Competencies for Occupational and Environmental Health Registered Nurses (RN)
Occupational and environmental health nursing is a subspecialty of public/community health nursing, with unique knowledge and skill sets not found in other nursing specialties. The American Association of Occupational Health Nurses, Inc. (AAOHN) has developed several documents (i.e., The Code of Ethics and Interpretive Statements, Standards of Occupational and Environmental Health Nursing, Competencies in Occupational and Environmental Health Nursing, and The Fundamentals of Occupational and Environmental Health Nursing, AAOHN Core Curriculum 4th Edition) that serve as the framework for the specialty practice of occupational and environmental health nursing. Together, these documents:
define the scope of occupational and environmental health nursing;
provide an ethical framework for occupational and environmental health nursing practice;
delineate principles supporting essential practice knowledge;
describe the abilities required for competent practice; and
provide a comprehensive resource for occupational and environmental health nurses.
All practicing occupational and environmental health nurses must adhere to various standards, regulations, and guidelines that apply to delivery of nursing care in their practice settings. The AAOHN foundational documents are an invaluable source of information for all occupational and environmental health nurses to assure delivery of competent, ethical, and legal nursing care.
It is incumbent upon the profession to maintain the documents describing the competencies required for occupational and environmental health nurses. AAOHN first established competencies for occupational and environmental health nurses in 1999, detailed by nine categories and three competency levels (AAOHN, 1999). The competencies were revised in 2003 and 2007, still retaining the nine categories and the levels of competent, proficient, and expert. Each revision attempted to simplify the language; shorten, streamline and reduce duplication in the competencies to clarify them for the profession, individual nurses and employers; and provide a baseline for certification support, performance evaluations, and developmental plans (AAOHN, 2003; AAOHN, 2007).
Since the last update of the AAOHN competencies was published, occupational and environmental health nursing has evolved, necessitating an in-depth review of existing competencies. New terminology and scientific evidence have expanded the knowledge base for practice. The United States (U.S.) healthcare system has changed dramatically. Numerous occupational and environmental health nurses have assumed global responsibilities for the health and safety of workers outside the US, and many workforces include expatriates and frequent international visitors and workers. Likewise, the specialty now includes more advanced practice nurses than was the case in 2007, and AAOHN expanded membership to include Licensed Practical/Vocational Nurses (LPN/LVN) in 2011. In 2014, the AAOHN Board of Directors created a Task Force of experts with diverse occupational and environmental health nursing backgrounds to revise and update the Competencies for Occupational and Environmental Health Nursing.
Competencies reflect the proficiencies required to perform a particular task or play a defined role (Oerman & Gaberson, 2013). Competencies are guidelines applicable to occupational and environmental health nurses who assume a variety of practice roles; competencies address the continuum of practice experiences. AAOHN (1999) defines competencies as outcome-oriented statements that describe the mastery of a particular skill or ability. To maintain competence, each health care professional is expected to manage an evolving scope of practice. Competencies do not address educational preparation or licensure. In addition to registered nurses (RNs) working in occupational health, LPN/LVNs may provide supportive, technical services in an occupational setting; but they must always work under supervision of (registered) nursing or medical personnel (AAOHN Position Statement, 2012). All nurses can enroll in continuing education courses offered by AAOHN and other organizations to learn the basics of occupational health nursing, and develop specific knowledge and skills to deliver occupational programs and services, such as spirometry and audiometry screenings. AAOHN specifically encourages LPNs/LVNs and non-BSN-prepared RNs to complete university degrees. Since LPNs/LVNs must have technical tasks delegated to them by RNs or medical personnel, these revised competencies are specifically written for registered professional nurses who work in occupational and environmental health.
Methods
To establish content validity (Grant & Davis, 1997), the Task Force included AAOHN members who practice across multiple geographic locations and represent single and multi-nurse units and hospitals/healthcare, manufacturing, education, global and military sectors. They practice clinically as BSNs and nurse practitioners, risk management/safety/environmental professionals, case managers, health promotion/wellness/chronic disease managers, consultants, and researchers.
Four members of the Task Force and the chair were doctorally-prepared clinicians, academicians, or researchers. Five more members were master’s-prepared clinicians with significant experience in their practices. Three were BSN-prepared and one had a diploma in nursing. Ten members were certified occupational health nurses (COHN or COHN-S). Every member had published in a peer-reviewed occupational health nursing journal or book. Several members had presented continuing education seminars and others had taught academic courses in occupational health nursing. Several Task Force members had served in elected positions in AAOHN at the national and/or state level. All members of the team contributed individually to the development, revision, and approval of the final version of the competencies document.
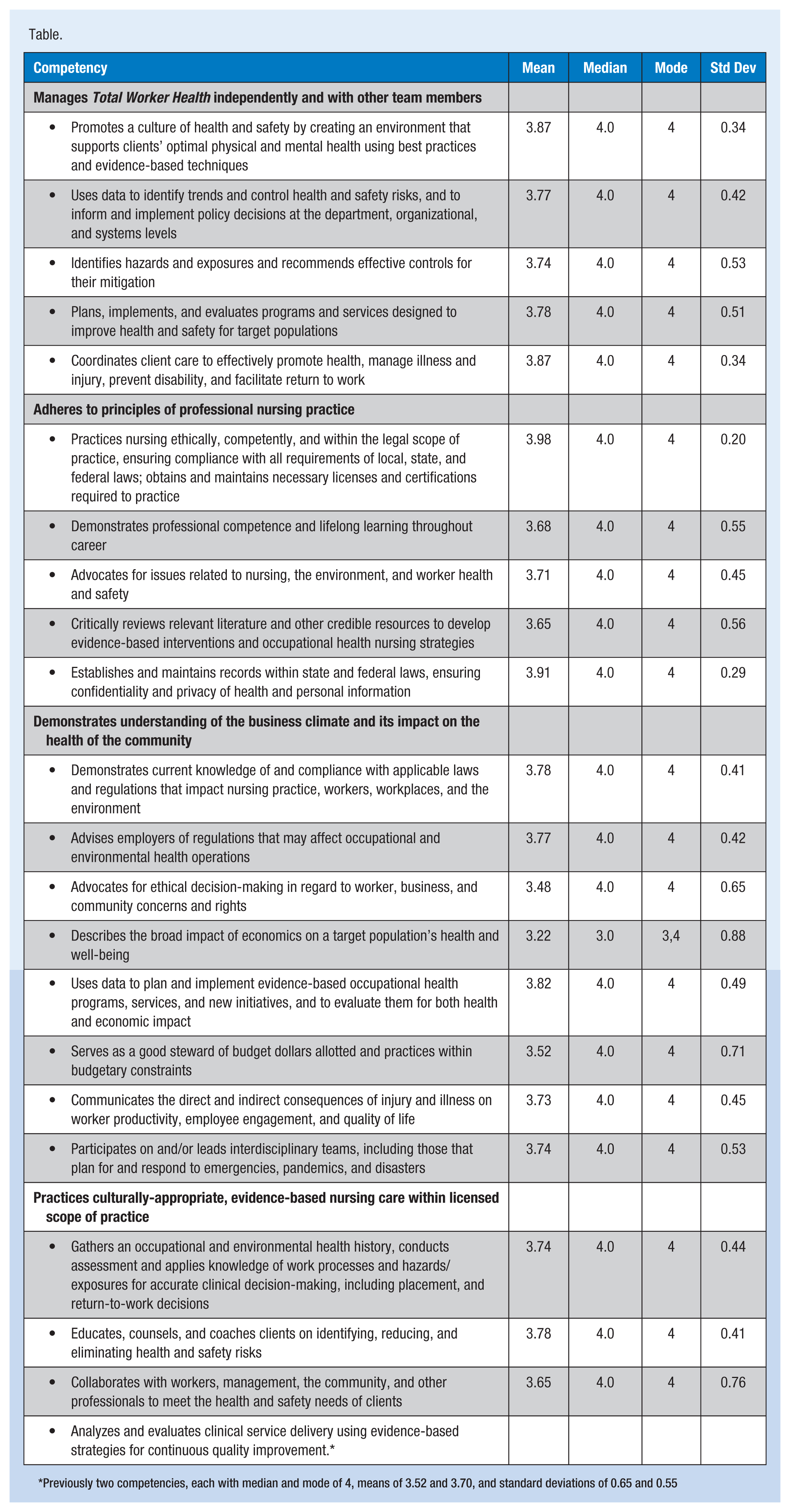
During eight telephone and one face-to-face meeting held over 15 months during 2014 and 2015, the Task Force extensively reviewed the literature, specifically documents containing the competencies of other professions (ACHE, 2012; ACOEM, 2014; Council on Linkages Between Academia and Public Health Practice, 2010; Fouad et al, 2009; Interprofessional Education Collaborative Expert Panel, 2011) and drew upon their own expertise to provide a framework for the revised document. The Task Force agreed that more emphasis should be placed on wellness and health promotion, evidence-based practice, and caring for the working populations and communities that occupational and environmental health nurses serve. The Task Force drafted a document containing four categories under which 22 competencies were organized (Table). The Task Force used a two-round modified Delphi process to validate their work (Lee, Johnson, Newhouse & Warren, 2013).
The Delphi method is widely used to build consensus on a topic. Its advantages are anonymity and the avoidance of bias due to the influence of a single individual (Huss & Shadford, 2007). The Task Force identified a second panel of thirty geographically-dispersed occupational and environmental health nurse experts representing diverse industries, universities providing occupational and environmental health nursing continuing education and advanced degrees, managers of occupational health programs, RNs and occupational health nurse practitioners, to participate as competency reviewers. Two iterations were reviewed to achieve consensus by the review panel (Polit & Beck, 2008).
The thirty occupational and environmental health nurse expert reviewers were contacted via email and asked to complete an on-line survey. For each competency, reviewers were asked to rate the competency’s relevance on a 4-point Likert scale: Not relevant, Somewhat Relevant, Quite Relevant, or Highly Relevant. The second question for each competency asked whether the item was well-written and distinct (yes/no). Each competency included a comment box as well as an opportunity to provide general comments at the end of the survey. Reviewers were asked to complete the survey within two weeks, at which time the survey was closed and results were analyzed.
Prior to sending the survey for the first round of the Delphi process, the Task Force agreed that to be included in the final document, a competency had to have a median score of at least 3.25, with 70% of the responding experts scoring the competency as Quite Relevant or Highly Relevant (3 or 4).
For the first round, only 13 experts (43%) completed the survey. Based on the feedback received from those experts, the Task Force revised the competencies. These revisions were included in the survey for the second round. Prior to the second modified-Delphi round, the 30 experts were contacted via email to alert them of the survey that would be arriving shortly. The link to the survey was then sent via email from AAOHN staff, rather than an automated Survey Monkey email. Expert panelists were given two weeks to complete the survey. A reminder email was sent in the middle of the second week to all participants, encouraging them to complete the survey if they had not already done so.
Task Force members who attended the Committees Meeting at the 2015 AAOHN Conference in Boston in March, discussed the results and the feedback received. Changes were made to some competencies based on feedback from the Delphi panelists. One competency did not achieve the a-priori requirement of a median score of at least 3.25, so Task Force members were surveyed to determine whether the competency should be included as written.
Results
For the second round, 23 experts (77%) completed the survey. Nearly all competencies met the a-priori standards of a median score of at least 3.25 with 70% of the responding experts scoring the competency as Quite Relevant or Highly Relevant (3 or 4) (Table). Many comments were submitted, and explanations in this article address the concerns voiced by the experts. The resulting 22 competencies divided among four categories are discussed here.
Manages Total Worker Health Independently and With Other Team Members
Promotes a culture of health and safety by creating an environment that supports clients’ optimal physical and mental health, using best practice and evidence-based techniques. Three Delphi panel members (13%) said that this competency is quite relevant, and 20 (87%) said this competency is highly relevant. One panelist recommended adding “wellness” to the competency. The World Health Organization (WHO) defines health as, “… a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity” (WHO, 1948, Preamble to the Constitution). In 2011 the National Institute for Occupational Safety and Health (NIOSH) created a program called Total Worker Health ™, which is defined as, “… a strategy integrating occupational safety and health protection with health promotion to prevent worker injury and illness and to advance worker health and well-being” (NIOSH, 2014, para 2). Although “wellness” is a term commonly used interchangeably with health promotion, neither NIOSH nor WHO includes this term in its definition, but both address individual well-being.
Uses data to identify trends and control health and safety risks, and to inform and implement policy decisions at the department, organizational, and systems levels. Five panelists (23%) said this competency is quite relevant, and 17 (77%) said it is highly relevant. Three panelists said the competency could have been written differently to provide more clarity, though 19 said the competency was well-written and distinct. One commenter suggested that this competency is not appropriate for front-line nurses, and should be reserved for managers. Another commenter suggested this competency is so enormous that it alone could be a full-time job. This competency does not suggest that the occupational and environmental health nurse must be solely responsible for using data for these reasons. However, given the grounding of occupational and environmental health nursing practice within population or public health, the occupational and environmental health nurse should be examining data. When several workers come from the same department with similar health problems in a given time period, the occupational and environmental health nurse must identify potential health or safety risks that should be addressed. Likewise, when policies are suggested, the occupational and environmental health nurse should provide input to decision-makers. Front-line occupational and environmental health nurses may not always be asked for data-based information, but occupational and environmental health nurses should be able to provide data when necessary.
Identifies hazards and exposures, and addresses effective controls for their mitigation. One panelist (4%) said the competency was somewhat relevant, 4 (17%) said the competency was quite relevant, and 18 (78%) said it was highly relevant. Three recommendations were made to improve the clarity of the item. One panelist said that the occupational and environmental health nurse does not always identify hazards, but rather recognizes health issues. Another panelist suggested that occupational and environmental health nurses work collaboratively with other team members to identify hazards. Occupational health nurses should learn to recognize worker health issues. It is insufficient for nurses to merely identify an employee’s rash; rather the occupational and environmental health nurse must determine which work processes are essential to the employee’s job, and the hazards to which the employee may be exposed. Occupational health nurses will need to ask questions of and collaborate with other team members, particularly when the occupational and environmental health nurse is a novice in the field. However, occupational and environmental health nurses who understand the work performed by workers in their companies will be able to identify hazards accurately.
Plans, implements, and evaluates programs and services designed to improve health and safety for target populations. One panelist (4%) said this competency is somewhat relevant, three (13%) said it is quite relevant, and 19 (83%) said it is highly relevant. Recommendations included adding language to emphasize health promotion or wellness, including language about collaboration, and specifying the working population. As discussed earlier, health promotion and wellness are included in the concept of health; when health improves, a higher level of wellness is achieved. This competency uses “target populations” rather than “worker populations” for environmental health nurses who may work in other non-occupational settings.
Coordinates client care to effectively promote health, manage illness and injury, prevent disability, and facilitate return to work. Three respondents (13%) said this competency was quite relevant, and 20 (87%) said it was highly relevant. Comments included recommendations to add language that addresses health promotion, and that change was made. A question was posed as to whether the occupational and environmental health nurse can really “prevent disability.” The focus of case management is largely to prevent permanent disability by ensuring clients are receiving the care they need and are following instructions related to treatment (AAOHN, 2012).
Adheres to Principles of Professional Nursing Practice
Practices nursing ethically, competently, and within the legal scope of practice, ensuring compliance with all requirements of local, state, and federal laws; obtains and maintains necessary licenses and certifications required to practice. One panelist (4%) said this competency was quite relevant, and 22 (96%) said it was highly relevant. A question was posed about obtaining and maintaining necessary licenses and certifications required to practice. In the United States, all practicing occupational and environmental health nurses must be licensed in every state where they engage in activities that would be considered nursing care. Occupational and environmental health nurses with responsibility for occupational health programs in more than one state should contact the state board of nursing when it is unclear whether a license to practice is required for the work being done in that state. The Nurse Licensure Compact by the National Council of State Boards of Nursing (NCSBN) currently has 25 participating states. Nurses may not need a separate license if they work in a compact state, but must know and abide by the Nurse Practice Act of the state in which they work.
Demonstrates professional competence and lifelong learning throughout career. One respondent (5%) considered this competency to be somewhat relevant, 5 (23%) said it was quite relevant, and 16 (73%) said it was highly relevant. One panelist said that it would be difficult to measure “lifelong learning throughout career” and suggested the competency be limited to something more present-oriented. The Task Force felt strongly that, although employers may not be interested in occupational and environmental health nurses’ lifelong learning, including this competency would communicate to employers that occupational and environmental health nurses must continue to read, attend seminars and conferences, and network with colleagues to ensure professional growth. Further, continuing professional education is required for recertification and may be required by the state for continuing licensure.
Advocates for issues related to nursing, the environment, and worker health and safety. Six panelists (29%) said this competency is quite relevant, and 15 (71%) said it is highly relevant. Suggestions were made to be more precise by using “work environment”; however, environmental health nurses are also concerned about the greater community’s environment. For example, if the public’s water and air are polluted, it is appropriate for occupational and environmental health nurses to speak to the need for clean air and water.
Critically reviews relevant literature and other credible resources to develop evidence-based interventions and occupational health nursing strategies. One panelist (4%) said this competency is somewhat relevant, 6 (26%) said it is quite relevant, and 16 (70%) said it is highly relevant. All panelists indicated that this item is well-written and distinct.
Establishes and maintains records within state and federal laws, ensuring confidentiality and privacy of health and personal information. Two respondents (9%) said this competency is quite relevant, and 20 (91%) said it is highly relevant. Ninety percent of respondents said the competency is well-written and distinct.
Demonstrates Understanding of the Business Climate and Its Impact on the Health of the Community
Demonstrates current knowledge of and compliance with laws and regulations that impact nursing practice, workers, workplaces, and the environment. Five panelists (22%) said this competency is quite relevant, and 18 (78%) said it is highly relevant. One panelist said that the competency should focus on “regulations of nursing practice that impact workers” because laws impacting nursing practice seemed confusing. If a nurse practitioner (NP) works in a state that requires NPs to have a written agreement with a “supervising physician,” that NP must obtain the necessary documentation to practice. If the NP is not familiar with regulations that impact practice, that legal requirement may not be met. Another reviewer commented that regulations such as the Americans with Disabilities Act (ADA), Genetic Information Nondiscrimination Act (GINA), Family and Medical Leave Act (FMLA) and Occupational Safety and Health Administration (OSHA) standards should be specified in this competency. However, because regulations are frequently introduced, specifying existing regulations would immediately outdate this competency.
Advises employers of regulations that may affect occupational and environmental health operations. Five panelists (23%) said this competency is quite relevant, and 17 (77%) said it is highly relevant. Ninety-five percent of the respondents felt this item was well-written and distinct.
Advocates for ethical decision-making in regard to worker, business, and community concerns and rights. Two panelists (8%) said this competency is somewhat relevant, 8 (35%) said it is quite relevant, and 13 (57%) said it is highly relevant. One expert said that the greater team (Human Resources, Legal) should be specified because occupational and environmental health nurses may not share this role. However, the Task Force felt that nurses must address ethical issues when they arise. For 14 of the last 15 years, the nursing profession has been the most trusted profession, according to the Gallup Poll (Rifkin, 2014). Part of the reason nursing is so highly regarded is because nurses are ethically grounded. At the very least, occupational and environmental health nurses should express their concerns to their supervisors. For example, when a nurse learns that employees do not wish to report injuries as work-related for fear of reprisal from management, the occupational and environmental health nurse should bring that issue to the attention of management.
Describes the broad impact of economics on a target population’s health and well-being. This is the only competency that did not achieve a median score of 3.25; however, the Task Force felt that the competency is essential and the majority agreed to include it in the final document. Two experts (9%) said this competency is not relevant, 1 (4%) said it is somewhat relevant, and 10 each (44%, 44%) said it is quite relevant and highly relevant. Although only 2 experts (9%) did not agree that the item is well-written and distinct, several provided comments. Among the comments was a general concern that occupational and environmental health nurses may not possess the knowledge or skills to meet this competency. One reviewer questioned how nurses would learn to meet this competency. At the most basic level, occupational and environmental health nurses should understand that issues such as lay-offs or threats of lay-off cause stress to workers, and workers under stress are at greater risk of illness. Occupational and environmental health nurses should also understand that poor lifestyle choices increase the risk for negative health outcomes; illness, injury, and disease result in increased use of the health care system, resulting in greater costs. Occupational and environmental health nurses must appreciate the needs of part-time workers who may not have company benefits, and the economic impact on their health. Occupational and environmental health nurses must recognize that most companies exist to support owners’ and shareholders’ profit. Companies that do not make a profit are not viable long term (even “non-profits” and “not-for-profits” must earn sufficient profits for sustainability). Additionally, occupational and environmental health nurses should know that if an employer goes out-of-business and employees lose their jobs, the entire community is affected. Workers without jobs may not be able to buy products and services. Unemployment has a trickle-down effect on businesses in the community because the unemployed may not be able to purchase goods and services from local businesses, thus resulting in more unemployment.
Uses data to plan and implement evidence-based occupational health programs, services, and new initiatives, and to evaluate them for both health and economic impact. One expert (5%) said this competency is somewhat relevant, 2 (9%) said it is quite relevant, and 19 (86%) said it is highly relevant. One reviewer suggested that this item is very high level and would be difficult to demonstrate. Evidence-based practice is being taught in all BSN programs, and it is a topic commonly seen in professional nursing journals, including Workplace Health & Safety, the professional journal of AAOHN. Planning and implementing cannot be done without assessment, and data are the outcome of any assessment. Evaluation is part of the basic nursing process, which all nurses learn prior to licensure. Certainly, as occupational and environmental health nurses accrue experience and education, their data collection efforts and evaluations will become more refined. Even nurses new to occupational health have the skills necessary to meet this competency to some degree. More experienced nurses have additional skills in providing evidence-based information and justification for health and safety programming using cost-benefit analyses.
Serves as a good steward of budget dollars allotted and practices within budgetary constraints. One panelist (4%) said this competency was not relevant, 8 (35%) said it was quite relevant, and 14 (61%) said it was highly relevant. The previous wording on this competency was unclear to many panelists, so it was reworded as one expert suggested. Nurses who accept occupational health positions after working in acute-care institutions may believe that “nurses are necessary.” Nurses who have worked in occupational health often learn that their services are necessary only as long as those who control the budget believe nurses are necessary. In many settings, occupational health is a “cost center,” meaning it does not generate income the way other departments may. Prudent occupational and environmental health nurses ensure that they are practicing efficiently, not wasting time or other resources. Most occupational and environmental health nurses are proactive by not waiting for injured employees to arrive at the occupational health clinic, but rather actively seek opportunities to prevent injuries and illnesses. Experienced nurses may perform cost-benefit analyses to decide if the company would benefit from internal versus outsourced health services.
Communicates the direct and indirect consequences of injury and illness on worker productivity, employee engagement, and quality of life. Six experts (27%) said this competency is quite relevant, and 16 (73%) said it is highly relevant. Some respondents wanted more detail included in this competency, such as to whom and why the occupational health nurse communicates this information, and the benefits of preventing illness and injury. The competency was intentionally left succinct to not constrain nurses with varying circumstances (e.g., reporting structures) in their workplaces. For example, some nurses may communicate with management, while others may communicate with the chief executive officer (CEO). None of the competencies includes rationale for the competency, so the “why” was not addressed here either. Another expert was concerned that many occupational and environmental health nurses do not understand the meaning of employee engagement. If that is the case, then this competency can guide occupational and environmental health nurses in their educational goal-setting.
Practices Culturally-Appropriate, Evidence-Based Nursing Care within Licensed Scope of Practice
Gathers an occupational and environmental health history, conducts assessment, and applies knowledge of work processes and hazards/exposures for appropriate clinical decision-making, including placement, fitness-for-duty, and return-to-work decisions. Six respondents (26%) said this competency is quite relevant, and 17 (74%) said it is highly relevant. “Fitness for duty” was added based on one reviewer’s comment.
Educates, counsels, and coaches clients on identifying, reducing, and eliminating health and safety risks. Five experts (22%) said this competency is quite relevant, and 18 (78%) said it is highly relevant. “Identifying” was added to this competency based on a comment from one expert. Another expert wanted to include some reference to personal protective equipment in this competency, but because that is just one method of achieving this competency, it was ultimately not included. A third respondent said that the use of “client” sounds impersonal, and it is difficult to discern employee from the company. In this competency, the client could, indeed, be the company. Not only should individuals understand how to reduce their personal risk, but the company should also be reducing risk to all employees by applying engineering and administrative controls. For instance, if the company can buy equipment that produces less noise, employees may not need to wear hearing protection devices.
Collaborates with workers, management, the community, and other professionals to meet the health and safety needs of clients. One expert (4%) said this competency is not relevant, one (4%) said it is somewhat relevant, 3 (13%) said it is quite relevant, and 18 (78%) said it is highly relevant. The client in this case can be an individual, department, company, or community.
Analyzes and evaluates clinical service delivery using evidence-based strategies for continuous quality improvement. This competency was created after the second round of the modified Delphi process by combining two very similar competencies. The original competencies separately focused on clinical care (Evaluates effectiveness of care within a quality improvement framework) and other occupational health programs (Analyzes and evaluates clinical service delivery using evidence-based strategies; recommends improvements). The original competencies were rated highly with 91% judging the first competency and 96% judging the second competency to be quite relevant or highly relevant. The Task Force was unanimous in their agreement that the combined competency addresses the intent of the previous two competencies. This competency can include conducting chart audits for quality, time studies for efficiency measures, customer satisfaction surveys, or other approaches.