components are balanced by corresponding lower levels of three maladaptive components: (1) overidentification (i.e., getting ‘caught up’ in the difficult emotion); (2) isolation (i.e., feeling alone in the experience of emotional pain); and (3) self-criticism (i.e., responding to difficulties with harshness or self-judgement). Together, higher levels of compassionate responding and lower levels of uncompassionate responding are considered beneficial for coping with life’s challenges with greater ease and resilience (Neff, 2023). Self-compassion can also be thought of treating oneself with the same kindness and support as one treats a good friend when struggling. For example, if an individual failed an important exam, rather than over-identifying (i.e., “I always make such stupid mistakes on exams! I’ll never graduate and get a decent job!”), one can be mindful (i.e., “This was disappointing, but I know this one exam doesn’t define me.”). Instead of succumbing to feeling isolated (“I’m sure I’m the only one who did this poorly!”), one can remember common humanity, that not performing well at times is part of being human (“Everyone messes up sometimes.”). Finally, rather than responding with self-judgement (i.e., “I’m such a failure!”), one can respond with self-kindness (i.e., “It’s okay to be imperfect. I can learn from this, and I trust I can do better on the next one.”).
Meta-analyses of studies conducted in adult and adolescent populations have found that greater self-compassion is linked to reduced psychopathology (i.e., depression, anxiety, stress, non-suicidal self-injury, suicidal ideation) with moderate to large effect sizes (MacBeth & Gumley, 2012; Marsh et al., 2018; Suh & Jeong, 2021). In particular, self-compassion provides an alternative response to difficult emotional challenges, which contrasts with self-criticism, which is a key predictor of depression and anxiety (Neff, 2023; Neff et al., 2007). Self-compassion has been shown to support mental health via the use of skills and adaptive strategies that one uses to regulate difficult emotions (Finlay-Jones, 2017; Inwood & Ferrari, 2018). For example, self-compassion has been associated with improved tolerance of negative emotions (Diedrich et al., 2017), lower levels of rumination and worry (Raes, 2010), and higher levels of emotion-related skills such as emotional understanding, clarity, and acceptance (Paucsik et al., 2022). In addition, self-compassion has been inversely associated with emotion regulation difficulties in general for populations of emerging adults exposed to adversity (Prentice et al., 2021; Vettese et al., 2011).
Moreover, self-compassion has been linked to positive emotional states and capacities such as greater happiness, positive affect, life satisfaction (Zessin et al., 2015), and greater resilience, or the ability to adapt to or bounce back from challenges. Self-compassion is also associated with greater social connectedness (Neff, 2003b; Neff et al., 2007; Smeets et al., 2014), and more recently, to reductions in psychopathology and loneliness over a 5-year time span (E. Lee et al., 2021). Self-compassion provides an internal support system that is available even under the constraints of social distancing and disconnection that were prominent during the height of the pandemic; research conducted during this period demonstrated the role self-compassion played in alleviating the emotional pain of loneliness than many experienced due to working from home (Andel et al., 2021). Self-compassion mitigated the relationship between work loneliness and depression perhaps by giving employees the perspective to cope with the challenges they were facing with greater kindness and understanding (Andel et al., 2021).
Considering these benefits and the state of their mental health, it may be advantageous for emerging adults to learn to be more self-compassionate. Fortunately, self-compassion is a learnable skill that can be fostered through intervention. Mindful Self-Compassion (MSC) is an 8-session program that was created to teach adults how to cultivate self-compassion skills and has been empirically tested in a range of contexts (Friis et al., 2016; Neff & Germer, 2013). Similarly, an adaptation of MSC has been developed and tested for adolescents (Bluth & Eisenlohr-Moul, 2017; Bluth et al., 2016; Bluth et al., 2023). Both programs have demonstrated significant improvements in mental health outcomes, such as depression, anxiety, stress, resilience, and life satisfaction. Further, a meta-analysis of 27 randomized controlled trials of self-compassion interventions – programs that ranged from short inductions 10 minutes in length to the more in-depth 8-week Mindful Self-Compassion program - demonstrated large effect sizes for rumination and eating disorders, and moderate effects for self-compassion, stress, depression, and anxiety, compared to controls (Ferrari et al., 2019). Authors concluded that self-compassion interventions “appear to foster improvement across a range of both clinical symptoms and indicators of wellbeing” (p. 1468).
Unfortunately, however, many of these self-compassion programs have not yet made their way onto college campuses and to emerging adults in general, or at least to the extent that they are able to reach many of those who need them. Further, existing self-compassion programs developed for adults and adolescents require a significant time commitment which may be too demanding for busy college students (adults, 24 hours; adolescents, 12 hours). The new curriculum, Embracing Your Life: A Mindful Self-Compassion Program for Emerging Adults, is shorter and requires only a 9-hour commitment over 6 weeks. It also includes exercises that are specifically relevant to emerging adults (i.e., reflecting on the effects of social media use). Moreover, it was designed prior to the pandemic to be taught online as most emerging adults are tech-savvy and communicate easily in online platforms.
Our research questions are: 1. Is Embracing Your Life: A Mindful Self-Compassion Program for Emerging Adults feasible and acceptable to this population? 2. Does Embracing Your Life improve psychosocial outcomes of depression, anxiety, stress, loneliness, resilience, and emotion regulation?
Methods
Participants and Procedure
Demographics (n = 39).
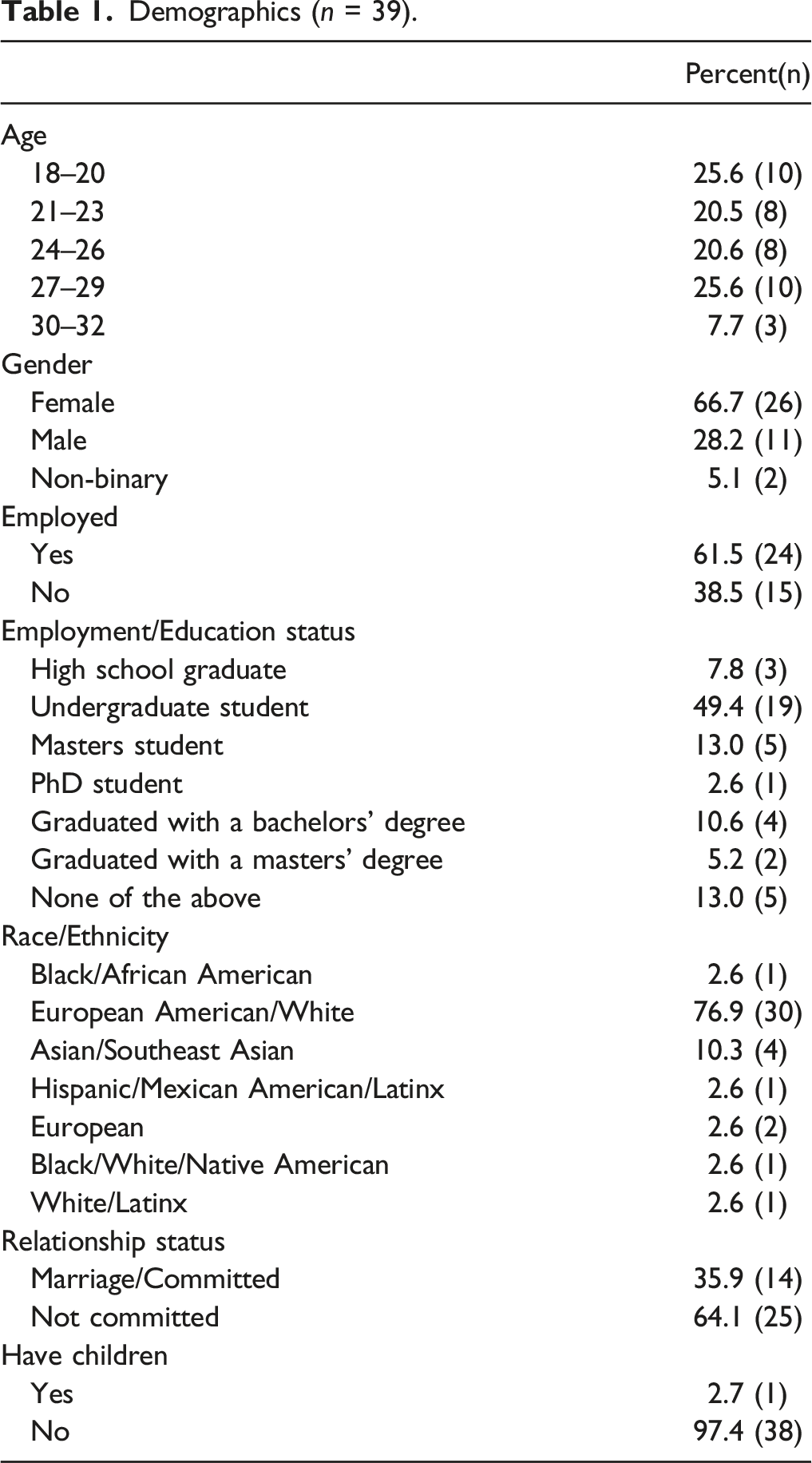
Measures
Feasibility and Acceptability
Feasibility was assessed through attendance (i.e., 80% of participants attending five out of the six sessions) and 75% retention (completing the post-survey). Acceptability was assessed through qualitative feedback provided through open-ended questions at the end of the post-survey.
Qualitative Methods
Within the post-intervention survey, participants were provided with a space to respond to the open-ended questions: “Overall, what did you like or dislike about the program? Is there anything you think we should do to change it?” Participants were provided space for comments. Thirty participants provided open-ended comments.
De-identified comments were compiled and uploaded into Atlas.ti Windows version 23. Author CL, a white, middle aged, cisgender, female assistant professor with a personal self-compassion practice and with qualitative and self-compassion research experience, followed the six steps of Braun and Clarke’s thematic analysis (2012), in an iterative fashion, as described below. Thematic analysis was chosen because the approach is flexible (e.g., allows both use of researcher-derived codes and codes derived from the data) and is useful in making sense of a collective experience by “identifying, analyzing and reporting patterns (themes) within the data.”
In step one, the analyst read through all data multiple times to become familiar with the content and made notes. In step two, the analyst developed initial codes, which were primarily inductive (derived from the data), but also included three codes based on the open-ended survey questions: (1) positive aspects of the program; (2) challenges with the program; and (3) recommended changes to the program. This resulted in a total of 35 initial codes, which were primarily descriptive (e.g., “needs adaptation for age”) or contained information about what the participant might value (e.g., “fit into life”). In step three, searching for themes, the codes were organized into three overarching themes as mentioned above (program positives, challenges with the program and recommended changes). Subthemes were created by re-reading the data, merging and splitting of codes, and placing reformatted codes into appropriate subthemes. For example, codes “positive instructor qualities,” “safe space,” and “peer connection” were merged to form the subtheme “warm and connected atmosphere.” This process resulted in three overarching themes, five subthemes, and 14 codes. In step four, reviewing themes, theme groupings were re-arranged and finalized after reviewing the entire data set to ensure that they represented the body of data. At this point, co-authors provided input on a codebook which described themes, subthemes, codes and their definitions and sample quotes. In step 5, final themes and subthemes were defined and named with input from co-authors. In the final step, the report was generated.
Intervention
The content in the program Embracing Your Life: An Online Self-Compassion Program for Emerging Adults (EYL) is drawn from both the Mindful Self-Compassion program for adults and Mindful Self-Compassion for Teens. EYL was designed to be taught online, and is comprised of six sessions, each of which is 1.5 hours in length (9 hours total). Each session has a theme, and incorporates didactic teaching, guided meditation practices, group discussion, and exercises. Home practice is assigned and encouraged. The six sessions are: 1. Discovering Mindful Self-Compassion – Includes a discussion of how to approach the course and group guidelines, provides an introduction to mindfulness and self-compassion, an introduction to the guided meditation Compassionate Friend, and to Supportive Gestures practice. 2. Paying Attention with Kindness – Doubts about self-compassion are discussed, mindfulness and lovingkindness practices are introduced. 3. Self-Compassion – Reasons why we criticize ourselves are discussed and how we can motivate ourselves with self-compassion rather than self-criticism is elicited through an exercise. A brief body scan and music meditation are included. 4. Self-Compassion vs. Self-Esteem – The difference between these two constructs is discussed, and an exercise on how to contend with our natural tendency for social comparison, especially through social media, is introduced. An exercise which strengthens the ability to accept oneself is presented. 5. Living Deeply – An exercise elicits one’s core values, obstacles to those values, and how self-compassion can help one to live more in agreement with their core values. 6. Embracing Your Life – How to capture and savor joy in one’s life is the focus of this session. Gratitude practice is introduced, and a wrap-up exercise of the class is completed.
Analytic strategy
All statistical analyses were conducted with SPSS version 28 (Armonk, NY). Prior to analyses, all variables were checked for distributional assumptions; for example, all outcome variables were found to be normally distributed. No outliers were removed, and only those who provided both pre-and post-data were included in analyses. As this was a feasibility study and was the first study conducted on this novel intervention, psychosocial outcomes were exploratory and we did not conduct a power analysis. Paired t-tests were conducted to ascertain changes in means from pre-to post-intervention. Hedges’ g was calculated to determine effect size; similar to Cohen’s d, Hedges’ g includes a correction factor for small samples. Conventional interpretation of effect sizes is 0.20 = small, 0.50 = medium, and 0.80 = large (Borenstein et al., 2009; Cohen, 1988).
Results
Feasibility
We expected at least 80% of the participants to attend at least five out of the six classes to indicate feasibility, and at least 75% to be retained in the study. This is comparable to that which is indicated in similar studies in this age (MacDonald & Neville, 2022). In total, 52 participants enrolled in the Embracing Your Life study over six cohorts from July 2020 to January 2022 and attended the first of the six classes. Of those, 81% (n = 33) attended at least five classes. Participants were considered “completers” if they completed the post-survey, and 75% (n = 39) met the criteria.
Acceptability
Qualitative comments to open-ended prompts were provided by 30 of 39 participants. Authors grouped comments into three main themes: (1) Positives about the program; (2) Challenges with the program; and (3) Recommended changes to the program. Each theme is grouped into subthemes and described below.
Positives about the program
This theme refers to any positive comment about participants’ experience with the program or perceived benefits occurring outside of the program. This theme is grouped into two subthemes: warm, connected program atmosphere and EYL program material.
Warm, connected program atmosphere
Many participants described the warm, connected atmosphere of the EYL online group as a positive aspect of the experience. The group was described as “welcoming and inclusive,” “a safe space to learn,” and non-judgmental. Important contributors to this atmosphere were the characteristics of the facilitators. One described the facilitators as bringing a sense of “patience and acceptance”; another noted the facilitators fostered “a level of respect and interest.” Yet another participant cited they felt motivated and encouraged by the way that the facilitator offered or invited rather than pressured participants to speak during sessions or to do home practices. In addition, for one participant, “the frequent mentioning of scientific studies” by the facilitators appeared to add to their comfort with and enjoyment of the program.
Another major contributor to the positive atmosphere was peer connection. In particular, being with peers rather than a mixed-age group helped the participants to bond and accentuated the feeling of common humanity. One participant said, “Meeting people who are experiencing the same feelings of inadequacy that you have is a nice reminder that you’re not alone.” Indeed, this aspect was so important that many wished for more opportunities to connect with their peers (see Recommended Changes).
EYL program materials
Many participants expressed that the content of the EYL program was enjoyable and beneficial. Regarding in-class content, participants referred to writing exercises, practices, meditations, music, discussions, videos, and resources provided as interesting, beneficial, or enjoyable. Some activities that were specified were: self-compassionate letter writing, a ‘building your house’ writing exercise that helped to clarify values, and videos on mindfulness and negativity bias. Others expressed that having structured home practice, weekly summary emails with links to recordings, and access to shorter practices were helpful in establishing home practice routines.
Two participants described using skills learned from the program in everyday life. One described a new self-awareness that was useful in coping with difficulties: This program was eye-opening for me. Before I was feeling stuck in my life when I was passing through hard situations and basically, I had no idea of my behavior to myself. As I did not know what the problem was, I could not find my way out of things. After taking the course, I can now see when I behave badly to myself and remember that tools are available.
A second participant, who was admittedly “skeptical” at the start of the program, made similar comments regarding using mindfulness to “approach stressful situations a little bit differently.”
Challenges with the program
Participants also cited the following challenges with the EYL program: (1) one participant did not like going into breakout rooms; (2) one participant found it difficult to use the skills they learned in daily life; (3) one participant did not like the music used during the music meditation; (4) one participant noted some difficulty with several exercises and meditations, and this made them feel isolated from the rest of the group.
Recommended Changes to the Program
Time changes
Three participants would have liked the program to last longer with additional sessions. Two participants would have liked longer session lengths to facilitate more time for participant sharing. One participant would have appreciated session times that accommodated participants in Asia.
Other Changes to Program Structure/Content
Three participants noted that additional resources (e.g., TEDTalks, a reading list, websites, help creating a personalized plan for maintaining skills) for continued learning and sustained practice after the program ends would be helpful. Several participants thought more structure to the program would be an improvement. Some suggestions for this structure included: a weekly “roadmap” of the sessions to help the material feel more connected and “relevant” across sessions; a “small workbook or virtual PDF” to accompany the program; a summary email with all resources listed; daily activities to reinforce self-compassionate talk; and use of an online discussion board, as well as a platform to house program resources. Two participants felt further adaptation for emerging adults is needed, including “something that really supports difficulties we young adults face”- although they did not elaborate on how to accomplish this. Finally, one participant suggested that the program be marketed as an introductory course.
More peer connection
Several participants recommended that the program could be improved through more opportunities for the emerging adult participants to share personal experiences and engage with each other. Some recommendations for increasing peer connection included encouraging each participant to share about how their home practice is going or about their plans to incorporate skills in the upcoming week, including more time for deeper personal sharing/group discussions and more focused prompts for breakout rooms, mixing up people in the breakout rooms so that participants meet different people each time, and creating an online forum for participants to connect outside of the sessions.
Psychosocial Outcomes
Means, Standard Deviations, Cronbach’s alpha and Effect Sizes (Hedges’ g) for All Variables (n = 39).
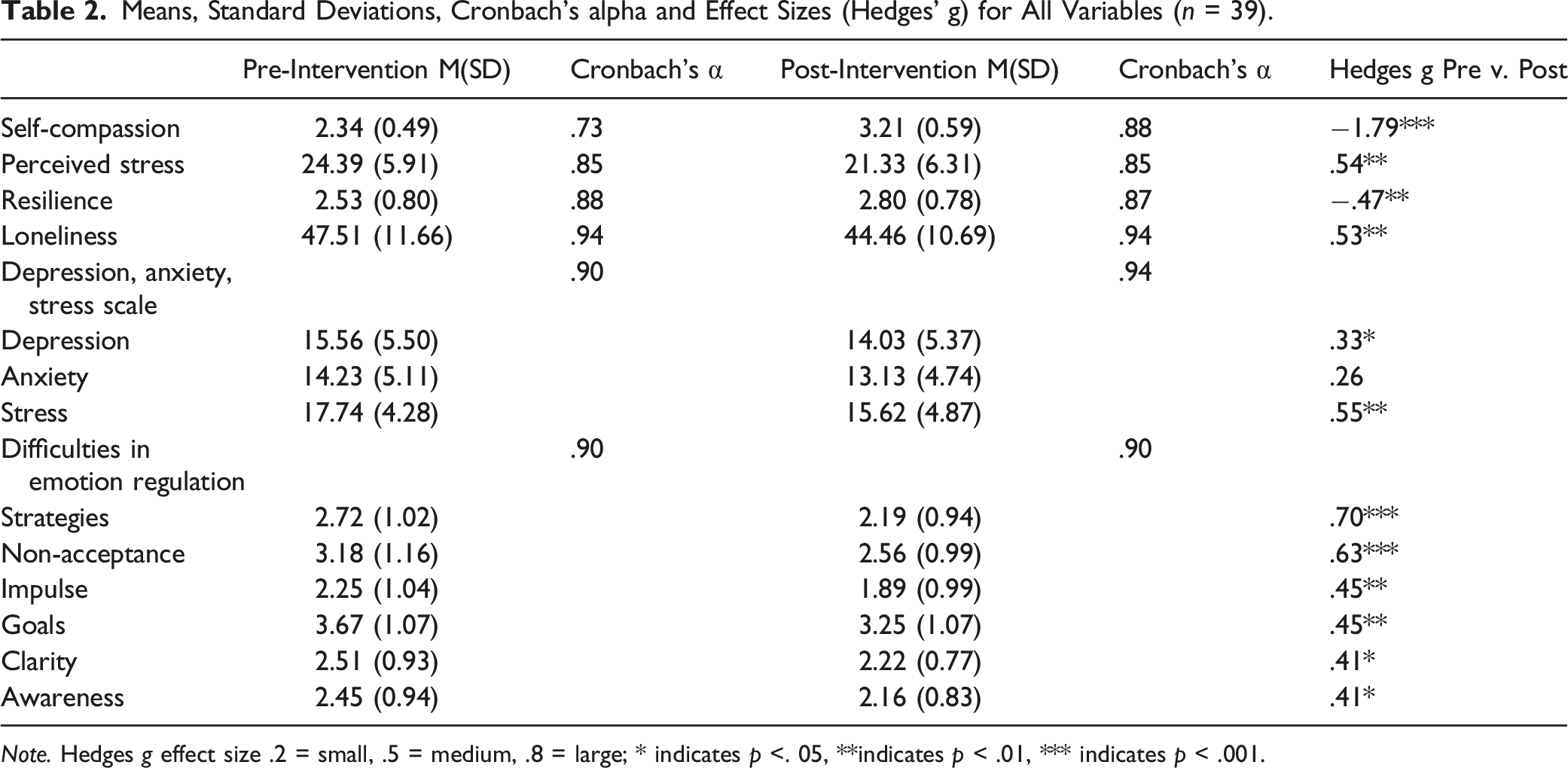
Note. Hedges g effect size .2 = small, .5 = medium, .8 = large; * indicates p <. 05, **indicates p < .01, *** indicates p < .001.
Discussion
This study assessed the feasibility, acceptability, and psychosocial outcomes of a newly created program for emerging adults called Embracing Your Life: An Online Mindful Self-Compassion Program for Emerging Adults. Based on the previously created program Mindful Self-Compassion for adults and its associated program Mindful Self-Compassion for Teens, this program was designed to meet the needs of emerging adults who are often occupied with college or starting careers, and have limited time to engage in a longer, more in-depth program, such as the 24-hour Mindful Self-Compassion program. Also, because most emerging adults are proficient in using technology and familiar with socializing on the Internet, this program was designed to be taught online.
Results indicated that EYL was both feasible and acceptable to emerging adults. Eighty-one percent of those who consented to participate in the study attended at least five of the six classes, and 75% completed the study (i.e., took the post-survey), meeting the criteria for feasibility. Qualitative findings indicated that participants generally liked the course, with most participants indicating the material was beneficial and relevant. In particular, the social connection aspect was valuable and created an emotionally safe space to explore self-compassion skills. To improve the program, they recommended more peer engagement, adaptation for emerging adults, and more opportunity to dive deeper with supporting materials to make the program even more enriching and sustain their self-compassion practice. Efforts are underway to integrate their feedback and address their needs to enhance the program.
Results of psychosocial outcomes demonstrate that those who participated in EYL had overall improvements in their emotional wellbeing. Depression, stress, loneliness, and all aspects of difficulties in emotion regulation decreased from pre to post while resilience and self-compassion increased. Anxiety also decreased but did not reach significance; this finding may in part be related to participation during the height of the pandemic. These results are consistent with self-compassion interventions conducted in various settings with diverse populations that demonstrate self-compassion is beneficial to multiple well-being outcomes (Ferrari et al., 2019).
To fully understand how self-compassion supports emerging adults’ emotional wellbeing, the relationships between the variables measured in this study, and other unmeasured variables, further examination is required. For example, does improvement in self-compassion precede improvements in loneliness and depressive symptoms, or vice versa? Additionally, extant literature suggests that self-compassion may be positively related to well-being via its impact on emotion regulation and the ability to tolerate negative emotions. Thus, increased use of adaptive emotion regulation strategies, and decreased use of maladaptive strategies, may mediate improvements in well-being (Inwood & Ferrari, 2018). Although not measured in this study, both low self-compassion and difficulties with emotion regulation have been linked to trauma exposure and childhood maltreatment in young adults (Barlow et al., 2017; Vettese et al., 2011); thus, future work might explore how higher levels of these experiences impact treatment effects.
The findings related to decreased loneliness post-program are understandable given the salience of peer connection described by participants in the qualitative data. It is possible that being together in a supportive online space with peers at the height of pandemic-associated restrictions contributed to decreased feelings of isolation and loneliness. It is also possible that enhanced self-compassion skills, including the emphasis on common humanity, facilitated decreased feelings of loneliness. Furthermore, self-compassion has been shown to be negatively associated with loneliness among adolescents (Liu et al., 2020), and this relationship is mediated by social anxiety; additionally, self-compassion mitigated the relationship between work loneliness and employee depression among workers during Covid-19 (Andel et al., 2021). Other studies have shown that self-compassion is linked to several other adaptive interpersonal characteristics in emerging adults—including decreased rejection sensitivity (Xie et al., 2022), higher quality relationships (Lathren et al., 2021) and increased feelings of relatedness to and trust of others (Yang et al., 2019). Thus, there are other unmeasured interpersonal factors that may have mediated program effects on loneliness.
The limitations of this study include the small sample size, the relative homogeneity of the participants in gender and race/ethnicity (predominately White females), and unknown variables such as trauma history and socioeconomic status. Additionally, all participants self-selected the EYL program and paid to take this course. This limits the ability to generalize these results more broadly and precludes a full understanding of the characteristics of individuals who benefit the most from participation. Examination of the EYL program in a larger, more diverse sample and compared to a credible, active control condition would further clarify the benefits of the self-compassion content and separate out benefits related to peer connection alone. Finally, it is unknown how the feasibility, acceptability, and outcomes might be affected if this program was offered outside of the context of heightened COVID-19 restrictions.
Despite these limitations, our initial findings are promising. Next steps include confirming results using a larger, diverse sample and comparing it with an active control. In addition, it will be important to understand both how and for whom self-compassion skills are most beneficial, so that programming can be appropriately targeted. Finally, college campuses may offer an ideal setting to reach emerging adults who may benefit from self-compassion skills, particularly to bolster coping during the transition to college (Kroshus et al., 2021) and mitigate the effects of trauma exposure (Shebuski et al., 2020) and chronic academic stress (Zhang et al., 2016). Future work could explore integration of self-compassion programming into existing wellness offerings on college campuses, including through counseling centers, residence halls, and other student-centered programming. These strategies would increase access to a transdiagnostic mental health resource for emerging adults that may be more acceptable and less stigmatizing than individual therapy, and thus address a significant public health issue.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
