Abstract
Background
Workplace violence (WPV) and its health consequences should continue to be investigated to foster a healthy and safe working environment, which may reduce nurse staff turnover and improve nurse staff shortages. This study aimed to address the gap in understanding WPV in non-western nurses by examining the relationship between psychological WPV experience, psychological well-being, subjective job stress, and presenteeism among South Korean nurses.
Methods
This cross-sectional study used data from the fifth Korean Working Conditions Survey (KWCS), and 477 nurses were analyzed. For the analysis, selected variables were extracted from the KWCS through a review of the existing literature. In the analysis, we included psychological WPV experiences, such as verbal abuse, unwanted sexual attention, threats, and/or humiliating behaviors over the past 1 month. We measured health outcomes including nurses’ psychological well-being, subjective job stress, and presenteeism.
Findings
Psychological WPV within the previous month was experienced by 11.1% of the participants. Experience with verbal abuse, threats, or humiliating behaviors was associated with more job stress, higher presenteeism, and poor psychological well-being.
Conclusion/Application to Practice
Study findings suggest that a comprehensive WPV prevention program accompanied by interventions aiming to reduce job stress and improve the well-being of nurses should be actively implemented. To prevent psychological WPV and improve the health of nurses, evidence-based efforts, such as establishment of WPV prevention procedures and education/training of workers at the national, organizational, and individual levels are needed.
Background
Workplace violence (WPV) against nurses is a widespread problem in both developing and developed countries. Most studies on WPV and its health consequences have been conducted in Western nations (Cheung & Yip, 2017). Currently, the health-related impact of WPV on nurses in non-Western countries remains insufficiently studied. Compared with nurses in other Asian countries, hospital nurses in South Korea generally care for a higher number of patients due to nursing staff shortages (Lee, 2019). In addition, it is hypothesized that the task-oriented Korean culture, which values organizational goals and productivity, and the hierarchical organizational culture in nursing may contribute to the high WPV against nurses (Kim & Oh, 2016). Indeed, high levels of WPV among nurses have been extensively reported (Chang & Cho, 2016; Chang et al., 2019; Choi and Lee, 2017; Park et al., 2015). However, the impacts of WPV on health are not sufficiently known.
WPV in health care settings may cause serious consequences for nurses, such as anxiety (Cheung & Yip, 2017), poor sleep quality (Sun et al., 2017), psychological stress (Cheung & Yip, 2017; Itzhaki et al., 2018; Sun et al., 2017), poor self-reported health status (Sun et al., 2017), burnout, low job satisfaction, high intention to leave (Chang & Cho, 2016), high absenteeism (Hogh et al., 2016), and other dimensions of physical and mental health (Cheung & Yip, 2017; Kahsay et al., 2020). WPV may also have a negative effect on quality of health care and patient safety (Al Omar et al., 2019).
Previous WPV studies involving South Korean nurses only focused on WPV and job performance in terms of nurses’ intentions to leave or levels of commitment to the workplace (Chang & Cho, 2016; Choi & Lee, 2017). Therefore, the present study focused on the dimensions of individual health and job performance (e.g., presenteeism and job stress), which were not previously covered. Moreover, unlike physical violence, psychological violence goes unnoticed, because its impacts are hardly visible (Park et al., 2015). Psychological violence refers to the intentional use of power, including threats of physical harm, against another person or group (e.g., sexual harassment, threats, bullying, and verbal abuse) (Xing et al., 2016). Accordingly, the present study aimed to examine whether exposure to psychological WPV is related to psychological well-being, subjective job stress and presenteeism among South Korean nurses.
Method
This cross-sectional study was a secondary analysis of the fifth Korean Working Conditions Survey (KWCS) conducted by the South Korean Occupational Safety and Health Research Institute (OSHRI) in 2017. Modeled on the European Working Conditions Survey, the KWCS has provided information on the overall working environment and workers’ exposure to risk factors across the country since 2006. The KWCS questionnaire has been shown to be highly valid and reliable (Kim et al., 2013).
The fifth KWCS included a representative sample of workers aged ≥ 15 years who were paid for more than 1 hour a week before the study interview (OSHRI, 2017). The survey enrolled 50,205 participants, who then underwent interviews which were conducted in their homes using tablet computers. The electronic questionnaire was developed using Blaise, which is a computer-assisted interviewing system developed by Statistics Netherlands (OSHRI, 2017). Respondents who indicated they were employed as nurses (n = 477) were selected for the present analysis.
Based on the existing literature, we ascertained nurses’ demographic and job characteristics that have been previously associated with WPV (Cheung & Yip, 2017; Ferri et al., 2016; Hogh et al., 2016; Jiao et al., 2015; Shafran-Tikva et al., 2017), such as sex (male/female), age category (<30 years, 30–39 years, 40–49 years, and ≥50 years), education level (<bachelor’s, bachelor’s, >master’s degree), work position (staff/head), shift work(yes/no), work experience, income level, and working hours were included in the analysis. In this study, net monthly income levels were classified into <2 million KRW (1,800 USD), <3 million KRW (2,700 USD), <4 million KRW (3,600 USD), and ≥4 million KRW (≥3,600 USD). Work experience was surveyed by the total number of months worked as a nurse, categorized as <5 years, 5–10 years, and ≥11 years. Working hours were measured as the total hours worked as a nurse over the past week. According to the Labor Standards Act, domestic statutory working hours are 40 hours per week, and if overtime is required, it cannot exceed 52 hours per week. Taking this regulation into account this, working hours are classified as follows: <40 hours, 40 hours, 41–52 hours, and ≥53 hours.
Psychological WPV experience was measured using the KWCS questions “Have you ever suffered verbal abuse, unwanted sexual attention, threats, or humiliating behaviors (Yes/No or refusal) from colleagues, managers, patients, or the families of patients during your work in the last month?” To minimize recall bias, the current study measured WPV within the past month.
Psychological well-being was measured using the five-item World Health Organization (WHO-5) Well-being Index (ver. 1998), which is a generic global scale that measures subjective well-being within the past 2 weeks from the time of their responses. The index consists of five items on a 5-point Likert-type scale, with total scores ranging between 0–25. A total score below 13 indicates poor psychological well-being (World Health Organization Collaborating Centres for Mental Health, 1998).
Subjective job stress was measured using the 5-point single-item measure (1 = never, 2 = rarely, 3 = sometimes, 4 = most of the time, 5 = always). In line with previous research (Eurofound, 2012), participants who experienced stress at work “most of the time” or “always” were classified as the stress group. This single-item measure of job stress is relatively valid, as reported by Houdmont et al. (2019).
Presenteeism, which is defined as the problem of employees attending work despite having health problems, is one cause of productivity loss (Lohaus & Habermann, 2019). We assessed presenteeism by using the question “Over the past 12 months, have you worked when you were sick?” Participants who answered “yes” were classified as suffering from presenteeism. Using a single question to measure presenteeism demonstrates high test–retest reliability, as proven by European studies (Demerouti et al., 2009; Lohaus & Habermann, 2019).
This study involved a secondary analysis of existing data and was exempted from research ethics review by the Institutional Review Board of the University of Ulsan.
Data Analysis
Descriptive statistics were employed for purposes of describing the study sample’s demographic and occupational characteristics. The prevalence of psychological WPV and various health outcomes (psychological well-being, subjective job stress, and presenteeism) was calculated using descriptive statistics and differences compared by chi-square tests where sample sizes permitted. Associations between psychological WPV and health outcomes was evaluated by multiple logistic regression analysis in which adjusted odds ratio (AOR) and 95% confidence intervals (CIs) were calculated, adjusting for confounding variables. Considering that male, inexperienced, graduate-level, and rotating shift nurses are more likely to report WPV (Cheung & Yip, 2017; Jiao et al., 2015; Shafran-Tikva et al., 2017), we included sex, age, education level, position, work experience, income level, shift work, and working hours as co-variates.
Results
Table 1 summarizes the demographic, job, and health characteristics of the participants. Most were female (98.3%), and 41.5% were in their 30s. More than half (58.3%) had a bachelor’s degree, and almost all were staff nurses (99.8%). Approximately 47% of the participants had less than 5 years of work experience, and 52.3% reported monthly income amounts of more than 2 million Korean Won (KRW) and less than 3 million KRW (≤1,800 and <2,700 USD, respectively). Nearly 65% of the nurses worked by shift, and 51.2% worked 40 hours a week. Poor psychological well-being, job stress, and presenteeism were experienced by 25.6%, 40.7%, and 20.8% of the participants, respectively.
Demographic, Job, and Health Characteristics of a Sample of Korean Nurses From the Korean Working Conditions Survey (n = 477)
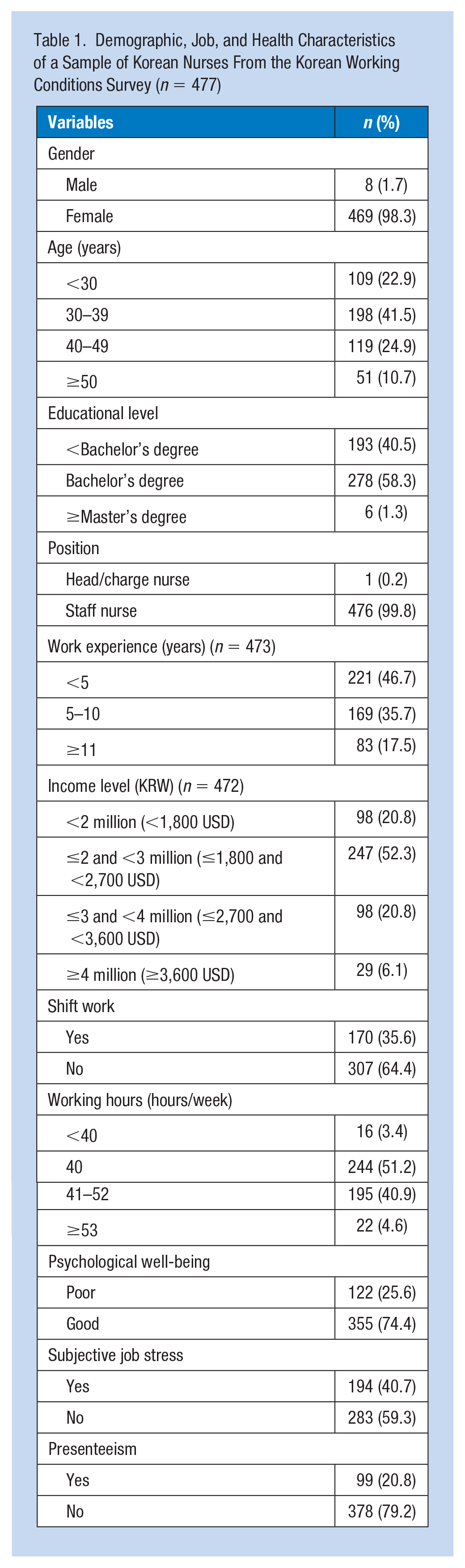
Table 2 presents participants’ psychological WPV prevalence. Overall, 11.1% reported having experienced at least one type of psychological WPV within the previous month. Furthermore, 8.0% of nurses reported having experienced verbal abuse, 1.7% suffered unwanted sexual attention, and 1.7% reported being threatened. In addition, nearly 6% reported having experienced humiliating behaviors.
Prevalence of Psychological Workplace Violence Among Nurses From the Korean Working Conditions Survey (n = 477)
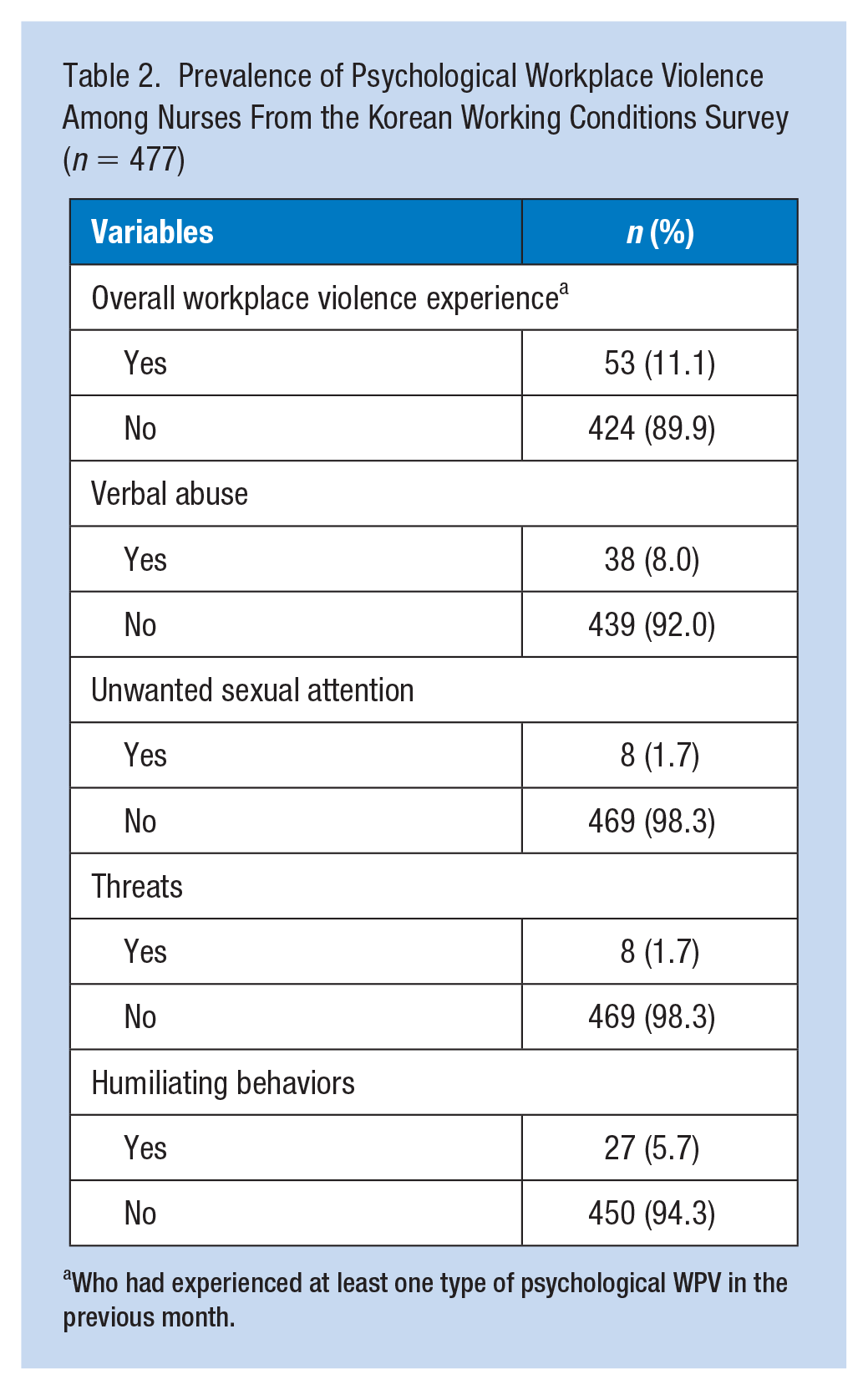
Who had experienced at least one type of psychological WPV in the previous month.
Table 3 shows the bivariate relationship of the health outcomes by participants’ psychological WPV experience. Participants with overall psychological WPV experience had significantly higher rates of poor psychological well-being than those without (p < .001). In particular, psychological well-being was poorer in nurses with verbal abuse experience than in nurses without (p < .001). Nurses with overall psychological WPV experience reported significantly higher rates of job stress than those without (p < .05). Presenteeism was more frequent in nurses with overall psychological WPV experience than in nurses without such experience (p < .001). In particular, nurses who had experienced verbal abuse (p < .001), and humiliating behaviors (p < .001) showed higher rates of presenteeism than those who had not experienced these aspects of WPV.
Bivariate and Multivariate Associations Between Psychological Workplace Violence by Psychological Well-Being, Subjective Job Stress, and Presenteeism Among Nurses From Korean Working Condition Surveys (n = 477)
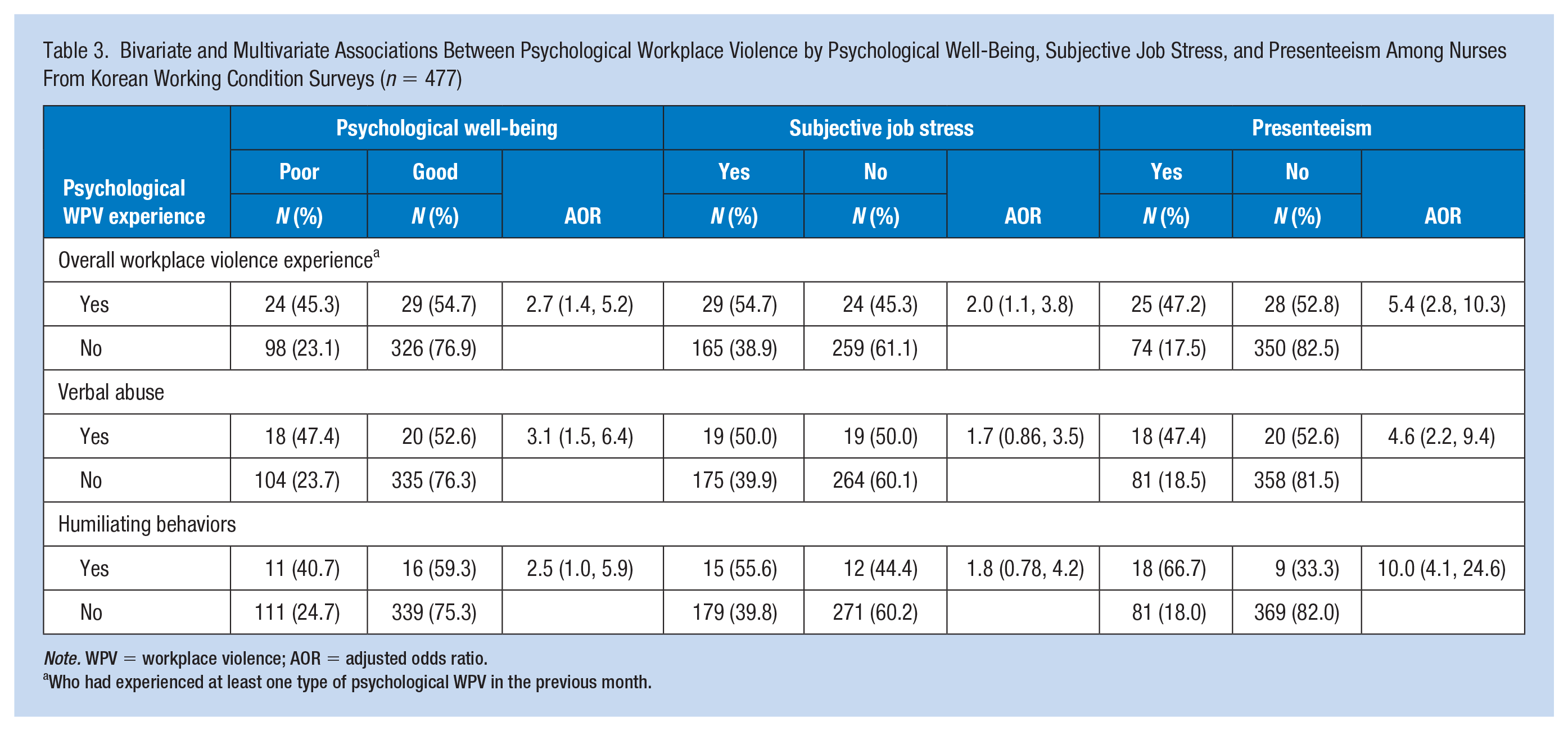
Note. WPV = workplace violence; AOR = adjusted odds ratio.
Who had experienced at least one type of psychological WPV in the previous month.
For the multivariate analyses, we found that nurses with overall psychological WPV experience (AOR = 2.7, 95% CI = [1.4, 5.2]) were more likely to have poor psychological well-being than those without. Experiencing verbal abuse was associated with a three-fold increase in the odds of poor psychological well-being (AOR = 3.1, 95% CI = [1.5, 6.4]). Nurses who had experienced humiliating behaviors were 2.47 times more likely to report poor psychological well-being than those who had not (AOR = 2.5, 95% CI = [1.0, 5.9]). Nurses who had experienced overall psychological WPV were two-times more likely to have job stress than those who had not (AOR = 2.0, 95% CI = [1.1, 3.8]). In addition, we found that the experience of overall psychological WPV (AOR = 5.4, 95% CI = [2.8, 10.3]) was a significant predictor of presenteeism, including experience with verbal abuse (AOR = 4.6, 95% CI = [2.2, 9.4]).and humiliating behaviors (AOR: 10.0, 95% CI = [4.1, 24.6]) which were significantly associated with presenteeism.
Discussion
This study evaluated psychological WPV “within the past month” from the time of collecting participant responses to minimize recall bias. The overall prevalence estimate for psychological WPV was 11%, which is far lower than that of other studies. Previous studies that surveyed nurses’ WPV during the previous 12 months reported the prevalence of WPV from 71.0% to 95.5% (Chang & Cho, 2016; Chang et al., 2019; Choi & Lee, 2017; Park et al., 2015).
Consistent with previous studies, our study revealed that verbal abuse is the most common form of WPV (Chang & Cho, 2016; Cheung et al., 2017; Cheung & Yip, 2017; Choi & Lee, 2017; Ferri et al., 2016; Park et al., 2015; Shafran-Tikva et al., 2017). Our analysis however, did not examine the relationship of the perpetrator of the violence to the nurses. It has been theorized that verbal abuse against nurses may be mainly caused by power differentials or unequal physician–nurse relationships and nursing staff shortages (Brewer et al., 2013; Sofield & Salmond, 2003). In South Korea, nurses, which are predominantly female are considered supplemental to physicians rather than as partners in patient care (Yi, 2018). The relatively low social status of nurses may be one of the causes of increase in the risk of verbal abuse against nurses (Shafran-Tikva et al., 2017).
This study suggests that experience with verbal abuse and humiliating behaviors is associated with more job stress, higher presenteeism, and poor psychological well-being. These findings agree with those of previous studies that showed an increased level of stress in people who experienced verbal violence and bullying (Einarsen & Nielsen, 2015; Itzhaki et al., 2018). Exposure to WPV makes one feel unsafe, which not only impacts job stress but also potentially induces poor psychological well-being (Einarsen & Nielsen, 2015; Neto et al., 2017). According to Choi et al. (2018) presenteeism is highly probable among workers who have experienced adverse social behaviors (e.g., sexual harassment and harassment). In addition, frequent exposure to workplace bullying is associated with 8 days or more of presenteeism (Conway et al., 2016).
This study has several limitations. First, based on the cross-sectional survey design, the KWCS investigates experiences with psychological WPV during the previous month, psychological well-being over the past 2 weeks, and presenteeism over the past 12 months from the time of participant responses. Considering the cross-sectional survey and various time frames, we could not confirm whether the health outcomes in all participants were preceded by psychological WPV. Second, the small sample size makes it difficult to generalize the results of this study. Third, considering the low number of cases for some variables herein, CIs were wide. In other words, the effect estimation was less accurate. Nevertheless, the results of goodness-of-fit tests for our prediction model showed no indication that the effects were caused by chance. Fourth, experience with WPV or negative health outcomes might be underestimated, given that nurses experiencing WPV or negative health outcomes may not have wanted to relive their experiences by reporting them (Kowalenko et al., 2013). Finally, given the use of a secondary dataset, other potential variables influencing the effects of psychological WPV (i.e., fear, confidence, or ward type) (Ferri et al., 2016; Hanson et al., 2015) could not be considered in this analysis.
Despite these limitations, this study improves our understanding of the relationship between psychological WPV and health consequences in non-Western nurses, whose working conditions and social status are very different. Our findings can provide insight into national health care quality and safety policy as well as provide guidance for employers and managers of nurses. WPV prevention programs should be accompanied by interventions focusing on reducing job stress and improving the well-being of nurses.
As our results show, psychological WPV has negative effects on nurses’ health. The poor health status of nurses may reduce patient care quality and may lead to a higher turnover of nurses (Tourangeau et al., 2017). Therefore, preventing psychological WPV and improving the health of nurses are critical issues of the nation and health care institutions but may depend on efforts at the national, organizational, and individual levels. In 2018, the Korean government enacted regulations to prevent WPV for interpersonal service workers. For these regulations to be more effective employers must foster a culture of respect in health care settings and develop a comprehensive WPV prevention program that includes interventions that aim to reduce job stress and improve the well-being of nurses.
Applying Research to Occupational Health Practice
Experience with psychological workplace violence (WPV) was associated with more job stress, higher presenteeism, and poor psychological well-being. This study provides evidence for Occupational Health Providers (OHPs) of the possible health deterioration of nurses with WPV experience, and OHPs should, thereby, link occupational health services, such as psychological counseling and treatment, rest, and leave for these nurses. Furthermore, in October 2018, employers’ obligations to prevent WPV were newly established in the South Korea Occupational Safety and Health Act. OHPs provide expertise to ensure that employers to fulfill their legal obligations. They can collaborate with management and human resources to develop evidence-based programs aimed at fostering a respectful workplace culture. A comprehensive WPV prevention program should accompany interventions that aim to reduce job stress and improve the nurses’ well-being.
Footnotes
Acknowledgements
The authors thank the Occupational Safety and Health Research Institute (OSHRI) Statistics Team for providing raw data from the Korean Working Conditions Survey (KWCS). The content of this paper is solely the responsibility of the authors and does not represent any official views of OSHRI.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the 2020 Research Fund from the University of Ulsan in South Korea.
Author Biographies
Jinhwa Lee is assistant professor of nursing at the University of Ulsan and a member of the editorial board of the Korean Journal of Occupational Health. She has researched workers’ health outcomes as well as workplace health promotion and prevention.
Bokim Lee is professor of nursing at the University of Ulsan and a vice-president of the Korean Association of Occupational Health Nurses (KAOHN). Her research focuses on workplace environment and workers’ health outcomes, as well as workplace participatory interventions to improve workers’ health.
