Abstract
Needlestick and sharps injuries (NSIs) are a major cause of occupational injuries for health care workers worldwide. In this study, the authors report the prevalence of and risk factors for NSIs among Chinese nursing students. A cross-sectional survey was distributed to 442 nursing students; 393 completed questionnaires were submitted. A total of 237 (60.3%) nursing students reported NSIs, which were more commonly reported by female students, younger students, students who worked frequent night shifts, students without safety training, and students who did not use personal protective equipment. Among those injured, 59.9% were injured by syringe needles, 21.9% by glass items, and 3.4% by scissors. Of those needles and sharps causing injuries, 36.3% of devices had been used on patients, 41% were unused, and 22.7% were unknown. Opening ampoules or vials was the most common injury agent. A total of 86.9% of NSIs were not reported to hospital infection control. Nursing students are at high risk of NSIs in China. Occupational safety training should be developed and implemented to prevent NSIs among this vulnerable population.
Needlestick and sharps injuries (NSIs) are a potential source of serious occupational injuries to health care workers, including nursing students (Cheung, Ching, Chang, & Ho, 2012; Pruss-Ustun, Rapiti, & Hutin, 2003; Yao et al., 2013). The World Health Organization (WHO) reported an annual rate of four NSI injuries per health care worker in Africa, the western Mediterranean, and Asia (Mantel, 2002). In addition, 600,000 to 800,000 NSIs occur annually among health care workers in the United States and about half to two thirds of these NSIs were unreported to infection control personnel (Makary et al., 2007). Due to limited clinical experience and insufficient attention to personal safety, nursing students are particularly susceptible to occupational NSIs (Cheung et al., 2012).
More than 20 blood- or body-fluid–borne pathogens can be transmitted to health care workers by occupational exposure to NSIs. Among these blood- or body-fluid–borne pathogens, hepatitis B virus (HBV), hepatitis C virus (HCV), and human immunodeficiency virus (HIV) are the most commonly transmitted during health care workers’ contact with patients (Cheung, Ho, Ching, & Chang, 2010). Health care workers, including nursing students, are at high risk of acquiring blood- or body-fluid–borne infections because of frequent injections and suturing (Cheung et al., 2012; Pruss-Ustun et al., 2003; Yao et al., 2013). Hazards related to NSIs are further compounded because the prevalence of HBV, HCV, and HIV among hospitalized patients is many times higher than in the general population (Wicker et al., 2008). The risk of infection due to occupational exposure ranges from as high as 40% for HBV and 3% to 10% for HCV, to as low as 0.2% to 0.5% for HIV (Cheng, Su, Yen, & Huang, 2012). Nursing students’ occupational exposures to blood- or body-fluid–borne pathogens cannot be ignored because nursing students rank third, after registered nurses and medical staff, for risk of sustaining NSIs (Cheung et al., 2010).
Nursing is a practice profession, so nursing education includes both classroom and clinical education (Cheung et al., 2012). To apply knowledge to practice, students are required to perform various types of skills and procedures involving sharps and subcutaneous, intramuscular, and intravenous needles. However, nursing students have limited clinical experience and lack skill in handling needles and sharps safely. Results of previous studies have shown that prevalence of NSIs among nursing students vary by country. Prevalence rates of 9.4%, 13.9%, 49%, and between 26.05% and 32% were found in the United States, Australia, Turkey, and China, respectively (Hambridge, 2011; Smith & Leggat, 2005; Talas, 2009; Yao et al., 2010; Wang, Fennie, He, Burgess, & Williams, 2003).
China has one of the highest rates of endemic HBV infection in the world, with an estimated 93 million hepatitis B surface antigen (HBsAg) carriers nationwide (Zhang, Zhong, & Guo, 2013). Moreover, the prevalence of HCV and HIV is rising in China (Phipps et al., 2002). However, no regulations govern the use of safety needles and devices in China; thus, safety needles and devices are less commonly used in China compared with other countries due to the high cost of these devices (Zhang, Gu, Cui, Stallones, & Xiang, 2015). Results of previous studies in China showed that nursing students are at high risk of NSIs (Wang et al., 2003; Yao et al., 2010). Therefore, exposure to blood- or body-fluid pathogens is likely to be a serious occupational hazard for Chinese nursing students. Despite this, little data have been published about patterns of and risk factors for NSIs among Chinese nursing students. The aim of the present study was to estimate the prevalence and characteristics of NSIs, and identify risk factors for these injuries among nursing students in China.
Method
This cross-sectional study included senior nursing students from three universities in Nanjing, the capital city of Jiangsu Province, China. Based on an estimated 20% NSI prevalence among Chinese nursing students, a total of 384 participants were needed to achieve a study power of 0.80 and an alpha of .05. The total number of senior nursing students in the selected universities was 615. Anticipating a 15% nonresponse rate, a goal of 442 nursing students was set for the sample. The Institutional Review Board of Southeast University School of Public Health approved the study protocol. Informed consent was secured from participants when data were collected.
Instrument
Based on the literature review and a special focus group discussion with nurses and nursing students, the research team at the Southeast University Injury Prevention Research Institute developed a questionnaire to gather information about NSIs among nursing students. The questionnaire included five sections (i.e., sociodemographic data, classroom and job training about personal protective equipment [PPE] to reduce NSIs, common treatment procedures/sharps handling during past year, details of any NSIs during past year, and reasons for reporting or not reporting NSIs over past year) with a total of 24 items. The survey questionnaire was pilot tested with 10 nursing students in the study area during May 2015; the students were interviewed and provided feedback about the questionnaire, which resulted in minor changes to the questionnaire.
Data Collection
Survey data were collected in June 2015. A list of all potential participants and their departments were provided by the nursing departments of the three selected universities. Participants were approached by the researchers and provided with a copy of the questionnaire. Questionnaires were collected several hours after distribution. Data collection was completed in 1 week. No personal identifiers (e.g., name, phone number, or home address) were collected to protect the privacy of the participants and confidentiality of the data.
Data Analysis
Data were entered into EpiData 3.0 and analyzed using SAS 9.1. First, chi-square analyses assessed the association between NSIs and selected demographic characteristics. Second, to control for confounding among selected variables, multivariate logistic regression analyses were conducted to identify those statistically significant independent variables, which increased the risk of NSIs in the year prior to the survey. Third, the proportion of patients with blood- or body-fluid–soiled items was calculated in “used” items involved in causative devices and causative events of NSIs. Finally, the researchers described NSI reporting to the infection control department of each hospital and reasons nursing students did not report NSIs.
Results
Of the 442 nursing students who received the questionnaire, 393 completed the questionnaire, yielding an overall response rate of 88.9%. The 49 nursing students who did not respond were either absent from the university when the survey was distributed or did not complete the questionnaire. Most of the participants were female (81.9%) and above 20 years of age (67.9%).
The prevalence of NSIs by selected demographic characteristics is presented in Table 1. A total of 237 cases of NSIs (60.3%) were reported. The prevalence of NSIs was significantly higher in females than in males (69.3% vs. 19.7%,p < .001). Needlestick and sharps injuries disproportionately affected younger students, with more than 80% of injuries among those students 20 years and younger (p < .001).
Comparison of Needlestick and Sharps Injuries by Selected Demographics
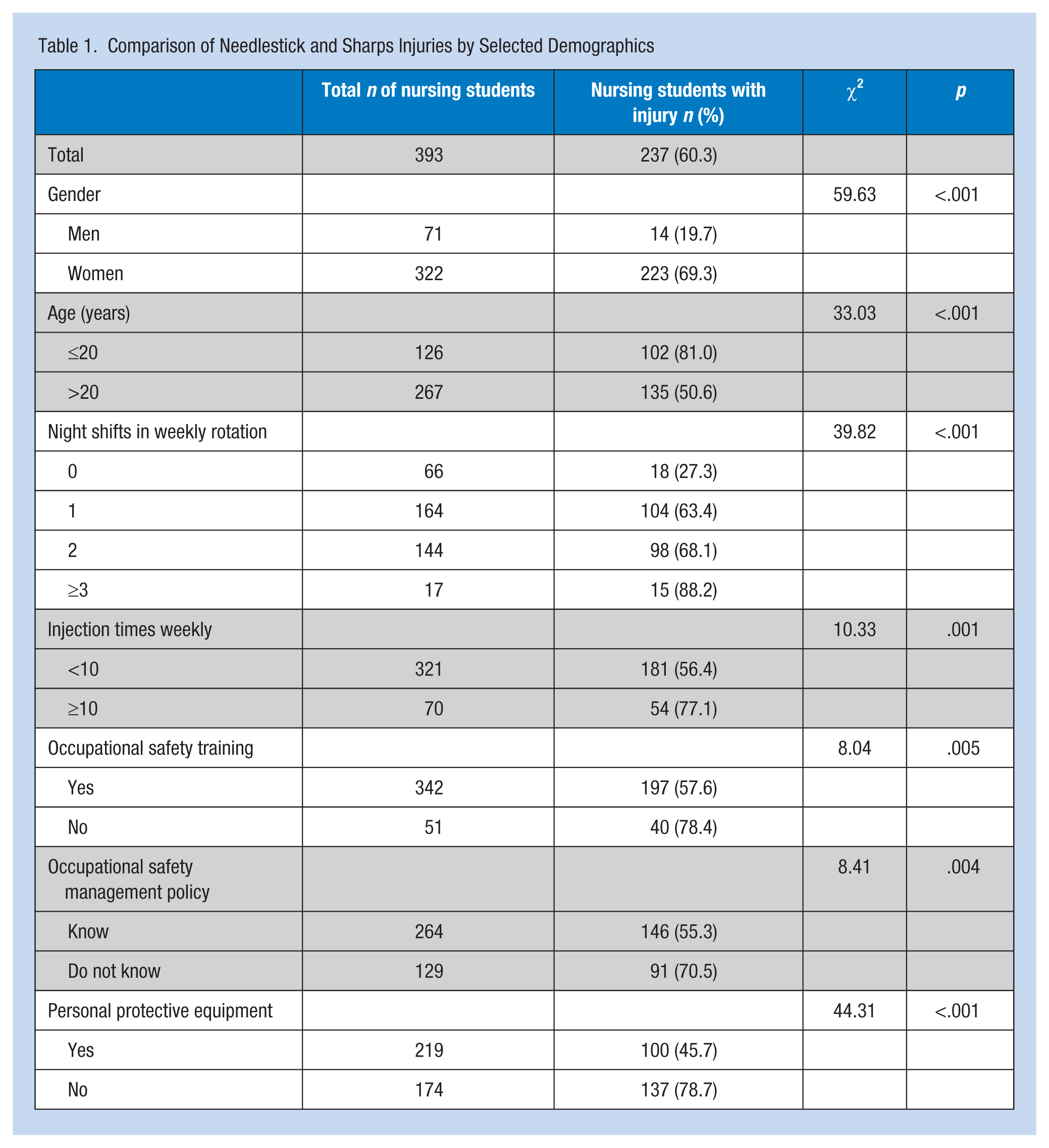
The highest prevalence rates of NSIs among nursing students were found among those who worked night shifts three or more times per week (88.2%), who provided 10 or more injections each week (77.1%), who did not have safety training (78.4%), who were unaware of needlestick and sharps safety policies (70.5%), and who did not wear PPE when exposed to needles and sharps (78.7%).
Table 2 presents multivariate logistic regression models. Results suggested that NSIs were significantly more likely to occur among nursing students with the following characteristics: gender (women vs. men, odds ratio [OR] = 3.99, 95% CI = [1.95, 8.14]), age (≤20 years vs. >20 years, OR = 2.02, 95% CI = [1.12, 3.65]), frequent night shifts in weekly rotation (three times or more vs. 0-1 times, OR = 5.90, 95% CI = [1.10, 31.75]), lack of occupational safety training (no vs. yes, OR = 3.21, 95% CI = [1.44, 7.17]), and lack of PPE use (no vs. yes, OR = 2.20, 95% CI = [1.25, 3.87]).
Logistic Regression Models of Needlestick and Sharps Injuries
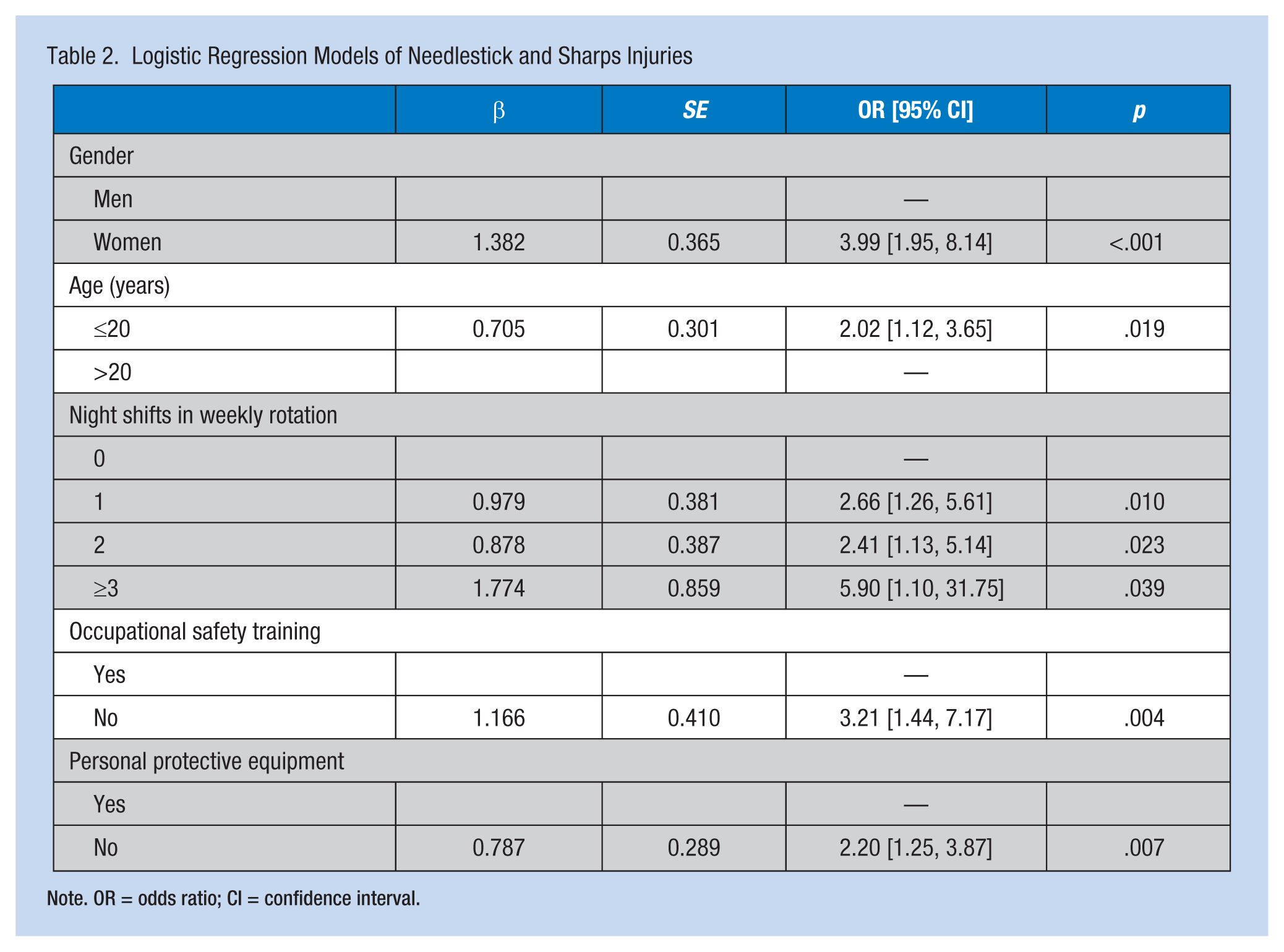
Note. OR = odds ratio; CI = confidence interval.
Devices causing injuries and usage status related to the occurrence of NSIs are presented in Table 3. Syringes (i.e., intramuscular, hypodermic, intracutaneous, and intravenous needles) accounted for the highest proportion of all NSIs (59.9%), followed by glass items (21.9%), and scissors (3.4%). Injuries caused by special puncture needles, probes, and suture needles were rare (1.3% for each). A total of 36.3% of devices were contaminated by patient blood or body fluids; 41% had not been previously used on any patients and occurred during drug preparation. In 22.7% of the NSIs, specific patient contact history was not known.
Causative Devices for Needlestick and Sharps Injuries (n = 237)
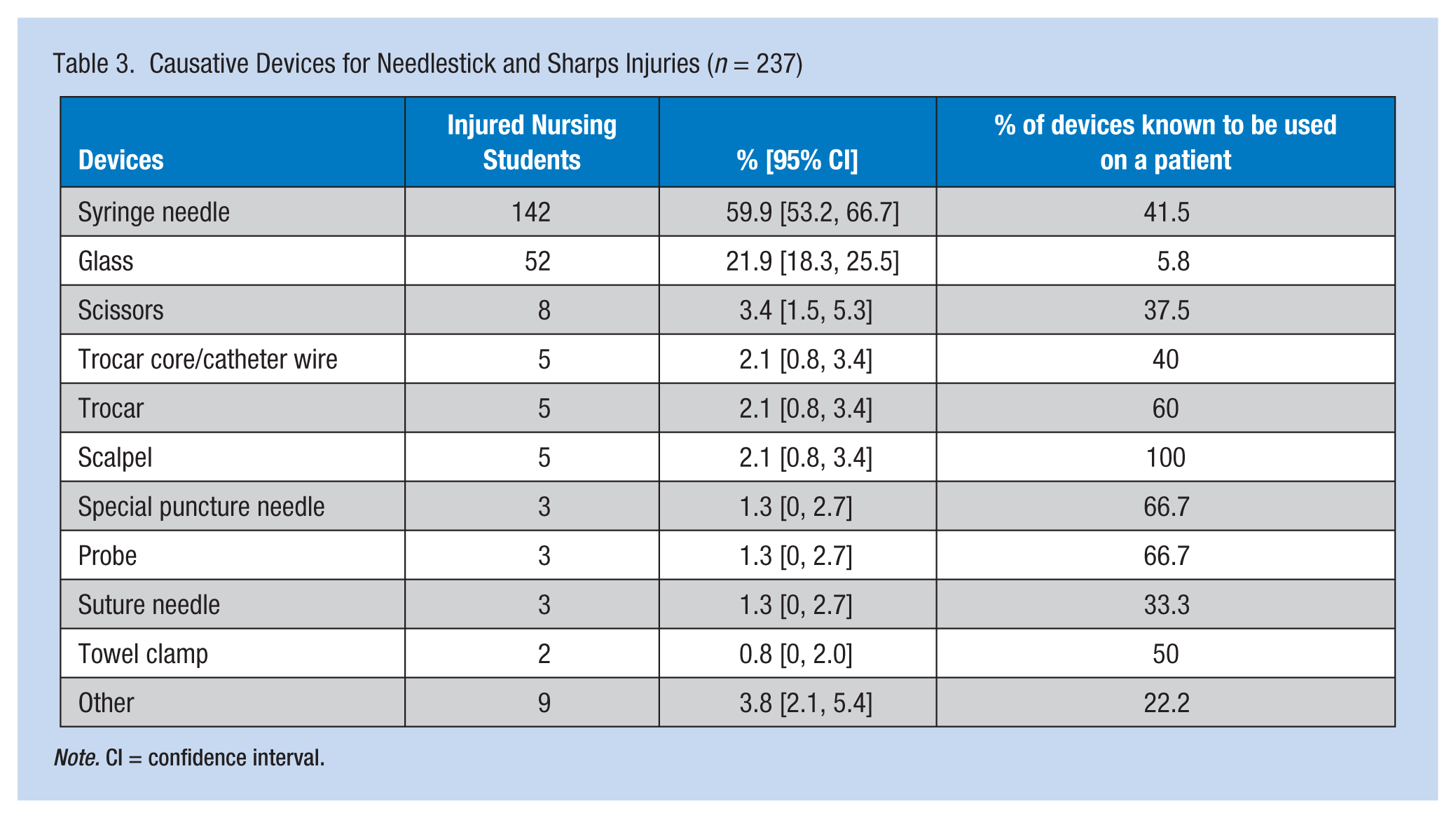
Note. CI = confidence interval.
Circumstances of injury events and usage status of NSIs are presented in Table 4. In the needle-related injuries, withdrawal needles after intravenous injection was the most common circumstance (11.4%), withdrawing medication was the next most common (11%), followed by improperly disposing of needles (9.7%). Opening ampoules or vials was the most common event resulting in sharps-related injuries (14.3%).
Causative Events Resulting in Needlestick and Sharps Injuries (n = 237)
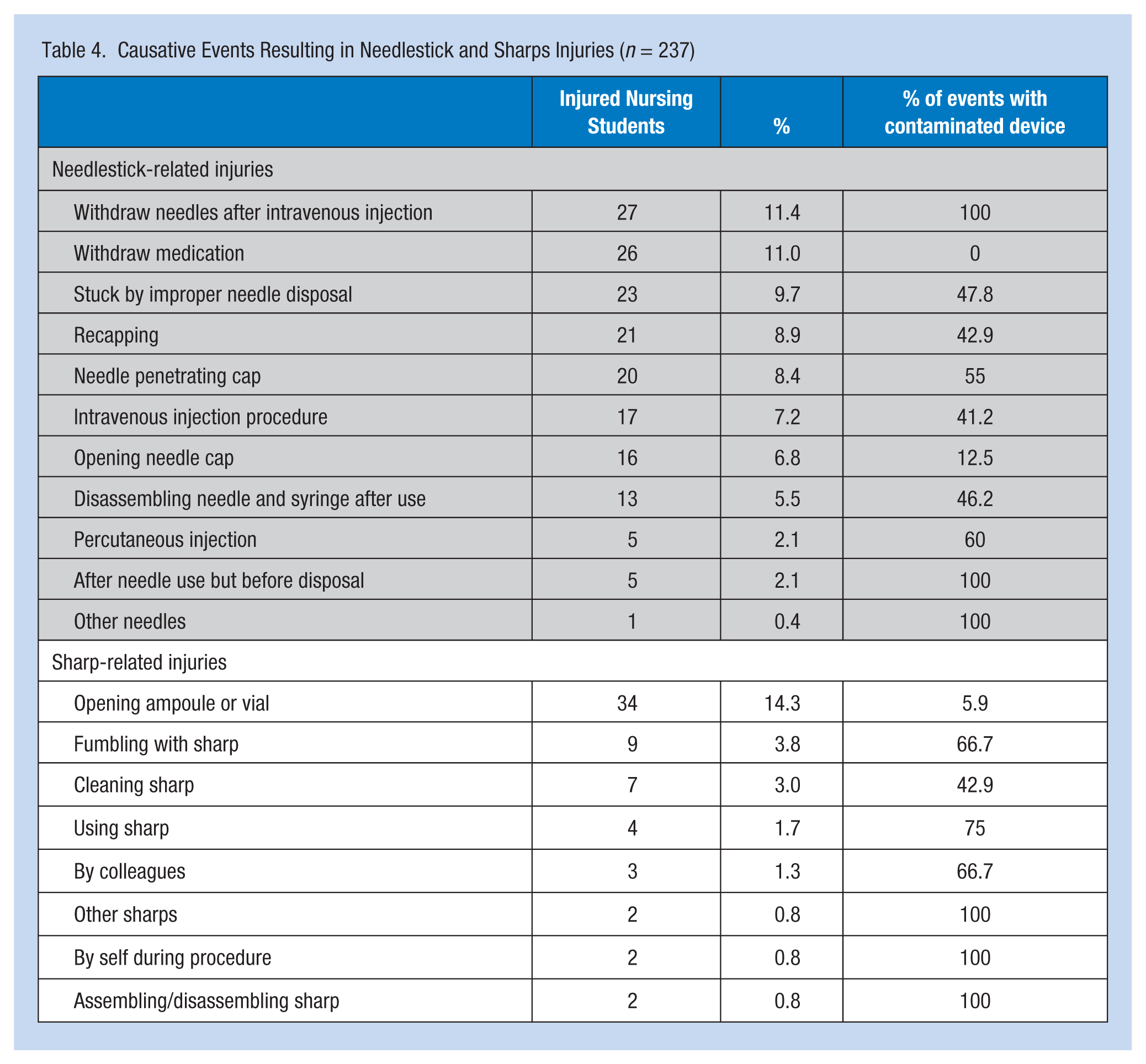
Reasons for reporting (or not reporting) NSIs are presented in Table 5. A total of 206 cases of NSIs were not reported to the infection control department of the hospital (86.9%); 35.4% of injuries were not reported due to sharp or needle not having been used on patients, 35% due to a subjective evaluation that the patient was noninfectious, and 24.5% due to a subjective evaluation of no need for reporting to the infection control department. Other reasons for not reporting NSIs by injured nursing students included being unaware of how to report NSI incidents (17.7%), being too busy at the time (10.5%), and being worried that reporting the injury to the infection control department would be criticized (3.8%). The most common reason for reporting NSIs was needing a preventive injection and monitoring (10.1%), followed by required examinations (8.9%) and treatment of wounds (4.6%).
Reasons for Reporting/Not Reporting Needlestick and Sharps Injuries (n = 237)
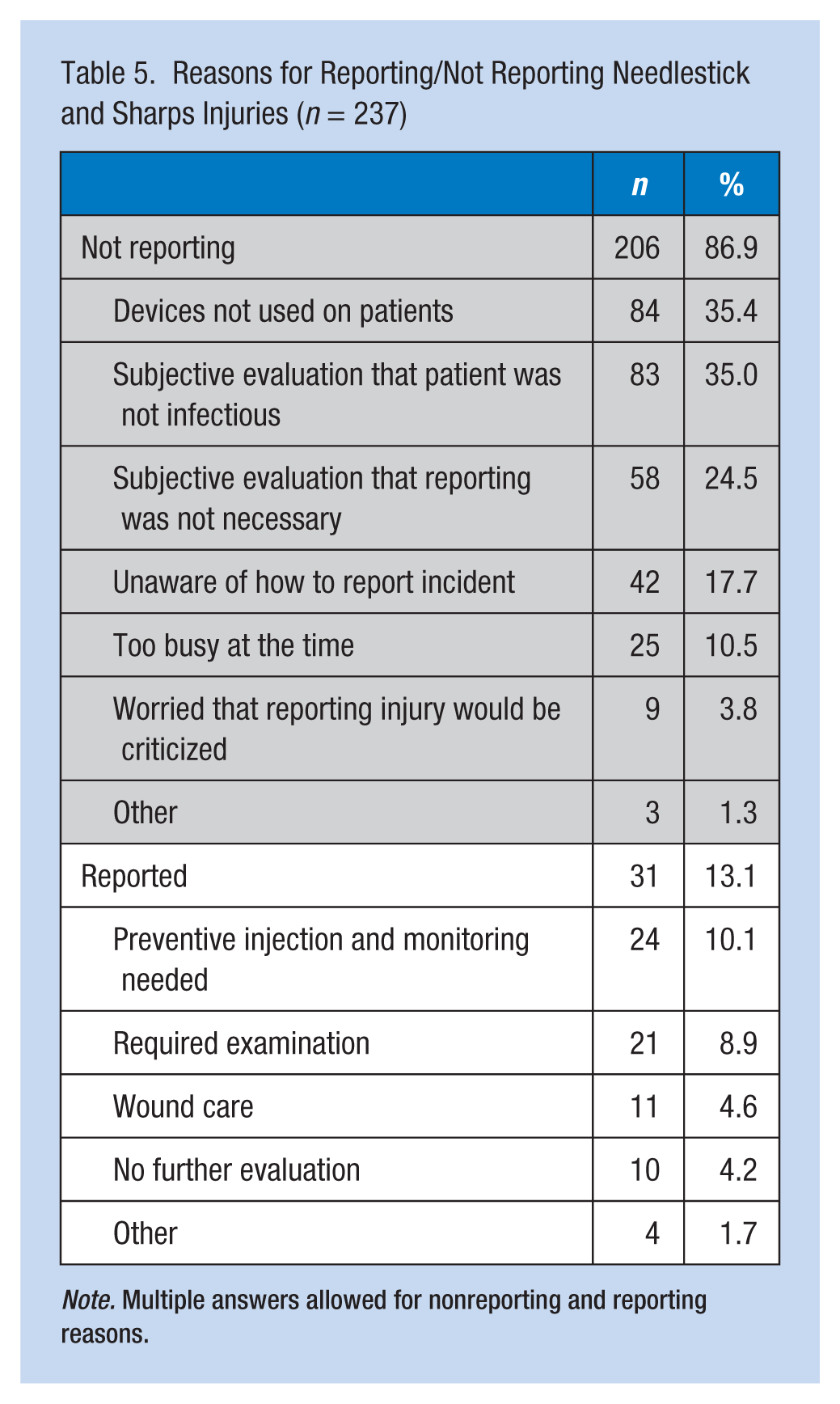
Note. Multiple answers allowed for nonreporting and reporting reasons.
Discussion
This descriptive study of NSIs among nursing students in southern China suggested that 60.3% of nursing students who provided invasive treatments and other nursing procedures in the past year suffered NSIs. Similar results have been reported by researchers from other developing countries and China (Talas, 2009; Wang et al., 2003; Yao et al., 2010). These prevalence rates in developing countries, especially China, are higher than those reported in developed countries, such as the United States and Australia (9.4% and 13.9%, respectively; Hambridge, 2011; Smith & Leggat, 2005). This study also found that the risk of NSIs due to invasive treatments and nursing procedures was significantly associated with factors such as student gender, age, night-shift frequency, injection frequency, lack of safety training, knowledge of safety management policies, and lack of PPE use. Results from multivariate modeling suggested that gender, age, night-shift frequency, lack of safety training, and lack of PPE use were statistically significant risk factors for NSIs affecting these nursing students. This study suggested that nursing students in China are at high risk of occupational exposure to blood- or body-fluid pathogens due to NSIs.
In this study, the prevalence of NSIs among female nursing students was nearly three times greater than among male nursing students, and more than 80% of NSIs occurred among nursing students aged 20 years and younger. Limited clinical experience and underdeveloped skills may increase the risk of NSIs among nursing students (Hambridge, 2011; Talas, 2009; Yao et al., 2010). However, the risk of NSIs is associated not only with skill, which is related to the frequency that a procedure is practiced, but also with hazards inherent in the procedures, such as type of needles and glass used or whether patients’ blood or body fluid is involved (Hambridge, 2011).
Night-shift frequency, as a risk factor for NSIs among these Chinese nursing students, may be explained by lack of sleep resulting in inattention and less ability to concentrate when these students are providing treatments. This study suggested nursing students who reported three or more night shifts per week were nearly six times more likely to experience NSIs than those who did not work night shifts. Nursing students have cited poor quality sleep as a contributing factor for NSIs in another study (Hambridge, 2011).
Learning clinical nursing skills and supervision by nursing instructors or seasoned practicing nurses could reduce NSIs. One noticeable result of this study is the significantly high rate of NSIs among nursing students who have not received any safety training. This finding is consistent with previous research (Cheung et al., 2012; Hambridge, 2011; Talas, 2009). Inadequate clinical skill training has been identified as the most significant risk factor for NSIs among nursing students (Shiao, Mclaws, Huang, & Guo, 2002). Safety training to prevent NSIs is essential and should focus on high-risk procedures such as various types of injections, needle disposal, removing needle caps, and opening ampoules and vials (Hambridge, 2011; Smith & Leggat, 2005). Guidelines from the National Institute for Health and Clinical Excellence recommended that sharps should not be passed from one clinician’s hand to another, and that needles must not be recapped, bent, broken, or disassembled before use or during disposal (Hambridge, 2011). A previous study conducted using the “plan (planning the change), do (implementing the change), study (reflecting on the change), act (planning the next change)” approach showed that the risk of NSIs was reduced and safe sharps disposal practices improved (Hambridge, 2011; Hatcher, 2002). The chance of NSIs was also reduced significantly by improving clinical skills during nursing students’ training (Hambridge, 2011; Petrucci, Alvaro, Cicolini, Cerone, & Lancia, 2009). Wang et al. (2003) found an association between better training (e.g., 60-minute lecture, a 20-minute video, and printed material over a 4-month period) and fewer NSIs in Chinese nursing students who had been trained. Researchers found that the group that received training scored significantly higher than the control group on both NSI prevention knowledge and behavior (Wang et al., 2003). However, students and registered nurses reported that nursing schools and training hospitals often provide inadequate occupational safety training (Hambridge, 2011; Shiao et al., 2002). In Chinese hospitals, nursing students are generally supervised by experienced nurses. This study suggests that occupational safety training and supervision by seasoned nurses should be developed and implemented for nursing students who receive their training in hospitals.
Needle protection is an effective prevention method for needlestick injuries. A review showed that reported needlestick injuries reduced by 22% to 100% after the introduction of these devices in the workplace (Tuma & Sepkowitz, 2006). Another study found that 80% of needlestick injuries were prevented by using needle-protection devices (Cullen et al., 2006). However, safety needles and devices are less commonly used in China due to their high cost (Zhang et al., 2015).
The syringe needle is believed to be the most common injury-causing device because most NSIs result from intramuscular, subcutaneous, intradermal, and intravenous needles (Phipps et al., 2002; Smith & Leggat, 2005; Zhang et al., 2015). The results of this study show that syringe needles and glass accounted for 59.9% and 21.9% of all NSIs in study nursing students, respectively. Study findings are also consistent with a previous study from Australia, where 37% of all nursing student NSIs were caused by syringe needles and 22% were due to glass containers (Smith & Leggat, 2005). A study from China also showed that most NSIs were caused by intravenous needles (44%) or syringe needles (32%). Phipps et al. found that syringe needles caused many NSIs among Chinese nurses (Phipps et al., 2002). In addition, a longitudinal study showed that syringe needles may be responsible for the highest rates of NSIs among nurses (Perry, Jagger, & Parker, 2003). This study suggested that 36.3% of injury-causing devices had been contaminated by patient blood or body fluids and 41% occurred during drug preparation. This finding is consistent with a previous study (Shiao et al., 2002).
More than 40 million individuals are currently infected with HCV, and HCV is the fourth most commonly reported infectious disease in China (Lu et al., 2013; Qin et al., 2015). The use of contaminated injection equipment may cause a significant number of undocumented exposures every day and is a major risk factor for HCV infection (Prati, 2006). Results from this study suggest that Chinese nursing students are at high risk of blood- or body-fluid pathogen exposure and perhaps transmission of HCV from contaminated devices. One study found that at least 60 blood- or body-fluid pathogens, including the most common HBV, HCV, and HIV, can be transmitted to health care workers by contaminated devices (Tarantola, Abitebout, & Rachline, 2006). Studies have suggested that only one part per 10,000 mL of HBV-infected blood is required for HBV transmission (Costigliola, Frid, Letondeur, & Strauss, 2012), and the average risk of HCV and HIV transmission after exposure due to NSIs from HCV-infected and HIV-infected blood is approximately 1.8% and 0.3%, respectively (Beltrami, Williams, Shapiro, & Chamberland, 2000).
Opening ampoules or vials was the most common incident that caused NSIs, followed by withdrawing needles after intravenous injections. Shiao et al. also reported that opening ampoules accounted for 19.3% of all NSIs in their study (Shiao et al., 2002). Furthermore, Wang et al. found that giving an injection (24%) and discontinuing an intravenous line (20%) were the most common events leading to NSIs among Chinese nursing students (Wang et al., 2003). Current study results are also consistent with findings from the United States and Australia (Smith & Leggat, 2005). Lack of clinical experience and insufficient safety training are probably responsible for the high proportion of NSIs among nursing students, as many of these injuries may actually occur the first time students handle needles (Smith & Leggat, 2005).
More than 85% of nursing students did not report NSIs to the infection control department of their hospitals, a higher proportion than the 39.5% reported in Italy, and the 56.1% reported in Turkey (Petrucci et al., 2009; Talas, 2009). In addition, research from the United States and China has shown that more than 95% of nursing students did not report NSIs to any hospital infection control department (Hambridge, 2011; Yao et al., 2010). Among Chinese nursing students, reasons for not reporting NSIs included low perceived risks, lack of safety knowledge about reporting procedures, and being too busy to report. However, even if the needle is contaminated, nurses may take a “fatalistic” view that nothing can be done and, therefore, may choose not to report the injury (Hambridge, 2011). Studies have suggested that NSI reporting must improve and training often increases NSI reporting (Hambridge, 2011; Wang et al., 2003; Yao et al., 2010).
Some study limitations must be considered when interpreting study results. First, information on NSIs was collected only for the previous 12 months prior to the survey through a cross-sectional survey. Recall bias might have led to inaccurate estimations of NSI prevalence and risk factors. Second, the study sample of nursing students was solicited from three universities in China; therefore, results of this study may not be generalizable to all nursing students in China. However, main patterns of NSIs and risk factors may be applicable to the majority of nursing students in China. Third, due to the cross-sectional design of the study, it is not possible to determine causal relationships between risk factors and NSIs. Finally, the researchers did not collect detailed information about postexposure care for injured nursing students. One troubling finding in this study is that 86.9% of injured nursing students never reported NSIs to the hospital infection control department and very few sought postexposure care or other treatment. Because NSIs have potentially significant health consequences (e.g., HBC, HCV, and HIV infections), guidelines and policies regarding reporting these injuries to hospital inflection control departments and postexposure care for nursing students and their supervising nurses should be high priority in China.
Conclusion
Needlestick and sharps injuries are a significant occupational hazard facing nursing students in China because NSIs affect Chinese nursing students at a higher rate than nursing students internationally. Syringe needles were the most common injury-causing device, and about 40% of NSIs involved devices that had been contaminated with patients’ blood or body fluids. Opening ampoules or vials was the most frequent agent of NSIs. Most surveyed nursing students did not report NSIs to the infection control department of their hospitals. Occupational safety training that targets nursing students must be strengthened before they begin clinical practice in China. Further studies are needed to develop and evaluate effective interventions to prevent NSIs among Chinese nursing students.
Applying Research to Practice
Needlestick and sharps injuries are a major cause of occupational injuries for health care workers worldwide. Nursing students are at high risk for needlestick and sharps injuries among health care workers. Females, younger students, night shift frequency, lack of occupational safety training, and lack of personal protective equipment use were significant risk factors for needlestick and sharps injuries among nursing students in China. Syringe needles were the most common causative device, and 36.3% of devices were contaminated by patient blood or body fluids. A total of 86.9% of needlestick and sharps injuries were not reported to any hospital infection control departments. Chinese nursing students are at high risk of being infected with HBV, HCV, and HIV because of their high risk of needlestick and sharps injuries at work. Further studies are needed to develop and evaluate effective interventions to prevent needlestick and sharps injuries among nursing students in China.
Footnotes
Author Contributions
X.Z., L.S., and H.X. conceived and designed the project. Y.C., Y.L., J.H., C.Z., and Z.L. were responsible for data collection. X.Z., Y.C., Y.L., J.H., C.Z., Z.L., L.S., and H.X. were involved in the data analysis, drafting the article, and its critical review. All authors read and approved the final article.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
Xujun Zhang is a professor in the Department of Epidemiology and Biostatistics, School of Public Health, Southeast University. He is the president of the Injury Prevention Research Institute at Southeast University. His research interests include multidisciplinary injury research in road safety and agricultural, childhood, and occupational injuries.
Yu Chen is a physician specializing in public health. He works at the Zhenjiang Centers for Disease Control and Prevention. His research interests include injury epidemiology and environmental epidemiology.
Yang Li is a physician specializing in public health. He is studying for a public health graduate degree at the Southeast University School of Public Health.
Jie Hu is a physician specializing in public health. She is studying for a public health graduate degree at the Southeast University School of Public Health.
Cong Zhang is a physician specializing in public health. She is studying for a public health graduate degree at the Southeast University School of Public Health.
Zhen Li is a physician specializing in public health. He is studying for a public health graduate degree at the Southeast University School of Public Health.
Lorann Stallones is a professor in the Department of Psychology, Colorado State University and in the Department of Epidemiology, Colorado School of Public Health. Her research interests are occupational injuries, agricultural safety and health, and community based injury prevention.
Henry Xiang is a professor of pediatrics, College of Medicine and a professor of Epidemiology, School of Public Health, The Ohio State University. He is the director of the Center for Pediatric Trauma Research and the director of research core and international programs for the Center for Injury Research and Policy at the Nationwide Children’s Hospital. His primary research interests include injury epidemiology among individuals with disabilities, trauma outcome research, and injury research and prevention in the developing world.
