Abstract
This study examined nurse practitioners’ (NPs) previous experiences and comfort levels in treating adolescents with work-related injuries in two states where NPs have statutory authority to treat work-related injuries. The authors surveyed all actively licensed NPs in Washington and Oregon (N = 4,849). Factors associated with NPs’ previous experiences and comfort in treating adolescents with work-related injuries were identified using modified Poisson regression. Less than a quarter of respondents (21.1%, n = 225) reported having ever treated an adolescent for a work-related injury. Nearly half (43.6%) of respondents reported being uncomfortable or very uncomfortable in treating adolescents with work-related injuries. Previous experience and male gender were associated with greater likelihood of feeling comfortable (p < .01). Nurse practitioners serve as primary care providers for adolescents who may experience work-related injuries. This study documents the need for developing educational and outreach efforts to better prepare NPs to treat adolescents’ work-related injuries.
Keywords
Across the United States, nurse practitioners (NPs) provide health care to patients in communities where access to primary care providers is often limited. In Washington and Oregon, NPs are licensed independent providers who can provide care and services to patients without authorization from an attending physician. Previous research has documented that care provided by NPs is cost-effective, safe, and of high quality compared with care provided by physicians (Chenoweth, Martin, Pankowski, & Raymond, 2008; Newhouse et al., 2011; Sears, Wickizer, Franklin, Cheadle, & Berkowitz, 2008).
Nurse practitioners play important roles in treating injured workers, especially in rural areas. An analysis of Washington State workers’ compensation (WC) data showed that in the year after NPs gained statutory authority to treat WC injuries, they served as the first attending provider for 3,211 claims (7.5% of 42,533 claims), with NPs caring for proportionally more patients in rural and underserved areas (Sears, Wickizer, Franklin, Cheadle, & Berkowitz, 2007a, 2008). In Washington State, a series of studies identified little to no difference between WC claimants’ health care quality, associated costs, duration of lost work time, and case mix when NPs’ patients were compared with the patients of other providers (Sears et al., 2007a; Sears, Wickizer, Franklin, Cheadle, & Berkowitz, 2007b).
An estimated 1.5 million 16- and 17-year-olds are employed in the United States each year (Bureau of Labor Statistics, Employment and Earnings, 2014), primarily working in the summer or part-time during the school year (Herman, 2000; Staff, Messersmith, & Schulenberg, 2009). Compared with adult workers, young workers experience higher fatal and nonfatal occupational injury rates (Breslin & Smith, 2005; Estes, Jackson, & Castillo, 2010), yet underreporting of work-related injuries is relatively common among adolescents (Tucker, Diekrager, Turner, & Kelloway, 2014). Given that treating work-related injuries is within the scope of NP practice in Washington and Oregon, it is critical that NPs feel comfortable treating adolescents with work-related injuries.
As part of a larger study, the authors surveyed NPs in Washington and Oregon about their experience and comfort level in treating adolescents with work-related injuries. Study objectives were to (a) describe the characteristics of NPs who reported experience in treating work-related injuries in adolescents and (b) identify factors associated with NPs who indicated that they felt comfortable or very comfortable in treating adolescents with work-related injuries. Although the first objective was exploratory, the researchers hypothesized that previous experience in treating work-related injuries in adolescents would be highly associated with comfort in providing treatment.
Method
This study was conducted as part of a large cross-sectional survey about adolescent concussion diagnosis and management administered to all actively licensed family, pediatric, adult, and psychiatric mental health NPs in Washington and Oregon. The survey sample (N = 4,849) was derived from state licensing registries; respondents with home addresses in Washington, Oregon, or bordering states (Idaho, California, Nevada, or British Columbia) were included in the sampling frame.
The survey was administered online only. Initial contact was via postal invitation with the web survey URL and instructions. Each participant received a unique identification code to access the survey. Nonrespondents were sent up to six reminder notifications (three postal and three electronic invitations) over 16 weeks. Electronic invitations were only sent to nurses with email addresses (n = 3,549; 73%). Respondents were offered entry into a raffle for an iPad mini ($329) for participation. The authors were blinded to participant name and email address; responses did not include identifiable information. This study was considered exempt from human subjects review by the Washington State University institutional review board.
Outcome Variables
The first outcome variable was NPs’ experience in treating work-related injuries in adolescents, determined by the question “Have you ever treated an adolescent for an injury that occurred while they were working in a job?” The second outcome variable of comfort was determined by the question “How comfortable would you say you are in treating occupational or work-related injuries in adolescents?” with possible responses ranging from “very uncomfortable,” “uncomfortable,” and “neutral” to “comfortable” and “very comfortable.” Responses were recoded as “comfortable” with selections of “comfortable” or “very comfortable.”
Respondent Characteristics
Respondent demographic characteristics included gender and age (categorized as <35 years, 35-44 years, 45-54 years, 55-64 years, and ≥65 years). Licensing state (Washington or Oregon) was derived from the state licensing registry data. Respondents indicated the year they completed their NP training, which was subsequently categorized as before 1980, 1980-1989, 1990-1999, 2000-2009, or 2010 or later. They also reported their NP specialty as family NP, psychiatric/mental health NP, pediatric NP, adult NP, or other (i.e., midwives, acute care NPs, or dual specialty) and whether they held board certification in the same areas as their educational training.
Practice Characteristics
The percent of pediatric patients in the NPs’ practice was ascertained by self-report and categorized as 50% or fewer, or more than 50%. Respondents also indicated whether they currently practice in an outpatient setting (including urgent care or emergency departments), as opposed to an academic or inpatient setting (yes/no).
Analysis
Bivariate techniques were used to evaluate the association between respondent and practice characteristics and the two outcome variables; significant associations were identified using Pearson’s chi-square test. Characteristics of respondents and nonrespondents were assessed using the Pearson’s chi-square test for state and Fisher’s exact test for specialty. The relationship between the two outcome variables was also assessed in a similar fashion. The researchers used a modified Poisson regression approach with robust error variance (Zou, 2004) to evaluate the association between respondent and practice characteristics and the outcome variables. First, crude, unadjusted models were generated to estimate the relative risk of each variable independently contributing to (a) NPs’ report of ever having treated an adolescent with a work-related injury in the past and (b) NPs’ indications of feeling “comfortable” or “very comfortable” in treating adolescents with work-related injuries. Next, multivariable models were used to estimate the likelihood of each outcome while controlling for aforementioned covariates. To assess collinearity between categorical variables in the regression models, the researchers examined Pearson’s correlation and investigated any pairs with correlation coefficients more than .5, removing one variable from the multivariable regression model if applicable. Descriptive and inferential analyses were performed using the svy command in Stata/MP 13.1 (StataCorp, College Station, Texas). Poststratification weights were applied to survey responses to account for differential responses across states and specialty areas between respondents and nonrespondents.
Results
Of 4,849 eligible NPs, 1,156 completed the survey at least partially (23% response rate). Among these, 92% (n = 1,064) of NPs responded to questions pertaining to work-related injuries in adolescents. Respondents differed slightly from nonrespondents in terms of specialty and state (Table 1); poststratification weights were applied. Respondents were predominantly more than 45 years of age (67%), female (87.3%), from Washington (65.4%), and family NPs (64.9%; Table 1). Most completed NP training after 2000 (61.6%) and worked in outpatient settings (76.5%). Few (16.9%) respondents indicated serving a population of mostly pediatric patients.
Characteristics of Study Population Based on Experience and Comfort Treating Adolescents With Work-Related Injuries
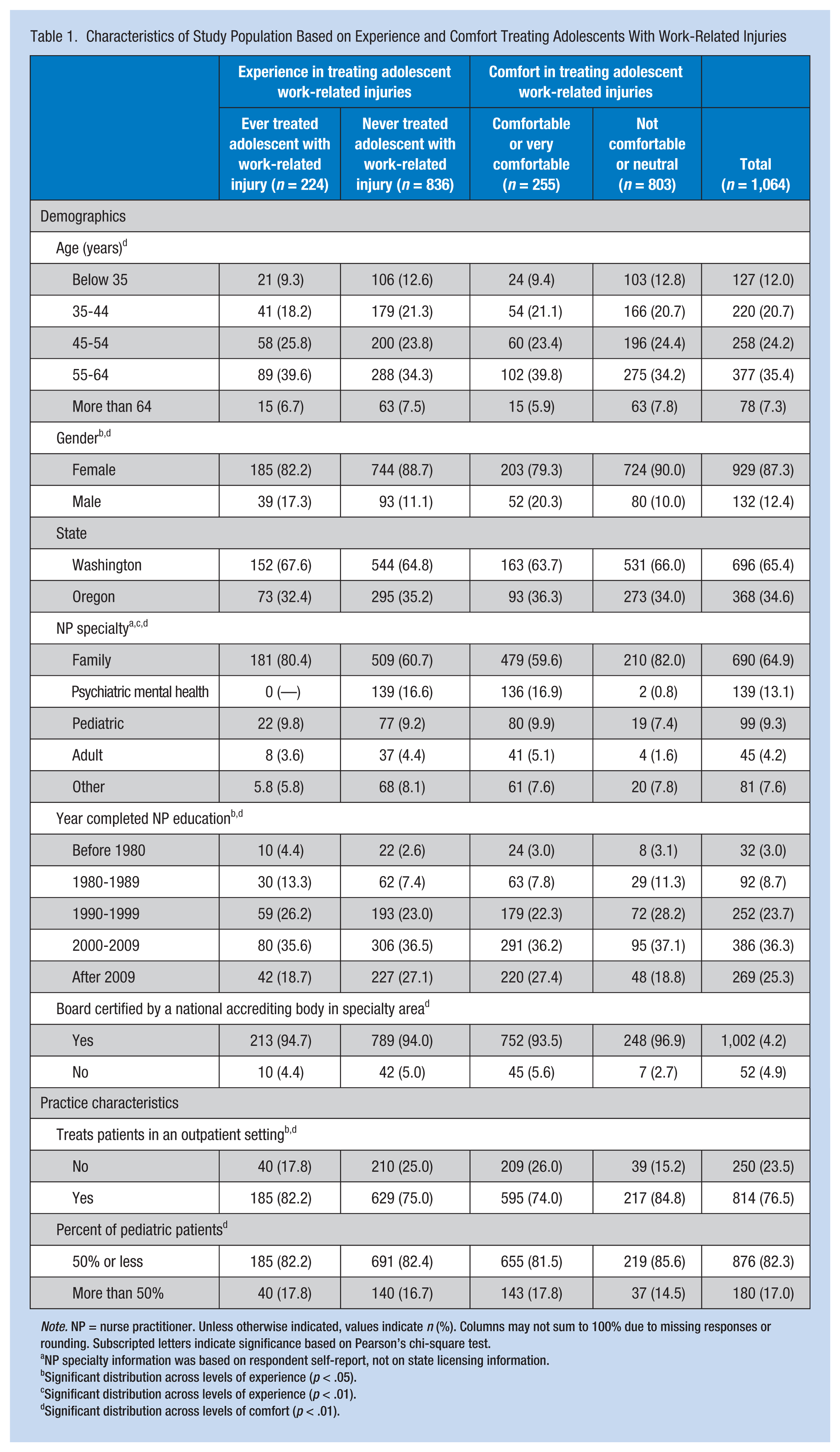
Note. NP = nurse practitioner. Unless otherwise indicated, values indicate n (%). Columns may not sum to 100% due to missing responses or rounding. Subscripted letters indicate significance based on Pearson’s chi-square test.
NP specialty information was based on respondent self-report, not on state licensing information.
Significant distribution across levels of experience (p < .05).
Significant distribution across levels of experience (p < .01).
Significant distribution across levels of comfort (p < .01).
Experience in Treating Adolescents With Work-Related Injuries
Less than a quarter of respondents (21.1%, n = 225) reported having ever treated an adolescent for a work-related injury. Nurse practitioners with training in family practice more frequently reported having ever treated an adolescent with a work-related injury (chi-square test, p < .01; Online Supplemental Table 1). Other characteristics associated with experience in treating adolescents with work-related injuries included gender (p = .01), year of completion of NP training (p < .01), and treating patients in an outpatient setting (p = .02; Table 1).
For this outcome, regression models estimated the relative risk of reporting ever treating an adolescent with a work-related injury. Unadjusted regression models reflect associations presented in bivariate analysis: Male NPs were significantly more likely to report having previous experience treating work-related injuries in adolescents as were NPs who completed their degree programs between 1980 and 1989, and those who did not treat patients in an outpatient setting (Table 2). Collinearity across variables was not observed, so all covariates listed in Table 1 were included in multivariable regression models. Multivariable results indicated that male NPs were 53% more likely to report having ever treated an adolescent work-related injury (risk ratio [RR] = 1.53, 95% confidence interval [CI] = [1.15, 2.04]), compared with female NPs, after adjusting for all other covariates (Table 2).
Factors Associated With Report of Previous Experience in Treating Adolescent Work-Related Injuries
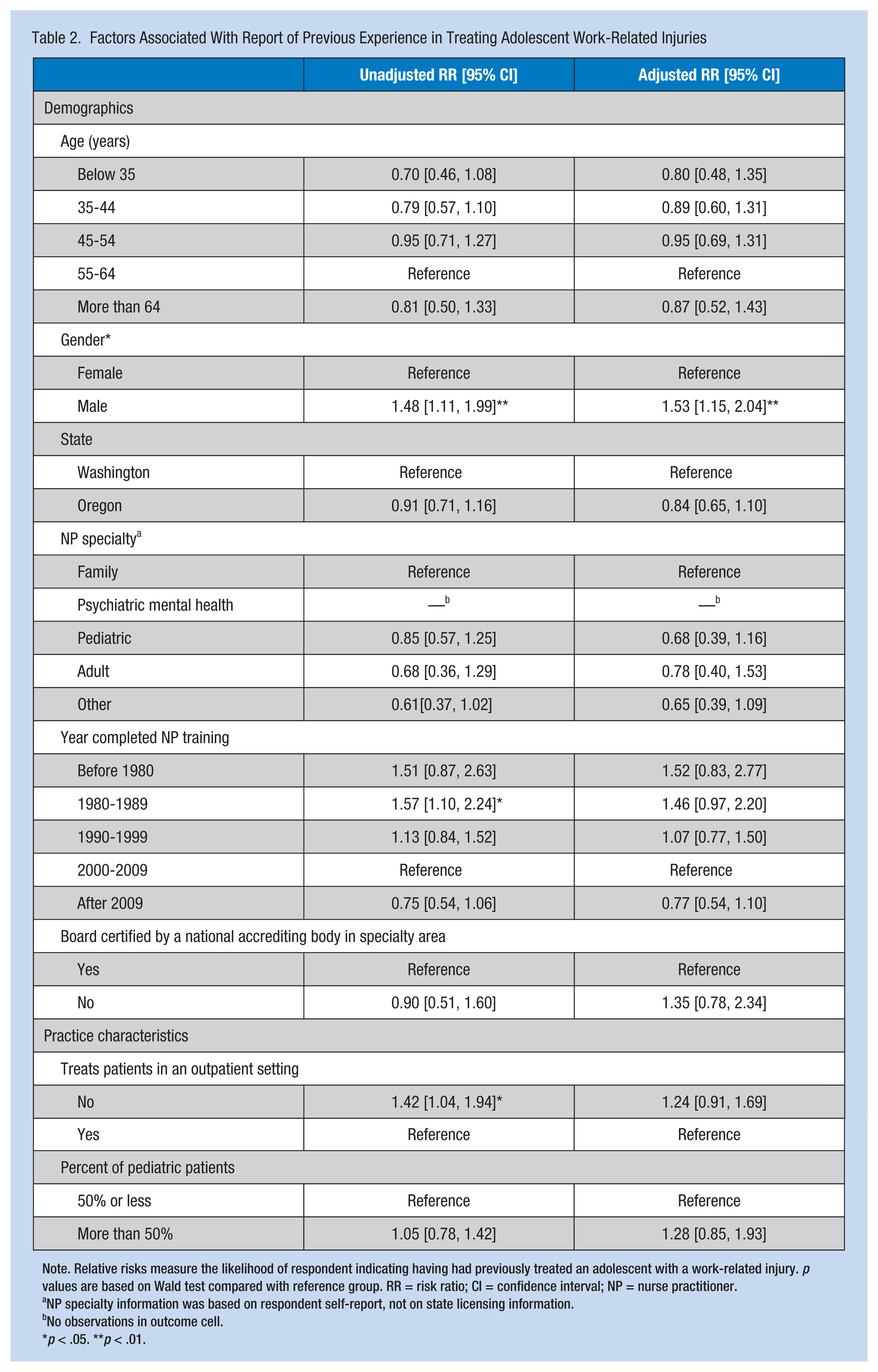
Note. Relative risks measure the likelihood of respondent indicating having had previously treated an adolescent with a work-related injury. p values are based on Wald test compared with reference group. RR = risk ratio; CI = confidence interval; NP = nurse practitioner.
NP specialty information was based on respondent self-report, not on state licensing information.
No observations in outcome cell.
p < .05. **p < .01.
Comfort Level
Few NPs indicated a high level of comfort (“very comfortable”) in treating occupational or work-related injuries in adolescents (5.7%), whereas nearly 43.6% reported being uncomfortable or very uncomfortable (25.0% and 18.6%, respectively). Overall, 255 NPs reported being comfortable or very comfortable in treating adolescents with work-related injuries, compared with 803 NPs who reported feeling either neutral or uncomfortable. Variables showing significant relationships with comfort include age, gender, specialty, year training was completed, board certification, treating patients in an outpatient setting, and percent of pediatric patients (Table 1). Previous experience in treating adolescents with work-related injuries was correlated with greater reported comfort in treating such injuries (Figure 1). For instance, among the 61 NPs who indicated they were “very comfortable” treating adolescent work-related injuries, 75.4% (n = 46) reported having treated similar patients in the past.
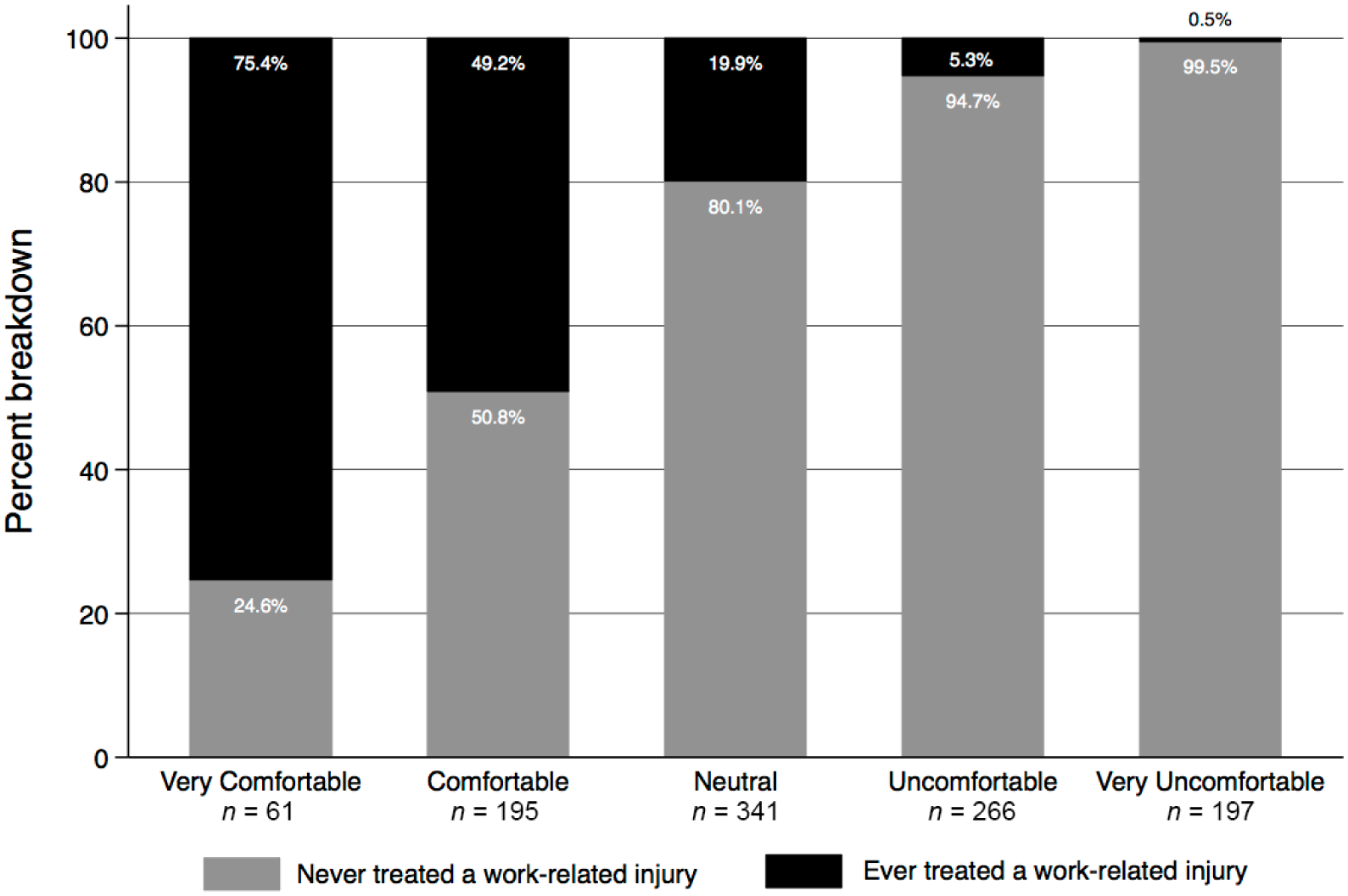
Nurse practitioners’ comfort and experience in treating adolescents with work-related injuries.
Unadjusted regression models showed that previous experience, certain NP specialties, and not treating patients in an outpatient setting reflected an increased likelihood of comfort in treating an adolescent with a work-related injury (Table 2). Multivariable regression results indicate that NPs with previous experience treating work-related injuries in adolescents were 3.5 times more likely to indicate that they were comfortable or very comfortable in treating those patients, after adjusting for covariates (RR = 3.51, 95% CI = [2.87, 4.29]; Table 3). Accounting for previous experience and other demographic and practice characteristics, other factors significantly associated with comfort in treating work-related injuries in adolescents included gender (i.e., male NPs were 50% more likely to indicate feeling comfortable) and not working in an outpatient setting, even after adjusting for previous experience. Conversely, psychiatric and adult NPs indicated significantly lower likelihood of feeling comfortable in treating adolescents with work-related injuries, even after accounting for their relatively limited experience and other characteristics (Table 3).
Factors Associated With Comfort in Treating Work-Related Injuries in Adolescents
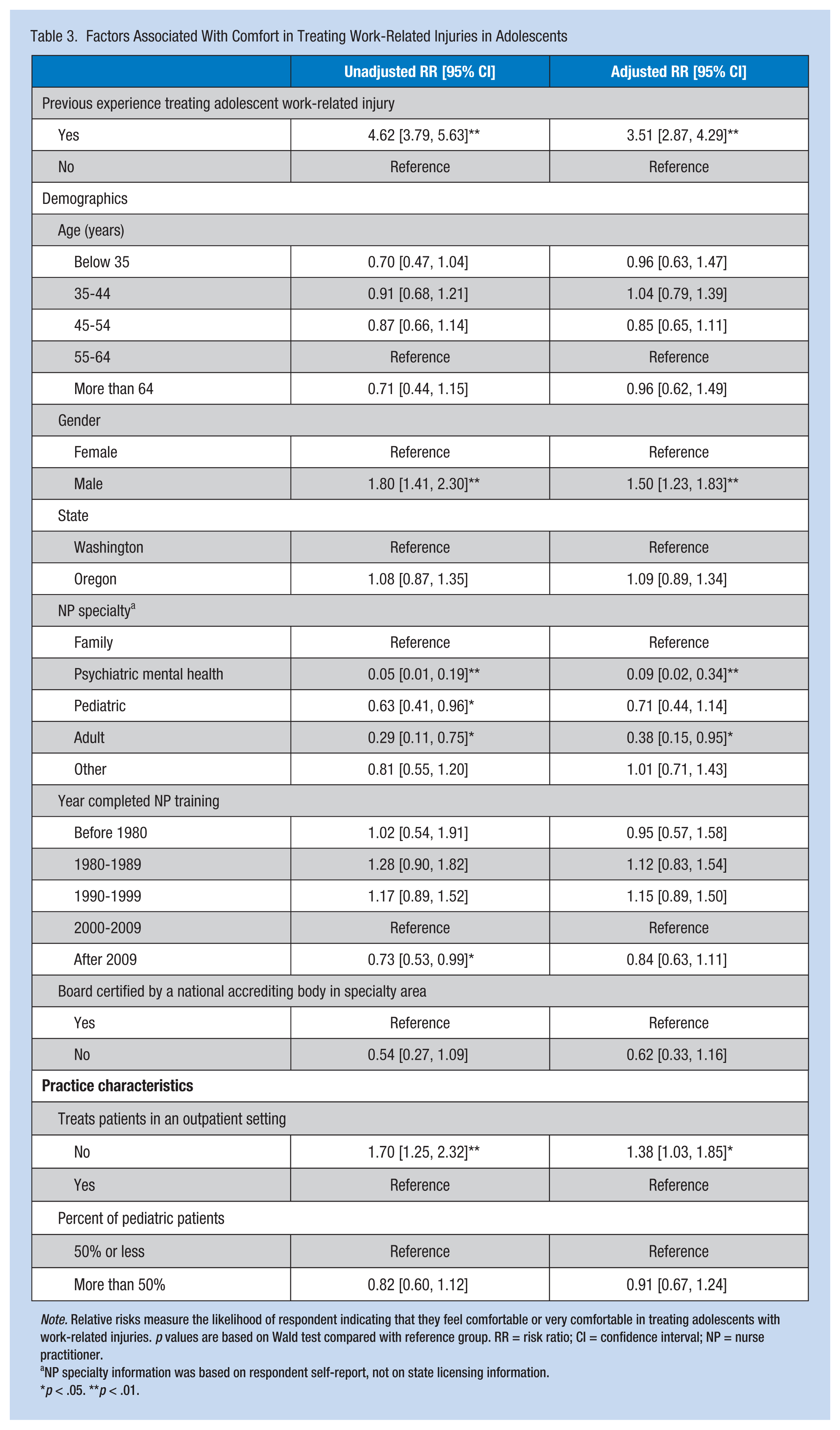
Note. Relative risks measure the likelihood of respondent indicating that they feel comfortable or very comfortable in treating adolescents with work-related injuries. p values are based on Wald test compared with reference group. RR = risk ratio; CI = confidence interval; NP = nurse practitioner.
NP specialty information was based on respondent self-report, not on state licensing information.
p < .05. **p < .01.
Discussion
In Washington and Oregon, NPs have statutory authority to treat work-related injuries for all patients, including adolescents. In this study, few NPs reported previous experience in treating work-related injuries for this priority population, potentially due to the relatively low incidence of adolescent work-related injuries in these states or the types of settings in which study respondents worked. Although accurate estimates of all work-related injuries among adolescents are difficult to determine, partially due to underreporting, which is common among young workers (Linker, Miller, Freeman, & Burbacher, 2005), WC data provide estimates of reported claims in Washington and Oregon. Washington WC data from 1988 to 1991 showed 19.4 injuries per 100 adolescent workers, resulting in an average of 4,450 claims per year (Miller & Kaufman, 1998). More recent data from Oregon (1990-1997) showed an average 1,008 accepted adolescent claims per year, with a much lower estimated claim rate of 1.3 (95% CI = [1.2, 1.4]) per 100 adolescent workers (McCall, Horwitz, & Carr, 2007).
Nurse practitioners in Washington and Oregon are familiar and comfortable treating adolescents with work-related injuries. However, this study showed that nearly one in two NPs in these states reported at least some level of discomfort. Previous experience in treating adolescent work-related injuries was positively associated with increased comfort. In these states and others where NPs have expanded scope of practice to treat WC claimants, it is crucial that NPs receive appropriate training and education to prepare them to treat injured young workers specifically. Study results suggest that male NPs were more likely to report previous experience in treating adolescent work-related injuries. Reasons for this finding could be differential clinic settings or variability in patient panels across male and female NPs. Future research may be warranted to determine whether male NPs are more likely to work in occupational clinics or other types of settings for injured workers and whether male NPs receive more referrals for adolescent males (who exhibit a higher injury incidence overall).
For young workers, underreporting of work-related injuries is a challenge. A recent study showed that among 4,554 young (predominately aged 14 to 25 years), part-time Canadian workers who indicated that they had missed work time due to work-related injuries on at least one occasion, 48.5% (n = 2,207) did not report this injury to a physician (Tucker et al., 2014). Although not reported in the Canadian study, a proportion of individuals with work-related injuries did seek treatment but did not disclose the occupational nature of the injuries (Azaroff, Levenstein, & Wegman, 2002). Provider–patient relationships are a component of reporting work-related injuries. Health care providers, including NPs, can provide education and support to injured workers who may minimize their injuries, believe their injuries are not job-related, or are unaware of the WC process (Shannon & Lowe, 2002).
Nurse practitioners can play significant roles in the prevention of work-related injuries among adolescents. Given that most adolescents are employed at some point in high school, an inquiry or discussion about teens’ jobs at annual well-child visits are both appropriate and prudent (Runyan, 2007). Questions focusing on work-related safety can be incorporated into routine well-child history forms for adolescent patients to guide open inquiry. Materials are also available, which specifically target adolescents and younger children in rural environments who may be informally employed on family farms (“Farm Safety Just for Kids”; Runyan, Lewko, Rauscher, Castillo, & Brandspigel, 2013).
The limitations of this study include self-report and low response rate. Nurse practitioners’ experience and comfort were measured by self-report, which is subject to recall or social desirability bias. The response rate for this survey was 23%, which is similar to other surveys of health care providers (Chrisman, Schiff, & Rivara, 2011; Kinnaman, Mannix, Comstock, & Meehan, 2013; Perhats et al., 2012; Rosenfeld, Kobayashi, Barber, & Mezey, 2004). However, results of this survey may not fully represent the population of NPs in Washington and Oregon. The parent survey, in which the work-related injury questions were included, focused on adolescent concussions, so respondents to this survey may have been more interested in the adolescent population or head injuries than the general population of NPs in these states. Although the researchers used postestimation weights to account for differential response rates by state and specialty, this procedure could not account for all differences. Finally, the brief nature and online format of this survey did not allow for a more nuanced investigation of NPs’ experiences or comfort levels. Indeed, additional exploration, perhaps using qualitative approaches, may better describe NPs’ level of comfort in treating adolescents and work-related injuries.
This study documents the need for developing educational and outreach efforts to better prepare NPs to treat work-related injuries among adolescents. Practicing NPs should familiarize themselves with each state’s WC guidance, and apply these regulations to their specific practice setting and screening examination forms. The National Institute for Occupational Safety and Health (NIOSH) provides information and recommendations for the prevention of work-related injuries (U.S. Department of Health and Human Services, 1995), as do academic articles (Linker et al., 2005; Miara, Gallagher, Bush, & Dewey, 2003; Ward et al., 2010). Raising awareness of the specific needs of and resources for adolescent workers can also enhance the comfort levels of NPs who routinely counsel children regarding safety at home and during recreation.
Implications for Practice
Many NPs serve as primary care providers for teens, most of whom will likely work during adolescence. As care providers, it is critical that NPs recognize the potential exposures and risks relevant to their patient population. In the case of teens, NPs should be aware of their patients’ potential exposures at work and their high risk for occupational injury. This study shows that NPs have limited experience treating adolescents with work-related injuries and few report feeling comfortable doing so.
NIOSH has prioritized incorporation of industry and occupational data elements into electronic health records (Baron et al., 2013), certainly a first step in alleviating providers’ burdens and ensuring consistency across providers and facilities. Until this initiative is achieved, however, all providers, including NPs, should inquire about their patients’ work and be familiar with potential occupational exposures. For adolescent patients, NPs should be aware that teens are at increased risk for work-related injuries.
Within many health systems, especially those with integrated coverage and health care (e.g., health maintenance organizations), it is common practice for providers to ask whether adults’ injuries occurred at work. This practice should also be standard for adolescent patients to ensure that these injuries are appropriately attributed to their source and cause, and that the correct steps are taken to ensure appropriate reporting and treatment.
Caring for patients with work-related injuries often includes knowledge of WC programs or systems in a particular region or state. To be prepared for adolescent patients with work-related injuries, providers with panels of predominantly adolescent patients should familiarize themselves with these processes. Nursing personnel who work with adolescent patients have multiple opportunities through school, sports, and other wellness examinations to educate adolescents about laws in their states. Washington State, for example, has developed a series of videos and resources that can be used to educate parents and adolescents regarding related laws (Washington State Department of Labor and Industries, 2015). These resources can also be used to raise awareness among those professionals who provide health care to these workers.
Applying Research to Practice
This research demonstrated that the more often NPs treat adolescent patients for work-related injuries, the more comfortable NPs become in doing so. Nurse practitioners may have already treated adolescents for work-related injuries but neglected to identify the injuries as occupational. Use of screening tools and educational resources discussed in this article may educate NPs, their colleagues and patients to better identify individuals injured on the job. Knowledge of the particular needs of adolescents and their risk factors for injuries should be incorporated into continuing education opportunities for nurses in all practice settings. Because of their unique statutory role, NPs who can legally authorize and manage care for injured workers are particularly important targets for continuing education and awareness outreach. Sharing tools and websites with adolescents in multiple settings and through multiple methods (e.g., social media and phone-based applications) could generate more inquiry from adolescents when they interact with their health care providers during routine nonacute visits. Further research regarding barriers to care provision (e.g., fear of legal processes or concern about parental involvement) may enhance NP comfort with treating adolescent workers and in turn advocating for their continued safety in the workplace.
Footnotes
Acknowledgements
The authors thank Thom Allen at the Washington State University Social and Economic Sciences Research Center (SESRC) for his assistance in survey administration and management. The authors also thank all of the NPs who completed the survey that informed this study.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the Washington State University New Faculty Seed Grant and the American Nurses Foundation/Western Institute of Nursing Grant.
Author Biographies
Janessa M. Graves is an assistant professor at the Washington State University College of Nursing in Spokane, Washington. Her research focuses on pediatric injuries and occupational safety and health among young workers.
Tracy A. Klein is an assistant professor at Washington State University College of Nursing in Vancouver, Washington. A family nurse practitioner, Dr. Klein is a regulatory and health policy expert in scope and prescribing practices of advanced practice nurses.
