Abstract
A 2007 study in the United Kingdom showed that three of 98 surgeons surveyed admitted using dedicated smoke extractors; 72% of respondents believed inadequate precautions were in place to protect staff from the potential dangers of electrosurgical smoke. Surgical smoke contains harmful chemicals (e.g., hydrogen cyanide, acetylene, and butadiene) that can circumvent standard masks used in the operating room (OR). In addition, bacteria and viruses can be transmitted through this smoke. The topic of electrosurgical smoke is important to occupational health nurses not only because of their responsibility to protect workers, but also because they, like other health care providers, may be exposed to smoke routinely. The authors of this review recommend the regular use of smoke evacuation in ORs and avoidance of electrosurgery whenever possible to protect OR personnel from the potential long-term harmful effects of electrosurgical smoke.
William Bovie was the first proponent of widespread use of electrical energy for heating tissue during surgical procedures. However, electricity had been used to dissect tissue before Bovie patented his famous cautery device (the Bovie) in 1931. For example, William Bierman of New York City was granted a patent in 1926 for a device shaped like pincer forceps that could heat and cut tissue (Carter, 2013).
Few articles on electrosurgical smoke combine the history of the Bovie device, the principles of its use, the dangers of the smoke plumes it creates, and recommendations for avoiding smoke plumes. Surgeons and nurses should be aware of the potential hazards of electrosurgery, and both should communicate openly about dangers in the operating room (OR) to promote change. Operating room personnel wear lead vests to protect themselves from radiation during procedures, and the authors of this article contend that surgical smoke plumes should be regarded similarly. Some health care personnel are aware of the potential dangers of electrosurgical smoke and take steps to avoid it such as using suction with electrocautery, but others do not believe electrosurgical smoke causes harm or fail to implement protective measures. A 2007 study in the United Kingdom showed that only three of 98 surgeons surveyed used dedicated smoke extractors, but 72% of respondents believed inadequate precautions were in place to protect staff from the potential dangers of electrosurgical smoke (Spearman, Tsavellas, & Nichols, 2007).
To better understand the hazards of electrosurgery, several terms must be defined. The term diathermy has been used to describe the act of passing high-frequency electrical current through deeper tissues in the body and has also been used to refer to cutting tissue. However, electrosurgery more accurately describes the process of cutting or coagulating using electrical current (Taheri et al., 2014). For the purpose of this article, the term electrosurgery will be used for any instance where cutting, coagulation, or fulguration occurs. Surgical smoke refers to any smoke, visible or microscopic, created by electrosurgical devices.
During the process of electrosurgery, current is produced by a generator and sent to an active electrode. In monopolar electrosurgery, the active electrode concentrates the current in a small tip before cutting. When the electricity exits the body, it does so through a large return electrode so the exiting current is dispersed over a greater area. Burn is a common complication of monopolar electrosurgery (Barrett, Vella, & Dellon, 2010).
In bipolar electrosurgery, the instrument contains an active electrode on one side of a pair of forceps and a return electrode on the other side. The only tissue exposed to current is the tissue grasped by the forceps. Created by Emile-Rioux, a Canadian gynecologist, bipolar energy alleviates complications that may occur with monopolar energy (Barrett et al., 2010). The remainder of this article discusses the dangers of surgical smoke created by either monopolar or bipolar energy. The most basic settings of the electrosurgical tool are for cutting and coagulation. The pure cut mode vaporizes cells using intense heat. The coagulation setting is used when the electrode is held against tissue causing hemostasis without cutting (McCauley, 2010).
Background
Physicians and other health care personnel are exposed to various carcinogenic materials and radiation in hospitals, which may lead to an increased risk of malignant tumors (Eriksson, Hardell, Malker, & Weiner, 1998). Moreover, a total of approximately 500,000 surgeons, nurses, anesthesiologists, and technicians are exposed to surgical smoke in the OR, and these exposures are cumulative over their lifetimes (Choi, Kwon, Chung, & Kim, 2014).
Electrosurgical smoke contains potentially hazardous organic and inorganic compounds; the researchers of one study found the amount of surgical smoke produced in a plastic surgery operating theater was equivalent to 27 to 30 cigarettes (Hill, O’Neill, Powell, & Oliver, 2012). The scientific community has demonstrated increasing interest in identifying the contents of surgical plumes, and the behavior and protective measures of some OR staff. Researchers and providers are also concerned about patient health, as a closed gaseous environment created during abdominal laparoscopic surgery can result in systemic absorption of toxic compounds created by electrosurgery (Canadian Standards Association [CSA], 2013; Dobrogowski, Wesolowski, Kucharska, Sapota, & Pomorski, 2014). This article provides a review of the evidence regarding hazards of electrosurgical smoke so that OR and occupational health and safety personnel can make informed decisions about protecting worker health. Measures to avoid the smoke or be protected from it are also discussed.
Method
A PubMed search was initiated using the search terms electrosurgical smoke, electrocautery smoke, diathermy smoke, and William Bovie. These terms were determined to be the most pertinent to this review and resulted in the greatest number of potential articles. The authors then searched these articles for any available data on the harmful effects of electrosurgical smoke as well as smoke composition to determine what, if any, toxic substances are present in electrosurgical smoke. Websites of national organizations were also reviewed for guidelines on smoke evacuation. Articles selected from the initial search were peer-reviewed, published between 1981 to present, and published or translated in English. Articles included were those that discussed principles of electrosurgery, composition and effects of electrosurgical smoke, and methods for minimizing exposure to smoke.
After combining the results from all PubMed search terms previously mentioned, 191 articles were identified. Of these, 16 were excluded because they were not written in or translated to English. Another 132 articles were deemed irrelevant. Overall,43 articles met inclusion criteria for this review. The search strategy is diagrammed in Figure 1.
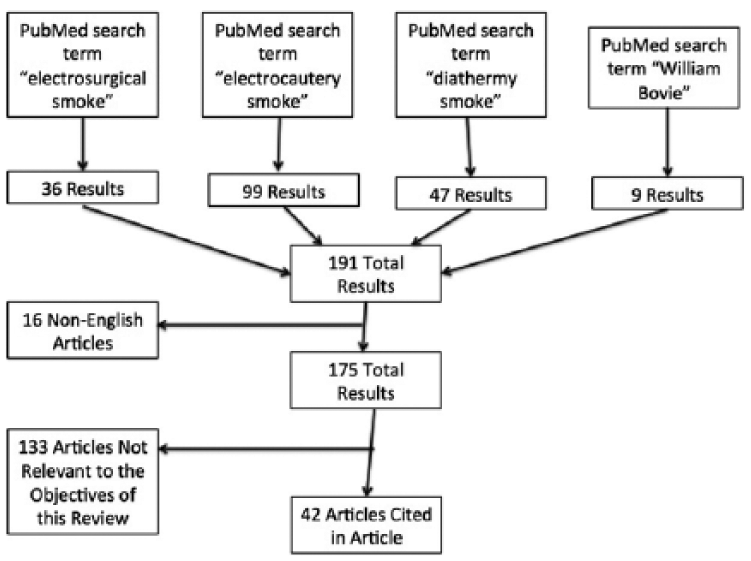
Search strategy.
Results
Table 1 provides a summary of each article cited in this review with the title, year, category, and important findings. A total of 22 articles discussed the composition of smoke and its harmful effects, 12 articles contained information about smoke evacuation and protection, and nine articles provided background information.
Articles Cited From Literature Review
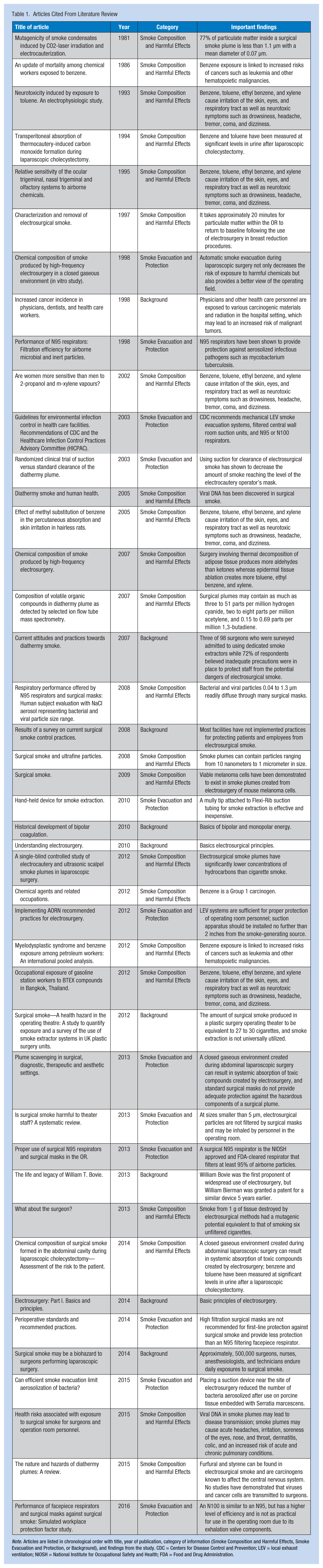
Note. Articles are listed in chronological order with title, year of publication, category of information (Smoke Composition and Harmful Effects, Smoke Evacuation and Protection, or Background), and findings from the study. CDC = Centers for Disease Control and Prevention; LEV = local exhaust ventilation; NIOSH = National Institute for Occupational Safety and Health; FDA = Food and Drug Administration.
Composition
Approximately 77% of the particulate matter inside a surgical smoke plume is less than 1.1 µm with a mean diameter of 0.07 µm (Tomita et al., 1981). However, these plumes can also contain extremely high levels of ultrafine particles ranging from 10 nm to 1 µm (Brüske-Hohlfeld et al., 2008). At sizes smaller than 5 µm, these particles are not filtered by surgical masks and may be inhaled by personnel in the OR (Mowbray, Ansell, Warren, Wall, & Torkington, 2013).
Surgical plumes may contain as much as three to 51 parts per million hydrogen cyanide, two to eight parts per million acetylene, and 0.15 to 0.69 parts per million 1,3-butadiene (Moot et al., 2007). Surgery involving thermal decomposition of adipose tissue produces more aldehydes than ketones whereas epidermal tissue ablation creates more toluene, ethyl benzene, and xylene (Al Sahaf, Vega-Carrascal, Cunningham, McGrath, & Bloomfield, 2007). Other chemicals found in electrosurgical smoke include the eye and respiratory tract irritants furfural and styrene, a teratogen, and carcinogen known to affect the central nervous system (Lindsey, Hutchinson, & Mellor, 2015).
Although many potentially hazardous chemicals exist in surgical smoke, electrosurgical smoke plumes have been found to have significantly lower concentrations of hydrocarbons than cigarette smoke (Fitzgerald, Malik, & Ahmed, 2012). However, a 2013 study found that the smoke from 1 g of tissue destroyed by electrosurgical methods had the mutagenic potential of smoking six unfiltered cigarettes (Khajuria, Maruthappu, Nagendran, & Shalhoub, 2013).
Potential harm to patients from exposure to electrosurgical smoke is an additional concern because benzene and toluene have been measured at significant levels in patients’ urine after laparoscopic cholecystectomies (Dobrogowski et al., 2014; Esper et al., 1994). The effects of short-term exposure to toxic compounds in these patients, however, may be negligible compared with the effects of chronic gaseous exposure on OR personnel. It is also important to note that chemical compositions and gaseous concentrations can vary widely based on specific surgical procedures studied.
Bacterial transmission to nearby sites has been shown to occur during blended current electrosurgery on infected tissue but was not evident with pure coagulation electrosurgery (Schultz, 2015). This finding suggests that disease can be transmitted directly to OR personnel. In addition, bacteria may potentially seed to distant OR surfaces or adjacent exposed tissue within patients.
Viral DNA has been identified in surgical smoke (Christie, Jefferson, & Ball, 2005) and could potentially transmit disease (Okoshi et al., 2015). Viable melanoma cells have been found in smoke plumes created during electrosurgery of mice with melanoma (Fan, Chan, & Chu, 2009). However, no studies have demonstrated the transmission of viruses or cancer cells to OR personnel during electrosurgery (Lindsey et al., 2015).
Effects of Electrosurgery Smoke
In recent years, providers and researchers have shown increasing concern for the safety of electrosurgical devices. Studies have demonstrated an association between smoke plumes from electrosurgery and acute headaches; eye, nose, and throat irritations; dermatitis; colic; and acute and chronic pulmonary conditions (Okoshi et al., 2015). Although few articles discussed the link between electrosurgical smoke and specific health problems, these effects may be a direct result of the smoke’s composition.
Avoiding Smoke Exposure
Protection from surgical smoke can be achieved by local extraction of smoke at the site of the electrosurgery or by use of personal filtration masks to prevent inhalation of particles and any viable biological pathogens (Benson, Novak, & Ogg, 2013). To remove electrosurgical smoke from the OR, mechanical local exhaust ventilation (LEV) devices are used. These devices may attach directly to a Bovie device or operate separately.
A surgical mask is a Food and Drug Administration (FDA)–cleared mask that protects the wearer from microorganisms, body fluids, and large particles greater than 5 µm in size. A surgical N95 respirator is National Institute for Occupational Safety and Health (NIOSH) approved and FDA cleared; it filters at least 95% of airborne particles. Before using an N95, all operators should be fit-tested to a specific sized mask to ensure an adequate face seal. In support of their use, N95 respirators have been shown to provide protection against aerosolized infectious pathogens such as mycobacterium tuberculosis (Qian, Willeke, Grinshpun, Donnelly, & Coffey, 1998). An example of the N95 respirator can be seen in Figure 2.

Example of N95 respirator.
An N100 respirator is similar to the N95, but has a higher level of efficiency and is not as practical for use in the OR due to its exhalation valve components (Gao, Koehler, Yermakov, & Grinshpun, 2016). The powered air purifying respirator (PAPR) is another commonly used mask, but it does not protect OR personnel from smoke (Benson et al., 2013).
The CSA states that standard surgical masks do not provide adequate protection against the hazardous components of a surgical plume (CSA, 2013). Even high filtration surgical masks are not recommended for first-line protection against surgical smoke inhalation or protection from chemical and particulate contaminants found in surgical smoke (Conner, Denholm, & Burlingame, 2014). In the case of electrosurgical smoke, these high filtration masks provide less protection than a filtered N95 filtering facepiece respirator (Conner et al., 2014). A major concern is that surgical masks often fit loosely and allow aerosolized particulates to be inhaled, bypassing all filters. Bacterial and viral particles 0.04 to 1.3 µm readily diffuse through surgical masks, resulting in failure of these masks to reach minimum standards of respiratory protection required by the Occupational Safety and Health Administration (OSHA; Lee, Grinshpun, & Reponen, 2008).
In the Guidelines for Environmental Infection Control in Healthcare Facilities, the Centers for Disease Control and Prevention (CDC) recommends three ways to minimize exposure to surgical smoke:
Mechanical LEV smoke evacuation systems with high-efficiency filtration systems should be used during procedures involving ablation of Human Papilloma Virus (HPV) infected tissue.
Filtered central wall room suction units can evacuate surgical smoke.
Personal protective equipment such as N95 or N100 respirators can reduce exposure to the contents of surgical plumes (Sehulster & Chinn, 2003).
The CDC suggests that a suction device operating at a minimum of 100 to 150 feet per second should be used in conjunction with air filters effective with particles as small as 0.1 µm in size (Spearman et al., 2007).
The Association of periOperating Room Nurses publication, Recommended Practices for Electrosurgery, states that LEV systems are sufficient for proper protection of OR personnel and that the suction apparatus should be installed no further than 2 inches from the smoke-generating source (Spruce & Braswell, 2012). According to Schultz (2015), placing a suction device near the site of electrosurgery reduced the number of bacteria aerosolized after use on porcine tissue embedded with Serratia marcescens. In addition, automatic smoke evacuation during laparoscopic surgery not only decreases the risk of exposure to harmful chemicals but also provides a better view of the operating field (Hensman, Baty, Willis, & Cuschieri, 1998). Using suction for clearance of electrosurgical smoke has been shown to decrease the amount of smoke reaching the level of the electrocautery operator’s mask (Pillinger, Delbridge, & Lewis, 2003).
Although suction catheters with mully tips attached to Flexi-Rib suction tubing for smoke extraction are effective and inexpensive (King & Ferguson, 2010), smoke extractors are not universally utilized (Hill et al., 2012), and most facilities have not implemented practices for protecting patients and employees from electrosurgical smoke (Edwards & Reiman, 2008). Without the use of adequate evacuation systems, one study reported that it takes approximately 20 minutes for particulate matter within the OR to return to baseline following the use of electrosurgery devices during breast reduction procedures (Brandon & Young, 1997). Table 2 includes a summary of the recommendations to guide occupational health nurses in reducing worker exposures to electrosurgical smoke. The table also contains methods that may not protect OR personnel from smoke exposure.
Recommendations for Avoiding Electrosurgical Smoke Exposure
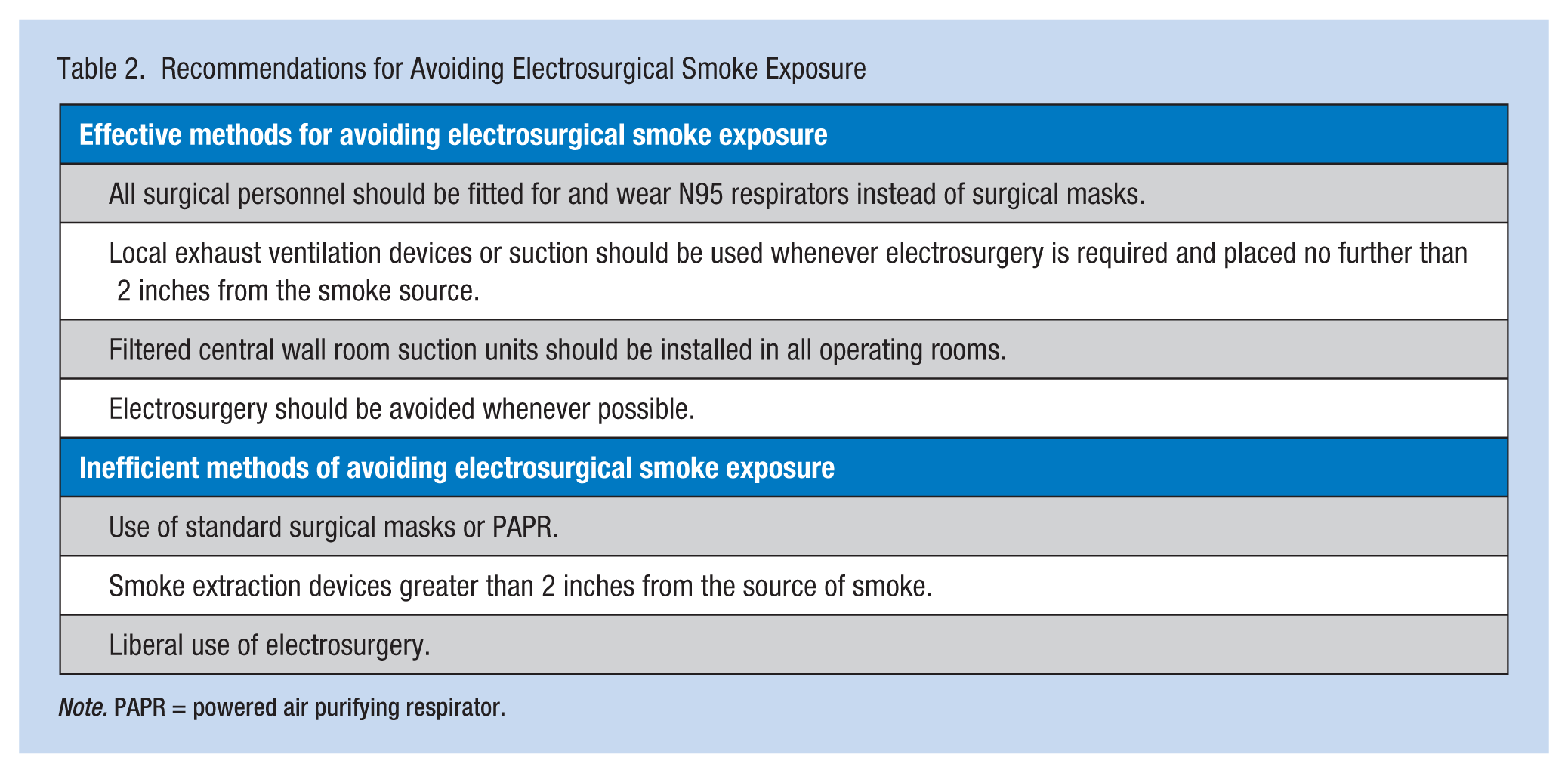
Note. PAPR = powered air purifying respirator.
Conclusion
Although evidence is currently inadequate to directly link electrosurgical smoke to increased morbidity and mortality among OR personnel, the authors of this review recommend the regular use of smoke evacuation in ORs and to avoid the use of electrosurgery whenever possible. Many of the particles produced by electrosurgery are small enough to be inhaled through a surgical mask, and several of the particles contain known carcinogens. Benzene, for example, was categorized in 2012 by the International Agency for Research on Cancer (IARC) as a Group 1 carcinogen, meaning exposure to benzene has a high potential of causing cancer in humans (Abbate, Giorgianni, Munaò, & Brecciaroli, 1993; IARC Working Group on the Evaluation of Carcinogenic Risk to Humans, 2012). Current literature also links benzene exposure to increased risk of leukemia and other hematopoietic malignancies (Bond, McLaren, Baldwin, & Cook, 1986; Schnatter, Glass, Tang, Irons, & Rushton, 2012). In addition, benzene, toluene, ethyl benzene, and xylene cause irritation of the skin, eyes, and respiratory tract as well as neurotoxic symptoms such as drowsiness, headache, tremor, coma, and dizziness (Abbate et al., 1993; Ahaghotu, Babu, Chaterjee, & Singh, 2005; Cometto-Muñiz & Cain, 1995; Ernstgård, Gullstrand, Löf, & Johanson, 2002; Tunsaringkarn, Siriwong, Rungsiyothin, & Nopparatbundit, 2012).
Exposure to carcinogens and the development of malignant cancers are a cumulative process. The adverse effects of inhaling surgical smoke have historically been downplayed because exposure to such smoke does not cause obvious short-term adverse health effects. Although no study has demonstrated that electrosurgical smoke alone causes cancer, chronic exposure to the contents of surgical smoke may contribute to this process. The authors advocate for a long-term prospective study that examines the incidence of comorbid conditions among OR personnel, monitoring their daily exposure to electrosurgical smoke to separate real from perceived hazards of electrosurgery smoke exposures. A study of this type may delineate a link, if one exists, between electrosurgical smoke and adverse health outcomes.
Operating room personnel should continue to assess the hazards of long-term exposure to electrosurgical smoke, and systematic steps should be taken to reduce exposure to aerosolized toxic compounds generated during electrical pyrolysis of human tissue. Clearly, long-term studies on the relationship between electrosurgical smoke and health risks among OR personnel compared with the general population are warranted to determine the risk of chronic electrosurgical smoke exposures to health care workers.
In Summary
Inadequate steps are being taken to protect operating room personnel from the harmful effects of surgical smoke, which contains particulate matter, various chemicals, and some microorganisms.
Standard surgical masks are ineffective at filtering potentially harmful substances from electrosurgical smoke; N95 respirators are the preferred personal protective equipment for operating room personnel exposed to harmful chemicals during electrosurgery.
Smoke evacuation systems or suction devices should be used whenever electrosurgery is performed and should be no further than 2 inches from the source of the smoke. However, to protect workers, electrosurgery should be avoided whenever possible.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
Kevin Bree is a PGY1 general surgery resident at the Wright State University Boonshoft School of Medicine in Dayton, Ohio.
Spencer Barnhill is a third-year medical student at the Wright State University Boonshoft School of Medicine in Dayton, Ohio.
William Rundell is a clinical professor at the Wright State University Boonshoft School of Medicine in Dayton, Ohio. He is also the emeritus surgical director of the Transplant Program at Miami Valley Hospital in Dayton, Ohio.
