Abstract
Background:
The textile industry, a vital sector in Türkiye, exposes workers to numerous occupational risks, including physical, chemical, and ergonomic hazards. The weaving stage, in particular, involves prolonged exposure to chemicals, noise, and dust, posing significant health challenges. Identifying workplace hazards is critical to safeguarding employee health and productivity.
Methods:
This cross-sectional study was conducted in two textile factories in Türkiye. This research investigated perceived workplace risks and related factors to which weaving workers are exposed. Sociodemographics, work-related characteristics and perceptions of chemical, noise, and dust exposures were analyzed. A total of 355 people participated in the study.
Findings:
Nearly three-quarters of participants were male, 40% were smokers, and 55.8% worked over 45 hours weekly. Chemical exposure was reported in 21.1% of workplaces, 75.5% identified noise as a hazard, and 65.9% noted dusty environments. About 19.3% did not use personal protective equipment (PPE), citing discomfort and perceived inefficacy. Health complaints in the past week included skin issues (10.7%), eye irritation (17.5%), hearing problems (12.7%), and respiratory symptoms (11.5%).
Conclusions:
Weaving workers face significant occupational risks, particularly from chemical, noise, and dust exposures. Long-term exposure to these hazards may lead to chronic diseases, reducing workers’ quality of life. Training and preventive measures are essential to mitigate these risks and improve workplace safety.
Application to Practice:
Implementing targeted interventions, such as enhanced workplace planning, safer technologies, regular maintenance, ergonomic support, and comprehensive training programs, can improve health and safety conditions for weaving workers while boosting productivity and reducing healthcare costs.
Background
Approximately 430 million people, 12.6% of the world’s working population, are involved in fashion, clothing, and textile production, with most of them working informally or without job security and benefits typically associated with full-time employment. The global fashion industry is valued at $2 trillion, with exports by the top 10 textile and apparel manufacturers in 2021 totaling almost $8 billion (Solidarity Center, 2023). The textile industry provides extensive employment, has an essential share in the macro economy, and is one of the most critical sectors of the Turkish economy (World Trade Organization, 2023). Besides increasing industrial growth, technological developments bring along several factors that may pose potential health hazards for workers (International Labour Organization, 2022).
The textile sector harbors many hazards and risks in terms of the health and safety of its employees at every stage. The weaving industry is one of the crucial stages in terms of the health of the workers in the textile sector in terms of working conditions and exposure factors (Çat et al., 2022). In the textile weaving process, workers are at risk in terms of exposure to noise, dust, and chemicals (Sivakami & Janani, 2023). During fabric weaving from yarn, workers exposure to dust from materials such as silk, cotton, wool, linen, hemp, and jute may cause various respiratory system diseases (Islam, 2022). Respiratory system diseases such as byssinosis due to inhalation of cotton dust and occupational asthma and bronchitis caused by other organic particulate matter have been observed in weaving industry workers (Chandurkar & Kakde, 2019). Noise exposure is frequent in textile industry workers, especially in developing countries (Abbasi et al., 2011). In addition to hearing loss from exposure to industrial noise, which is generally caused by obsolete machines and failure to take necessary protective measures sleep disorders, anxiety, and occupational accidents due to distraction may also be observed (Sangeetha et al., 2012). Chemicals such as acetic acid, surfactants, cyanide, formaldehyde, sodium chloride, sodium hydroxide, and chlorine-based bleaches are used in the textile industry for different purposes, including product treatment (Pavan et al., 2024). Chemical exposure during weaving processes can cause endocrine-disrupting effects and can lead to liver damage, kidney failure, and cancer (Mohapatra & Gaonkar, 2021).
Globally, limited research has addressed the specific health and safety risks faced by weaving workers, particularly in Türkiye, where the textile industry is a major economic sector (Duran & Temiz Dinç, 2016). While existing studies predominantly focus on the general risks of the textile industry, they often overlook the distinct hazards encountered during the weaving stage, such as combined exposures to noise, dust, and chemicals. This study aims to bridge this gap by identifying and analyzing the workplace risks and contributing factors specific to weaving workers. The findings are expected to guide occupational and environmental health nursing practices by highlighting areas where targeted interventions can prevent occupational diseases and improve workplace safety in this high-risk sector.
Methods
Design and Sample
This cross-sectional study was conducted in weaving factories located in two major textile-producing cities in Türkiye: Bursa and Kahramanmaraş. These provinces rank 3rd and 4th in textile exports among Türkiye’s 81 provinces, reflecting the economic importance of the textile industry in these regions.
The study population included employees who had been working in weaving factories for at least 1 year. The total workforce across the factories was 381 employees, with 194 and 187 workers in two different factories. A total of 355 participants completed the study. Recruitment involved entering the factories and explaining the study objectives to employees. Ethical approval was obtained from Gazi University Ethics Committee on July 10, 2023 (2023-837).
Written informed consent was obtained by the researchers before participation in the study, and voluntary and anonymous responses were ensured. In total, 23 employees were unavailable due to shift work, annual leave, illness, or work assignments, and three employees declined participation over privacy concerns.
Data Collection
Data were collected by the researchers between August 7 and 25, 2023, using a structured questionnaire with four sections comprising 40 questions. The first section contained sociodemographic characteristics and work-related information. In contrast, chemical exposure perceptions were analyzed in the second, noise exposure perceptions in the third, and dust exposure perceptions in the fourth section. No objective workplace environmental measurement method was used.
The answers to the questions related to workplace monitoring were checked and recorded during the visits to the factories with occupational safety experts. Factories were visited at least twice, a checklist was used, records were analyzed, and face-to-face interviews were conducted. One questionnaire took 8 to 10 minutes to complete. Information on health surveillance was obtained by analyzing the health records in the workplace. The questions about the participant’s medical conditions such as skin problems, noise-related hearing problems, respiratory and eye problems were answered during the medical examinations carried out by the workplace physicians, and recorded to the data collection form by the researchers.
Study Variables
The independent variables of the study included gender, age, education level, total and weekly working hours, department of work, smoking, employment, periodic examination, risk factors encountered in the workplace, use of personal protective equipment, occupational health and safety training, presence of protective practices, and health problems arising due to workplace risk factors. The dependent variables of the study are use of chemical resistant personal protective equipment, personal protective equipment for hearing, and respiratory protective mask. After a comprehensive literature review, it was thought that these dependent variables might be related to occupational health and safety training in the last year, and analyzes were carried out in this direction.
Variables related to chemical substances, noise, and dust exposure were analyzed among relevant subgroups of participants who reported being exposed to these specific workplace conditions.
Statistical Analysis
This study aims to bridge this gap by identifying and analyzing the workplace risks and contributing factors specific to weaving workers.
The data obtained were analyzed using the Statistical Package for Social Science (SPSS) for Windows 26.0. Descriptive statistics, including frequencies, percentages, means, ranges, and standard deviations, were used to summarize the sociodemographic, work-related, and exposure characteristics of the participants. For the analysis of categorical variables, Pearson’s chi-square test, Fisher’s exact test, and Yates’ continuity correction were applied to evaluate group comparisons based on their suitability. The level of statistical significance was set at p < .05.
Results
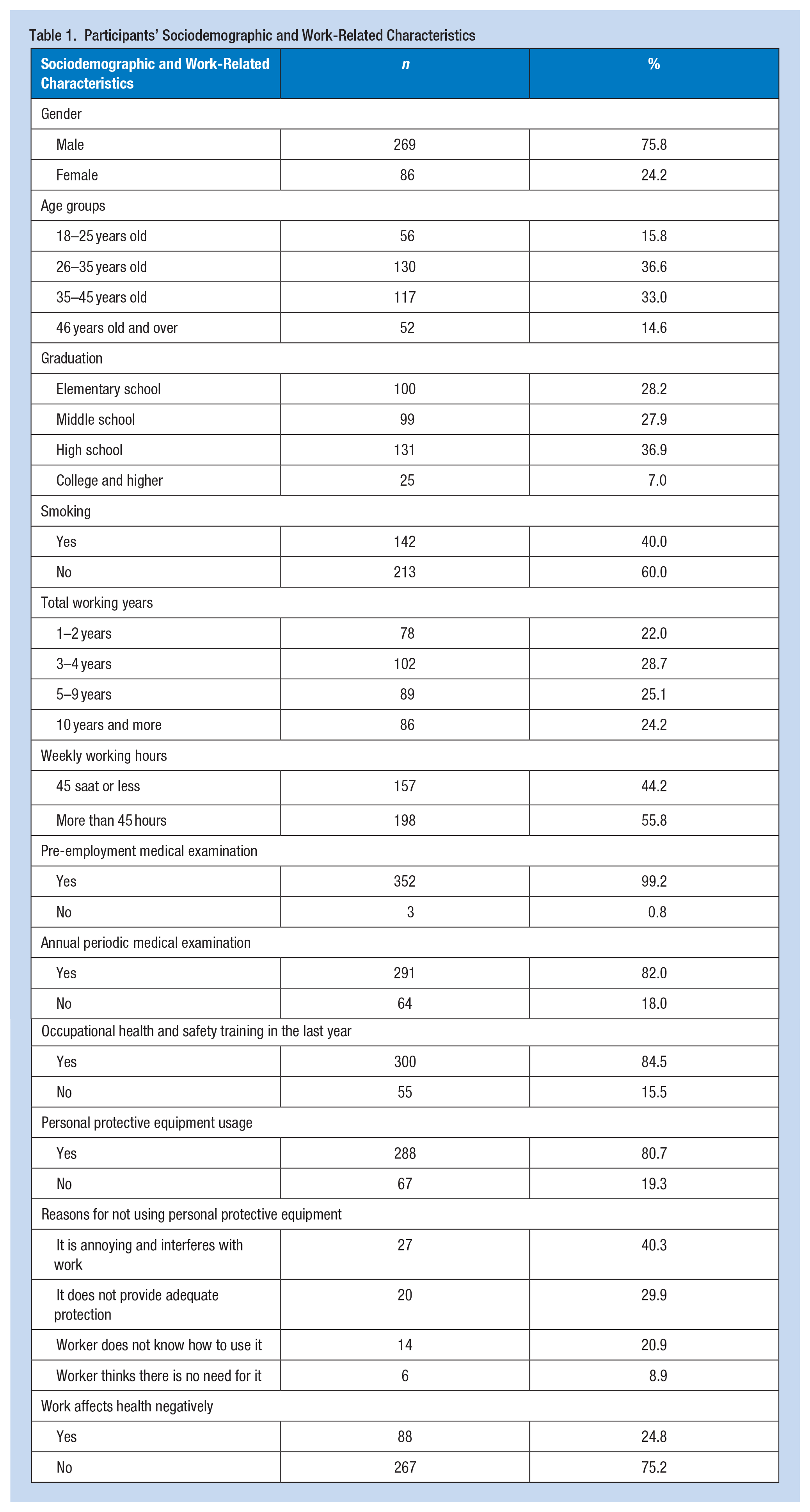
Out of 381 eligible workers, 355 participated in the study, achieving a participation rate of 93.2%. Regarding demographics, three-quarters of the participants were male, 69.6% were aged 26 to 45, 36.9% were high school graduates, and 40.0% were smokers. Half of the participants had a total working period of less than 5 years, while 55.8% worked more than 45 hours per week. In terms of occupational health practices, 99.2% of the participants reported undergoing a pre-employment medical examination, 82.0% reported having an annual periodic medical examination, and 84.5% had received training on occupational health and safety in the last year. Regarding the use of personal protective equipment (PPE), 19.3% of the participants admitted not using PPE while working. The top three reasons for not using PPE were: the perception that PPE did not provide adequate protection (40.3%), discomfort or interference with work caused by PPE (29.9%), and lack of knowledge about how to use PPE (20.9%). Almost a quarter of the participants believed their work negatively impacted their health (Table 1).
Participants’ Sociodemographic and Work-Related Characteristics
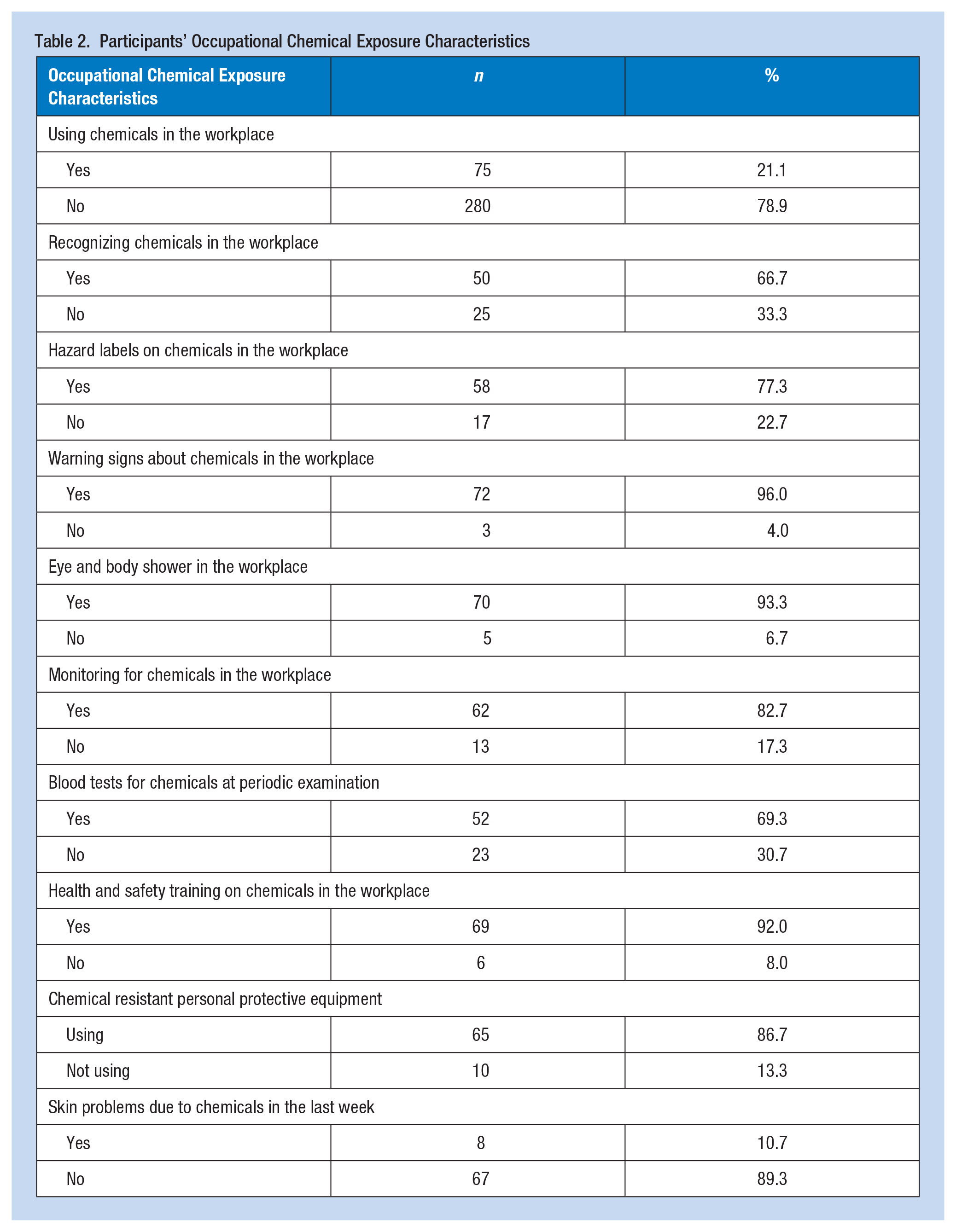
Chemical substances were used in the departments where 21.1% of the participants worked. Among the participants, 66.7% of those who used chemical substances could not identify the chemical used. Chemicals used by more than three-quarters of participants had labels with information about safety precautions. Ninety-six percent of participants had instructions and warning signs about chemicals in the work environment, while 93.3% reported the presence of emergency eye and body shower stations. According to the information obtained from occupational safety experts, measurements have been taken for 82.7% of workplace chemicals, and 92.0% received training on the health effects of chemical substances, safety precautions to be followed, the use of personal protective equipment, and what to do after exposure. According to the health records, 69.3% of the participants had blood tests for chemicals in periodic health examinations. Of the participants, 86.7% used personal protective equipment such as gloves, clothes, shoes, and goggles while working. One-tenth of the participants had complaints such as itching, redness, dryness, scaling, staining, and blisters on the skin due to chemicals in the last week (Table 2).
Participants’ Occupational Chemical Exposure Characteristics
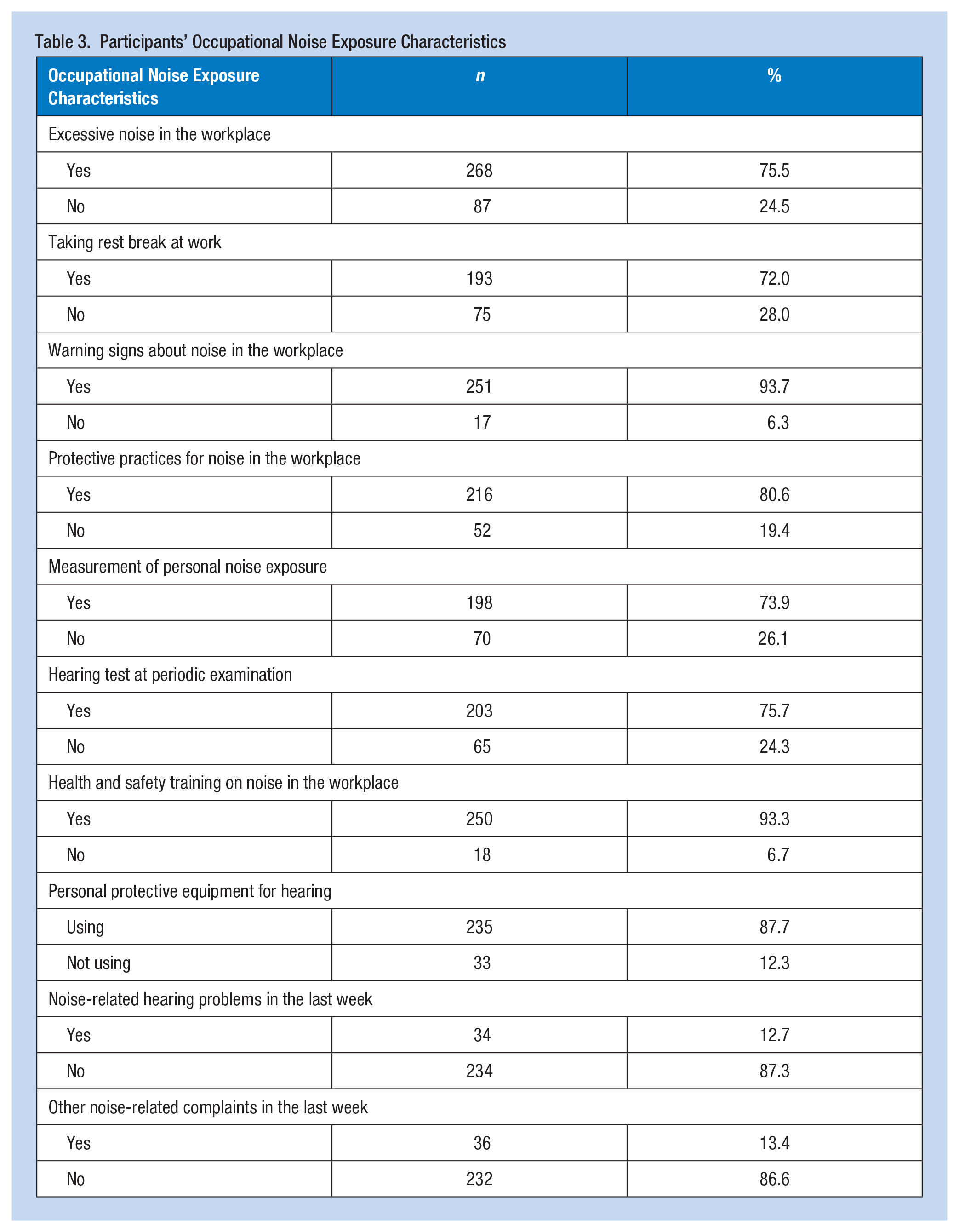
About three quarters of the participants (75.5%) stated that the working environment was noisy. More than a quarter of those exposed to noise reported that they were not given rest breaks away from noise during working hours. Four-fifths had protective practices for noise in the workplace, such as insulation, damping, screening, closure, and absorbent covers in the working environment. Approximately three-quarters of the participants had regular noise measurements of personal exposure and hearing tests during periodic health examinations. More than 90% have received training on the health effects of noise, precautions to be taken, and the correct use of personal protective equipment, including personal protective equipment for noise. However, 12.7% experienced temporary or permanent hearing loss and ringing or buzzing last week. One-seventh of the participants developed problems such as headaches, distraction, sleep disturbance, irritability, restlessness, and hypertension in the last week (Table 3).
Participants’ Occupational Noise Exposure Characteristics
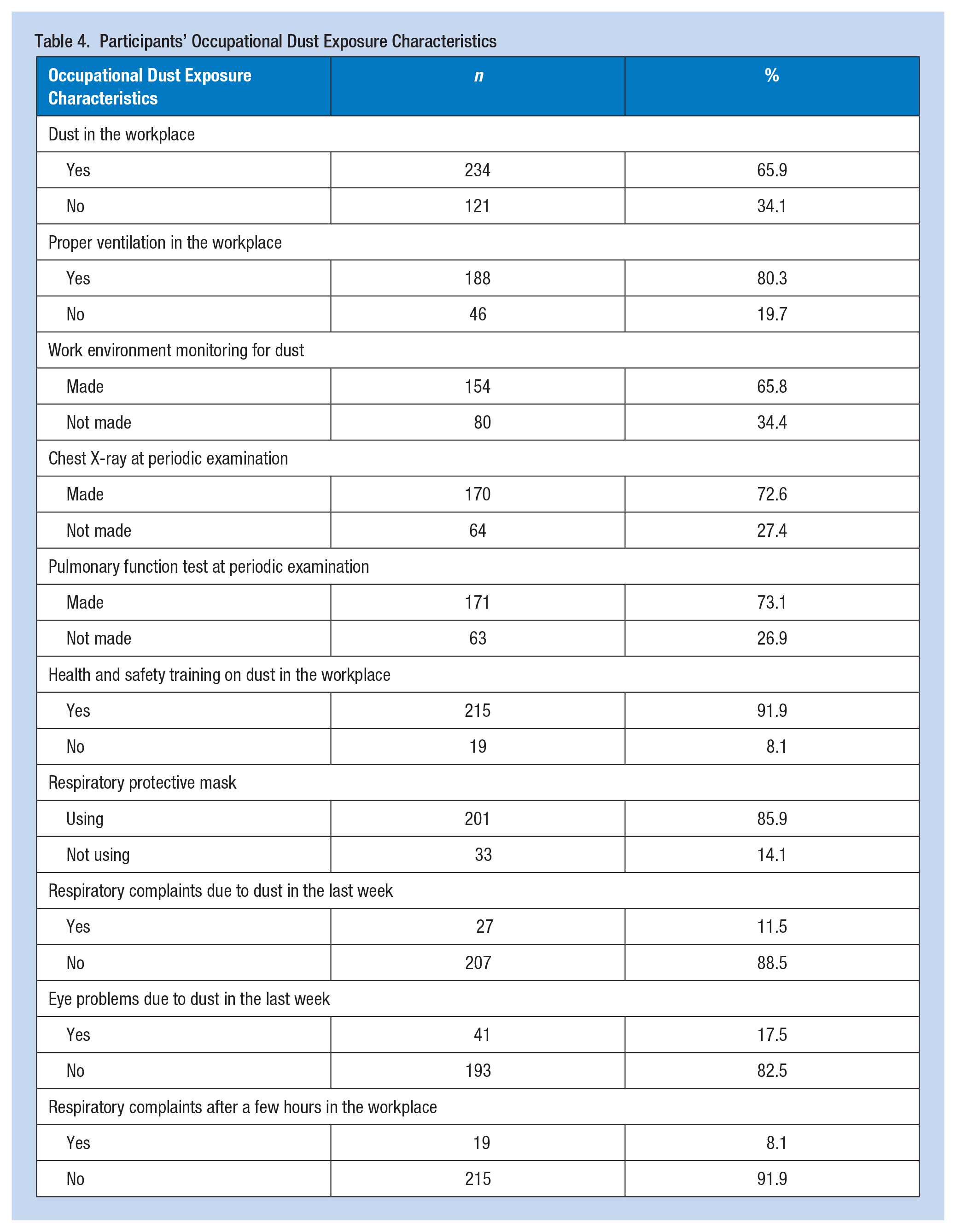
About two thirds of the participants (65.9%) stated that the working environment was dusty. Of those, 80.3% had proper ventilation in the working environment, 65.8% had regular respirable dust measurements in the working environment, 72.6% had chest X-rays, and 73.1% had pulmonary function tests during periodic health examinations. Most participants (91.9%) received training on the health effects of dust, protective measures, and the use of appropriate masks, and 85.9% used respiratory protective masks at work. Of the participants, 11.5% reported that they experienced coughing, shortness of breath, burning, and tightness in the chest within the last week, and 17.5% reported that they experienced redness, itching, and watery eyes. Participants (8.1%) also reported respiratory complaints after a few hours in the workplace, initially starting work at the respective facility (Table 4).
Participants’ Occupational Dust Exposure Characteristics
While 90.8% of those who use chemical-resistant personal protective equipment have received occupational health and safety training, 50% of those who do not have received occupational health and safety training. Among respondents, 90.6% of those who used personal protective equipment for hearing had received occupational health and safety training in the last year, compared to only 72.7% of those who did not use such equipment. Among participants using a respiratory protective mask, 92.0% received occupational health and safety training in the last year, while only 63.6% of those not using the mask had received the training. Significant differences were found, indicating that those who received occupational health and safety training in the last year were likelier to use PPE (p < .05; Table 5).
Participants’ Personal Protective Equipment Use by Occupational Health and Safety Training Status
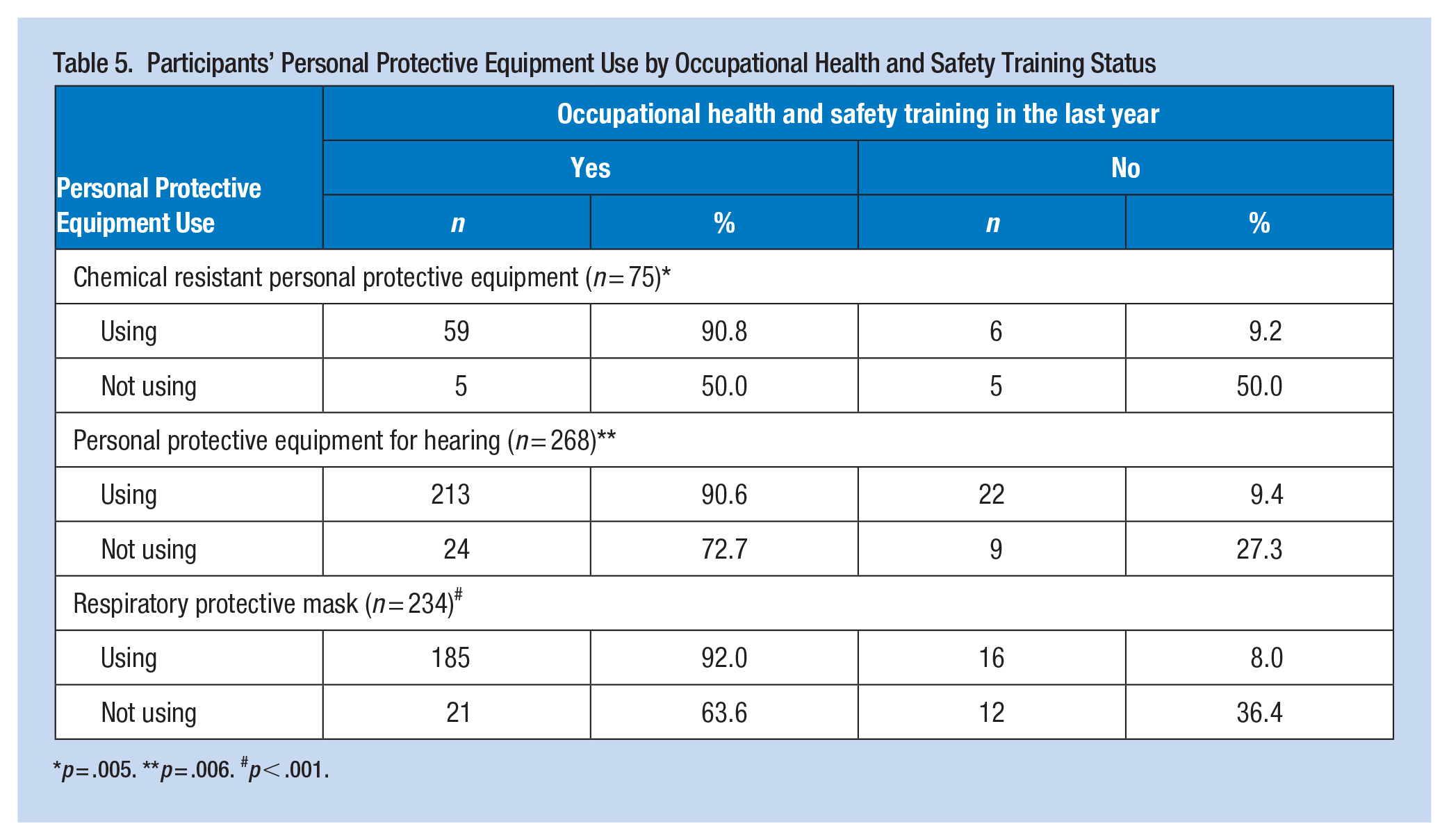
p = .005. **p = .006. #p < .001.
Discussion
In this study, the smoking prevalence was higher than that observed in similar studies and the general population. Specifically, 40% of participants were smokers, which is notably higher than the national average of 28% for Türkiye, where 41% of men, 15% of women, and 28% of the overall population use tobacco daily (The Ministry of Health General Directorate of Health Information Systems, 2023). Comparable studies, such as one conducted in a textile factory in Ethiopia, reported a lower smoking rate of 14%, likely due to the different demographic and socio-economic context (Tadesse et al., 2016). In Iran, a study of textile workers with a predominantly male workforce found a smoking rate of 24% (Jahanbani, 2003), while a similar study in Türkiye reported one-fourth of participants as smokers (Acar et al., 2021). The higher smoking prevalence in our study could be attributed to specific social, cultural, and economic factors that influence smoking behaviors in this particular population. Future research should focus on understanding these local factors, as well as exploring the impact of gender distribution on smoking rates in different industrial settings.
In the study, nearly all participants had undergone a medical examination at recruitment; however, approximately one-fifth had not completed the required periodic medical exams. In Türkiye, pre-employment medical examinations are mandatory, but periodic exams, which are also required based on workplace hazard classifications, are sometimes overlooked due to gaps in the enforcement of regulations. This finding aligns with concerns about the inconsistent implementation of periodic health checks, which is a well-documented issue in occupational health. The results highlight the need for improved monitoring and enforcement of workplace health examination protocols.
In our study, 10.7% of workers exposed to chemicals reported experiencing chemical-related skin problems in the last week. This finding is lower than the 1-year prevalence of contact dermatitis among clothing manufacturing workers in China (29%; Chen et al., 2017), and the 69% prevalence of skin symptoms observed in Moroccan textile workers, particularly those with 8 or more hours of daily chemical exposure (Tounsadi et al., 2020). A Polish study found that 24% of textile workers reported work-related skin problems (Kurpiewska et al., 2011). In contrast, the 1-year prevalence of eczema in the general population of Europe is only 5.5% (Richard et al., 2022). Although the skin problems reported in this study were relatively low in frequency, they remain significantly higher compared to the general population. Differences in the prevalence of skin issues across studies may be attributed to variations in factors such as the type of chemicals used, work conditions, the duration of exposure, and personal protective equipment usage.
In this study, 75.5% of participants were exposed to noise, and 12.7% reported noise-related hearing problems. This is lower than the 85% prevalence of hearing loss found among weaving department workers in Nigeria (Osibogun et al., 2000). Similarly, a study on weaving industry workers in India found a high noise-induced hearing loss rate, with 36% of workers experiencing severe hearing loss (Kallur & Hasalkar, 2021). In Myanmar, two-thirds of textile workers were exposed to noise levels of 85 dB or higher, and 25% had hearing loss (Zaw et al., 2020). The differences in prevalence across these studies may reflect variations in national policies, organizational safety cultures, and the sociodemographic and occupational characteristics of workers.
In the study, 65.9% of participants reported exposure to dust, with 11.5% experiencing respiratory complaints and 16.5% reporting eye problems in the past week. These findings are consistent with studies in similar settings. For example, 47.8% of textile workers exposed to cotton dust had respiratory issues (Daba Wami et al., 2018), while 53.8% of textile workers in another study reported at least one respiratory complaint (Tefera Zele et al., 2020). A study on garment factory workers found 38.7% had asthenopic symptoms (Sharma et al., 2021), and in the informal sector, 48.3% of men and 58.9% of power loom workers reported respiratory and eye issues (Nag et al., 2016). In contrast, a small-scale weaving study found 18% of workers had coughs and 13% had eye problems (Tahir et al., 2012). While these studies highlight a similar pattern of dust-related health problems, differences in prevalence rates may be attributed to variations in study design, population characteristics, and environmental conditions.
In our study, the use of PPE was significantly higher among participants who had received occupational health and safety training in the last year. This finding is consistent with studies in other countries, such as Iran, where training was also linked to higher PPE use (Abdelhameed et al., 2012), and Uganda, where increased safety knowledge led to greater PPE utilization (Izudi et al., 2017). Similarly, a study in Ethiopia found a significant relationship between training and PPE use (Tadesse et al., 2016). In contrast, a study in Pakistan found that although 81% of workers had the right attitude, only 21% applied safety measures (Khoso & Nafees, 2015). A study in Türkiye also noted no significant differences in PPE usage based on training (Çetin & Beğik, 2021). These findings suggest that while occupational health and safety training generally improves PPE usage, the gap between knowledge and actual practice remains an issue. This highlights the need for more than just theoretical training; regular inspections and practical enforcement are essential to ensure that safety measures are effectively implemented.
In this study, 19.3% of employees reported not using PPE. The main reasons cited included inadequate protection, discomfort, interference with work, and lack of knowledge on proper use. These reasons are consistent with findings from several studies conducted in Ethiopia, where common barriers to PPE use were lack of knowledge, discomfort, difficulty accessing equipment, and concerns about its effectiveness (Baye et al., 2022; Debela et al., 2023; Zegeorgous et al., 2020). Similarly, in Pakistan, PPE use was hindered by discomfort and limited access (Hussain et al., 2019). While there are some contextual differences across countries, the reasons for not using PPE appear to be consistent. These findings suggest that occupational health and safety policies, along with their implementation, play a crucial role in shaping employees’ behaviors and workplace safety culture.
Limitations
This study has some limitations that should be considered when interpreting the findings. The research was conducted in two weaving factories, which may limit the generalizability of the results. Any measurements were not made and reliance on self-reported data for variables such as PPE use and health complaints could have introduced recall or reporting bias, even though health records and observations were used to enhance data accuracy. The study did not delve deeply into psychological or ergonomic factors. Future studies should adopt a comprehensive approach to address these dimensions and provide a fuller understanding of workplace risks and health outcomes.
Implications for Occupational Health Nursing Practice
This study highlights critical occupational hazards faced by weaving workers, including exposure to chemicals, noise, and dust, and the challenges associated with low PPE usage. Exposure to these environmental factors is linked to respiratory issues, hearing loss, and other chronic health conditions, underscoring the need for comprehensive risk management strategies. The findings suggest that occupational health nurses can play a pivotal role in addressing these issues by implementing targeted interventions that focus on education, accessibility, and behavioral change. Regular occupational health and safety training sessions should emphasize the proper use and maintenance of PPE and address common barriers such as discomfort or perceived inefficacy. Nurses should advocate for workplace policies that prioritize health surveillance, including periodic medical examinations, hearing tests, and pulmonary function tests, to detect early signs of occupational diseases. Nurses can contribute to smoking cessation programs tailored to the high prevalence of smoking among workers, which could include counseling, support groups, and workplace incentives to quit smoking. These programs, combined with efforts to foster a culture of safety and well-being, can significantly reduce health risks and improve workers’ overall quality of life. By integrating these strategies, occupational health nurses can lead efforts to enhance workplace safety and prevent chronic health conditions in the textile industry.
Applying Research to Occupational Health Practice
Weaving workers face compounded risks due to the combined impact of occupational exposures and the high prevalence of smoking. Occupational health professionals can address these challenges through holistic interventions. Smoking cessation programs tailored to workers’ needs—including counseling, peer support groups, and workplace incentives—can reduce health risks and enhance overall well-being. By fostering collaboration between employers and employees, occupational health practices can lead to policies prioritizing health monitoring and risk reduction. These efforts can enhance workplace safety, reduce chronic health conditions, and contribute to a healthier and more productive workforce in the textile industry.
Footnotes
Acknowledgements
We acknowledge Dr. Sezai Çubuk for their contributions during the data collection phase.
Data Availability
Data and materials can be provided as needed.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from Gazi University Ethics Committee on July 10, 2023 (2023-837).
